Abstract
We present the case of a 12-year-old girl with severe pernio as the sole clinical presentation of celiac disease (CD), without associated gastrointestinal symptoms. Lesions greatly improved once a gluten free diet was initiated. At 5-year follow-up, she remains in clinical remission throughout the year with no pharmacological treatment, without skin lesions flare-up in the winter months.
Introduction
Pernio, or chilblains, is an inflammatory condition precipitated by cold temperature affecting acral sites with tender erythemato-violaceous macules, papules or nodules. 1 Lesions can also blister or ulcerate. It is generally idiopathic, but secondary causes have been described, including systemic lupus erythematosus (SLE). 2 Its pathophysiology is still poorly understood, but appears to be mostly related to vasoconstriction/vasospasm following the exposure to cold temperature. Treatment is symptomatic and includes avoidance of precipitating factors (cold temperature, smoking). Topical corticosteroids and calcium channel blockers like nifedipine can also be helpful. 1
Celiac disease (CD) is a chronic autoimmune enteropathy caused by gluten intolerance in genetically predisposed individuals. Classic gastrointestinal symptoms are mainly triggered by malabsorption and include abdominal pain and distension, diarrhea, weight loss, steatorrhea and nutritional deficiencies.3,4 A mild presentation or complete absence of gastro-intestinal symptoms is also possible. 4 Extra-intestinal manifestations, such as skin manifestations, may be the only clue leading toward the diagnosis of CD. 5 Dermatitis herpetiformis (DH) is a well-known manifestation, but several other skin conditions have also been related with CD. We are presenting the case of a 12-year-old girl in whom the only presenting symptom of CD was pernio.
Case report
A previously healthy 12-year-old girl was initially referred to the dermatology division for lingering painful lesions localized at the tip of her fingers, toes and ears. Lesions were ongoing for the past 5 years, occurring yearly from around October to mid-April when weather was cold and intensified over years. Patient describes erythema of her fingers and toes accompanied by some degree of swelling and a tingling sensation. She denied taking any medication. The review of systems, including gastro-intestinal symptoms and weight loss, was negative. Family history was irrelevant except for iron deficiency anemia in her mother, and a history of pernio for her father.
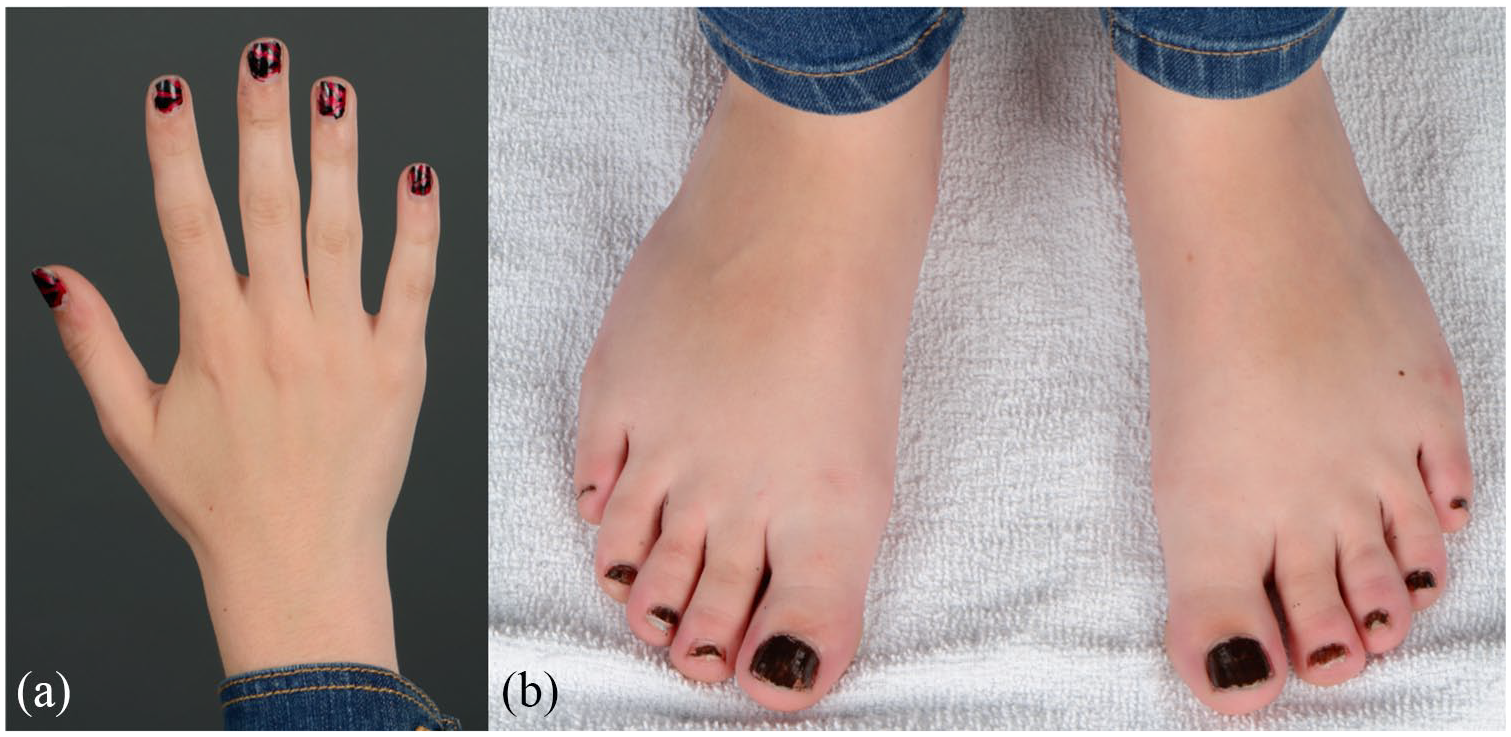
Physical examination demonstrated erythematous to violaceous macules and edematous papules on the distal portion of the fingers and toes (Figure 1(a) and (b)). These typical lesions in conjunction with the patient’s observations led to the diagnosis of pernio. No ulcers, skin tightening or vasculitic lesions were noted. The patient also exhibited onychodystrophy, probably induced by poor blood supply in cold weather due to pernio. The remainder of the physical exam was normal.

Erythematous to violaceous macules and papules on the distal portion of the (a) fingers and (b) toes few months after the initial presentation of the patient.
Nifedipine up to 20 mg daily was initially prescribed and symptoms slightly improved. Losartan 25 mg daily was substituted when new lesions appeared on the heels and ears despite treatment.
Further evaluation was done in conjunction with a rheumatologist. No connective tissue disease symptoms were found except for the typical lesions of pernio. Work-up revealed positive ANA at a titer of 1/320, although other autoantibodies (including extractable nuclear antigens (ENA) and anti-dsDNA) were negative. The remaining laboratory tests were all normal, including thyroid function and cryoglobulins. Interestingly, the mother suggested testing for anti-tissue transglutaminases (TTG) as she had herself found in the literature cases of pernio associated with CD. TTG came back significantly positive at a titer of 55 units/mL (normal value < 10).
Patient was therefore referred to gastroenterology. The gastroduodenoscopy revealed a flattened appearance of the mucosa associated with multiple scars. Biopsies were performed and revealed typical changes of CD (complete loss of villous architecture and crypt hyperplasia). A gluten-free diet was then established and cutaneous symptoms greatly improved in the following months (Figure 2(a) and (b)). Patient was able to stop her medication, especially Losartan as it may contain gluten. Anti-TTG antibodies decreased throughout follow-up and the rheumatologic work-up remained negative. Patient remained in clinical remission off pharmacological treatments, except for one episode associated with accidental gluten exposure.
A complete resolution of the lesions can be seen on the (a) fingers and (b) toes few months after the gluten-free diet was introduced.
Discussion
CD is a gluten-sensitive enteropathy caused by gliadin, a protein component of gluten. It is characterized by malabsorption in the small intestine that can lead to nutritional deficiencies. The suspicion of CD relies on symptoms and serologies such as positive anti-TTG antibodies, while the diagnosis relies mainly on duodenal biopsies as well as a positive response to a gluten-free diet.6–8 However, several cases of CD can be clinically silent and cutaneous symptoms can be the only manifestation of the underlying disease.7,8 Early diagnosis is important to prevent the development of further complications such as T- and B-cell lymphoma and intestinal adenocarcinoma. 6
Skin manifestations are known to be associated with CD, dermatitis herpetiformis (DH) being the most common by far, although less than 25% of pediatric patients will have these lesions. Multiple cutaneous signs have also been described in case series or case reports, such as alopecia areata, chronic urticaria, aphthous stomatitis, vitiligo, cutaneous vasculitis, linear IgA dermatosis, erythema elevatum diutinum and auto-immune connective tissue disorders.5,9 Various hypotheses have been studied: autoimmune inflammatory response secondary to altered intestinal permeability to antigens, vascular alterations, increased number of T-cells and nutritional deficiencies.3,10 Multiple studies have also reported a possible correlation between SLE and CD.10–12 However, our patient had no positive rheumatologic findings other than a positive ANA at 1/320.
Many diseases of abnormal sensitivity to cold (DASC) are known, including acrocyanosis, Raynaud and pernio, the latter being the most common. DASC can be primary or secondary to collagen vascular diseases, vasculitis, nutritional disorders and an early manifestation of lupus in some patients. 2 Severe cases could even display blisters or ulcers. 13 Numerous hypotheses have been discussed for the pathogenesis such as vasoconstriction/vasospasm inducing inflammation, as seen in anorexia nervosa secondary to severe weight loss or in patients taking a psychostimulant, 14 or with hyperviscocity conditions. 13 Our patient presented with lesions in acral regions which were typical for pernio and were the sole clinical presentation for her CD. The mechanism in this context remains unknown to our knowledge, but subtle nutritional deficiencies, commonly seen in CD patients, could have a role in the induction of the symptoms as we see in patients with eating disorders. 15 However, there is no clear immunological connection between the two diseases to our knowledge, like seen with the association of DH and CD that are both IgA-mediated.
Gluten-free diet was effective in reducing the patient’s lesions, demonstrating a probable correlation between pernio and CD. The symptoms gradually disappeared over the few months after the introduction of the diet, and all pharmacological treatments could be stopped. Children have been shown to have a higher and faster rate of symptom resolution following the introduction of a gluten-free diet. 16 Since the introduction of this diet, the patient didn’t demonstrate any symptoms of pernio in the following four winters despite exposition to cold temperature and no medications. One episode of symptoms was correlated with an accidental exposure to gluten by the patient. To our knowledge, St Clair et al. 17 reported the only other known case of pernio related to CD in a patient back in 2005 with a similar clinical presentation. Therefore, pernio may represent a rare and poorly recognized cutaneous manifestation of CD and its recognition may lead to an earlier diagnosis and treatment.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
The patient provided informed and written consent for publication of the case report.
