Abstract
We present a case of a 17-year-old female who presented to an urgent care for evaluation of a right-sided abdominal mass. Prior to her evaluation, she had undergone advanced imaging and exploratory laparotomy that did not reveal a diagnosis for her symptoms. Our case emphasizes the importance of listening to the patient who persists in describing a particular clinical symptom and highlights the forgotten, yet historically well-known, diagnosis of nephroptosis.
Introduction
Nephroptosis, also known as a floating or wandering kidney, is defined as the descent of the kidney either by two vertebral bodies or >5 cm on intravenous pyelogram when moving from a supine to erect position. 1 It most commonly affects young, thin females, probably due to a deficiency in support from the intra-abdominal adipose tissue. While once historically well-known, many younger urologists are no longer familiar with this condition and its management. 2 We present a case of nephroptosis in a teenage female, who had undergone a significant, costly workup prior to being diagnosed with this relatively simple and straightforward condition.
Case description
A 17-year-old female, with a past medical history of multiple sclerosis, presented to our outpatient urgent care to obtain a second opinion regarding a mass in her right lower abdomen. She was initially seen for this condition 2 months earlier. At that time, a general surgeon evaluated her for the complaint of a mass which had been progressively worsening and enlarging over the 6 weeks prior to her presentation. A computed tomography scan and ultrasound had been performed prior to the visit, and the radiologists did not report organomegaly, tumor, or any significant abnormality. The general surgeon suspected that she had a 3-cm intramuscular lipoma. She was taken to the operating room for exploratory laparotomy. However, no mass was palpated or discovered during surgery.
Seven weeks later, she presented to the urgent care affiliated with our practice group for evaluation. She reported pain and the persistence of a right-sided abdominal mass. On evaluation, her height was 64 inches and she weighed 107.5 pounds with the body mass index of 18.45 (13th percentile) (Records indicate that she had lost nearly 8 pounds in the last 5 months.). Physical examination was significant for an “8–9 cm-sized mass to the right of the umbilicus—well circumscribed when patient upright.” The patient was subsequently referred to a second general surgeon. She reported abdominal pain, nausea, and vomiting with standing. This surgeon suspected the palpable mass to be a ptotic kidney. The patient underwent an intravenous pyelogram which showed bilateral nephroptosis with descent of at least two vertebral bodies and greater than 5 cm. Her right kidney dropped approximately 8 cm when position changed from flat to erect (see Figures 1 and 2 below). She was referred to a local adult urologist, who suspected her pain was secondary to Dietl’s crisis, transient ureteral obstruction resulting in abdominal pain. As she was symptomatic only on the right side, she underwent successful robotic-assisted right nephropexy to the psoas muscle. Follow-up intravenous pyelogram showed resolution of right-sided renal nephroptosis. Symptoms improved after nephropexy.

Patient flat.
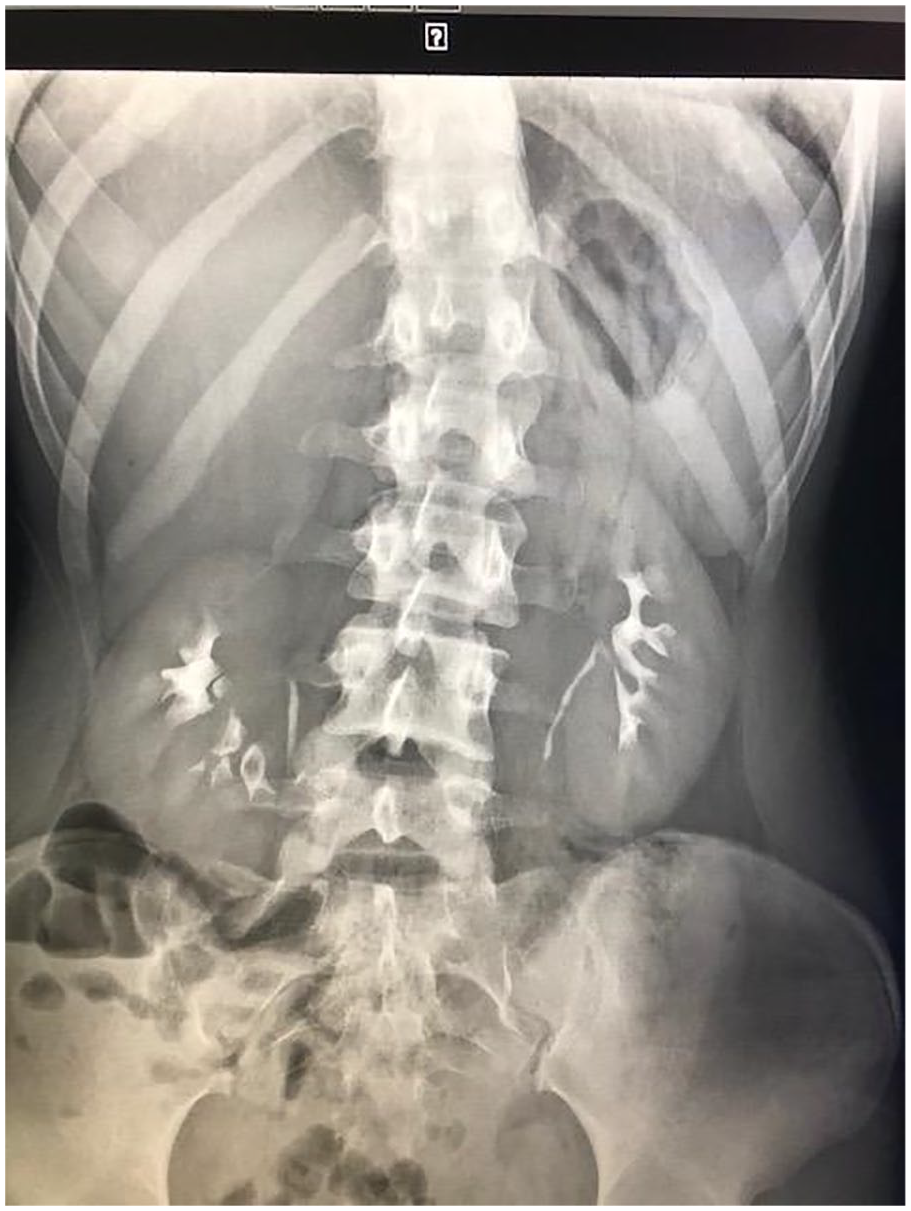
Eight cm descent of right kidney when patient erect.
Discussion
Nephroptosis was diagnosed quite commonly at the end of the 19th century, and many nephropexies were performed to treat nephroptosis, but the diagnosis fell out of favor as high morbidity and mortality was associated with the operation and patients did not always experience symptomatic relief afterwards. 3 As a result, many urologists have little knowledge of this clinical entity. 2 Nephropexy for nephroptosis was acknowledged as one of the “ineffective treatments for imaginary diseases” by McWhinnie and Hamilton in 1984. 4 While the exact incidence is unknown, it is thought to be present in around 20% of thin females, although it only rarely causes symptoms, which can include pain upon standing, nausea, vomiting, recurrent urinary tract infections, hypertension, and renal ischemia. 5 However, in the past few decades, there has been renewed interest in diagnosing nephroptosis, as today’s treatments—including laparoscopic and robotic-assisted nephropexy—are less invasive than surgical interventions in the past.
This diagnosis should be considered in thin, young females. When considered, diagnosis can easily be made with ultrasonography and intravenous pyelography. When not considered as the source of symptoms, however, even visualization of the kidney may be dismissed. Of utmost importance is the awareness that a ptotic kidney will return to its normal position when a patient is supine, thus explaining why no “mass” was detected on computed tomography or exploratory surgery.
The case also underscores the importance of listening to the patient who reports a persistent clinical symptom. The patient did not demonstrate any signs of malingering or factitious disorder, and in fact, documentation indicates that her physician palpated a mass on examination prior to surgery. Her mass was not detected on the operating table, because the kidney moved backward on supine positioning. Sadly, an understanding of the condition of nephroptosis would have made diagnosis much simpler and could have saved our patient from unnecessary radiation exposure and laparotomy.
Conclusion
In clinical medicine, there remains no substitute for listening intently to the patient in front of us. Our case report presents a young lady who clearly and consistently reported her symptoms to multiple physicians before ultimately being diagnosed with a relatively straightforward, although lesser known, clinical condition.
Footnotes
Acknowledgements
The authors thank Patricia Kelly, MD who reviewed the manuscript and suggested edits.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for her anonymized information to be published in this article. She was no longer a minor at the time of case write-up.
