Abstract
A 68-year-old woman with chronic kidney disease receiving dialysis and iron supplementation presented to our hospital with painful blisters, fragile skin, and changes to skin pigmentation on the dorsal side of both upper and lower limbs. Skin biopsy findings and an increase in urine porphyrins confirmed the diagnosis of porphyria cutanea tarda. Upon examination, extremely high serum ferritin levels (6000 µg/L) suggested iron overload. Oral iron supplementation was immediately discontinued, and the patient received treatment with the iron chelators deferoxamine, 10 mg/kg/day intravenously for 4 days, and deferasirox, 540 mg/day orally. After a 4-month follow-up, ferritin levels were normal (97.7 µg/L) and the cutaneous manifestations of porphyria cutanea tarda had improved. Complete remission has been maintained for the last 2 years, and the patient’s liver and heart function are normal. This case of porphyria cutanea tarda caused by secondary hemosiderosis highlights the potential toxicity of iron accumulation as a result of excessive iron supplementation. Although not approved for the treatment of patients on hemodialysis, we report the efficacy of deferasirox without any adverse effects in this case. We also stress the importance of the close monitoring of serum iron levels in kidney dialysis—and indeed all iron-supplemented—patients to avoid potential hepatic, cardiac, and endocrine damage.
Introduction
Secondary hemosiderosis, or secondary iron overload, can occur as an acquired etiology of other medical conditions, such as frequent blood transfusions (thalassemia, myelofibrosis) or chronic liver disease (hepatitis C infection or alcoholism). 1 If iron levels exceed the capacity of reticuloendothelial cells, iron can be deposited in multiple organs resulting in organ failure, 2 principally of the liver (cirrhosis, hepatocellular carcinoma), heart (cardiomyopathy), and pancreas (diabetes mellitus, pancreatic carcinoma).
A well-established relationship exists between secondary hemosiderosis and porphyria cutanea tarda (PCT), 3 a disorder of heme biosynthesis caused by a deficiency of the enzyme uroporphyrinogen decarboxylase (UROD). This deficiency leads to the accumulation of porphyrins (heme precursors) in the blood, skin, urine, and feces. As porphyrins are photoactive molecules, their accumulation in the skin can result in fragility, the formation of lesions, and the darkening of sun-exposed areas. 4
PCT may be either sporadic (type 1, approximately 80% of cases) or familial (type 2, approximately 20% of cases), with acquired factors including hepatitis C virus, HIV/AIDS, alcohol, smoking, or estrogen treatment. 4 Pathogenetically these iron-dependent disorders are linked, as iron overload can interfere with the heme synthesis pathway. Thus, conditions with elevated hepatic iron and/or increased serum iron indices have also been associated with PCT.
This case report, written in accordance with the Case REport (CARE) guidelines, 5 describes an adult patient with chronic renal disease who presented with PCT caused by secondary hemosiderosis. This case is important because it draws attention to the essential need of carefully managing iron levels in hemodialysis patients, and other at-risk patient populations, as iron overload can cause serious damage to multiple organs if left uncontrolled.
Case presentation
A 68-year-old female patient was referred for hematology consultation from our hospital’s dermatology department in June 2016. On physical examination, the patient presented with painful blisters, bullae formation, and fragile skin on the dorsal side of both her upper and lower limbs (Figure 1). The patient frequently had to prick the lesions to stop the spread of bullae so she could utilize the limb. She also presented with increased generalized skin hyperpigmentation, which had been noticed by her family and friends. Otherwise, the patient was in good condition, with no weight loss or pain.
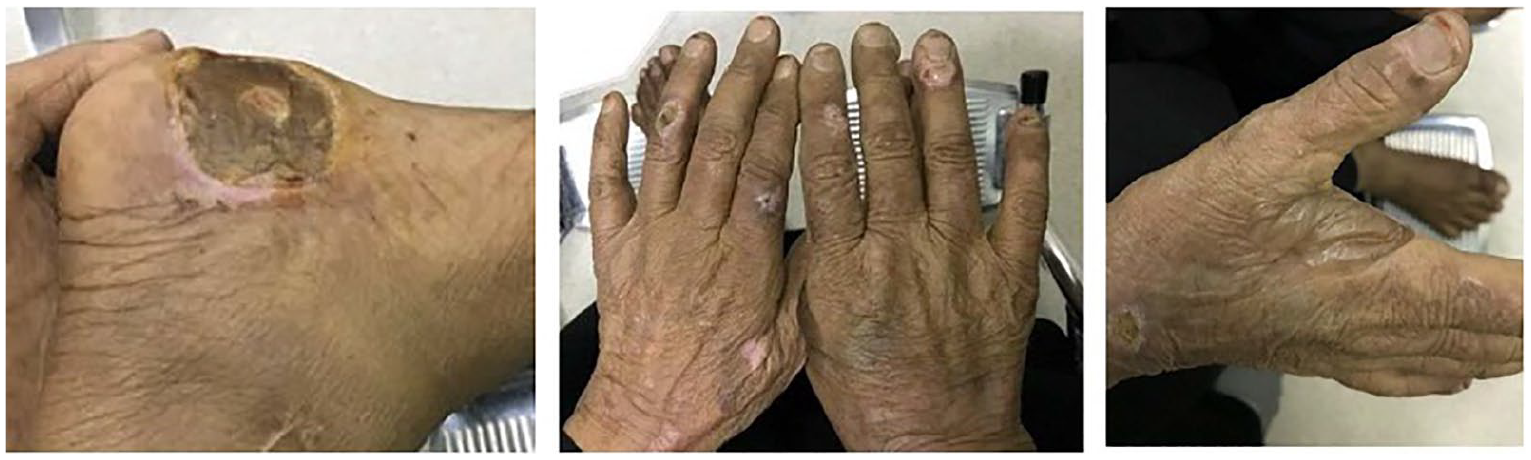
The patient presented with blistering lesions in various stages of healing characteristic of porphyria cutanea tarda.
Patient history
The patient had previously been diagnosed with arterial hypertension, type 2 diabetes mellitus, and end-stage renal disease, receiving dialysis with oral iron supplementation (ferrous fumarate, 325 mg/three times per day) for over 4 years, with a monthly average iron dose of 29.66 g since dialysis initiation (see timeline, Figure 2). There was no family history of porphyria or photosensitivity.

Timeline of important clinical information from the patient’s case.
Diagnostic assessment
A 2-mm punch of right finger revealed subepidermal cleft with separation of epidermis and dermis. Immunofluorescence was negative for IgM and C3, and positive for IgG in blood vessel walls and along the basement membrane. No inflammatory infiltrate was seen. Mild thickening of dermal blood vessels was observed (highlighted by PAS (periodic acid–Schiff) stain) with solar elastosis. Immunohistochemical stain for collagen IV showed positive staining along the roof of the blister and around blood vessels. Thus, the skin biopsy results were consistent with porphyria. The diagnosis of PCT was confirmed by the finding of increased urine porphyrins.
Complete blood counts and red blood cell indices MCV and MCH were normal, Hb 11.2 g/dL. However, initial blood tests revealed extremely high serum ferritin levels (6000 µg/L) suggesting iron overload (serum ferritin >300 ng/mL indicates iron overload and if >1000 µg/L at diagnosis suggests a risk of liver damage).
Other factors of secondary hemosiderosis were ruled out: There was neither patient history of alcoholism nor indications of inflammation, and serologic assays of HIV and hepatitis C virus were negative. Liver enzyme activity was normal. Neurological examination was normal.
Therapeutic intervention
The patient was admitted to our hospital, and oral iron supplementation was immediately discontinued. The patient received an aggressive series of therapeutic iron chelators, which bind iron in the bloodstream and help reduce its levels via excretion. The treatment consisted of 4 days of intravenous treatment with deferoxamine 10 mg/kg/day, followed by oral treatment with deferasirox 540 mg/day. 6 Serum ferritin levels were monitored every month, with close patient monitoring of hepatic function.
After a 4-month follow-up, ferritin levels had returned to normal levels (97.7 µg/L) and the cutaneous manifestations of PCT had gradually improved. Repeated MRI scans revealed no damage to the patient’s liver or heart.
The iron chelation treatment was well accepted and no common adverse effects, such as skin rash or gastrointestinal discomfort, were experienced.6,7 Hepatic function was closely monitored during therapy due to potential contraindications.
The patient was pleased with the outcome of the treatment, reporting an improvement in skin tone in addition to the healing of skin lesions (Figure 3). Complete remission of PCT has been maintained for the last 2 years. The patient’s ferritin levels are measured every 3 months, according to recent guidelines, 8 and remain within the normal range.

Improvements in skin lesions and pigmentation following the discontinuation of iron supplementation and treatment with iron chelators.
Discussion
We present a cautionary case of a woman with chronic kidney disease receiving hemodialysis and iron supplementation to correct associated anemia who developed PCT as a result of toxic iron overload due to a lack of appropriate monitoring.
Recognition of PCT-characteristic skin lesions was the first sign that led to the diagnosis. However, the patient’s secondary hemosiderosis could have been diagnosed earlier if routine serum ferritin analysis—a cheap, widely available, and reliable indicator of iron status—had been performed. A recent case report suggested a similar link between PCT development in a patient with end-stage renal disease and the use of oral iron supplementation (saccharated iron oxide 50 mg/week). 9 Therefore, there is a clear need within this patient population for the closer monitoring of serum ferritin levels. In fact, one experienced clinician even published “a plea for moderation,” calling the high incidence of iron overload in the dialysis population an epidemic, 10 although no studies to date have examined the incidence of secondary hemosiderosis in hemodialysis patients.
The early recognition of symptoms of secondary hemosiderosis is of crucial importance so that action can be taken to promptly reduce the patient’s iron levels. In this case, phlebotomy was not a suitable option as the patient had acquired secondary hemosiderosis. 1 However, the patient responded well to iron chelation therapy, which led to a significant, rapid, and prolonged reduction of the patient’s serum ferritin levels.
Deferasirox was approved by the U.S. Food and Drug Administration (FDA) in 2005 for the treatment of blood-transfusion-related iron overload, but its use has not been approved in patients on hemodialysis, although it has been shown to be effective and well–tolerated in such patients. 11 In this case, treatment with deferasirox was well tolerated with no minor adverse effects nor hepatic toxicity.6,7,11 Iron chelation improved symptoms of PCT and also prevented further damage, since liver biopsy and MRI monitoring of the heart and liver revealed no signs of organ damage.
Increasingly, MRI is replacing the use of liver biopsies in the assessment of iron stores as an effective non-invasive method. Notably, treatment with deferoxamine has been shown to reduce organ iron load by quantitative measurement by MRI with T2* imaging, and consequently improve heart and liver function. 12
The pathogenesis of iron overload in primary and secondary hemosiderosis is similar. Therefore, without genetic testing, we cannot exclude the possibility that this patient had a genetic predisposition to iron overload, that is, harbored a
Nevertheless, this case highlights that iron supplementation to correct anemia needs meticulous follow-up by serum ferritin analysis to prevent repercussions that include the development of secondary hemosiderosis and/or PCT. We particularly recommend the close monitoring of serum iron levels in at-risk patients, such as patients with cirrhosis or those receiving hemodialysis, to avoid the morbidity and health costs associated with subsequent organ failure.
Conclusion
This case warns clinicians as to the importance of the careful management of serum iron levels for the early detection of secondary hemosiderosis to prevent potential hepatic, cardiac, and endocrine damage.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article. The patient has read and approved the contents of this case report and given informed consent for its publication.
