Abstract
The bilobed flap is most often used for the reconstruction of small cutaneous defect of the nose. Under certain circumstances, it can also be useful in the reconstruction of much larger defects of the face. Our objective is to report a case of bilobed flap reconstruction in a patient with a large defect of the zygomatic cheek following a Mohs micrographic surgery for lentigo maligna.
Introduction
The bilobed flap is most often used for the reconstruction of small cutaneous defect of the nose. Under certain circumstances, it can also be useful in the reconstruction of much larger defects of the face. 1 Substantial cutaneous defect on the face can result when treating skin cancer, especially with lentigo maligna (LM). Our objective is to report a case of bilobed flap reconstruction following Mohs micrographic surgery (MMS) in a patient with a large right zygomatic cheek LM.
Case report
A previously healthy non-smoking 76-year-old female patient was referred for MMS in October 2016 for an irregular pigmented patch on her right cheek. She noticed a slowly growing brown discoloration evolving for more than 5 years (Figure 1). Unsurprisingly, an incisional skin biopsy showed LM in situ.

Lentigo maligna of the cheek.
Pre-operative assessment showed a 38 mm × 25 mm lesion on her right lateral infraorbital cheek. Excision of the lesion was done by MMS later in October 2016. After performing a debulking of the lesion that was sent for permanent sections, the first level of MMS achieved pathological clearance, leading to a cutaneous defect of 45 mm × 35 mm (Figure 2). The reconstruction was done thereafter under local anesthesia with a large bilobed flap based on the lateral cheek (Figure 3). In this particular case, this choice of reconstruction was motivated by a more flexible skin than that directly adjacent to the defect, in respect of cosmetic subunits and good skin match. After careful measurements based on the modified bilobed technique reported by Ricks and Cook, 2 the flap was incised and elevated with blunt dissection through mid-subcutaneous tissue. Meticulous hemostasis was achieved using a monopolar biterminal cautery device. An anchoring dermal buried key stitch was first placed on the flap’s first lobe to the right infraorbital rim of the zygomatic bone to prevent ectropion. Layered closure was then achieved with buried dermal sutures using 4.0 and 5.0 Polyglecaprone 25 sutures and with a running epidermal suture using a 5.0 Polypropylene suture.

Cutaneous defect following MMS (45 mm × 35 mm).

Large bilobed flap based on the lateral cheek.
Prophylactic antibiotic was prescribed, and cefadroxil 500 mg BID was started on the same evening for 5 days. Epidermal sutures were removed at 7 days post-operatively. At the 3-week follow-up, a small area of partial dermal necrosis was unbridled at the distal upper part of the flap. At the 2-month follow-up visit, 0.5 cc of triamcinolone acetonide 10 mg/cc was injected into each distal lobe to treat a mild hypertrophy. The patient was very satisfied with the esthetic result of the flap at the 6-month follow-up visit (Figure 4).
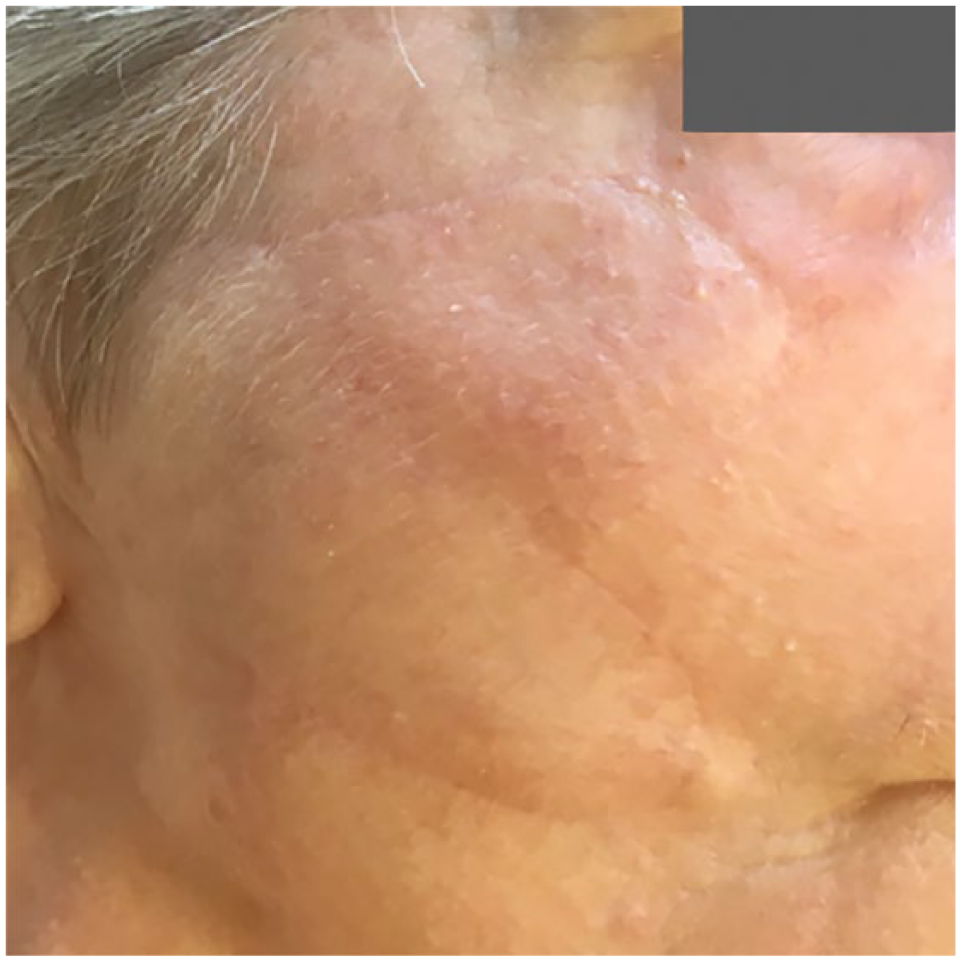
The 6-month follow-up visit.
Discussion
The bilobed flap is a random cutaneous transposition flap composed of two lobes based on a pedicle. In 1989, Zitelli adapted the original flap design by reducing the total rotation from 180° to between 90° and 110°. This modification led to fewer postoperative deformities, making this flap a great option for facial defects. 3 Cook 4 reviewed the flap design in order to minimize the distortion of the alar margins. One advantage of this flap is the possibility of recruiting tissue at a site distant from the defect. The proximity of the flap usually allows a good skin match. It is most often used for reconstruction of small defects of less than 1.5 cm of the distal nose (nasal ala, tip, and side wall). 2 Under certain circumstances, it can be useful in the reconstruction of much larger defects elsewhere on the face. Mourad et al. recruited 23 patients on whom a giant bilobed flap was performed in the head and neck area. Ten of these patients had a cheek defect following excision of basal cell carcinoma or squamous cell carcinoma. The mean size of deficit was 29.0 cm2. There were no wound complications or flap breakdowns, and esthetic results were acceptable. 1 Other extranasal applications of the bilobed flap have also been described for the lower lip, chin, ear, and hand. 5 The bilobed flap can be used almost anywhere on the face, particularly where a greater area of skin reservoir is located above or below the defect and can be accessible through a transposition movement, like the zygomatic and the medial subunits of the cheek.
In our case, areas of laxity were assessed before reconstruction. The best areas of skin recruitment consisted of two adjacent cosmetic subunits, the lateral cheek and the buccal cheek. The bilobed flap was chosen over a rhombic flap to access a better skin reservoir. A unilateral rotation flap could also have been a great reconstruction option, but the need for a larger undermining zone, the considerable length of the scar, and the higher tension closure led us to favor the bilobed flap. Another option could have been the use of an island pedicle flap originating from the inferior cheek. Although in this case, this robust muscular-based flap traveling from the lower/medial cheek to the infraorbital cheek would have led to a higher risk of postoperative ectropion. Finally, we have not considered a partial closure combined with a Burrow’s graft in order to minimize the risk of a postoperative ectropion due to the subsequent graft contraction and to achieve a better cosmetic outcome.
Like every cutaneous flap, the bilobed flap has some disadvantages. The complex suture lines cannot hide completely parallel to the relaxed skin tension lines. Also, pin-cushioning is well recognized as a characteristic complication of the bilobed flap. Undermining the primary defect and proper sizing of the flap are key steps to prevent this complication. Infections, hematoma, flap necrosis, and hypertrophic scarring are other less specific disadvantages of the bilobed flap. 5
In conclusion, surgeons should keep in mind the possibility of a laterally based bilobed flap for substantial cutaneous defect of the zygomatic and the medial subunits of the cheek when adjacent skin is not a good reservoir.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
The patient granted consent for publication of the case report.
