Abstract
In this case study, we have presented a rare case of concomitant human papillomavirus condylomata lesions of both breast nipples and giant vulval warts in an HIV-positive woman on antiretroviral therapy. The woman underwent successful surgical excision and reconstruction for both breast nipple condylomata and vulval warts. Histology of the excised breast nipple and vulval tissue confirmed low-risk human papillomavirus infection. Concomitant vulval and bilateral breast nipple condylomata pose a management dilemma. It is possible that the pathogenesis of these lesions is through both direct contact spread as well as haematogenous dissemination of the human papillomavirus.
Keywords
Introduction
Condyloma acuminatum (CA) is caused by infection with human papillomavirus (HPV), mainly HPV-6 or HPV-11 subtypes.1,2 In general, it occurs on anogenital mucosa and skin. It may also be found in the inguinal region or on the buttocks.2–4 Condyloma acuminatum of the nipple is uncommon and to date, only a few cases have been reported internationally. However, condylomata of the nipple with concomitant vulval warts is exceedingly rare, with very few cases having been reported. 3
Skin lesions of the breast may pose a challenge to physicians because they may have a varied clinical differential diagnosis ranging from HPV warts, molluscum contagiosum to bowenoid papulosis.5–7 These lesions may occur in isolation or may coexist with lesions on the genitalia and skin from elsewhere on the body. The association of breast malignancies and HPV is a contentious issue. 8 De Villiers et al. identified HPV DNA in 25 of 29 samples of breast carcinoma as well as in 20 out of 29 samples from the corresponding nipple. The predominant subtype in both breast carcinomas and nipple tissue was HPV 11. HPV 6 was the next most common subtype. 8 These authors suggest that nipple and areola epithelium may be infected by human papillomavirus. The histological features noted in human papillomavirus infected nipple and areola epithelium are analogous to those seen in infected epithelium elsewhere in the body. This study demonstrated a retrograde spread of human papillomavirus infection through the ‘nipple, areola, lactiferous ducts and sinuses’. 8
Differential diagnosis of warty breast nipple skin lesions
Molluscum contagiosum (MC) is a contagious skin infection from a pox virus (Poxviridae) that tends to affect the face and trunk in children and those who are immunocompromised. 5 Clinically, nodules with umbilicated centres are seen and at times a giant molluscum may be formed. The virus is spread by direct skin contact. It may be seen in association with HIV and HPV infections 5 and hence it is important to rule out when there are CA lesions.
Bowenoid papulosis (BP) of the breast, while uncommon, should also be considered in the differential diagnosis of nipple lesions. BP is a cutaneous condition characterized by pigmented verrucous papules. 6 Histologically, there is papillomatosis and acanthosis of the epidermis. The epidermis also shows varying degrees of dysplasia with loss of orderly maturation of keratinocytes. The lesions are induced by HPV and commonly HPV-16 subtypes. While extra-genital BP is usually accompanied by coexistent anogenital lesions, some cases of isolated extra-genital BP have been reported. 6
Case report
We present the case of a 36-year-old Para3 Gravida3, HIV-positive female who had a CD4 count of 275/mm3 and was on antiretroviral therapy. Her viral load at presentation was 35 copies/mL. The patient gave consent for publication and the case study was approved by the University of Witwatersrand Human Research Ethics Committee (Medical) with the clearance number M1706113. She presented with extensive vulval and nipple warts that were untreated for a period of 2 years prior to consultation. She was referred from a regional hospital to our quaternary level hospital complex in Johannesburg, South Africa, for surgical management of the warts. A diagnostic incisional biopsy of the vulval warts was performed at the regional hospital and histologically showed condylomata acuminata (HPV-induced genital warts).
At presentation, she complained of vulval pain and an offensive discharge. She previously utilized injectable contraceptives but now used barrier methods. She denied having been diagnosed with other sexually transmitted infections. She was anaemic with a haemoglobin of 7.9 g/dL and had a platelet count of 104 × 10^9/l.
On examination, she had evidence of mild pallor. She had a blood pressure of 116/48 mmHg with a pulse of 110 beats/min on admission.
Breast examination revealed bilateral 4 × 4 cm2 condylomatous lesions on the nipples. There was no bleeding. There were no areola masses or surrounding skin changes. No axillary lymph nodes were palpable. The warts covered the entire nipple with no extension to the areola (Figure 1(a)–(c)). Abdominal, respiratory and cardiovascular system examinations were unremarkable.
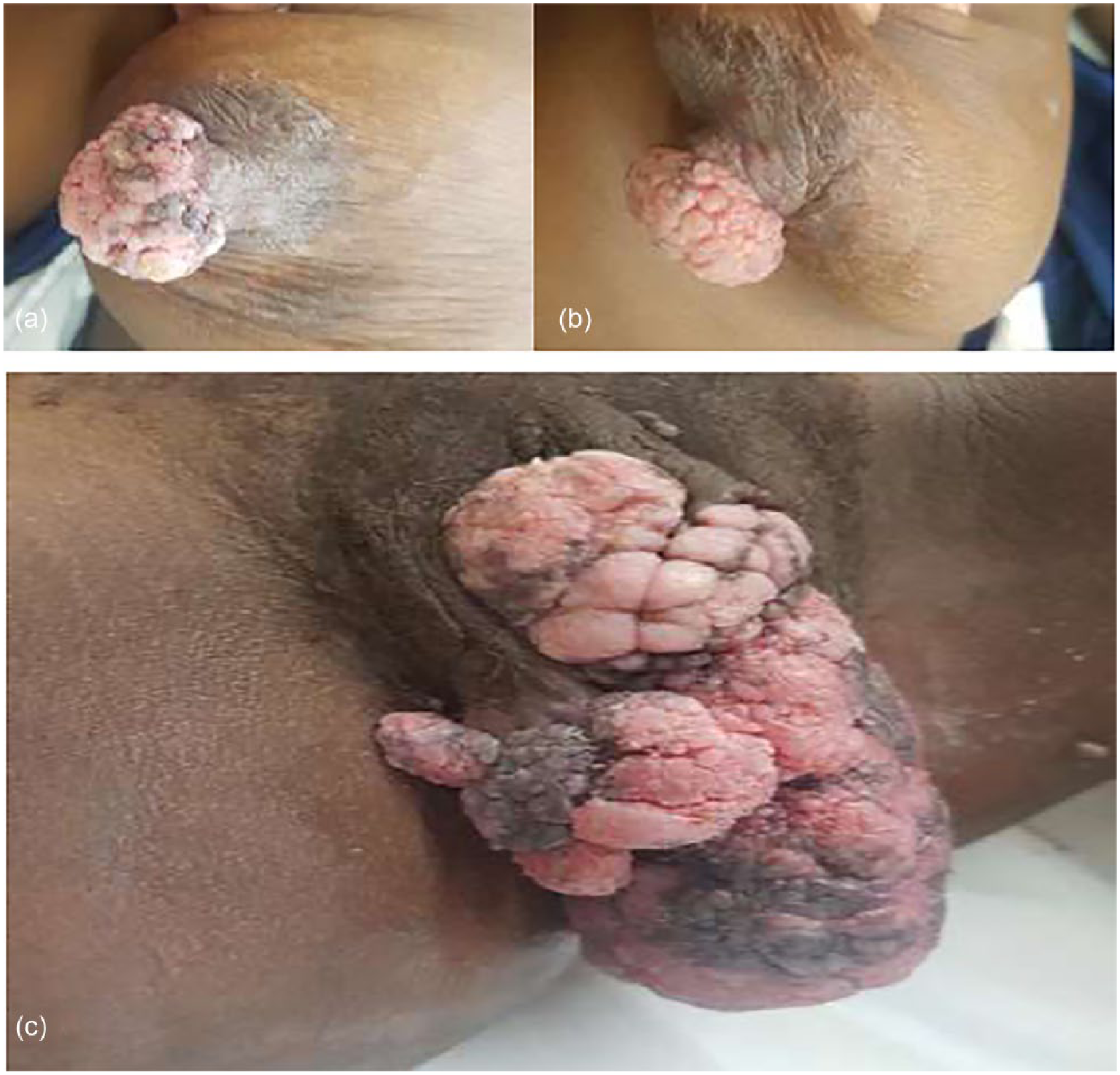
Bilateral breast nipple warts and giant vulval warts. (a) Picture of the right breast and nipple showing the condylomata accuminata lesion involving the entire nipple as well as hyperpigmentation of the areola suggestive of HPV infection and skin fungal infection. (b) A picture of the left breast and nipple showing the condylomata accuminata lesion involving the entire nipple as well as hyperpigmentation of the areola suggestive of HPV infection and skin fungal infection. (c) Vulval condyloma acuminatum involving labia major and minor and extends to the posterior commissure.
Vulval examination revealed extensive warts bilaterally measuring 15 × 10 cm2 in aggregate. They covered the labia minor and labia major. The warts extended and involved the posterior commissure. Anteriorly, the clitoris and clitoral hood were uninvolved.
Additional history obtained from the patient at a later stage, revealed regular sexual practices that involved penetrative sex followed by rubbing male genitals against her breast and nipples.
The breast surgeons were consulted for advice on management of the breast lesions. The surgical team had decided to excise the warts and follow this with reconstruction.
A vulvectomy with sparing of the clitoris was performed and the specimen was submitted for histological evaluation. A biopsy of the breast lesions was also performed and each was submitted in a separate specimen container. The vulvectomy wounds healed well with no complications. To date there is no evidence of disease recurrence (Figure 2).

Picture of breast nipples and vulva at post-surgery follow-up. (a and b) The right and left breasts and nipples with spontaneous resolution of the lesions without surgical resection, destructive procedure or medical treatment of the warts. (c) Vulval area after vulvectomy and primary repair.
Pathology
Macroscopic examination of the vulvectomy specimen revealed the left side which measured 90 × 50 × 40 mm3 and the right side which measured 70 × 40 × 28 mm3. Both sides had numerous exophytic warts.
The left and right nipple biopsies consisted of free-lying warts which measured 16 × 12 × 10 mm3 and 20 × 15 × 10 mm3, respectively. The nipple specimens were processed in their entirety.
Microscopic examination of sections from the vulvectomy specimen showed papillomatosis and acanthosis of the surface squamous epithelium (Figure 3(a)). The epithelium showed basal and parabasal hyperplasia in the lower one-third. Within the upper two-thirds of the epithelium, the cells showed differentiation but had raised nuclear to cytoplasmic ratios. The infected epithelial cells showed features of koilocytosis in which there was nuclear hyperchromasia, irregularities of nuclear membranes and the development of perinuclear halos (Figure 3(b) and (c)). These features are consistent with a diagnosis of condyloma acuminatum. In addition, the vulval epithelium contained areas of vulval intraepithelial neoplasia (VIN) 2/high grade squamous intraepithelial lesion (HSIL) which extended to the medial resection margin on the left side and to the inferior resection margin on the right side. Histological sections from both the left and right nipples (Figures 4 and 5) showed prominent papillomatosis, acanthosis and parakeratosis of the epidermis, together with koilocytosis, consistent with condyloma acuminatum.

Photomicrogram of the vulva lesion. (a) A low-power photomicrograph of vulval condyloma acuminatum showing papillomatous, acanthotic squamous epithelium. (H&E 2 μm, original magnification: 20x.) (b) Intermediate power magnification showing koilocytes with perinuclear halos at the arrows. (H&E 2 μm, original magnification: 100x.) (c) High-power magnification showing koilocytes with perinuclear halos at the arrows. (H&E 2 μm, original magnification: 400x.) (d) Positive blue staining of low-risk HPV family 6 in-situ hybridization. (4 μm section original magnification: 100x.).

Photomicrogram of the left nipple. (a) A low-power photomicrograph of condyloma acuminatum of the left nipple showing papillomatous, acanthotic squamous epithelium. (H&E 2 μm, original magnification: 20x.) (b) Intermediate power magnification showing koilocytes with perinuclear halos at the arrows. (H&E 2 μm, original magnification: 100x). (c) High-power magnification showing koilocytes with perinuclear halos at the arrows. (H&E 2 μm, original magnification: 400x). (d) Positive blue staining of low-risk HPV family 6 in-situ hybridization. (4 μm section original magnification: 100x.)

Photomicrogram of the right nipple. (a) A low-power photomicrograph of condyloma acuminatum of the right nipple showing papillomatous, acanthotic squamous epithelium. (H&E 2 μm, original magnification: 200x.) (b) Intermediate power magnification showing koilocytes with perinuclear halos at the arrows. (H&E 2 μm, original magnification: 100x.) (c) High-power magnification showing koilocytes with perinuclear halos at the arrows. (H&E 2 μm, original magnification: 400x.) (d) Positive blue staining of low-risk HPV family 6 in-situ hybridization. (4 μm section original magnification: 100x.)
The vulvectomy and both nipple biopsies underwent in-situ hybridization studies, which revealed positive staining for the low-risk VENTANA INFORM® HPV family 6 probe (Figures 2(d), 3(d) and 4(d)). The cocktail contained probes for the following HPV subtypes: 6, 11, 42, 43 and 44. High-risk HPV family 16 in-situ hybridization was negative in both nipple biopsies. Focal positive staining of high-risk HPV family 16 was identified in areas of vulval intraepithelial neoplasia (VIN) 2/high grade squamous intraepithelial lesion (HSIL). (HPV polymerase chain reaction testing is not available at our institution.)
Discussion
Condyloma accuminatum resulting from HPV infection is a common, highly contagious sexually transmitted disease that is often located on the vulva, penis and in the perianal region.1–4,9 The pathogenesis of coexistent nipple and vulvo-vaginal warts has not been fully elucidated and it is unclear if these warts are caused by the same HPV subtype. In our patient, there was positive staining of low-risk INFORM HPV family 6 by in-situ hybridization in the vulva and nipple biopsies. In light of the sexual practices proffered by the patient, we hypothesize that cross-infection from direct skin/mucosal contact resulted in spread of the condyloma acuminatum from genitalia to the nipples. However, studies by Bodaghi et al. 10 have suggested that HPV may be spread haematogenously via peripheral blood mononucleocytes. It is thus possible that both direct spread and haematogenous dissemination may result in spread of the virus, although this has not been ascertained in our patient.
Conclusion
Concomitant genital and nipple condyloma acuminatum is uncommon and as such, little is known about effective therapeutic modalities which may reduce risk of recurrence. The surgical management of vulval warts and nipple lesions by means of cauterization, cryotherapy or excision is both disfiguring and often offer temporary relief with many patients having recurrence of warts. As such, both medical and surgical methods of treatment may be necessary in an attempt to curb the infection in infected individuals as well as their sexual partners.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethics approval
Ethical approval to report this case was obtained from WITS HUMAN RESEARCH ETHICS COMMITTEE: (MEDICAL) CLEARANCE CERTIFICATE NUMBER
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
The copy of the Consent will be forwarded if and when required.
