Abstract
Objectives:
Stigmatization was reported throughout the COVID pandemic for COVID-19 patients and close contacts. The aim of this systematic review was to comprehensively examine the prevalence and impact of stigmatization during COVID-19 pandemic.
Methods:
English articles were searched using online databases that included PubMed, Scopus, Embase, and Web of Science up to 24 August 2022. A two-step screening and selection process was followed utilizing an inclusion and exclusion criteria and then data was extracted from eligible articles. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses checklist was followed, and the risk of bias was assessed using the Newcastle-Ottawa Scale.
Results:
Seventy-six studies were eligible for inclusion. Twenty-two studies reported the prevalence of social stigma due to COVID-19 infection with social isolation being the most commonly reported stigma. There were 20 studies that reported the majority of participants experienced stigma due to COVID-19 infection, which was as high as 100% of participants in two studies. Participants in 16 studies reported blaming from others as the second most common type of stigma, with various other types reported such as psychological pressure, verbal violence, avoidance, and labeling. The most common effect of the stigma was anxiety followed by depression, and then reduction of socialization.
Conclusion:
Findings from the present review have identified that COVID-19-related stigma studies have generally focused on its prevalence, type, and outcome. Greater awareness of this topic may assist with improving public education during pandemics such as COVID-19 as well as access to support services for individuals impacted by stigmatization.
Introduction
People who are considered to be a possible source of disease and may constitute a threat to social life in society may be subjected to stigmatization. 1 Consequently, this activity is associated with unfavorable discriminating attitudes, sentiments, and behaviors against persons with specific physical, behavioral, or ethnic characteristics who are considered a risk to society. 2
Historically, stigma has been related to several infectious diseases, resulting in prejudice against particular patient groups, with harmful repercussions for both people and society.3,4 During epidemics or pandemics, social anxiety emerges from concern about a disease with an unknown source and potentially lethal consequence, particularly when patient safety procedures such as isolation and quarantine are used to ensure community safety. 5
It seems to be a cultural tendency to accuse someone of the outbreak. This issue has deteriorated because of unproven claims about the virus. As a result, even individuals who have recovered and have passed their quarantine time may face social stigma. Groups susceptible to social stigma face discrimination in the manner of rejection by those who boycott and disregard them, as well as denial of good medical care and access to social facilities. They are also subjected to physical and verbal assault. 6
After COVID-19 was announced as a pandemic,7–9 individuals all over the world readily adopted stigmatizing attitudes and beliefs against COVID-19 patients and their close connections, as well as places, people, and ethnic communities suspected to be the source of the pandemic.10,11 COVID-19-related stigma results in a wide range of undesirable outcomes, including hesitation to access health care services after testing positive for the COVID-19 infection and severe exacerbations of pre-existing mental health issues. 12
COVID-19 patients may be charged with not obeying to stay in a safe place or neglecting to take precautions when moving outside. 13 Even if people have not been infected with the virus, they may be stigmatized. Someone with allergies, for instance, who has coughing and sneezing, may be embarrassed in society. 14
Exploration of the impact of stigma during the COVID pandemic is of great importance in identifying its effects and developing strategies to minimize any harmful effects. The aim of this systematic review was to comprehensively examine the prevalence and impact of stigmatization during COVID-19 pandemic.
Methods
This systematic review comprehensively explored the social stigma during the COVID-19 pandemic with regard to prevailing literature. To ensure that the outcomes reported were reliable and authentic, this review conforms to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist.
Data sources
Four online databases were searched including PubMed, Scopus, Embase, and Web of Science for relevant articles published in English until 24 August 2022. Keywords and their combinations were used when searching the databases and are shown below:
“Coronavirus disease 2019” OR “COVID-19” OR “Novel coronavirus” OR “2019-nCoV” OR “SARS-CoV2” OR “Severe acute respiratory syndrome coronavirus 2” OR “SARS-CoV-2” [Title/Abstract]
“Stigma” OR “Social stigma” OR “Public stigma” [Title/Abstract]
[A] and [B]
Study selection
A two-step screening and selection process was used to identify eligible articles. Initially, seven researchers assessed titles and abstracts and cultivated appropriate articles for the second and more diligent step. This second step involved full-text screening which was carried out by another five researchers. Studies were eligible for inclusion in our investigation if they were original and descriptive articles that were written in English language and published in a peer-reviewed journal related to stigma/social stigma during COVID-19. Exclusion of studies occurred for any systematic review publications, non-human research studies, investigations lacking published data, studies including abstracts without available full text, duplicated articles, case series, case reports, conference abstracts, letters to editors, preprints, and opinions.
Data extraction
Data extraction was performed for the studies that met the eligibility criteria. Five researchers were responsible for the extraction of data from the full texts. Another researcher was responsible for checking the eligibility of the included papers (i.e., possible duplications of papers) and the accuracy of extracted data. Data/information extracted included ID, reference number, and country of origin of the publications, articles type of social stigma, prevalence of social stigma, outcome of social stigma, and other important findings relevant to the research topic.
Quality assessment and bias risk evaluation
We utilized Newcastle-Ottawa Scale (NOS) 15 to evaluate the bias risk of the included studies. The criterion of this numerical tool is divided into three sections that include selection, comparability, and exposure/outcome. Maximum values of 4, 2, and 3 are allocated to these sections respectively. Studies are graded one point each for all items except for comparability which has the potential to score up to two points, with the minimum and maximum possible scores of 0 and 9. Studies which are rated 0–2 are considered poor quality, 3–5 are fair quality, and 6–9 are considered good/high quality. Table 1 shows ratings for individual studies by this tool.
Risk of bias for the included studies.

Results
Description of reviewed studies
The reviewed studies were published between 2020 and June 2023, and included a total of 76 studies (Figure 1). Of these studies, 73 included both male and female subjects, while two studies exclusively included male subjects, and one study did not report. The sample size for all studies combined was 1,988,008 individuals, with data collected from both male and female participants. The findings of the studies are presented in Table 2.

PRISMA flow diagram of study retrieval process.
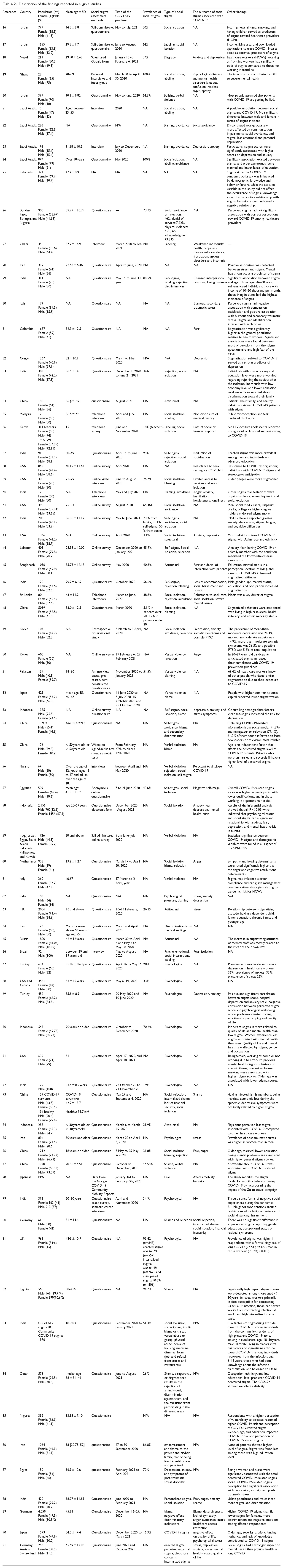
Description of the findings reported in eligible studies.
Prevalence
Out of the 37 studies that reported on the prevalence of social stigma related to COVID-19 infection, 20 studies found that the majority of participants experienced stigmatization16–20,24,26,27,29,37,41,42,44–46,51,70,83,84,86–88,91; In two studies conducted in China (28 participants) and Saudi Arabia (847 participants), the prevalence of social isolation and labeling reached 100%.19,24 In another study conducted in India with 91 participants, 98% of participants reported experiencing self-stigma, rejection, and social isolation. 37 The remaining 17 studies reported a prevalence ranging from 3.1% to 44.56%,33,36,39,43,47,48,57,63,67,68,72,74,76,77,79,84,89 the lowest prevalence of 3.1% was associated with social isolation and structural stigma and was found in a study conducted in the USA with 1366 participants.
The stigmas experienced by patients of COVID-19 in the present study were classified into three categories: personal, interpersonal, and organizational stigmas.
Personal stigmas
The personal stigmas identified through the literature review included attitudinal stigma, self-stigma, psychological pressure (Depression, anxiety, and symptoms of post-traumatic stress disorder), psycho-emotional stigma, internalized shame, lack of financial security, and shame.
Interpersonal or social stigmas
In the interpersonal domain, the following stigmas were identified: labeling, social isolation, disgrace, bullying, verbal violence, blaming, avoidance, physical violence, social rejection or avoidance, discrimination, and secondary discrimination (as presented in Table 2).
Organizational stigmas
Finally, at the organizational level, the study identified denial of services and discrimination in medical settings as forms of stigma.
The most important stigmas were the interpersonal or social stigmas. The most common was social isolation.16,17,19–21,33–35,37,39,41,42,44,47,48,53,56,57,60,73,76,88 In 16 studies blaming from others was the second most common social stigma reported due to being infected with COVID-19.22,23,39,40,46,48,51–55,60,62,72,83,89 In 13 studies, participants experienced rejection from the social environment.29,33,37,44,46,47,50,56,60,73,76,80,83 Other stigmas experienced by COVID-19 patients included psychological pressure,62,66–72,75,79,81 verbal violence,20,50–52,55,56,59,61,77,83 avoidance,22–24,26,40–42,47,54 labeling,17,19,21,23,27,29,34,35 attitudinal stigma,34,45,63,64,74 disgrace,18,26 discrimination,54,64 shame,73,77,80,82–84,86 structural stigma, 43 bullying, 20 denial of service and physical violence.26,83,84 In eight studies self-stigma due to being infected by SARS-CoV-2 was reportedly experienced by participants.29,37,42,44,46,53,54,57
Negative consequences were reportedly experienced by COVID-19 patients with anxiety being the most common,18,19,23,27,40,43,49,53,58,62,69,86,91 followed by depression,18,23,32,43,49,53,58,62,69,91 reduction of socialization,22,37,39,45–47,66,80 fear,31,45,58,66,76,87,89 distress,19,52,63,75 anger,40,50,58,76 mental health disorders,19,47,58,90 secondary traumatic stress,30,49 non-disclosure of COVID-19,35,56 reluctance to test/seek care,38,47 loss of financial support, 36 loss of accommodation, 46 helplessness, 40 loneliness, 40 burnout, 30 less happiness, 27 insomnia, 27 losing business, 29 changed interpersonal relation, 29 shame, 73 negative self-image, 57 somatic symptoms, 49 and affects mobility behavior. 78
In the present study, the majority of information was obtained through questionnaires, and studies reporting a prevalence of social stigma higher than 50% were mostly collected through questionnaires. This suggests that self-report questionnaires may have advantages over interviews and focus groups, as participants are more likely to report their experiences truthfully. Self-report questionnaires allow participants to answer anonymously, which may help reduce social desirability bias and encourage more honest responses.
Discussion
The purpose of this systematic review was to explore the social stigma surrounding the COVID-19 infection. There were 76 studies included which represented 37 countries worldwide. Most of the studies were conducted in eastern countries (Middle East and East Asia). The most common method used to collect data was via questionnaires. A relatively even split of sexes was represented (52.16% females and 47.84% males) with a mean age of 36.74 years. Prevalence of social stigma, the types of social stigma, the outcomes of social stigma, and other important findings were examined.
Prevalence
Among the top 10 countries with the highest prevalence of stigma, the majority were underdeveloped, with over 50% of the population experiencing stigma. However, the reported prevalence of stigma varied significantly between studies, even within the same country or among different nations. Possible reasons for this variability include a lack of standardized COVID-19 stigma questionnaires, limited access to medical services, and a shortage of accurate information about the disease in underdeveloped countries.
The degree to which disease-related stigma is prevalent varies among communities, and socioeconomic factors at both the individual and community levels impact different types of stigmas in distinct ways. 92 For example, communities with a better understanding of the disease and higher levels of mobilization efforts are less likely to exhibit stigma, while communities with concerns regarding providing aid and care during epidemics are more likely to endorse stigma.93,94 Additionally, individuals with higher socioeconomic status or education levels experience less stigma, likely due to their greater access to accurate information about the disease. These results are consistent with earlier research demonstrating that individuals from lower social classes experience more stigma compared to those from higher social classes.
For the studies included in the present review there was a higher prevalence of stigma in Asian countries,16,18,21,29,44,45,51,70,82,83,86 which could be attributed to the Asian origin of the virus, for example, Asians being accused of spreading the disease. The prevalence of stigma is exacerbated by an excess of news and conflicting messages, particularly during large-scale disasters such as COVID-19.95–97 In similar studies, the prevalence of infectious diseases such as H1N1, bubonic plague, Asian flu, cholera, Ebola, Zika virus, tuberculosis, SARS, and middle east respiratory syndrom (MERS) has been associated with stigma and discrimination against patients. 98 A recent comparative study reported a higher prevalence of stigma for COVID-19 infection than AIDS/HIV, which has been one of the most stigmatized health conditions worldwide for decades. 54 COVID-19 infected patients and their family members were stigmatized and isolated as being infectious or dangerous to the health of those coming into contact with them. The widespread concern and media coverage of COVID-19 contributed to its high prevalence of stigma, which was fueled by individuals perceiving the disease as a mortal infection, and the lack of treatments for the virus. Misleading news likely caused people to be frightened, but accurate knowledge about the disease may have reduced the stigma. Education and good communication have the potential to significantly improve the knowledge, attitudes, and behaviors related to infectious diseases, such as Ebola and COVID-19, and reduce infectious disease-related stigma.99,100
Types of stigma
In previous studies, various types of stigma have been defined for AIDS/HIV disease. For instance, a study that investigated a conceptual model of HIV/AIDS stigma from five African countries identified three types of stigma: received, internal, and associated. 101 Received stigma is a type of stigma directed toward a person living with HIV/AIDS by others. It includes various stigmatizing behaviors such as neglecting, fearing contagion, avoiding, rejecting, labeling, pestering, negating, abusing, and gossiping. Internal stigma is the negative thoughts and behaviors that a person living with HIV has about themselves based on their HIV status. This type of stigma is based on the person’s own perceived view of stigma, and can include self-perception, social withdrawal, self-exclusion, and fear of disclosure. 102
Associated stigma refers to the stigma that arises from a person’s association with individuals who have HIV/AIDS, such as having an HIV-positive family member or working with HIV-positive individuals. In the present review, the most reported stigma was social isolation.16,17,19,21,24,33,35–37,39,41–44,47–49,53,56–58,60,73,76,80,88 Furthermore, in 16 studies22,23,39,40,46,48,51–55,60,62,76,83,89 participants experienced blaming from others. Additionally, participants in 14 studies reported rejection from social environment.26,33,37,44,46,47,49,50,56,60,73,76,80,84 Labeling was reported in nine studies,17,19,21,24,27,29,35,36,66 and avoidance was also reported in 10 studies.22–24,26,40–42,47,49,54 Denial of service, and violence were reported in two studies,26,83 disgrace was also claimed in only two studies.18,84 In another study, discrimination and self-stigma were reported,29,84,89,91 and verbal violence and bullying in 10 studies.20,50–52,55,56,59,61,77,83 Attitudinal stigma was reported in eight studies.34,45,63,65,74,83,84,91 Other related studies also reported psychological distress and decreased resilience during the outbreak of viruses H1N1, H7N9, MERS, and Ebola. 103
The stigmatization of various diseases has both similarities and differences. While isolation is a common stigma in infectious diseases, different diseases have varying prevalence and types of stigma. For example, tropical infectious diseases with visible symptoms such as scars and deformities have the highest rates of stigmatization and social isolation, while HIV is stigmatized due to its origin and being a sexually transmitted disease. COVID-19 patients also face stigma due to a perceived lack of precautionary measures or social distancing, making them a potential threat to others’ health.
The COVID-19 pandemic has resulted in a variety of isolation and social avoidance behaviors toward patients infected with the virus. These behaviors are possibly due to community fears of getting infected since the disease is highly contagious. Social isolation and other forms of rejection from others were frequently reported and are consistent with previous studies on attitudes toward patients during epidemics and pandemics. 104
Outcomes of stigma
The review findings indicated there were various outcomes experienced by participants, such as anxiety which was the most experienced one,18,23,27,40,43,49,53,58,62,69,88,91 followed by depression,18,23,32,43,49,53,58,62,69,91 fear,31,45,58,66,76,88 anger,19,40,50,60,76,87,89 mental health disorders,19,47,49,58,90,91 secondary traumatic stress,30,53,62,63,76 non-disclosure of COVID-19,25,35,47,56,80,89 loss of financial support,36,73,80 burnout, 30 less happiness, 27 insomnia, 27 losing business, 29 changed interpersonal relation,29,66 psychological pressure,62,67,68,70–72,75,90 discrimination from medical settings,54,64,89 psycho-emotional, 66 internalized shame.73,77,80
Stigma can cause unpleasant feelings such as anxiety and depression, which can threaten mental health. In turn, mental health can also act as a predictor of stigma. The consequences of stigma can be serious, as evidenced by patients who were reluctant to disclose their symptoms and seek medical attention during the early stages of COVID-19 due to social stigma. This non-disclosure can lead to a more rapid spread of the disease. 105 Evidence in other studies suggests that stigma has caused psychological distress and post-traumatic stress disorder (PTSD) in infected patients and healthcare workers during outbreaks of SARS, H1N1, MERS, Ebola, and COVID-19.106–109 Similar findings have been reported in studies on other diseases, such as AIDS and previous SARS epidemics.
In various infectious diseases, including human immunodeficiency virus (HIV), hepatitis C virus (HCV), tuberculosis, and Zika, stigma persists at all levels and impedes effective treatment. This stigma may lead to reduced treatment uptake and under- or non-participation in available treatments. 110 HIV/AIDS has always been stigmatized with negative connotations such as drug abuse, sex work, poverty, or incarceration associated with deviant behavior disapproved by society. 111 In contrast, epidemic-related diseases like SARS and COVID-19 are caused mainly by external factors, which are not considered morally reprehensible. Hence, stigmatization of these infectious diseases is primarily driven by fear of the disease itself, and the perceived threat level will decrease as public awareness of the disease increases.112,113 It is crucial to improve public awareness of the nature of the disease to reduce fear and anxiety and, subsequently, reduce stigma. 114 Furthermore, people with higher education levels and socioeconomic status may be less likely to stigmatize others, especially in high-income countries. 115
Strengths and limitations
This review provided a broad and representative overview of the COVID-19-related stigma issue. The methods used to find, screen, and select the included studies were rigorous. Additionally, data was extracted via three researchers and the discrepancies were addressed by a third researcher to ensure the quality of included studies and reduce the risk of bias. However, the results of this review may be subject to limitations related to the selection process of eligible studies. Specifically, studies published in outlets other than the first-tier journals were included in the review. Due to the heterogeneity of the included studies, performing a meta-analysis was not suitable; therefore, we only performed a qualitative synthesis of selected literature.
Conclusion
This systematic review identified the three most researched targets of COVID-19-related stigma. First, prevalence of social stigma: limited access to medical services, shortage of accurate information about the disease in underdeveloped countries, socioeconomic, and geographical location. Second, types of stigma: social isolation, labeling, rejection from the social environment, blaming from others, denial of service, violence, discrimination, self-stigma, verbal violence, and attitudinal stigma. Third, the outcome of the stigma: anxiety, depression, fear, anger, mental health disorders, secondary traumatic stress, non-disclosure of COVID-19, loss of financial support, burnout, less happiness, insomnia, losing business, changed interpersonal relations, psychological pressure, discrimination from medical settings, psycho-emotional, internalized shame. The stigma associated with COVID-19 is closely related to the quality of life and mental health of individuals, and our findings can inform policymakers to ensure the availability of a safe environment with respectful care and urgent action is needed to tackle COVID-19 at every level, from the personal to the political. It seems that according to the issues raised in this review, it is necessary to deal with the psychosocial discomforts that society is facing during the outbreak of COVID-19. To deal with these feelings, psychological evaluations, and support, including ensuring a cultural approach, and taking into account different needs in society, are necessary. In addition, social support is necessary to reduce the adverse effects of stigma that may lead to further spread of disease and social unrest. It is better to correct health education, social behaviors, and psychological interventions by targeting people as the most effective method to prevent social stigma caused by COVID-19, which is recommended to form specialized teams of medical, social, and behavioral science experts. To update the review, more studies are recommended in the future. Greater awareness of this topic may assist with improving public education during pandemics such as COVID-19 as well as access to support services for individuals impacted by stigmatization.
Supplemental Material
sj-doc-1-smo-10.1177_20503121231208273 – Supplemental material for Social stigma during COVID-19: A systematic review
Supplemental material, sj-doc-1-smo-10.1177_20503121231208273 for Social stigma during COVID-19: A systematic review by SeyedAhmad SeyedAlinaghi, Amir Masoud Afsahi, Ramin Shahidi, Arian Afzalian, Pegah Mirzapour, Mohammad Eslami, Sepide Ahmadi, Parisa Matini, Soudabeh Yarmohammadi, Seyed Saeed Tamehri Zadeh, Pooria Asili, Parinaz Paranjkhoo, Maryam Ramezani, Sahar Nooralioghli Parikhani, Foziye Sanaati, Iman Amiri Fard, Elham Emamgholizade Baboli, Somaye Mansouri, Ava Pashaei, Esmaeil Mehraeen and Daniel Hackett in SAGE Open Medicine
Footnotes
Acknowledgements
The present study was conducted in collaboration with Khalkhal University of Medical Sciences, Iranian Institute for Reduction of High Risk Behaviors, Tehran University of Medical Sciences, and the University of Sydney.
Authors’ contributions
The conception and design of the study: Esmaeil Mehraeen, Seyed Ahmad Seyed Alinaghi. Acquisition of data: Ramin Shahidi, Arian Afzalian. Analysis and interpretation of data: Amir Masoud Afsahi. Drafting the article: Esmaeil Mehraeen, Pegah Mirzapour, Sepehr Eslami, Sepide Ahmadi, Parisa Matini, Soudabeh Yarmohammadi, Seyed Saeed Tamehri Zadeh, Pooria Asili, Parinaz Paranjkhoo, Maryam Ramezani, Sahar Nooralioghli Parikhani, Foziye Sanaati, Iman Amiri Fard, Elham Emamgholizade, Somaye Mansouri, Ava Pashaei. Revising it critically for important intellectual content: Seyed Ahmad Seyed Alinaghi, Daniel Hackett. Final approval of the version to be submitted: Seyed Ahmad Seyed Alinaghi, Esmaeil Mehraeen, Daniel Hackett.
Availability of data and material
The authors stated that all information provided in this article could be shared.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
Not applicable.
Consent to publication
Not applicable.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
