Abstract
Objectives:
Vascular access is an important procedure for drug administration during the resuscitation of a patient with cardiac arrest; however, it can be challenging under emergent conditions. This study aimed to investigate the efficiency of ultrasound-guided internal jugular venous access using a midline catheter versus peripheral intravenous access during cardiopulmonary resuscitation.
Methods:
This was a prospective single-center observational study among patients who received cardiopulmonary resuscitation. The primary outcomes were the success rate of first attempt and the time taken for vascular access via the internal jugular and peripheral veins. We also measured the diameter of the internal jugular and peripheral veins at the access point and the distance from the access point to the heart.
Results:
In all, 20 patients were included in the study. Internal jugular and peripheral venous access had a first-attempt success rate of 85% and 65%, respectively (p = 0.152). The time to access the internal jugular and peripheral veins was 46.4 ± 40.5 s and 28.8 ± 14.7 s, respectively (p = 0.081). The diameter of the internal jugular and peripheral veins was 10.8 ± 2.6 mm and 2.8 ± 0.8 mm, respectively (p < 0.001). The distance from the vascular access point to the heart was 20.3 ± 4.7 cm and 48.8 ± 13.1 cm for the internal jugular and peripheral veins, respectively (p < 0.001).
Conclusions:
There was a trend toward higher success rates in the internal jugular vein rather than the peripheral intravenous approach, which was not statistically significant.
Objectives
The initial approach for administering drugs during cardiopulmonary resuscitation (CPR) for cardiac arrest is usually through the peripheral intravenous (PIV) route. Alternate routes for drug administration include the intraosseous (IO), central venous, or endotracheal routes. 1
During cardiac arrest, PIV access can be difficult due to circulatory collapse. The first-attempt success rate of PIV access during CPR varies and ranges from 30% to 75% in adult patients. 2 If alternate routes for drug administration can be rapidly accessed in case of difficult PIV access, emergency drugs can be delivered effectively, and a better quality of resuscitation could be achieved, rather than without any vascular routes. 3
The internal jugular vein (IJV) can be an alternate site for vascular access in patients with difficult intravenous (IV) access. Ultrasound (US)-guided IJV access using a PIV catheter, called the “easy IJ” in previous studies, is a fast and safe alternative in patients with difficult PIV access.4,5 However, due to the short length of the peripheral IV catheter cannula, it can get dislodged during CPR.
A midline IV catheter is a long peripheral catheter ranging from 8 to 12 cm in length and is usually inserted under US guidance into the basilic or brachial veins of the arm using the Seldinger technique. The midline IV catheter has a longer dwell time of up to 29 days and is unlikely to be dislodged compared to the conventional PIV catheter. 6
We hypothesized that IJV access using a midline catheter could be performed rapidly under US guidance and could deliver drugs safely during CPR. Therefore, we designed this study to investigate the efficiency of US-guided IJV access using midline catheters versus conventional PIV access during CPR. This is the first such study among adult patients receiving CPR, to the best of our knowledge.
Methods
This study was approved by the Institutional Review Board of Chungbuk National University Hospital (2021-10-018) and was conducted in the emergency department (ED) of Chungbuk National University Hospital. This study protocol adheres to the ethical principles outlined in the 1975 Declaration of Helsinki. The requirement for consent was waived because consent could not be obtained during CPR.
Study design and patients
A prospective single-center observational cohort study was conducted among patients who received CPR between October 2021 and February 2022. The primary endpoints were the success rate of first attempts and the time taken for vascular access via PIV and IJV. We also measured the diameter of the PIV and IJV at the insertion site and the distance from the insertion site to the ipsilateral sternoclavicular joint, and the third intercostal space on the right side. Patients of age below 18 years, with traumatic cardiac arrest, with preexisting venous access, with return of spontaneous circulation (ROSC) before ED arrival, with “do not resuscitate” orders, and who did not finally secure PIV or central venous catheterization (CVC) were excluded (Figure 1).
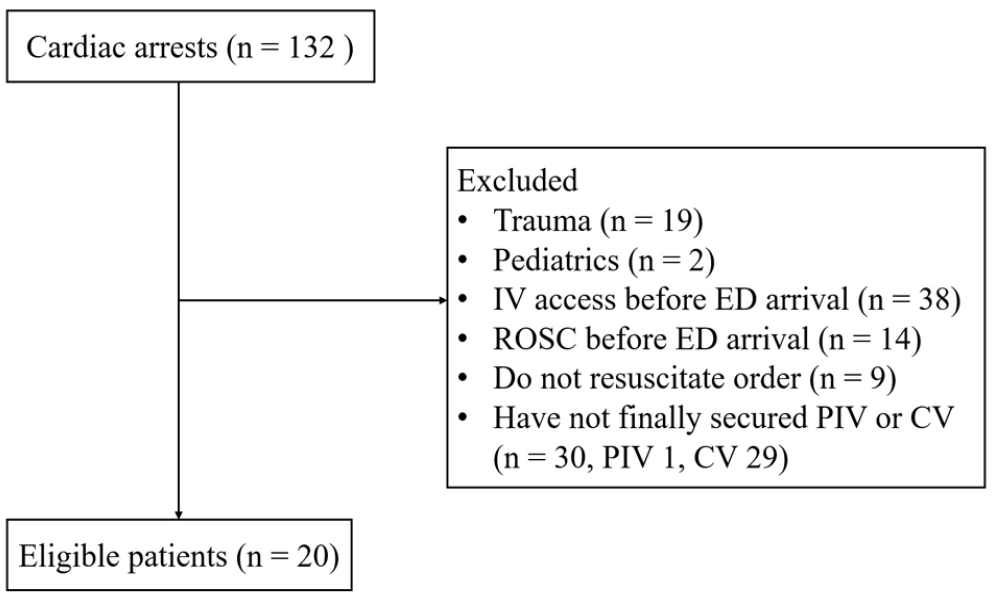
Study flow chart. Despite several attempts during CPR, PIV was not secured in one patient, and IJV using midline catheter was the only IV route. This patient was excluded from the study. In addition, 29 patients who did not attempt CV access with the midline catheter were excluded from the study.
Study protocol
All protocols in this study were conducted during CPR. To compare the duration of the procedure and success rate between PIV and IJV access, only patients who needed venous access because of arrival at the ED without available preexisting venous access were included. Both PIV and IJV access were attempted on each patient to compare the success rate at the first attempt and throughout the duration of the procedure. Chest compressions were performed using a mechanical chest compressor (LUCAS-2; Physio-Control/Jolife AB, Lund, Sweden) or by emergency medical technicians certified in advanced cardiac life support (ACLS) through the American Heart Association. A senior attending physician directed the resuscitative efforts as the team leader followed the protocols of ACLS for critically ill patients and advanced trauma life support for severely traumatized patients. Immediately after the patient arrived at the ED, PIV access and advanced airway were obtained from two physicians simultaneously. IJV access was attempted after successful endotracheal intubation from a physician who attempted PIV access. The first-attempt success rate of the procedure was defined as the successful administration of drugs or fluids through the newly inserted PIV or IJV access at the first effort. The measurement of the catheter insertion time (PIV and IJV access time) was started when the skin was sterilized before catheter insertion and ended when the flow of drug or fluid was subjectively considered suitable for use. The procedure was considered to have failed when a good flow of drug or fluid was not accomplished, despite three attempts at PIV or IJV access. All procedures were recorded by a camera, and all the measured time values were rounded to the nearest second.
Interventions
During initial resuscitation, right or left peripheral median cubital vein (MCV) access was first attempted. If unsuccessful, opposite MCV access was attempted. If both failed, peripheral upper extremity venous access or lower extremity venous access was attempted. After successful endotracheal intubation, US-guided IJV access was attempted. Small linear array US (HS60; Samsung Medison, Seoul, South Korea) probe with high-frequency transducers (5–15 MHz) that can be placed in a transverse position relative to the vessel were used; this allowed for a “short-axis” view to be displayed on the US screen, which showed a cross-sectional image of the vessel.7,8 If unsuccessful, opposite IJV access was attempted. If both failed, femoral vein access was attempted. PIV and IJV access were attempted without interruption of chest compressions. Operators were trained specialists or senior residents who had experience in performing at least 25 successful US-guided CVC procedures without supervision. Before the commencement of the study, operators participated in a 2 h education program on the use of the midline catheter device under US guidance and the PIV catheter device, followed by hands-on training. For PIV access, an 18 gauge × 30 mm PIV catheter (Angiocath Plus Pro™; Bard Access Systems, Inc., Salt Lake City, UT, USA) was placed in the PIV to administer the fluids. For IJV access, an 18 gauge, 8 cm midline catheter (PowerGlide Pro™; Bard Access Systems, Inc., Salt Lake City, UT, USA) was inserted into the IJV. The US-guided IJV access procedure was performed using the “accelerated Seldinger technique” (Figure 2).9,10

Ultrasound probe and midline catheter orientation during resuscitation, “accelerated Seldinger technique” (a) and midline catheter placement after the procedure (b). After the procedure was completed, skin tape was placed over the insertion site.
Data collection
The time taken for catheter insertion via the PIV and IJV during CPR was measured. The following data were collected using a case report form that we had developed prior to the main study, including age, sex, body mass index, underlying diseases, the time and the total number of PIV and IJV access attempts, and the diameter of PIV and IJV at the insertion site. The vessel diameter was measured as the maximal anterior–posterior dimension of the vein, just proximal to the catheter insertion point (Figure 3). Additionally, we measured and compared the distance from the vascular access point to the heart using a disposable paper measuring tape. We referred to a previously published measurement method to determine the length of the peripherally inserted central catheter, distance from the insertion site to the ipsilateral sternoclavicular joint, and the third intercostal space on the right side. 11

Ultrasound image of IJV and PIV in one enrolled patient. The diameter of IJV was 13.0 mm (a) and the diameter of MCV was 2.7 mm (b).
Sample size
The number of patients required for this study was calculated using the G*Power program (Faul et al.). 12 Based on the previous studies with approximately 30% absolute difference in success rate at the first attempt, it was expected that 20 patients were needed in each group to yield 80% power with an α of 0.1.2,4,5 Therefore, we enrolled 20 patients.
Statistical analysis
For continuous variables, means and standard deviations were reported based on the normality of the distribution. Categorical variables were reported as counts and percentages. The paired t-test and analysis of variance were used to determine if there were significant differences in the success rate and the procedure time between IJV and PIV access. All statistical analyses were conducted using the PASW/SPSSTM software, version 22 (IBM Inc., Chicago, IL, USA). p-Value < 0.05 was considered statistically significant.
Results
Patient characteristics
The study included 20 patients in the ED (Figure 1) who suffered a cardiac arrest. Six women and 14 men aged 24–93 years (mean, 67.0 ± 18.9 years), were included. The body mass index ranged from 20.3 to 35.0 (mean, 23.7 ± 3.3) kg/m2. ROSC was achieved after resuscitation in seven patients (Table 1).
Baseline characteristics of patients.

Values are presented as mean ± standard deviation or number (%).
MI, myocardial infarction; ROSC, return of spontaneous circulation.
IJV and PIV diameter and distance from the insertion site
The diameters of the IJV and PIV were 10.8 ± 2.6 and 2.8 ± 0.8 mm, respectively (p < 0.001). The distance from the catheter insertion site to the third intercostal space was significantly different between IJV and PIV access (20.3 ± 4.7 vs 48.8 ± 13.1 cm; p < 0.001; Table 2 and Figure 4).
Comparison between internal jugular and brachial vein access.

Continuous variables expressed as mean (standard deviation) or number (%).
ED, emergency department; IJV, internal jugular vein; PIV, peripheral intravenous.

Comparison of (a) vascular access time, (b) diameter of vessels, and (c) distance from the catheter insertion site to the third intercostal space on the right with CIV and PIV access. In two patients, lower extremity veins were accessed due to failure of access to upper extremity veins. In one patient, femoral vein was accessed due to failure of access to both IJVs (c).
First-attempt success rate and vascular access time between IJV and PIV access
The first-attempt success rates were 85.0% (17/20) and 65.0% (13/20) for IJV and PIV access, respectively (p = 0.152). There were three IJV access failures due to two collapsed IJV and one carotid artery hematoma; however, there were seven failures overall during PIV access due to collapsed vessels. Although the mean PIV access time was shorter (28.8 ± 14.7 s) than the IJV access time (46.4 ± 40.5 s), the difference was not statistically significant (p = 0.081; Table 2 and Figure 4).
Discussion
In this study, IJV access using a midline catheter technique had a vascular access time similar to that of PIV access; however, it had a higher success rate and a shorter distance to the heart compared to that of the PIV access.
The reason for the higher first-attempt success rate of IJV access (85.0%) compared to that of PIV access (65.0%) in our study is thought to be because the IJV diameter is larger than that of the PIV (10.8 ± 2.6 versus 2.8 ± 0.8 mm, respectively). The IJV diameter was twice more than that of the PIV, making it easier to perform US-guided procedures. The results of the vessel diameter in our study were similar to those reported in previous studies.13,14
Previous studies have reported that CVC achieved a higher drug peak concentration and shorter time to drug peak concentration than the peripheral vascular approach.15,16 One of the factors leading to the higher peak concentration and shorter time to peak concentration is thought to be the shorter distance to the heart in CVC than in PIV access. Therefore, we can predict that drug administration through a midline catheter inserted at the same position as the CVC will show a similar peak drug concentration and peak concentration time to that achieved with CVC. Despite the advantages, CVC is not recommended during CPR because it can interfere with chest compression, has a long procedure time, and can cause complications (e.g., pneumothorax).1,3 The PowerGlide Pro™ is not a CVC approach but can be considered a good option to compensate for the shortcomings of CVC during CPR and maintains the advantages of CVC by providing a vascular access point closer to the heart compared with the PIV access. Another interesting feature of PowerGlide Pro™ is that it has an integrated guide wire built in to enable the use of the “accelerated Seldinger technique,” which allows the US probe to be adjusted with one hand and the catheter to be easily advanced with the other. Furthermore, it has a catheter hub stabilizing device called StatLock and, therefore, does not require sutures for stabilization, unlike other CVCs. 17 Due to these features, PowerGlide Pro™ might be associated with a shorter procedure time than CVC.
IO access is another alternative route for vascular access during CPR. However, several researchers have found that IV access was associated with better clinical outcomes than with IO access.18–20 Furthermore, IO access is not easy to perform, and opportunities to become familiar with the procedure are limited due to few cases per year. The US-guided midline IV access is similar to the CVC, which is one of the essential procedures for an emergency specialist. Therefore, a midline catheter using IJV might be a good alternative for patients with cardiac arrest, hypovolemic shock, or those with difficult peripheral blood vessel access.
This study had some limitations. First, it is a single-center study with a small sample size, which can limit the generalizability of our results and result in a selection bias with respect to the patient subset. Second, IJV access was performed sequentially after PIV access and endotracheal intubation, which could act as a confounding bias. However, it was not possible to perform endotracheal intubation and jugular vein access simultaneously due to limited space during CPR, and it was an inevitable method to secure the IV access as quickly as possible. Third, two different catheters were used in this study. The authors have previously used a peripheral catheter to secure the IJV during CPR, but the catheter had been dislodged easily due to its short length. Therefore, we used midline catheter for IJV access. Finally, we measured the vascular access point to the heart using a measuring tape from the surface of the patient’s body, which might not be very accurate.
Conclusion
Based on our results, there was a trend toward higher success rates in the IJV rather than the PIV approach that was not statistically significant. Further studies are needed to determine how vascular access routes during CPR affect clinical outcomes in adults.
Footnotes
Author contributions
Conceptualization: HSC and JHL; Data curation: HSC and JHL; Formal analysis: HSC and JHL; Investigation: HSC and JHL; Methodology: HSC and JHL; Project administration: HSC and JHL; Resources: HSC, JHL, and HJP; Software: HSC and JHL; Supervision: HSC, JHL, GJP, SCK, HK, SWL, and YMK; Validation: HSC and JHL; Visualization: HSC and JHL; Writing—original draft: HSC and JHL; Writing—review and editing: HSC, JHL, GJP, SCK, HK, SWL, YMK, and HJP.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the research grant of the Society of Emergency Critical Care Imaging (2022).
Ethics approval
Ethical approval for this study was obtained from the Institutional Review Board of Chungbuk National University Hospital (CBNUH, 2021-10-018).
Informed consent
Informed consent was not sought for the present study because the requirement for consent was waived from the IRB of CBNUH because it was not possible to obtain consent during CPR.
Availability of data
The data presented in this report are available from the corresponding author.
