Abstract
Objective:
The need for telemedicine was felt more than ever during the COVID-19 pandemic, which impacted health care worldwide. Therefore, this study aimed to determine the difficulties faced by patients in visiting the cardiac outpatient department during COVID-19, along with assessing the awareness and acceptability of telemedicine.
Methods:
In this cross-sectional study, selected patients presenting to outpatient department of a tertiary care cardiac hospital were interviewed regarding the difficulties faced by patients in visiting the outpatient department during COVID-19 and their awareness and acceptability of telemedicine using a self-designed structured questionnaire.
Results:
Of the 403 patients, 58.3% were male, the mean age was 53.04 ± 11.73 years, and most (77.7%) were urban residents. Ischemic heart disease was present in 69.5%, followed by hypertension (38.7%) and heart failure (29.3%). A total of 26.6% required emergency room visits. Limited appointments (55.6%) was the most common problem faced by patients during COVID-19, followed by financial issues (17.1%), fear of acquiring infection (13.4%), and limited mobility due to lockdown (22.6%). Only 12.2% were aware of telemedicine, 4.5% had previously used it, and 41.2% were willing to opt for telemedicine in the future. No internet access (39.2%) was the key barrier to the usage of telemedicine, followed by a lack of free medicine (39%) and a lack of a smart device (31.5%).
Conclusion:
Limited appointments due to COVID-19 restrictions has made it difficult for patients to visit the clinics, which has led to increased emergency room visits. Telemedicine awareness was found to be limited; however, many patients were willing to adopt it provided their limitations could be overcome.
Introduction
COVID-19 disease is a disease of the lower respiratory tract, caused by the SARS-Cov-2 virus; it starts with flu-like symptoms. However, it may progress to a more pronounced and aggressive state, requiring conservative management, oxygen support, non-invasive ventilation, or ventilatory support. However, many cases may be asymptomatic and do not show any symptoms. 1 The COVID-19 virus pandemic started in Wuhan, China, in 2019 and then rapidly engulfed the entire globe, including America, Asia, Africa, Europe, and Australia. 2
The peak of the cases reached in the mid of 2020, with both developing and developed countries fighting against this deadly pandemic. As of December 23, 2022, the total number of cases of the disease worldwide was 651,918,402. Out of this number, the number of deaths was 6,656,601. 3 WHO labeled COVID-19 infection as a worldwide pandemic on March 11, 2020. 4 In Pakistan, the first case of the COVID-19 virus was officially confirmed on February 2020.5,6 The country has been battling a series of COVID-19 cases and variants since then.
The last updated figure depicting the total number of COVID-19 cases was 1,575,772, out of which 25 occurred in the last 24 h. Deaths due to COVID-19 disease were 30,636. This is as on December 30 2022. 7 The disease shook the entire world in a wave of restrictions. From travel to work and outdoor gatherings to large audiences, all were banned to prevent the spread of the virus. 8
On the one hand, this put the world economy in a grave setback; on the other hand, the global health industry also took a toll. The latter was not only due to the increasing number of COVID-19 pneumonia cases, but also due to other medical conditions that predisposed an individual to acquire COVID-19 infection.
Many individuals were reluctant to go to hospitals due to commute restrictions or the fear of catching the disease. So much so that their condition worsened, and they had to be brought to the emergency room (ER) in critical condition.
Research conducted by Khalid et al. in 2020 highlighted the challenges brought by the COVID pandemic and the need of the hour to tackle those. 9 A recent (2020) study by Shifat et al. gave a narrative of the health conditions in Pakistan, Kenya, Bangladesh, and Nigeria and pointed out that the COVID-19 pandemic and the necessary restrictions due to it hindered access of people to healthcare facilities for non-COVID conditions, particularly in slum areas, and also emphasized on the need of remote healthcare consultation. 10
This was a problem faced throughout the world in different areas. Considering these scenarios, telemedicine was highly recommended for the remote provision of healthcare facilities. Data published during the mid-COVID-19 crisis in June 2020 highlighted the urgent need for coordinated and digitalized healthcare records so that telemedicine may be taken into action. Health facilities may be provided in this way in both outpatient and inpatient/emergency cases. 11
Considering the ongoing COVID-19 pandemic across the globe and the people affected because of the disease and lack of access to health care, the dire need for telemedicine was recognized. However, data regarding it and its implications are almost nil in our setup.
This study aims to target the reasons behind the masses avoiding healthcare facilities during the COVID-19 pandemic and their reviews of telemedicine. It will also depict the pros and cons of reduced healthcare consultation due to the lockdown and its implications for accessing health facilities during the COVID-19 pandemic.
Methods
This cross-sectional study was conducted at the largest tertiary care cardiac hospital in Karachi, Pakistan. The total duration was 6 months, from April 11, 2021 to October 10, 2021. Participants of this study were adult patients aged more than 18 years and visiting outpatient department (OPD) for regular assessment. To avoid biases, OPD clinical of a single consultant, with the frequency of two clinics per week, was selected for data collection. Considering the survey nature of the study, the needed sample size for the study was not calculated formally, but a judgmental sample of 400 was decided by the principal investigator. Verbal consent for participation was taken from all the patients regarding their participation in the study, and all consecutive patients were recruited in this study.
Data were collected using an online questionnaire that consisted of two sections, one included the experience of patients in OPD during the COVID-19 pandemic, and the other one was for the use and acceptability of telemedicine. Difficulties faced, during the COVID-19 era (the year 2020), in visiting OPD were obtained on the patient recall basis, which included “limited mobility due to lockdown,” “fear of acquiring infection from the hospital,” “lack of transportation,” “limited appointments,” “restrictions on attendants being allowed,” “financial issue,” and others. In addition, the need for ER visits/hospitalization, medication adherence, and lifestyle compliance, such as exercise, walking, and other kinds of physical activities, during the COVID-19 era were also recorded.
The questionnaire used for data collection is provided as a Supplemental Material. It was a self-designed questionnaire reviewed by the two independent senior faculty members for validity and relevance of the content and questions. The questionnaire was also evaluated and approved by the ethical review committee and research development committee of the institution. Prior to the final execution of the survey, the questionnaire was used on 15 patients as a pilot run, and sequencing of the questions and linguistic corrections were made to meet the comprehension level of patients.
Statistical analysis
Data were collected after verbal consent from patients. The collected data were entered using IBM SPSS version 21, mean ± SD was calculated for continuous variables, and frequency and percentages were calculated for the categorical variables. Participants were stratified based on their residence as urban or rural, and the results were compared between the two groups with the help of the chi-square test and independent sample t-test appropriately. A p value ⩽ 0.05 was considered statistically significant.
Results
A total of 403 patients were interviewed, 58.3% (235) were male, the mean age was 53.04 ± 11.73 years, and a majority (77.7%) were from urban areas. The chief presenting complaint was shortness of breath followed by chest pain. Regarding cardiovascular diagnosis, most had ischemic heart disease, and more than one-fourth suffered from heart failure (Table 1). The limited appointments was the main difficulty faced by the patients, followed by limited mobility due to lockdown as the second most common difficulty faced by patients visiting OPD during the COVID-19 era (Table 1).
Demographic and clinical profile and healthcare-seeking experience of study participants during COVID-19.

CAD: coronary artery diseases; ER: emergency room; OPD: outpatient department.
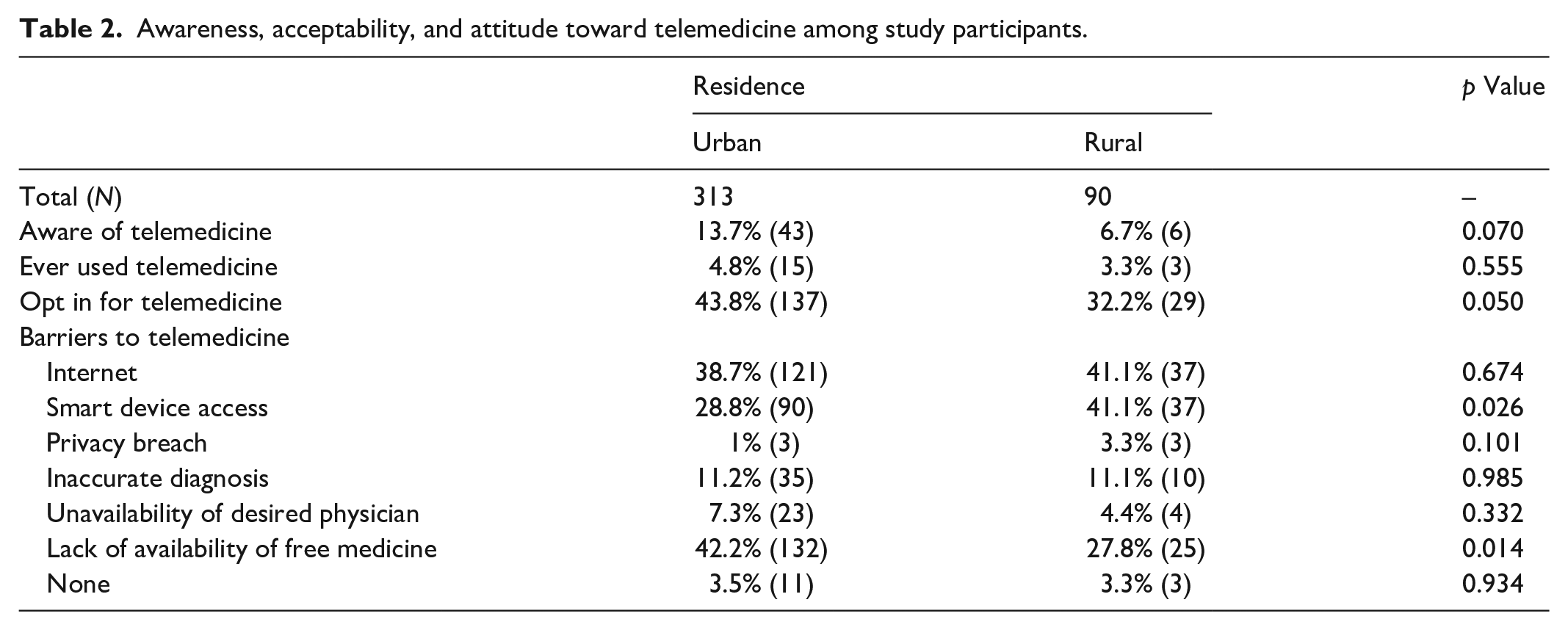
Regarding telemedicine, 12.2% of the patients were aware of it, and only 4.5% had previously used it, with 41.2% willing to opt for telemedicine in the future. Regarding barriers to telemedicine usage, 39.2% of patients had no access to the internet, 31.5% did not have a smart device, and 11.2% were afraid of being misdiagnosed (Table 2).
Awareness, acceptability, and attitude toward telemedicine among study participants.
Discussion
This study was conducted in one of the largest tertiary care settings in Karachi, Pakistan, to assess the accessibility of people to healthcare facilities during the COVID pandemic. Male and female patients from urban and rural areas were interviewed regardless of the presenting complaint. Most participants in our study had difficulty accessing health care due to the COVID-19 pandemic. A high percentage of patients had trouble obtaining outpatient appointments as the number of appointments offered was reduced due to COVID-19; few had financial constraints due to the pandemic and rising costs, some feared contracting COVID-19 from hospitals or clinics, and others mentioned limited mobility and commute due to lockdown as the reason for lack of consultation. Some studies reported similar findings; all sites reported decreased access to health care, including preventive services, due to COVID-19. Healthcare expenses rose while average family incomes fell. Hurdles in getting to hospitals or clinics were a common complaint from residents. Health care was less sought because people were afraid of contracting COVID-19.10,12,13 A drastic reduction in the number of primary care consultations was observed by Schäfer et al. 12 This effect was independent of the general practitioner’s specialty, patients’ age, gender, and urban or rural location. Particularly impacted were consultations for low back pain, gastrointestinal complaints, vertigo, and fatigue, as well as services such as house calls/calls to nursing homes, wound treatments, pain therapy, and screening examinations for the early detection of chronic diseases. Pillay et al. conducted a study in South Africa and found that accessibility to normal health care decreased as a consequence of the COVID-19 pandemic reactions, which included varying degrees of lockdowns, the limiting of health services, a shortage of employees due to COVID-19 infection, fear, and stigma. Nonetheless, the situation varies by service type, province, and area, with some faring worse than others. All provinces restricted access to public health care between March 2020 and December 2020. However, this was not linear since not every service in every region was impacted in the same way. Prenatal appointments before 20 weeks, access to contraception, and HIV and TB testing were the services worst hit. The effect on maternal and neonatal mortality was quantifiable and observable. 13
Participants in our study were given a choice between telemedicine and in-person consultation, and their opinions were recorded. For most participants, this was a novel phenomenon, as only a small percentage of people were familiar with this technology. Less than half of those who were aware of telemedicine had used it before, whereas nearly half of those who were unaware were willing to use it in the future. Diverse causes may account for the varying inclination of people to choose telemedicine. In our study, many individuals resisted this technology because they lacked internet access, did not have smartphones, feared being misdiagnosed via the internet, and lacked access to free medication.
In a study conducted by Jordan DN et al., participants quoted that the patient’s first interaction with the physician should be physical, allowing for proper history and examination. For chronic cases, telemedicine can be a good option as the doctor is also acquainted with the condition of the patient and the nature of their recovery. 14 Another recent study conducted in 2019 by Bokolo AJ et al. also gave similar results, with the people dictating that they feared the insecure internet facility might not give the full benefits of telemedicine. 15 In a study conducted in Bulgaria among young adults, although a good number of the participants were well versed with technology, a limited number were willing to use telemedicine due to concerns of information security. 16
As the benefits of telemedicine were discussed and studied, people also favored it as it was cost-effective and did not need long commutes or waiting lines in the clinics. 14
The current COVID pandemic has brought us to terms with reality and the downside of the medical field. With the digitalization in every other field, it is the need of the hour to make medical records digital and individualized to keep them secure and easily accessible. The leading heads of the healthcare industry need to sit down and devise a plan for its strategic planning and execution. Multiple measures must be taken for its success, including training of the healthcare personnel, general awareness among the masses, setup of the gear, funding of the projects, good internet availability, software development for the project, and IT maintenance of it. It would be cost-effective and easy as waiting in the clinics, and long commutes can be prevented this way.15,17
Experiencing telemedicine alters attitudes concerning its use. In our research, the majority of participants had no prior experience with telemedicine and exhibited some reluctance; nevertheless, in a similar study with a comparable demographic, reactions were more favorable among respondents who had prior telemedicine experience. 18
During future COVID-19 waves, it is essential to guarantee that routine services are not negatively affected. Care providers must meticulously plan and communicate with patients and communities. 13 Telemedicine provides a handy and effective method for providing healthcare services in emergency and primary care settings to reduce the risk of infection. However, the acceptability of digital solutions may be hindered by possible cultural, moral, and religious disputes among users. Digital technologies may give communal advantages to public health; nevertheless, they may be obtrusive and undermine individual liberties or leave vulnerable groups behind. During the COVID-19 pandemic, various digital health technologies were evaluated, and their potential was shown. To guarantee that future digital health projects have a more considerable effect on the pandemic and satisfy the most strategic demands to improve the lives of those at the frontline of the issue, more concentrated measures should be adopted. 11 Despite the fact that a significant percentage of participants expressed a positive reaction to telemedicine, it is necessary to develop local telemedicine standards, educate consultants, and enhance technology. A survey was conducted in Pakistan among those who had availed services through telemedicine. A total of 251 patients replied to the telemedicine survey. Overall, 61% of patients said that they did not need assistance with the use of technology during consultations, and 96% of patients reported that telemedicine reduced their trip time. Gender, education, and age were shown to be strongly connected with the ease of technology, but only education and age were found to be significantly associated with future telemedicine usage. 18
Our research recommends expanding the network for telemedicine: allow the public to experience this convenience and create more centers and train the employees. The level of generalized awareness must rise. It is possible to overcome obstacles such as internet access and smart gadgets by building small, well-equipped centers nearby or promoting cheaper alternatives. Concerning the community’s worries that the service is equally effective or not, reassurance is necessary. A maximum number of doctors may be connected to compensate for the unavailability of the participants’ selected providers. Concerning the issue of the non-availability of free medication via telemedicine, plans may include free medicine delivery services or health cards linked with online prescriptions. We urge that future research examine the concerns and benefits of telemedicine among those who have used it and those who have not. Effects on hospital patient load and overall patient management must be determined through follow-up studies.
The limitations of our study were that we only included patients who reached the OPDs and could not interview the ones who failed to reach out due to various limitations. Second, the sample size for the survey was not explicitly calculated, and a judgmental sample size was taken. After working on the limitations highlighted during our investigation, a follow-up study is required to see how things changed from a patient’s perspective.
Conclusion
It was found that limited appointments due to COVID-19 restrictions, distancing measures, lockdowns, and restricted mobility of the masses have made it difficult for patients to visit the clinics, which has led to patients visiting the ER. Telemedicine awareness was limited; however, it was encouraging to see that many patients were willing to adopt, provided their limitations could be overcome.
Supplemental Material
sj-docx-1-smo-10.1177_20503121231153755 – Supplemental material for Impact of COVID-19 on cardiovascular clinics: Are we ready for telemedicine?
Supplemental material, sj-docx-1-smo-10.1177_20503121231153755 for Impact of COVID-19 on cardiovascular clinics: Are we ready for telemedicine? by Mustajab Mujtaba, Sapna Kotwani, Danish Qayyum, Tahir Saghir, Khalid Iqbal Bhatti, Muhammad Rahman Khalid, Muhammad Faisal Khanzada, Saba Aman, Khalil Ahmed Shaikh, Sharfuddin Buraro and Musa Karim in SAGE Open Medicine
Footnotes
Acknowledgements
The authors wish to acknowledge the support of the staff members of the Clinical Research Department of the National Institute of Cardiovascular Diseases (NICVD) Karachi, Pakistan.
Author’s contribution
MM, SK, MK, DQ, TS, and KIB contributed to the concept and design of study; MM, MK, SK, DQ, KA, and SB contributed to the analysis and interpretation of data; MM, SK, MK, DQ, KA, MRK, SA, SB, and MFK collected data and drafted the manuscript; and TS, KIB, and MK critically analyzed for content. All authors approved the final draft of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
This study was approved by the ethical review committee of the National Institute of Cardiovascular Diseases (NICVD), Karachi (ERC-88/2020).
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Verbal informed consent was obtained from all subjects before the study.
Trial registration
Not applicable.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
