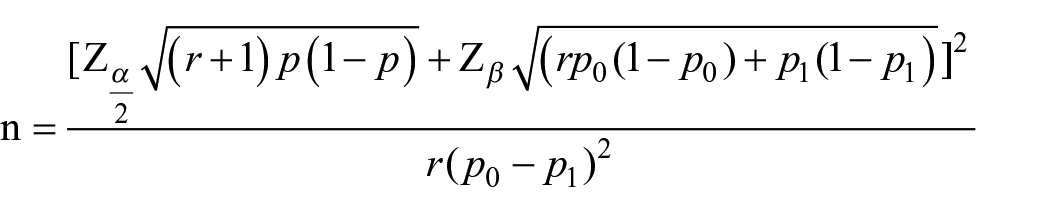Abstract
Objectives:
Maternal undernutrition is a burning issue in Ethiopia. However, updated evidence is limited in the eastern part of the country; particularly the mental health-related factors of undernutrition. The study, hence, aimed at assessing the prevalence and predictors of undernutrition among rural pregnant women in eastern Ethiopia.
Methods:
A cross-sectional research was carried out at a community level among 1015 randomly selected pregnant women. A structured questionnaire was used to collect the data through face-to-face interviews. The characteristics of participants were described and summarized by frequencies, percentages, and summary measures. Logistic regression was performed to find out factors related to undernutrition.
Results:
The prevalence of undernutrition was 43.8% (95% confidence interval: 40.8, 47.0). Early marriage (adjusted odds ratio = 2.63, confidence interval: 2.00, 3.47), no antenatal care follow-up (adjusted odds ratio = 1.73, 95% confidence interval: 1.31, 2.29), inadequately diversified diet (adjusted odds ratio = 2.48, 95% confidence interval: 1.77, 3.48), current substance use (adjusted odds ratio = 1.50, 95% confidence interval: 1.02, 2.19), history of mental illness (adjusted odds ratio = 2.44, 95% confidence interval: 1.02, 5.82), and common mental disorders (adjusted odds ratio = 1.81, 95% confidence interval: 1.34, 2.43) were the significant predictors of undernutrition among pregnant women.
Conclusions:
Undernutrition was a significant public health issue among rural pregnant women. Age at first marriage, antenatal care follow-up, dietary diversity, current substance use, history of mental illness, and common mental disorder were the independent predictors of undernutrition. Therefore, the health offices of Kersa and Haramaya districts should invest their efforts to prevent undernutrition among pregnant women through nutrition counselling and education, and mental health and psychosocial support.
Introduction
Malnutrition affects one-third of the world’s population. 1 Its burden and consequences are exceedingly prevalent in low- and middle-income countries and cause a significant increase in mortality.2–4 This is due to low socio-economic status, poor food intake, unbalanced food share within households, food insecurity, food taboos, repeated infectious diseases, and poor care practices in these countries.5,6
Women of reproductive age (15–49 years) are among the vulnerable groups to all forms of malnutrition.7,8 The highest burden of maternal malnutrition occurs in South-central and Southeast Asia, and sub-Saharan Africa (SSA).9,10 The prevalence of maternal undernutrition was more than 15% in nine African countries from 2000 to 2015, where maternal underweight surpasses 20% in three of these countries, including Ethiopia.11,12
Maternal nutrition has a paramount significance in determining maternal, newborn, and child health outcomes.13,14 It is important for the prevention of child stunting in the first 2 years of life, and consequent obesity and non-communicable diseases in later life.15,16 Maternal undernutrition increases the risk of poor obstetric and birth outcomes, and long-term physical and cognitive consequences.17–22
The World Health Assembly, in line with the Sustainable Development Goal 2 (SDG-2), endorsed a comprehensive implementation plan to achieve the ending of all forms of malnutrition and ensure healthy lives and well-being for all at all ages.23,24 The assembly underlined the importance of introducing a nutrition policy that gives due consideration to maternal and child nutrition by its member states.9,25 Following this, the government of Ethiopia developed different strategies, programs, and policies, including the recently approved food and nutrition policy, to accelerate the reduction of malnutrition.26,27 For the implementation, monitoring, and evaluation of such a plan of interventions, up-to-date evidence is required.
Several community-based studies were done in Ethiopia regarding undernutrition in pregnant women.28–42 The average pooled prevalence of undernutrition from these studies was 29.07%, 43 where the lowest (14.4%) and highest (47.2%) prevalence were reported from Amhara and Oromia regions, respectively.28,36 In addition, these studies identified factors associated with undernutrition in women of reproductive age including age, marital status, level of education, income, workload, women’s decision, dietary advice, dietary diversity, meal frequency, family planning, unplanned pregnancy, antenatal care follow-up, parity, gravidity, gestational age, and iron supplementation.30,32–35,43
Despite all these studies being done in Ethiopia, the prevalence can vary with time and place, and updated evidence is limited in the eastern part of the country. On top of that, the mental health-related factors of undernutrition are not well investigated. As both undernutrition and mental health problems are major public health issues, endless up-to-date evidence is required for context-specific interventions, including the integration of mental health assessments into nutrition programs and services. Hence, the study was designed to assess the prevalence of undernutrition and related factors—including mental health factors—among rural pregnant women in eastern Ethiopia. We concentrated on rural women because the burden of undernutrition is more pronounced among rural residents of Ethiopia.12,44
Methods
Study setting
The research was undertaken in the Kersa and Haramaya Health and Demographic Surveillance System (HDSS) sites of Haramaya University from 30 January to 30 April 2021. Kersa and Haramaya HDSS are among the seven HDSS sites of Ethiopian universities intended to reveal some profiles of the country related to health and demography. Kersa HDSS is found in the Kersa District of East Hararghe Zone in Oromia Region. Kersa Town is the district’s administrative center, which is situated 484 km to the east of the capital Addis Ababa, on the way to Harar City. Kersa district has 35 rural and 3 small-town Kebeles (Kebele is the smallest administrative unit in Ethiopia). The total population of the district is 172,626, where urban residents account for 6.9%. The Kersa HDSS consists of 24 kebeles, 4 health centers, and 10 health posts. There were 1834 pregnant women during the study period. Haramaya district is another district found in the East Hararghe Zone of the Oromia Region. Haramaya Town is its administrative center, which is found at 506 km to the east of the capital Addis Ababa, on the way to Harar City. Haramaya district has a total population of 220,986 living in 33 rural and 2 urban kebeles. Haramaya HDSS covers 12 rural kebeles. There were 1036 pregnant women during the study period. The main sources of income for the residents include farming, small-scale trade, government employment, and daily labor.
Study design and population
This research used a community-level cross-sectional study design. The source population of the study was all pregnant women living in the HDSS sites, while the study population was pregnant women living in the selected kebeles of the HDSS sites. Women who were unable to respond to the questionnaire due to health problems were excluded from the study.
Sample size determination and sampling techniques
The study aimed to address two objectives: One was “to assess the prevalence/magnitude of undernutrition among pregnant women” and the second was “to identify the predictors of undernutrition among pregnant women.” Sample sizes were calculated for these objectives separately. Finally, the sample size calculated for the second objective (i.e. 1026) was planned for this study as it is larger than the sample size calculated for the first objective.
To assess the prevalence/magnitude of undernutrition among pregnant women (i.e. the first objective), the sample size was calculated by the formula for single population proportion 45
where Zα/2 at two-sided significance level of 95% = 1.96; level of precision (d) = 5%; design effect (deff) = 1.5; proportion of undernutrition (p) in pregnant women from previous study in the Kersa District of eastern Ethiopia = 47% 28
Adding 10% for the non-response rate, gives 631.
To identify the predictors of undernutrition among pregnant women (i.e. the second objective), the sample size was estimated using Epi Info version 7 (freely available statistical software from the Centers for Disease Control and Prevention (CDC) in Atlanta, Georgia, USA). The software estimates sample sizes for both exposed and unexposed groups based on the Fleiss formula for double population proportion with continuity correction 46
where
Proportion of undernutrition in pregnant women learned up to elementary level or below (
Proportion of undernutrition in pregnant women learned above elementary level (
The software produced a total sample size of 622 (311 for exposed and 311 for unexposed groups). Then, we multiplied the total sample size by a design effect of 1.5, Which resulted in 933. Adding 10% for non-response, the final calculation provided a sample size of 1026.
Regarding the selection process of participants, 30% of the total kebeles were randomly chosen from each HDSS, that is, 8 kebeles from Kersa (out of the total 24) and 4 kebeles from Haramaya (out of 12). At this stage, 1259 pregnant women were excluded (773 from Kersa and 486 from Haramaya). Then, the total sample size was proportionally allocated to each selected kebele based on their population size. Again, at this stage, 585 women were excluded (385 from Kersa and 200 from Haramaya). Finally, the individual pregnant women (actual study participants) were chosen from each selected kebele by lottery method.
Data collection and measurements
A structured and interviewer-administered questionnaire was used to gather the data. The questionnaire contains questions on socio-demographic and economic characteristics; reproductive, medical, and mental conditions; and feeding practices. In addition, the mid-upper arm circumference (MUAC) measurements of women were recorded to evaluate their nutritional status. Twenty data collectors and six supervisors were involved in the data collection. An open data kit (ODK) application (a freely available application from Google Play Store) was applied to gather and record the data in a face-to-face interview. The application is installed on Android mobile devices, where data collectors submit their data to a central server. In case a connection is interrupted, data collectors can save their data and proceed with data gathering upon Internet re-connection.
To assess and measure economic/wealth status, data were gathered on household properties/assets using a tool adapted from the Ethiopia Demographic and Health Survey (EDHS) of 2016. 12 Then, households were classified into tertiles as a poor, medium, and rich based on the level of wealth index.
A standard model questionnaire of 10 food groups was applied to gather data on diet diversity, in which the food items were adapted to the local context. 48 The 10 food groups include the following: (1) grains, white root, tubers, and plantains; (2) pulses (beans, peas, and lentils); (3) nuts and seeds; (4) dairy; (5) meat, poultry, and fish; (6) eggs; (7) dark green leafy vegetables; (8) other vitamin-A-rich fruits and vegetables; (9) other vegetables; and (10) other fruits. The Minimum Dietary Diversity for Women (MDD-W), a population-level validated indicator for women aged 15–49 years, was used to classify women into two categories. Accordingly, pregnant women who consumed at least 5 of the 10 food groups over a 24-h recall period were classified as having adequate diet diversity. 48
Data regarding CMD were collected and measured among pregnant women using locally validated World Health Organization’s (WHO) Self-Reporting Questionnaire-20 (SRQ-20).49–51 The SRQ-20 is composed of 20 “yes/no” items asking about the experience of depression, anxiety, panic, and somatic symptoms in the preceding 30 days. Pregnant mothers who answer “yes” to six or more of the SRQ-20 were categorized as having a high level of CMD.52,53
To evaluate the substance use behavior of pregnant women, we adapted questions from the Alcohol, Smoking, and Substance Involvement Screening Test (ASSIST) with modifications. The tool is validated and covers 10 substances: tobacco, alcohol, cannabis, cocaine, amphetamine-type stimulants (ATS), inhalants, sedatives, hallucinogens, opioids, and other drugs. 54 In this study, khat and shisha were included under the stimulant and tobacco categories, respectively. If participants had used any type of substance in the last 3 months preceding the study, they were classified as “current substance users” and those who ever used at least one type of substance in their lifetime were classified as “lifetime substance users.”54–56
To evaluate the nutritional status of pregnant women, two MUAC measurements were taken from the non-dominant arm with a non-stretchable standard MUAC tape with no clothing on the arm. Measurements were recorded to the nearest 0.1 cm, and an average of the two measurements was used for analysis. Women with average MUAC measurements of less than 23 cm were classified as having “undernutrition” while those with MUAC ⩾ 23 cm as “no undernutrition.”10,57,58
Operational definitions
ANC follow-up: This variable was categorized as “yes” if a pregnant woman attended at least one ANC visit for her current pregnancy and “no” if no visit at all.
Gravidity: This is defined as the number of times that a woman has been pregnant. Gravidity was classified into primigravida (a woman who has been pregnant once), multigravida (a woman who has been pregnant 2–4 times), and grand multigravida (a woman who has been pregnant 5 times or more). 59
Parity: This is defined as the number of times that a woman has given birth to a viable fetus (⩾28 weeks of gestation), regardless of whether the child was born alive or was stillborn. Parity was categorized into primipara (a woman who has given birth once), multipara (a woman who has given birth 2–4 times), and grand multipara (a woman who has given birth 5 times or more).59,60
Data quality control
To maintain the quality of our data, the data collectors and supervisors were trained for 4 days on the data collection instrument and data gathering procedure. To minimize errors in MUAC measurements, anthropometric standardization was carried out using the ENA software program version 2020 (freely available software from SMART—an inter-agency initiative launched in 2002). Questionnaire pre-testing was undertaken on 5% of the sample size, and modifications were made based on the results of the pre-test. The data gathering was closely supervised by supervisors and investigators. The completeness of each questionnaire was checked daily.
Statistical analysis
The data stored in the server were downloaded as an Excel (.xls) file. The data were explored for completeness and cleaned accordingly. STATA version 16 for windows 61 was applied for analysis. Frequencies, percentages, summary measures, tables, and figures were used to describe and present the descriptive information of respondents. Both numerical and visual normality tests were carried out to choose the appropriate summary measures for the continuous/discrete variables. The outcome (dependent) variable was dichotomized as “1” for “having undernutrition” and “0” for “no undernutrition.” We performed principal component analysis to produce the indicator “household wealth index” in the form of tertiles.
Bivariate analysis was carried out to assess the crude relationship between each predictor and outcome variables. Crude odds ratio (COR) with a 95% confidence interval (CI) was computed to show the crude associations. Predictors having a p-value less than 0.25 in the bivariate analysis were considered for further multivariate analysis. The variables were included in the final multivariate analysis model by the stepwise forward variable selection method. A multicollinearity diagnostic test was undertaken by a variance inflation factor (VIF) to observe whether there were significant linear relationships among the predictor variables. However, no considerable collinearity (VIF ⩾ 2.5) 62 was detected; the highest VIF value was 1.21 for the variables “gestational age” and “ANC follow-up.” Hosmer–Lemeshow test was applied to evaluate the final model goodness-of-fit, and the model was found well-fitted (p-value of the test = 0.42). Finally, an adjusted odds ratio (AOR) with 95% CI was computed in the final model to show the presence, strength, and direction of associations, thereby controlling the confounding effects. A p-value of <0.05 was considered for statistical significance.
Results
Socio-demographic characteristics
One thousand fifteen pregnant women were involved in the final analysis (response rate = 98.9%). The median age of the participants was 28.9 years (interquartile range (IQR) =10.4) and 676 (66.6%) were in the age range of 20–35 years. Nine hundred eighty-two (96.8%) participants were married, 1012 (99.7%) were Muslims, and 1010 (99.5%) were ethnic Oromo. About three-fourths (76.1%) of the participants were neither able to read nor write, and 900 (88.7) were housewives in occupation. Regarding the wealth status of participants’ households, 388 (38.2%) of them were in the first tertile (poor) category (Table 1).
Socio-demographic characteristics among rural pregnant women at Kersa and Haramaya HDSS sites, eastern Ethiopia, September 2021.

Petty trader, student, retired, unemployed.
Mental and medical health conditions
The study showed that 26 (2.6%) of the participants included in this study had a previous history of mental illness, with an average illness duration of 2.7 years (SD = 1.4). Of them, 10 (38.5%) were on treatment during the study period. On the other hand, 23 (2.3%) of the participants had chronic medical illnesses and 17 (73.9%) were on treatment. Hypertension (43.5%), kidney disease (43.5%), and other chronic illnesses such as diabetes and asthma (30.3%) were the medical conditions reported by the women.
Reproductive, obstetric, and gynecological conditions
Of the participants included in the final analysis, 542 (53.4%) were grand multigravida, while 472 (46.5%) were multipara. About half (52.1%) of the participants were in the third trimester of pregnancy, with a median gestational age of 32 weeks (IQR = 8.0). Ninety-eight (9.7%) participants had a previous history of abortion, and 488 (48.1%) were on ANC follow-up for their current pregnancy. Besides, 70 (6.9%) of the participants had a history of gynecological problems, where tumor (41.4%) was the most prevalent one. The mean inter-pregnancy interval and age at first marriage of the participants were 1.7 (SD = 0.6) and 17.7 (SD = 2.1) years, respectively (Table 2).
Reproductive, obstetric, and gynecological conditions among rural pregnant women at Kersa and Haramaya HDSS sites, eastern Ethiopia, September 2021.

HDSS: Health and Demographic Surveillance System; ANC: antenatal care.
Common mental disorders and substance use
The median SRQ-20 score of the pregnant women was 2.0 units (IQR = 7.0). The overall prevalence of CMD was 37.5% (i.e. they had high CMD symptoms). Four hundred fifty-four (44.7%) of the women had low CMD symptoms, while 180 (17.7%) had no CMD symptoms. Regarding substance use, 207 (20.4%) and 158 (15.6%) of the participants were lifetime and current substance users, respectively (Figure 1).
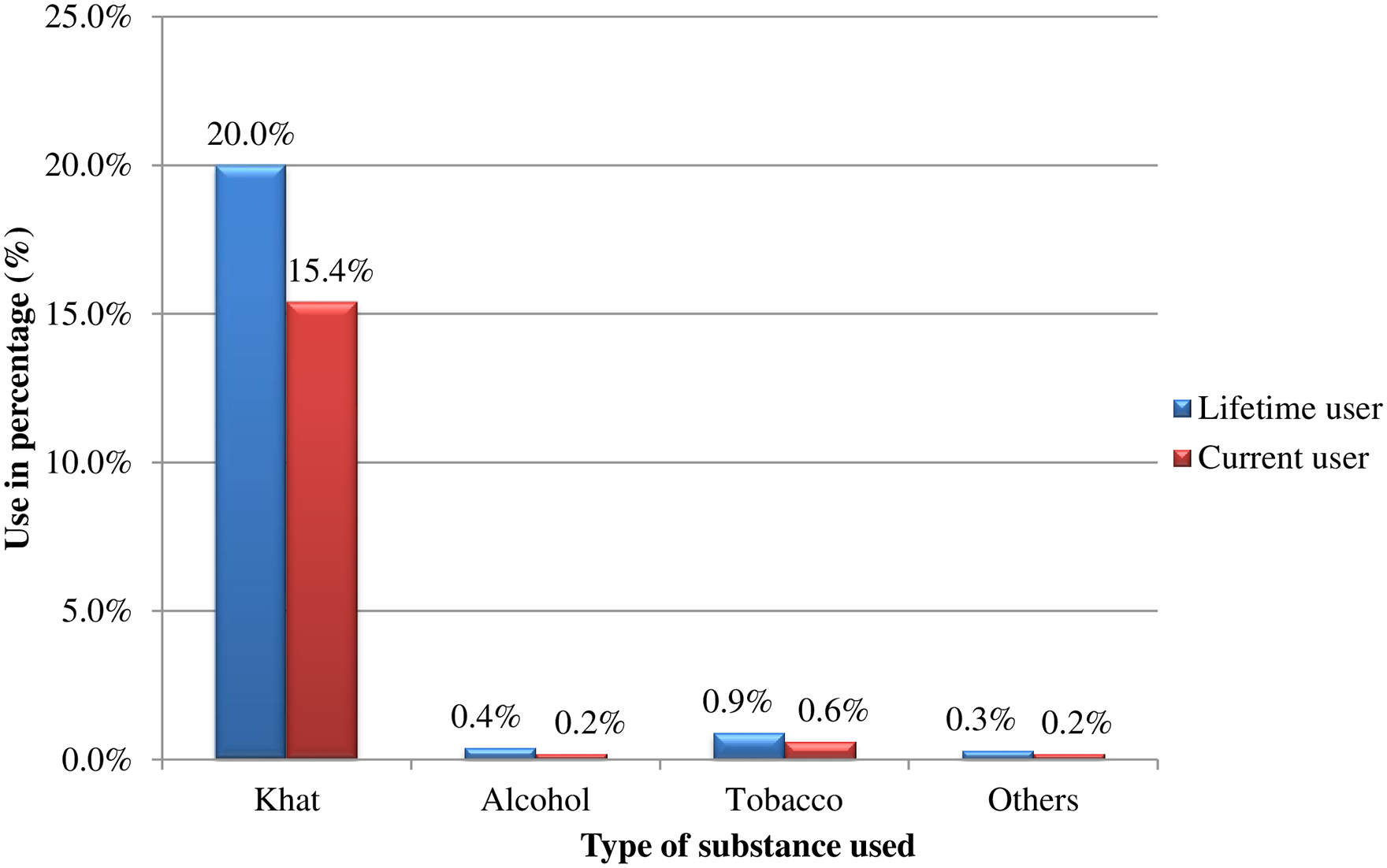
Types of substances used by rural pregnant women at Kersa and Haramaya HDSS sites, eastern Ethiopia, September 2021.
Food intake and nutrient supplementation
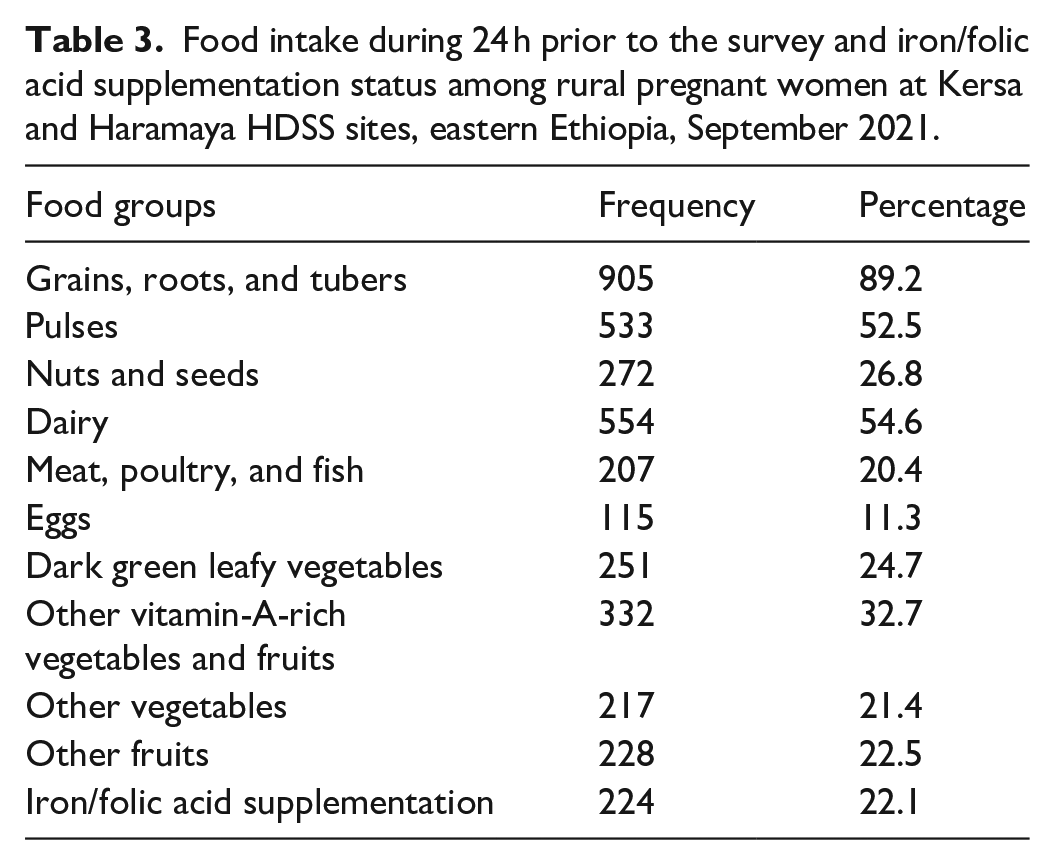
The study revealed that the median meal frequency of pregnant women during the 24-h before the survey was 2.0 (IQR = 1.0) and 415 (40.9%) of the women reported as they consume at least one extra meal per day. The median dietary diversity score of the women was 3.0 (IQR = 3.0), and 287 (28.3%) met the minimum dietary diversity for women. Grains, white roots, tubers, and plantains were the commonest consumed food group (89.2%) by the women, followed by dairy products (54.6%) and pulses (52.5%). On the contrary, eggs (11.3%) and meat/poultry/fish (20.4%) were the least consumed food groups. Concerning iron and folic acid supplementation, 224 (22.1%) of the women reported as they received the supplementation in the current pregnancy (Table 3).
Food intake during 24 h prior to the survey and iron/folic acid supplementation status among rural pregnant women at Kersa and Haramaya HDSS sites, eastern Ethiopia, September 2021.
Prevalence of undernutrition and its predictors
The median MUAC measurement of the pregnant women included in this study was 23.0 cm (IQR = 1.2), and 445 (43.8%) of the women were found to have undernutrition (95% CI: 40.8, 47.0). The prevalence of undernutrition was higher among women who were below 18 years old at marriage (65.8%) than those who were married at 18 years old or above (34.2%). Undernutrition was also higher among women who were in their third trimester of pregnancy (59.6%) than those in their second (38.9%) and first (1.6%) trimesters. Furthermore, undernutrition was found higher in multipara (53.7%) and grand multipara (40.7%) than in primipara (5.6%) women.
In the bivariate analysis, age at first marriage, gestational age, ANC follow-up, dietary diversity, current substance use, and CMD were significantly associated with undernutrition, whereas early marriage, not attending ANC follow-up, inadequate dietary diversity, being a current substance user, history of mental illness, and CMD were the significant predictors of undernutrition in the final multivariate model.
Pregnant women, who were below 18 years old during their first marriage, were 2.63 times more likely to have undernutrition compared to those married at 18 years or above (AOR = 2.63, CI: 2.00, 3.47). The odds of undernutrition were 1.73 times higher among women who did not attend ANC follow-up in their recent pregnancy than those who did attend at least one visit (AOR = 1.73 95% CI: 1.31, 2.29). Likewise, the occurrence of undernutrition was 2.48 times higher in women who consume inadequately diversified diets than those who consume adequately diversified (AOR = 2.48, 95% CI: 1.77, 3.48). Current substance user women were 1.50 times more likely to develop undernutrition compared with non-users (AOR = 1.50, 95% CI: 1.02, 2.19). Besides, the odds of undernutrition were 2.44 times higher in women with a previous history of mental illness (AOR = 2.44, 95% CI: 1.02, 5.82). Furthermore, pregnant women diagnosed to have CMD were 1.81 times higher to develop undernutrition than their counterparts (AOR = 1.81, 95% CI: 1.34, 2.43) (Table 4).
Factors associated with undernutrition among rural pregnant women at Kersa and Haramaya HDSS sites, eastern Ethiopia, September 2021.

COR: crude odds ratio; CI: confidence interval; AOR: adjusted odds ratio; ANC: antenatal care.
Significant at p < 0.05; **significant at p < 0.001.
Discussion
The findings of our research reported the magnitude and related factors of undernutrition among rural pregnant women in Kersa and Haramaya HDSS sites, eastern Ethiopia. Consequently, the MUAC measurement results indicated that 43.8% (95% CI: 40.8, 47.0) of the women had undernutrition. Early marriage, not attending ANC follow-up, inadequate dietary diversity, current substance use, history of mental illness, and CMD were identified as significant predictors of undernutrition in rural pregnant women.
The global burden of undernutrition during pregnancy seems to be declining in nearly all regions of the world. However, the magnitude of undernutrition during pregnancy has been increasing progressively in Africa. 63 In line with this, the occurrence of undernutrition in this research was found four times greater than the cutoff value to declare maternal undernutrition as a main public health issue, which is 10%.8,63,64 The prevalence was also consistent with previous studies,40,42,65,66 and higher than other study findings37,38 conducted in different parts of Ethiopia. The reasons for the higher prevalence in eastern Ethiopia might be due to variations in socio-demographic characteristics, study setting, sample size, and population. While our research was community-based and focused on rural women, the other studies were institution-based 37 and conducted among urban women. 38 Evidence shows that undernutrition is more common among rural residents than urban dwellers in Ethiopia.12,44
According to this study, undernutrition was more likely to occur in women who were less than 18 years at their first marriage, which is in agreement with a previous study conducted in Ethiopia. 30 Women aged less than 18 years need more energy and nutrients to attain full growth and development. If they get married before achieving maximum growth, they face early pregnancy and high fertility with short birth intervals, unwanted and unplanned pregnancies, and unsafe abortions. These all negatively affect and deteriorate their nutritional status.67,68 Consistent with previous studies done in Ethiopia, women who did not attend ANC follow-up for at least one visit were more likely to be affected by undernutrition in our study.30,42 Visiting health facilities for ANC follow-up is a good opportunity for pregnant women to obtain nutrition information and counselling from health professionals. This could, in turn, improve their nutrition knowledge, healthy dietary practices, and nutritional status. 69
The likelihood of undernutrition was higher in this study among the rural pregnant women who did not meet the minimum dietary diversity for women, which is in line with the findings of the previous studies.42,70–72 This could be expressed as consuming a variety of food items is fundamental to obtaining all the important nutrients to prevent undernutrition related to nutrient inadequacy.6,73,74
The current study found that mental illnesses and substance use were among the significant predictors of undernutrition, which are poorly assessed, particularly in Ethiopia. Women who reported having a history of mental illnesses were more likely to develop undernutrition. Similarly, the occurrence of undernutrition was higher in women who were diagnosed with CMD. This could be explained as mental health problems leading to unhealthy behavioral changes, including unhealthy eating behaviors, which have negative effects on nutrition. 75 Furthermore, undernutrition was significantly higher in current substance users than non-users, which is supported by a previous study finding reported from Ethiopia. 40 The use of substances can result in disordered lifestyles such as less food expenditure share and poor eating habits, which finally lead to undernutrition.76,77
Limitations of the study
As the study is cross-sectional type, a temporal relationship cannot be established. The research might have suffered from a recall bias as the data gathering tools for dietary diversity, mental illnesses, and substance use were recall-based. To reduce this bias, we trained enumerators by what method to probe the study participants—for instance, beginning with events that occurred recently and allowing adequate time for participants to remember events that happened a long time back. The study might also have suffered from MUAC measurement errors. To lessen this problem, we trained the enumerators and supervisors on MUAC measurements, followed by standardization tests.
Conclusion
The magnitude of undernutrition was found to be a major public health issue; where about two of every five pregnant women had undernutrition. Early marriage, not attending ANC follow-up, inadequate dietary diversity, current substance use, history of mental illness, and CMD were identified as significant predictors of undernutrition among rural pregnant women.
Therefore, the health offices of Kersa and Haramaya districts, in collaboration with other stakeholders, should work to improve the nutrition of pregnant women through behavioral changes at a community level. Continuous key messages should be disseminated to the community on the effects of early marriage, ANC follow-up, feeding practices, substance use, and mental illnesses on maternal nutrition, especially during pregnancy. In addition, efforts should be made to integrate mental health interventions into maternal nutrition programs and services.
Supplemental Material
sj-docx-1-smo-10.1177_20503121221104430 – Supplemental material for Undernutrition and associated factors among rural pregnant women in Eastern Ethiopia
Supplemental material, sj-docx-1-smo-10.1177_20503121221104430 for Undernutrition and associated factors among rural pregnant women in Eastern Ethiopia by Berhe Gebremichael, Tadesse Misgana, Dawit Tamiru, Mandaras Tariku, Dejene Tesfaye, Daniel Alemu, Adisu Birhanu Weldesenbet and Merga Dheresa in SAGE Open Medicine
Footnotes
Acknowledgements
Our appreciation goes to Haramaya University for providing the budget funding. We extend our acknowledgements to the staff of the Kersa and Haramaya HDSS, supervisors, enumerators, and all respondents for their assistance.
Author contributions
All authors had substantial involvement in the conception and designing of the research, fieldwork, data analysis, interpretation, and article drafting, revising, and final approval for submission.
Data availability
Data are available from the corresponding author upon request.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval and consent to participate
This research was carried out in conformity with the Declaration of Helsinki. Ethical approval was obtained from the Institutional Health Research Ethics Review Committee (IHRERC) of the College of Health and Medical Sciences at Haramaya University (ethics approval number: IHRERC004/2021). A written informed consent was obtained from all subjects before the study. The participants were interviewed and measured in private areas/rooms. To ensure the confidentiality of the study participants, we avoided all possible personal identifiers from the questionnaire.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The fund for this research was acquired from Haramaya University. However, the funding body had no role in planning the research, fieldwork, analysis, interpretation, and article writing up.
Informed consent
Written informed consent was obtained from all subjects before the study.
ORCID iDs
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.