Abstract
Objectives:
Non-pharmaceutical interventions (e.g. quarantine and isolation) are used to mitigate and control viral infectious disease, but their effectiveness has not been well studied. For COVID-19, disease control efforts will rely on non-pharmaceutical interventions until pharmaceutical interventions become widely available, while non-pharmaceutical interventions will be of continued importance thereafter.
Methods:
This rapid evidence-based review provides both qualitative and quantitative analyses of the effectiveness of social distancing non-pharmaceutical interventions on disease outcomes. Literature was retrieved from MEDLINE, Google Scholar, and pre-print databases (BioRxiv.org, MedRxiv.org, and Wellcome Open Research).
Results:
Twenty-eight studies met inclusion criteria (
Conclusion:
Implementation of multiple non-pharmaceutical interventions at key decision points for public health could effectively facilitate disease mitigation and suppression until pharmaceutical interventions become available. Dynamics around
Keywords
Introduction
In the absence of a vaccine, mitigation of the coronavirus disease 2019 (COVID-19) pandemic requires non-pharmaceutical interventions (NPIs), such as social distancing, increased hand hygiene, mask wearing, and surface decontamination, which have been implemented across the globe. 1
However, the effectiveness of NPIs is difficult to measure, especially for a rapidly evolving disease like COVID-19. To help understand the implications of using NPIs, singly or in combination with other NPIs or pharmaceutical interventions (PIs), epidemiologists are relying on evidence from retrospective studies of past outbreaks to manage the current COVID-19 pandemic. With emerging but limited current evidence around COVID-19, the effectiveness of NPIs to mitigate and control other viral diseases from retrospective studies may offer valuable information to improve pandemic preparedness and response.
Social distancing NPIs have historically decreased the spread of viral infectious diseases. These interventions lower the likelihood that a healthy individual will come in contact with an infected person, help limit disease spread, and promote suppression of new cases, such as in the 1918 influenza A pandemic,2,3 epidemics related to coronavirus (e.g. 2003 severe acute respiratory syndrome coronavirus (SARS-CoV)), 4 and various others. Studies have been recently conducted to show the observed impact of NPIs on a variety of pathogens, including influenza and norovirus, during the COVID-19 pandemic.5,6
The objective of this study is to identify and synthesize evidence regarding the effectiveness of social distancing NPIs on respiratory infectious viral disease outcomes. This rapid evidence-based review and meta-analysis focuses on studies describing the implementation and assessment of social distancing-related NPIs, including general distancing strategies, quarantine, and/or isolation using single or multiple interventions during respiratory viral epidemics or pandemics. The knowledge gained from this review could help public health policy makers, clinicians, researchers, and so on to strategically plan and implement these interventions in order to limit the spread and mitigation of COVID-19 or other future respiratory viral pandemics.
Methods
Study design
A rapid evidence-based review7,8 was conducted to identify studies examining the effectiveness of single or multiple social distancing NPIs on infectious viral disease (pandemic or epidemic) outcomes (e.g. incidence, transmission, and mortality) with comparisons to examine the effects of the intervention, its timing, and/or combination(s) of interventions. Included studies with the following social distancing NPIs were clustered into three main groups: (1) General: voluntary or mandatory steps taken to reduce face-to-face interactions among people in the community; (2) Quarantine: imposed separation or restriction of movement of persons who are exposed, who may or may not be infected but are not ill, and may become infectious to others; and (3) Isolation: the separation and confinement of individuals known or suspected to be infectious or ill with a contagious disease in order to prevent them from transmitting the disease to others. Primary or secondary studies published in English, conducted in humans, and with an abstract, were considered. Supplementary Tables I and II present the study methodology details.
Search strategy
A search of published literature in MEDLINE via PubMed, Google Scholar, and pre-print databases (BioRxiv.org, MedRxiv.org, and Wellcome Open Research) was conducted to identify references published or available online through 27 March 2020 (Supplementary Table I). The search strategy queried the terms (‘non pharmaceutical intervention*’ or ‘non-pharmaceutical intervention*’) or (‘social distancing’) in titles.
Screening, data extraction, qualitative synthesis, and quality assessment
Two-reviewer screening of both titles/abstracts and full-texts was performed independently against a priori inclusion criteria (Supplementary Table II), and conflicts were resolved with adjudication by a third reviewer. Inter-rater reliability (IRR) was determined by the kappa statistic. 9 Results were tracked in Microsoft Excel and EndNote®. Data were abstracted into standardized forms for synthesis and thematic analysis. Systematic reviews with the same inclusion criteria were included and evidence was abstracted from the primary study for qualitative synthesis. Study quality was assessed by dual review using the Oxford levels of evidence (Table 1). 10
Summary of study characteristics.

NA: not applicable.
Adapted from Oxford Levels of Evidence: 10 Level 2a, systematic review with homogeneity of 2b or better studies; modeling studies were considered similar to economic and decision analysis study types; Level 2b, analysis based on clinically sensible costs or alternatives; limited review(s) of the evidence, or single studies, and including multi-way sensitivity analyses; Level 3b, analysis based on limited alternatives or costs, poor-quality estimates of data, but including sensitivity analyses incorporating clinically sensible variations; Level 4, case-series.
Funding source considerations: academia includes both government and private institutions; government; industry; and research councils include both for-profit and not-for-profit.
Meta-analysis
Meta-analyses were performed using a random-effects DerSimonian–Laird model
35
for proportions, using the inverse variance method with logit transformation to yield a pooled estimate and 95% confidence intervals (CIs) for attack rates. Separate analyses were conducted for ‘no intervention’, ‘single intervention’, and ‘multiple interventions’. Between study heterogeneity was assessed using the τ
2
statistic. Statistical heterogeneity was also assessed using the
Results
Literature searches identified 399 unique records from 434 references retrieved. Forty-three full-texts were reviewed (IRR = 89%), and 28 studies met inclusion criteria (Figure 1).
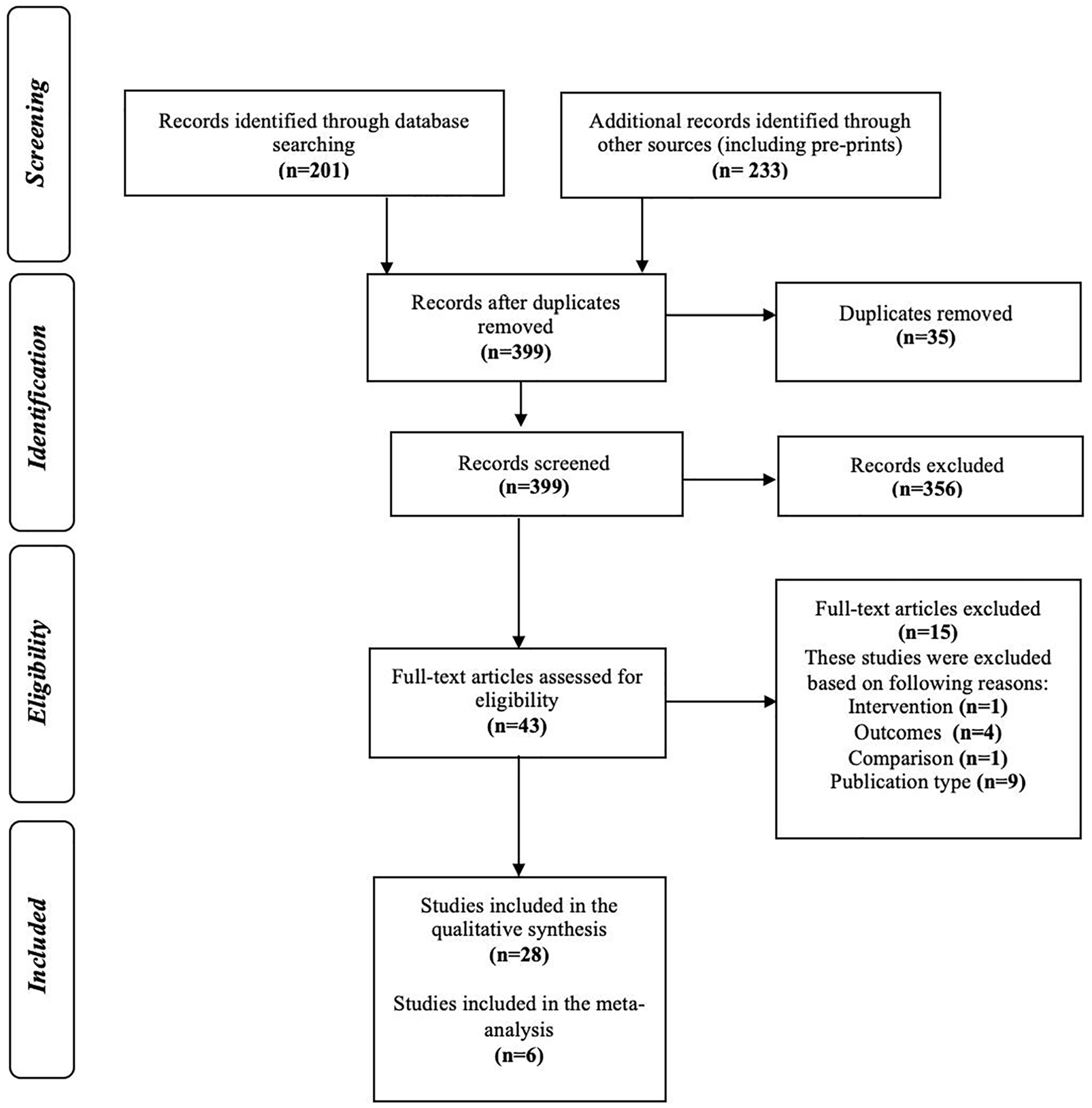
Study selection process.
Study characteristics
Study characteristic are provided in Table 1. The following results are reported as number of studies (
Summary of outcome-based evidence from social distancing non-pharmaceutical interventions identified.

COVID-19: coronavirus disease 2019;
Details provided in abstraction Supplementary Table III.
Multiple subtypes of social distancing NPIs were used in studies.
Substantial heterogeneity was noted in outcome measures employed to report each outcome, that is, disease incidence (e.g. infection rate or incident rate, incidence proportion or attack rate); disease transmission (e.g.
General social distancing (i.e. reduced interactions between potentially infectious individuals—but not diagnosed—in a broader community).
Quarantine (i.e. involves the restriction of movement of presumably infectious individuals as they may have been exposed to disease).
Isolation (i.e. separation of diagnosed individuals).
Included suspected and undiagnosed cases.
Types of interventions and outcomes
Social distancing NPIs of interest included general social distancing (referred to as general), quarantine, and isolation (for intervention definition, see Supplementary Table III; Figure 2).

Study intervention hierarchy for data analysis. This graphic visualizes the study details regarding data collection concerning interventions to mitigate or control viral pandemics or epidemics. Single (non-pharmaceutical interventions (NPIs) or pharmaceutical interventions (PIs)) interventions and/or multiple interventions with combinations of exclusive social distancing NPIs, social distancing NPIs plus other NPIs, social distancing NPIs plus PIs, and/or social distancing NPIs plus other NPIs and PIs.
Social distancing NPIs were used as a single intervention (19, 68%)1,3,11–13,16–22,24–26,31–34 and/or multiple interventions (24, 86%)1–4,12–18,20–22,24,26–34 with other NPIs and/or PIs including antiviral treatment and prophylaxis, and/or vaccination. Infectious viral disease outcomes were limited to disease incidence, transmission, and mortality (Figure 3, Supplementary Tables III and IV).

Summary of outcomes by study with respect to basic reproduction number (
Thematic analysis stratified results related to the effectiveness of general, isolation, and quarantine social distancing NPIs (Table 2). General social distancing was most frequently observed (27, 96%),1–4,11–21,23–34 with school closures identified as a common subtype (20, 71%).1–4,11–15,17–21,23–33 Other types of general social distancing identified included non-specific (7, 25%),1,13,17,26,27,30,33 avoidance of contact, crowding, or mass gatherings (7, 25%),1,4,18,20,31–33 workplace policies to limit contact (12, 43%),4,17,18,20,23,26–30,32,33 and travel restrictions (3, 11%).13,15,18 Isolation and quarantine were similarly identified (both: 16, 57%).1–4,13–20,22,26,28–31,33,34 Case isolation was identified in 13 studies (13, 46%)2,4,14–16,19,20,22,29–31,34 but only two studies (2, 7%) described hospitalization.15,18 Household quarantine (11, 39%)2,3,4,13,18,20,28–31,34 was most common, with fewer studies examining other quarantine conditions, including border control (2, 7%),18,15 geographic region by city or zone (1, 4%), 17 onboard (e.g. airline or ship) (1, 4%), 18 and voluntary self-protection (3, 11%).1,16,18
If
School closure predicted age-specific reductions in percent cumulative attack rate comparing school-age children (21%–22%) to adults >53 years (40%) and adults <53 years (12%) by child-to-child community and household transmission. 25 Early implementation of school closure or generalized social distancing may result in better mitigation than the very early implementation of public travel restrictions.13,18
General social distancing plus quarantine and isolation NPIs substantially decreased
15
or predicted decrease30,34 of COVID-19
Timing and duration of school holidays played a critical role in limiting COVID-19 and influenza transmission rates in observational and modeling studies.11,15 Combinations of these general social distancing NPIs (e.g. changes in population behavior to limit public contact) with quarantine and isolation had a greater effect on decreasing COVID-19 transmissibility when the intervention duration was extended beyond holiday-related school closures (holiday only, 14% – 15%; extension beyond holiday, 33% – 44%). 15 A detailed summary of data abstraction for included studies is provided in Supplementary Table III.
Effectiveness summarization
All studies (28, 100%) reported some degree of effectiveness for each social distancing NPI examined across mild-to-moderate (
Disease incidence including meta-analysis on attack rate
Disease incidence was examined in 16 studies (57%)1–4,12,13,17–19,25–29,32,33 with primarily percent attack rate, and secondarily, infection rate reported (Figure 3 and Supple-mentary Table III) and had mixed results when comparing the effectiveness of single versus combined NPIs.
Combining social distancing NPIs may be more effective in decreasing attack rate than single NPIs, in both COVID-19 and non-COVID-19 settings.1,3,13,26,32 As shown in the modeling studies, timeliness of and compliance with multiple interventions and the
Modeling studies examining single social distancing NPIs’ effectiveness suggest wide variation in general viral attack rate change (range = 0% – 99%), and greater effects on influenza when the frequency of new cases remains low. 13 Simulation of influenza outbreaks revealed school closure was a common single NPI and may substantially lower attack rate (typically 20% – 60%), 25 but had the highest impact when implemented in combination NPIs, 1 especially early in pandemics 25 and when continued for adequate duration. 27 The remaining general social distancing subtypes of mass gathering prohibitions, contact avoidance, and workplace policies to limit contact had similar effectiveness with a moderate (<20% decrease) effect on COVID-19 attack rate; 1 however, when used in combination NPIs, the impact was larger (>20% decrease). 1 Case isolation may be less effective than other single general social distancing NPIs on influenza attack rate, but changes in attack rate could improve with early implementation (3 weeks, −25.3%; 8 weeks, −8.3%). 18
A meta-analysis was conducted on six studies3,12,13,19,26,27 that reported influenza attack rates and the population at-risk for both no intervention and social distancing NPIs as a proxy (Supplementary material, Figures I and II). Some studies provided attack rate estimates assuming different model parameters (e.g.
Disease transmission
Disease transmission was examined in 15 (54%) studies3,11,15–18,20–25,30,33,34 as percent or effective decrease in
Generally, combinations of social distancing NPIs predicted18,24 or changed18,20 viral transmissibility in both COVID-19 and non-COVID-19 settings (range = −14% to −54%),18,15,24 but compliance affected their success. One modeling study noted that there was greater than 90% probability of obtaining 0% influenza transmission rates with a combination of general social distancing NPIs; 90% achievement with socially targeted antiviral treatment and prophylaxis and 80% with reduced movement in affected zones following geographic targeting of quarantine interventions.
17
Isolation15,17,18,22,30,34 and quarantine16,18,30 are both effective in limiting influenza and COVID-19 disease transmission when used in combination NPIs. Modeling of isolation combined with contact tracing decreased COVID-19 transmission (pre-intervention
Intervention timing influenced NPI effectiveness on limiting transmission. Early and short-term (e.g. 3 months) general social distancing NPIs could delay the timing of peak infections by as much as 7 months, but would have a modest impact on COVID-19 transmission.
33
Modeling effectiveness of workplace policies improved with increasing
Mortality
Mortality was examined in 10 studies (36%)1,3,14,18,20,21,25,28,31,34 as were case fatality proportion, mortality rate, peak excess death rate, and total deaths (i.e. all-cause mortality) (Figure 3). Single and multiple social distancing NPI modeling had large variability on influenza-related mortality rate (ranges of single: range = 3% – 78%; multiple = 6% – 97%).
31
A COVID-19 modeling study determined mortality could be further decreased by 34%–49% by adding age-dependent (>70 years) general social distancing interventions to quarantine and isolation.
1
However, general social distancing NPIs plus PIs could further lessen mortality in predictive models; using general social distancing NPIs, influenza-related mortality could be decreased by 93%, but by providing antiviral prophylaxis and treatment (e.g. adamantanes and neuraminidase inhibitors) to 2% of the affected region, mortality could be decreased by 97%.
3
The number of general social distancing NPIs was associated with lower peak excess influenza death rates (0.002 >
Temporal relationships with mortality were similarly identified whereby duration and timing impacted the effectiveness of social distancing NPIs. Influenza-related mortality could be further decreased by extending intervention durations;14,31 one modeling study noted that a substantial decrease in mortality could be obtained by extending a combination of NPIs (e.g. general social distancing, handwashing, mask wearing, and case isolation) by 5 months (no extension, 6% – 43%; with extension, 38% – 92%).
14
Quarantine by controlling movement within infected geographies with lower
Study quality
Using Oxford levels of evidence, 10 two (7%) studies provided Level 2a evidence;18,25 22 (79%) studies were assessed as Level 2b;1–4,11–17,19,21–24,26–29,32,33 three (7%) were Level 3b;30,31,34 and one (4%) 20 provided Level 4 evidence. The quality of the evidence is moderate as the majority of studies were Level 2 quality (descriptions in Table 1 and Figure 3).
Discussion
NPIs are important public health measures, implemented either as a single measure or in combination with other NPIs, to help decrease incidence, transmission, and mortality of viral and other infectious diseases. Early, sustained, and combined application of various NPIs could mitigate and control primary outbreaks and prevent more severe secondary or tertiary outbreaks,20,24,34 provided decision-makers consider dynamic
Retrospective observational and modeling studies suggest the effectiveness of social distancing NPIs depends on disease severity as well as intervention timing and adherence (e.g. implementation delays, duration, and population compliance/coverage). Thus, an outbreak could be effectively suppressed through strict and early implementation of an intervention (single or in combination) for a pre-determined duration. The more widespread the infectious disease and/or the longer the delay in implementation of a measure, the more limited the effectiveness of the intervention.3,12,17,18,26,33
Effective mitigation requires combined social distancing interventions (e.g. school closure, quarantine, or isolation), supplemented by other NPIs (e.g. mask wearing and handwashing) and PIs (e.g. antiviral treatment and/or vaccinations). Several studies suggested that multiple interventions are more effective than a single intervention.1,16,18,29,30 Timely and continuous but evolving adoption of evidence-based social distancing strategies could substantially mitigate and control the pandemic until an efficacious treatment and or/matched vaccine become available.28,33
The majority of included studies implemented modeling to predict the effects of social distancing NPIs on viral disease outbreaks. Further work is needed to model case fatality rates, mortality, and costs, and to predict disease transmission, effects of differing vaccination rates, and case severity and their correlation with NPIs.
Public health implications
This study provides both qualitative and quantitative evidence related to the implications of using NPIs to contain infectious diseases, mostly from past studies, supported by current experiences. Public health policy makers, educators, clinicians, and researchers could better understand the factors that could facilitate more favorable outcomes resulting from implementations of NPIs. These include matching the right intervention type to specific community circumstances such as the stage of the curve or type of venue (school closures, mass gathering cancelations, contact tracing, etc.) and/or strategizing implementation time, duration, and intensity (early, prolonged and strict lock down, prioritization of protecting the high-risk patient population first, for example, elderly having other comorbidities).
Strengths and limitations
To our knowledge, this is a novel review employing a rapid methodology to provide both qualitative and quantitative synthesis of the evidence related to the effects of social distancing NPIs on respiratory viral disease outcomes including incidence, transmission, and mortality. Our results should be interpreted in the context of the limitations of this study. Studies with a search cutoff of 27 March 2020 were limited from online searches of MEDLINE, Google Scholar, and pre-print databases. In addition, more relevant studies may be identified from other databases and those published after the search cutoff date. Handsearching of included studies or conference proceedings was not performed. In addition, articles were limited to English language with an abstract. Meta-analyses were limited to influenza attack rate and results had high statistical heterogeneity. These quantitative findings conflict with the narrative results relating to the effectiveness of single versus combined NPIs on disease incidence. Potential explanations could be the high study heterogeneity (i.e. different models, varying parameters for the models, variable
Conclusion
This review provides evidence that a proper deployment of strategically combined social distancing NPIs as a public health measure, along with other non-pharmaceutical and PIs, could mitigate and control disease by decreasing viral disease incidence, transmission, and mortality.
Supplemental Material
sj-doc-1-smo-10.1177_20503121211022973 – Supplemental material for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis
Supplemental material, sj-doc-1-smo-10.1177_20503121211022973 for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis by Rubina F Rizvi, Kelly J Thomas Craig, Rezzan Hekmat, Fredy Reyes, Brett South, Bedda Rosario, William J Kassler and Gretchen P Jackson in SAGE Open Medicine
Supplemental Material
sj-docx-2-smo-10.1177_20503121211022973 – Supplemental material for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis
Supplemental material, sj-docx-2-smo-10.1177_20503121211022973 for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis by Rubina F Rizvi, Kelly J Thomas Craig, Rezzan Hekmat, Fredy Reyes, Brett South, Bedda Rosario, William J Kassler and Gretchen P Jackson in SAGE Open Medicine
Supplemental Material
sj-tiff-3-smo-10.1177_20503121211022973 – Supplemental material for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis
Supplemental material, sj-tiff-3-smo-10.1177_20503121211022973 for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis by Rubina F Rizvi, Kelly J Thomas Craig, Rezzan Hekmat, Fredy Reyes, Brett South, Bedda Rosario, William J Kassler and Gretchen P Jackson in SAGE Open Medicine
Supplemental Material
sj-tiff-4-smo-10.1177_20503121211022973 – Supplemental material for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis
Supplemental material, sj-tiff-4-smo-10.1177_20503121211022973 for Effectiveness of non-pharmaceutical interventions related to social distancing on respiratory viral infectious disease outcomes: A rapid evidence-based review and meta-analysis by Rubina F Rizvi, Kelly J Thomas Craig, Rezzan Hekmat, Fredy Reyes, Brett South, Bedda Rosario, William J Kassler and Gretchen P Jackson in SAGE Open Medicine
Footnotes
Acknowledgements
The authors thank Winnie Felix and Courtney VanHouten for helping with searching for relevant papers, and Dr Van C. Willis for his critical reading and support for the completion of the revisions.
Availability of data and materials
All supporting data has been provided in additional files.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research study was supported by IBM® Watson Health® (no grant number to disclose).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
