Abstract
Background
Despite an increasingly biopsychosocial approach to pain management in healthcare, limited research exists on psychological features in dentistry including endodontic-related pain. This study aimed to identify the scope of evidence on the relationship of psychological variables to pain associated with dentistry specifically endodontics, as a first step towards addressing them for treatment.
Methods
This scoping review was conducted according to the JBI Manual for Evidence Synthesis. Literature searches were performed in MEDLINE, EMBASE, PsycINFO, Web of Science, Scopus, Cochrane, and CINAHL, alongside grey literature sources, including ProQuest, ClinicalTrials.gov, and conference materials, reference lists, medRxiv pre-prints, EBSCO theses, and data from clinical trial registers such as ClinicalTrials.gov and Cochrane trials (via Ovid) (from inception to February 2025). Two independent reviewers screened records, and data extraction was cross-verified. The protocol was registered on Open Science Framework (DOI: 10.17605/OSF.IO/FSRJP).
Results
Forty eight studies were included. Twelve broad psychological constructs were evaluated in relation to pre, during, and post-endodontic pain: pain expectancies, positive treatment expectancies, depression, anxiety, positive and negative mood (affect), beliefs about pain, desire for control of dental treatments, perceptions of dentists, somatic focus or awareness, pain coping strategies, personality, and psychiatric diagnoses. Pre-procedural pain was most frequently linked to anxiety. Procedural and post-procedural pain was consistently associated with anxiety, pain expectations, depression, and pain beliefs.
Conclusion
A variety of psychological factors have been investigated in relation to endodontic pain at different time-frames. Whilst associations between endodontic pain and psychological constructs were found, further research is needed to evaluate the strength of these associations, and the scope of evidence for interventions designed to address these psychological contributors to pain in dental practice. Identifying psychological contributors to endodontic pain can enhance pain prediction, patient communication, and clinical care strategies.
Introduction
Effective pain management is crucial in clinical endodontics, 1 as research consistently links pain during dental procedures, including endodontics, to complications, persisting pain, and flare-ups.2–4 Current guidelines for dental pain management focus primarily on pharmacological approaches 5 : Non-steroidal anti-inflammatory drugs (NSAIDs) are recommended in combination with paracetamol as first-line treatments,5–7 and opioids like codeine and oxycodone as second-line treatments.5–7 Report of 5 to 49% of pain at different stages of endodontic procedures2,8 suggests that there is a need to improve our approach to pain management in dentistry. 4
The fear-avoidance and cognitive-affective models of pain provide a conceptual framework for understanding how psychological constructs such as anxiety, depression, expectations, and feelings of helplessness shape the experience of endodontic pain. The fear-avoidance model suggests that these fear-related psychological constructs amplify pain by creating hypervigilance to threat and promoting avoidance behaviours. 9 Also, the cognitive-affective model of pain suggests that beliefs about pain and anxiety could modulate pain experience because negative appraisals (e.g. expectation of uncontrollability) heighten attention to pain, increase threat perception, and activate emotional distress, which in turn intensify central nociceptive processing. 10 Both these models support biopsychosocial approaches to pain management. Also medical literature provides substantial evidence that psychological factors such as preoperative anxiety, depression, and pain catastrophizing are associated with both greater acute procedural and post-operative pain and longer term chronic postsurgical pain.11–13
Recognizing pain as a biopsychosocial phenomenon is an important first step towards improving pain management in dentistry. 14 A large body of research demonstrates the modulation of pain by a range of psychological factors.15–17 However, knowledge of psychological to endodontic pain remains limited. 18 A systematic review found that psychological factors (e.g. Catastrophizing, beliefs, coping, and mood) are strong predictors in the transition from acute to chronic pain across many medical conditions. 19
This paper focuses on the psychological aspects of pain and aims to address this gap in endodontics by using a systematic scoping review methodology to describe available research on psychological variables in endodontic-related pain. Specifically, the objectives of this review were to investigate psychological variables related to periprocedural (pre-procedural, procedural, and post-procedural) endodontic pain.
This initiative seeks to enhance the understanding of the psychological aspects in endodontic pain to guide pain management practices in this specialized field and assess the research body’s sufficiency for a potential systematic review and meta-analysis. Due to concerns about feasibility, the current review excludes an examination of social contributors to pain.
Materials and methods
To uphold rigorous standards, our scoping review adhered to the Joanna Briggs Institute (JBI) Reviewer’s Manual 20 and PRISMA Extension for Scoping Reviews (PRISMA-ScR) reporting guidelines. 21 The research protocol was registered on Open Science Framework (DOI number: 10.17605/OSF.IO/FSRJP). The focus was on exploring the link between psychological factors and pain measures in English-language studies.
Eligibility criteria, population, concepts, and context
The inclusion criteria encompassed studies involving patients undergoing endodontic procedures, including various study designs such as cohort, case-control, cross-sectional, clinical trials (interventional, observational), systematic reviews, and meta-analyses, with an evaluation of at least one psychological factor before, during, or after the endodontic procedure. Pain assessment for pre-procedural, procedural, or post-procedural, and reporting of the association between psychological factors and pain, was also required. Only studies published in English were considered. Exclusion criteria included case reports, case series, animal studies, letters, comments, editorials, and non-systematic reviews.
Search strategy
The relevant keywords were selected by reviewing relevant articles and in consultation with a librarian. We conducted a pilot search on a random sample of 50 records retrieved from PubMed, and achieved 80% agreement in screening. 20 The search strategy was then refined based on discrepancies identified during team discussions with experts in the field (Appendix 1).
We performed a search of multiple databases, including MEDLINE (via PubMed), EMBASE (via Ovid), PsycINFO (via Ovid), Web of Science (all databases), Scopus, Cochrane Database of Systematic Reviews (via Ovid), and CINAHL (via EBSCOhost). For the Grey Literature, we searched reference lists of the included studies as well as pre-prints available on medRxiv, theses via ProQuest Dissertations and Theses/EBSCO Open Dissertations, clinical trial registers such as ClinicalTrials.gov and the Cochrane Central Register of Controlled Trials (via Ovid), and conference materials including abstracts and proceedings via the Conference Proceedings Citation Index (via Web of Science) and Scopus (from inception to February 2025). To ensure the final search strategy adhered to the recommended guidelines, we employed the Peer Review of Electronic Search Strategies (PRESS) Checklist. 21
Study selection
We used EndNote and Covidence Systematic Review software 22 for duplicate removal and screening. Literature selection followed predetermined eligibility criteria through a two-pass screening of titles, abstracts, and full texts, resolving disagreements through consensus by two-reviewer or third-reviewer intervention.
Data extraction
There was no methodological quality or bias evaluation of studies included, in line with JBI 20 guidelines for scoping reviews. A single reviewer extracted the data, with a second reviewer cross-verifying data in a random sample. Key information was recorded in a charting table for a descriptive summary aligned with the aims and objectives of the review.
Results
The screened search ended with 48 articles for the final data extraction (Figure 1). Flow chart of the studies selection process and screening.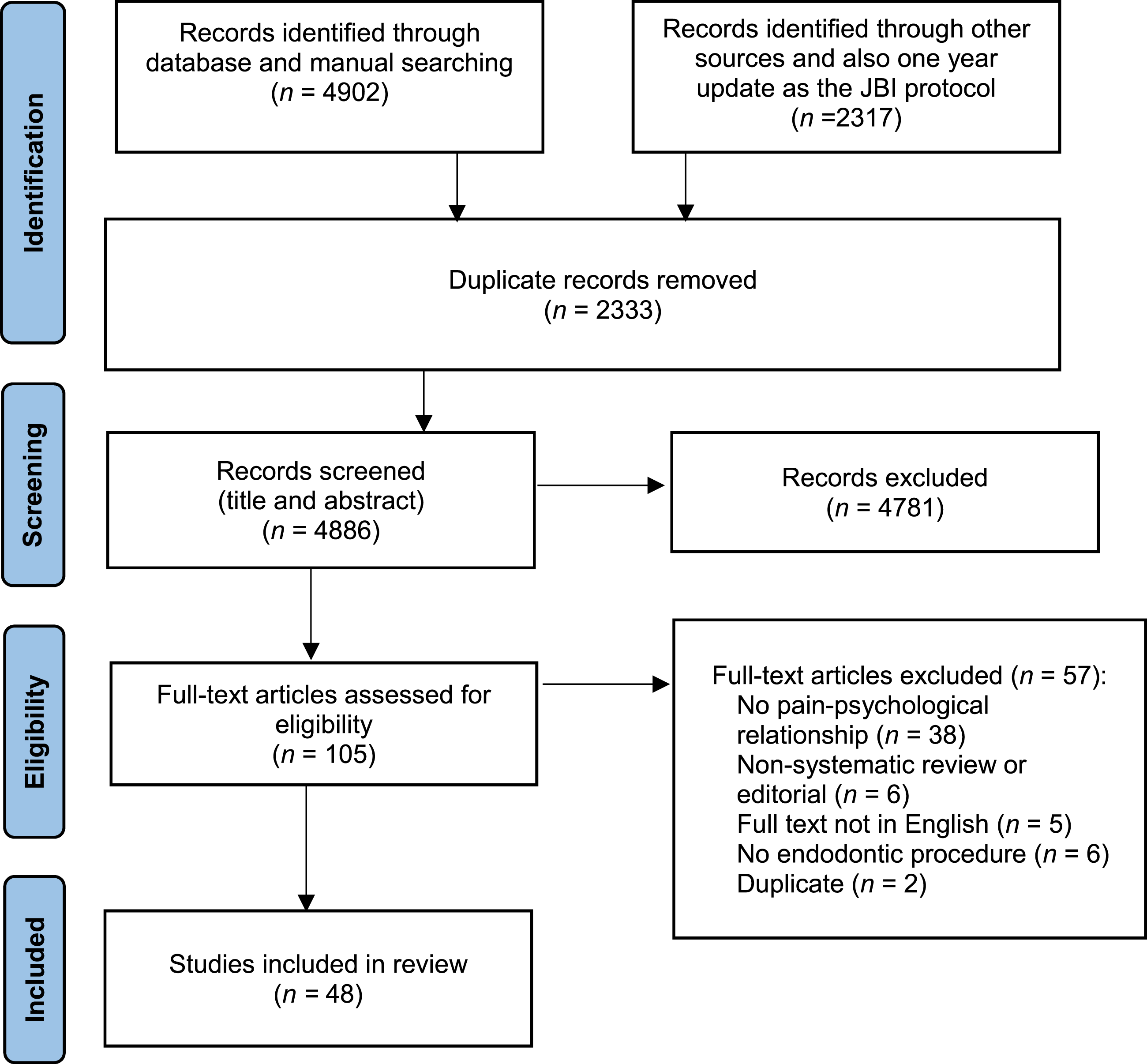
Characteristics of the selected studies
The majority of the studies, comprising over two-thirds, are observational studies, predominantly prospective, with four retrospective studies and four cross-sectional studies, supplemented by four clinical trials. Fourteen studies 14 were from North America (the United States and Canada), with 17 conducted in Europe (United Kingdom, Germany, France, Spain, Croatia, The Netherlands, Sweden, and Denmark), 9 conducted in Asia (Australia, China, India, Japan, Korea, Singapore, Taiwan), 4 conducted in the Middle East (Saudi Arabia, Israel, Iran), and 4 across multiple continents.
Study participants
Studies included sample sizes ranging from 30 to 300 patients for observational studies and 1500 to 4800 for national surveys. Participant ages ranged from 6 to 86 years (mostly adults). Samples were 55% female on average, with 80% of patient cohorts coming from university educational dental clinics/hospitals and the remaining 20% from private surgeries.
Pain measurement
Various self-reporting scales measured pain at different stages of the endodontic procedure (pre-procedural, procedural, and post-procedural). Pain intensity, frequently assessed by the Visual Analog Scale,
23
was the most common outcome measured, as shown in Figure 2. Details of scales used for pain measurement based on numbers.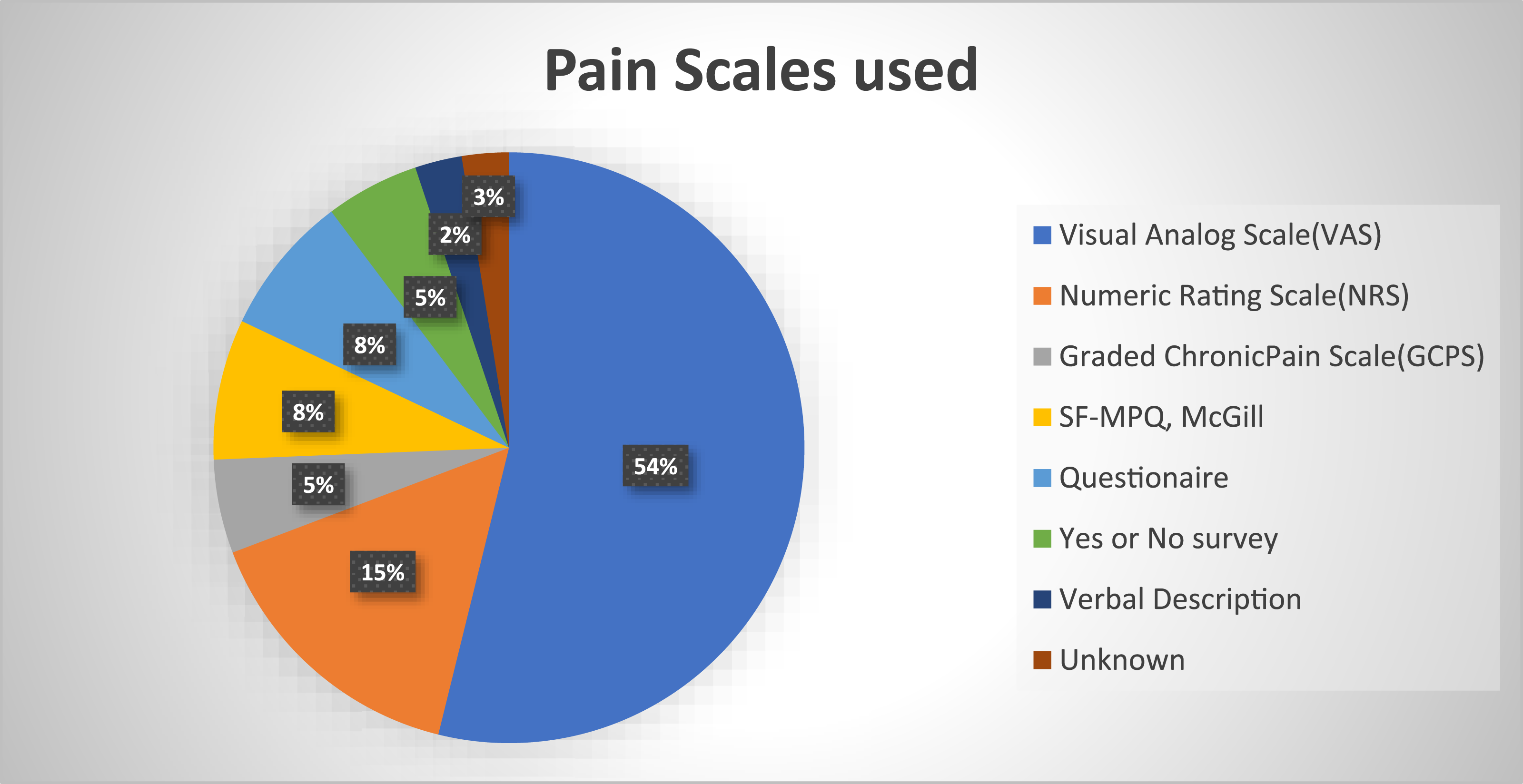
Psychological constructs
Details of data extraction.
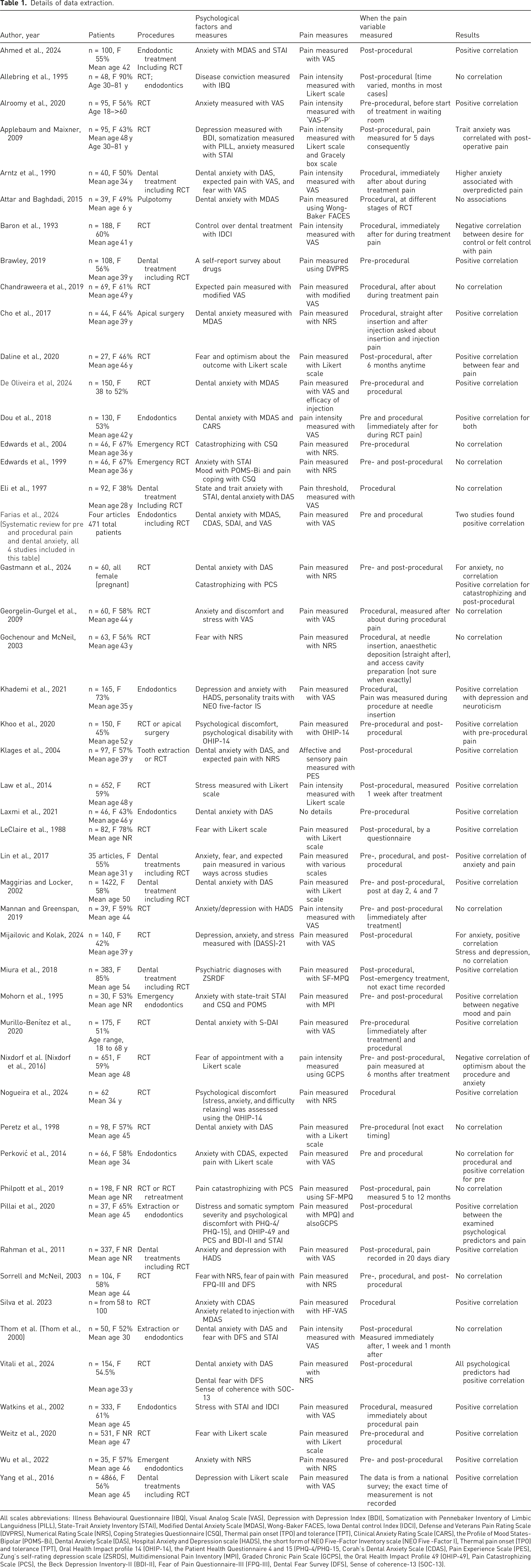
All scales abbreviations: Illness Behavioural Questionnaire (IBQ), Visual Analog Scale (VAS), Depression with Depression Index (BDI), Somatization with Pennebaker Inventory of Limbic Languidness (PILL), State-Trait Anxiety Inventory (STAI), Modified Dental Anxiety Scale (MDAS), Wong-Baker FACES, Iowa Dental control Index (IDCI), Defense and Veterans Pain Rating Scale (DVPRS), Numerical Rating Scale (NRS), Coping Strategies Questionnaire (CSQ), Thermal pain onset (TPO) and tolerance (TPT), Clinical Anxiety Rating Scale (CARS), the Profile of Mood States-Bipolar (POMS-Bi), Dental Anxiety Scale (DAS), Hospital Anxiety and Depression scale (HADS), the short form of NEO Five-Factor Inventory scale (NEO Five -Factor I), Thermal pain onset (TPO) and tolerance (TPT), Oral Health Impact profile 14 (OHIP-14), the Patient Health Questionnaire 4 and 15 (PHQ-4/PHQ-15, Corah’s Dental Anxiety Scale (CDAS), Pain Experience Scale (PES), Zung’s self-rating depression scale (ZSRDS), Multidimensional Pain Inventory (MPI), Graded Chronic Pain Scale (GCPS), the Oral Health Impact Profile 49 (OHIP-49), Pain Catastrophizing Scale (PCS), the Beck Depression Inventory-II (BDI-II), Fear of Pain Questionnaire-III (FPQ-III), Dental Fear Survey (DFS), Sense of coherence-13 (SOC-13).
Summarized comparison of psychological constructs found associated with pre-procedural, procedural, and post-procedural pain.
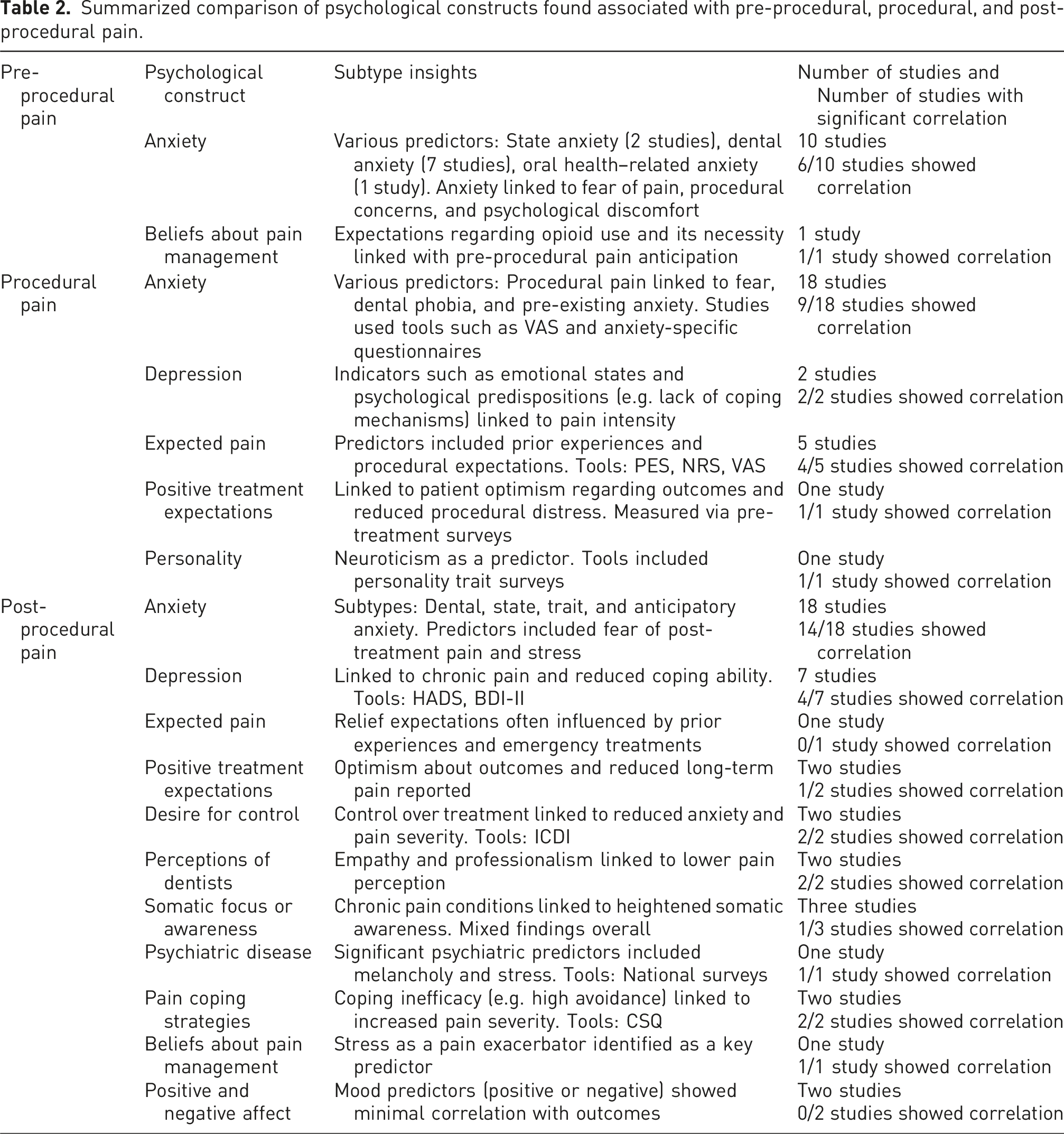
Psychological constructs associated with pre-procedural pain
Two psychological constructs – anxiety and beliefs about pain – were investigated in association with pre-procedural pain.24–31
Anxiety
Ten studies investigated various forms of anxiety in relation to pre-procedural pain. State anxiety was measured in two studies,24,31 while dental anxiety was measured in seven studies,27–30,32,33 and one study 26 measured oral health–related anxiety. Six of the 10 studies reported a correlation between some form of anxiety and pre-procedural pain of endodontics.24,26–28,31
Beliefs about pain management
One study 25 measured patient perceptions of pain relief and expectations of receiving an opioid medication together with pre-procedural pain. The study reported a positive relationship between the expectation of receiving an opioid medication and pre-procedural pain.
Psychological constructs associated with procedural pain
Numerous studies investigated the association between psychological variables and procedural pain, with 20 studies identified in this review.18,28,30,34–50 The five psychological constructs investigated for procedural pain were anxiety, depression, expected pain, positive treatment expectations, and personality.
Anxiety
Eighteen studies investigated the association between various forms of anxiety and procedural pain18,28,30,34–44,46,48–50 with mixed results. Of these, 9 out of 18 studies reported a significant positive association between anxiety and procedural pain.
Depression
Two studies42,45 reported a positive correlation between depression and procedural pain.
Expected pain
Expected pain was evaluated in relation to procedural pain of endodontic treatment in five studies.36,39,43,46,47 Expected pain was measured using various tools including visual analog scales (VAS), numerical rating scales (NRS), and the Pain Expectation Scale (PES). Four of these studies36,39,43,47 showed a positive association between pain expectation and procedural pain.
Positive treatment expectations
Weitz et al. 48 was the only study in this category that measured the expected outcome of root canal therapy for procedural pain, reporting a significant association between higher outcome expectancy and anaesthesia failure or procedural pain.
Personality
Personality was investigated by one study, 42 which reported a positive correlation between neuroticism scores and pain experience during needle insertion for injection or procedural pain.
Psychological constructs associated with post-procedural pain
The present review included 24 studies that investigated the relationship between 11 psychological variables and post-procedural pain, including anxiety, depression, ‘expected pain’, ‘positive treatment expectations’, ‘positive and negative effect’, ‘pain coping strategy’, ‘desire for control’, ‘perception of the dentist’, ‘somatic focus and awareness’, ‘psychiatric disease’, and ‘beliefs about pain’.18,30,31,33,51–64
Anxiety
Anxiety was investigated in relation to post-procedural pain in 18 studies,18,26,30,31,33,43,52,53,56–65 with 14 different anxiety measures used. Overall, 14 out of 18 studies reported a significant association between anxiety and post-procedural pain.
Three studies measured state and trait anxiety, one with a pain diary questionnaire and the other with NRS.31,59,61 Nine studies measured dental anxiety, using an 11-point NRS, Graded Chronic Pain Scale (GCPS), or another questionnaire (details below).18,30,43,52,56,65 Four studies measured pain catastrophizing using either the Pain Catastrophizing Scale (PCS) or the Pain Coping Scale (PCS).33,53,57,58 Two studies measured oral health–related anxiety, one with the Oral Health Impact Profile Questionnaire (OHIP-14), measuring psychological discomfort, psychological disability, and social disability, 26 and the other with PHQ-4, PHQ-15, and OHIP-49, measuring discomfort, somatic symptom, and psychological disability. 58 One study measured stress through a questionnaire in a national survey. 60 Both state and trait anxiety were significantly correlated with post-procedural endodontic pain,31,59 with trait anxiety (HADS) identified as a significant predictor of pain in the first 5 days after endodontic treatment. 59 Seven out of nine dental anxiety studies showed a positive correlation between post-procedural pain and anxiety, while two (NRS, GCPS) found no relationship.18,56 One study 30 showed a significant correlation between pain and the Dental Fear Survey-Physiological Score (DFS), but had limitations of low sample size. Except for Pillpott et al., 57 two out of three studies investigating pain catastrophizing reported a significant correlation with post-procedural endodontic pain.
Depression
Seven studies evaluated the relationship between depression and post-procedural pain. Three studies57,63,66 showed no significant relationship between depression and post-procedural pain, and four studies45,58,60 reported a significant association between depression and post-procedural pain. Mannan and Greenspan 45 and Rahman et al., 59 who used the Hospital Anxiety and Depression Scale (HADS) to measure depression, found depression increases post-procedural pain. Pillai et al. 58 and Yang 60 reported higher pain in their depressed groups, measures using the Beck Depression Inventory-II and a questionnaire, respectively, after root canal treatment or in patients with Post-Traumatic Trigeminal Neuralgia (PTTN), a chronic pain condition after dental treatment.
Expected pain
Only one study 31 examined the correlation between expected pain relief and post-procedural pain after emergency endodontic treatment. There was no significant correlations between expected pain and post-procedural pain. 31
Positive treatment expectations
Two studies examined positive treatment expectations in relation to post-procedural pain.31,52 Daline et al. 52 assessed expected outcomes through a questionnaire in patients experiencing chronic pain after root canal therapy and reported no association between long-term persistent pain and patients’ optimism about the treatment outcome measured during the 6 months after treatment. However, Wu et al. 31 evaluated expected pain relief in patients undergoing emergency endodontic treatment and found a positive correlation between expected pain relief and post-procedural pain reduction.
The desire for control over dental treatment
The desire for control over dental treatment was investigated in relation to post-procedural pain in two studies,51,65 both of which reported a significant correlation between this psychological construct and post-procedural pain using the Iowa Dental Control Index (ICDI).
Baron et al. 51 assessed patients’ desire for control and felt control in the dental chair 30–40 min before the start of treatment. Participants were asked about the degree to which they wanted to have control over dental treatment and how much they felt they had control. The high desire for control or felt control was reported to be associated with lower pain and higher sensory focus than emotional focus measured with a questionnaire. In addition, Maggirias and Locker 65 reported that pain was significantly higher in participants with higher scores on the ICDI Felt Control scale than in those who did not report experiencing pain.
Perceptions of dentists
Positive perceptions of the dentist was evaluated in relation to post-procedural pain in two studies46,65 which both reported negative correlations with pain. Maggirias and Locker 65 assessed patients’ perceptions of the dentist and how dental care was delivered during endodontic treatments using a baseline question to assess whether patients had ever had a painful, frightening, or embarrassing experience with a dentist. They found a negative correlation between the high reported empathy of dentists and post-procedural pain onea week after treatment.
Somatic focus or awareness
Three studies reported mixed results regarding the relationship between somatic focus or awareness and post-procedural pain.58,60,61 Pillai et al. 58 measured somatic symptom severity using the Patient Health Questionnaire 15 (PHQ-15) before various dental treatments, including endodontics, and reported that patients with painful post-traumatic trigeminal neuropathy (PTTN), which is a chronic pain condition, had higher scores for somatic symptoms than healthy controls. Conversely, Applebaum and Maixner 61 measured somatization using the Pennebaker Inventory of Limbic Languidness (PILL) completed after root canal treatment (within 5 days after treatment) and found no significant association between post-treatment somatization and post-procedural pain.
Psychiatric disease
One study 60 used a national survey to measure melancholy, consultation with a psychiatrist, and suicidal thoughts before various dental procedures, including root canal therapy, and found significant differences in melancholy, suicidal thoughts, or consultation with a psychiatrist between those with and without self-reported dental pain. 60
Pain coping strategies
Two studies54,55 used the Coping Strategies Questionnaire (CSQ) to measure pain coping before emergency endodontic treatment and post-procedural pain (1-2 weeks after surgery). Both these studies reported that higher scores on CSQ subscales were significantly associated with higher post-procedural pain.54,55
Beliefs about pain management
Beliefs about pain were evaluated in only one study. 67 The study administered a questionnaire to patients before root canal treatment to assess any relationship between the belief that ‘stress makes the pain worse’ and severe post-procedural pain. Patients who reported pain in the previous 7 days were asked if stress made their pain worse (yes or no). The results showed that the belief that pain is made worse by stress was a significant predictor of severe post-procedural pain. 67
Positive and negative affect
The relationship between ‘positive and negative affect’ and post-procedural pain was examined in two studies.54,55 Both studies used the Profile of Mood States (POMS) questionnaire prior to emergency endodontic treatment and reported no significant association between mood and post-procedural pain.
Discussion
Although many studies in dentistry and endodontics focus on psychological constructs, particularly anxiety,68,69 our specific focus was on those studies that evaluated the relationship between psychological factors and endodontic pain. The current review synthesizes the results of 48 studies investigating 12 psychological constructs in relation to pre-procedural, procedural, and post-procedural pain.
Study participants
The majority of studies were conducted in high-income countries, and over 80% of participants were recruited from university educational dental clinics/hospitals and public health centres.
Psychological contributors to pain
Anxiety, with a focus on dental anxiety, emerged as a frequently studied psychological construct, showing a significant association with patients’ pain experiences. Previous research has also indicated a positive correlation between anxiety and pain.47,70,71 However, it is notable that some studies found no correlation between anxiety and pain.31,46
This review also underscores the significance of anticipated pain as an important psychological predictor for procedural and post-procedural pain. Perković et al. 46 investigated the correlation between anxiety and expectations of intraoperative endodontic pain, revealing a positive link between these variables. The relationship between expected and actual pain experiences has also been documented in prior oral surgery studies.72,73 It is important to recognize that what patients expect before treatment can affect their experience, and this holds for different stages of treatment. Additionally, these expectations can be influenced by factors like thoughts and emotions, such as anxiety and the patient’s memory of past experiences. For instance, anticipating pain has been connected to feeling anxious about the treatment,72,73 and remembering the pain felt during past procedures is related to both anxiety and what was expected beforehand.72,74
The majority of presented constructs (11 out of 12) were related to post-procedural pain. Anxiety emerged as the most commonly studied predictor similar to pre-procedural or procedural pain with most studies reporting a positive correlation. This trend aligns with findings from a separate study involving anxiety in other dental procedures, which demonstrated a correlation between state anxiety, anticipated pain, and experienced pain. 70 Furthermore, similar positive correlations have been observed in the context of post-procedural pain in oral surgery. 74
Regarding the importance of depression as a psychological construct, it displays a significant relationship with both procedural and post-procedural pain in most studies. This finding is in concordance with a study in the field of oral surgery but contrasts with observations regarding pain following another oral surgery study and implant procedures maybe due to measurement scale difference.70,75
For the 12 constructs described, the construct of personality received limited attention with only one study 42 addressing it. Khademi’s study, 42 investigating the positive correlation of neurotic personality with post-procedural pain, yielded similar results to an oral surgery study. 70 Consequently, further research in this area is warranted.
For the majority of studies reporting post-operative pain, the exact timing of assessment was either mostly short-term (immediate/within days) with two long-term studies of ∼6 months’ follow-up,52,56 which show psychological variables (anxiety and positive beliefs about treatment) remain relevant in predicting persistent pain. Our result is consistent with a study that showed some young people develop chronic postsurgical pain (>4 months) with distress and expectations as psychological predictors found. 76 This supports our aim that psychological factors contribute across pain phases rather than only in acute settings.
Regarding psychological and pain measurement, inconsistencies in defining and measuring scales were evident in the reviewed studies, which may complicate any future meta-analysis; for example, dental anxiety has been measured with different scales (DAS, MDAS, DFS) without proper justification. A 2025 update on the DAS highlights limited longitudinal validity evidence, limiting the use across time. 77 Another example would be the Mannan and Greenspan study, 45 who utilized the Hospital Anxiety and Depression Scale (HADS) to measure depression, which increased the study’s feasibility, cost, and potential sample size. Regarding the pain scale, a recent oral-medicine review summarizes practical pros/cons of VAS, NRS, VRS, and face scales in dental settings, which can guide more consistent selection. 23 Most studies used single-dimention pain intensity measures, VAS or NRS, which are valid for pain intensity but do not capture affective factors (like mood), which may influence observed anxiety, pain correlations.23,78 Another potential avenue for improvement could involve shifting the focus from measuring individual pain experiences to assessing the ‘relief of pain’ as suggested in some studies.31,74,79 Pain reduction and pain relief represent distinct concepts with different assessment directions. Pain relief is associated with both cortical and descending pain modulation, which supports the notion of an association between pain relief and pain behaviour. 80 Additionally, thoughtful study design, considering multiple time points for pain measurement and consistent assessment protocols, is vital to enhance the accuracy and comprehensibility of research findings. Many of the studies reviewed assessed procedural pain after treatment, yet the exact timing was often unclear. 31 For instance, it was unclear whether the effects of local anaesthesia had dissipated at the time of procedural pain measurement. 48 This practice enhances the comprehensibility of research outcomes and facilitates meaningful comparisons with other investigations.
Our broad inclusion of age groups and treatment types reflects the aim of mapping the scope of available evidence rather than establishing clinical specificity. While this approach may increase heterogeneity, it provides a comprehensive overview and highlights areas where evidence is limited, and future research needed.
Despite the possibility of conducting a systematic review to elucidate the significance of psychological factors, challenges originating from study design heterogeneity and data collection methods must be addressed.
Limitations
Limitations to this study include restricting our search to studies published in English only, and also to psychological and not social factors. We acknowledge that certain constructs, such as perceived empathy, contains social as well as psychological dimensions. We intentionally narrowed the focus to psychological factors in line with our inclusion criteria. This choice does not diminish the importance of social determinants, which need dedicated investigation in future research. The anxiety construct in this review groups together some distinct psychological variables for easier interpretation, which may oversimplify the unique contributions of each individual factor. Also differences in design or treatment protocols may affect associations between psychological factors and pain outcomes. This heterogeneity limits direct comparability; findings therefore should be interpreted with caution.
Future direction
We found some studies working on interventions to address the psychological factors in dental pain, mostly in paediatric patients, with techniques such as distraction employing virtual reality 81 and audio-visual video eyeglasses. 82 While the literature offers limited insight into interventions for anxiety reduction in adult dental settings, certain strategies, including ‘tell-show-do’,68,83,84 hypnosis, 85 auditory distraction through background music, 86 and cognitive therapy, 83 have shown some promise in the field of general dentistry. To advance the development of effective interventions, our next research step should involve a comprehensive review specifically focused on existing interventions relevant to endodontic treatment to reduce anxiety or expected pain as the most common pain contributing factors in research. Understanding the interplay between psychological factors, patient expectations, and technical complexities can contribute significantly to enhancing the patient experience and treatment outcomes in endodontic procedures. Future research should examine other constructs with limited research identified in this review, such as coping strategies, beliefs about pain, personality, and desire for control, to determine whether interventions targeting these factors could complement anxiety-focused approaches.
Clinical Implication
Although this scoping review was not designed to establish causality, it is important to acknowledge the potential bidirectional relationship between anxiety and pain: higher pre-treatment anxiety may heighten pain, while greater pain intensity may in turn reinforce anxiety which needs more investigation in future studies. For endodontic practice, realistic intervention targets include brief chairside strategies such as routine anxiety screening, expectation setting conversations, and offering patients simple control mechanisms (e.g. stop signals) to reduce perceived helplessness.87,88 Evidence from adult dentistry suggest that short interventions like relaxation guidance, targeted reassurance, or cognitive techniques can be integrated into routine workflows with minimal disruption, though their evaluation in endodontics in limited.87,89–92 The feasibility of these interventions may depend on factors such as the limited clinical time available in general practice, as well as the level of training and expertise required for dentists to recognize patient anxiety and deliver appropriate support, so a psychology–dentistry collaboration is required for effective results.
Conclusion
Many different psychological factors have been found that relate to pain of pre-procedural, procedural, and post-procedural endodontics. We have classified these predictors into 12 overarching constructs, among which anxiety and expected pain have emerged as the most commonly studied factors. More research is required to understand the main factors with positive correlations to pain and how to manage these psychological factors to help manage pain better in dentistry.
Supplemental Material
Supplemental Material - Psychological contributors to pain before, during, and after endodontic procedures: A scoping review
Supplemental Material for Psychological contributors to pain before, during, and after endodontic procedures: A scoping review by Atieh Sadr, Ali Gholamrezaei, Amy G. McNeilage, Cameron L. Randall, Flavia P. Kapos, Christopher C. Peck, and Claire E. Ashton-James in British Journal of Pain
Footnotes
Author contributions
AS conceived the presented idea with CAJ, AG, CCP, CLR, and FPK. AS, AG, CLR, FPK, and CAJ prepared the study protocol. Data collection and analysis were done by AS and AGM and subsequently checked and reviewed by AG. AS, AG, and AGM drafted the results. The main draft was written by AS and edited by CAJ, AGM, and AG. All authors read, revised, and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
