Abstract
This study explored the psychological sense-making of people with amputations towards their phantom limb pain. Interviews with eight participants were analysed using interpretative phenomenological analysis. Four themes were developed: (1) ‘Everybody just thinks you’re some kind of freak’: Making personal and social sense of phantom limb pain; (2) ‘If you talk about them, they seem to come’: Perceiving phantom limb pain as an externalised threat; (3) ‘The sooner you accept things, truthfully accept things, then life becomes better’: Achieving acceptance; and (4) The unrecognised role of psychology in managing phantom limb pain. The findings indicate the importance of (1) education and validation for those who experience phantom limb pain, (2) education around the role psychology can have in managing with the pain, and (3) psychological interventions being available and offered to those with phantom limb pain.
Introduction
An estimated 64% of people who have an amputation experience pain in the place of the limb or organ that is missing; referred to as phantom limb pain (PLP). 1 The most posited theory for the occurrence of PLP is that after a limb is amputated, the associated somatosensory brain regions undergo a process of reorganisation with other nearby brain regions. This is theorised to cause sensations, including the experience of pain.2,3 The pain varies in severity, frequency and sensation, and is often described as a stabbing, burning or shooting pain.3–5 The onset is typically within the first week following limb loss, 3 and although the pain can resolve quickly, many people with PLP meet the criteria for chronic pain (defined as pain lasting for more than 3 months).6–8
PLP is associated with a range of psychosocial difficulties.9–12 Grief for the missing limb, 13 loss of independence, 14 and difficulty accepting pain in a limb that is no longer there are commonly reported. 15 Psychosocial factors may also exacerbate the symptoms of pain.16,17 People with pain may experience pain-related fear, which can be exacerbated when individuals have difficulty making sense of why the pain is occurring.18,19 This phenomenon may be more pronounced for individuals with PLP who experience pain in the absence of a limb, a circumstance which may be difficult to make sense of. In one qualitative study, people with back pain experienced shifts in their sense of identity, with their ‘real self’ being replaced by a ‘self with pain’. 20 Individuals with PLP may also experience this, alongside changes to identity as a result of having a physical disability. 21
Effective pharmacological and non-pharmacological treatment options for reducing PLP are limited.22–24 A biopsychosocial MDT approach is standard practice for both the management of individuals receiving an amputation 25 and in pain management services which those with PLP may be referred to.7,26 Psychological approaches for the management of PLP are under researched, and existing studies are limited by small sample sizes and a lack of controlled trials, though provide some evidence for the use of cognitive behavioural therapy (CBT), hypnosis, and Eye Movement Desensitisation and Reprocessing (EMDR) (e.g. 27–33).
Acceptance and Commitment Therapy (ACT) and CBT are recommended for people with pain conditions 7 as cost effective non-invasive alternatives to pharmacological or neuromodulation techniques. 7 Though ACT has not been investigated within the context of PLP, two qualitative studies described participant reports of using acceptance as a method of managing pain.15,34 To date there is only one published case study investigating CBT for PLP 31 which found it to be an effective method of reducing the intensity and frequency of pain experienced. The findings suggest CBT may be a particularly suitable approach when the individual is also experiencing somatic symptoms of pain due to catastrophising and rumination.
Qualitative research has highlighted a decrease in pain, and an increased ability to manage pain, following psychological interventions for PLP. 35 Increased empowerment, improved self-awareness and changes to their perspective of the pain and their control over the impact it has on participants’ lives were reported to contribute to this improvement. Barriers to people with PLP engaging with psychological therapy may include low expectations for improvement in physical difficulties 35 and fear of being viewed as ‘insane’ by health professionals if they describe their experience of PLP. 36 Qualitative research has highlighted the importance of a biopsychosocial approach when delivering non-psychological interventions, such as phantom motor execution. For example, identifying person-centred goals, promoting belief in the intervention, and establishing a good therapeutic alliance were all factors identified as positively influencing participant outcomes.37,38
Further qualitative studies are needed to explore individuals’ psychological experience of coping with PLP, particularly around openness to thinking psychologically about the pain and barriers to this. Only a small number of qualitative studies have been carried out in this area. One explored veterans’ perspectives on PLP, which found a theme suggesting the importance of acceptance and resilience, 34 and another reported adjustment to amputation in which pain featured but was not specific to PLP. 39
The research reviewed above highlights the central role of experiences, beliefs, perceptions and sense-making in determining outcomes for people living with PLP. Therefore, it was important to adopt a methodological approach suited to achieving an understanding of how people with PLP utilise psychological coping strategies in making sense of and managing their pain. Interpretative phenomenological analysis (IPA) 40 is a qualitative approach that is concerned with the lived experiences of participants, and the sense they make of these. Using this approach to data collection and analysis, this study explores: (i) how do people with PLP adjust to the pain and the impact of this; (ii) the use of psychological strategies for making sense of and coping with the pain, and any barriers to this; (iii) how their psychological understanding or approach to the pain has changed over time and what this was in response to; (iv) any potential barriers to engaging with psychological intervention. Recommendations will be made regarding the psychological support that is needed for people with PLP and how psychologists in chronic pain settings can tailor psychological interventions for this group.
Method
Design
This study took a qualitative approach to investigate how individuals interpret and make sense of PLP. Interpretative phenomenological analysis (IPA) was used to collect and analyse data. 40 IPA has been used widely with different health populations, including pain.41,42 This method explores the lived experience (phenomenology) and meaning-making (hermeneutics) of phenomena, most commonly identified in one-to-one, semi-structured interviews, for well-defined, small, homogenous samples. 40
Procedure
The study was approved by the Faculty of Health and Medicine Research Ethics Committee at Lancaster University in 2022. Data collection and analysis occurred from June 2023 to April 2024.
Recruitment and participants
A purposive sampling method was used to recruit people with limb loss who had experienced phantom limb pain. Participants also had to meet the following criteria: (i) aged 18 years or over; (ii) experienced an amputation of a limb at least 8 months prior; and (iii) able to read and speak English. Participants were recruited through limb loss and chronic pain charities. Interested participants contacted the researcher and provided verbal or written consent to participate.
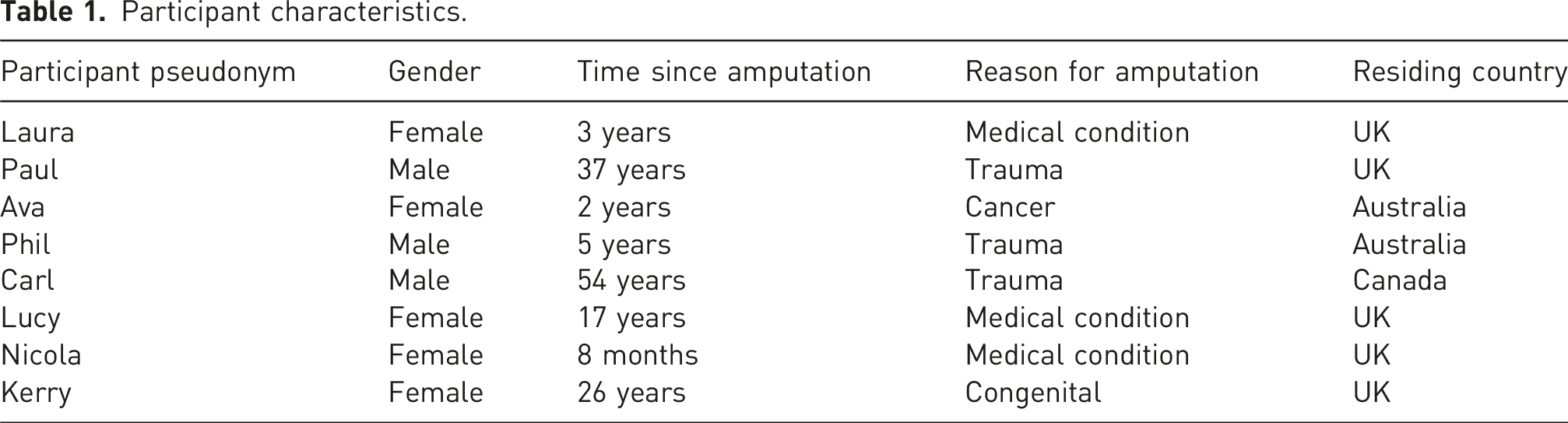
Participant characteristics.
Data collection
All participants took part in video-recorded (via Teams) interviews (over 1–3 sessions) with the first author (mean = 79 min, range 52–220 min).
The interview schedule (Supplemental File) was developed by the research team who had expertise in clinical and health psychology, limb loss, and chronic pain. The interview questions guided participants to explore how they made sense of their pain from a psychological perspective and how this influenced their experience. For example, questions included ‘What did you know about PLP before you started experiencing it’? and ‘How would you feel if you were offered psychological support for managing the pain’? A debrief sheet was provided to participants, listing details of organisations who could be contacted for emotional support or support related to limb loss or pain.
The interviews were recorded using an encrypted device and transcribed verbatim by the first author. The participants were assigned pseudonyms at this stage to maintain anonymity.
Analysis
The analysis process followed the IPA methodology from Smith et al., 40 and followed the auditable steps outlined in Murray and Wilde. 44
The analysis was principally carried out by the first author. The transcripts were read through repeatedly to achieve familiarity with the interview data. They were then coded line by line, focusing on individual experiences and sense-making. In IPA, coding is a process of assigning bespoke summary phrases (rather than codes or phrasing that can be repeatedly applied in the data) to segments of analysed text that encapsulates specific observations that the researcher wants to make in relation to the research questions. The codes were then grouped into clusters through a process of identifying relationships between them. This included the re-occurrence of similarly phrased codes, or codes which provided insight, or elaborated on, differently worded but conceptually related codes. An interpretative narrative summary was written for each theme along with an explanatory title. This process was then repeated for each participant. Themes identified for each transcript were then grouped and synthesised into overarching themes (titles were changed as necessary to encompass the synthesised content) for the whole sample. This was through a process of identifying relationships between participants’ themes, including areas of commonality and divergence. Regular meetings to discuss the analysis process were conducted at all stages of the analysis between the first and fourth authors. These meetings were used to develop and audit the analysis by raising and considering together alternative interpretations, or to extend them, and check the warrantability of these against the data. At the coding stage, this included the fourth author reviewing the coding of the first transcript in full, in addition to selected excerpts from further transcripts. At the identification of themes stage, this included multiple iterations of all individual and group participant theme narratives against supporting data excerpts. At these various stages, refinements in coding, theme content, titling, and data drawn on to evidence the analysis were made by agreement.
Reflexivity
IPA acknowledges the role of the researcher in making sense of what participants communicate. This emphasises the need for the researcher to reflect on their own beliefs, assumptions, and experiences in order to adopt a reflexive position, thereby minimising the influence of these on the analysis. To illustrate engagement with reflexivity during the project, the following reflections are provided by the first author.
During the interview process I was aware that the participants knew my role as a trainee clinical psychologist, and that this may have influenced how they answered questions if they felt I had beliefs and views about the role psychology should have in managing the condition. To try and overcome this I explained my stance as a researcher in this process at the start of the interviews. At times when participants expressed views which may contradict those ‘of a psychologist’, I was careful in how I worded follow up questions. For example, there were times when participants expressed views around mental health or psychology and their relation to the experience of pain, which may have contradicted those of a psychologist. I would begin exploring this further by restating my position as a curious researcher, for example, by saying ‘it’s really useful to understand your views and experiences, would it be okay to explore that more’? This hopefully enabled the participants to be honest about their perspectives and not be concerned about my professional views as a clinical psychologist.
As a trainee clinical psychologist, I was aware of psychological approaches to managing pain, such as the role accepting the pain has in this. When analysing the data, acceptance was a concept often referred to by the participants. This is something that I had anticipated to arise, and there was a risk that my own views could bias my interpretations. The inclusion of acceptance in the final themes was decided to be appropriate as this was a theme among the majority of the participants, and was described as ‘acceptance’ by them, with data excerpts to back this up.
Results
The analysis resulted in the creation of four themes: ‘How can I have pain in my foot when I don’t have one’: Making personal and social sense of phantom limb pain; ‘If you talk about them, they seem to come’: Perceiving phantom limb pain as an externalised threat; ‘The sooner you accept things, truthfully accept things, then life becomes better’: Achieving acceptance through gaining new perspective and having autonomy over current circumstances; and The unrecognised role of psychology in managing phantom limb pain.
‘How can I have pain in my foot when I don’t have one’: Making Personal and Social Sense of Phantom Limb Pain
Participants described having a phantom limb with pain as ‘bizarre’ (Carl) and ‘strange’ (Nicola). The non-volitional positioning of the phantom limbs and their unpredictability contributed to the phenomenon’s ‘strangeness’: ‘my arm was in the air hanging’, and I said ‘I couldn’t bring it down’ (Ava); ‘the timeline makes it even more unbelievable because they took the foot on the Friday and I never felt anything, on the Tuesday they took the leg below the knee, I started feeling the foot’ (Lucy).
Participants expressed difficulty in making sense of PLP as they struggled to comprehend how pain could exist in the absence of a limb. This subsequently led to a lack of direction in how to manage the pain: ‘When you’re in a situation where you experience pain that you don’t know where it’s coming from, you just try anything’ (Nicola).
Challenges in understanding PLP contributed to participants’ negative experiences, such as worrying that they were ‘nuts’ (Laura), and experiencing or fearing judgement from others: ‘everybody just thinks you’re some kind of freak’ (Lucy). Participants emphasised the difficulty in explaining PLP to others: ‘it is weird because if you don’t experience it, I don’t think you would understand’ (Ava). This was exacerbated by participants’ attempts to ‘look as normal as possible’ (Ava) and not let the pain hold them back. Friends and family would misinterpret this appearance of ‘normality’ to mean the pain had resolved: ‘my mum says to me “ohh you still get that pain then”…if they’re not seeing me in pain, you’re not in pain, that’s how people are’ (Lucy). In Ava’s case she found herself persuading her doctor to acknowledge the severity of the pain ‘he’s “ohh yes…everything is fine.” I said… “but what about my phantom pain?”…“oh…you need to be positive”’.
In addition to trying to understand the anatomical origin of the pain, participants described the psychological ways they had made sense of it. For Carl this was a sense of the mind being ‘psychologically stuck’, and Lucy and Laura hypothesised that the pain was manifested from memories of pre-amputation pain or from having an expectation that they would develop PLP. For some participants, receiving an explanation from professionals of why they were experiencing this pain significantly aided their understanding, enabling them to better explain it to others and advocate for themselves.
Connecting with others who had experienced PLP was a valuable resource: ‘to speak to people that actually have had it…just sort of reiterates the fact that you’re not nuts’ (Laura). These peer interactions were viewed by some as more meaningful than support from a psychological professional with no direct experience of PLP: ‘if I walked in and somebody was going to try and tell me about phantom pains but they were sitting with four limbs, how do they know what phantom pain is?...it’s the hardest thing to try and explain’ (Paul). It was through connecting to people with similar experiences that participants felt validated and less alone: ‘it sounds weird, but you feel a bit like it’s just you at first...and then you’re like, “oh, this has happened to loads of people”’ (Kerry).
Some participants drew upon the confusion around the pain’s ‘realness’ and used this as a coping mechanism, though this wasn’t always successful: ‘I think it’s just a case of convincing myself that it's not real...get into a frame of mind and a state of meditation where I can sort of mentally visualise that it's not there if that makes sense...sort of trick your mind into accepting that it's not there’ (Laura); ‘a lot of times I’ll just tell my brain that it is not there, forget about it, but it…doesn’t work because...it is there because I have all the sensations’ (Ava).
‘If you talk about them, they seem to come’: Perceiving phantom limb pain as an externalised threat
With the exception of Phil, participants described PLP as an intense and aggressive sensation, using terms like ‘stabbing’ (Paul), ‘crushing’ (Lucy) and ‘electric shock’ (Ava). The descriptions personified the pain as something external and hostile which was out of their control and came ‘with a vengeance’ (Laura & Kerry). For some, the threat of the pain was like a constant companion always looming in the background: ‘the pain is with me always’ (Lucy); ‘family knows…don’t talk about them, because if you talk about them, they seem to come’ (Paul). Carl described how the pain ‘seemed to come on its own schedule...it...decided to come and there was nothing I could do’.
This externalisation also extended to the brain, which Laura, Phil, Nicola and Carl, viewed as the source of the pain: something that the ‘mind does…to you’ (Carl). This externalisation influenced how participants responded to the pain. For Nicola, this relinquished any blame on herself for not doing enough to prevent it. Lucy described the pain as being ‘my body’s way of telling me you’ve got to slow down’ when she is anxious or stressed. Phil interpreted his milder PLP from a more humorous perspective, as a prank that his ‘brain’ was playing on him and would converse with the brain as a way to manage with it: ‘“good one brain!...the other foot, I might have believed you, not this one!”…I just have a bit of a conversation with it’.
Overall, while participants could not directly control the pain, externalising it allowed them to feel more in control of how they responded to it.
‘The sooner you accept things, truthfully accept things, then life becomes better’: Gaining through gaining new perspective and having autonomy over current circumstances
All the participants described the importance of gaining control over the pain and the impact it had on their life. For some participants this related to not letting it bring their mood down, and for others it was not letting the pain hold them back from engaging in meaningful activities.
Participants identified that the pain sometimes led to low mood, anxiety, and frustration. For some, this was in the past, but for others such as Ava, this was something she was still experiencing significantly: ‘at times I think that…if I start crying, maybe I would never stop’ (Ava). For some participants, mental health affected how they experienced the pain. For Lucy, poor mental health made her focus more on the pain, and Laura described being able to manage better with the pain if she was in a good mindset: ‘I can say… “you’re not gonna beat me today”’. To manage the emotional impact of the pain, participants used various coping techniques such as peer and professional support, distraction, keeping a diary and writing stories.
Participants described moving towards acceptance of the pain alongside the impact of having lost a limb: ‘it is loss of limb, loss of independence and then the phantom pain on the top…it is quite complex’ (Ava). Participants were at different stages of their journey towards acceptance. Carl described the process of acceptance happening naturally, and recognition that this process cannot be forced: ‘you can’t tell a person...go ahead and accept it...that’s something they have to do internally’. Acceptance was viewed by participants as a step to moving forward in life: ‘the sooner you accept things, truthfully accept things, then life becomes better because you can only move forward’ (Lucy). Ava, overwhelmed with the ongoing experience of severe pain and loss of independence had found reaching acceptance more of a battle. The grief she experienced for her past was illustrated by the stark contrast in words she used to describe her past (e.g. ‘beautiful’, ‘good’), her present (e.g. ‘terrible’, ‘depressing’), and her future (e.g. ‘no light at the end of the tunnel’). Though hoping to reach acceptance, she found she was held back by a lack of goals.
Four processes were identified by participants for achieving acceptance: (1) Letting go of grief for the past and instead viewing life in two parts (‘before amputation’ and ‘after amputation’): ‘if you accept the way things are, in a way where it’s not…“I need to accept that my life’s shit”- that’s not gonna help you...just that...your life is different now’ (Lucy); ‘I go well, I’m gonna be in pain. Now take this as being the baseline and work around that’ (Phil) (2) Accepting existence of pain is out of your control: ‘if nothing’s going to take [phantom limb pain] away then …I just deal with it’ (Laura) (3) Focusing on what you can change and setting goals for the future: ‘I was thinking about what I was going to do…thinking…planning’ (Carl) (4) Engaging in more meaningful and enjoyable activities: ‘doesn’t stop me doing anything else I want to do’ (Paul), or through taking their experiences as motivation to give back to others: ‘it’s very rewarding…seeing people get better and improve’ (Carl); ‘like to think I’m giving a bit back’ (Phil).
These processes helped participants to adapt and move forward despite the challenges associated with experiencing pain.
Participants described further methods for coping with the impact of the pain on mental health and quality of life which were more nuanced to the experienced of PLP. The first was through the sense of control they gained from the knowledge that they had chosen to have an amputation for a medical reason or their wellbeing (Laura, Phil, Lucy, Nicola and Kerry): ‘For me…it was just successful, that’s what I wanted and I was really positive’ (Phil). This also meant some of the participants had been more prepared for the possibility of having PLP (though not all) and were comforted knowing that they had been able to make an informed decision considering the risks of developing PLP.
Finally, participants found comfort or inspiration by comparing their current experience to past experiences, alternative realities and others’ experiences. For example, participants found comfort in the knowledge that their current pain was less severe than their pre-amputation pain: ‘I just remind myself...it’s not a bad as what I used to experience and sometimes that helps’ (Nicola). For Carl, comfort was found in thoughts of where he would have been had the amputation not happened: ‘[the amputation was] probably the best thing that ever happened to me in my life…because…I wasn’t doing anything with my life…because of the [amputation], I got my education status’. Paul found solace in his understanding that everyone has their own burdens in life, and this was his ‘lot’ in life to manage with: ‘I put it down to people that’ll get migraines, to me, this is my kinda migraine, when it comes…you just deal with it’. Some found inspiration from other’s positive stories: ‘I was just in total awe of this woman…how far she’d come… I thought…even if I was to get an amputation, that’s my hero’ (Laura).
These comparisons helped the participants gain a more positive perspective, enabling them to live their lives without allowing the pain to overwhelm them. For Ava however, comparisons to other people were less helpful: ‘hearing from others, how they…experience [PLP] doesn’t help me because…it is me who is going through it’, instead preferring to hear positive stories and being around positive energy helped to lift her mood.
The unrecognised role of psychology in managing phantom limb pain
Following their amputations, participants initially focused on physical healing, with less attention given to phantom limb pain (PLP) from participants and clinical staff: ‘I wasn’t given much information [about phantom limb pain] at all’ (Ava). Pharmaceutical interventions for managing PLP tended to be prioritised with a lack of psychological support offered: ‘I never spoke about mental health side of things…I’d more concentrate on the physical’ (Lucy), ‘no-one’s going “oh would you like to try [therapy] as well as the meds?” They just go “oh here’s your tablets”’ (Kerry).
There was some divergence in participants’ views on the role psychological interventions could have in supporting with PLP. Those who felt it did have a role either had personal positive experiences of receiving psychological support for pain such as Lucy: ‘I did benefit…a lot…from the therapy’, or could see the potential benefit it could have had for others as stated by Phil: ‘I can think of a few people who would have really benefited from psychological support’. Lucy identified that helpful aspects of the psychological therapy she received were psychoeducation around pain and mental health, having space to talk to someone, being guided to make changes to improve her life, and adopting a more positive perspective. Some did not see as direct a role of psychology in managing with the pain, which related to the pain not being ‘that kind of a problem’ (Carl) or not fitting with who they are as a person ‘it’s not really my sort of thing’ (Paul). Other barriers to engaging in therapy described by the cohort included the travel and financial burden of attending and not holding hope that it could help.
Despite psychological input not always being a priority and varying views on the role psychology has in managing PLP, all participants described having used techniques to manage with the pain which were psychological in nature. Alongside working towards acceptance, these other psychological techniques were described: (1) Talking to others with shared experience: ‘because it’s a new voyage and…you’re trying to figure it out’ (Carl). (2) Meditation: ‘meditation…helps…if I can sort of convince my brain that it’s not real’ (Laura). (3) Relaxation: ‘if I do my relaxation exercise…[the pain] could go away…sort of acquiescing instead of fighting’ (Carl). (4) Distraction and redirecting attention: ‘keep your mind occupied’ (Paul); ‘not concentrating on my phantom pain, so I’m…distracting myself to think about something else’ (Ava). (5) Looking after their physical and emotional wellbeing ‘if I exercise regularly…sleep better…eat well…my brain’s in a better place’ (Kerry). (6) Nicola also theorised how EMDR could have a potential role: ‘amputation is traumatic, there is a lot of trauma in that...so I think EMDR does have a place...it helps to deal with trauma’ (Nicola).
Being able to make sense of the pain and recognising it as ‘real’ was an important process before being open to psychological therapy. Participants described concerns over the effect of pain relief medication on their health and wellbeing, and that they were open to more ‘natural’ interventions: ‘EMDR…is natural…that’s why I’m hoping it works so that I can...cut down on my tablets’ (Nicola).
Discussion
The aim of this study was to understand how people with PLP adjust and make use of psychological ways of coping with the pain.
The study highlighted the complex and often isolating nature of this condition which can be difficult to understand and navigate. The results suggested that while some people with PLP receive adequate explanations of the condition or do not feel a need to understand it, others may have difficulty in making sense of the pain. In comparison to findings with people with chronic low back pain who did not doubt the realness of the pain, 45 the current study found that doubts about what the pain means can result in people worrying that it is not real or worrying about their sanity. These findings mirror those of Sherman et al., 36 who found that concerns around being viewed as ‘insane’ created a barrier to disclosing their experiences to health professionals. The present study furthers these findings by identifying factors contributing to these concerns which included the ‘illogical’ nature of pain where there is no physical limb, the unusual and unpredictable sensations, and not being well informed about the condition. While participants in this study felt more comfortable approaching healthcare professionals compared to a previous study, 36 further efforts are needed to raise awareness of PLP and normalise this.
Bunzli et al. 18 identified that difficulty in making sense of the cause of the pain and understanding how to fix it contributed to the pain-related fear the individuals with back pain experienced. The present study indicates how these processes may occur for people with PLP. Participants’ difficulty in understanding the cause of the pain created feelings of confusion for some and distress around not knowing how to resolve it, or concerns that they were ‘going mad’. This contributed to the emotional impact of the pain and fear of others’ reactions to this. Research indicates that people with unexplained chronic pain have to overcome the belief that pain means there is something physically wrong with them that needs to be fixed 46 and that pain is something to be feared and avoided. 19 This study identified that for those with PLP, they need to overcome beliefs that there could be something wrong mentally, as well as any ongoing physical issues.
This study found that people with PLP may externalise and personify their pain as something that is hostile, aggressive and always looming. This may also extend to the ‘brain’ or ‘mind’, as the entity giving these painful sensations to the individual. This aligns with findings from Hearn et al. 47 regarding neuropathic pain, where the pain was viewed as an external entity from which they are a victim of assault, of which they have no control over. The current study demonstrated the beneficial role that externalising the pain can have. For some this was accepting that the control over the pain did not belong with them, removing responsibility and blame from themselves. They could then focus on how they respond to the pain, rather than trying and failing to control the pain. Externalising the ‘problem pain’ has been found to reduce perceived pain and improve wellbeing. 48
A key process in participants’ managing with these emotions is through reframing their pain, by comparing it to worse previous or alternative experiences (e.g. by finding comfort in the knowledge that they had autonomy over their situation by choosing to have an amputation). This process of shifting their perspective of their circumstances is a mechanism theorised to support people in accepting their circumstances and working towards a more meaningful life. 49
Though there was some divergence in participants’ views as to whether psychology had a role in the management of PLP, all described using psychological approaches to managing the pain and had found these helpful. These included engaging in psychological therapy, practicing relaxation, meditation, distraction, self-talk, engaging in meaningful activities, and moving towards acceptance of the pain. Out of all these strategies, accepting the pain seemed to be the most salient. This research expands upon previous findings (e.g. 15) by exploring the pathways through which acceptance is achieved. These included looking to the future, moving focus from things out of their control to things are, goal setting, and engaging in meaningful activities. These resonate with theories underpinning psychological therapies such as Acceptance and Commitment Therapy, which aims to move the focus from fighting with the pain and preoccupation with this, to instead focusing on engaging in behaviours which are in line with values, despite the experience of pain.49,50 The findings suggest that this process of moving towards acceptance is something that may happen naturally as people learn to live with PLP; however, psychological therapy may support with this.
Clinical implications
A number of clinical considerations can be identified from this study, relating to pre- and post-amputation care.
Pre-amputation
Patients should be informed about PLP and the risk of developing this post-amputation to enable them to make fully informed decisions. This should be reflected in professional guidance (e.g. British Society of Rehabilitation Medicine, 51).
Post-amputation
Clinicians should facilitate discussions about PLP and offer validation, psychoeducation, and provide explanations to help patients understand what they are experiencing and be able to communicate this to others.
Signposting to organisations which connect people who have undergone amputations would be helpful to facilitate understanding and validation for those experiencing PLP. 52
Role of clinical psychology
Clinical Psychologists could have a valuable role in supporting amputees with managing PLP alongside the trauma and disability associated with undergoing an amputation.
Participants found that processes such as mindfully accepting what is out of their control and engaging in meaningful values and goals-based activities were helpful. ACT may be an appropriate intervention for supporting this population. There was also interest from one participant in the role EMDR could have in addressing traumatic experiences related to experience of pain.
Facilitating engaging with psychological support
People with PLP should be informed about available psychological support and potential benefits of these, backing this up with research to foster hope for positive change.
Limitations
Only one participant had an upper limb amputation, with the other seven participants having a lower limb amputation. The impact of the disability is different for upper and lower limb amputations, and this could influence the way PLP is experienced and how individuals manage with it.
The clinical implications drawn from this study are presented to raise awareness of potential factors influencing individual’s experience of PLP and considerations when clinical teams are supporting them. The findings are drawn from a small sample and as such may not be generalisable to all people with PLP.
Further research
The research highlighted differences in whether psychological interventions were considered or offered for people with PLP. Further research could explore how often the pain management includes a psychological component and explore clinicians’ awareness of the potential benefits of this.
Future studies could explore the difference in experience of PLP in upper versus lower limb amputation and how psychological support could be used to support these individuals.
Conclusion
This study has added to the literature on chronic pain by developing a more thorough understanding of how PLP is experienced and made sense of from a psychological perspective. The findings emphasised the importance of providing psychoeducation to validate individuals’ experiences and support them in understanding why they experience this pain. A range of psychological techniques are described for the use of coping with the pain, suggesting a need for further integration of psychology in the management of PLP.
Supplemental Material
Supplemental Material - Experiences of coping with and adjusting to phantom limb pain: An interpretative phenomenological analysis
Supplemental Material for Experiences of coping with and adjusting to phantom limb pain: An interpretative phenomenological analysis by Anna Packham, Melanie Smith, Katherine Gerrard, and Craig Murray in British Journal of Pain.
Footnotes
Acknowledgements
We would like to thank all the participants for giving us their time to take part in the interviews and share their experiences with us. We would also like to thank the following organisations for their support with recruitment: Finding Your Feet, Tasmanian Amputee Society, Amputation Foundation, Pain UK, England Amputee Football Association, Northern Ireland Amputee Forum, Irish Chronic Pain Association.
Ethical considerations
This study was approved by the Faculty of Health and Medicine Research Ethics Committee at Lancaster University (approval no. FHM-2022-1027-RECR-1) on November 17, 2022.
Consent to participate
Participants gave either written or verbal consent prior to interview. Consent to publish participant’s study data was obtained.
Author contributions
AP conceived and conducted the study under the supervision of CM, MS and KG. AP drafted the article and all authors commented on and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Guarantor
The guarantor is the person willing to take full responsibility for the article, including for the accuracy and appropriateness of the reference list. This will often be the most senior member of the research group and is commonly also the author for correspondence.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
