Abstract
Increases in lung vascular permeability is a cardinal feature of inflammatory disease and represents an imbalance in vascular contractile forces and barrier-restorative forces, with both forces highly dependent upon the actin cytoskeleton. The current study investigates the role of Ena-VASP-like (EVL), a member of the Ena-VASP family known to regulate the actin cytoskeleton, in regulating vascular permeability responses and lung endothelial cell barrier integrity. Utilizing changes in transendothelial electricial resistance (TEER) to measure endothelial cell barrier responses, we demonstrate that EVL expression regulates endothelial cell responses to both sphingosine-1-phospate (S1P), a vascular barrier-enhancing agonist, and to thrombin, a barrier-disrupting stimulus. Total internal reflection fluorescence demonstrates that EVL is present in endothelial cell focal adhesions and impacts focal adhesion size, distribution, and the number of focal adhesions generated in response to S1P and thrombin challenge, with the focal adhesion kinase (FAK) a key contributor in S1P-stimulated EVL-transduced endothelial cell but a limited role in thrombin-induced focal adhesion rearrangements. In summary, these data indicate that EVL is a focal adhesion protein intimately involved in regulation of cytoskeletal responses to endothelial cell barrier-altering stimuli.
Keywords: cytoskeleton, vascular barrier, sphingosine-1-phosphate, thrombin, focal adhesion kinase (FAK), Ena-VASP like protein (EVL), cytoskeletal regulatory protein
Introduction
Acute inflammatory diseases are characterized by inflammatory cell- and cytokine-mediated disruption in the integrity of the endothelial cell (EC) barrier resulting in prominent vascular leak, interstitial edema and organ dysfunction. 1 The vascular barrier is regulated by the actin cytoskeleton that maintains a balance between barrier-disrupting contractile forces2,3 and barrier-protective forces that include cell–cell and cell matrix interactions. 4 We have earlier5–8 demonstrated that sphingosine-1-phosphate (S1P), a vascular barrier-enhancing agonist, promotes EC myosin light chain kinase (MLCK)-mediated myosin light chain (MLC) phosphorylation, and cytoskeletal remodeling in peripheral regions, including lamellipodia, processes critical for closure of intercellular gaps and restoration of vascular barrier integrity.8,9 In contrast, thrombin, a vascular barrier-disrupting agent, causes centrally-distributed MLC phosphorylation and actin stress fiber formation that results in cell contraction and loss of vascular barrier integrity. 10 The process of vascular barrier regulation is highly dynamic involving actin polymerization via multiple cytoskeletal effector proteins that include cortactin, nmMLCK, Arp2/3, p21-activated kinase and a number of other effectors.5–8
The Ena/VASP family of proteins are involved in processes regulating the actin cytoskeleton, 11 sharing a common C-terminal EVH2 domain involved in G- and F-actin binding and tetramerization via the oligomerization domain located at the terminal end of the protein. Ena/VASP proteins contain a central proline-rich region, while the N-terminus comprises an EVH1 domain that mediates interaction with other proteins and promotes localization to focal adhesions (FA). 12 The localization of Ena-VASP members at lamellipodia protrusions, filopodia, FA and cell–cell contacts enables its involvement in dynamic actin rearrangements that occur at these sites.12–14 The critical role of these proteins in maintaining a functional endothelium is highlighted by mice lacking all three family members (Ena-VASP-like (EVL), Mena and VASP 15 ) that exhibit defects in acto-myosin contractility and structural integrity of the vasculature resulting in edema, hemorrhage and lethality. 16 Recent studies using CRISPR/Cas9 have highlighted the role of Ena/VASP proteins in maintenance of the lamellipodia architecture and actin network through effects on the capping protein and the Arp2/3 complex. 17
The actin cytoskeleton is connected to the cell exterior through FAs that are sites of protein complexes including integrins, paxillin, vinculin, focal adhesion kinase (FAK) and several other proteins.18,19 FAK is a non-receptor kinase that is involved in lamellipodia dynamics and assembly and disassembly of FAs. These effects are highlighted in FAK-deleted ECs that show reduced tubulogenesis, proliferation and migration. 20 Work from our laboratory has demonstrated important differential roles for FAK mediated protein phosphorylation in both S1P-induced EC barrier enhancement and thrombin-mediated barrier disruption.21,22 Therefore, we hypothesized that EVL, an FA protein, regulates vascular barrier permeability through participation of FAK.
In the current study, we investigated the role of EVL in vascular barrier regulation with a focus on cytoskeletal interactions and FA function. We demonstrate the important participation of EVL in regulating EC barrier integrity utilizing biochemical assays, as well as measurements of trans-endothelial electrical resistance (TEER) and total internal reflection fluorescence (TIRF) microscopy. TIRF microscopy allowed quantification of the cellular changes occurring in FAs and lamellipodia in response to S1P and thrombin challenge. Finally, we characterized FAK phosphorylation in cells over-expressing EVL in response to S1P and thrombin. Taken together, these data indicate that EVL is a novel regulator of vascular barrier integrity via interactions with FAK and cytoskeletal regulatory proteins.
Materials and methods
EC culture
Human pulmonary artery ECs (Lonza, Walkersville, MD) were cultured in Endothelial Basal Medium supplemented with bullet kit (Lonza, Walkersville, MD). Cells were passaged using trypsin-EDTA (ThermoFisher Scientific, Waltham, MA) and used between passages 6 and 8. 23
siRNA transfection
Non-targeting and EVL siRNAs were obtained from IDT (Coralville, IA). HPAEC cells were transfected using Siportamine (ThermoFisher Scientific, Waltham, MA) as described previously. 24 Media was replaced 6–8 h after transfection.
Lentivirus and overexpression of EVL
Human EVL was cloned into the pGIPZ vector as a myc tag fusion to generate pGIPZ-myc-EVL. Lentiviral particles were generated by co-transfecting pGIPZ-myc-EVL, pMD2G (Addgene, Watertown, MA, USA), and psPAX2 (Addgene, Watertown, MA, USA) using XFect (Takara Bio, Mountain View, CA). Supernatant containing virus particles were concentrated using Lenti-X Concentrator (Takara Bio, Mountain View, CA) and used to infect HPAEC cells. 25
Transendothelial electrical resistance
Transendothelial electrical resistance (TEER) measurements of HPAEC cells plated in 96-well TEER plates (Applied Biophysics, Troy, NY) were performed using an electrical cell–substrate impedance sensing system (ECIS) (Applied Biophysics, Troy, NY). Thrombin (Sigma, St Louis, MO) and S1P (Sigma, St Louis, MO) were used in these experiments to simulate vascular disruption and vascular protection respectively. 23 Resistance values obtained were normalized to the initial resistance. Differences between treated vs. control were plotted as increase or decrease in normalized resistance upon S1P and thrombin treatment at the peak (S1P) or the nadir (thrombin) effects.
Western blotting
Following transduction, ECs were washed twice with PBS and cells were lysed in 1× LDS sample buffer (Thermo Fisher Scientific, Waltham, USA). Cell lysates were centrifuged at 12,000 r/min and protein was estimated in supernatants. Equal amount of protein was loaded onto 4–12% Bis Tris gels (Thermo Fisher Scientific, Waltham, USA), transferred to PVDF membranes, blocked for 1 h using blotting grade blocker non-fat dry milk (Bio-Rad, Hercules, USA). Primary antibodies used were EVL (Santa Cruz Biotechnology, Dallas, USA), FAK (CST, Danvers, MA, USA), FAK-Y397 (CST, Danvers, MA, USA), MLC2 (CST, Danvers, MA, USA), pMLC2-T18/S19 (CST, Danvers, MA, USA), FAK-Y576 (Abcam, Cambridge, MA, USA) and vinculin (MilliporeSigma, St. Louis, MO, USA) and imaging was carried out using a ChemiDoc MP imaging system (Bio-Rad, Hercules, USA). β-actin was visualized using HRP-conjugated antibodies (MilliporeSigma, St. Louis, MO, USA). 26
Immunohistochemistry
HPAEC transduced with GFP or GFP-EVL lentivirus were plated on collagen coated coverslips and fixed in 4% paraformaldehyde/PBS at various time points (0, 5, 10, 20) after treatment with thrombin (0.5 U/ml) or S1P (1 μg/ml) at 37°C. Fixed HPAEC were stained for paxillin using mouse IgG1 anti-paxillin (610619) (1.25 µg/ml) (BD Biosciences, San Jose, USA) followed by secondary antibody Alexa Fluor 594-conjugated goat anti-mouse IgG (Jackson ImmunoResearch, Westgrove, USA); for filamentous actin using Alexa Fluor 647 phalloidin (A22287) (5 units/ml) (Thermo Fisher Scientific, Waltham, USA); Hoechst 33258 (5 µg/ml) (23491-45-4) (MilliporeSigma, St. Louis, MO, USA). Slides were mounted using Aqua Poly/Mount (Polysciences Inc., Warrington, USA). Immunofluorescence images were obtained using Ti-E inverted microscope (Nikon), with a 100× Apo TIRF 1.49 NA objective (Nikon, Melville, NY) using TIRF illumination, an ORCA-Flash 4.0 V2 complementary metal-oxide semiconductor (CMOS) camera (Hamamatsu, Bridgewater, NJ), and a motorized stage. FA area was analyzed based on paxillin immunofluorescence representing FAs. Total FA area per cell was quantified by measuring paxillin area of non-clustered cells using Elements software (Nikon, Melville, NY). Area measurements were performed by equally thresholding all images within an experiment using an average background fluorescence intensity and generating a binary mask. Individual FA area was measured utilizing 8–15 cells per timepoint and biological replicate, with a total of three biological replicates for each experimental condition. Automated area measurements of binary masks for both cell size and FA size were obtained, and the paxillin-positive area of each cell as well as the number of FA per cell was plotted. A two-way ANOVA followed by Sidak’s multiple comparison test was used to analyze the effect of GFP and GFP-EVL in Thrombin or S1P treated cells.
FAK analysis
Western blotting images were quantified using Image Lab (Bio-Rad, Hercules, USA). Individual blots were run for total and FAK phosphorylation analysis to overcome problems with stripping and re-probing. The ratio between FAK phosphorylation levels to total FAK levels was obtained with normalization being carried out using β-actin. FAK phosphorylation levels were compared to controls at 0 time. Results were evaluated using Student’s t-test (unpaired) as previously described 27 and P < 0.05 was considered statistically significant.
Results
EVL regulates EC barrier responses to S1P
Via the ligation of G-protein coupled receptors, S1P is a vascular barrier-enhancing agonist that reduces existing permeability and results in restoration of EC barrier integrity. 9 To investigate the role of EVL in vascular barrier processes, we overexpressed EVL by transducing human lung EC with lentivirus vectors pGIPZ-Myc-EVL or pGIPZ-GFP to generate myc-EVL or GFP cells, respectively. EVL and GFP overexpression was verified using western blotting against the MYC tag and GFP, and equal loading was confirmed using vinculin as a loading control (Fig. 1c). Transduced EC cells were plated and changes in TEER were recorded. Untreated myc-EVL and GFP control cells maintained a steady baseline (Fig. 1a). We stimulated both groups of cells with either 1 or 2 μM of S1P, which rapidly increased TEER indicating enhanced EC barrier integrity (Fig. 1a and b). The magnitude of 1 and 2 μM S1P-induced TEER was further increased in EC overexpressing EVL (myc-EVL) when compared to GFP-expressing EC.
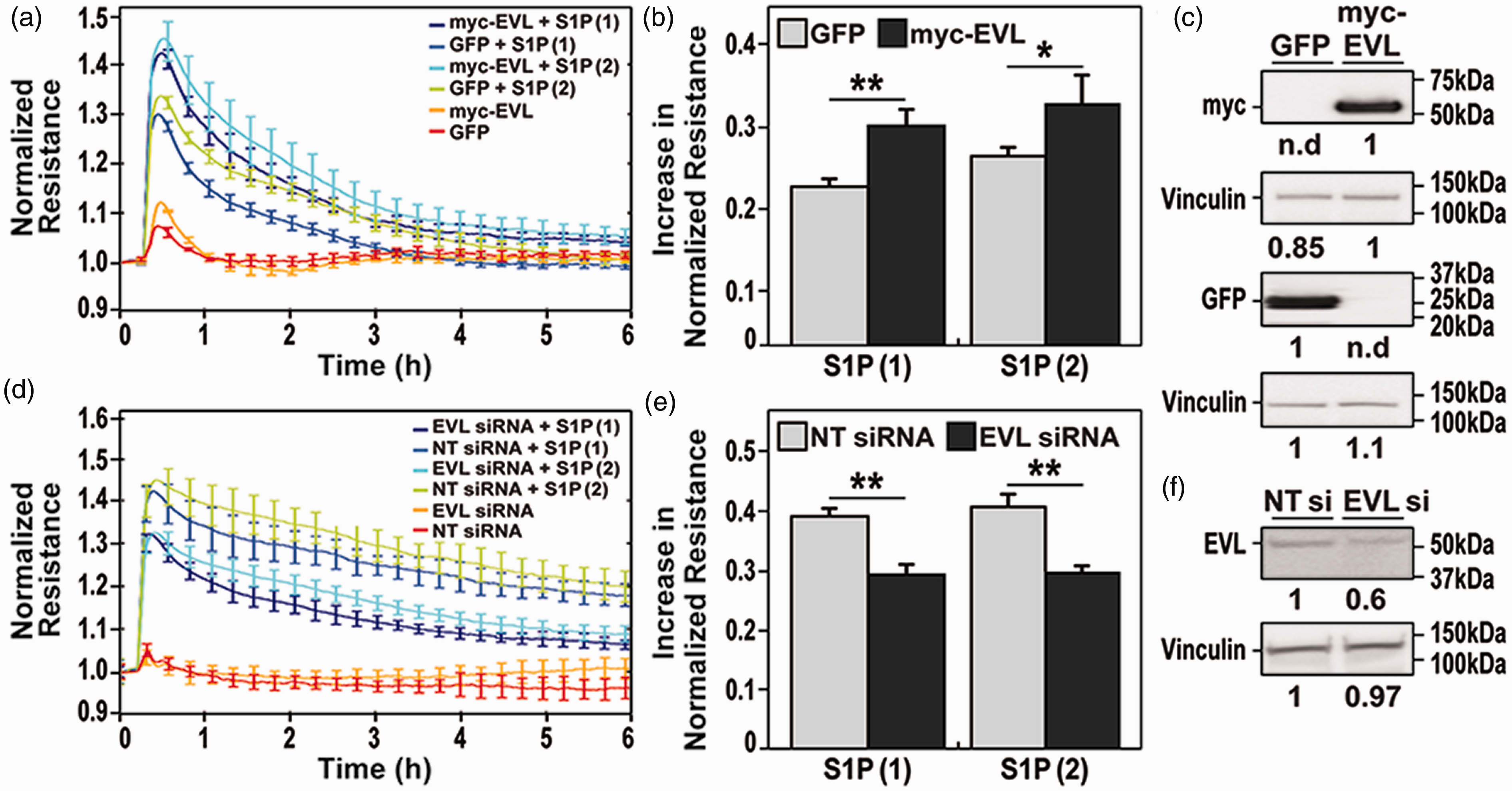
EVL enhances EC barrier-promoting response to sphingosine-1-phosphate. Human pulmonary artery cells were transduced with either GFP or with myc-EVL (a–c) or transfected with siRNA against EVL or a non-targeting sequence (d–f). Cells were plated on ECIS dishes and treated with S1P (1 and 2 μM) and vascular barrier regulation was assessed by changes in resistance. (a). myc-EVL overexpressing EC showed an elevated resistance in response to S1P when compared to GFP transduced cells. Over-expression of myc-EVL and GFP was verified using Western blotting against Myc and GFP (b). Quantification of TEER increases upon S1P treatments (n = 4, *=p < 0.05 and **=p < 0.01). (c) Lane 1. GFP and Lane 2. Myc-EVL-transduced cells. The loading control was vinculin to verify loading. (d) Upon treatment with S1P, HPAEC transfected with EVL siRNA showed a lower resistance when compared to non-targeting siRNA transduced cells. The responses to S1P are also dose dependent. (e) TEER responses increases over control upon S1P treatment are shown (n = 4, **=p < 0.01). The efficiency of knockdown was verified using Western blotting against EVL and vinculin was used as the loading control (f). Lane 1. Non-targeting siRNA and Lane 2. EVL siRNA transfected cells. Band intensity is indicated in (c) and (f).
To validate these findings, we performed the converse TEER experiment in which EVL-specific siRNAs were utilized to reduce EVL expression. EVL silencing was verified using Western blotting against EVL and vinculin was used as a loading control (Fig. 1f). EC transfected with a non-targeting siRNA served as a control. Baseline TEER values were comparable between EVL siRNA- and non-targeting-siRNA-transfected cells (Fig. 1d). Upon S1P stimulation (1 and 2 μM) both groups of cells showed an increase in electrical resistance (Fig. 1d and e). However, non-targeting siRNA-transfected cells exhibited higher TEER when compared to EVL-silenced cells upon S1P stimulation. Together, these data highlight the involvement of EVL in S1P-mediated vascular barrier responses.
EVL protects against thrombin-induced loss of vascular barrier integrity
We next sought to investigate the role of EVL in vascular permeability induced by thrombin, a potent vascular barrier-disrupting agent. 28 For these studies we again utilized the lentiviral myc-EVL or GFP constructs for EC transduction plated in 96 well TEER plates. Protein over-expression was verified by western blotting against the MYC tag and GFP with vinculin as the loading control (Fig. 2c). Both untreated myc-EVL and GFP cells maintained a steady electrical resistance values at baseline, while thrombin (0.25 or 0.5 U/ml) caused an immediate decline in TEER (Fig. 2a and b), indicating disruption of the cell-cell junctions and loss of EC barrier integrity. Thrombin-mediated TEER declines were more pronounced in the GFP-expressing cells when compared to EVL-over expressing EC.
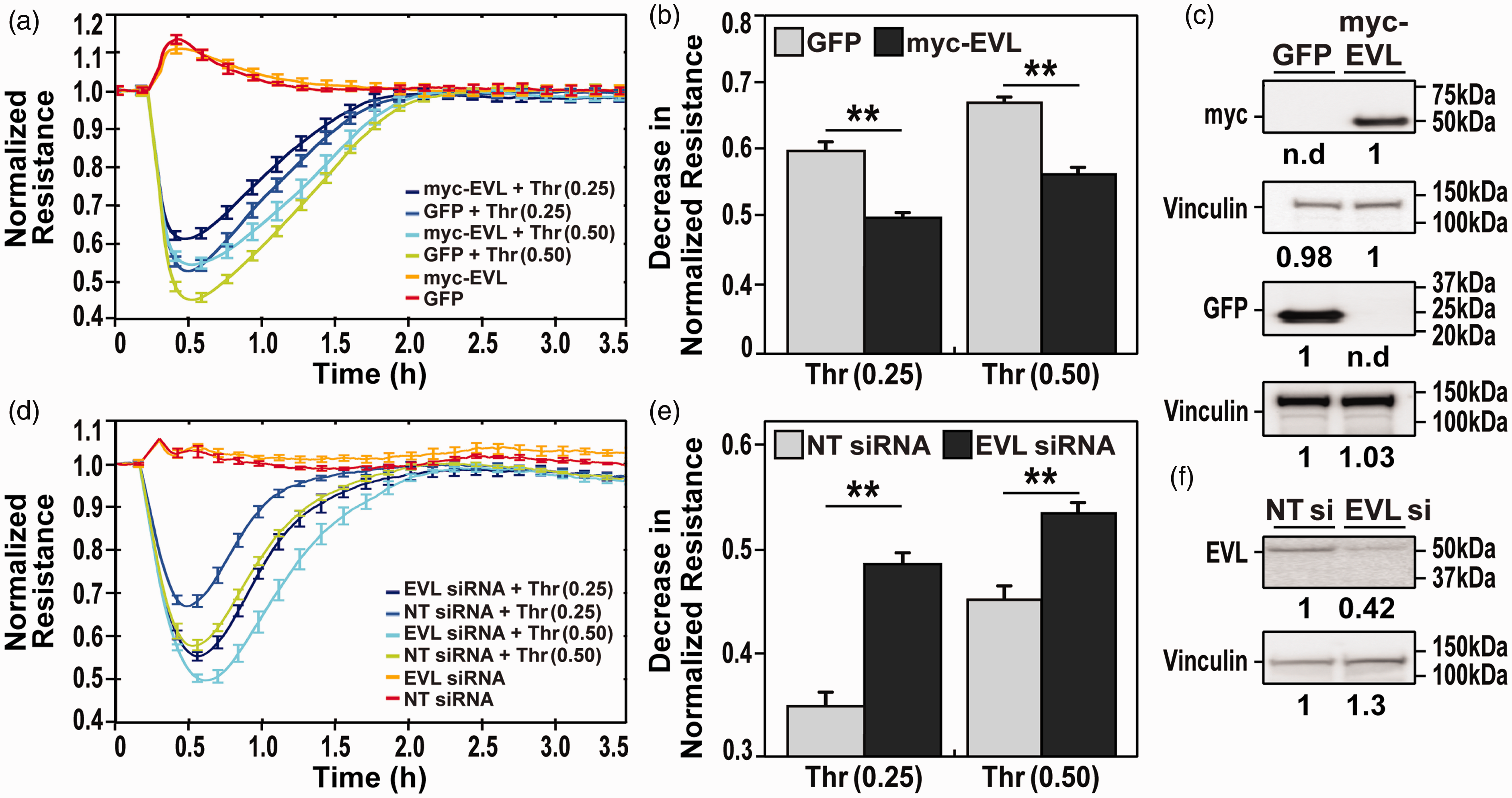
EVL involvement in regulation of thrombin-induced endothelial cell barrier dysfunction. HPAEC were transduced with either myc-EVL or GFP (a–c) or transfected with a siRNA against EVL or a non-targeting sequence (d–f). EC were treated with the vascular barrier-disrupting agent thrombin and TEER followed over time. (a). HPAEC cells over-expressing myc-EVL showed a lower electrical resistance in response to thrombin (0.25 and 0.50 units/ml) in comparison to GFP-transduced cells indicating that that EVL stabilized the vascular barrier upon thrombin treatment. (b) Stabilization is indicated by the reduction in thrombin-induced barrier disruption in EVL-transduced cells. Responses to thrombin was dose-dependent (n = 4, **=p < 0.01). Over-expression of the EVL-myc and GFP was confirmed using Western blotting against myc and GFP (c). Lane 1. GFP and Lane 2. myc-EVL-transduced cells. Vinculin was used as the loading control. (d) HPAEC transfected with EVL siRNA showed a greater drop in electrical resistance in response to thrombin indicating increased vascular leak and underscoring the role of EVL in vascular barrier stabilization. (e) The increased leakage is highlighted by the greater decrease in resistance of EVL siRNA treated cells (n = 4, **=p < 0.01). The efficiency of knockdown was verified using Western blotting against EVL and vinculin was used as the loading control (f). Lane 1 Non-targeting and Lane 2. EVL siRNA transfected cells. Quantification of band density is shown in (c) and (f).
We next performed experiments in EC transfected with EVL-specific siRNA to reduce EVL protein expression levels using a non-targeting siRNA as a control, with effects on EVL protein expression again biochemically verified (Fig. 2f). As in Fig. 1, transfection with neither EVL- nor control-siRNA altered baseline TEER values. However, in EVL siRNA-treated cells, thrombin (0.25 and 0.5U/ml) produced an enhanced barrier-reducing EC response as compared to non-targeting siRNA cells (Fig. 2d and e). Thus, these data indicate that similar to S1P-induced barrier responses, EVL is critical to maintaining EC barrier integrity in face of potent vascular disruption produced by thrombin, highlighting the role of EVL in vascular barrier regulation.
EVL overexpression alters S1P-induced FA remodeling
To further investigate the role of EVL in vascular barrier regulation, ECs were transduced with GFP or GFP-EVL using a lentivirus and treated with S1P for 5, 10 and 20 minutes. Cells were fixed, stained as described above, and TIRF images were obtained. The FA marker paxillin was used to analyze alterations in FA area and the number of FAs per cell. FAs were prominent in both GFP and GFP-EVL transduced cells, however, cells transduced with GFP-EVL displayed an increase in FA size at all time points analyzed (Fig. 3a and b) when compared to GFP-transduced cells and remained persistent upon S1P addition. However, the number of FAs per cell was similar in both treatments at all time points analyzed (Fig. 3c).
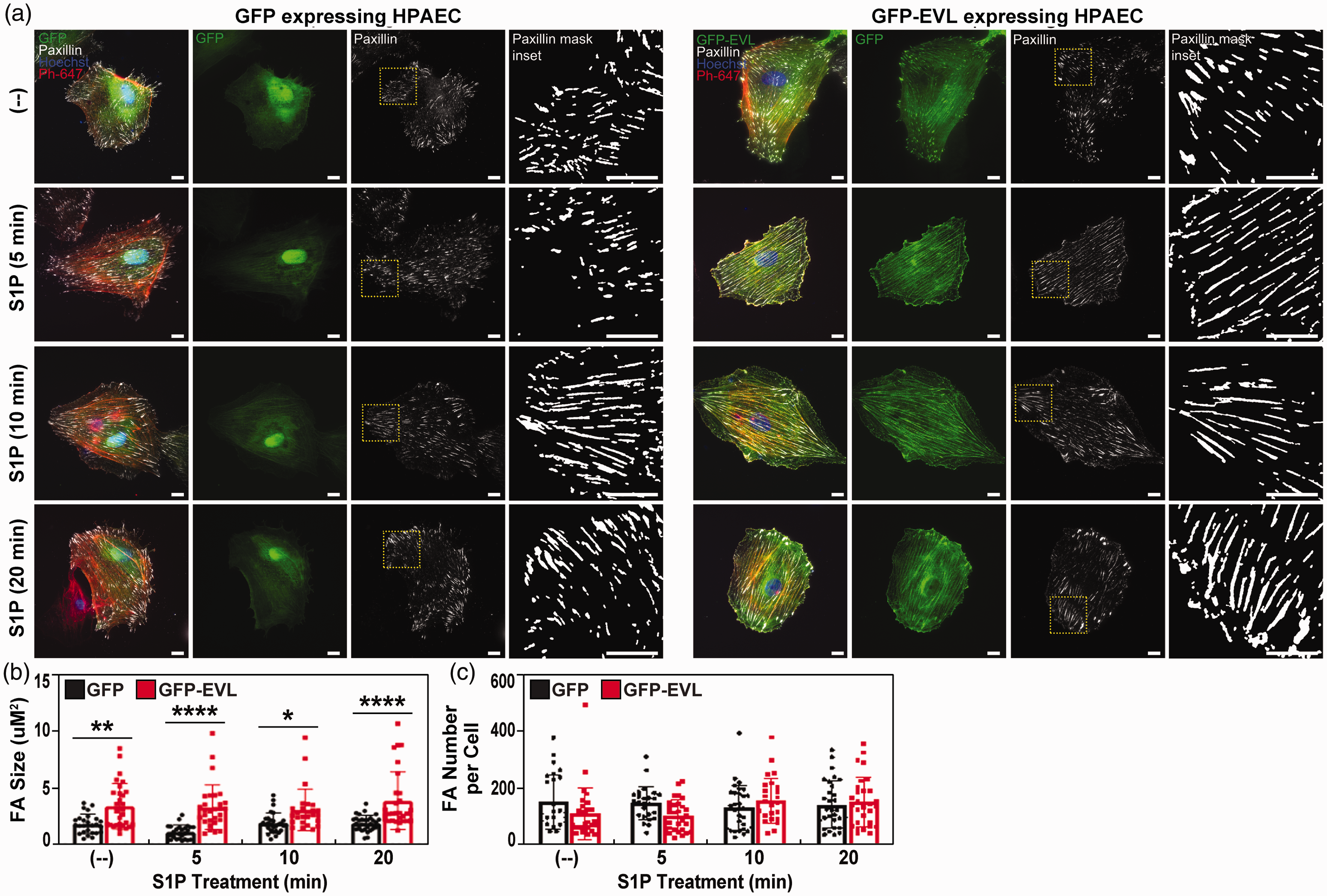
EVL overexpression promotes larger focal adhesion formation in S1P-challenged EC. ECs transduced with GFP or GFP-EVL were treated with S1P for 5, 10 or 20 minutes. HPAEC were then fixed and stained for paxillin, actin (Phalloidin 647) and Hoechst (nucleus). (a) TIRF images showing GFP (left panels) and GFP-EVL (right panels) upon treatment with S1P for 5, 10 and 20 minutes. Each set of images show an overlay of all channels, GFP, paxillin (FA marker) and paxillin using a threshold mask to highlight paxillin rich focal adhesions. (b) Quantification of FA size shows an increase in EVL transduced cells. (c) Quantification of number of FA per cell. The number of FA did not vary significantly among the different treatments or between GFP vs GFP-EVL. Data were analyzed using a two-way ANOVA followed by Sidak’s multiple comparison test. n = 25–30 cells, *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001. Mean and standard deviation are shown. Scale bar = 10 μm.
Thrombin challenge promotes FA coalescence
ECs transduced with GFP and GFP-EVL as described were treated with thrombin and imaged for 5, 10 and 20 min. The size and number of paxillin-derived FAs were analyzed in these images. Consistent with our observation in Fig. 3, EVL transduced cells maintained larger FAs than GFP-transduced cells (Fig. 4a and b). Upon thrombin treatment, EVL transduced cells displayed further increases in FA size 5 min post thrombin (Fig. 4b) and remained elevated 20 minutes after thrombin treatment. This increase in FA size was accompanied by a decrease in FA number in EVL-transduced cells upon thrombin treatment, suggesting FA coalescence (Fig. 4c) due to cell contraction.
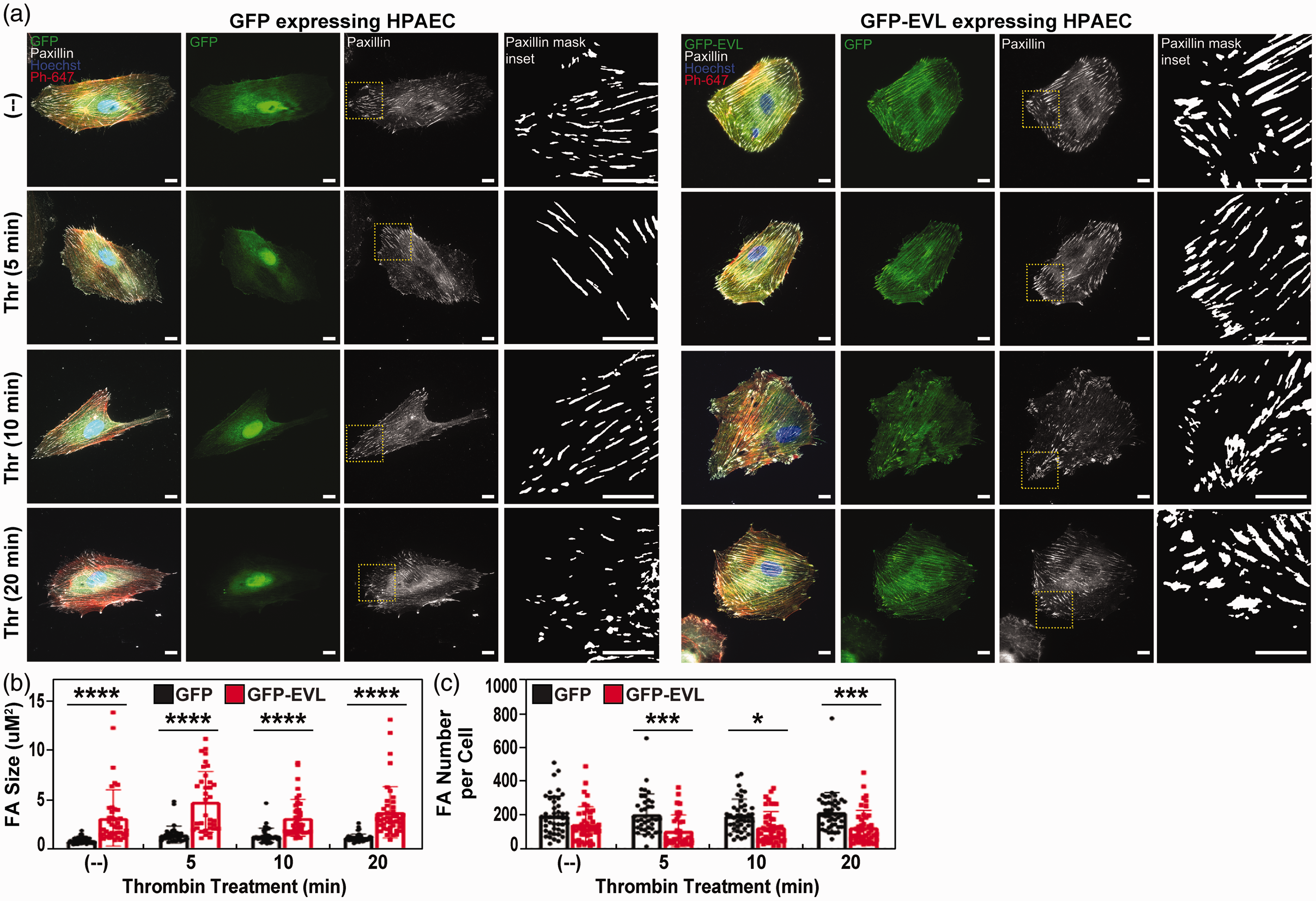
EVL overexpression increases focal adhesion size and thrombin reduces the number of focal adhesions.
S1P enhances FAK phosphorylation in EVL-transduced cells
The increase in FA size suggests a role for FAK in the processes occurring in response to vascular barrier effectors such as S1P and thrombin. To analyze the role of FAK in these processes, we over-expressed EVL in ECs and stimulated cells with S1P or thrombin and analyzed total FAK levels and FAK phosphorylation status on Y397 and Y576, sites we previously identified to be involved in vascular barrier regulation.21,22 S1P treatment caused an increase in FAK phosphorylation in both GFP- and EVL-transduced cells (Fig. 5a). However, the levels of FAK phosphorylation was greater at Y397 and Y576 in EVL-transduced cells compared to GFP-transduced cells (Fig. 5b and c). Similar to S1P treatments, thrombin altered FAK phosphorylation at both Y397 and Y576 sites (data not shown), however, levels of phosphorylation were similar in both GFP- and EVL- transduced cells. Taken together the data indicate a potential role for EVL in determining FAK phosphorylation status in response to S1P.
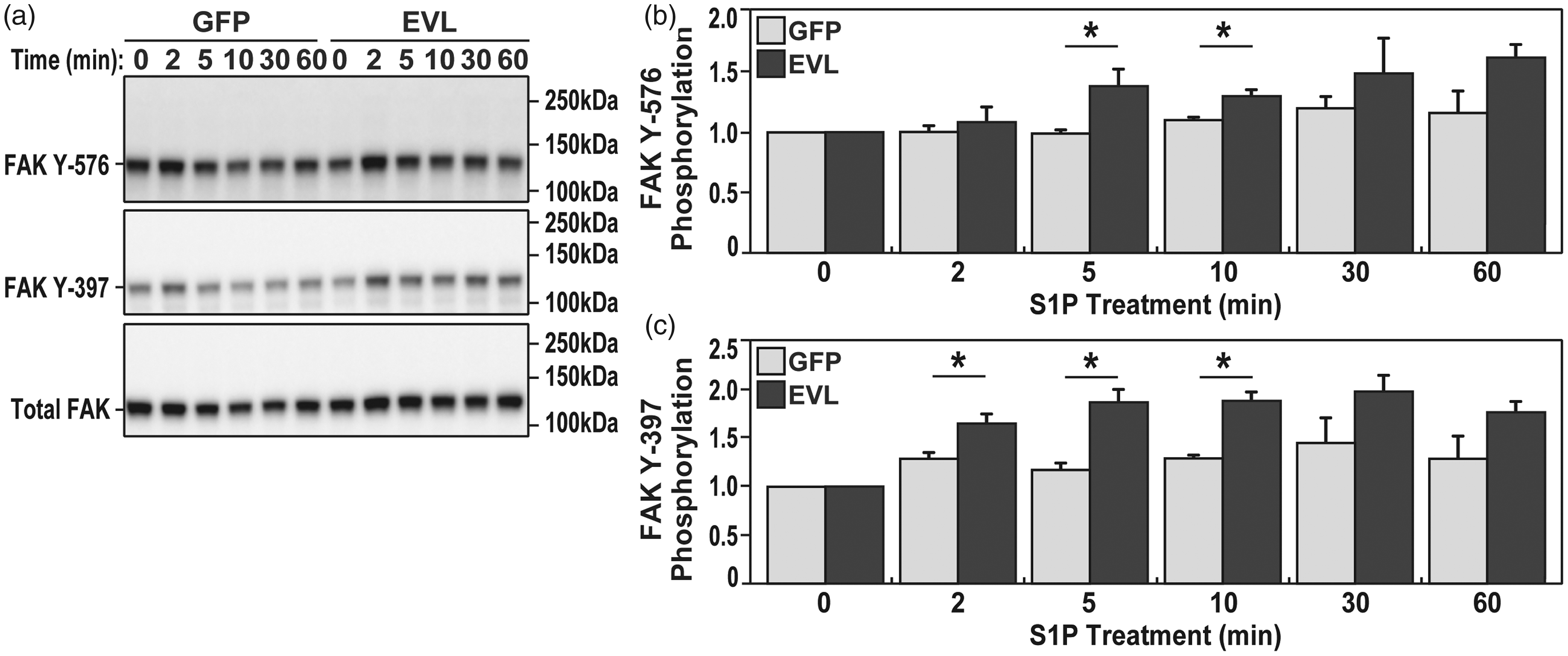
S1P challenge enhances FAK phosphorylation in EVL-transduced ECs.
Discussion
We have demonstrated a role of EVL in promoting vascular barrier integrity as EVL over-expression promotes vascular barrier enhancement in response to S1P and protects ECs from the barrier-disruptive effects of thrombin. These findings were solidified in EVL knockdown experiments where reduced EVL expression resulted in attenuation of S1P-induced vascular barrier enhancement and increased the sensitivity of ECs to thrombin, further highlighting the role of EVL in vascular barrier regulation. These results are consistent with other members of the EVL family of proteins, such as VASP, with reduction of its expression by siRNA previously reported to increase thrombin-induced vascular disruption. 29 Consequently, microvascular permeability is increased when VASP is absent, resulting from direct effects on EC junctions and defects on the endothelial cytoskeleton through disruption of VE-cadherins. These results suggest that these family members have closely related functions and are important in regulating endothelial barrier integrity.
Previously, we have characterized the role of S1P and thrombin in regulating vascular barrier permeability via the actin cytoskeleton and active participation of several key participants such as nmMLCK and cortactin in these processes.8,9,30 The observation that EVL regulates thrombin- and S1P-mediated barrier responses is consistent with its known role in regulating actin polymerization.14,31–33 EVL facilitates these processes through actin elongation and actin nucleation.34,35 EVL is characterized by EVH1 and EVH2 domains that are linked together via a proline rich region. Functionally these domains are distinct, with EVH1 being implicated in targeting of the protein to FA, 36 while the EVH2 domain is involved in regulation of actin polymerization through its binding to both F- and G-actin and thereby facilitating actin chain growth at the barbed ends of filamentous actin. 37 Recent studies using CRISP/Cas9-mediated deletion of Ena/VASP proteins revealed that the lamellipodia architecture was altered and was accompanied by abnormalities in the Arp2/3 complex. 17 The binding of EVL to WAVE localizes the Arp2/3 complex 38 and inhibition of this complex reduced S1P- induced barrier enhancement and delayed recovery after thrombin. 39 It is known that p21-activated kinases regulate the vascular cytoskeleton and deletion of Pak2 in ECs leads to increased vascular barrier permeability 40 suggesting that similar pathways might be involved in EVL-induced vascular barrier regulation. Our results suggest that EVL overexpression may enhance EC barrier function by facilitating increased actin polymerization and causing lamellipodia protrusion to stabilize the cell-cell junctions and close intercellular gaps.
To evaluate the role of FAs in EVL-mediated vascular barrier changes, we utilized TIRF microscopy and evaluated changes in FA size and number by staining for paxillin, a key FA protein. Upon EVL transduction, we observed a significant increase in the size of paxillin-stained FA suggesting that paxillin, EVL and/or integrins are increasingly present in these FAs. These integrins can serve as attachment points to the extracellular matrix and serve as linkage to the actin stress fibers. 41 FA maturity is indicated by size and based on previous classification the large FA can be classified as mature (1–3 μm2) and super-mature (>3 μm2). 42 Based on this classification system, EVL-overexpressing cells showed a greater number of both mature and super-mature FAs that promotes adhesion and stabilization required for vascular barrier regulation. Reduction in FA size particularly of large mature FA in ECs treated with oxLDL caused FA dysfunction and detachment from the matrix. 42 Functionally, FA size determines cell migration 43 and in ECs wherein neuropilin 2 depletion causes reduction in FA size and maturity effecting migration. 44 Therefore, it is also possible that the stabilized FA upon EVL transduction are important during vascular barrier regulation.
Consequent to S1P treatment, we observed larger FA size suggesting a role for FAK in regulating EVL-mediated vascular regulation. FAK is a non-receptor tyrosine kinase that is phosphorylated on a number of tyrosine residues through integrin engagement and several other signaling pathways.45,46 FAK activation results from autophosphorylation at Y397, a site important for Src recruitment, following which the activation loop is exposed resulting in phosphorylation on Y576. 47 Upon S1P treatment, we observed rapid FAK phosphorylation on Y397 and Y576 consistent with FAK activation, which was significantly increased in EVL-transduced cells. Our findings of FAK activation and S1P stimulation are consistent with previous findings from our laboratory21,22 and others 48,49 that favored formation of protective cortical actin rings critical to vascular barrier regulation.
In response to thrombin, EC transduced with EVL exhibit a protective TEER-defined response and exhibited larger size FA. As outlined for S1P-induced changes, thrombin regulates cellular tensile forces through conformational changes in FAK and its activation through phosphorylation 50 thereby initiating a signaling cascade at the FA. 51 We observed enhanced FAK phosphorylation on Y397 and Y576 after thrombin at similar levels in both GFP and EVL transduced EC. These phosphorylation sites were shown to influence the interaction between FAK, paxillin and G-protein-coupled receptor kinase interacting proteins 21 and rearrangements of proteins such as vinculin. 52
Surprisingly, increases in FA size were accompanied by decreases in the number of FAs after thrombin challenge of EVL-transduced cells. We performed western blots in thrombin-stimulated cell lysates to determine levels of MLC phosphorylation, a read out of nmMLCK activation6,50,53 and observed robust phosphorylation of MLC (Figure S1), indicating that the contractile apparatus within these cells was highly activated. Therefore, the observed reduction in FA numbers could be a result of coalescence of the larger FAs observed with EVL transduction. It was also observed that FAK phosphorylation was only partially attenuated by PP2, a src kinase inhibitor while it completely blocked S1P induced phosphorylation 21 suggesting that differential activation of the src kinase might be involved in FAK activation/interaction.
Vascular permeability is a tightly regulated process and our findings regarding EVL regulation of permeability support the notion that similar mechanisms regulate other pathological conditions. Metastatic growth is promoted due to vascular endothelial growth factor overexpression (VEGF) resulting from hypoxic conditions in the tumor microenvironment. 54 In other conditions such as hemorrhagic stroke alterations of vascular permeability cause neuronal damage and prolong the recovery. 55 Finally in ocular diseases perturbations in the endothelial barrier cause edema and disruption of the retinal surface that produces loss of central vision. 56
Contrasting our findings upon estrogen stimulation in breast cancer cells induction of EVL transcription produces suppressive cortical actin bundles of these cells, 57 occurring as a result of changes on global transcription within these cells. Recent findings have also indicated a role for EVL in hematopoiesis and overexpression in murine primary cells driving lymphopoiesis 58 and indicate that effects vary depending on cell type.
In summary, these data support the hypothesis that EVL promotes vascular barrier regulation by direct effects on FA dynamics including FA size and FAK phosphorylation. These findings contribute to the understanding of processes governing vascular barrier integrity and permeability that are critical to the severity of a diverse array of acute inflammatory disorders.
Footnotes
Author contributions
J.B.M performed and analyzed the experiments and was the primary writer; T.M.L, R.M, S.N, C.G contributed by writing the manuscript and performing imaging and analysis; S.M.C, A.A.G, J.R.J, A.E.C, S.M.D contributed to writing and analysis; and J.G.N.G was the project leader and contributed to experiment design and writing of the manuscript.
Acknowledgements
The authors would like to thank Drs. Sara Parker and Marco Padilla-Rodriguez for their invaluable contributions to analyzing the microscopic images.
Conflict of interest
Joe GN Garcia MD is CEO and founder of Aqualung Therapeutics Corporation. All other authors declare no competing financial interests.
Funding
This work was supported by NHLBI grants R01 HL91889, P01 HL058064, and P01 HL126609 (JGNG).
