Abstract
Pulmonary arterial hypertension (PAH) and novel coronavirus (SARS-CoV-2) disease COVID-19 are characterized by extensive endothelial dysfunction and inflammation leading to vascular remodeling and severe microthrombi and microvascular obliterative disease. It is hypothesized that those patients with underlying lung disease, like PAH, represent a high-risk cohort in this pandemic. However, reports of COVID-19 in this cohort of patient have been scaring and an observational survey showed that the disease was relatively well tolerated. We postulate that specific PAH vasodilator may offer some protection and/or advantage in the case of concomitant COVID-19. Here we review the literature describing mechanisms of action for each of the broad categories of PAH therapy, and offer potential hypothesis about why this therapy may impact outcomes in COVID-19.
Pulmonary arterial hypertension (PAH) is characterized by extensive vascular remodeling and endothelial dysfunction leading to characteristic changes in the neointimal, medial, and adventitial layers of the pulmonary arterioles culminating into an expansive microvascular obliterative phenotype. This translates clinically to high pulmonary vascular resistance (PVR), progressive right heart failure, and eventual death.1,2 Patients with PAH are prescribed specialized medications that have anti-inflammatory properties in addition to the better known vascular modifying effects. These medications include: nitric oxide (NO) donors (phosphodiesterase inhibitors and soluble guanylate cyclase stimulators), endothelin receptor antagonists and prostacyclin analogs, as well as a host of novel medications with potential PAH benefits such as,3,4 vasoactive intestinal peptide (VIP), 10-nitrooctadec-9(E)-enoic acid (CXA-10), and tocilizumab (monoclonal antibody against IL-6).
A novel coronavirus (SARS-CoV-2) was identified in Wuhan, China in December 2019 and rapidly spread throughout the world leading to a global pandemic, impacting now more than 2 million individuals.5–10 The SARS-CoV-2 virus leads to clinical disease (COVID-19) which predominantly affects the respiratory system. In its most severe form, COVID-19 produces severe acute respiratory distress syndrome (ARDS), and frequently involves a viral sepsis picture, which may ultimately result in multi-organ dysfunction.5,6 Widespread multisystem organ failure is hypothesized to result from immune-mediated cytokine release from rapid replication of the virus upon entry into the alveolar epithelial cells. 6 Patients with COVID-19 have demonstrated pulmonary vascular microthrombi, diffuse pulmonary interstitial fibrosis, alveolar hemorrhage, and inflammatory infiltrates at autopsy.9,10 These findings likely contribute to severe hypoxemia driven in part, by ventilation-perfusion (VQ) mismatch.
Interestingly, there is overlap of some of the pathologic and physiologic findings in PAH and COVID-19, including microvascular thrombi, endothelial dysfunction and severe inflammatory response.1,2,11,12 Although patients with PAH may theoretically represent a high-risk category if infected with COVID-19, given early reports that underlying cardiopulmonary disease increase morbidity and mortality,6–10 case reports for COVID-19 infection in this group are rare. In fact, the only publication evaluating PAH during the pandemic came from the Pulmonary Hypertension Association, where 13 PAH patients infected with COVID-19 were described. Interestingly, despite the aforementioned risks, only three were intubated and one death was reported. 13 In light of this intriguing preliminary evidence, we postulate that medications targeting PAH may offer some protection and/or advantage in the case of concomitant COVID-19. Here we review the literature describing mechanisms of action for each of the broad categories of PAH therapy, and offer potential hypothesis about why this therapy may impact outcomes in COVID-19.
Nitric oxide donors
To best understand the impact of NO donors on those afflicted by COVID-19, we must first understand the pathophysiology of ARDS. Patients with COVID-19 pneumonia may not have the typical ARDS phenotype despite meeting Berlin criteria for the syndrome. Anecdotal observations describe dissociation between their relatively well preserved lung mechanics/compliance and the severity of hypoxemia, 14 suggesting the source for the acute and rapidly progressive hypoxemia is in the capillaries (profound endothelial dysfunction) and not in the alveoli. 15 Thus, NO may serve as a more suitable treatment in the COVID-19 induced respiratory failure compared to “traditional” ARDS.
Classically, ARDS presents clinically with acute respiratory failure with non-cardiogenic pulmonary edema, mild pulmonary hypertension, and progressive systemic hypoxemia (PaO2/FiO2 ration of <200 mmHg). 16 In ARDS, there is hypoxia-induced pulmonary vasoconstriction, which is perhaps intensified by thromboxane A2 and platelet activating factors. These together limit pulmonary blood flow to poorly oxygenated segments of the lungs and further worsen VQ mismatch, thereby contributing to alveolar dead space and hypoxemia.17–19 The collective result of these changes triggers elevations in PVR, ultimately leading to pulmonary hypertension and right ventricular (RV) dysfunction. In the setting of COVID-19, pathophysiologic changes triggered by ARDS may be intensified by the use of non-selective arterial vasoconstrictors required for hemodynamic support and by the deleterious effects of mechanical ventilation including: ventilator associated lung injury, bio-trauma, and elevated positive-end-expiratory pressure.
There are three potential benefits to NO in the patient with COVID-19 as discussed here: (1) direct treatment of endothelial dysfunction and VQ mismatch, (2) improvement in cardiac reserve, and (3) potential direct anti-viral properties. Treatment strategies to combat and reverse the effects of pulmonary vasoconstriction are supportive efforts directed at managing ARDS in general, but additional direct therapies may be more pertinent to the COVID patient due to aforementioned unique vascular manifestations in the affected lungs. NO and NO synthetase isoforms play an important supportive role in pulmonary vascular physiology. 20 The beneficial effects of NO involve specific mechanisms, which enhance endothelial and smooth muscle relaxation, inhibit platelet aggregation as well as direct effects on the immune system.21–23 Inhaled NO (iNO) improves oxygenation and VQ mismatch in ARDS patients selectively without systemic vasodilation. 24 Selective vasodilation within the pulmonary vascular bed is due to its binding rapidly to hemoglobin hence inactivating it before it reaches the systemic circulation. 25 Subsequent studies in ARDS; however, were not uniformly positive. While there is a transient improvement in oxygenation, the effects are not long lasting.26–28 According to a random-effects meta-analysis, iNO did not reduce mortality in patients with severe (risk ratio (RR), 1.01; 95% CI, 0.78–1.32; p = 0.93, n = 329 patients, 6 trials) or mild to moderate hypoxemia (RR, 1.12; 95% CI, 0.89–1.42; p = 0.33, n = 740 patients, 7 trials). 27
From a cardiac standpoint, it has been demonstrated that COVID-19 may cause direct myocardial injury resulting in cardiogenic shock.8,29 In the patient who may have cardiac toxicity as a result of SARS-CoV-2, iNO may potentially be beneficial, as it has been shown to improve RV systolic function in patients with severe ARDS, independent of change in pulmonary pressure. 30 This improvement in cardiac activity is noted for other disease processes as well, including those with acute RV myocardial infarction and cardiogenic shock. 31 iNO is already recommended for treatment of severe RV failure per the AHA guidelines. 32 iNO’s cardiac benefits likely stem from both a reduction in PVR and improved gas exchange and oxygenation, resulting in enhanced right and left ventricular function, respectively.31,33 Thus, NO donors could mitigate some of the hemodynamic abnormalities in severe COVID-19 infection.
From a direct immune perspective, it is known that NO is a part of the acute immune and inflammatory response system, and is necessary for healing via macrophage-induced NO upregulation. 34 In vitro studies have shown that the NO donor S-nitroso-N-acetylpenicillamine significantly inhibits the replication cycle of SARS-CoV in a concentration-dependent manner.35,36 In a clinical study of SARS patients in 2004, iNO resulted in improved arterial oxygenation, reduction in supplemental oxygen and need for ventilatory support. 37 The same patients experienced shorter duration of hospitalization, and improvements in radiographic evidence of the disease. Based on the genomic similarities between the two coronavirae, the data in SARS-CoV suggest there may also be a potential benefit in using iNO in the setting of COVID-19.
Endothelial receptor antagonists (ERA)
To appreciate the potential theoretic role for ERA therapy in the patient with PAH and COVID-19, one must first appreciate the evolving landscape of pathophysiologic mechanisms presumed at play in COVID-19. The disease itself is characterized by respiratory failure secondary to acute lung injury evolving to ARDS.5,6,38 However, in addition to the direct pathologic effects at the level of the pulmonary system, SARS-CoV-2 has been shown to induce a system-wide coagulopathy. 39 Pathologic specimens have shown microthrombi in the pulmonary vascular system and throughout the body, consistent with the hypercoagulable state SARS-CoV-2 appears to induce.11,40 It is generally felt that SARS-CoV-2 produces system-wide inflammation and activation of deleterious cytokines, proposed responsible for both direct viral, and immune-mediated pathologic changes, particularly evident in the pulmonary system and vasculature.
Endothelin-1 (ET-1) is a vasoconstricting polypeptide. In PAH, there is an imbalance between NO and ET-1, thereby leading to increased vascular tone and vascular remodeling. 41 mRNA ET-1 expression is increased in the presence of growth factors, cytokines, and other vasoactive substances.42,43 It has been proposed that the ET-1-induced necroptotic pathways may be exacerbated by SARS-CoV-2 via RIP-3 activation and ORF-3a. 44 ET-1 pathway also regulates other factors that may be associated with lung injury and ARDS in SARS, such as urokinase pathway-mediated defective extracellular matrix remodeling, 45 enhanced epidermal growth factor signaling, 46 and complement activation. 47 It is therefore suggested that ERAs may be a reasonable therapeutic consideration in COVID-19.
Besides, ET-1 causes significant downregulation of angiotensin converting enzyme 2 (ACE2), similar to effects seen with angiotensin II and reduces myocyte ACE2 mRNA. 48 ACE2 is a critical enzyme of the renin-angiotensin system (RAAS) that is present in various tissues important in the regulation of cardiovascular function. This association may be crucial as SARS-CoV-2 enters lung cells by binding to ACE2 receptors.6,49 Yet, there is much uncertainty regarding whether ACE2 expression may potentiate SARS-CoV-2 infectivity or be protective of severe infection. SARS-CoV-2 appears not only to gain initial entry through ACE2 but also to subsequently down-regulate ACE2 expression such that the enzyme is unable to exert protective effects in organs. 49 It has been postulated but unproven that unabated angiotensin II activity may be in part responsible for organ injury in COVID-19. After the initial engagement of SARS-CoV-2 spike protein, there is subsequent downregulation of ACE2 abundance on cell surfaces. Downregulation of ACE2 activity in the lungs facilitates the initial neutrophil infiltration in response to endotoxins. In experimental mouse models, exposure to SARS-CoV-1 spike protein induced acute lung injury, which is limited by RAAS blockade. 50 These hypotheses have prompted trials to test whether RAAS blockers can be used as treatment for COVID-19. Treatment with ERAs could have direct effect in ACE2 expression and theoretically be beneficial for the treatment in this disease as well.
Patients with severe ARDS can develop pulmonary fibrosis, leading to extensive and irreversible deterioration of pulmonary function that requires lung transplantation. 51 ET-1 signaling emerged as a potential target for pharmacological intervention in the treatment of fibrosis.52,53 ET-1 promotes fibroblast differentiation to a myofibroblastic cell type, inducing the expression of proteins that contribute to a contractile phenotype including a smooth muscle actin. Moreover, ET-1 has been shown to initiate alveolar epithelial cell transition into fibroblast-like cells, a process termed epithelial-mesenchymal transition, and thereby contribute to pulmonary fibrosis. Nevertheless, the results of a number of clinical trials examining the efficacy of ERAs in the context of these diseases did not achieve the primary objectives, a reduction in morbidity/mortality, although they showed a tendency towards those goals. The ARTEMIS-IPF trial 54 was designed to evaluate if ambrisentan reduces the rate of idiopathic pulmonary fibrosis progression, however was terminated early because an interim analysis indicated a low likelihood of showing efficacy for the primary endpoint. Ambrisentan treated patients had more disease progression (p = 0.01) and respiratory hospitalizations (p = 0.007). Complex nature of the fibrotic disease, involving multiple factors, or alternative plausible explanations, such as the establishment of no-return points in the onset of fibrosis beyond which the pharmacological intervention offers little or no beneficial effects, might also contribute to the lack of positive results. ERAs, if initiated early in the process of acute lung injury, may have a potential effect preventive advanced disease and hypoxemia.
Prostacyclin analogs
Prostacyclins resemble endogenous prostacyclin (PGI2) and are most commonly used for treatment of PAH. 2 Therapy is available in oral, inhaled, and intravenous forms. Prostacyclin is produced predominantly by endothelial cells and induces potent vasodilation of all vascular beds. 55 Prostacyclin binds to its receptor (a G-protein coupled receptor) found on the surface of vascular smooth muscle and platelets, activates cyclic adenosine monophosphate (cAMP), and results in the most potent endogenous inhibitor of platelet aggregation, vascular smooth muscle relaxation and vasodilation of the pulmonary arteries. It also appears to have both cytoprotective and antiproliferative properties.
The rationale for prostacyclin use in COVID-19 associated ARDS is three-fold. First, inhaled prostacyclin therapy has been used in the treatment of ARDS and has been shown to improve oxygenation and VQ mismatch.56,57 While it has not been associated with improved patient outcomes and is not routinely recommended, it may be used in severe, life-threatening hypoxemia refractory to conventional ARDS management, such as has been seen in COVID-19. Much regarding the pathophysiology of severe COVID-19 respiratory failure remains unknown, but a profound out-of-proportion to lung mechanics hypoxemia is observed, 14 which is believed to be related to vascular injury and microthrombi. Similarly to NO, prostacyclins’ potent endothelial effects such as prevention of vasoconstriction and platelet aggregation may be particularly important in this viral-induced ARDS. It has the additional advantage over iNO in that it does not require special equipment and may be directly administered through a standard ventilator (close circuit).
The second potential benefit of prostacyclin therapy in the management of COVID-19 is to mitigate direct SARS-CoV-2-associated coagulopathy. Microvascular thrombosis and large vessel thromboembolism have been described anecdotally and in case reports38,40,58 and abnormal coagulation parameters are associated with increased mortality.39,59 Prostacyclin exerts an overall control of platelet aggregability. It inhibits platelet adhesion to exposed vascular subendocardium, but at much higher concentration than those required to prevent platelet aggregation. Therefore, they allow platelet to adhere to damaged vascular tissue and participate in the repair process, while at the same time, preventing or limiting thrombus formation. Prostacyclin therapy combats prothrombotic effects of endothelin and may mitigate thrombosis in situ seen in PAH itself, and potentially in patients with COVID-19-associated respiratory illness.60,61
Finally, prostacyclins enhance NO production, whose beneficial effects are described earlier in the manuscript. The downstream effect of prostacyclins and NO leads to the respective activation of cAMP and cyclic guanyl monophosphate in a synergistic pattern in endothelial cells. Interestingly, these mediators intertwine the activities of prostacyclins and NO in a synergistic manner.
55
The bond between prostacyclins and NO is not expected to be different for COVID-19 compared to other pulmonary infections, but their interaction is important in inflammatory processes and endotoxemic stress conditions, where there is significant increase in IFNγ and/or LPS concentrations in activated cells, especially monocytes/macrophages.
62
The NO antithrombotic effect in platelets aggregation is potentiated by prostacyclins, and their vasodilatory effect in vessels is additive.55,60 This concerted relationship between NO and prostacyclin is also evident clinically,
63
as treatment with epoprostenol restores vasodilatory responses to NO in the pulmonary vasculature. In seven PAH patients who were primary nonresponders to iNO, intravenous long-term administration of epoprostenol for a mean of 18 months, abolished the lack of responsiveness to NO, causing significant improvement in pulmonary hemodynamics and improvement in oxygenation. The underlying mechanism for desensitization of pulmonary arterial tissue to NO is yet unknown, it is conceivable that changes in the contractility mechanisms, such as intracellular calcium concentration, play a role. The synergistic relationship between prostacyclins and NO described above on vascular function would likely benefit those afflicted by COVID-19 given the known endothelial dysfunction seen in this disease, which results both form direct viral endotheliitis and the indirect effect of circulating cytokines. Lastly and speculatively, prostacyclins and NO have important anti-inflammatory effects, especially on monocytes/macrophage function that may be beneficial in the COVID-infected patient
64
(Fig. 1).
Beneficial properties of PAH vasodilators in COVID-19 infection.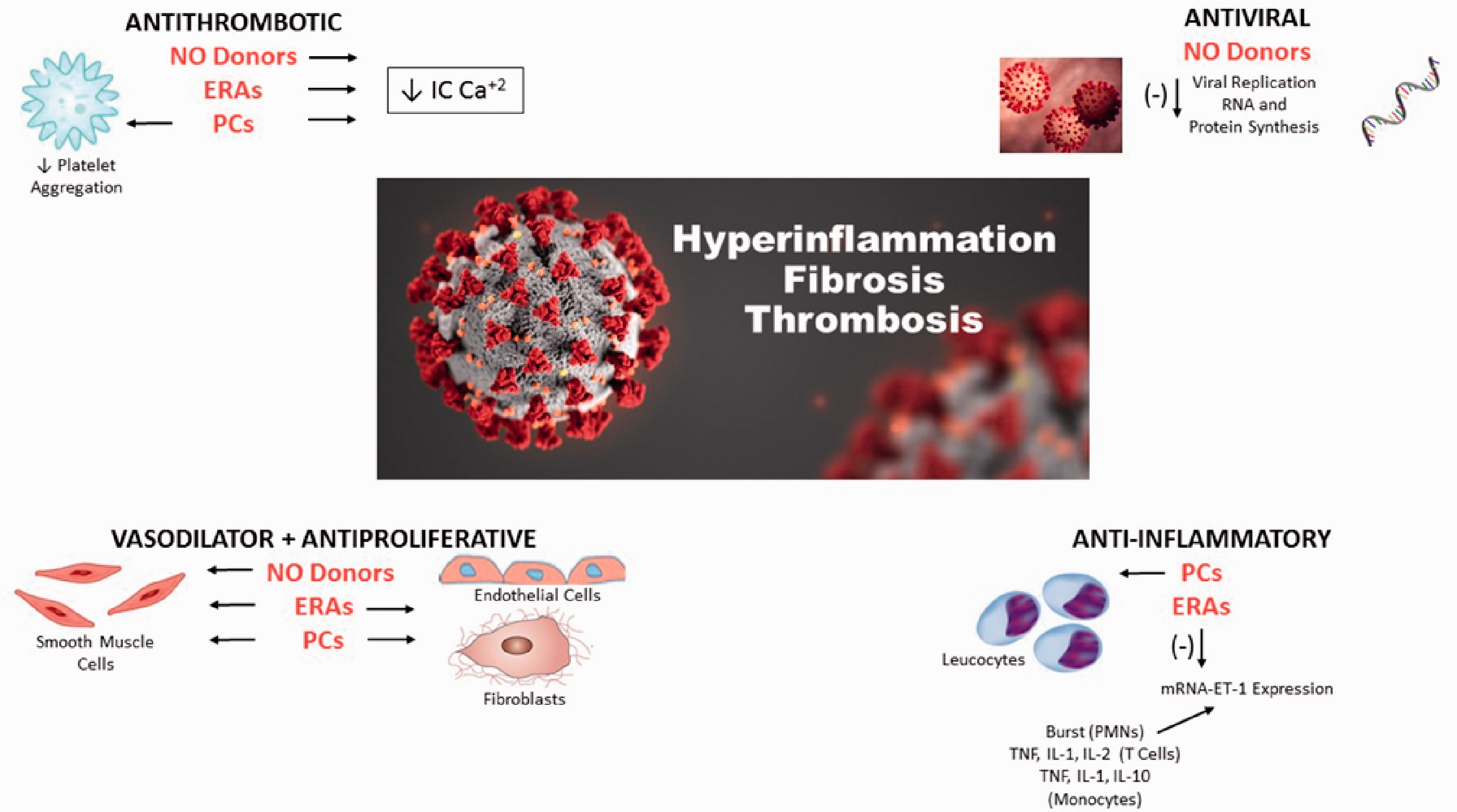
New class of PAH therapy under evaluation: vasoactive intestinal peptide
It is emerging as a critical regulator of tone and structural remodeling in the pulmonary circulation.3,65 VIP is being developed as adjunctive therapy for PAH given its vasodilatory, inotropic, and lusitropic properties. Mice lacking the gene for VIP exhibit moderate to severe PAH characteristics and administration of VIP to these animals attenuated vascular remodelin and RV hypertrophy. It also inhibits proliferation of pulmonary vascular smooth muscle cells in patients with idiopathic PAH. VIP’s immunomodulatory effects over TNF alpha, IL-1 B, IL-10, and IL-6, which are believed to contribute to cytokine-mediated acute lung injury and ARDS, 65 could provide significant benefit for COVID-19 patients.
Future COVID-19 research
The medical emergency created by this viral pandemic has unified global actions to produce therapies that improve survival. Current and ongoing treatment paradigms are aimed at mitigating severe COVID-19 disease utilizing several key targets: (1) ARDS prevention and treatment; (2) mitigating post-ARDS lung fibrosis; (3) reversing or preventing coagulopathy and microthrombi; (4) enhancing anti-viral effects. PAH-specific therapeutics offer potential solutions to many of these aforementioned key targets. In fact, there are now more than 10 clinical trials utilizing various PAH specific therapeutics (iNO, inhaled epoprostenol, and VIP) in patients with severe respiratory failure (clinicaltrials.gov) associated with COVID 19, as well as a proposed scientific registry looking at the effects of COVID-19 on PAH patients. The designs of some of these innovative trials are highlighted below.
A double-blind, placebo-controlled study is being launched to assess the efficacy and safety of inhaled epoprostenol delivered via dedicated delivery system (VentaProst from Aerogen Pharma) in subjects with COVID-19 requiring mechanical ventilation. Patients will receive continuous, inhaled epoprostenol via mechanical ventilator ∼3.5–30.5 ng/kg/min for 10 days. The primary endpoint will be efficacy and safety, with particular attention to reduction in the need for ECMO, time on ventilator, time in the intensive care unit, and prevention of hemodynamic collapse.
An open label study to assess the efficacy and safety of pulsed iNO was designed for subjects with COVID-19 requiring supplemental oxygen. It will evaluate if iNO ∼20 ppm, utilized for 5–14 days, prevents progression of respiratory disease and the requirement of mechanical ventilation (Bellerophon). The proprietary INOpulse® technology utilizes high concentration pulses to ensure a precise and constant dose regardless of a patient’s respiratory rate or inspiratory volume. The pulsatile technology enables dose titration and allows much higher doses/concentrations than currently available in hospital-based systems, as well as reduces the overall size of the therapeutic device. The potential benefits of prostacyclins and iNO in COVID-19 have been extensively discussed in this manuscript and are promising therapeutics in this disease.
Lastly, the efficacy of weekly VIP subcutaneous injections in prevention of severe respiratory failure / ARDS will be evaluated in a randomized, double-blind, parallel group, phase 2 study in hospitalized subjects with COVID-19 requiring oxygen supplementation (PB1046 VANGARD COVID-19 study). The medication will be given for a maximum of four weeks and could be administered to outpatient as well.
Footnotes
Authors’ contributions
Conception and design were performed by VF, RLB, EAB. Introduction: VF, RLB, EAB. Nitric oxide: VF, RLB, EAB, AS, SR. Endothelin receptor antagonists: VF, RLB, EAB, RB, SR. Prostacyclins: VF, RLB, EAB, LTL, SR. Drafting the manuscript for important intellectual content and final revision: VF, RLB, EAB, SR, AS, LTL, CJD, JSS, RB.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: VF, RJ, CJD, JSS -- research support UT, Bayer, Actelion, PhaseBio, Liquidia RB -- speaker / advisory boards from Bayer, MSD, Dompe, Galenica, GSK, Actelion, Ferrer, AOP, UT RLB -- research support UT, PhaseBio, Liquidia, Cerano, Abbott.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by NIH K08HL148701 (EAB).
