Abstract
Intravascular foreign body deposition in the form of talc or microcrystalline cellulose is an uncommon but increasing cause of pulmonary hypertension given the current opioid epidemic. Earlier cases describe the effect of talc introduced via intravenous injection of crushed pills when deposited throughout the lungs, typically in the capillaries or distal pulmonary arterioles. An angiogranulomatous reaction ensues with pulmonary vascular remodeling and the gradual development of pulmonary hypertension. Although the use of talc in the manufacture of tablets has largely been replaced with alternative inert binders including microcrystalline cellulose, a similar angiogranulomatous reaction and vascular remodeling can occur. We report a case of intravascular microcrystalline cellulosis that rapidly progressed to fatal pulmonary hypertension over months characterized by occlusion of more proximal pulmonary arterioles in an intravenous drug user.
Case report
A 26-year-old woman with a history of intravenous drug use and recent Methicillin-Resistant Staphylococcus Aureus (MRSA) osteomyelitis on intravenous antibiotics via a peripherally inserted central catheter (PICC) presented from a nursing facility to an outside hospital with fever and syncope. Her initial diagnostic evaluation was concerning for a catheter-related blood stream infection and sepsis and she was administered antibiotics and fluids. Shortly after fluid resuscitation, she developed hypoxia and shock requiring vasopressors. An echocardiogram revealed severe pulmonary hypertension (PH) with a right ventricular systolic pressure (RVSP) estimated at 88 mmHg and a severely enlarged right atrium and right ventricle (RV) with septal flatting consistent with RV volume and pressure overload. She clinically decompensated and was transferred to our medical intensive care unit. Diuresis resulted in hemodynamic improvement and a repeat echocardiogram showed RVSP had improved to 55 mmHg, but with severely reduced RV function (Fig. 1a).
(a) Four-chamber echocardiographic view demonstrating severely dilated RV with septal bowing. (b) Four-chamber echocardiographic view demonstrating normal size of all cardiac chambers taken two months prior to presentation. (c) Computed tomography demonstrating massively dilated main pulmonary artery and diffuse micro-nodularity. (d) Right lung cut section showing numerous centrilobular nodules consisting of foreign material emboli. (e) 40× H&E stain: medium artery with foreign material embolus, with associated giant cell reaction and acute inflammation. (f) Microcrystalline cellulose in a medium artery under polarized light.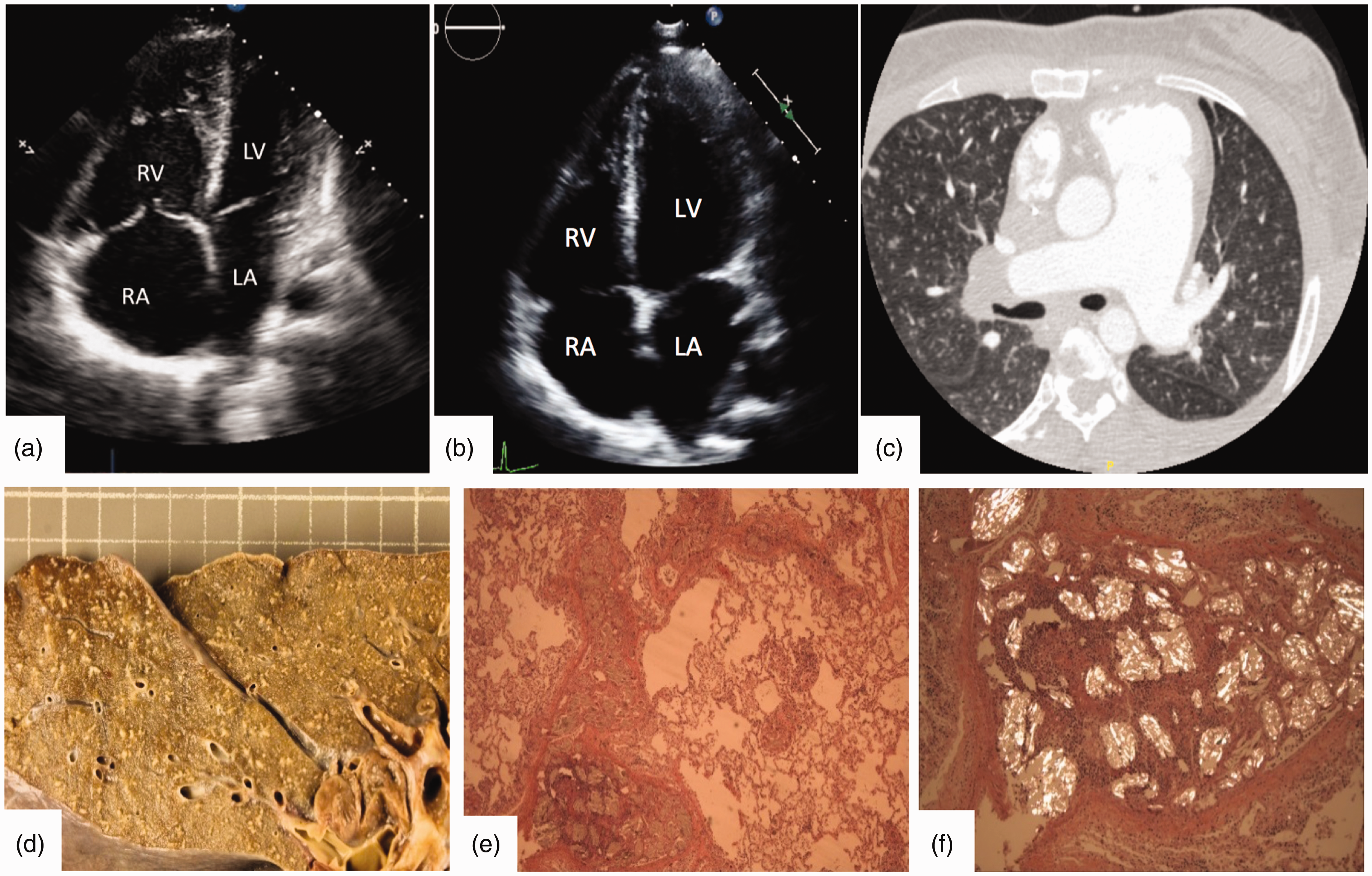
A previous echocardiogram performed two months prior to admission to evaluate for endocarditis demonstrated normal RV size and function with an RVSP of 19 mmHg (Fig. 1b). Computed tomography (CT)-angiogram demonstrated a markedly enlarged main pulmonary artery as well as extensive bilateral pulmonary micro-nodularity with scattered macroscopic nodules suggestive of talc granulomatosis (Fig. 1c). On further questioning, she reported allowing friends to inject crushed pills into her PICC while she was being treated at the nursing facility. On hospital day two, she developed acute onset bradycardia that progressed to asystole. Attempts at resuscitation failed. Post-mortem analysis revealed extensive pulmonary foreign body embolism involving small to medium arteries with occasional segmental and sub-segmental intraluminal involvement. Foreign material was also seen within the intimal layer of the vasculature with associated giant cell reaction (Fig. 1d and e). The material was Congo red positive, suggestive of microcrystalline cellulose (MCC) (Fig. 1f).
Discussion
We describe a case of rapidly progressive PH secondary to injection of crushed pills through a PICC line. The insoluble particulate matter occluded the capillary and distal arteriole beds, as has been described previously in cases of foreign material intravascular deposition. Unlike previously reported cases of foreign body granulomatosis associated with intravenous injection of crushed pills,1–3 our case was characterized by rapid progression from no detectable disease to wide spread occlusion of the pulmonary vascular bed and death from right heart failure within months of illicit drug use through her central catheter. This likely occurred due to the occlusion of more proximal pulmonary arteries from larger particle size afforded by the larger lumenal diameter of the central line. Although fatal PH due to intravascular foreign body embolism has been described, 3 most cases take many years to develop due to the high number of crushed tablets that are needed to obliterate the pulmonary microcirculation. The slow, more typical development of PH in intravenous drug abusers may be challenging to recognize. However, as seen here and in previous reports,3–5 the echocardiographic demonstration of RV dysfunction coupled with the CT demonstration of micronodularity, and mosaic attenuation, in a patient at risk for intravenous injection should raise a clinician’s suspicion of this process. While there is no clear treatment, cessation of exposure should be encouraged in an attempt to avoid progression to life-threatening disease. To our knowledge, the rapid progression of severe disease, involvement of larger vessels, and deposition of MCC eventually leading to death as seen in this case has not been previously reported in intravenous drug users. A previous case report outlines a similar rapid development of PH and death in a young patient receiving Total Parental Nutrition (TPN) from deposition of MCC, 4 the crystals identified in this case report. According to several pharmaceutical references, MCC is often an inert binder in pill preparation.6,7 The present case illustrates the potential danger of intravenous pill injection through a central line due to the larger particle size compared to traditional needles used for injection of powdered drugs or crushed tablets and adds to the literature outlining the different substances that may cause an angiogranulomatous reaction leading to the development of PH, either indolently or rapidly. These may be important considerations with increased outpatient and chronic infusion therapy in the context of the opioid epidemic.
