Abstract
This study aimed to explore the correlation of sodium ferulate and the renal protective effect on computed tomography pulmonary angiography in patients suffering from pulmonary hypertension. This prospective study enrolled 92 consecutive patients with pulmonary hypertension diagnosed by echocardiography, and all included patients underwent computed tomography pulmonary angiography after admission. The participants were randomized, divided into sodium ferulate group (n = 49) and control group (n = 43), of which patients in the sodium ferulate group received intravenous sodium ferulate 3.0 g per day from 12 h before computed tomography pulmonary angiography examination to 72 h after that, and patients in the control group were provided with routine treatment. Renal function was assessed by measuring serum creatinine, estimated glomerular filtration rate, Cystatin-C as well as 24 h, 48 h, and 72 h after computed tomography pulmonary angiography, followed by the calculation of the incidence of contrast-induced nephropathy for contrast-induced nephropathy and non-contrast-induced nephropathy grouping. Besides, renal resistive index was determined via Doppler ultrasound examination before, after 1 h and 24 h after computed tomography pulmonary angiography. There were no significant differences between the two groups in serum creatinine at baseline and 24 h after computed tomography pulmonary angiography (P > 0.05, respectively), but at 48 h and 72 h, it was lower in the sodium ferulate group (P < 0.05). There were no significant differences of estimated glomerular filtration rate between the two groups (P > 0.05). The level of Cystatin-C at 48 h and 72 h after computed tomography pulmonary angiography was lower than in the sodium ferulate group (P < 0.05). Contrast-induced nephropathy was identified in nine patients (9.78%). Sodium ferulate was associated with a decline in the incidence of contrast-induced nephropathy (4.08 vs. 16.28 %, P < 0.05). Compared to patients with contrast-induced nephropathy, lower renal resistive index were observed at 1 h and 24 h after computed tomography pulmonary angiography in patients without contrast-induced nephropathy (P < 0.05). Infusion of sodium ferulate before and after computed tomography pulmonary angiography was associated with a decline in incidence of contrast-induced nephropathy.
Keywords
Introduction
Pulmonary hypertension (PH) represents a progressive and destructive heterogeneous disease, which is induced by multiple factors that can cause progressive increase of pulmonary vascular resistance leading to right ventricular dysfunction and even sudden death. According to the characteristics of pathology, hemodynamics, clinical diagnosis, and treatment strategies, PH can be divided into five categories of arterial PH, PH caused by left heart disease, PH caused by hypoxia and/or pulmonary disease, chronic thromboembolic PH, and other PH of unknown mechanisms. On account of its high morbidity and mortality, people have kept an eye on it in recent decades increasingly. The diagnosis of PH can be confirmed traditionally by ECG, chest radiography, and Doppler echocardiography. The changes of right ventricular hypertrophy, overload, and enlargement of right atrium in ECG can be used as the basis for the diagnosis of PH. However, corresponding sensitivity and specificity for the diagnosis of PH are not high, other imaging approaches are required for the diagnosis of PH. Both multi-detector row computed tomography (CT) and magnetic resonance imaging have become complementary investigations in the evaluation of patients with suspected PH. 1 Meanwhile, CT pulmonary angiography (CTPA) examination is an important step in the process of finding the cause of PH, and various studies have demonstrated its imaging value in patients with suspected PH in the aspect of diagnosis, differential diagnosis, disease severity identification, etc.,2–4 with which attention shall be paid to the selection of high-quality contrast media (CM), selective injection of pulmonary arteries, and multi-angle observation. In view of the characteristic of the disease itself, and the application of CM, the risk of contrast-induced nephropathy (CIN) is greatly increased.
Contrast-induced acute kidney injury (CI-AKI) is defined as a rise in serum creatinine (SCr) of at least 0.5 mg/dL or 25% increase from baseline within 48–72 h after contrast exposure, and rule out the other reasons, known as CIN. Studies have shown that acute kidney injury (AKI) triggered by CIN accounts for 11% of the total cases, becoming the third most important cause of iatrogenic AKI. 5 CI-AKI is associated with patients’ mortality. Some studies have suggested that a potential interaction between oxidative stress, inflammation, reduction in renal blood flow, and direct damage to tubular cells by CM may be involved in CIN pathogenesis. 6 CM-induced alterations in renal microvascular hemodynamics are considered to be one of the mechanisms in the development of CIN. 7 The renal resistive index (RRI) is one of the most sensitive parameters in renal pathology and reflects alterations in renal plasma flow. 8 In this regard, we anticipate whether RRI can be considered as a marker of CIN.
In recent years, most studies have focused on the relation of CIN after percutaneous coronary intervention (PCI), but put too little emphasis on CTPA. In general, the usage of CM volume was apparently lower than that of PCI during CTPA. However, due to the different pathogenesis in PH compared with coronary heart disease, increased pulmonary artery pressure may lead to right heart failure (RHF) and systemic congestion, and the use of diuretics can affect the kidney function as well. So far, there are rare clinical studies focusing on the incidence of CIN in this cohort. Notably, it is of great significance to explore the preventive strategy considering that CIN is reversible in pathogenesis and curable in treatment.
Ferulic acid is an important active constituent identified in medicinal herbs Radix Angelica Sinensis and Ligusticum chuanxiong hort, 9 and sodium ferulate (SF) is the sodium salt of ferulic acid. Some studies have demonstrated that SF can reduce the injury of ischemia and reperfusion to protect the heart. Although SF exhibit beneficial effects in many diseases, such as diabetic nephropathy, whether it has positive effects on renal protection of PH is still obscure. In the present study, experiments were designed to investigate the renal protective effects of SF administration on patients with PH receiving CTPA.
Methods
From July 2018 to September 2019, a total of 92 consecutive PH patients were enrolled for exploration in the Cardiology Department of the Second Hospital of Hebei Medical University, all of which were diagnosed by echocardiography undergoing CTPA examination, with right heart catheterization (RHC) as the gold standard. Eligible patients were further randomly divided into two groups by means of random number table, namely, the SF group and the control group (CON group). There were 49 patients in the SF group who were provided with intravenous drip of 0.3 g SF (SF injection, SF dihydrate 100 mg/5 ml, Changchun Fuchun Pharmaceutical Co., Ltd) after dilution, once a day from 12 h before CTPA examination to 72 h after that. In the CON group, the 43 patients were given conventional treatment (including oxygen, furosemide, antisterone, potassium chloride, digoxin, etc.). SCr concentrations, estimated glomerular filtration rate (eGFR), Cystatin-C (Cys-C) and calculated CIN incidence were tested at admission, 24, 48, and 72 h after CTPA examination. During examination, all patients were provided with nonionic and low-permeability CM (Ultravist 370, iodine 370 mg/ml, Schering Pharmaceutical Ltd). CIN was defined as an increase of SCr of 25% or 0.5 mg/dL (44 micmol/L) at 72 h after operation compared with the baseline level. All patients underwent Doppler ultrasound examination to determine RRI before, after 1 h, and 24 h after CTPA, and then it was compared within CIN group and non-CIN group.
Inclusion criteria
Patients with estimated tricuspid regurgitation velocity (TRV) >3.4 m/s 10 and/or pulmonary systolic pressure >50 mmHg by using Doppler echocardiography. 11
Exclusion criteria
(1) Patients with severe respiratory failure, cardiogenic shock, arrhythmia or acute myocardial infarction, and other hemodynamic instability. (2) Patients who were allergic to CM or SF, or with severe liver and kidney diseases, and those who were not suitable for CTPA examination. (3) Patients with severe hypotension, systolic blood pressure < 90 mmHg, or who were unable to receive CTPA examination for other reasons. All examinations were performed by the same experienced physician.
This study was approved by the Ethical Committee of the Second Hospital of Hebei Medical University and performed in accordance with the Declaration of Helsinki. Written informed consents were obtained from all patients before enrollment.
Data collection
Data collection included the baseline demographics about age, sex, body mass index, medical history, WHO functional class, left ventricular ejection fraction, SCr level at admission, 24, 48, and 72 h after admission, and renal color ultrasound calculation of RRI. The eGFR was calculated by simplified modification of diet in renal disease study equation: eGFR = 186 × SCr – 1.154 × age – 0.203 × (0.742 if female). The incidence of CIN was calculated.
Statistical analysis
Statistical analysis was performed using SPSS statistical software (Version 25.0, IBM, Armonk, NY, USA) and GraphPad Prism software (Version 8.0, GraphPad Software Inc., La Jolla, CA, USA). Continuous data were presented as mean ± standard deviation, while categorical data were expressed as number (percentage of patients). Comparisons of continuous variables between CON and SF groups were made using independent sample t test, and Chi-square test or Fisher exact test for categorical data. Repeated-measures analysis of variance was applied to describe the changes of SCr and eGFR over time between groups. P < 0.05 was considered that the difference was statistically significant.
Results
Comparison of baseline data between groups
Baseline characteristics of enrolled patients.

BMI: body mass index; HR: heart rate; SBP: systolic blood pressure; DBP: diastolic blood pressure; NT-pro-BNP: N-terminal pro-B-type natriuretic peptide; HCY: homocysteine; BUN: blood urea nitrogen; SCr: serum creatinine; eGFR: estimated glomerular filtration rate; UA: urea acid; Cys-C: Cystatin-C; PO2: partial pressure of oxygen; PCO2: partial pressure of carbon dioxide; SaO2: oxygen saturation of blood; LA: left atrium; LV: left ventricle; RA: right atrium; RV: right ventricle; LVEF: left ventricular ejection fraction; sPAP: systolic pulmonary artery pressure; TAPSE: tricuspid annular plane systolic excursion; TRV: tricuspid regurgitation velocity; TRPG: tricuspid regurgitation pressure gradient; CM: contrast medium; WHO-FC: WHO functional class; SF: sodium ferulate; CON: control; PH: pulmonary hypertension.
Changes of renal function
Changes of SCr and eGFR.
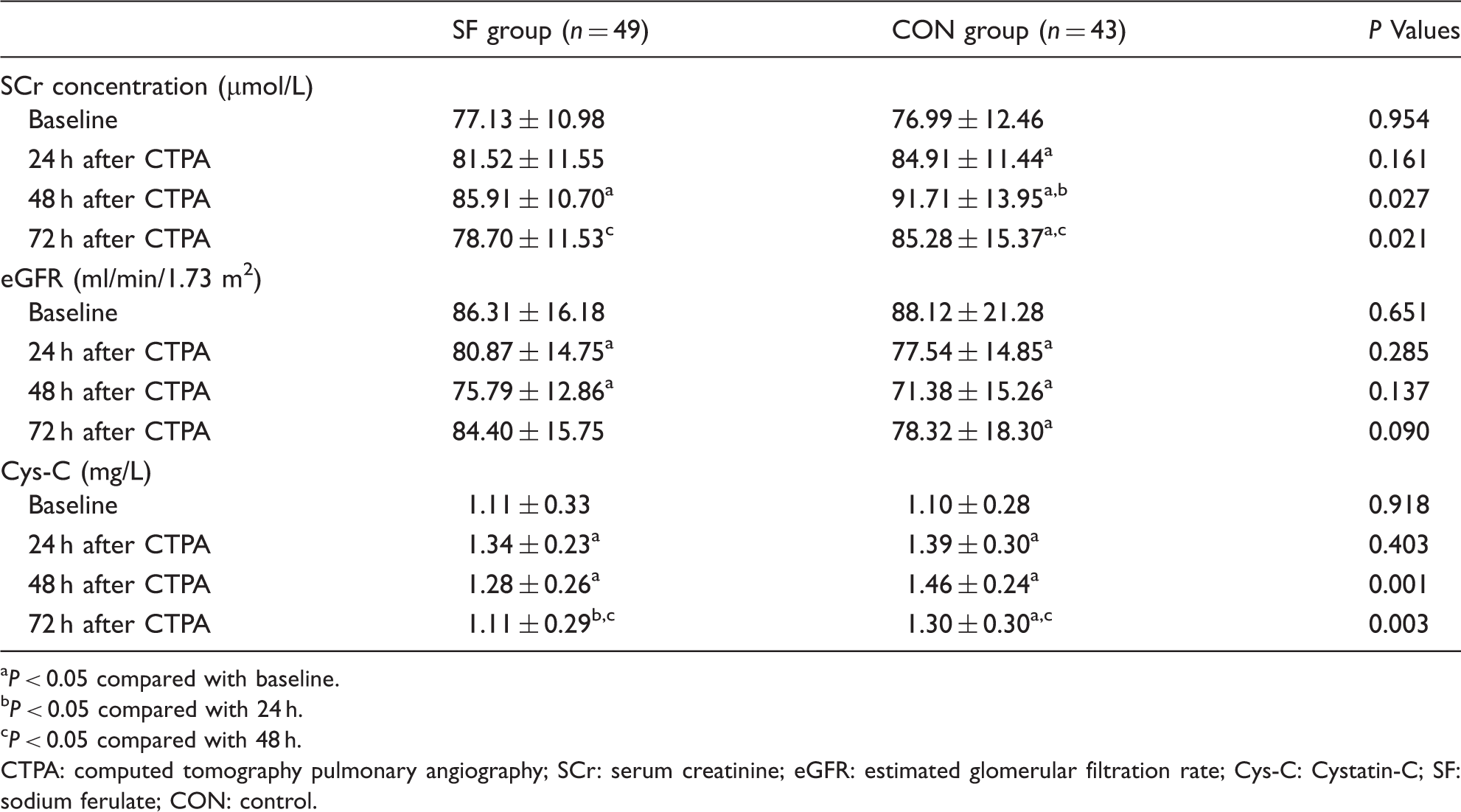
P < 0.05 compared with baseline.
P < 0.05 compared with 24 h.
P < 0.05 compared with 48 h.
CTPA: computed tomography pulmonary angiography; SCr: serum creatinine; eGFR: estimated glomerular filtration rate; Cys-C: Cystatin-C; SF: sodium ferulate; CON: control.
Incidence of CIN
Incidence of CIN at 72 h after CTPA examination.
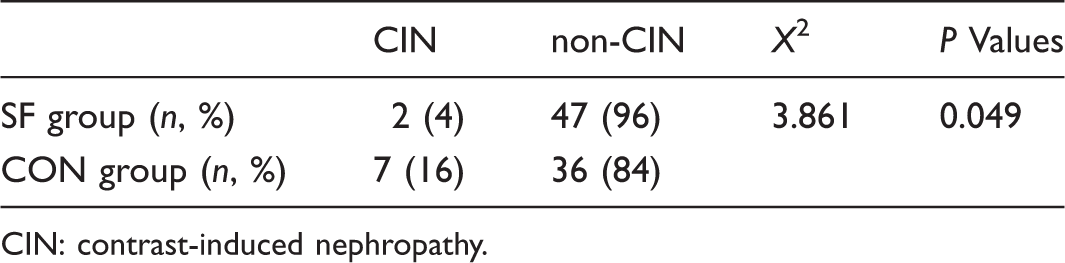
CIN: contrast-induced nephropathy.
Compared the RRI
Comparisons between and within groups in terms of RRI at different times.
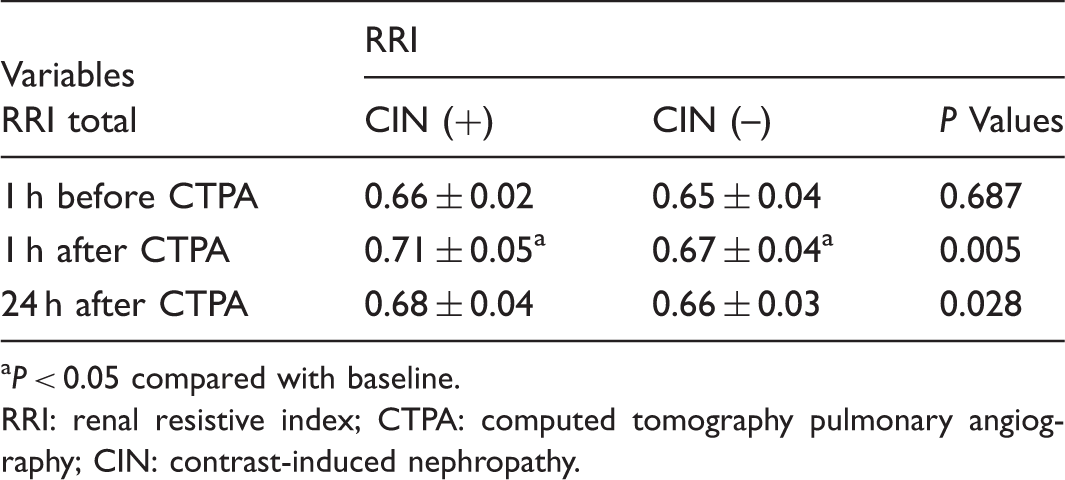
P < 0.05 compared with baseline.
RRI: renal resistive index; CTPA: computed tomography pulmonary angiography; CIN: contrast-induced nephropathy.
Discussion
PH is a potentially fatal disease and a cardiovascular syndrome affecting the right heart, which is characterized by pulmonary vascular remodeling, increased pulmonary arterial pressure, and right ventricular hypertrophy. The consequences of PH can be devastating, and PH can be caused by a variety of causes. With the increasing demand for physical examination and interventions based on the use of contrast agents, the incidence of CIN after CTPA is significantly increasing within PH patients, which may be related to RHF causing renal congestion, resulting in decreased renal effective circulating blood volume, and even acute kidney injury. Kriechbaum et al. revealed that patients with thromboembolic pulmonary hypertension underwent balloon pulmonary angioplasty treatment, the eGFR correlated moderately with right atrial pressure and N-terminal pro-B-type natriuretic peptide (NT-pro-BNP) at baseline but not with cardiac index, which interpret that venous congestions can be considered as a predominant role to induce the change of renal function. 12 RHF known as venous congestion may induce renal hypoperfusion and congestion, and has been reported to be the major underlying cause for renal dysfunction. 13 However, such renal injury is mostly reversible, which highlight the necessity of individualized risk-benefit strategy.
In recent years, a variety of preventive measures has been suggested to reduce the incidence of AKI, among which the greatest potential is found in the administration of natriuretic peptide, fenoldopam and dexmedetomidine. 14 For example, Mamoulakis et al. declared drugs such as sildenafil, tadalafil, vardenafil, and avanafil can act as protection against CIN to enhance the vasodilatory effect of released nitric oxide. 15 Meanwhile, Qian et al. reported in their research that prophylactic nitrates with matched adequate hydration is an effective strategy for chronic kidney disease (CKD) and chronic heart failure (CHF) patients to prevent CIN. 16 Furthermore, recombinant human brain natriuretic peptide (rhBNP) is effective in decreasing the incidence of CIN in patients suffering from primary PCI, 17 and acetylcysteine can be used to protect against CIN. 18 Ali-Hasan-Al-Saegh et al. pointed out that when the patients were provided with adequate hydration plus ascorbic acid, the incidence of CIN decreased significantly. 19 For example, Zhang B et al. 20 carried out a meta-analysis focusing on the effect of sodium bicarbonate in preventing CIN. In their study, patients were diagnosed with pre-existing renal insufficiency, and hydration with sodium bicarbonate was associated with a significant decrease in CIN in the targeted population, with no significant effect in lowering mortality yet.
Andreucci et al. pointed out that AKI is induced by multifactorial postoperatively, including renal ischemia, particularly in the medulla, reactive oxygen species (ROS) formation, reduction of nitric oxide production, and tubular epithelial and vascular endothelial injury. 21 Caiazza et al. pointed out that CM may induce hemodynamic alterations, resulting in renal medullary hypoxia, and direct toxicity on renal tubular epithelial cells seem to be major factors contributing to CIN. 22 The usage of CM may induce decreasing production of local prostaglandin-mediated vasodilatation and the damage caused by oxygen radicals. 23 SF is a sodium salt of ferulic acid (3-methoxy-4-hydroxy-cinnamate sodium), acts as a potent antioxidant by scavenging ROS and enhancing cell stress response through the upregulation of cytoprotective systems, such as heme oxygenase-1, superoxide dismutase, catalase, and Hsp70. 24 As evidenced by one prior study, ferulic acid could circumvent oxidative stress-mediated renal cell damage, which displayed significant function in hypoglycemic, antioxidant, anti-inflammatory, anti-apoptotic activities, and in autophagy, 25 SF is the sodium salt of ferulate acid. In our research, we intended to study the protective effect of SF on renal function of patients with PH. Chowdhury et al.’s findings suggested that ferulic acid could significantly ameliorate oxidative stress-induced renal tissue impairment and apoptosis by inhibiting ROS generation, nuclear factor kappa B (NF-κB) activation, stress signaling pathway (p38, JNK, ERK 1/2) activation, and by promoting autophagy, which revealed the molecular mechanisms by which ferulic acid exerted its protection against hyperglycemia-induced renal dysfunction under diabetic pathophysiology. 25
Ferulic acid has the property such as anti-inflammatory, antidiabetic, antiaging, anticancer, neuroprotective, etc., which relies largely upon their cell antioxidant potential. 26 Meanwhile, SF has the auxiliary ability to decrease the pulmonary pressure, which can improve heart failure, reduce the heart after-load be reduction and kidney congestion combined with the addition of conventional drug therapy. In the present study, the kidney function recovered fast to the baseline in patients of the SF group. McDonald et al. found no difference in AKI rates between enhanced CT and unenhanced CT patient. 27 However, an opposite result was reported in our study, which may be attributed to the reason that patients with PH are vulnerable subgroups within general population. Considering that heart failure and renal congestion are common complications with PH, CM exposure increased the incidence of AKI significantly.
In some clinical cases, RRI showed an independent and incremental role in predicting HF progression and it suggested the usefulness of RRI in better defining renal impairment in cardio-renal syndrome. 28 To understand the meaning of these results and the role of RRI in CHF patients and in the cardio-renal syndrome setting, the strong association between RRI and central venous pressure, observed in these and other previous data from the literature, has to be considered. 29 Hetzel et al. revealed that RRIs rose transiently after the administration of CM and then decreased progressively to baseline values. 30 It is consistent with the results of this study, which may be attributed to the benefit effect of SF and the relief of the heart function.
This study shows that SF has a protective effect on renal function in patients with PH after CTPA examination. After SF infusion, renal function damage was small and recovery was better in treated patients than that of the CON group. There was no obvious adverse reaction found in the experiment. The incidence of CIN in SF group was also lower than that in CON group. SF can significantly restore the parameters of SCr changed by CM to the baseline level at admission. For the above interpretation, timely application of SF may have a positive role in reducing the occurrence of CIN after CTPA examination.
Research limitations
First, it was a single-center study with a relatively smaller sample size of patients with PH. Second, the true incidence of CI-AKI may be overestimated that requires further verification. Some patients may have easily met the diagnostic criteria for CIN (a relative rise of SCr ≥ 25%) after CM exposure, especially when the baseline SCr was relatively low. In addition, SCr values could have been affected by hemodynamic changes in the setting of PH patient complication with RHF. Third, our study focused on the monitoring of renal function markers and the protective role of SF on CIN, however, we failed to record the evidence of renal impairment in the enrolled patients, there may be a requirement to explore the role of SF in patients with renal impairment and its effect on mortality clinically as well, which will in turn highlight the research value of this topic. Furthermore, a single dose of SF was used in our experiment, whether there is a consistent curative effect of SF at different dosages of administration remains to be explored in future study with larger sample size and different dosage grouping.
