Abstract
The present study aimed to propose the pulmonary hypertension for predicting left ventricular dysfunction in adults after patent ductus arteriosus closure. A total of 183 patients (age ≥18 years) after patent ductus arteriosus occlusion were retrospectively collected in this study. In brief, pre-, post-procedure and short-term follow-up transthoracic echocardiography were performed. Simpson’s method was used to measure the left ventricular ejection fraction (LVEF), and LVEF less than 50% after procedure was utilized as a criterion to identify left ventricular dysfunction. As a result, 36 (19.67%) patients developed newly identified left ventricular dysfunction. The rate of newly identified left ventricular dysfunction was significantly higher in moderate or severe pulmonary hypertension groups compared to the groups of mean pulmonary artery pressure (mPAP) <25 mmHg (P < .001). Logistic regression analysis showed that elevated mPAP ( ≥25 mmHg) was an independent predictive value for newly identified left ventricular dysfunction (OR = 3.584, 95%CI: 1.186–10.832, P = .024) after adjusting confounders. The ROC curve revealed a good discrimination power for predicting newly identified left ventricular dysfunction (AUC = 0.924, 95%CI: 0.885–0.963, P < .001). Taken together, newly identified left ventricular dysfunction after patent ductus arteriosus closure was prevalent in patients with elevated mPAP. The pre-procedure elevated mPAP is an independent risk factor for the prediction of the newly identified left ventricular dysfunction in adult patients undergoing percutaneous patent ductus arteriosus closure. It is feasible to propose a risk model for predicting post-procedure left ventricular dysfunction and a heart function monitoring in pulmonary hypertension patients.
Introduction
Patent ductus arteriosus (PDA) is defined as a congenital heart disease (CHD) with a persistent communication between the pulmonary artery (PA) and descending aorta. The percutaneous device closure has been proven as a safe and effective therapeutic approach compared with the surgery in most adult patients.1–3 Previous studies have also found an impairment of left ventricular function in children and adult patients undergoing PDA closure,4–6 which is known as newly identified left ventricular systolic dysfunction (LVD) resulting from a sudden closure of flow shunt. The post-procedure heart failure has also been reported in individual case or small clinical trial.7–9 However, there is a lack of reliable prediction model.
Pulmonary hypertension (PH) has long been reported in PDA patients in previous studies. A PH patient with PDA is burdened with pulmonary circulation overload, namely a high ratio of pulmonary blood flow to systemic blood flow. 10 A left ventricular (LV) volume overload is considered to subsequently increase LV volume and ejection fraction (EF) in accordance with the Starling’s law. 11 Compared with neonates or infants, cardio-pulmonary circulation of PDA is changed in adults. 12 The PH is considered to be related to left heart disorder in various diseases.13–15 However, it remains largely unknown whether the PH can predict the LVD after proper closure of PDA in adult patients.
Accordingly, this study was designed to investigate the clinical characteristics of newly identified LVD in PDA adult patients following percutaneous closure. Intriguingly, there is a prevalence of LVD among PH patients after procedure. We also aimed to identify the underlying association between pre-procedure elevated mean pulmonary artery pressure (mPAP) and post-procedure LVD.
Methods
Study population
The transthoracic echocardiogram (TTE) results were retrospectively screened from patients aged over 18 years in echo system of Guangdong Cardiovascular Institute (Guangzhou, China) from June 2015 to June 2018. In total, 375 patients were enrolled with multiple TTE results. After excluding the patients who only had pre- or post-procedure TTE examination (114), without PDA closure procedure (71), and with pre-procedure LVD (baseline LVEF <50%) (6), missing of documents (1), 183 patients were finally included in the final analyses. None of the patients were diagnosed with Eisenmenger. Trained clinical research coordinators were employed for data collection.
Procedure
This study was approved by the institutional ethics committee. Pre-procedure TTE was examined within six months. On the first day at admission, the blood samples were collected. All patients signed the written informed consent for the percutaneous transcatheter closure treatment. The buttoned devices included Amplatzer (AGA Medical Corporation, Plymouth, USA), HeartR (Lifetech scientific, Shenzhen, China), and LZ (Visee medical service, Shandong, China) or Cardi-O-Fix (Starway Medical Technology, Beijing, China), which were selected according to the decisions taken by the chief operator. Before releasing the occluder, the pulmonary artery pressure was measured with TruWave (Edwards Lifesciences, Irvine, USA) sensor through the delivery catheter. Then, the mPAP was calculated based on the pressure result of the main pulmonary artery (Fig. 1). The post-procedure TTE results were examined within 10 workdays. All the TTE examinations were performed by professional technicians. The parameters were measured by using the color Doppler imagining machine in our institution. Simpson’s method was used to calculate the LVEF. After a whole review of documents, a median follow-up of 37 (quartile: 34, 42) day post-procedural TTE of 108 patients was recorded.
The angiogram pictures during procedure and mPAP measurement plot. (a) The typical position of the catheter in the pulmonary artery and descending aorta; (b) the angiogram of PDA between the aorta artery (AO) and pulmonary artery (PA) in right front inclined projection before the occluder release (indicated by the arrow); (c) the example of pressure curve plot to measure the mPAP. The X axis indicates the time during procedure and the Y axis indicates the values of PAP; (d) the angiogram in right front inclined projection after the occluder release.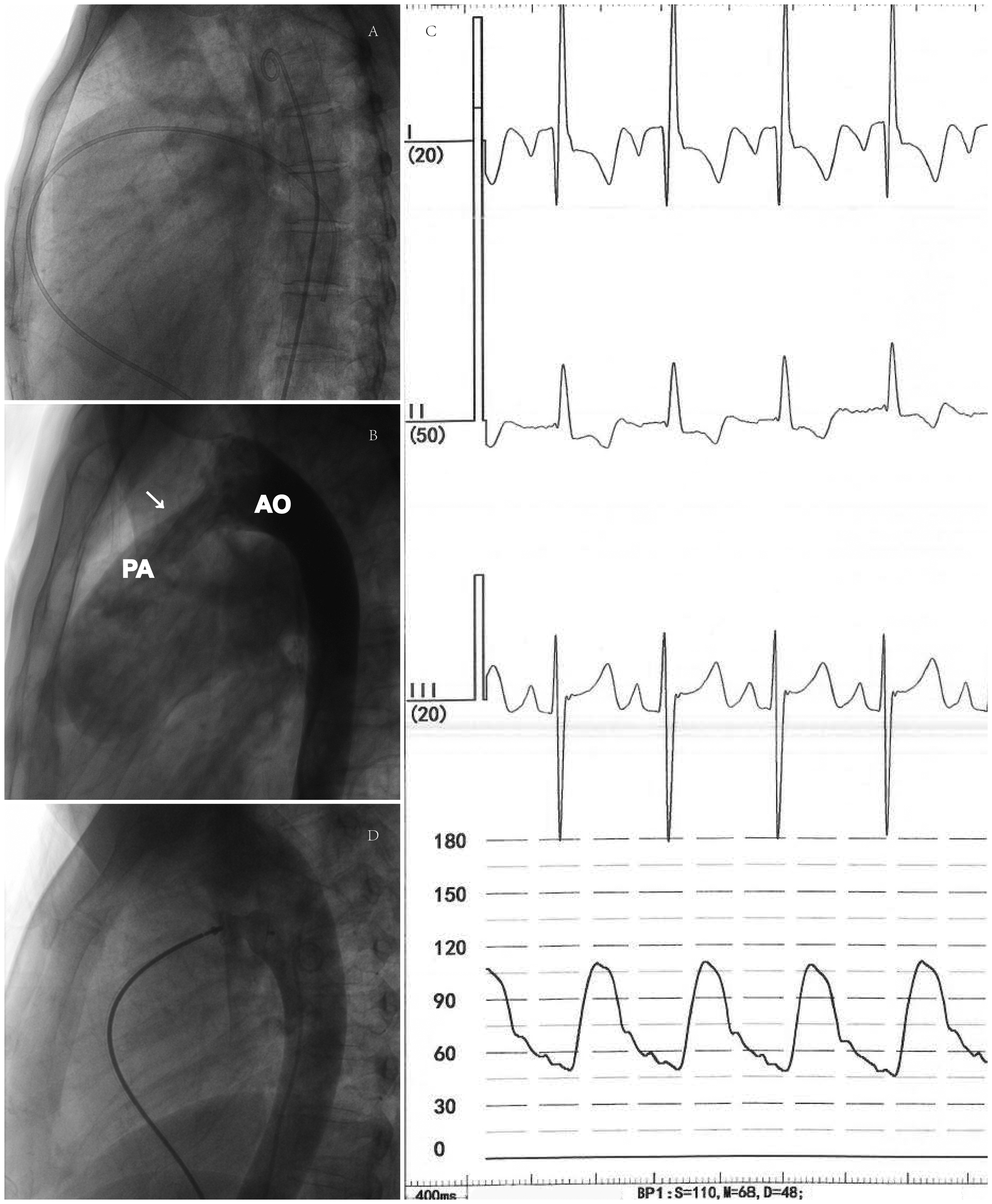
Definition of outcomes
An mPAP ≥25 mmHg was defined as PH. Newly identified LVD was used as the primary end point in our study, which was defined as the post-procedure LVEF less than 50%. In order to detect the possible effect between different decreased LVEF levels, these levels were analyzed according to the median and 10% in our database. Thus, the secondary end points were defined as the LVEF decrease by more than 5% and 10%, respectively. Furthermore, we use the post-procedure new-onset symptoms of heart failure such as chest distress or shortness of breath which need anti-heart failure medication like digoxin or furosemide and hospitalization to evaluate the difference of clinical outcomes between patients with elevated mPAP and those without.
Statistical analysis
The comparison of the baseline variables of interest was performed according to the LVEF change quartile. Continuous variables were denoted as mean ± standard deviation. Category variables were denoted as number (proportions). One-way ANOVA analysis was conducted to compare the variables between multiple groups. To compare the outcomes of different mPAP groups, the least significant difference (LSD) was performed. In addition, Student’s t test and ANOVA analysis were used to compare the difference of in-hospital medicine, stay length and follow-up LVEF between the patients with elevated mPAP and those without. Forward stepwise multivariate stepwise logistic analysis (likelihood ratio) was performed to investigate the predictors of primary end point. Receiver operating characteristic (ROC) curve analysis was further conducted to identify the discrimination of model. The statistical analyses were performed using IBM SPSS Statistics 19.0 (IBM Corporation, Chicago, USA), R software version 3.5.0 (R Foundation for Statistical Computing, Vienna, Austria) and Prism 6 for windows version 6.02 (GraphPad Software, California, USA). A two-sided P < .05 was considered as statistically significant.
Results
Among the 183 patients recruited in this study, 133 PDA patients (72.7%) suffered an impairment of LVEF after undergoing the percutaneous device closure, 36 (19.67%) developed newly identified LVD. The LVEF decreased by −19.43 ± 5.472% ranged from 10 to 29%. There was no gender predilection in our cohort. The mean age was 37.65 years (range 18 to 73) with an index LVEF of 64.7% (ranged 50 to 78%). The mean size of PDA was 6.66 mm (range 1.4 to 17 mm), and the mean mPAP was 27.61 mmHg. In addition, 67 patients had a pre-procedure PH.
The clinical characteristics of different LVEF impairment level.
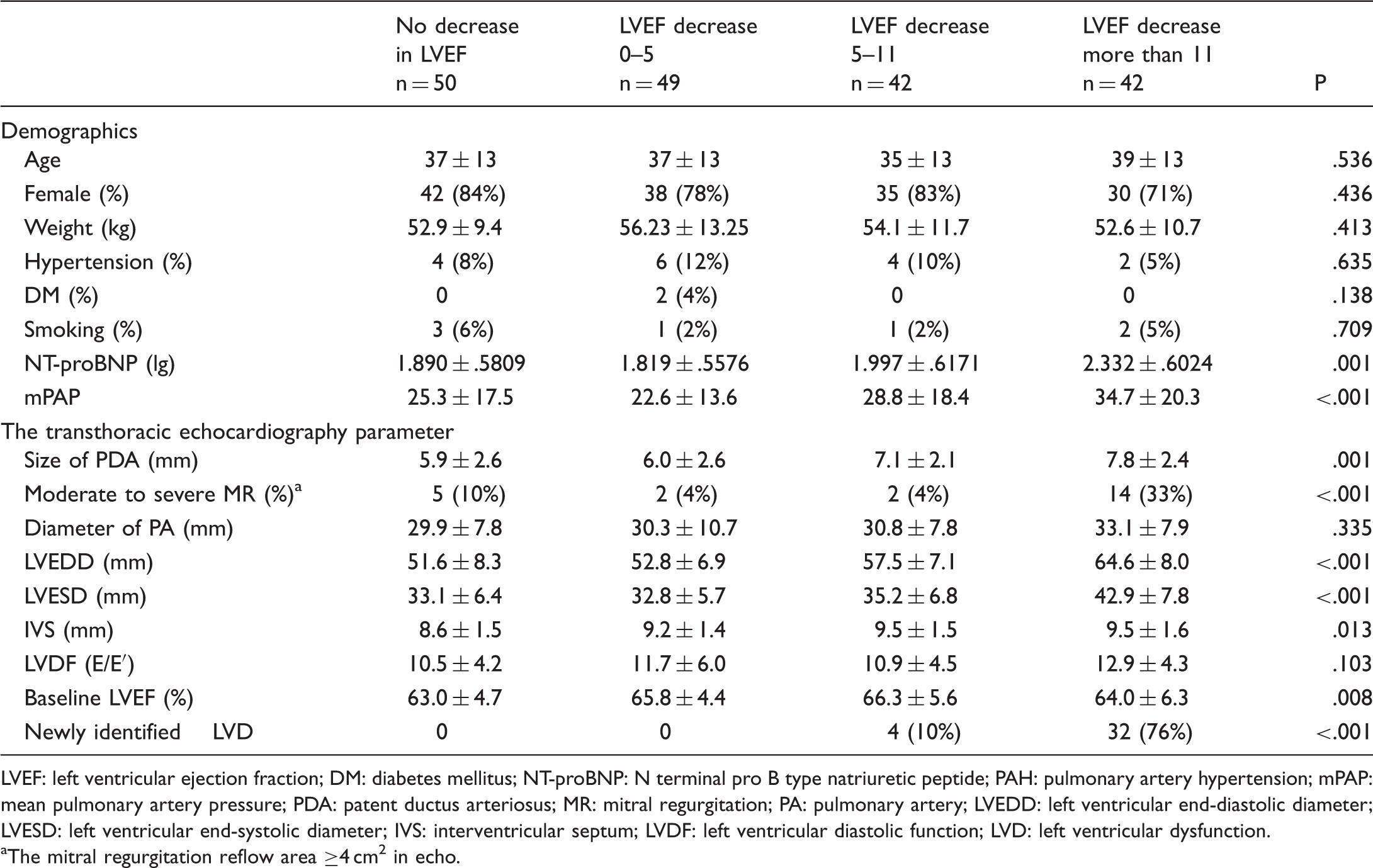
LVEF: left ventricular ejection fraction; DM: diabetes mellitus; NT-proBNP: N terminal pro B type natriuretic peptide; PAH: pulmonary artery hypertension; mPAP: mean pulmonary artery pressure; PDA: patent ductus arteriosus; MR: mitral regurgitation; PA: pulmonary artery; LVEDD: left ventricular end-diastolic diameter; LVESD: left ventricular end-systolic diameter; IVS: interventricular septum; LVDF: left ventricular diastolic function; LVD: left ventricular dysfunction.
The mitral regurgitation reflow area ≥4 cm2 in echo.
Baseline mPAP was categorized into three groups (normal group: <25 mmHg; moderate PH group: 25–50 mmHg, severe PH group: 50–100 mmHg) to compare the outcomes between different mPAP groups. As a result, the incidence rate of newly identified LVD (14 (12%) vs. 10 (27%) vs. 12 (50%), P < .001), LVEF decrease 5% (53 (44%) vs. 21 (57%) vs. 18 (75%), P = .005) and LVEF decrease 10% (25 (20.8%) vs. 14 (37.8%) vs. 18 (75%), P < .001) were all the highest in severe PH groups (Fig. 2a; Table S2). The follow-up LVEF analyses revealed that patients with mPAP ≥25 mmHg had lower LVEF both in-hospital (60.8 ± 8.9 vs. 52.3 ± 8.9, P < .001) and one-month follow-up (63.2 ± 6.9 vs. 57.5 ± 8.3, P < .001) (Fig. 2b). In-hospital characteristics revealed that PH patients had a higher rate of post-procedure heart failure (17 (25%) vs. 6 (5%)), digoxin (16 (24%) vs. 5 (4%)), furosemide (21 (31%) vs. 6 (5%)) (P < .001), and a longer in-hospital stay (3.8 ± 2.2 vs. 3.2 ± 1.5, P = .001) (Table 2).
The clinical outcomes of different mPAP levels and ROC curve of the current model. (a) The incidence rate of primary and secondary outcomes in different mPAP groups. The Y axis indicates the rate of different outcomes in different mPAP groups, and the X axis indicates the different mPAP groups. The different outcomes are shown in different patterning; (b) the LVEF change of in-hospital and one-month follow-up in different mPAP groups. The Y axis indicates the LVEF measured by TTE. The X axis represents the time point of pre-procedure, post-procedure and one-month follow-up. The in-hospital outcomes of patients with PH or without PH. PH: pulmonary hypertension; LVD: left ventricular dysfunction.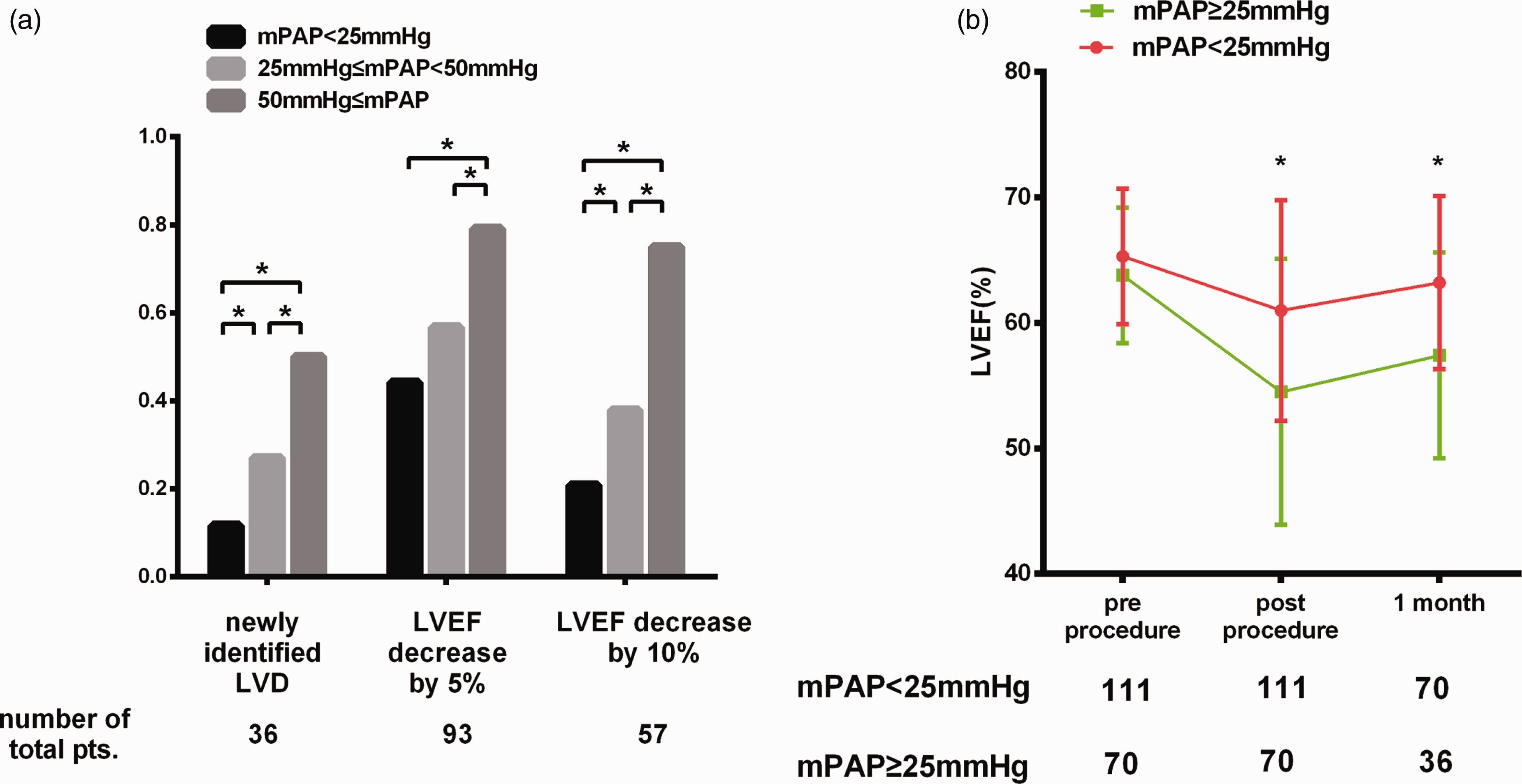

Univariate and multivariate analyses of primary and secondary end points.
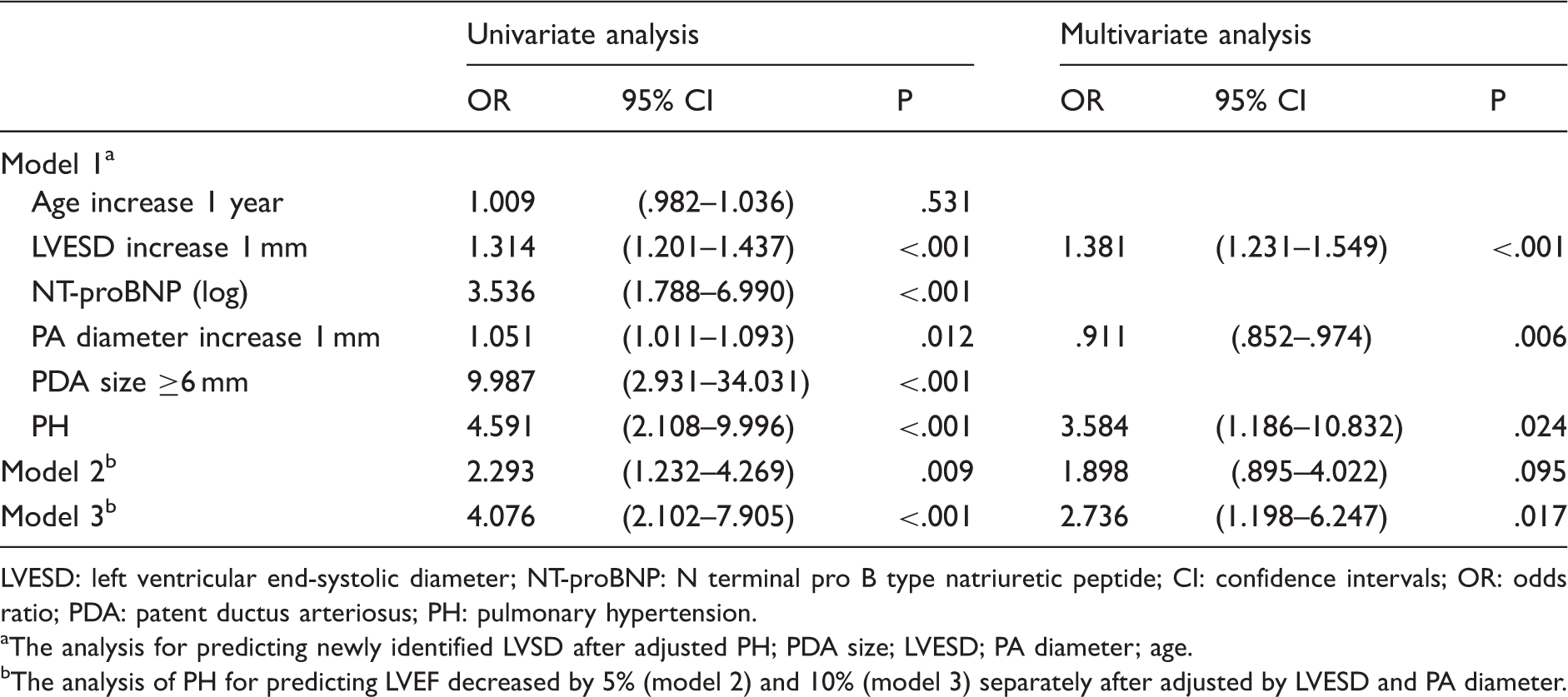
LVESD: left ventricular end-systolic diameter; NT-proBNP: N terminal pro B type natriuretic peptide; CI: confidence intervals; OR: odds ratio; PDA: patent ductus arteriosus; PH: pulmonary hypertension.
The analysis for predicting newly identified LVSD after adjusted PH; PDA size; LVESD; PA diameter; age.
The analysis of PH for predicting LVEF decreased by 5% (model 2) and 10% (model 3) separately after adjusted by LVESD and PA diameter.
According to ROC curve analyses, the model harbored a good ability to predict the newly identified LVD (AUC = 0.924, 95%CI: 0.885–0.963, P < .001) (cutoff: specificity = 0.7172, sensitivity = 1.0000), LVEF decrease by 10% (AUC = 0.834, 95%CI: 0.766–0.903, P < .001) (cutoff: specificity = 0.7239, sensitivity = 0.8936) (P < .001), and LVEF decrease by 5% (AUC = 0.677, 95%CI: 0.598–0.755, P < .001) (cutoff: specificity = 0.7955, sensitivity = 0.5484) (Fig. 3).
The ROC curve and the area under the curve (AUC) of the current model in different outcomes.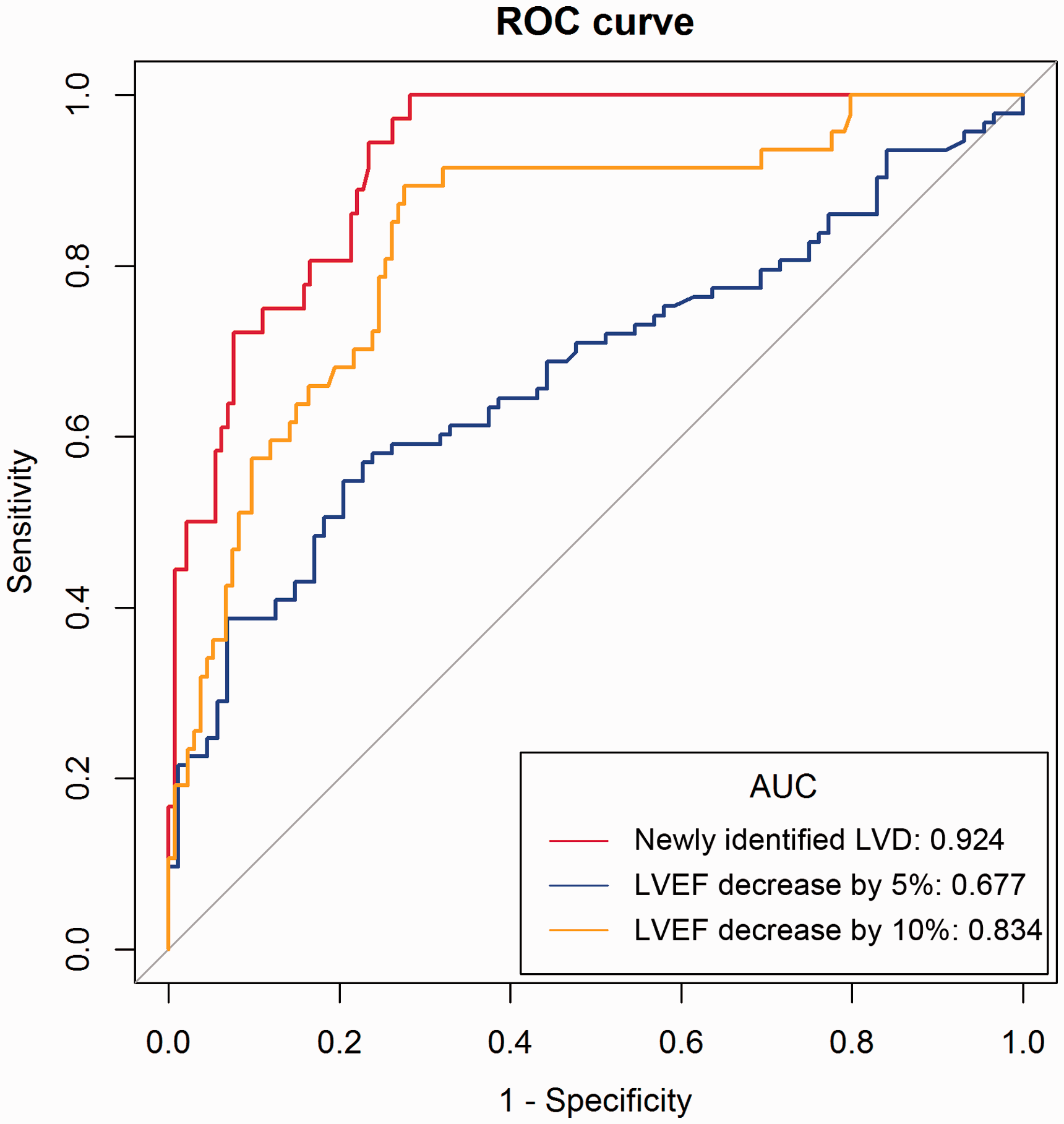
Discussion
In the present study, we showed that 133 PDA patients (72.7%) suffered an impairment of LVEF after the percutaneous device closure treatment. Newly identified LVD was prevalent among adult PDA patients, accounting for 19.67% of the cohort, with similar incident trends in different end points among different mPAP groups. Multivariate analysis further confirmed PH as a robust risk predictor of LVD (OR = 3.584, 95%CI: 1.186–10.832, P = .024) and severe impairment of LVEF (OR = 2.736, 95%CI: 1.198–6.247, P = .017) after adjusting possible confounding factors such as PDA size and age. Besides, improved LVESD and the diameter of PA have also been validated as independent risk predictors. The ROC curve analyses also verified the good discrimination power of the model to predict the newly identified LVD (AUC = 0.924, 95%CI: 0.885–0.963, P < .001) as well as LVEF decreased by 10% (AUC = 0.834, 95%CI: 0.766–0.903, P < .001).
To the best of our knowledge, this is the first study to demonstrate that the presence of increased PA pressure is a pre-operative predictor for the development of LV dysfunction post PDA closure. In addition, the mechanism for the predictive role of PH in LVD may be interpreted as follows. To be specific, the left-to-right shunt plays an important role in PDA patients. This abnormal shunt causes a persistent overload of the LV volume. The impairment of LVEF is attributed to a sudden closure of shunt, thereby reducing the LV overload consistent with the peri-procedure changes of TTE parameters in our cohort (Table S1), which has also been demonstrated in a limited population in previous studies.16–18 A previous study has demonstrated that pulmonary arterial hypertension is associated with fluid overload. 19 PH is a symbol of persistent overload situation that resulted in a LV remodeling known as a pre-existing LVD. Kiran and Tiwari have reported that a left ventricular dysfunction (LVEF less than 55%) after device closure of PDA is highly associated with the size of index PDA. 20 According to their database, the overall incidence of LV systolic dysfunction is 22.8%, which is rather comparable to our result. However, in their research, the age of most patients (71.14%) is under five. According to another cohort, the PDA patients aged above 18 years are more likely to have a fewer LV volume overload, Qp/Qs and elevated mPAP compared with neonates and infants. 12 Despite this, in our study, multivariate analysis was further performed by including factors such as age and size of PDA. It is intriguing to note that there is a significant exacerbation ratio of dysfunction among index PDA size more than 6 mm in Viralam’s study due to the LV preload, which, however, is insignificant in the current study. However, interpretation of the discrepancy might be that all the patients were aged >18 now. Not only the shunt but also a persistent overload could cause LV remodeling.
In a previous study, 21 the baseline pulmonary vascular resistance (PVR) was 9.12 ± 1.73 woods and Pp/Ps was 0.94 ± 0.10, while in the current study, the cardio-pulmonary circulation blood gas analysis was only performed only for patients with mPAP >45 mmHg. Thus, it is impossible to compare the hemodynamic parameter between the pulmonary artery hypertension (PAH) patients and the healthy control. The baseline PVR was 7.24 ± 4.01 woods, and the baseline Pp/Ps was 0.71 ± 0.19 (n = 23), indicating a higher pressure gradient (Table S3), which could also explain the higher prevalence of LVD in the current study. The previous research also demonstrated that an increased PA diameter was associated with the progression in pulmonary pressures. 22 In addition, PH has been validated to cause right ventricular dysfunction, 23 which could be easily interpreted that a decompensation of right heart dysfunction could release the burden of the LV overload. Furthermore, there is a lack of consistent criterion for LVD after PDA closure in previous study. According to our present outcomes, we suggest an LVEF decreased by 10% as a severe LVD because all the newly identified LVD were not less than 10%.
The closure of PDA with PAH in adult patients has also been recommended in the latest guideline. 24 Pulmonary over-circulation and left heart volume overload are the underlying causes of congestive heart failure in patients undergoing PDA closure. 25 The shunt volume can be accurately tested by the routine RHC after collecting the blood gas result from the aorta and PA. However, the guideline just suggests the RHC examination for decision support on correction of PAH patients with CHD, which is suggestive to be conducted among patients with mPAP more than 45 mmHg. 15 And according to the PDA closure procedure, the mPAP can be examined when the catheter passes the PA. The newly identified LVD can be predicted by PH instead of complete blood gas examinations, which would be more convenient in clinical practice. According to previous studies, there is a recovery of LVEF in a long-term follow-up, which is similar to our findings. 26 LVEF might be immediately decreased on a large scale after closure rather than after one month. A prolonged hospitalization has been found in patients with elevated mPAP. Although the trend in current study may result from a bias of missing follow-up data, a heart failure symptom is developed in specific patients especially in PAH patients instantly after procedure both in our study and previous studies.9,27 Thus, it is reasonable to emphasize the post-procedure monitor in LVEF just after PDA closure in patients with elevated mPAP, so that timely anti-heart failure medicine may be initiated.
Our present findings indicate that PDA patients accompanied with PH may have a pre-existing LVD due to the LV remodeling or the left-to-right shunt. And it is rational to emphasize the monitoring of heart function in PDA adult patients with PH according to the high prevalence of newly identified LVD. However, the causality relationship between the PH and LVD remains largely undefined. And large-scale trials with longer follow-up are required to determine whether additional medical treatment is beneficial for the long-term outcomes of these patients.
Limitation
The biggest limitation of current study was the retrospective design. To the best of our knowledge, the present study included the PDA adult patients with the large sample size to date. Although patients were recruited from a single-center data, all the echo examinations were performed by high-volume center technicians properly in a short time after procedure. In consideration of the possible interobserver bias, all the data were collected by independent trained staffs to assure the authenticity and objectivity. All the confounders cannot be adjusted to ensure the stability of model. Thus, the findings should be preliminary. The blood gas analyses were not conducted routinely; therefore, a complete cardio-pulmonary hemodynamics parameter cannot be obtained. A specific designed research that compares hemodynamics parameter with PH is required. And the PH is also an easily obtained symbol of overload during procedure. Besides, further studies are warranted to determine whether the closure benefits the PH patients and whether newly identified LVD will affect the long-term prognosis. Even though there is a trend in LVEF recovery according to the current result, a close care instantly after procedure should be reasonable. Despite these shortcomings, in the current study, we revealed a significant relationship between the PH and newly identified LVD by providing the evidence of determination of PDA closure in PH adults. According to the prolonged hospitalization and high rate of heart failure post-procedure, a closer monitoring is rational in PDA patients with elevated mPAP.
Conclusion
To sum up, adult PDA patients with pre-procedure elevated mPAP are significantly associated with higher prevalence of the newly identified LVD after closure. The pre-procedure elevated mPAP can be used to predict newly identified LVD. There is a clinical model consisting of PH, LVESD and diameter of PA that can predict the LVD, and severe impairment level of LVEF. Further studies are required to determine the long-term prognosis among PH with newly identified LVD and to identify the possible therapeutic benefits on these patients.
Supplemental Material
PUL888428 Supplementary material1 - Supplemental material for Prediction value of pulmonary hypertension in newly identified left ventricular dysfunction among adult patients after patent ductus arteriosus closure
Supplemental material, PUL888428 Supplementary material1 for Prediction value of pulmonary hypertension in newly identified left ventricular dysfunction among adult patients after patent ductus arteriosus closure by Peng-yuan Chen, Dong-ling Luo, He-zhi Li, Hong-wen Fei, Tao Huang, Yi-gao Huang, Ji-mei Chen, Jian Zhuang, Peng-cheng He and Cao-jin Zhang in Pulmonary Circulation
Supplemental Material
PUL888428 Supplementary material2 - Supplemental material for Prediction value of pulmonary hypertension in newly identified left ventricular dysfunction among adult patients after patent ductus arteriosus closure
Supplemental material, PUL888428 Supplementary material2 for Prediction value of pulmonary hypertension in newly identified left ventricular dysfunction among adult patients after patent ductus arteriosus closure by Peng-yuan Chen, Dong-ling Luo, He-zhi Li, Hong-wen Fei, Tao Huang, Yi-gao Huang, Ji-mei Chen, Jian Zhuang, Peng-cheng He and Cao-jin Zhang in Pulmonary Circulation
Footnotes
Acknowledgements
Flora Gordillo-Martínez (the postdoctoral fellow of Guangzhou Medical University, China) gave us a language support. We appreciate the efforts of all the congenital heart disease (CHD) physician operators (Dian-hua Zhou, Jun Chen, Guangdong cardiovascular institute) and the CRCs (Yong-quan Yang,Yin-xin Li, Shao-jun Xin, Jing-ru Deng, Xiao-ling Cen, Xiao-hua Dai, Guangdong cardiovascular institute). And the first author would like to appreciate the support from the girlfriend, Ms. Lu Liu, when there were many obstacles during the writing.
Authors’ contribution
Conceptualization, Caojin Zhang; Data curation, Pengyuan Chen and Caojin Zhang; Funding acquisition, Caojin Zhang; Investigation, Pengyuan Chen and Dongling Luo; Methodology, Pengyuan Chen, Dongling Luo, Hezhi Li and Hongwen Fei; Project administration, Pengcheng He and Caojin Zhang; Resources, Caojin Zhang; Software, Pengyuan Chen, Dongling Luo, Hezhi Li and Hongwen Fei; Supervision, Jimei Chen and Jian Zhuang; Validation, Tao Huang and Yigao Huang; Writing – original draft, Pengyuan Chen; Writing – review and editing, Pengcheng He and Caojin Zhang.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This work was supported by the National key Research and Development Program (2018YFC1002600), the Science and Technology Department of Guangdong Province (No. 2014A050503048, 2017A070701013 and 2017B090904034, 2017030314109), National Nature Science Foundation of China (No. U1401255).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
