Abstract
This study aimed to determine the benefits and correlated mechanisms of pulmonary artery denervation (PADN) for heart failure (HF) pulmonary hypertension (PH). PH secondary to HF is associated with poor clinical outcomes because there is no proper therapy for it. PADN showed improved outcomes for patients with HF-PH. However, the underlying mechanisms remain unknown. Supracoronary aortic banding (SAB) was used to create HF-PH models. Sprague-Dawley rats were randomly assigned to control, SAB, sham, SAB with PADN, and SAB without PADN groups. Surgical (longitudinally damaging vessel nerves) and chemical (10% phenol applied to the surface of nerves) PADN was performed for animals in the SAB with PADN group. Morphological, echocardiographic, hemodynamic, and protein expression changes were measured four weeks thereafter. Adrenergic receptor (AR) expressions of pulmonary arteries from four HF-PH patients and four patients without PH were measured. Ten HF-PH patients who underwent PADN were followed-up for six months. SAB-induced HF-PH was achieved by 50% of animals. Surgical and chemical PADN was associated with significant improvements in pulmonary artery muscularization, hemodynamics, and right ventricular functions. In pulmonary arterial specimens from HF-PH patients, β2-AR and α1A/B-AR, as well as eNOS, were downregulated and α1D-AR was upregulated compared to those from patients without PH. PADN led to a mean increase of 84 m during the 6-min walk distance for HF-PH patients at six-month follow-up. HF-PH was characterized by downregulated β2-AR, α1A-AR, and α1B-AR and by upregulated α1D-AR. PADN is associated with significant improvements in hemodynamics and pulmonary artery remodeling.
Heart failure (HF), a multifactorial and systemic disease, is estimated to affect approximately 1–2% of the adult population. 1 Over the past few decades, despite dramatic reductions in morbidity and mortality and the development of numerous medical and device-based therapies,2–4 patients with pulmonary hypertension (PH) still have poor clinical outcomes due to HF.1,3,4 Based on the fifth world symposium on PH, 5 long-term elevated left ventricular filling pressure triggers pulmonary arterial vasoconstriction with resultant pulmonary arteriolar remodeling, thereby shifting post-capillary PH to mixed post-capillary and pre-capillary PH, a stage defined as having a diastolic pulmonary pressure gradient (DPG) ≥ 7 mmHg independent of left ventricular ejection fraction (LVEF). Endothelin receptor antagonists and phosphodiesterase 5 inhibitors, two classes of target drugs used for patients with World Health Organization (WHO) class 1 pulmonary arterial hypertension (PAH), have failed to demonstrate evidence of regression during left ventricular (LV) remodeling or improvements in LV function.6,7
HF is associated with sustained and excessive levels of sympathetic nerve activity. 8 More importantly, increased cardiac noradrenaline spillover was greater and occurred before that of other organs, 9 indicating that the heart is exposed to higher levels of noradrenaline release for longer periods than other organs. Similarly, sympathetic overactivation should have a crucial role in the initiation and development of pulmonary arterial constriction. 10 Although β-blockers have become the first line of treatment for HF,8,9 previous clinical studies11–15 have not reached an agreement regarding the benefits of β-blockers for HF-PH. Recently, European Society of Cardiology/European Respiratory Society PH guidelines suggested β-blockers as an alternative medical therapy to treat PH-HF. 16 This implied complicated interactions between different AR in the pathophysiology of HF-PH. Percutaneous pulmonary artery denervation (PADN) has been used for PAH since 2013. 17 A subgroup analysis (HF-PH patients) of a consecutive study including 66 patients with different etiologies of PH18 showed improvements in exercise capacity, hemodynamics, and clinical results for HF-PH patients. However, correlated mechanisms of PADN treatment remain to be studied. The present study aimed to elucidate the effects and mechanisms of PADN for animals with PH induced by supracoronary aortic banding (SAB) and to determine the abnormal regulation of AR in pulmonary artery (PA) specimens from HF-PH patients. Finally, we analyzed the benefits of PADN for patients with HF-PH.
Methods
Animal groupings based on supracoronary aortic banding
Animals used in this study were on the controlled temperature (25 ± 2℃) and 12-h light/dark cycle conditions and provided with a standard rodent chow and water. Male Sprague-Dawley rats (Nanjing Medical University Animal Laboratory, Nanjing, China) aged four weeks and weighing 100–150 g were randomly divided into control (n = 6), sham (n = 12, thoracotomy (but not SAB), and SAB (n = 60) groups (Suppl. Fig. S1). The study protocol was approved by the Institutional Animal Care and Use Committee and the study was performed in accordance with the Guide for the Care and Use of Laboratory Animals (National Research Council).
Supracoronary aortic banding procedure
For SAB-induced HF models (Suppl. Fig. S2), animals were administered general anesthesia and their chests were opened using a surgical knife. A titanium clip with a residual open diameter of 0.71 mm (to create a diameter stenosis of 70–80% by visual estimation) was then implanted on the ascending aorta at least 1 mm distal to the origins of the coronary arteries. At four weeks after SAB, animals with successful HF-PH models (n = 30; 50%), defined as the presence of HF (LVEF < 60% and LV posterior wall thickness [LVPWT] > 2.5 mm) and PH (right ventricular systolic pressure [RVSP] > 35 mmHg and PA velocity time integral <30 ms), were randomly assigned to SAB (n = 6), SAB with PADN (n = 12), and SAB without PADN (n = 12) groups (Suppl. Fig. S1).
PADN for animals with HF-PH
The SAB animals in the SAB with PADN group underwent surgical and chemical PADN (Suppl. Fig. S2). First, the main PA (MPA) and major branches were isolated from the surrounding tissues following thoracotomy at the left third intercostal space. Surgical PADN was then performed according to the method reported by Jurastch et al. 19 Finally, 10% phenol was applied to the surface of the MPA and the bifurcation area for 5 min after removal of the deep adventitial tissue in the MPA wall. For animals in the SAB without PADN group, surgical PADN was not performed following thoracotomy; instead of 10% phenol, saline was smeared on the surface of the MPA and bifurcation area for 5 min. All animals were monitored for an additional four weeks after PADN.
To confirm the blocking effects by surgical and chemical PADN, peri-vessel tissues near the main PA trunk and bifurcation area (each 0.5 mm in length) were subsequently sliced at a thickness of 4 µm. Tyrosine hydroxylase (TH) immunostaining (Suppl. Fig. S3) was performed to compare the changes in nervous density.
Echocardiographic measurements for animals
Animals were anesthetized with 1.0–1.5% isoflurane inhalation. Echocardiographic measurements were then performed (Vevo 770; VisualSonics Co. Ltd.) before and four weeks after PADN. LVPWT, LV end-diastolic diameter, LVEF, right ventricular (RV) end-diastolic diameter, and RV anterior wall thickness were measured. The PA velocity time integral was quantified as an indicator of longitudinal RV systolic function and PH. Each parameter was averaged over three cardiac cycles.
Right heart catheterization for animals
Right heart catheterization (RHC) was performed at four weeks after PADN. A right heart catheter with an external diameter of 0.9 mm was inserted through the jugular vein, advanced to the MPA, and connected to a PowerLab system (AD Instruments Co., Australia). Right atrial pressure (RAP) and RVSP were then measured and recorded. Hemodynamic data were presented as the mean of 10 measurements.
Collection of lung and heart tissues
After hemodynamic measurements, all animals were euthanized. The lung and heart tissues were perfused with ice-cold saline to remove the blood. The lungs, right ventricle, and left ventricle with septum were then rapidly excised, dried, and weighed. The RV hypertrophy index was defined as the ratio of the RV to the left ventricle with septum.
Pathological assessment of pulmonary artery muscularization
The lung issues were fixed, paraffin-embedded, sectioned, and stained with hematoxylin and eosin (H&F) (Jiangsu; KeyGen Biotech, Nanjing, China). Double-staining for von Willebrand factor and α-smooth muscle actin (α-SMA) was performed to evaluate pulmonary vessel muscularization, which was classified as none (0–25%), partial (25–75%), or full (75–100%). Two slices from each rat and 20 pulmonary vessels (diameter < 150 µm) in each slice were assessed. The medial wall thickness of the pulmonary vessels (diameter < 150 µm) was acquired according to Rabinovitch’s method. The ratio of the vascular wall thickness to its outer diameter was determined by an Olympus BHS microscope (San Jose, CA, USA) using Image-Pro Plus 6.0 software (Media Cybernetics, Rockville, MD, USA).
Biochemical measurements
Lung tissues were ground, lysed, and centrifuged at 3000 rpm, and the supernatant was collected. cAMP and cGMP concentrations were subsequently measured using an enzyme-linked immunosorbent assay kit (Sigma, St. Louis, MO, USA), as instructed by the manufacturer. The enzyme-linked immunosorbent assay was also used to assay plasma noradrenaline levels. Nitrate and nitrite levels were assayed using a nitric oxide synthase activity assay kit (KeyGen Biotech). The supernatant was collected and treated with nitrate reductase to assay nitrite levels, and the absorbance was measured at 530 nm by a spectrophotometer (NanoDrop 2000; Thermo Scientific, Waltham, MA, USA).
Western blotting
The lung tissues and pulmonary arterial specimens were homogenized on ice, and the proteins were extracted using the appropriate kit. Horseradish peroxidase-conjugated secondary antibody (1:4000) was purchased from Santa Cruz (Dallas, TX, USA). Primary antibodies against GAPDH (1:2000), AKT (1:1000) and its phospholate sites at 308 (1:1000) and 473 (1:1000), PKA (1:1000), and Phospho-PKA (1:1000) were obtained from Cell Signaling Technology (Danvers, MA, USA). The primary antibodies against endothelial nitric oxide synthase (eNOS; 1:1000) and its phospholate sites at Ser1177 (1:1000), Thr495 (1:1000), and Ser633 (1:1000) were from R&D Systems (Minneapolis, MN, USA). Primary antibodies against various AR (1:500) were obtained from Santa Cruz.
Human pulmonary arterial specimens
Pulmonary arterial branches were obtained from eight patients at Nanjing Cardiovascular Research Center: four with HF-PH who underwent a heart and lung transplantation and four patients without PH who had localized lung cancer and underwent pneumonectomy (peritumor normal tissues). The PA segments were carefully separated from the surrounding tissues. Then, the most distal segments (tertiary intralobar segment) were obtained. All patients provided informal consent to provide their blood, tissues, and organs.
Percutaneous PADN for HF-PH patients
The results of 10 patients with HF-PH (defined as mean pulmonary arterial pressure [PAP] ≥ 25 mmHg at rest, pulmonary arterial wedge pressure [PAWP] > 15 mmHg, pulmonary vascular resistance [PVR] ≥ 3 Wood units, and DPG > 7 mmHg) after maximal medication for 5–7 days agreed with those of the study protocol for percutaneous PADN. PADN has been described previously. 18 Briefly, a PADN catheter with 10 electrodes was positioned at the distal MPA. Denervation was then performed at the conjunctional area between the distal main trunk and the ostial left branch with a temperature of 45–50℃, energy ≤ 15 W, and a time of 120 s/site. N-terminal brain natriuretic peptide (NT-proBNP) level, 6-min walk distance, and RHC before and six months after PADN were assessed according to standard methods. 18 Echocardiographic parameters of 10 patients were independently measured by Dr. Jing-Ping Sun (Hongkong Chinese University), who was blinded to the study protocol. This protocol was approved by the ethics committee of Nanjing First Hospital and informal consent was obtained from all patients. After PADN, all baseline medications were continued during the six-month follow-up.
Statistical analysis
Parameters were reported as counts and mean ± SD, mean ± SEM, or percentages when appropriate. Categorical variables were performed to chi-square test or Fisher’s exact test. Continuous variables were performed to Student’s t test or Wilcoxon rank-sum scores for non-normally distributed data. SPSS 19.0 software (SPSS Inc., Chicago, IL, USA) was used to perform the statistical analysis. Student t-tests and one-way analysis of variance were used to assess the differences in measurement data among the multiple groups. Differences in the continuous variables between the two therapies were analyzed using a paired t-test. All experiments were repeated at least three times. A P value < 0.05 was considered statistically significant.
Results
SAB-induced severe HF-PH
Hemodynamic and echocardiographic parameters before and four weeks after PADN.
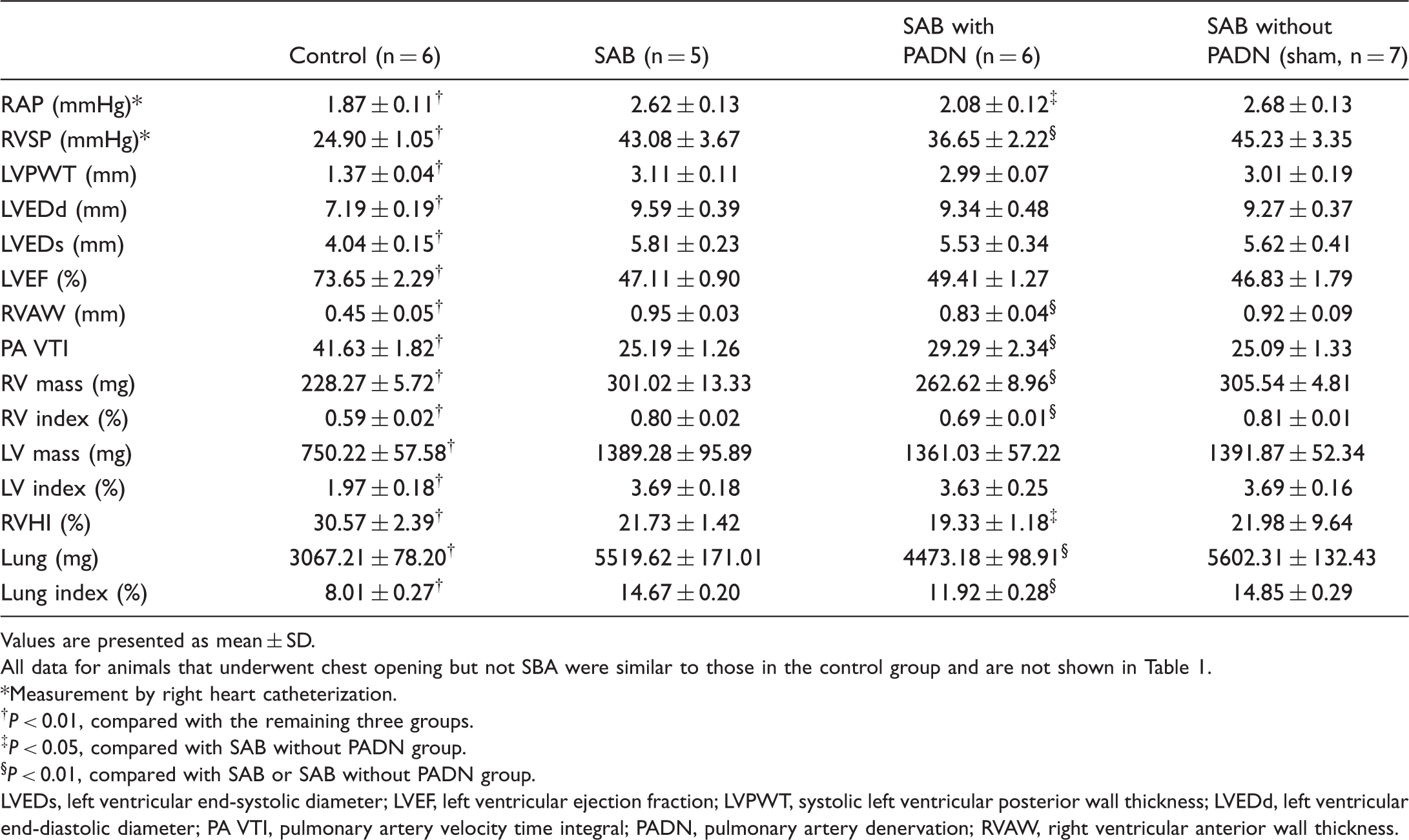
Values are presented as mean ± SD.
All data for animals that underwent chest opening but not SBA were similar to those in the control group and are not shown in Table 1.
Measurement by right heart catheterization.
P < 0.01, compared with the remaining three groups.
P < 0.05, compared with SAB without PADN group.
P < 0.01, compared with SAB or SAB without PADN group.
LVEDs, left ventricular end-systolic diameter; LVEF, left ventricular ejection fraction; LVPWT, systolic left ventricular posterior wall thickness; LVEDd, left ventricular end-diastolic diameter; PA VTI, pulmonary artery velocity time integral; PADN, pulmonary artery denervation; RVAW, right ventricular anterior wall thickness.
Surgical and chemical PADN significantly improved hemodynamics and RV function
At four weeks after PADN, both PA hemodynamics (RAP and RVSP) and RV functional indexes were significantly improved by PADN treatment (Table 1) compared to those in the SAB group or SAB without PADN group. Unfortunately, slight but non-significant improvements in LV chamber size, LV mass, and LVEF were noted after PADN treatment.
Surgical and chemical PADN significantly improved PA remodeling
Although SAB led to severe PA remodeling, as reflected by the higher percentage of partial/full muscularization and media thickness (Fig. 1), PADN resulted in a significant increase in partial muscularization (53.50 ± 3.01%) but a decrease in full muscularization (21.5%) when compared with the SAB group (30.0% and 47.8%) or the SAB without PADN group (31.1%% and 42.5%) (all P < 0.001) (Fig. 1).
Surgical and chemical PADN attenuated pulmonary structural remodeling in animals with HF-PH induced by SAB. H&E staining (a; scale bars = 50 µm) and α-SMA-staining (b) for lung tissues. Vessel wall thickness (c) and percentage of pulmonary arterial muscularization (d) were measured. The bars represent the mean ± SEM for each group. *P < 0.001 vs. control group; #P < 0.001 vs. control and SAB groups. H&E, hematoxylin and eosin; HF, heart failure; PADN, pulmonary artery denervation; PH, pulmonary hypertension; SAB, supracoronary aortic banding; SEM, standard error of the mean; SMA, smooth muscle actin.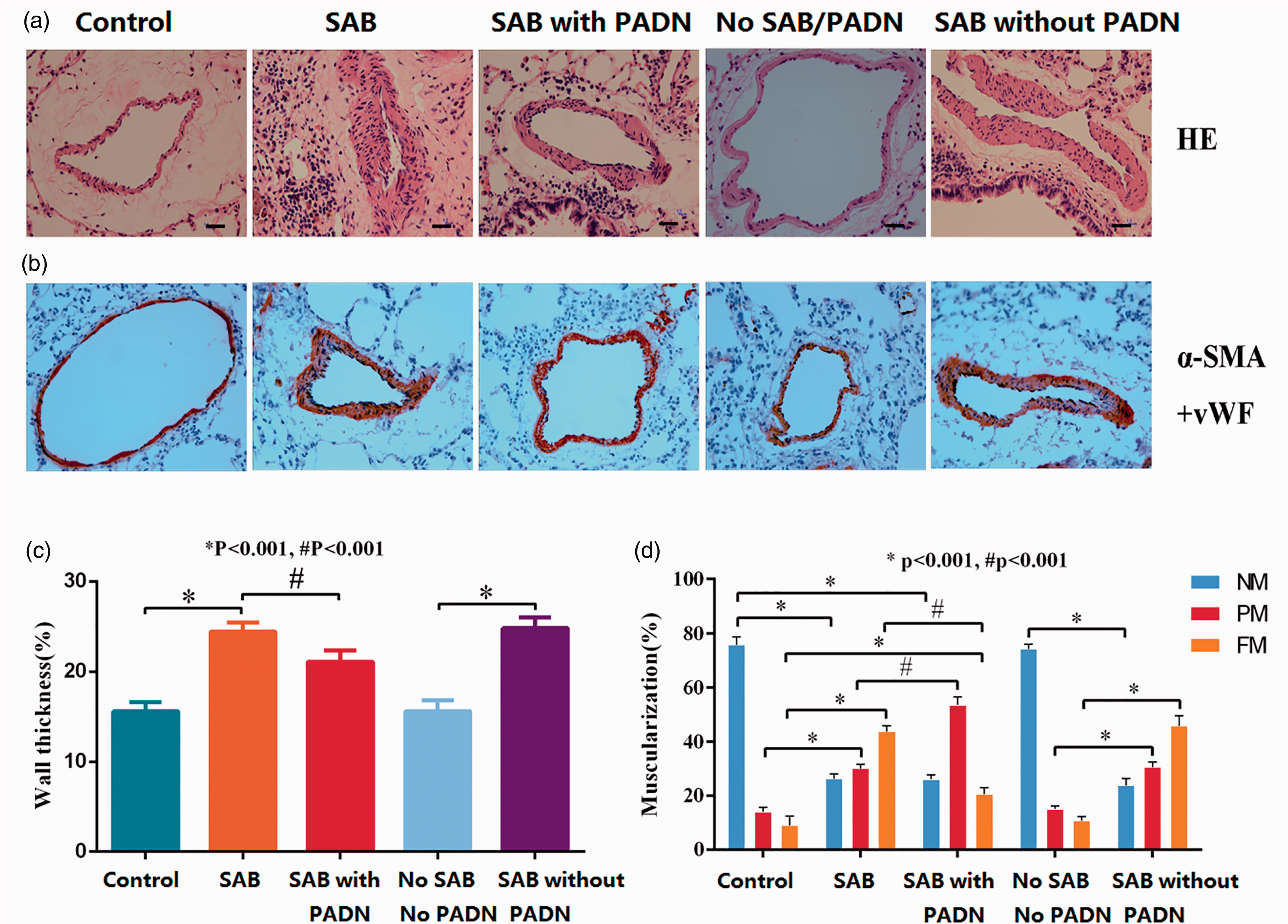
Surgical and chemical PADN improved pulmonary arterial relaxation
As shown in Fig. 2, SAB was accompanied by significantly increased serum NE and decreased concentrations of cAMP, nitrite, and cGMP as well as protein expressions of PKA, Akt, and eNOSSer-633, eNOSSer-1177 in lung tissues of animals (Fig. 3a). These changes were significantly improved by PADN treatment, thus indicating at least partial recovery of pulmonary arterial relaxation.
Changes in serum NE (a), lung tissue cAMP (b), cGMP (c), and NOx (d) levels. The results are expressed as the mean ± SEM. *P < 0.001 vs. control group; #P < 0.01 vs. control and SAB groups. NE, noradrenaline; NOx, nitrite; SEM, standard error of the mean; SAB, supracoronary aortic banding. Protein expression and receptor activity. Using western blotting, surgical and chemical PADN were associated with increased phosphorylation of eNOSSer-633/Ser-1177, AKTSer-473, and PK, and with decreased phosphorylated eNOS Thr-495 in animal lung tissues (a). Upregulated levels of α1-A-AR, a1-D-AR, β2-AR, and β3-AR were restored by PADN treatment (b). The expression levels of the proteins (c) and receptors (d) were normalized and quantified. *P < 0.01 vs. control group. **P < 0.01 vs. SAB group, #P < 0.05 vs. SAB group. AR, adrenaline receptor; eNOS, endothelial nitric oxide synthase; PADN, pulmonary artery denervation; PK, protein kinase; SAB, supracoronary aortic banding.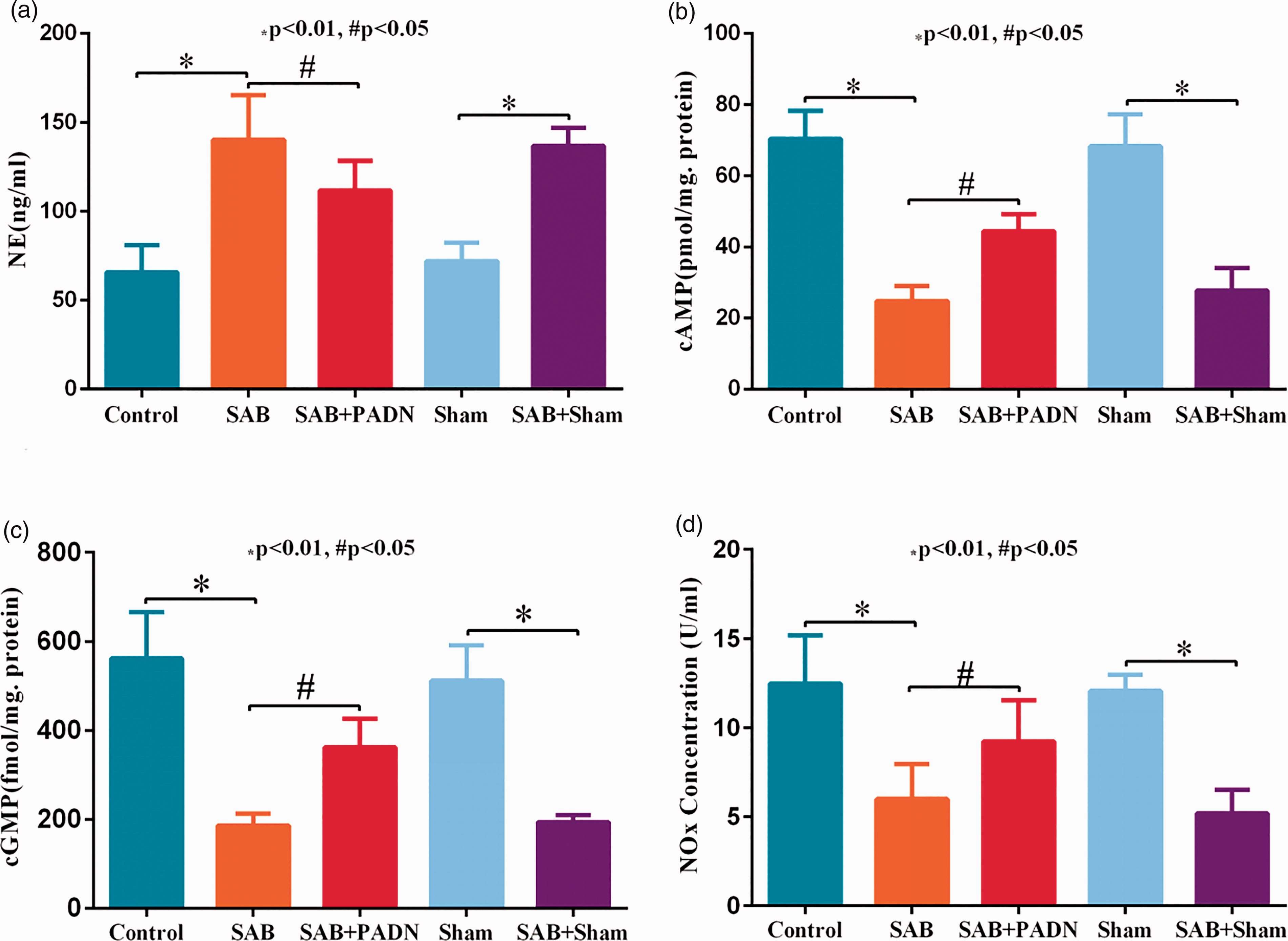
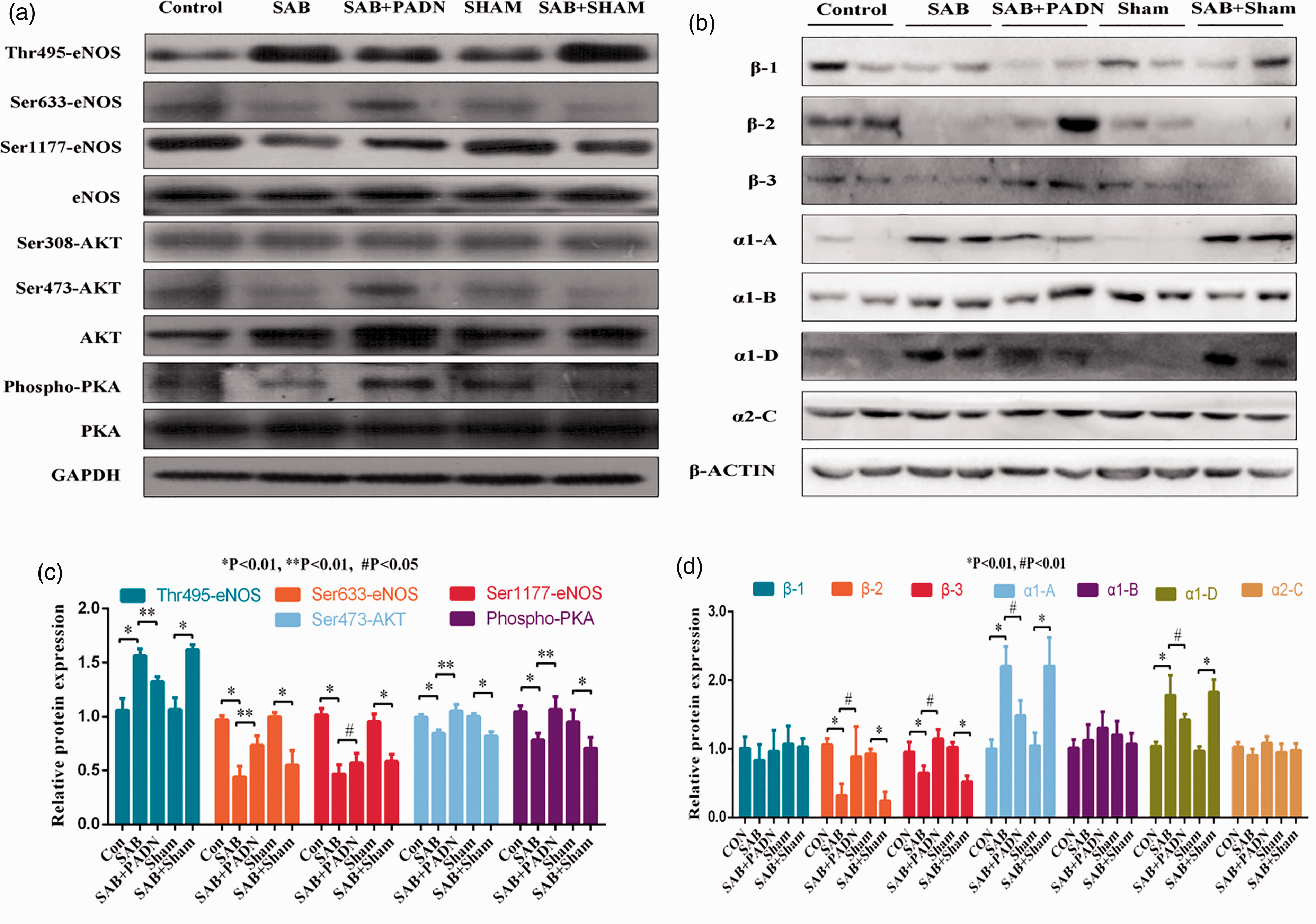
Differences in expressions of adrenergic receptors
In SAB animals, β2-AR and β3-AR were downregulated, but α1-A-AR and α1-D-AR were upregulated in lung tissues (Fig. 3b and 3c). In contrast, PADN was associated with upregulation of β2-AR and β3-AR and downregulation of α1-A-AR and α1-D-AR (Fig. 3b and 3d). There were no changes in β1-AR and α1-B/C-AR in the SAB group or the SAB with PADN group.
Abnormal regulation of receptors in the PA of patients with HF-PH
Compared to patients without PH, patients with HF-PH had significantly downregulated β2-AR, α1-A-AR, α1-B-AR, and eNOS;Ser-633 however, they had upregulated α1-D-AR (Fig. 4).
Receptor expressions in human pulmonary arterial tissue specimens. (a) Western blotting analysis showed downregulation of β2-AR, α1A-AR, and α1B-AR, but upregulation of α1D-AR in human pulmonary arterial tissues. (b) Protein expression levels were normalized against those of GAPDH and quantified. (c) Pulmonary arterial tissue lysates were immunoprecipitated with an anti-eNOS antibody and blotted with an anti-phospho-Ser633-eNOS antibody. (d) Bar graph shows quantitative results for phospho-Ser633-eNOS. *P < 0.05 vs. control. AR, adrenaline receptor; eNOS, endothelial nitric oxide synthase.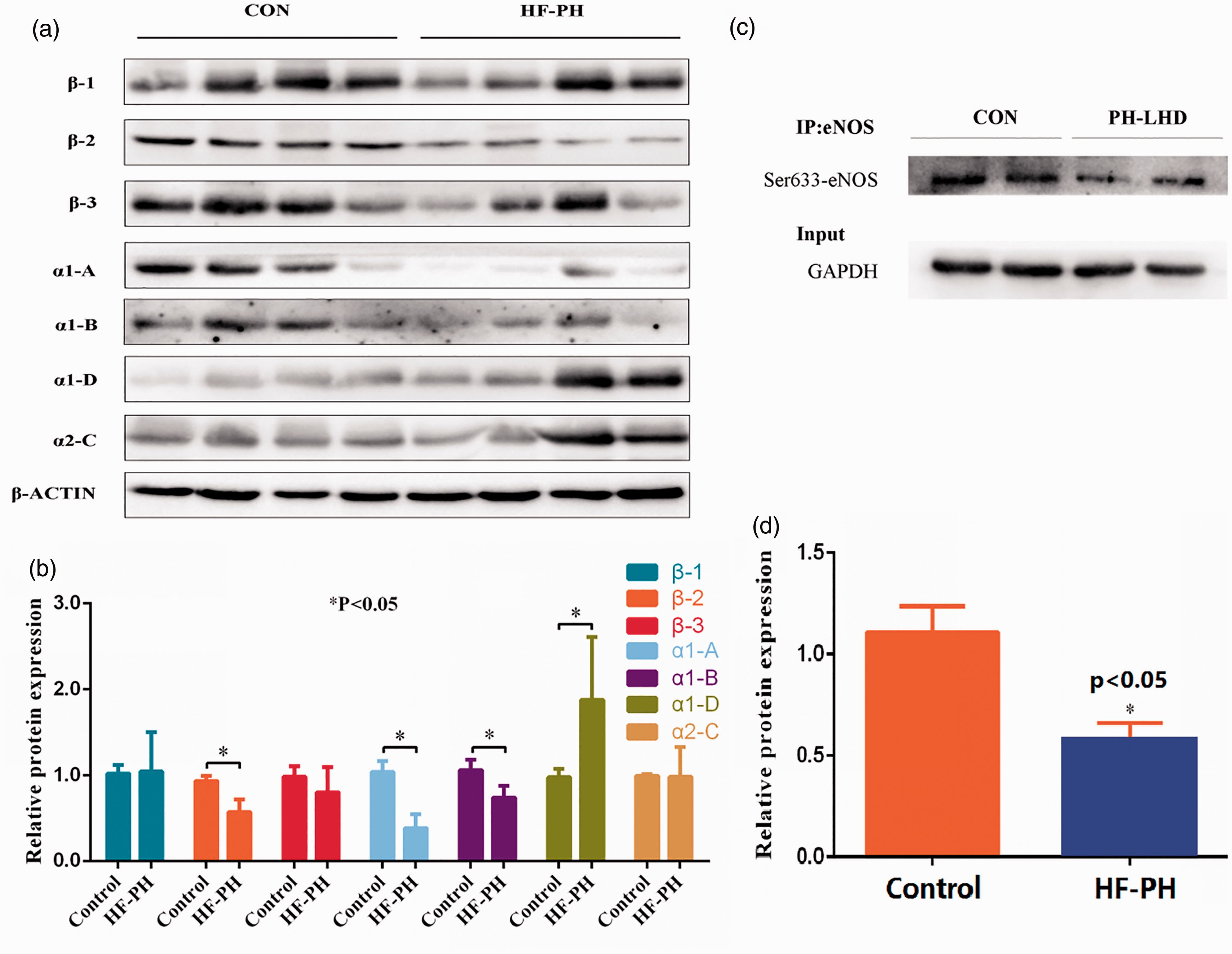
Clinical results of PADN for patients with combined post-capillary and pre-capillary PH
Ten HF-PH patients (seven men; average age = 67.5 years) underwent percutaneous PADN (Suppl. Table S1). Of them, three patients had ischemic cardiomyopathy after a previous myocardial infarction and stent implantation, two had hypertrophic obstructive cardiomyopathy after percutaneous trans-septal myocardial ablation, four had hypertension, and six had diabetes. Five patients had atrial fibrillation. β-blockers were prescribed for six patients and diuretics were prescribed for all patients. In particular, sildenafil was required for eight patients. Seven patients had DPG ≥7 mmHg (combined post-capillary and pre-capillary PH [Cpc-PH]) and the remaining three patients had a DPG < 7 mmHg.
Immediately after PADN, all but one patient showed an average mPAP reduction of >10% with RHC (data not included in this analysis). No periprocedural complications were recorded. As shown in Table 2, PADN resulted in significant reductions in PAP and PVR (Fig. 5, Suppl. Fig. S4). Notably, we also found a statistically significant reduction in LVEDP at six months after PADN, with a net increase in cardiac output of 31%, which was in line with the reduction of N-proBNP.
Changes in the 6-min walk distance (6MWD), pulmonary arterial hemodynamics, and LVEF. CO, cardiac output; m, mean; LVEF, left ventricular ejection fraction; NT-proBNP, N-terminal brain natriuretic peptide; PAC, pulmonary arterial compliance; PAP, pulmonary arterial pressure; PCWP, pulmonary capillary wedge pressure; PVR, pulmonary vessel resistance; RVP, right ventricular pressure; s, systolic; SV, stroke volume. Central illusion. Pulmonary artery denervation (PADN) is associated with the improvements in hemodynamic, pulmonary arterial remodeling, and cardiac function via damaging sympathetic nerves. NE, noradrenaline; AR, adrenaline receptor; NM, non-muscularization; PM, partial muscularization; FM, full muscularization; mPAP, mean pulmonary arterial pressure. Changes in exercise capacity, hemodynamics, and cardiac function of 10 patients with HF-PH at six months after PADN. HF, heart failure; NT-proBNP, N-terminal brain natriuretic peptide; PADN, pulmonary artery denervation; PH, pulmonary hypertension; WHO, World Health Organization.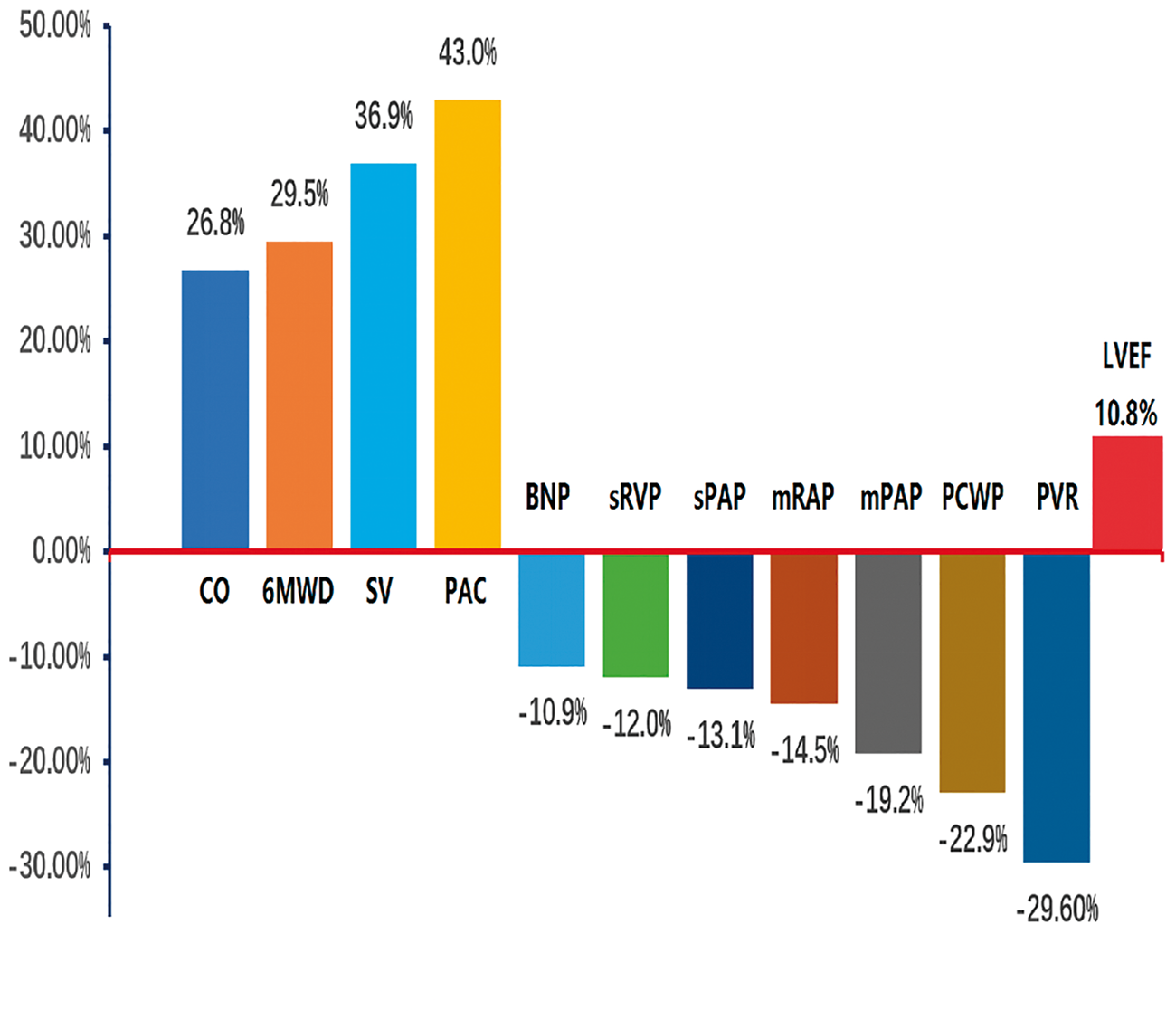
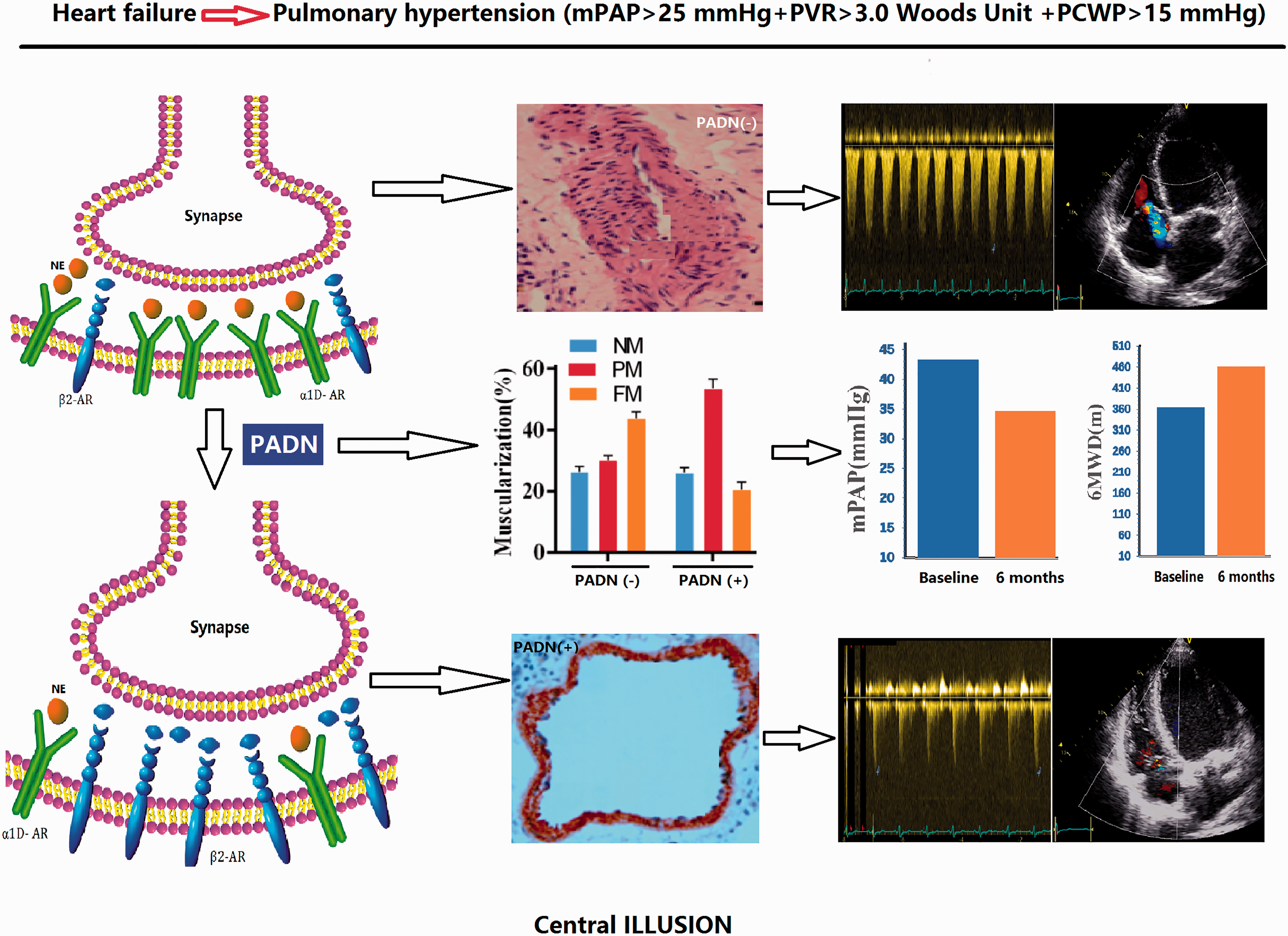
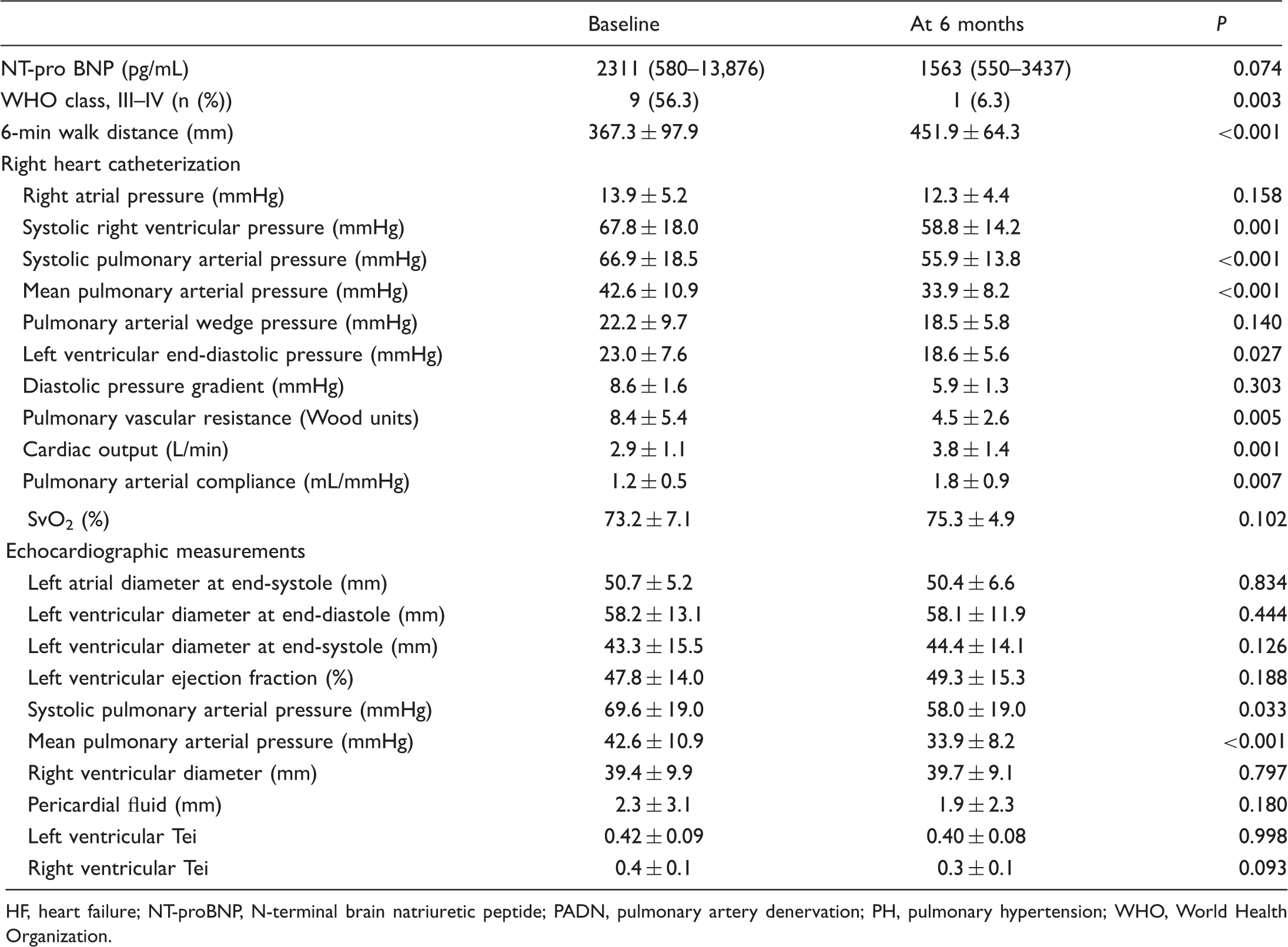
Echocardiographic measurements showed that the significant reduction of PAP was not accompanied by significant improvements in either LV or RV function, although those functional parameters tended to be slightly changed (Table 2). As shown in Suppl. Fig. 4, three patients had reduced LVEF at six months after PADN (case 1, from 63% to 57%; case 2, from 62% to 54%; and case 3, from 50% to 48%). Of these three patients, only case 1 had repeated LVEDP (20 mmHg) at six months after PADN compared to baseline LVEDP (19 mmHg). During six months of follow-up, no all-cause death was observed. Two patients were readmitted to the hospital because of worsening dyspnea.
Discussion
The present study is the first to demonstrate the effects and mechanisms of improvements in cardiac function and hemodynamics due to PADN. The main findings were: first, sympathetic nerve damage by surgical and chemical PADN is associated with confirmed reductions in RVSP/RAP and improvements in RV function; second, downregulation of β2-AR and upregulation of α1-D-AR may have critical roles in the development of HF-PH; and third, percutaneous PADN is feasible and effective for improving hemodynamics, exercise capacity, and cardiac function of HF-PH patients.
The pulmonary vasculature is generally innervated by sympathetic, parasympathetic, and sensory nerve fibers. Decreased arterial PO2 increases sympathetic nerve stimulation, which further stimulates baroreceptors and noradrenergic fibers in the PA with excessive release of NE and proximal airway segments. 20 This is supported by our finding that SAB animals had a large number of sympathetic nervous endings. We previously reported 21 that the PA sympathetic nervous bundle usually localizes at the left lateral wall of the main PA, with the shortest distance from nerve endings to the vessel lumen being <1 mm, which is an anatomic feature indicating the feasibility of using radiofrequency to damage nerves.
Two classes of abundant receptors in PA (endothelial and smooth muscle cells) are β-ARs and α1-ARs. Although increased vascular resistance is mediated by α-AR on sympathetic nerve stimulation, Hussain et al. 22 found that contractions of the PA due to phenylephrine are mediated, in part, via the α1D-subtype adrenoceptor. Our results showed that different expressions of AR might be explained by different tissues used for analysis (lung tissues from animals and PA from patients). However, the consistent finding was the upregulation of α1D-AR; this result further suggests that antagonists particularly targeting this subtype of α1-AR are expected. Similarly, we also found profound downregulation of β2-AR in either animal lung tissues or human PA. β2-AR has been reported to be important for mediating vasorelaxation and cAMP synthesis in lymphocytes of patients with primary pulmonary hypertension 23 and for attenuating lung injuries. 24 These results are in agreement with our results indicating that downregulation of β2-AR occurs parallel to reduced cAMP and cGMP in SAB. Furthermore, Pourageaud et al. 25 described that β2-AR-mediated (but not β1-AR-mediated, β3-AR-mediated) relaxation in the PA was NO-independent and endothelium-independent, as supported by our findings. However, even the interaction between β2-AR and α1-D-AR 26 balancing the pulmonary vascular tone was not fully understood from the present study, it was obviously that β2-AR and α1-D-AR may be the two most important AR for mediating PA contractions, smooth muscle cell proliferation, and endothelial dysfunction. This might be why nebivolol 27 had significant advantages over older β-blockers for PAH patients. On the other hand, eNOS mainly localize at endothelium and has not been reported to be measured in smooth muscle cells. The significantly reduced expression of PKA-Akt-eNOS signaling might largely reflect the injury of endothelial cells.
SAB is an accepted model used to study human pathophysiologically compatible models of valvular aortic stenosis-induced LV hypertrophy. 28 With the development of diastolic HF due to SAB, both diastolic and systolic HF occurred, which was in agreement with our results indicating that SAB animals had significantly reduced LVEF. Importantly, in SAB rats, we found that improvements in RV function and PA hemodynamics due to surgical and chemical PADN were independent of LV functional status. This finding further indicated that the presence of PH was mainly caused by progressive PA remodeling and contraction, similar to Cpc-PH in HF patients. However, non-significant improvements in the LV function of animals may be due to the short (only four weeks) follow-up.
Left heart disease is the most common cause of PH; it is mainly caused by left heart systolic or diastolic dysfunction. 29 Recently, DPG ≥ 7 mmHg has been considered an indicator of HF-PH severity regardless of LV function. Seven patients in this study were classified as having Cpc-PH. Although targeting PAH medications were not extensively accepted for the routine treatment of HF-PH, our team tested the efficacy of PADN for PH caused by left heart disease, 18 thus confirming the potential of PADN for this particular PH population. In the present study, we found significant improvements in pulmonary arterial hemodynamics according to either RHC or echocardiography; furthermore, the results supported our previous report. 18 Similar to an animal study, we did not observe significant improvements in either LV or RV functions after PADN for HF-PH patients. Possible explanations could include the short (only six months) follow-up and small patient numbers (n = 10). Furthermore, of three patients who had reduced LVEF after PADN (Suppl. Fig. 4), two had well-preserved LVEF at baseline (63% for case 1 and 62% for case 2). Even if we could find correlations between HF-PH patterns, because of the small patient population, the findings mentioned might have indicated that different mechanisms contributed to the development of PH induced by diastolic or systolic cardiac dysfunction.
Limitations
This study had some limitations. First, we could not measure ARs in the PA of animals because the distal vessel segments were too small to be separated. However, western blotting was performed with the PA of humans, which could conclusively analyze the abnormal regulation of adrenaline receptors. Second, we did not analyze the relationship between abnormally regulated protein expressions and the severity of PH in animals or patients. Third, endothelial cells and smooth muscle cells from human PA were not separately cultured, which caused trouble in interpreting the differences between two types of cells. As eNOS is usually expressed in endothelium, downregulated eNOS and PKA-Akt expressions strongly indicated the severe endothelial injury. Fourth, shorter follow-up and small patient numbers might have been the major reasons for not observing improvements in cardiac function. However, reduced LVEDP and PAWP at six months after PADN might underscore the potential of PADN for treating HF-PH. In the near future, we will report our first randomized study comparing PADN with sham for HF-PH patients.
Conclusion
The present study reported significant improvements in hemodynamics achieved by PADN. The mechanism is that upregulating β2-AR density and downregulating α1-D-AR density modulate downstream signaling to improve NO bioavailability, thereby improving pulmonary vascular remodeling and contraction. Further randomized clinical studies are warranted to confirm the benefits of PADN for patients with HF-PH.
Supplemental Material
Supplemental material for Pulmonary artery denervation improves hemodynamics and cardiac function in pulmonary hypertension secondary to heart failure
Supplemental Material for Pulmonary artery denervation improves hemodynamics and cardiac function in pulmonary hypertension secondary to heart failure by Hang Zhang, Wande Yu, Juan Zhang, Dujiang Xie, Yue Gu, Peng Ye and Shao-Liang Chen in Pulmonary Circulation
Footnotes
Acknowledgments
The authors thank Ms. Ling Lin, Ms. Wen Teng, and Ms. Hai-Mei Xu for their data monitoring and data collection throughout the study.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This study was funded by grants from the National Science Foundation of China (NSFC 91639303, NSFC 81770441), Jiangsu Natural Science Funds (2016-870), Jiangsu Six Talent Peaks (2015-WSN-069), and Nanjing Science and Technology Committee (201402045).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
