Abstract
Atrial arrhythmia (AA) occurrence in pulmonary arterial hypertension (PAH) may determine clinical deterioration and affect prognosis. In this study we assessed AA incidence in idiopathic (IPAH) and systemic sclerosis related PAH (SSc-PAH) and evaluated risk factors, management, and impact on mortality. We collected baseline data from consecutive IPAH or SSc-PAH patients prospectively enrolled in the Johns Hopkins Pulmonary Hypertension Registry between January 2000 and July 2016. During follow-up AA onset, treatment, and outcome were recorded. Among 317 patients (201 SSc-PAH, 116 IPAH), 42 developed AA (19 atrial fibrillation, 10 flutter-fibrillation, 9 atrial flutter, and 4 atrial ectopic tachycardia) with a 13.2% cumulative incidence. Most events were associated with hospitalization (90.5%). Electrical or pharmacological cardioversion was attempted in most cases. Patients with AA had higher right atrial pressure, pulmonary wedge pressure (P < 0.005), NT-proBNP (P < 0.05), and thyroid disease prevalence (P < 0.005). Higher mortality was observed in patients with AA, though not statistically significant (LogRank P = 0.323). Similar long-term mortality between IPAH with AA and SSc-PAH without AA was observed (LogRank P = 0.098). SSc-PAH with AA had the worst prognosis. In PAH patients AA occurrence is a matter of significant concern. Therapeutic strategies aimed at restoring sinus rhythm may represent an important goal.
Introduction
Pulmonary arterial hypertension (PAH) is characterized by a progressive increase in pulmonary vascular resistance (PVR) leading to chronic right ventricular (RV) pressure overload. 1 Chronic overload of the RV leads to functional tricuspid regurgitation with a subsequent increase in right atrial (RA) pressure. The longstanding elevation of atrial pressure induces progressive atrial dilatation and electrophysiological remodeling which, in conjunction with autonomic system modulations, may predispose these patients to the development of atrial arrhythmias (AA). 2
The incidence of AA in patients with PAH has not been well established and scant data exist concerning the correlation of AA with hemodynamics, clinical parameters, and clinical consequences in these patients.3–7 While most of the prior studies include more heterogeneous patient populations, limiting the ability to generalize to the PAH population, they suggest that AA occurrence may have prognostic implications.3–5,7 RA function contributes importantly to right heart function in patients with PAH as intact atrioventricular synchrony optimizes biventricular filling and is an important determinant of systemic output in patients with RV compromise.5,8 Despite growing evidence of the negative impact of AA on patients with pulmonary hypertension (PH), the clinical impact and optimal management approach in PAH remain undefined.
In this study we sought to verify the hypothesis that development of AA would negatively impact the clinical course of PAH. We describe the incidence of AA (specifically, atrial fibrillation, atrial flutter, or atrial ectopic tachycardia) in patients with PAH and explore the possible correlations between the onset of AA and baseline hemodynamics, co-morbidities, 6-min walk distance (6MWD), and serum biomarkers. We also aimed at assessing the impact on long-term mortality. Additionally, given our unique patient population, we compared the impact of AA on morbidity and mortality in idiopathic (IPAH) versus systemic sclerosis (SSc) related PAH (SSc-PAH).
Methods
Patient population
This prospective cohort study was approved by the Johns Hopkins University Institutional Review Board (NA_00027124, Baltimore, MD, USA); informed consent was obtained for all patients. The study was conducted in accordance with the Declaration of Helsinki. Consecutive patients with either IPAH or SSc-PAH evaluated at the Johns Hopkins Pulmonary Hypertension Program between January 2000 and July 2016, with at least six months of follow-up, were included. A diagnosis of PAH was confirmed by right heart catheterization (RHC) at rest and defined as the presence of mean pulmonary arterial pressure (mPAP) ≥ 25 mmHg, pulmonary artery wedge pressure (PAWP) ≤ 15 mmHg, and PVR > 3 Wood units (WU). 9 All patients with other potential causes of PH, including congenital heart disease, human immunodeficiency virus, portopulmonary hypertension, left heart disease (LHD), significant chronic obstructive pulmonary disease or interstitial lung disease, chronic thromboembolic disease, and sickle cell disease were excluded. The diagnosis of SSc was based on specific criteria as previously reported 10 and all diagnoses were confirmed by rheumatologists with expertise in SSc.
Data collection
Data were collected prospectively in the Johns Hopkins Pulmonary Hypertension Registry. Baseline demographics, hemodynamics, medical history, and World Health Organization (WHO) functional class (FC), 6MWD according to the recommendations of the American Thoracic Society, 11 and hemodynamics by RHC were obtained. Hemodynamic data included: right atrial pressure (RAP), mPAP, PAWP, cardiac output, and PVR. Baseline electrocardiography was performed in all patients. Serum measurements of N-terminal pro B type natriuretic peptide (NT-proBNP), creatinine, and uric acid were obtained. All patients underwent regular follow-up visit every three, six, and 12 months or when clinically indicated. During follow-up visits, medical history, physical examination, WHO FC, and details concerning any interim hospitalizations and alterations in treatment were recorded.
The arrhythmias considered were atrial fibrillation, atrial flutter, and atrial ectopic tachycardia detected on electrocardiography. Treatment was individualized and dictated by the treating physician; however, a rhythm control strategy was adopted and applied in the majority of our patients whenever feasible and clinically indicated. For the purpose of this study, sinus rhythm was considered stable when it was maintained for the entire follow-up period. Initial treatment included pharmacologic cardioversion, direct current cardioversion, and electrophysiological study with radiofrequency ablation. When these interventions were not successful at restoring sinus rhythm, rate control strategy was prescribed (primarily digoxin or diltiazem). According to guidelines, anticoagulation therapy was prescribed to all patients who experienced AA, unless contraindicated. 12
The primary outcome was all-cause mortality. Survival was assessed from the date of diagnostic RHC.
Statistical analysis
Continuous variables were expressed as mean ± standard deviation and categorical variables were expressed as number or percentages. Group comparisons were performed using independent sample t test or Mann–Whitney non-parametrical analysis for continuous variables and χ 2 statistics for categorical variables, as appropriate. Survival analysis was performed by means of Cox regression model, log-rank test, and Kaplan–Meier survival curves. A P value < 0.05 was considered significant. Statistical analysis was performed using SPSS version 22.0 (IBM Corp., Armonk, NY, USA).
Results
Study population and incidence of AA
Clinical characteristics of the study population.
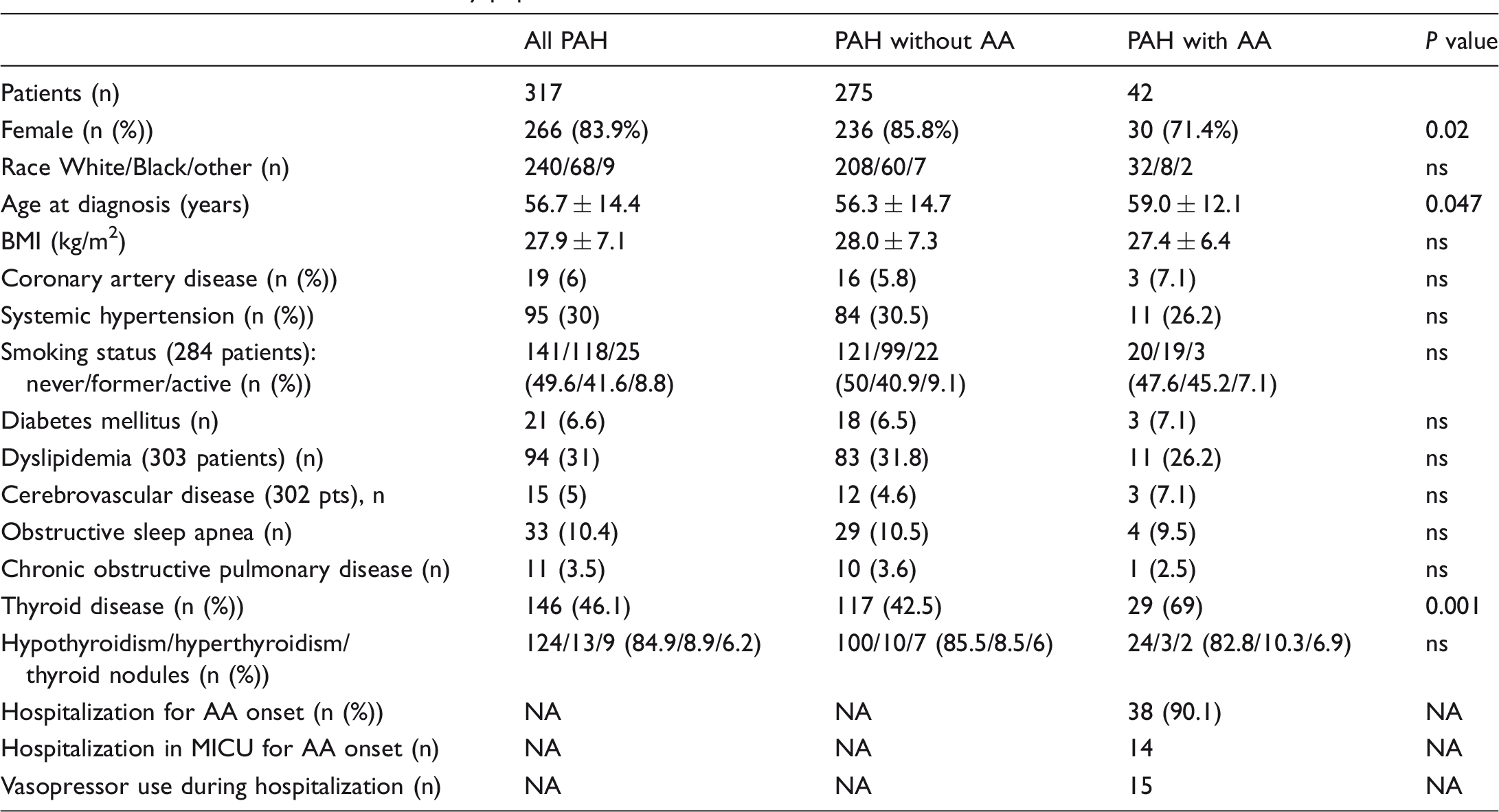
Data are presented as mean ± standard deviation, number, or percentage.
Comparison between groups (PAH without AA vs. PAH with AA) was made with independent sample t-test or Mann–Whitney non-parametrical analysis for continuous variables and χ2 statistics for categorical variables, as appropriate, and a P value < 0.05 was considered significant.
PAH, pulmonary arterial hypertension; AA, atrial arrhythmias; BMI, body mass index; NA, not applicable; MICU, medical intensive care unit.
Similar co-morbidities and risk factors for cardiopulmonary disease were present, with the exception of a significantly higher prevalence of thyroid disease, defined as either hypo or hyperthyroidism, or radiological evidence of thyroid nodules, in the AA group.
Right and left heart filling pressures are higher in patients with PAH who develop AA
PAH etiology, functional class, pulmonary vasodilator treatment, hemodynamics, and serum measurements of the study population at baseline.
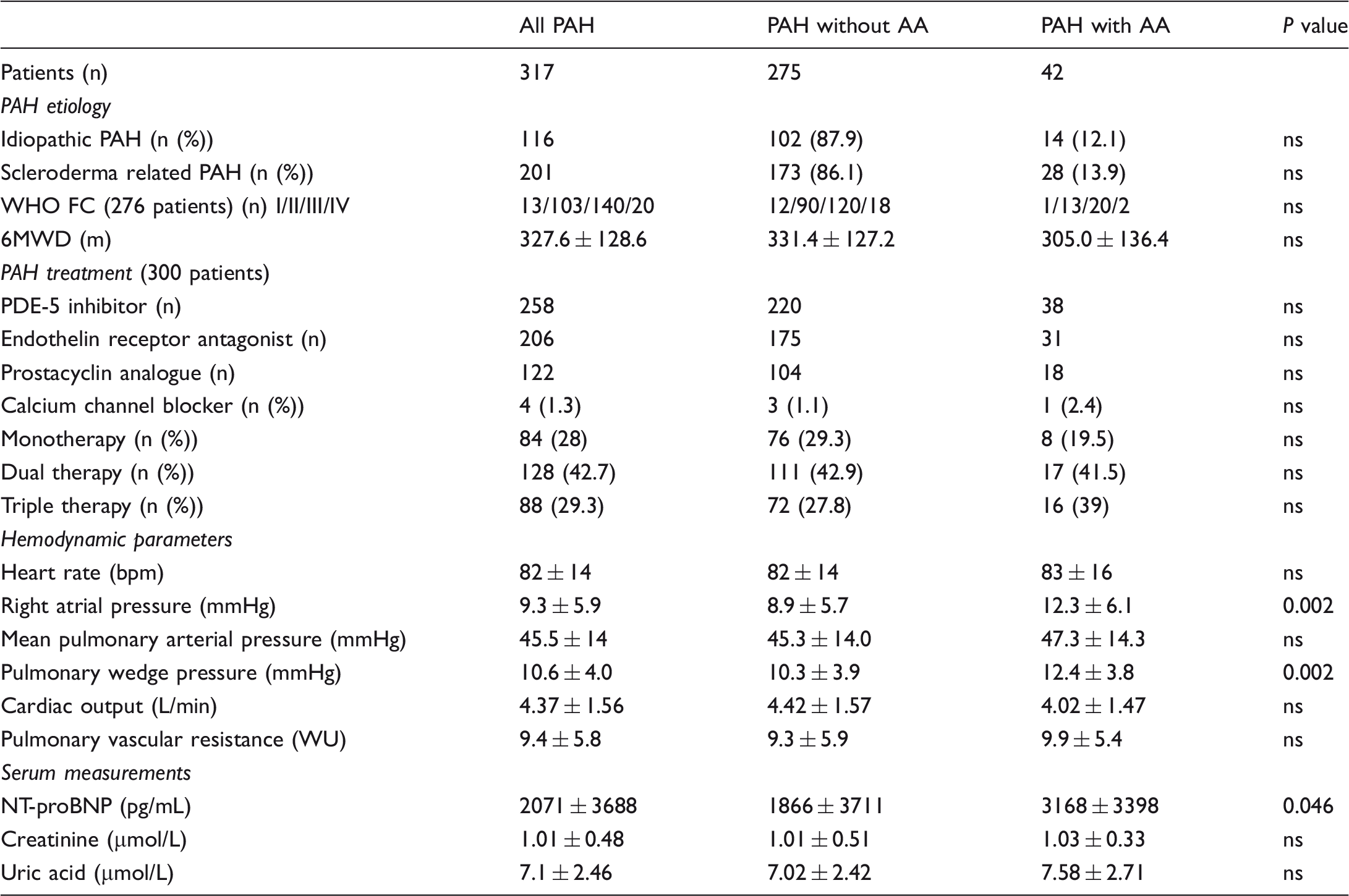
Data are presented as mean ± standard deviation, number, or percentage.
Comparison between groups (PAH without AA vs. PAH with AA) was made with independent sample t-test or Mann–Whitney non-parametrical analysis for continuous variables and χ2 statistics for categorical variables, as appropriate, and a P value < 0.05 was considered significant.
PAH, pulmonary arterial hypertension; AA, atrial arrhythmias; WHO, World Health Organization; PDE-5, phosphodiesterase 5; WU, Wood Units; NT-proBNP, N-terminal pro b type natriuretic peptide.
AA occurrence determines clinical worsening in patients with PAH
Type and treatment of AA SVA in PAH patients.
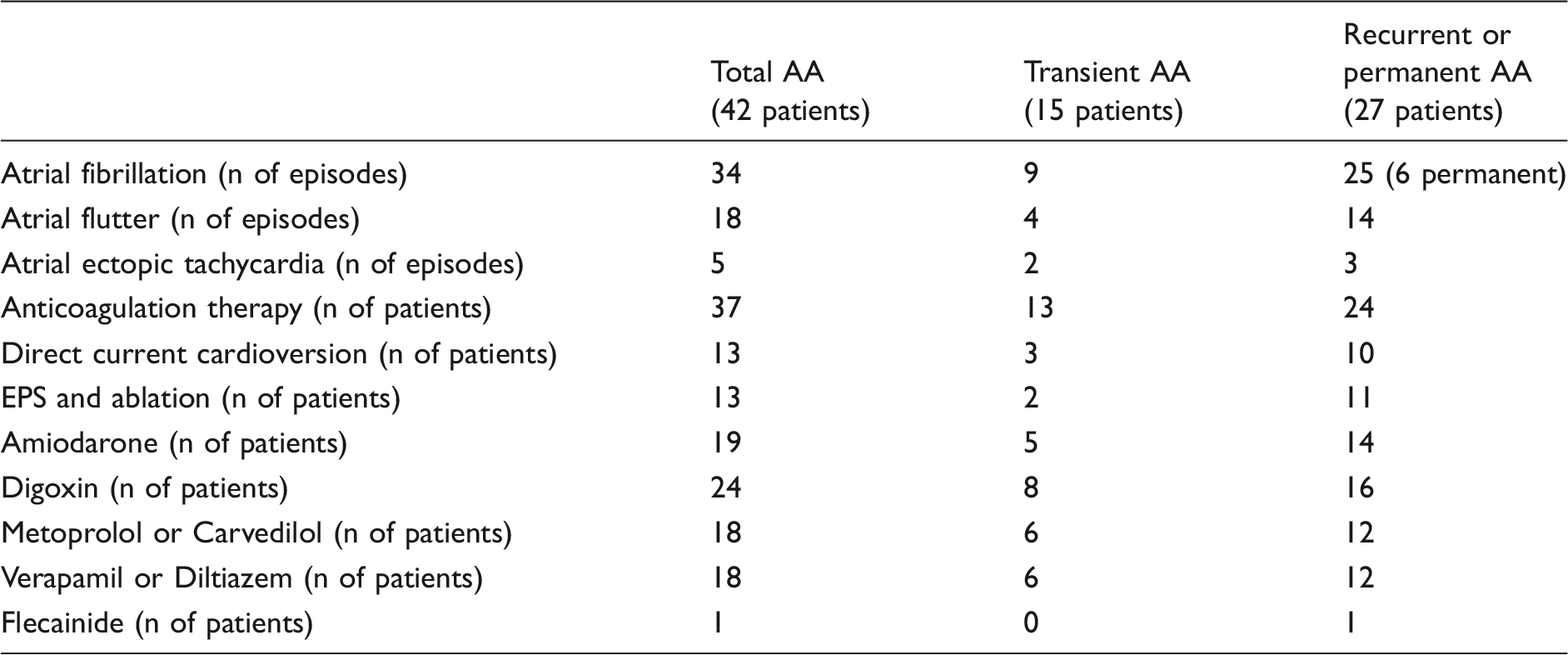
AA, atrial arrhythmia; PAH, pulmonary arterial hypertension; EPS, electrophysiological study.
Survival analysis
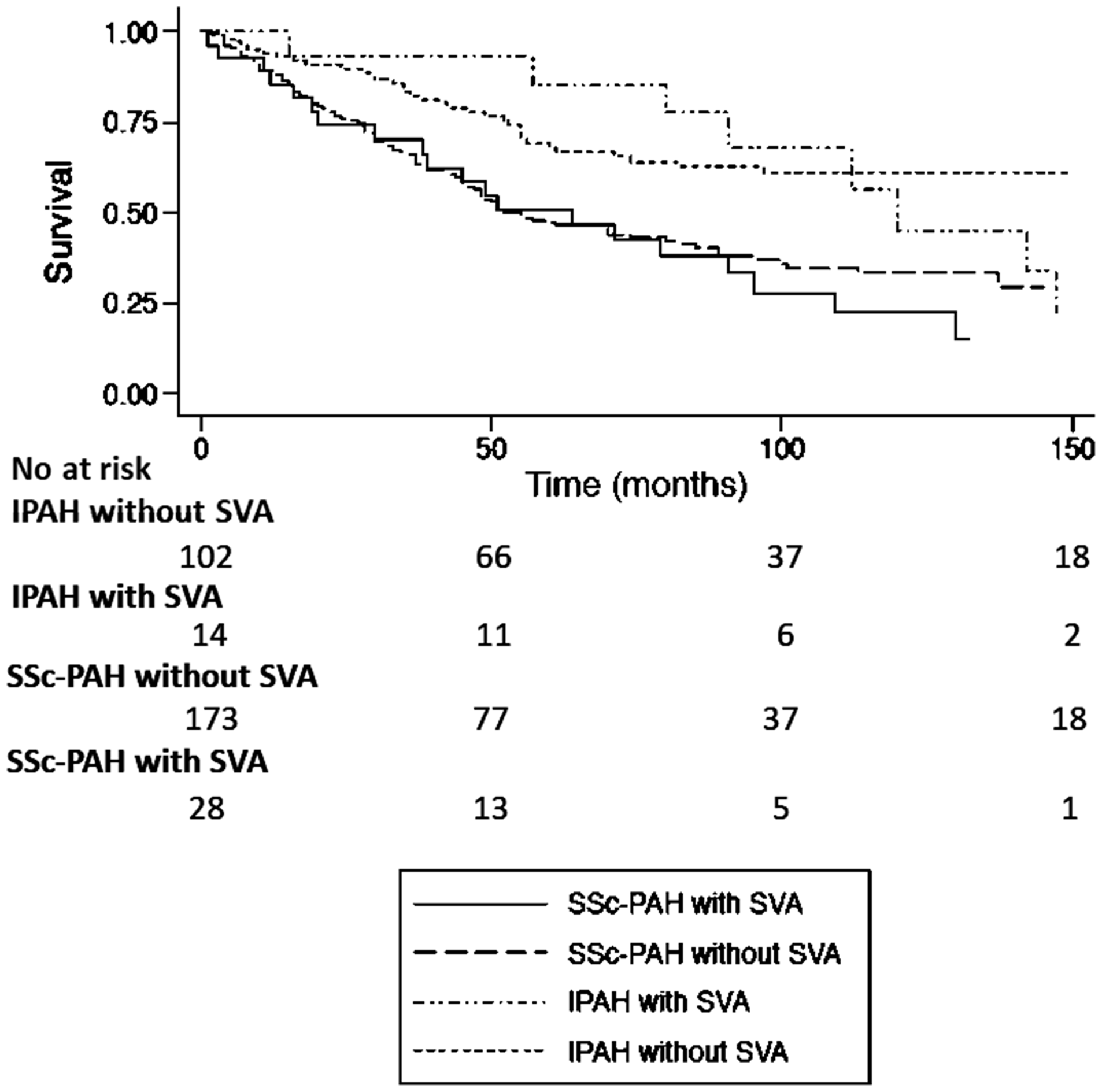
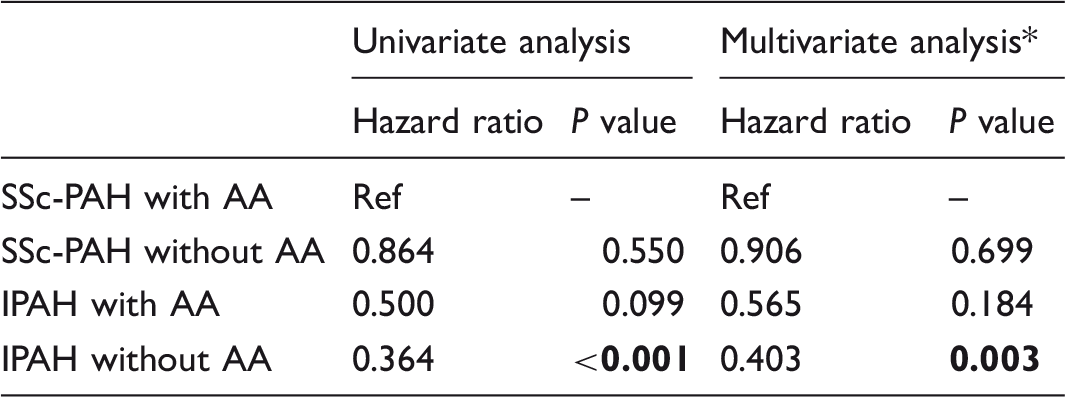
Among the overall PAH population, a total of 170 (53.6%) deaths were observed: 141 (51.3%) in the group without AA and 29 (69%) in the group with AA. Kaplan–Meier survival curves are shown in Figs. 1 and 2. Patients with AA had a higher but not statistically significant long-term mortality in comparison to patients without AA (Log Rank P = 0.323). Etiology-based analysis revealed that patients with SSc-PAH, both with and without AA, had a significantly worse prognosis when compared to IPAH patients (SSc-PAH without AA vs. IPAH without AA Log Rank P < 0.001; SSc-PAH with AA vs. IPAH with AA: Log Rank P = 0.031). Interestingly, the mortality between SSc-PAH patients without AA and IPAH patients with AA was not statistically different (Log Rank P = 0.098), as shown in Fig. 2. These results were confirmed by the Cox regression univariate and multivariate analysis, adjusted for age, sex, and thyroid function (Table 4). Patients with SSc-PAH who developed AA had the worst long-term prognosis. Survival between patients on anticoagulation before AA versus patients not on anticoagulation was not significantly different (Log rank test P = 0.794).
Kaplan–Meier curves for all-cause mortality among PAH patients according to the occurrence of AA. P value PAH with AA vs. PAH without AA: Log Rank P = 0.323; Breslow P = 0.985; Tarone-Ware P = 0.717. PAH, pulmonary arterial hypertension; AA, atrial arrhythmia. Kaplan–Meier curves for all-cause mortality among PAH patients according to the etiology and the occurrence of AA. P value SSc-PAH with AA vs. SSc-PAH without AA: Log Rank P = 0.454; IPAH with AA vs. IPAH without AA: Log Rank P = 0.410; SSc-PAH without AA vs. IPAH without AA: Log Rank P < 0.001; SSc-PAH with AA vs. IPAH with AA: Log Rank P = 0.031; SSc-PAH without AA vs. IPAH with AA: Log Rank P = 0.098; SSc-PAH with AA vs. IPAH without AA: Log Rank P < 0.001. PAH, pulmonary arterial hypertension; AA, atrial arrhythmias; IPAH, idiopathic pulmonary arterial hypertension; SSc-PAH, systemic sclerosis related pulmonary arterial hypertension. Cox regression analysis for all-cause mortality among PAH patients according to the etiology and the occurrence of AA in a univariate model and in a multivariate model, adjusted for age, sex, and thyroid dysfunction. Adjusted for age, sex, and thyroid dysfunction. SSc-PAH, systemic sclerosis related pulmonary arterial hypertension; AA, atrial arrhythmia; IPAH, idiopathic pulmonary arterial hypertension. The P values statistically significant are highlighted in bold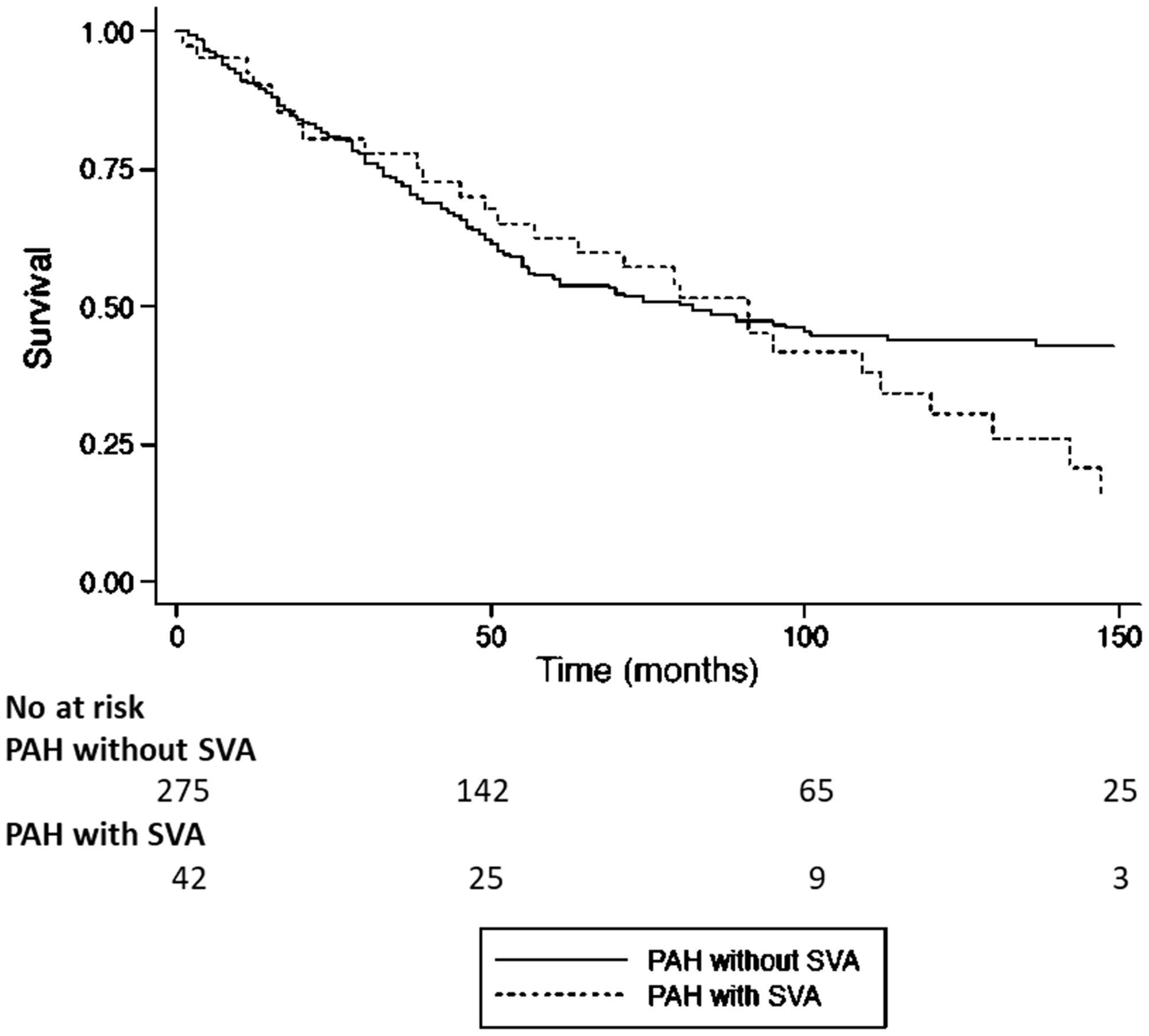
Discussion
This study demonstrates that AA are common in a cohort of 317 PAH patients, with a cumulative incidence of 13.2% during the five years of follow-up. In the existing literature, the incidence of AA in patients with PH has been reported to be in the range of 10–25% with a mean six years of follow-up.2,3,5–7,13–16 Importantly, we believe our reported incidence of AA is particularly accurate for these specific PAH etiologies (SSc-PAH and IPAH), given the fact that most of the previous studies included patients with heterogeneous etiologies of PH, including both pre- and post-capillary hypertension. Prior studies frequently included patients with PH due to LHD, thus demonstrating, as expected, a higher prevalence of arrhythmias2,14–16 in a condition with a distinct pathophysiology and possible confounding factors warranting evaluation as a separate entity from PAH.
In our study, the occurrence of AA was associated with higher pressures in both atria (the right and, as suggested by PAWP, the left), as well as higher levels of NT-proBNP. In addition, the presence of thyroid disease was significantly associated with the development of AA. A higher prevalence of thyroid disease has been described in patients with PAH,17–19 and, although the reason for this association is not completely characterized, the current results suggest that the presence of thyroid disease may affect prognosis. 20 In our cohort, survival analysis revealed that patients who developed AA without thyroid dysfunction had a significantly worse prognosis in comparison to patients without AA and without thyroid dysfunction (Log rank P = 0.048). The worst prognosis was observed in patients who developed AA that was not related to the presence of thyroid dysfunction. These results suggest that AA associated with thyroid dysfunction may be a relatively benign condition, while, on the contrary, AA unrelated to thyroid dysfunction may adversely affect prognosis in PAH patients.
In most cases, AA onset manifested as clinical worsening, leading to progressive symptoms of right heart failure and to hospitalization. In patients with PH, the loss of adequate atrial contraction, atrioventricular synchrony, and heart rate control progressively compromises global cardiac function, impacting morbidity and mortality. In normal individuals, longitudinal RV shortening accounts for approximately 70% of global RV function, with the remainder accounted for by RA function. When RV function is impaired, as seen in PAH, the RA accounts for a significantly larger proportion of global right heart function as measured by tricuspid annular plane systolic excursion (TAPSE). Augmented RA contraction enhances filling of the non-compliant RV and is essential for maintaining cardiac output. In a recent study evaluating PAH patients with echocardiogram, mean TAPSE was 1.7 cm and could have dropped as low as 0.8 cm in the absence of RA systolic function. 21 This difference illustrates the importance of RA function in total right heart function in patients with PAH, providing physiologic rationale for why AA are so poorly tolerated in these patients. In addition, this supports prior data demonstrating that increased RA size is a powerful predictor of mortality in PAH, suggesting RA size may correlate with RA dysfunction and represent a greater burden of total right heart dysfunction.22–24 Therefore, while in patients without PAH the RA is often described as a reservoir, storing blood when the tricuspid valve is closed, and a conduit, passively transferring blood into the right ventricle, in patients with PAH the most crucial role of the RA may be its pump function, with atrial systole adding substantially to RV filling and function. Losing this function with the onset of AA in patients with PAH should indeed be interpreted as a threatening sign. A rhythm control strategy is quite appropriate in LHD. However, in PAH most experts would agree that development of atrial fibrillation causes significant hemodynamic instability as these patients are for homeostasis on an adequate atrial kick. 21 Therefore, our initial strategy has always been to restore a sinus rhythm as the first therapeutic maneuver.
Prior studies suggest a causal relationship between development of AA and clinical deterioration in patients with PH.5–7,9 Indeed, restoration of sinus rhythm was followed by clinical improvement, and the development of permanent AA, but not transient AA, was associated with increased mortality in patients with PH. Importantly, our work supports this concept in the PAH population. There was no significant difference in 6MWD, FC, and RV afterload between groups, which suggests AA is not merely a marker of disease severity. Further, we found that AA occurrence, particularly if recurrent or persistent, is associated with worse long-term prognosis. Together, these observations suggest AA occurrence in PAH may be an independent cause of clinical decline leading to increased morbidity and mortality.
Furthermore, analyzing the impact of AA on mortality according the etiology of PAH (IPAH vs. SSc-PAH) highlighted another important result. It is well-known that among the many different etiologies of PAH, IPAH has a better long-term median survival (eight years), while the prognosis with SSc-PAH is one of the worst, with a median survival of less than four years.1,25,26 As shown in our analysis, IPAH patients with AA had a long-term mortality similar to the SSc-PAH patients without AA. Scleroderma heart disease is classified into primary and secondary forms. In primary SSc cardiac disease, there is direct involvement of the myocardium, pericardium, valves, coronary vessels, and conduction system due to vascular, fibrotic, and inflammatory changes of the disease itself. Secondary cardiac involvement develops in response to pulmonary vascular or interstitial lung disease. In primary SSc cardiac disease, the presence of focal fibrosis is the predominant pathologic finding – fibrosis of the conduction system can result in various types of heart block and/or arrhythmias. Interestingly, in our study, the incidence of atrial arrhythmias was similar in IPAH and SSc-PAH. The reason for the substantial prognostic differences between IPAH and SSc-PAH is poorly understood, but the significant difference in outcome with the development of AA supports the hypothesis that it is related to the burden of right heart disease with impaired ability of the right heart to adapt to elevated pulmonary vascular pressures in the absence of atrial systole. 27 In addition, there was no significant difference in RV load between groups (Table 2), further suggesting that prognosis is not directly related to the magnitude of RV afterload, but rather the ability of the RA and RV to adapt to that progressive change in afterload. By itself, myocardial involvement in SSc imparts an unfavorable prognosis with an overall five-year mortality of approximately 70%. Perhaps not surprisingly, patients with SSc-PAH and AA had the worst prognosis.
Study limitations
There are some study limitations that need to be taken into account. First, since there was no routine electrocardiographic monitoring, if arrhythmias were asymptomatic, some AA could be missed, thus leading to an underestimation of true incidence. Second, the presence of higher PAWP in patients with AA could indicate that some of these patients might have occult LHD (heart failure with preserved ejection fraction). While we are unable to fully characterize this difference between groups, there was importantly no difference in recorded risk factors for LHD (systemic hypertension, diabetes, coronary artery disease). Third, this was a single-center experience with unequal sample sizes between IPAH and SSc-PAH, which merely reflects referral bias to our program. As the analysis between IPAH and SSc-PAH is based on small and unmatched patient populations, interesting trends can be observed but definitive conclusions cannot be made.
Furthermore, the present study did not compare the different treatments of AA, and thus optimal treatment of these patients remains elusive and requires further investigation. Restoration and maintenance of sinus rhythm appear to be of mechanistic importance for preserving RV function and are important treatment objectives in this fragile patient population. However, optimal medical therapy remains unclear, since most of the existing anti-arrhythmic agents have relevant side effects or contraindications in patients with PAH. In addition, electrophysiological and anatomic mapping of the RA in patients with IPAH highlights the presence of RA electrical tissue remodeling, as patients were found to have prolongation of sinus node recovery times, reduction in tissue voltage with an increase in electrically silent areas, increased complex fractionated activity, and atrial conduction slowing. 2 A recognition of these changes associated with longstanding PAH is critical to understanding why response to pharmacologic and catheter-based strategies to restore and maintain sinus rhythm may be associated with lower success than in control patients without PAH who develop AA. 28 However, despite the robust myocardial remodeling observed in these patients, limited data suggest that this approach is feasible, safe, and effective in this patient population.28–30 Given the overall tenuous clinical status of these patients, long periods of atrial arrhythmia are likely to be detrimental to clinical stability and long-term outcomes, and pursuing ablation may be clinically beneficial for this patient population.
Conclusion
In conclusion, the onset of AA in patients with PAH is a clinically relevant issue. The occurrence of AA is associated with high morbidity and mortality, particularly if recurrent or persistent, highlighting the importance of atrial systole, atrioventricular synchrony, and heart rate control to total right heart function in this patient population. Interestingly, the survival of patients with IPAH, typically better in comparison to other forms of PAH, becomes comparable to that of SSc-PAH patients in the presence of AA, suggesting atrial arrhythmias are not only a cause of clinical decline but also a marker of progressive right heart disease. Further studies are needed to define the best approach to arrhythmia management in PAH.
Footnotes
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research is supported by NIH/NHLBI R01 HL114910 and U01HL125175-01 (PMH). VM received a grant from Italian Society of Cardiology-Merck Sharp & Dohme.
