Abstract
Endothelial dysfunction is a major player in the development and progression of vascular pathology in pulmonary arterial hypertension (PAH), a disease associated with small vessel loss and obstructive vasculopathy that leads to increased pulmonary vascular resistance, subsequent right heart failure, and premature death. Over the past ten years, there has been tremendous progress in our understanding of pulmonary endothelial biology as it pertains to the genetic and molecular mechanisms that orchestrate the endothelial response to direct or indirect injury, and how their dysregulation can contribute to the pathogenesis of PAH. As one of the major topics included in the 2017 Grover Conference Series, discussion centered on recent developments in four areas of pulmonary endothelial biology: (1) angiogenesis; (2) endothelial-mesenchymal transition (EndMT); (3) epigenetics; and (4) biology of voltage-gated ion channels. The present review will summarize the content of these discussions and provide a perspective on the most promising aspects of endothelial dysfunction that may be amenable for therapeutic development.
Keywords
Introduction
Pulmonary arterial hypertension (PAH) is a life-threatening disorder characterized by progressive elevation of pulmonary pressures that lead to right heart failure and death. 1 With an estimated prevalence of ∼12–15 per million, PAH is considered a rare disease that predominantly targets women and has a poor prognosis with a three-year survival rate of 58%. 2 Although vasodilation therapies can provide temporary symptomatic relief, PAH progresses until lung transplantation is the only option. 2 Thus, there is an unmet need for novel therapeutic approaches that can effectively target the underlying pathological mechanisms driving disease progression and alter the natural history of this devastating disease.
The abnormal rise in pulmonary pressures seen in PAH is a consequence of increased pulmonary vascular resistance (PVR) due to progressive loss and obliteration of small pulmonary arteries. The initial trigger is thought to be a combination of genetic and environmental factors that lead to endothelial cell (EC) injury and impaired vascular regeneration, resulting in aberrant vascular remodeling and loss of small pulmonary arteries.1–4 The abnormal remodeling ranges from marked hypertrophy and hyperplasia of the medial layer to cell-rich (i.e. plexogenic) lesions that cause luminal obstruction and reduced pulmonary blood flow.
At present, none of the available therapeutic modalities have shown the potential to prevent small vessel loss, induce vascular regeneration, and/or reverse plexogenic arteriopathy. A major barrier to the development of effective treatments for PAH is an incomplete understanding of the signaling pathways that drive the endothelium to produce and respond to vasoactive factors that orchestrate angiogenesis, the process by which damaged vessels are regenerated. These new blood vessels, comprising arteries, capillaries, and veins, are necessary for normal tissue growth and response to injury.3,4 When the dynamic regulation of angiogenesis is disrupted, these processes can rapidly become contributing factors to pathogenic processes. 5 For example, multiple cancers exploit angiogenic and vasculogenic pathways to supply oxygen and nutrients to tumors, driving their growth and fueling inflammatory responses.6–8 In addition, angiogenesis and vasculogenesis are relevant to many non-cancerous conditions. Specifically, impaired and/or inappropriate angiogenesis and vasculogenesis have been linked to multiple cardiovascular diseases, such as peripheral vascular disease, 9 coronary artery disease, 10 and diabetic retinopathy,11,12 and may also occur in PAH pathogenesis. 13
Angiogenesis—driven by the coordinated action of ECs—involves remodeling of the extracellular matrix and recruitment of mural cells, such as pericytes, fibroblasts, and smooth muscle cells (SMCs). There are two significant forms of angiogenesis: (1) intussusceptive angiogenesis, where new vessels are formed through pillars that result from the fusing of the plasma membrane of pre-existing vessels; and (2) sprouting angiogenesis, which is driven by coordinated movements of ECs in response to cytokine gradients and tissue hypoxia (Fig. 1). In sprouting angiogenesis, a highly motile, filopodia-enriched “tip cell” acts as the “pathfinder” that creates a path for its adjacent neighbors (the highly proliferative “stalk” cells) through the extracellular matrix. As a result of the coordinated action of tip and stalk cells, a new vessel branch arises that reaches through zones of hypoxia to merge with neighboring vessels for the re-establishment of blood flow and oxygen delivery to these areas. Through a stochastic process, any EC is intrinsically capable of becoming a tip or stalk cell, or to remain as a quiescent EC, or phalanx cell, in the stable vessel.
14
Interestingly, individual ECs actively rotate between each phenotype by the rapid induction and repression of a complex genetic program driven by the integration of extracellular pro- and anti-angiogenic chemotactic cues from surrounding tissues and neighboring vascular ECs.15–17 Furthermore, the ratio of tip cells to stalk cells is crucial for the proper formation of new vessels and is tightly regulated by cross-talk among several signaling pathways, such as ephrin, notch, bone morphogenetic protein (BMP), and Wnt signaling (Fig. 1).5,17–21
Mechanism of sprouting angiogenesis. When blood vessel is damaged or under proangiogenic factors activation, the pulmonary artery smooth muscle cells (PASMC) and pericytes (blue) leave the arterial wall and endothelial cells (PAECs) (red) start to degrade the basal lamina (1). PAECs then migrate in response to cytokine gradients and tissue hypoxia and create sprouts (2). The sprouts split and growth as the PAECs proliferate (3) until perivascular cells are recruited and a new basal lamina is created to stabilize the new microvessels.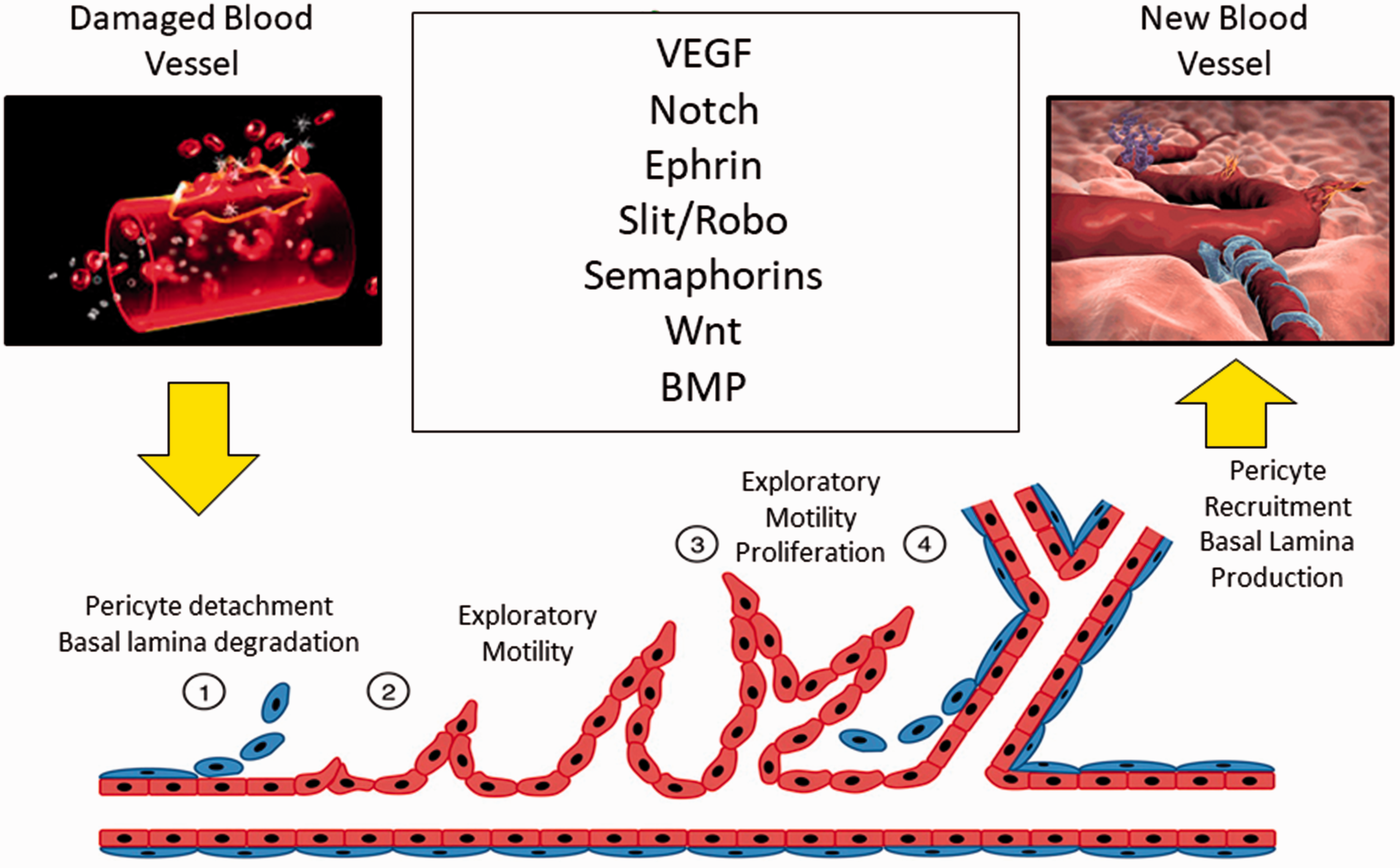
Any effort to understand the basis of the vascular pathology seen in PAH must take into consideration the contribution of each of the major signaling pathways that orchestrates angiogenesis. One of the most important is the vascular endothelial growth factor (VEGF) pathway, a crucial regulator of vascular development.22,23 In the setting of hypoxia, there is an increase in the expression of the ligand VEGF-A, which upon its release interacts with the VEGF receptor (VEGFR) 2 and triggers a complex signaling cascade that results in endothelial proliferation, survival, motility, and ultimately angiogenesis. 22 While the action and regulation of the VEGF pathway are well characterized in the systemic circulation, little is known about these functions in the pulmonary circulation. Immunohistochemical studies performed in lung sections of PAH patients have revealed that plexogenic lesions contain high levels of VEGF-A and VEGFR2, supporting the argument that these cells may be of endothelial origin and that the plexogenic lesions may arise from a process of “misguided” or inappropriate angiogenesis. 24 While these findings argue for pathological “hyperactivation” of the VEGF pathway, studies in pulmonary microvascular ECs (PMVECs) isolated from PAH patients suggest that, despite VEGF stimulation, these cells have a limited capacity to tolerate injury and assemble smaller vascular tube networks in vitro compared to healthy PMVECs.25–27 These findings suggest that, despite increased expression of VEGF ligands and receptors, PMVECs in PAH may have intrinsic defects that prevent them from appropriately responding to VEGF-A stimulation.
Besides being a master regulator of angiogenesis, the VEGF pathway is also known to cross-talk with an extensive network of signaling also implicated in proper vessel assembly. Research efforts should, therefore, prioritize dissection of these critical interactions along with the epigenetic and genetic alterations responsible for unleashing the angiogenic response required to regenerate lost or injured vessels. This review will summarize some of the most recent discoveries in the evolving landscape of angiogenesis research in PAH and how therapeutic interventions can be tailored to address the dysregulation associated with vascular remodeling in patient lungs.
Endothelial-to-mesenchymal transition in pulmonary hypertension
Aberrant vascular remodeling implicated in the increased PVR include concentric arterial wall thickening, occlusive intimal lesions, and neomuscularization of precapillary arterioles. Concentric pulmonary vascular wall thickening is characterized by significant intimal and medial hypertrophy due to dysfunction of pulmonary artery ECs (PAECs) and elevated proliferation/attenuated apoptosis of pulmonary arterial SMCs (PASMCs). While an imbalanced ratio of proliferation/apoptosis in PASMCs mainly contributes to the medial thickening, altered endothelial function contributes to neointimal formation, intimal thickening, and distal pulmonary arteries obliteration. 28
Pathological studies indicate that cell types found in the intraluminal occlusions express mesenchymal markers and SMC markers. 29 Increased expression of smooth muscle α-smooth muscle actin (α-SMA or Acta2) is a nearly universal finding in the remodeled pulmonary arteries and the occlusive lesions in patients with PAH. Until recently, resident PASMCs, via concentric migration, were considered the predominant source of the newly appearing α-SMA-expressing cells in the obliterative lesions. However, recent studies provided evidence that other sources might play an important pathogenic role, such as dedifferentiated α-SMA-positive cells through the KLF signaling pathway 30 and myofibroblasts derived from ECs via endothelial-to-mesenchymal transition (EndMT).
EndMT is a process by which ECs acquire a mesenchymal phenotype in association with the downregulation of EC-specific genes, such as platelet EC adhesion molecule 1 (PECAM1 or CD31) and vascular endothelial cadherin (VE-cadherin or CD144), and with the upregulation of SMC-specific genes, such as α-SMA and fibroblast-specific genes like vimentin. TWIST1, SNAIL (or SNAI1), and SLUG (or SNAI2) are transcription factors that initiate EndMT (and epithelial-to-mesenchymal transition). The obtained mesenchymal cells can then differentiate into other phenotypes such as fibroblasts, chondrocytes, or osteoblasts.31–36 As such, EndMT is considered to be a major contributor to tissue regeneration.
During EndMT, ECs lose their junctions to the endothelium and gain migratory and proliferative capacities as they gradually switch from endothelial to a mesenchymal phenotype. Recently, EndMT has emerged as a critical player not only in the pathogenesis of tissue fibrosis but also in the pulmonary vascular remodeling processes seen in PAH.37–39 In patients with PAH, the presence of EndMT was confirmed in remodeled arteries as typified by cells expressing both endothelial (CD31, CD34, VE-cadherin) and mesenchymal markers (αSMA, fibronectin 1). A signature of EndMT, including decreased expression of endothelial junction protein p120-catenin, increased expression of mesenchymal markers phospho-vimentine and over expression of transcription factors TWIST1, SNAIL, and SLUG was found in lungs from PAH patients and in an experimental pulmonary hypertension (PH) model using monocrotaline (MCT).37,39 It has been reported that 5% of ECs from the experimental PAH Sugen 5416/hypoxia mouse and systemic sclerosis-associated PAH also express both endothelial and mesenchymal phenotypes. 38
The molecular mechanisms inducing EndMT in PAH remain elusive with several pathways likely implicated. For example, the transforming growth factor β (TGF-β) signaling pathway is critical to PAH development and is also an important player in EndMT. Indeed, TGF-β induces α-SMA and type I collagen expression in detriment to VE-cadherin expression in PAECs. 40 Similarly, activation of the Wnt/β-catenin axis by TGF-β can potentiate EndMT by repressing VE-cadherin messenger RNA (mRNA) expression and by promoting vimentin and SLUG mRNA expression. 41 EndMT may also occur after exposure of PAEC to inflammatory molecules, such as IL-1β and TNF-α, or in response to vasoactive molecules like ET-1, all of which are implicated in PAH etiology.42,43 Another hallmark of PAH is the disruption of bone morphogenetic protein receptor type 2 (BMPR2) signaling. BMPR2 expression is reduced in idiopathic PAH and a mutation in BMPR2 are found in 70% of familial PAH and 25% of idiopathic PAH.44–46 Interestingly, Hopper et al. recently demonstrated that dysfunctional BMPR2 signaling promotes EndMT via activation of High Hobility Group AT-hook 1 (HMGA1) and SLUG pathways. 47
EndMT can also be controlled epigenetically by several microRNAs (miRNAs), including miR-21 which is critical to PAH development.48,49 TGF-β can significantly increase miR-21 expression in ECs and induce EndMT through an AKT-dependent mechanism. 50 Finally, HIF-2α, a key regulator of the molecular response to hypoxia, was also linked to EndMT. Besides its endothelial effect on vasoconstriction, through arginase 51 and endotheline-1, 52 and on PASMC proliferation, through endothelial CXCL12 overexpression, 53 it has been recently reported that HIF2-α also upregulates SNAIL and SLUG. 39 Under normoxic conditions, HIF2-α is mainly under control of prolyl hydroxylase domain protein 2 (PHD2) that enables its proteasomal degradation.54,55 Interestingly PHD2 expression was found decreased in PAECs from PAH patients which leads to abnormal HIF2-α stabilization under normoxic conditions and SNAIL/SLUG upregulation. 39 The endothelial depletion of PHD2 gene (egln1) in mice leads to spontaneous severe PAH,39,52,53 which was associated with overexpression of EndMT markers in remodeled vessels. 39
Epigenetic regulation of endothelial cell phenotypes in pulmonary hypertension
Genetic information is stored in a linear sequence of complementary DNA base pairings, which is further organized into a hierarchical biological infrastructure upon which additional regulation may be exerted to influence gene expression. This concept is known as epigenetics. Classically, epigenetics is defined as the study of changes in phenotype and gene expression not due to alterations in the nucleotide sequence but rather through the chemical modifications of DNA and its associated organizing histone proteins. 56 Epigenetic modifications are remarkably stable—thus conferring heritability—yet also highly dynamic reorganizations of chromatin that maintain specific cellular phenotypes and alter activity states via the selective expression or repression of various genetic programs.
Our understanding of PAH as a disease with multifactorial etiologies suggests that its manifestation may be due to a series of independent mechanisms converging into a single clinical phenotype. Moreover, instances of unexplained biological phenomena in PAH indicate that a role for epigenetic influence may exist. For example, a genetic predisposition to heritable PAH has long been established with known causative mutations, such as the autosomal dominant mutation in the BMPR2; however, the mutation in BMPR2 demonstrates markedly reduced penetrance in its carriers and, when coupled with the high rates of “sporadic” PAH, further confirms a requirement for other inciting stimuli in disease initiation. 56 Consequently, the inability of a singular sequence alteration to explain PAH pathophysiology strengthens arguments in favor for a role of epigenetic influence in disease manifestation.
ECs demonstrate an initial predisposition to apoptosis followed by an apparent resistance to apoptosis and a secondary hyperproliferative phenotype.57,58 When PAECs are isolated from the lung vessels of patients with longstanding PAH and cultured ex vivo, they maintain this resistance to apoptosis and hyperproliferative state, which is suggestive of a heritable and stable phenotype.
59
Accordingly, the observations of both endothelial apoptosis and proliferation in PAECs provides the foundation for a spatiotemporal model of EC reprogramming in PAH that may be, in part, mediated via epigenetic mechanisms. In fact, EC dysfunction in PAH models has been shown to act through DNA methylation, histone protein modifications, and non-coding RNAs, which, when taken together, may help reconcile the observed biological phenomena into a more unifying and cohesive epigenetic theory of PAH (Fig. 2).
Mechanisms of endothelial epigenetic regulation. in PH. The transcription of DNA is repressed via the covalent addition of a methyl group at the C5 position on cytosine bases by DNA methyltransferase. Methylation sterically hinders the binding of molecules necessary for messenger RNA synthesis, thereby preventing gene expression. Histones can be modified with the addition or removal of various molecules. The acetylation of histones alters chromatin structure to allow for enhanced gene expression. Likewise, the deacetylation of histones compacts chromatin and reduces the availability of genes for expression. RNA interference occurs through non-coding RNA. miRNAs negatively regulate gene expression by binding to a mRNA and targeting it for degradation or preventing its translation. lncRNAs are more widespread in their effects with the ability to bind to chromatin, RNA, or protein to modify function at various points both before and after the transcriptional and translational processing of genetic information. These various mechanisms of epigenetic regulation have been shown to have roles in the pathogenesis of PH. (Confocal image is reproduced from the Journal of Clinical Investigation with permission from the American Society of Clinical Investigation.)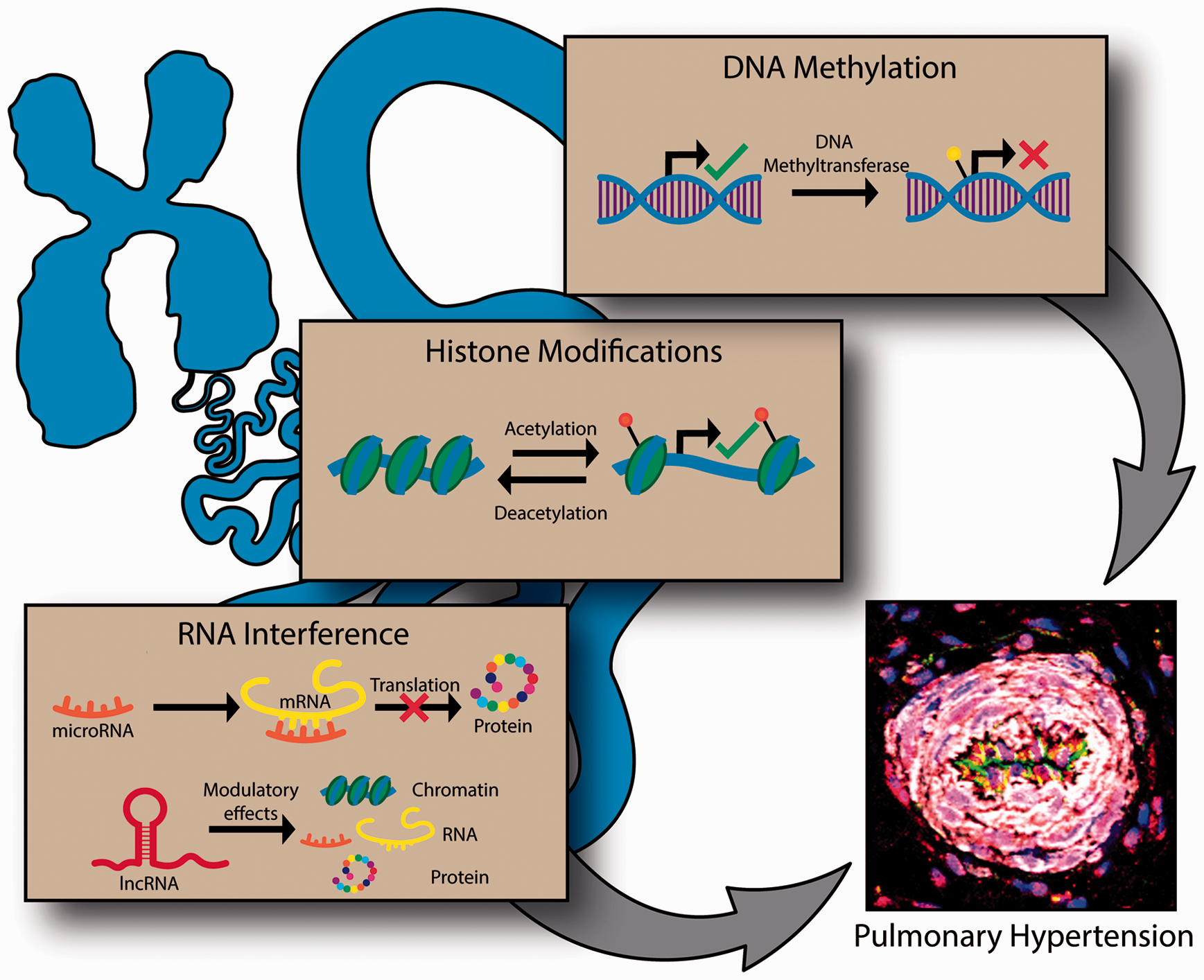
Mechanisms of epigenetic regulation: DNA methylation, histone post-translational modifications, and RNA interference
One of the most well-studied mechanisms of epigenetic regulation is the repression of DNA transcription via the methylation of DNA at cytosine residues in CpG dinucleotide sequences, where a methyl group is covalently attached at the C5 position of the nucleotide base by DNA methyltransferases. 60 These CpG islands are often found in the promoter or enhancer regions of genes, thereby conferring a mechanism through which DNA methylation can “shut off” or reduce gene expression through steric hindrance. Likewise, hypomethylation of CpG islands within promoter regions can lead to overexpression of genes. Within normal biology, DNA methylation is a stable yet highly dynamic mechanism in developmental and cellular differentiation processes, such as through the selective expression of tissue-specific gene programs. 61 The relevance of possessing both characteristics allows for cellular phenotypes to exist within a spatiotemporal framework, where cellular activity states can adapt to microenvironmental stimuli and maintain such activity states as cells divide. On the other hand, this mechanism of maintaining cellular identity in the face of external stress can also serve as a substrate for pathologic manifestations, which is increasingly demonstrated in various human diseases. 62 In the case of PAH, external stimuli may result in specific methylation patterns within vascular cells that alter cellular activity states to resist apoptosis initially and then subsequently become hyperproliferative.
The next level of organization of genetic material is within a functional unit known as the nucleosome. The nucleosome is an octameric complex of histone proteins with two copies of each H2A, H2B, H3, and H4 which DNA wraps tightly around. The nucleosome confers an added layer of epigenetic modification in which its chemical modification can restructure chromatin to control the accessibility and thus transcriptional activity of a given gene. Post-translational modifications of histones can occur in many ways, but the most common modification is acetylation. Histone acetylation often occurs at H3 and H4, where increased acetylation enhances gene expression, and decreased acetylation represses gene expression. Unlike DNA methylation, however, histone post-translational modifications are not stable, allowing for fluid and dynamic alterations in the structure of chromatin.
Lastly, RNA interference is mediated through non-coding RNA—transcripts from genes that do not code for proteins. Non-coding RNA is arbitrarily divided by nucleotide length as either small non-coding RNA (<200 nt) or long non-coding RNA (>200 nt). 63 miRNAs represent a type of small non-coding RNA that are evolutionarily conserved and negatively regulate gene expression at a post-transcriptional level by either targeting the mRNA transcript for degradation or through inhibition of its translation. Long non-coding RNAs (lncRNAs), on the other hand, can bind to chromatin, RNA, or protein to modify cellular function at multiple points before and after transcriptional and translational processes of genetic information. Within recent years, the functions of miRNAs have expanded to include direct regulation of other epigenetic mechanisms, such as DNA methylation and histone modifications. 64 This suggests that certain miRNAs may serve as master regulators in pathogenic, epigenetically mediated pathways, and that the selective targeting of regulatory miRNAs may serve as a viable therapeutic strategy.
DNA methylation in pulmonary hypertension
A recently published study examined differential gene expression through DNA methylation status in PAECs from PAH patients versus controls. DNA methylation profiles from both idiopathic and heritable PAH patients demonstrated only three promoter sites of differential methylation, thereby presenting a remarkably similar methylation profile despite the difference in etiologic origin. 65 Moreover, there was significant differential methylation in genes related to cholesterol and lipid transport pathways between PAH and control patients, such as ABCA1 (ATP-binding cassette 1), ADIPOQ (adiponectin), and APOA4 (apolipoprotein A4). 65 Interestingly, ABCA1 belongs to the super-family ATP binding cassette (ABC) transporters, which has demonstrated significance to pulmonary hemostasis in cases of persistent PH of the newborn secondary to loss-of-function mutations in ABCA3.66–68 The relevance of ABCA1 was further demonstrated using monocrotaline (MCT)-induced PH rat models. In this case, the administration of a positive regulator of ABCA1 expression—the liver X receptor-activating ligand T0901317—improved MCT-induced PH at both hemodynamic and histologic measures. 65 The significance of this work demonstrates how, unlike genetic mutations, epigenetic markings such as DNA methylation are pharmacologically reversible, making them an attractive target for the treatment of PAH.
In persistent PH of the newborn, there is a failure of the pulmonary vasculature to relax at birth, resulting in high PVR, and the development of PH and severe hypoxemia. 69 In this patient population, decreased gene expression of endothelial nitric oxide synthase (eNOS) is observed in vitro in umbilical vein ECs cultured immediately postpartum; 70 however, as hypoxemia worsens, there is a compensatory increase in the expression of eNOS within the pulmonary vasculature. 71 The highly restricted expression of eNOS to the endothelium via epigenetic mechanisms suggested that similar mechanisms may also be implicated in PAH pathophysiology.72–76 Increased eNOS expression was also reported in a neonatal rodent model of persistent PH of the newborn induced by hypoxia and indomethacin when compared to controls. In this model, the increased expression of eNOS was associated with decreases in DNA methylation and increases in H3 and H4 histone acetylation within its promoter region, suggesting a regulation of eNOS via epigenetic mechanisms. 77
Histone post-translational modifications in pulmonary hypertension
The relevance of histone post-translational modifications in PAH has also been related to PAH pathogenesis. Recent studies reported that the use of histone deacetylase (HDACs) inhibitors had improved various animal models of PAH.78–81 In one such study, PAECs isolated from PAH patients demonstrated a reduced expression of myocyte enhancer factor 2 (MEF2) mediated by a concomitant nuclear increase in HDAC4 and HDAC5. 82 Selective pharmacological inhibition of these class IIa HDACs restored MEF2 activity in PAECs and rescued MCT-induced and Sugen-5416/hypoxia models of PH. Furthermore, this study established that MEF2 controls the expression of miR-424/503, two miRNAs previously determined to be involved in pulmonary vascular homeostasis. HDAC6 was also found increased in PAEC and PASMC and its inhibition by Tubastatin A improved PH in Sugen 5416/hypoxia and MCT rats. 81 Those results highlight a complex interplay of epigenetic mechanisms, where chemical modifications of DNA or histone proteins can unleash or repress other epigenetic mechanisms. Understanding how these mechanisms exist within a network is crucial to minimize non-specific and unintended alterations of therapeutic strategies.
More recently, there has been an increased appreciation for epigenetic readers, such as bromodomain (BRD)-containing proteins, in gene regulation. BRD-containing proteins recognize and bind to histones, where they serve as molecular scaffolds for the recruitment of transcriptional regulators to influence gene expression. 83 The role for one such member of this protein family, BRD4, was demonstrated to be overexpressed in lung tissue from PAH patients—serving as the first observation for the role of an epigenetic reader in PAH. 84 Moreover, this same study demonstrated that BRD4 influences over at least three oncogenes involved in the hyperproliferative, anti-apoptotic cellular phenotype observed in PAH, suggesting a broad epigenetic role in disease pathogenesis.
Endothelial-specific RNA interference in pulmonary hypertension
microRNAs in PAH
Although numerous miRNAs have been implicated in the pathogenesis of PAH, only a subset of those have been linked directly to an EC, cell-type specific dysfunction in this disease.49,85–87 As previously discussed, miR-424/503 have been established as critically vital components of EC homeostasis within the pulmonary vasculature. More specifically, disruption of apelin (APLN) signaling within PAECs results in increased fibroblast growth factor 2 (FGF2) and FGF receptor 1 (FGFR1) expression. 88 The downregulation of APLN—a positive regulator of miR-424/503—results in miR-424/503 downregulation and thus prevents their ability to negatively attenuate FGF2 and FGFR1 expression, thereby leading to a hyperproliferative phenotype observed in PAECs. This observed phenotype, however, can be reversed in vivo with the restoration of miR-424/503 in experimental models of PH. 88 Interestingly, it was later demonstrated that the APLN-miR-424/503-FGF2 axis and ultimately EC proliferation is under the control of the miR-130/301 family—yet another example of the complex interplay among various epigenetic mechanisms. 89
Similarly, the miR-17/92 cluster has shown relevance in EC biology and angiogenesis. In human umbilical vein ECs (HUVECs), overexpression of miR-17 demonstrated an inhibition of endothelial angiogenic cell sprouting in vitro and in vivo. 90 Moreover, in HUVECs overexpressing miR-92a, there was downregulation of integrin α5, which directly attenuated expression of eNOS. 91
In order to sustain the hyperproliferative state observed in PAECs derived from PAH patients, miR-210 has shown regulatory roles in the facilitation of the metabolic shift toward glycolysis under hypoxic conditions by targeting hypoxia-inducible factor. 92 miR-210 downregulated expression of iron-sulfur cluster assembly proteins 1 and 2 (ISCU1/2)—prosthetic groups necessary for the proper functioning of the citric acid cycle and electron transport chain.93–95 Specifically, downregulation of ISCU1/2 by hypoxic miR-210 attenuated Fe-S-dependent mitochondrial respiration in favor of glycolysis, thereby promoting a metabolic shift to sustain a hyperproliferative phenotype in PAECs. 95 Although this metabolic shift is acutely protective, its chronic repression promotes PH in rodent models. 96
Analysis of miRNA expression within ECs reveals that miR-21 is highly expressed. 97 In one study, hypoxia and BMPR2 signaling—two stimuli involved in the pathogenesis of PH—independently upregulated miR-21 in PAECs in vitro. Furthermore, miR-21 directly repressed RhoB expression and Rho-kinase activity, thereby resulting in decreased angiogenesis and vasodilation. This finding was corroborated in rodent models of PH and in human PH, where miR-21 expression is upregulated in pulmonary tissue demonstrating a protective role of miR-21. As would be expected, miR-21 -/- mice demonstrated severe PH characteristics. 48 Another study demonstrated the role of miR-21 in PAEC apoptosis. When subjected to apoptotic stimuli, PAECs induced a programmed cell death 4 (PDCD4)/caspase-3 apoptotic pathway, which could be indirectly repressed by delivery of a miR-21 mimetic. In miR-21 -/- mice, there was activation of the PDCD4/caspase-3 axis and the development of PH. Similarly, miR-21 overexpressing mice demonstrated reduced PDCD4/caspase-3 axis activation and were partially resistant to PH-inciting stimuli. 98 On the other hand, however, studies have also demonstrated that inhibition of miR-21 may have therapeutic relevance. In a chronic hypoxia PH mouse model, the inhibition of miR-21 reversed pulmonary vascular remodeling and decreased the proliferation of PASMCs in vitro. 99 In another study, increased levels of the endogenous eNOS inhibitor asymmetric dimethylarginine (ADMA) is contributory in PH pathogenesis, and reduced levels of its metabolizing enzymes—dimethylarginine dimethylaminohydrolases (DDAH) 1 and 2—which are under the regulation of miR-21. Hypoxic exposure of human PAECs in vitro upregulated miR-21 and downregulated DDAH1 to induce EC dysfunction, which could be prevented by DDAH1 overexpression or miR-21 blockade. 100 In addition to influencing over other epigenetic mechanisms, miRNAs have demonstrated the ability to act as paracrine signals in cell–cell communication. Using multiple stimuli in the expression of the miR-143/145 cluster, it was demonstrated that upregulation of miR-143 in PASMCs is excreted via exosomes and taken up by neighboring PAECs to induce angiogenesis and cell migration. 101
Other miRNAs have shown EC-specific activities in the diseased pulmonary vasculature. For instance, the miRNA let-7b was found to have differential expression among various organ-specific ECs, suggestive of a potential role for miRNA signatures in the diversity of EC phenotypes. 102 Additionally, circulating let-7b is decreased in a patient population of chronic thromboembolic PH. In this same study, let-7b was shown to directly regulate the expression of endothelin-1 and TGF-β receptor 1 in PAECs. 103 In PAECs under conditions of hypoxia, there is an observed upregulation of miR-27 a that directly reduces peroxisome proliferator-activated receptor gamma (PPARγ) and increases endothelin-1 to stimulate PAEC proliferation in vitro. 104 In another study, increased miR-138 was found to downregulate expression of the calcium-binding protein S100A1 in ECs in a hypoxia-dependent manner, which is a critical activator of eNOS, thereby contributing to EC dysfunction. 105
Long non-coding RNAs in PAH
More recently, the role of lncRNAs in PAH has begun to be elucidated over the past few years. As early as 2015, comprehensive lncRNA and mRNA profiling of endothelial tissues from the pulmonary arteries of chronic thromboembolic PH patients was conducted with microarray analysis. Significant alterations were observed in the lncRNAs NR_036693, NR_027783, NR_033766, and NR_001284, which demonstrated through gene ontology and pathway analysis possible regulatory roles in disease pathogenesis either through regulation of mRNAs or vice versa. 106
Another study published in 2016 utilized next-generation sequencing technologies to examine transcriptomic changes occurring in HUVECs under hypoxic stress, demonstrating differential expression of lncRNAs H19, MIR210HG, MEG9, MALAT1, and MIR22HG. 107 Knockdown of H19 in vitro decreased HUVEC growth and promoted cellular accumulation in G1 of the cell cycle, while also decreasing HUVEC ability to form capillary-like structures. 107 Moreover, knockdown of MALAT1 in ECs increased cell migration in vitro, while reducing capillary density and blood flow in a model of hind limb ischemia. 108 Interestingly, a paper published this year described a functional polymorphism in MALAT that contributes to PAH in a Chinese cohort. 109 Lastly, an epigenetically controlled lncRNA—MANTIS—is controlled by the histone demethylase JARID1B. In MCT-induced PH rat models and PAH patients, MANTIS is downregulated, and when modeled in vitro through small interfering RNA silencing or CRISPR/Cas9 deletion of MANTIS inhibited angiogenic sprouting of ECs. 110
Ion channels and EC dysfunction
Ion channels are key regulator of vasoconstriction and proliferative/apoptotic phenotypes, and are therefore involved in PAH pathogenesis. 111 Their role is complex and may differ among vascular cell types. In this section, we will focus on the most studied endothelial ion channels that can contribute to altered functions of the PAECs.
Transient receptor potential channels
Transient receptor potential (TRP) channels are a group of voltage-independent cation channels located mostly in the cytoplasm of numerous vascular ECs, including PAECs. More than 15 TRP channels from different subfamilies, including canonical TRP (TRPC), melastatin TRP (TRPM), and vanilloid TRP (TRPV), are expressed in human PAECs. 112 Numerous studies demonstrated that certain TRP channels regulate vascular function. For example, TRPC1/4/6 are involved in the control of vascular remodeling and vascular permeability,113,114 TRPV1/4 play a role in the regulation of vascular tone and vascular remodeling, TRPM6/7 contribute to vascular remodeling, and TRPM2/7 mediate the response to oxidative stress.
Canonical TRP channels
Accumulating evidence suggests that PAEC and endothelial cytosolic Ca2+ play a major role in the initiation of pulmonary vascular remodeling during PAH. The endothelium or PAEC is believed to be a source of proteins and molecules that stimulate PASMC proliferation in a paracrine manner in patients with PAH. PASMC isolated from healthy subjects are quiescent within the medial layer of the pulmonary artery wall. During vascular remodeling or when the endothelium is injured, expression of endothelium-derived growth factors (e.g. platelet-derived growth factor [PDGF] and VEGF) in PAECs is upregulated. This change contributes to the subsequent alterations in the growth, migration, and differentiation of PASMCs in patients with PAH. PDGF released by PAECs upregulates TRPC6, Orai2, and STIM2 in PASMCs, essential components of receptor-operated Ca2+ channels (ROC) and store-operated Ca2+ channels (SOC).115–117 Genetic deletion or pharmacological inhibition of TRPC6 significantly attenuates both chronic hypoxia-mediated pulmonary vascular remodeling and acute hypoxia-induced pulmonary vasoconstriction. 118 Hypoxia-induced expression of TRPC6 is mediated by Notch signaling, 118 which in turn plays a major role in EndMT, alterations of cell phenotype from a cobblestone-like shape to a spindle-shaped fibroblast-like morphology, and increased endothelial proliferation in patients with idiopathic PAH.119–121 Accumulating data indicate that TRPC1/6 also regulate endothelial permeability by enhancing intracellular Ca2+ concentration,122,123 while TRPC1/4 interact with STIM1 and Orai1 to form SOC and disrupt endothelial barrier function. 124 Recently Orai1 and Stim1 have been established as key players in VEGF-mediated Ca2+ entry.125,126 Interestingly, knockdown of Stim1/2 and Orai1 inhibited EC proliferation but Orai1 silencing had more effect than that of Stim proteins. 125 Orai1 and TRPC1 contribute to cytosolic Ca2+ increase following store depletion but have different cellular functions. TRPC1-mediated Ca2+ entry is the primary regulator of KCa channel and partially activates NF-κB pathway while Orai1-mediated Ca2+ entry contributes to NFAT signaling. 127 This evidence suggests that activation of SOC is important stimuli for EC morphological change 128 and that EndMT could be a Ca2+-dependent event in PAH.
We demonstrated that TRPC4 might also participate in hypoxia-induced vascular remodeling. 129 Increased expression of TRPC4 in human PAECs exposed to hypoxia was associated with capacitative Ca2+ entry via SOC, which is considered an important mechanism for raising cytosolic Ca2+ concentration in PAECs. Interestingly, it results in the increased binding of activating protein-1 (AP-1) transcription factors involved in cell proliferation and migration by promoting genes such as VEGF and PDGF. These data allow us to suggest a link among endothelial TRPC4/6 activation, Ca2+ entry, and pulmonary vascular remodeling during PAH.
Recent studies reported that TRPC channels could also be involved in the resistance of ECs to apoptosis. For example, Ca2+ entry through TRPC1 channels is required to protect HUVECs from apoptosis via NF-kB signaling.130,131 Inhibition of NF-kB pathway reverses EndMT in animals with MCT-induced PH and human PMVECs treated with TGF-β1. 132 Interestingly, that 15% cyclic stretch for 48 h induces EndMT and changes cell morphology in HUVECs. 133 Mechanical stretch upregulates another TRPC3 that leads to Ca2+ influx and activation of the NF-kB pathway; however, the role of TRPC channels in the development of EndMT remains unknown.134,135
Melastatin TRP channels
At least three endothelial melastatin TRP channels, TRPM2, 4, and 7, are known to be activated by oxidative stress. Numerous studies showed that these channels modulate oxidative stress-induced cell death136–138 and endothelial proliferation. 139 However, different splice variants of TRPM2 (long and short isoforms) and their roles in tumor growth have been identified in neuroblastoma cells. 140 Cells expressing the short-length isoform of TRPM2 had reduced Ca2+ entry which led to reduced HIF-1/2α activation due to oxidative stress, increased mitochondrial dysfunction, and decreased cell viability. On the other hand, cells expressing the full-length isoform of TRPM2 had higher Ca2+ entry which led to increased HIF-1/2α activation and higher cell proliferation and survival. As previously described, elevated HIF-2α in PAEC might play a key role in PAH pathogenesis through arginase and endothelin-1 overexpression which promote vasoconstriction,51,52 and through CXCL12 and SNAIL/SLUG upregulations which contribute to vascular remodeling in PAH.39,53 Furthermore, the report by Ding et al. postulated that upregulation of endothelial TRPM4 channel in response to oxidative stress is connected with endothelial lesions. 141 The authors suggest that oxidative stress is one of the mechanisms underlying aldosterone-induced endothelial injury in hypertensive patients. Downregulation of TRPM7 prevents endotoxin-induced endothelial fibrosis, suggesting that the involvement of the subunit in the EndMT mechanism. 142 The direct role of TRPM channels in EndMT needs to be fully understood, but recent reports provided evidence that these calcium-permeable ion channels are involved in calcium-dependent epithelial-to-mesenchymal transition (EMT) induction in cancer cells.143,144 Moreover, TRPM7 may play a role in the cellular phenotype changes of PASMC by phosphorylating annexin A1, a Ca2+-dependent membrane-binding protein. 145 Lately, Yi et al. confirmed that upregulation of annexin A1 mediates hypoxia-induced pulmonary arterial remodeling in the development of PH. 146
Vanilloid TRP channels
Published data on the role of vanilloid TRP channels indicate that these channels are involved in the regulation of endothelial function. Thus, Ca2+-mediated activation of TRPV1 channels ameliorates EC inflammation, and vascular oxidative stress improves endothelium-dependent vasorelaxation and protects animals from systemic hypertension through the eNOS/NO pathway.147–150 Simvastatin activates TRPV1 and leads to the formation of the Ca2+/calmodulin-dependent protein kinase II- eNOS (CaMKII-eNOS) complex as well as inhibits TGF-β1–induced EndMT in vitro.151,152 Interestingly, we recently revealed that upregulated TRPV1 had the opposite effect in PASMCs and could contribute to idiopathic PAH due to augmented Ca2+ influx and excessive PASMC proliferation. 153 Genetic ablation of TRPV1 markedly enhanced TGF-β1 and VEGF expression, resulting in post-myocardial infarction fibrosis. 154 Geng et al. speculate that the long-term consumption of chili-pepper-rich diets can decrease the risk of cancer development because it promotes TRPV1 level and inactivates NF-κB signaling, thereby reducing lung epithelial proliferation and EMT. 155 Surprisingly, capsaicin (an ingredient of chili pepper) induces apoptosis in human small cell lung cancer cells via TRPV6 and but not TRPV1. 156 The authors reported a robust expression of the TRPV6 receptor in patients but no expression in normal lung tissues. Also, capsaicin induced very little apoptosis in normal lung epithelial cells. TRPV5 and 6 are the only known Ca2+-selective channels within TRP family. They are involved in a higher proliferation rate, increasing cell survival and apoptosis resistance in human cancer cells.157,158 Little is known about TRPV2 and 4 channels, but recent publications suggest a role in cell survival by regulating ERK- and Akt-pathways, respectively.159,160 It was also shown that increased lung endothelial permeability in response to 14,15-epoxyeicosatrienoic acid (14,15-EET) in rat lung requires Ca2+ entry via TRPV4 channels.161–163 More recently, it was shown that Ca2+ entry via TRPV4 channels selectively activates IK and SK, but not BK, channels; and that inhibition of IK and SK3 channel activity attenuates TRPV4-induced lung permeability. 164 Thus, these data suggest a functional link between TRPV4/IK/SK channels and Ca2+-dependent endothelial lung injury. Also in ECs TRPV4 acts as a mechanosensor. Both shear stress and agonist activation of TRPV4 leads to enhancement of EC proliferation and triggers collateral growth after arterial occlusion. 165
K+ channels
The membrane potential is an important regulator of cellular excitability. Therefore, it comes as no surprise that K+ channel activity plays a critical role in regulating pulmonary vascular tone. The resting membrane potential of PAECs typically falls in the range of −55 to −30 mV, which is close to the predicted equilibrium potential for K+ channels (–85 mV). Increased efflux or outward movement of K+ ions from the cytoplasm to the extracellular space leads to membrane hyperpolarization. A small change in K+ channel activity can have a significant impact on membrane potential. Downregulated or dysfunctional K+ channels can result in membrane depolarization which enhances Ca2+ entry via voltage-dependent calcium channels (VDCCs). Increased Ca2+ signaling in the pulmonary vasculature inevitably promotes excessive vascular remodeling and sustained vasoconstriction, two characteristic hallmarks of PAH. The main families of K+ channels identified in the pulmonary vasculature are: (1) voltage-gated K+ channels (Kv); (2) large-, intermediate-, and small-conductance Ca2+-activated K+ channels (BKCa, IKCa, and SKCa, respectively); (3) inward rectifier K+ channels (Kir); (4) ATP-sensitive K+ channels (KATP); and (5) two-pore-domain K+ channels (K2P). 166
Voltage-gated K+ channels
Another field of investigation in PH is focused on K+ channels. Kv channels are the most diverse family of K+ channel ubiquitously expressed in the pulmonary vasculature.167–169 There are currently more than 20 distinct Kv channels known to be expressed in the pulmonary vasculature. Although several Kv channels are ubiquitously expressed in ECs, very little is known about their function in the endothelium. A recent study suggests that Kv1.5 may play a major role in oxidative vascular endothelial injury. 170 It was demonstrated that pharmacological inhibition of Kv1.5 was capable of attenuating H2O2-induced EC apoptosis in rat carotid artery. Furthermore, targeted knockdown of Kv1.5 could mitigate EC injury, and decrease intracellular and mitochondrial ROS levels, whereas overexpression of Kv1.5 had the opposite effect.
Ca2+-activated K+ channels
KCa channels are activated by an increase in [Ca2+]cyt and membrane depolarization. These channels are subcategorized by their conductance: large (BK), intermediate (IK), and small (SK). Although all three groups are activated by intracellular [Ca2+]i, SK and IK display greater sensitivity to [Ca2+]i than BK channels. Furthermore, BK channels are highly voltage-sensitive, whereas SK and IK are predominately voltage-independent. Although all three subgroups of KCa channels are expressed in PASMCs and PAECs, BK channels are primarily expressed in PASMCs, while IK and SK channels are almost exclusively expressed in the PAECs. Increased expression of BK channels in PH associated with chronic obstructive pulmonary disease is linked to pulmonary vascular remodeling. 171 It was previously demonstrated that oxidized low-density lipoprotein (oxLDL), which plays an integral role in endothelial dysfunction, activates BK. Additionally, acetylcholine-induced NO synthesis is modulated by BK. 172 SK channels are preferentially localized to homocellular endothelial gap junctions and caveolin-rich domains and are linked with various connexins (Cx), while IK are preferentially localized at the sites of endothelial projections often related to myoendothelial gap junctions.173–176 Interestingly in PAECs, activation of KCa channels does not reduce calcium influx. Quite the opposite occurs as membrane potential hyperpolarization promotes calcium entry. As PAECs do not express VDCC, it is very likely that activation of TRP channels (TRPC1/3/4/6 and TRPV1/4) leads to an elevation of the electrochemical driving force for Ca2+.177,178 Endothelial IK and SK channels play a fundamental role in controlling vascular tone as they have been shown to contribute to PAEC membrane hyperpolarization, which in turn evokes NO synthesis to mediate NO-dependent vasorelaxation.179,180 Kefaloyianni et al. found that shear-stress can induce expression of several ion channel subunits, including KCa2.2, KCa2.3 (SK), and KCa3.1 (IK), in human coronary endothelial cells. Thus they suggested that altered expression of these ion channels may contribute to vascular pathologies associated with shear stress. 181 Another study focused on the relationship between ER-stress and IK/SK activity. It was indicated that IK/SK currents inhibited by the known ER stressor homocysteine, which ultimately leads to endothelial dysfunction. It is well established that coronary artery endothelial dysfunction is closely associated with diabetes. As such, Liu et al. demonstrated that diabetes significantly decreases endothelial SK/IK currents and endothelial-dependent relaxation compared with that of non-diabetics, suggesting that inactivation of endothelial SK/IK channels may contribute to endothelial dysfunction in diabetic patients. 182 In humans, diabetes during pregnancy is associated with an abnormal regulation of peripheral vascular tone in part due to vascular endothelial dysfunction.183,184 A recent study reported that IK channels play a prevalent role over SK channels in the initiation of endothelial K+ currents and vasodilation of uteroplacental arteries and that impaired function of IK channels contributes to diabetes-induced uterine endothelial dysfunction. 138 Because K+ channels are implicated in these endothelium-dependent responses, pharmacological activation of endothelial and/or smooth muscle KCa could prevent or reduce the occurrence of endothelial dysfunction. 185
Inward rectifier K+ channels
Inward rectifier K+ (KIR) channels conduct inward K+ current, however, little outward current; they are blocked by intracellular Mg2+ and Cs+ and extracellular Ba2+. KIR channels in PASMCs and PAECs are involved in setting the resting Em, preventing membrane hyperpolarization by the electrogenic Na+, K+-ATPase, mediating K+-induced vasodilation, and minimizing loss of intracellular K+. It was previously shown that pharmacologically increasing cGMP levels in bovine pulmonary artery and microvascular ECs causes membrane depolarization which is due, in part, to PKG-independent inhibition of KIR currents. It was suggested that this ensuing depolarization could be a protective mechanism that prevents EC barrier dysfunction by reducing the driving force for Ca2+ entry. 186 Additionally, suppression of KIR currents is one of the critical factors associated with hypercholesterolemia-induced endothelial dysfunction. 187
ATP-sensitive K+ channels
Native KATP channels are voltage-dependent channels that have low open probability under basal conditions. KATP channels are inhibited by intracellular ATP and glibenclamide and activated by intracellular adenosine diphosphate (ADP) and cromakalim. KATP agonist can reduce cardiac remodeling and improves endothelial dysfunction. 188 It has also been demonstrated that activation of KATP channels induces ischemic preconditioning (IPC) which affords endothelial protection in guinea pig hearts. 189 Another study found that glibenclamide (a KATP channel antagonist) abolishes, while diazoxide (a K+ channel activator) mimics endothelial IPC in humans. 190 Thus, activation agents that activate or modulate KATP channel function may have future therapeutic implications in vascular diseases associated with endothelial dysfunction.
Two-pore-domain K+ channels
K2P channels are key in stabilizing the negative membrane potential at rest and counterbalance depolarization by mediating leak K+ conductance.191,192 K2P channels are classified in six subfamilies (TWIK, TREK, TASK, TALK, THIK, and TRESK) based on functional similarity and sequence homology. K2P channels are also related to PAH pathogenesis as whole-exome sequencing revealed that mutation on KCNK3 might predispose individuals to PAH. The gene codes for K+ channel subfamily K member 3 (KCNK3), a K2P channel also called TWIK-related acid-sensitive K+channel (TASK1). 193 Antigny et al. recently discovered that KCNK3 expression and function are significantly reduced in ECs and PASMCs from idiopathic and heritable PAH but also in the MCT-induced rat model, where it correlates to PH development. Additionally, the inhibition of KCNK3 modulates pulmonary arterial tone and contributes to vasoconstriction. They also reported that KCNK3 inhibition in vivo increased PAEC and PASMC proliferation and distal artery remodeling, which lead to early signs of PH. 194
Conclusion
PAH involves a multifactorial and complex disease due to aberrant remodeling of distal pulmonary arteries and impaired angiogenesis. Vascular remodeling involves pre-capillary micro-vessels neomuscularization, the rise of neo-intima and media thickening that leads to increased PVR. EC dysfunction appears to play a key role in such pathological process through impaired vasoconstriction, unbalanced EC proliferation, aberrant EndMT, and altered production of endothelial vasoactive mediators. Although tremendous progress were made in the last decade, a lot of work remains to understand PAH complex mechanisms completely. In the present review, we summarized the current knowledge on how EC actively participate in PAH pathogenesis via aberrant mesenchymal transition, epigenetic dysregulation, altered ions homeostasis, and dysfunctional ion channels (Fig. 3). The identification of these molecular mechanisms and their role in the global PAH pathogenesis are crucial to the development of promising targeted therapies.
Molecular pathways implicated in the endothelial dysfunction implicated in PAH pathogenesis. PAH is a complex and multifactorial disease where endothelial cell (EC) dysfunction appears to play a key role through impaired vasoconstriction, unbalanced EC proliferation and apoptosis, aberrant EndMT, and altered production of endothelial vasoactive mediators. The present figure summarized how the presented epigenetic factors (yellow) and ion channels (green) can interact with the molecular pathways implicated EndMT and EC dysfunction that lead to vascular remodeling in PAH.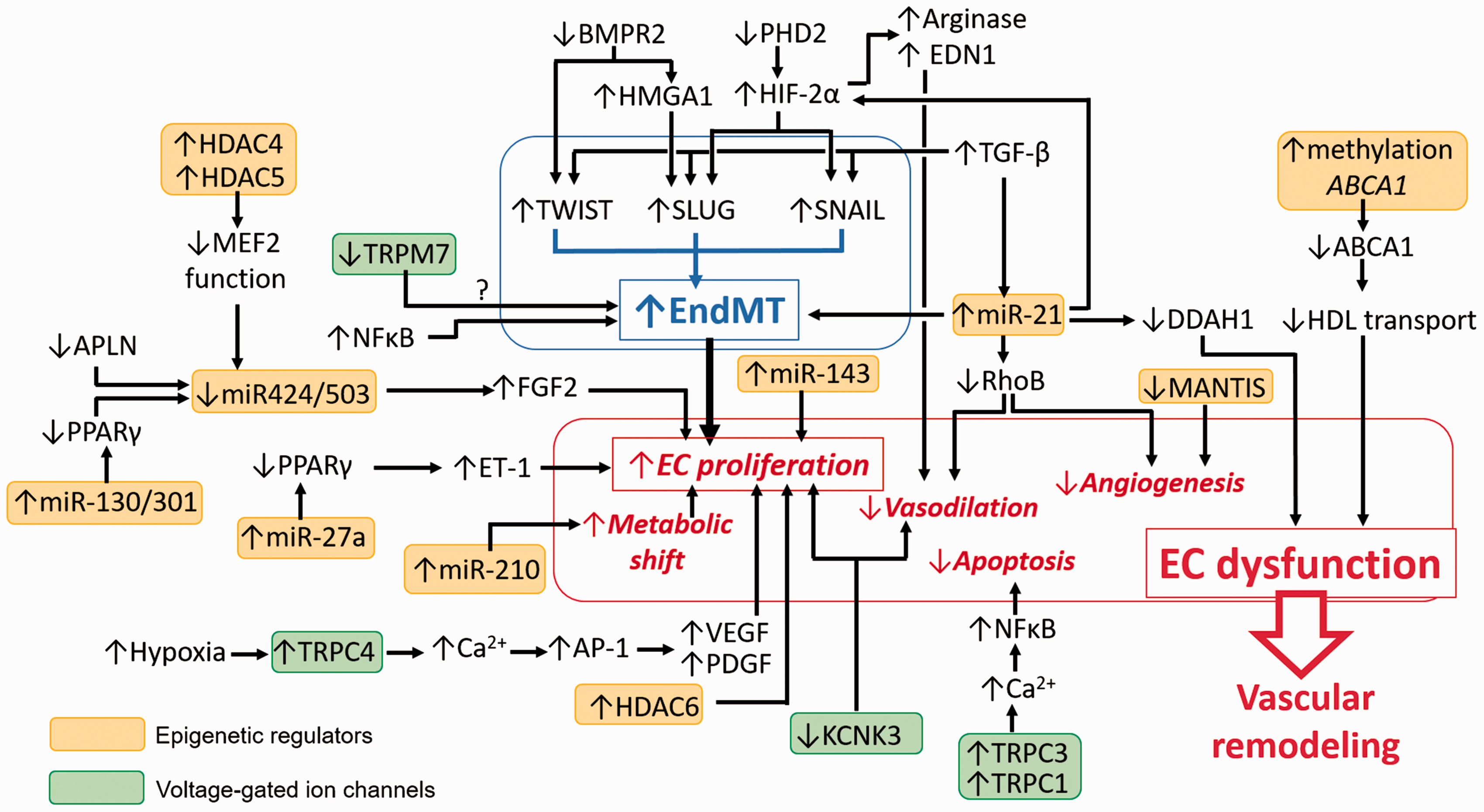
Footnotes
Conflict of interest
SYC reports consultancy agreements with Pfizer, Actelion, Gilead, and Vivus. The other authors declare that they have no competing interests.
Funding
This work was supported by National Institute of Health grants HL096834, HL124021, HL138437, and TR002073 (to SYC).
2017 Grover Conference Series
This review article is part of the 2017 Grover Conference Series. The American Thoracic Society and the conference organizing committee gratefully acknowledge the education grants provided for the support of this conference by Actelion Pharmaceuticals US, Inc., Gilead Sciences, Inc., and United Therapeutics Corporation. Additionally, the American Thoracic Society is grateful for the support of the Grover Conference by the American Heart Association, the Cardiovascular Medical Research and Education Fund, and the National Institutes of Health.
