Abstract
The lung endothelium is vulnerable to both exogenous and endogenous insults, so a properly coordinated efficient repair system is essential for the timely recovery of the lung after injury. The agents that cause endothelial injury and dysfunction fall into a broad range from mechanical forces such as pathological cyclic stretch and shear stress to bacterial pathogens and their virulent components, vasoactive agonists including thrombin and histamine, metabolic causes including high glucose and oxidized low-density lipoprotein (OxLDL), circulating microparticles, and inflammatory cytokines. The repair mechanisms employed by endothelial cells (EC) can be broadly categorized into three groups: (1) intrinsic mechanism of recovery regulated by the cross-talk between small GTPases as exemplified by Rap1-mediated EC barrier recovery from Rho-mediated thrombin-induced EC hyperpermeability; (2) agonist-assisted recovery facilitated by the activation of Rac and Rap1 with subsequent inhibition of Rho signaling as observed with many barrier protective agonists including oxidized phospholipids, sphingosine 1-phosphate, prostacyclins, and hepatocyte growth factor; and (3) self-recovery of EC by the secretion of growth factors and other pro-survival bioactive compounds including anti-inflammatory molecules such as lipoxins during the resolution of inflammation. In this review, we will discuss the molecular and cellular mechanisms of pulmonary endothelium repair that is critical for the recovery from various forms of lung injuries.
Introduction
The pulmonary endothelium is composed of a continuous monolayer of endothelial cells (EC) that forms a semi-permeable barrier between the blood and interstitium. Being a major component of the alveolar-capillary unit, the endothelium is prone to injury from diverse insults including mechanical forces and various barrier disruptive agents such as bacterial pathogens, endotoxins, oxidized low-density lipoprotein (OxLDL), thrombin, histamine, and pro-inflammatory cytokines from the pulmonary circulation.1,2 The increased endothelial permeability caused by the disruption of the EC barrier leads to an influx of protein-rich edematous fluid into the airspaces and subsequent inflammatory responses play a key role in the pathogenesis of acute lung injury (ALI) and its most severe form acute respiratory distress syndrome (ARDS).3–6 Both ALI and ARDS are clinically characterized by acute respiratory failure with a high mortality rate of 20–50% and ALI alone has an incidence of 200,000/year in the US population.7,8 Since no effective therapeutics have been developed to date for both of these severe respiratory disorders, understanding the molecular and cellular mechanisms of endothelial barrier repair and recovery is key to the development of novel drugs targeting the prevention of vascular leak and resolution of inflammation.
When basal endothelial function is perturbed by EC barrier disruption or inflammation, EC can employ three broadly categorized mechanisms of repair and recovery from injury. First, EC can undergo self-repair which is facilitated by the activation of small GTPases Rac and Rap1. This intrinsic mechanism of auto-recovery of EC barrier disruption is best exemplified during thrombin-induced EC hyperpermeability where Rho-dependent barrier dysfunction is restored by the activation of Rap1. 9 It appears that a cross-talk between these small GTPases mediates the recovery process. Second, various barrier protective agents also activate Rac and Rap1 to enhance basal endothelial barrier function as well as to induce the recovery from agonists-induced barrier disruption. The third described mechanism of EC barrier function restoration involves the secretion of various growth factors, numerous pro-survival bioactive metabolites, and anti-inflammatory molecules by the stimulated pulmonary endothelium. Mechanisms of auto- and agonist-assisted recovery will be discussed in the following sections.
In addition to the direct role of EC in the recovery of injured lung endothelium, its dynamic interaction and cross-talk with epithelial cells also contributes to the repair process. The precise mechanisms of epithelial–endothelial interactions and their role in EC barrier protection remains largely unknown, but the secretion of growth factors, cytokines, and other bioactive barrier protective molecules by one cell type may facilitate the protection and recovery of the other cell type against injurious stimuli, thereby enhancing the overall barrier function. For instance, soluble factors of endothelial origin have been shown to enhance epithelial barrier integrity.10,11 Conversely, a recent study showed that epithelial cell-derived prostaglandin E2 (PGE2) enhances endothelial barrier function via activation of EP4 and S1P1 receptors. 12 Furthermore, the same study also showed that cyclooxygenase-2 (COX-2), an enzyme involved in the synthesis of PGE2, expression is increased in epithelial cells following lipopolysaccharide (LPS) challenge, suggesting a possible recovery response of epithelial–endothelial interactions against LPS. With regard to the role of cell–cell interactions in the repair of injured lung endothelium, it is noteworthy to mention that immune cells, especially resident or inflammation-induced circulating macrophages, play a critical role in the resolution of inflammation (reviewed in Herold et al. 13 ). Macrophage-mediated resolution of inflammation is credited to their secretion of anti-inflammatory lipid mediators including lipoxins. 14 In brief, it appears that organ remodeling during recovery from injury is possible by the combined interactive actions of epithelial, endothelial, immune cells, and fibroblasts.
Small GTPases in the regulation of endothelial permeability and barrier recovery
In response to barrier disruptive stimuli, EC have a self-repair mechanism in place which involves the activation of small GTPases and their cross-talk. By cycling between GTP-bound active and GDP-bound inactive states, small GTPases act as a molecular switch in numerous signaling pathways that ultimately regulate various cellular functions. The switch of GTPase between active and inactive states is mediated by different factors. Guanine nucleotide exchange factors (GEF) promote an active GTPase state by exchanging GDP to GTP. GTPase activating proteins (GAP) lead to inactive GTPase by promoting GTP hydrolysis. Finally, guanine nucleotide dissociation inhibitors (GDI) also suppress small GTPases functional activity by stabilizing them in GDP-bound state. The Rho family of small GTPases RhoA and Rac1 as well as the Ras family GTPase Rap1 play a central role in regulating EC barrier function by modulating cytoskeletal remodeling.15–17 Among these, RhoA is responsible for increasing endothelial permeability thereby decreasing EC barrier function. RhoA also mediates the barrier disruptive pathway induced by various agonists including thrombin and vascular endothelial growth factor (VEGF).18–21 The increased phosphorylation of myosin light chain (MLC) mediated by Rho-associated kinase (ROCK)-induced inactivation of MLC phosphatase is considered as the mechanism by which RhoA causes actomyosin contractility. 22 On the other hand, Rac1 plays a major role in maintaining basal endothelial barrier function in resting cells and also mediates EC barrier enhancement induced by various barrier protective agents.5,23 In addition, recent studies, including from our group, have demonstrated the important role of Rap1 in positively modulating EC barrier function.9,24 These GTPases control EC barrier integrity by modifying cytoskeletal organization as evidenced by the formation of actin stress fibers, paracellular gaps with Rho activation and accumulation of peripheral actin, sealing of junctional gaps and enhanced junctional assembly with Rac or Rap1 activation.
Intrinsic mechanism of EC recovery
A dynamic cross-talk facilitated by the time-dependent activation of different small
GTPases seems to regulate the auto-recovery of EC following the disruptive insults. This
notion was established by our study where we showed that thrombin-induced EC permeability
and recovery coincide with activation of Rho and Rap1, respectively
9
(Fig. 1). The rapid activation of Rho mediates
thrombin-induced EC permeability.
19
In turn, barrier recovery is initiated by the activation of Src
kinase-dependent phosphorylation of Rap1-specific GEF C3G leading to the activation of
Rap1. Consistent with these functional roles of RhoA and Rap1, thrombin induced Rho
activation and Rap1 inhibition at early time points (∼ 10 min), which was followed by
activation of Rap1 and downregulation of Rho at later time points. Rap1-dependent recovery
of EC barrier function was evident with the dissolution of actin stress fibers, resealing
of intercellular gaps, and formation of lamelliopodia-like structures. The molecular
inhibition of Rap1 with small interfering RNA abolished thrombin-induced EC barrier
recovery, supporting that Rap1 controls the downregulation of Rho signaling during EC
recovery during thrombin challenge. Similar time-dependent activation of Rho, Rac, and
Cdc42 during thrombin-induced transient and reversible EC barrier disruption was
postulated by Beckers et al. based on the findings from multiple studies (reviewed in
Beckers et al.
15
).
Mechanism of EC barrier auto-recovery after thrombin challenge. In parallel with
rapid activation of the Rho pathway leading to increased EC permeability, thrombin
causes activation of Src kinase, which stimulates the Rap1-specific GEF C3G and, via
Rap1-Tiam1, turns on the Rac1 signaling. Activation of the Rap1–Rac1 signaling axis
downregulates the Rho pathway of barrier disruption and promotes reassembly of AJ
complexes and endothelial monolayer barrier restoration.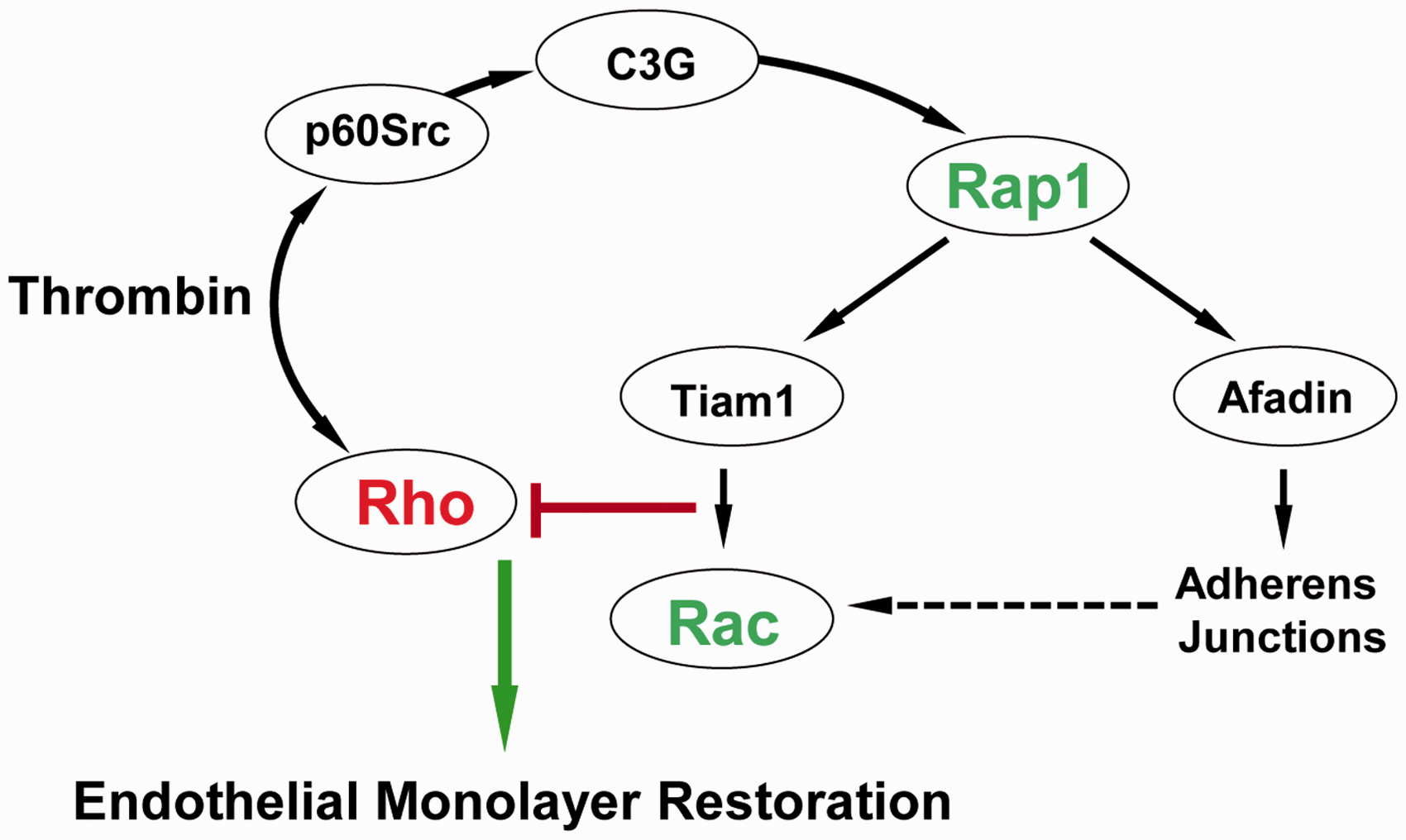
In light of the pivotal role of cross-talk among small GTPases in governing self-repair of EC barrier dysfunction, it is essential to explore the role of various intermediate signaling molecules that facilitate the interaction between these GTPases. From our findings, Rap1-mediated association of afadin with p120-catenin appeared critical in downregulation of Rho. 9 Moreover, Rap1 can also activate Rac1 via Tiam1, a Rac-specific GEF, and thus Rap1-mediated EC barrier recovery may also involve Rac, which is known to suppress Rho activation by multiple mechanisms including direct interaction with RhoGDI, PAK1-dependent inhibition of p115RhoGEF, and stimulation of p190RhoGAP.25–27 Based on the findings from a plethora of studies, it can be concluded that activation of a Rap1/Rac pathway might be a universal mechanism of EC barrier auto-recovery by reversing Rho-mediated disruption. This notion is further validated as various barrier protective agonists also upregulate Rap1/Rac to neutralize the detrimental effects of Rho activation during EC barrier protection which will be discussed in the next section.
EC recovery assisted by endogenous bioactive molecules and therapeutic agonists
In the past two decades, a significant amount of studies have focused on identifying potential EC barrier protective agents that can be developed into therapeutics against vascular leak and inflammation caused by endothelial barrier dysfunction. These studies have led to the discovery of a number of EC barrier protective agonists and their synthetic analogs with therapeutic potential to increase basal endothelial function and offer protection in clinical settings of lung injury. In addition, in response to noxious stimuli, the activated endothelium secretes various bioactive molecules that can trigger the recovery process. This type of EC recovery and resolution of lung inflammation is best exemplified by upregulated production of growth factors, and anti-inflammatory and barrier protective peptides.28–32 In addition, the change in repertoire of pro-inflammatory bioactive lipid mediators secreted during the acute phase of ALI to anti-inflammatory lipid mediators such as lipoxins, resolvins, and protectins synthesized during ALI resolution drives the recovery of inflammation.33,34 Barrier-promoting agonists and mechanisms of their action will be discussed in more detail below.
cAMP and cAMP derivatives
An elevation in cAMP levels in EC has been shown to enhance EC barrier function and also to provide protection via protein kinase A (PKA)-dependent mechanisms against EC barrier disruption evoked by disruptive agents such as thrombin.35,36 PKA-independent mechanism of cAMP-induced EC barrier protection against thrombin or VEGF occurs by the activation of Epac-Rap1 signaling which promotes enhancement of VE-cadherin-containing adherens junctions in endothelial cells. 37 The role of Epac-Rap1 pathway in improving EC barrier function has been further substantiated by other studies.38–40 Several reports have also demonstrated the role of Rac in mediating cAMP-induced EC barrier function.41–43 Our study described the positive cross-talk between Rap1 and Rac, as a convergence mechanism of RhoA inhibition and EC barrier protection against thrombin caused by administration of atrial natriuretic peptide (ANP). 44 Rac1 was determined as a central hub for both PKA-dependent and -independent EC barrier recovery pathways. 45 The results from all of these studies strongly indicate that cAMP-elevating agents such as forskolin, rolipram, and other cell permeable synthetic cAMP analogs including 8-Bromoadenosine 3’, 5’-cyclic monophosphate and 8-(4-chlorophenylthio)adenosine 3’, 5’’-cyclic monophosphate could be potential therapeutics against lung injury and inflammation elicited by endothelial barrier dysfunction.
Prostaglandins
Prostaglandins (PGs) and some of their derivatives have been known to exert barrier protective and anti-inflammatory effects on the pulmonary endothelium.46–48 However, the cellular effects of PGs are determined by the engagement of different receptor types and often show detrimental effects in the lung. 49 Nevertheless, a series of studies from our group have established the protective effects of various PGs in several models of ALI and inflammation in vitro and in vivo. Among these, PGE2 and PGI2 protected from thrombin-induced EC barrier disruption by activating both PKA-dependent and PKA-independent Epac-Rap1 pathways. 50 In the same study, PGI2 analog beraprost protected mechanical ventilation-induced lung barrier dysfunction in mice. By employing pharmacological activators/inhibitors and knockout mice, our study further substantiated the role of beraprost-activated Rap1 pathway in protecting LPS-induced in vitro and in vivo lung injury. 51 Multiple studies testing the role of another prostacyclin analog, iloprost, also showed its potent protective effects against mechanical ventilation and LPS-induced lung injury by activating Rap1 and inhibiting Rho.51–53 Given that both of the aforementioned prostacyclin analogs are clinically used to treat pulmonary hypertension, their marked protective effects in several models of lung injury and inflammation also bolsters their potential therapeutic use in these conditions.
Phospholipids
In recent years, a number of studies have highlighted EC barrier protective and
anti-inflammatory properties of various phospholipids. In particular, treatment with
oxidized 1-palmitoyl-2-arachidonoyl-sn-glycero-3-phosphorylcholine
(OxPAPC) has shown great promise in preventing lung injury and inflammation. Extensive
studies by our and other groups have established that OxPAPC exerts protection against a
diverse range of barrier disruptive and pro-inflammatory agents including mechanical
forces (ventilator, cyclic stretch), thrombin, LPS, and heat-killed
Staphylococcus aureus54–57 which was due
to antagonistic effects of OxPAPC on agonist-induced activation of toll-like receptors
TLR2, TLR4, and TLR9.58–61 Independently on TLR antagonism, OxPAPC exhibits potent
barrier-enhancing effects on vascular endothelium which are initiated by interaction of
OxPAPC with cell surface-associated molecular chaperone with signaling properties,
GRP78.
62
OxPAPC-induced barrier protection was facilitated by cytoskeletal remodeling with
enhanced assembly of adherens junctions and tight junctions mediated by Rap1 and Rac
activation.23,63,64 Additional activation of prostaglandin
E receptor-4 (EP4) which triggers cAMP-PKA and cAMP-Epac1-Rap1 pathways of cytoskeleton
remodeling and cell junction enhancement may also mediate the barrier protective effects
of OxPAPC as evidenced in our latest study.
65
More detailed analysis of phospholipid
oxidation products contained in the OxPAPC preparation revealed that full-length PAPC
oxidation products provide EC barrier protection while fragmented products evoke barrier
disruption.
66
A summary of OxPAPC-induced signaling pathways leading to EC barrier enhancement is
presented in Fig. 2. Summary of signaling mechanisms activated by barrier-protective oxidized
phospholipids.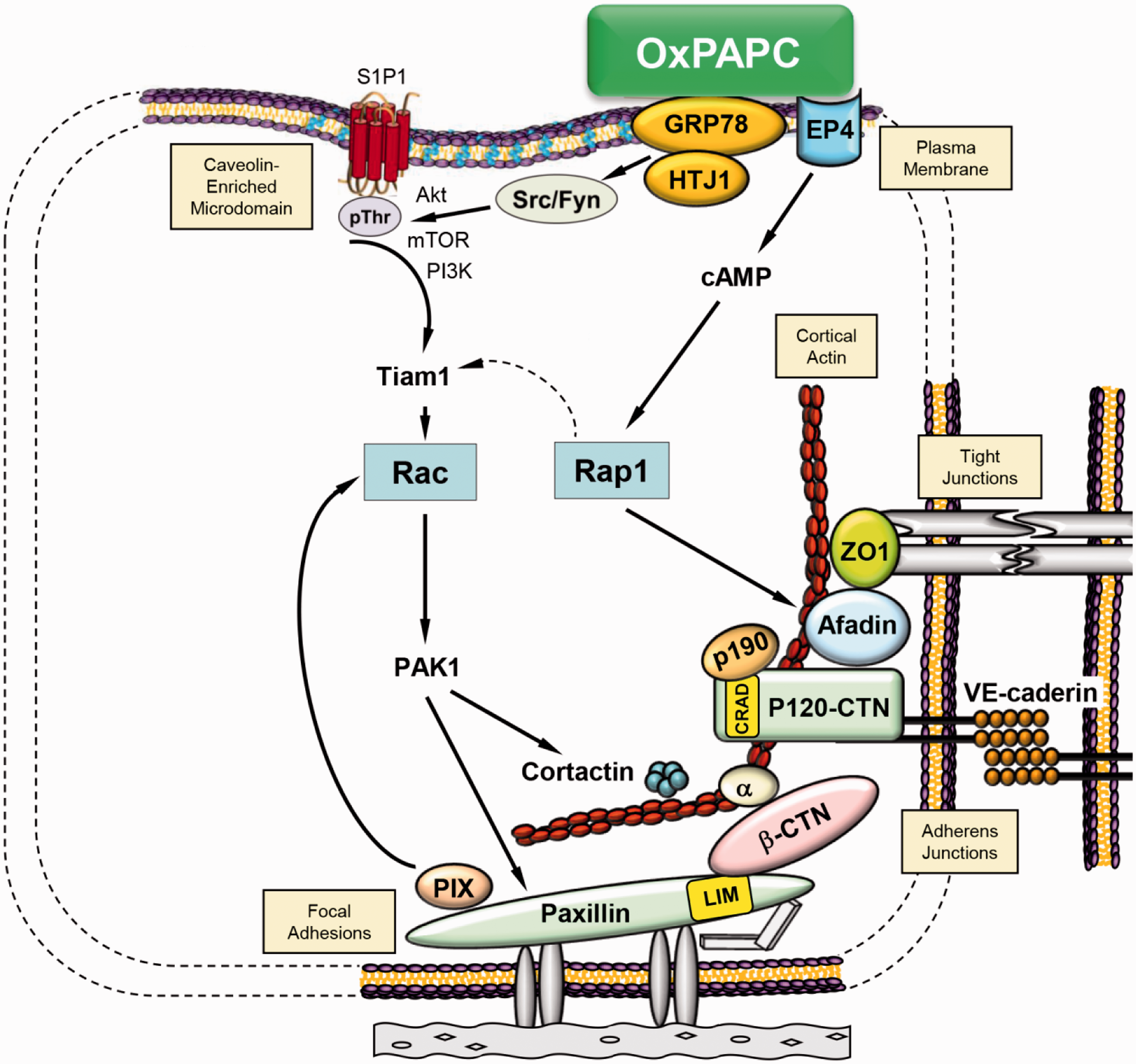
Our most recent study showed that preconditioning of both quiescent or inflamed pulmonary EC with OxPAPC or injection of OxPAPC to LPS-challenged mice induces the production of lipoxin A4 (LXA4), which contributes to anti-inflammatory effect of OxPAPC in vitro and in vivo; and the mechanism of LXA4 action involves activation of EC-expressed formyl-peptide receptor-2 (FPR2/ALX). 67 EC-protective effects of LXA4 have also been confirmed by other groups.68–70
In addition to oxidized phospholipids, another lipid mediator, sphingosine-1-phosphate (S1P), also exhibits potent barrier protective effects on pulmonary EC via binding to its receptor S1PR1 and activation of Rac1 signaling.71–73 Interestingly, OxPAPC also transactivates S1PR1 and this event contributes to OxPAPC barrier-enhancing properties. FTY720, a potent agonist of S1PR1, also enhances EC barrier function, although involvement of S1PR1 receptor-mediated mechanism in FTY720 effects is controversial.74–76
Growth factors
Among growth factors, hepatocyte growth factor (HGF) is a prominent EC barrier protective agent. HGF increases basal endothelial function by cytoskeletal rearrangement mediated by the activation of various kinases including phosphatidylinositol 3’-kinase (PI3K), extracellular signal-related kinase (Erk), p38 mitogen-activated protein kinase, and PKC leading to the phosphorylation of glycogen synthase kinase-3β. 77 HGF protects against thrombin-induced EC dysfunction by Tiam1-mediated activation of Rac and inhibition of Rho pathways. 78 Likewise, HGF-induced protection against LPS-caused lung injury and inflammation was dependent on the activation of Asef, a Rac-specific GEF. 79 Microtubules also appear to play a key role in mediating HGF-induced EC barrier enhancement. 80 Contribution of other growth factors upregulated during lung injury in EC barrier function recovery still remains to be clarified. A recent study has shown that epidermal growth factor (EGF) protects blood–spinal cord barrier disruption during acute spinal cord injury by activating the PI3K/Akt/Rac pathway. 81
Other barrier protective molecules
Statin, an inhibitor of the rate-limiting enzyme in cholesterol synthesis, has been shown to protect against thrombin-induced endothelial permeability in vitro by inhibiting membrane translocation of Rho and prevents vascular leaks in vivo. 82 The EC barrier protective functions of simvastatin has been confirmed by several other studies.83–85 Hyaluronan is a major glycosaminoglycan component of extracellular matrix of many tissues. High molecular weight hyaluronan, a natural component of extracellular matrix also present in circulation in soluble form, enhances EC barrier function in part via transactivation of S1PR1 receptor 86 and protects LPS-induced vascular leak. 87 An endogenous peptide adrenomedullin is reported to protect vascular barrier integrity.88,89 Angiopoietin protects against VEGF-induced endothelial permeability by inhibiting Src activation and preventing the phosphorylation of VE-cadherin. 90 The endothelial barrier protective and anti-inflammatory roles of angiopoietin have been observed in various settings.91,92
Conclusion
The timely and efficient recovery of the endothelium from various toxic insults and
injuries is vital for the proper function of the lung. The repair process in EC is assisted
by either intrinsic or agonist-induced small GTPases activation with cytoskeletal
remodeling. Sequential activation and dynamic cross-talk between these GTPases regulate the
overall endothelial function (Fig.
3). In response to toxic stimuli, the endothelium also generates various bioactive
molecules which assist during the recovery. Among them, lipoxins appear to be of significant
importance with their potent barrier protective and anti-inflammatory functions as well as
their accumulation by EC barrier enhancing oxidized phospholipid species, OxPAPC. The
comprehensive understanding of the molecular and cellular mechanisms of intrinsic or
agonist-mediated endothelium repair and recovery will pave a way for the development of
novel therapeutics against pulmonary disorders associated with endothelial dysfunction. Balance of EC-disruptive and EC-protective mechanisms in the course of lung injury
and resolution phase. Lung injurious factors (bacterial pathogens, excessive
mechanical stretch, cytokines, disruptive bioactive molecules) trigger pathologic
signaling (i.e. oxidative stress, RhoA pathway, signaling kinases, secreted factors)
leading to endothelial hyperpermeability, inflammation, and lung dysfunction. However,
pathologic stimuli also activate mechanisms of auto-recovery such as secretion of
pro-survival growth factors and anti-inflammatory lipid mediators which suppress
inflammation, downregulate pro-inflammatory and disruptive RhoA GTPase-mediated
pathways, and stimulate Rap1 and Rac1 GTPase-mediated cytoskeletal remodeling leading
to EC barrier recovery.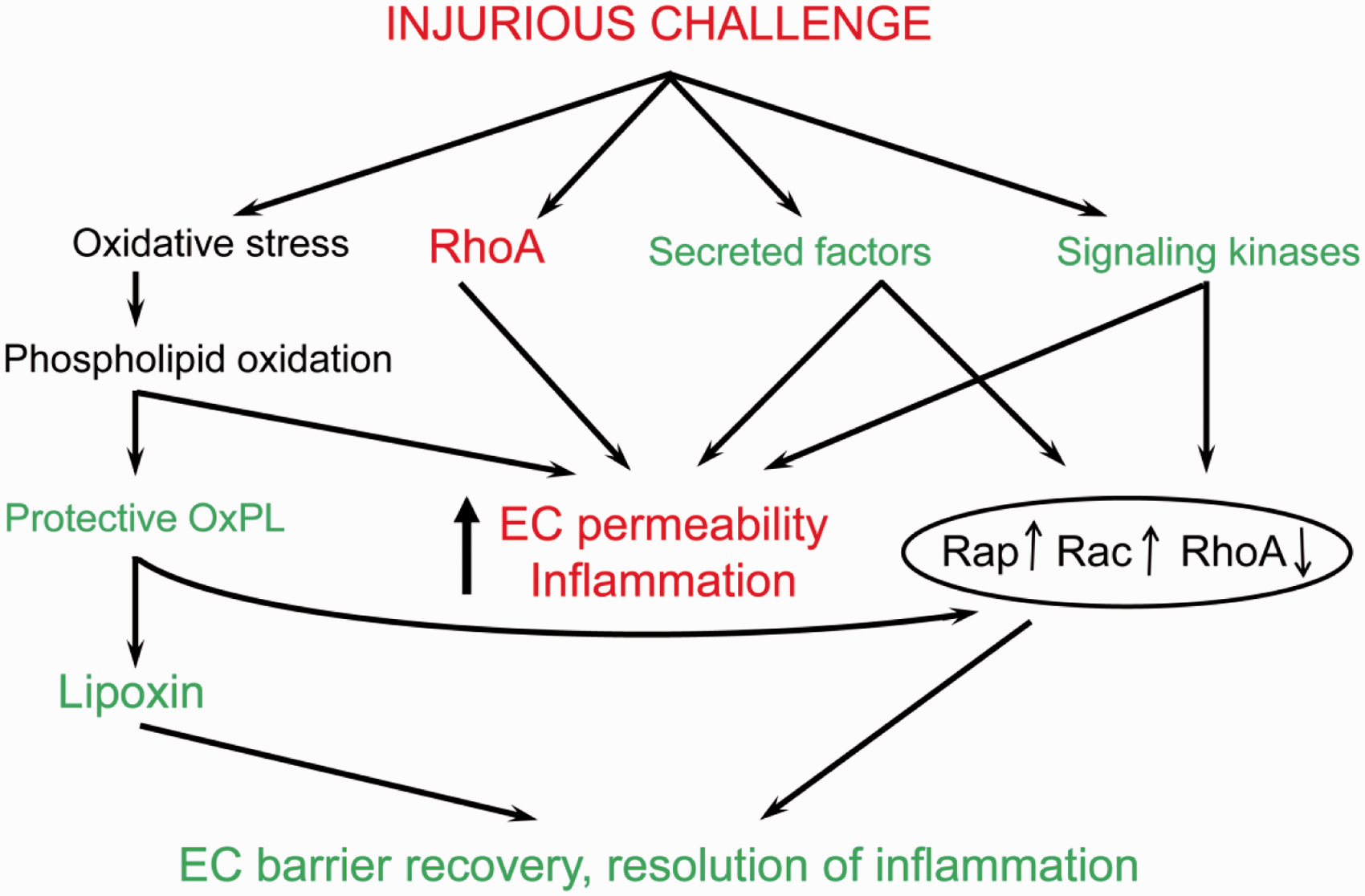
Footnotes
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research has been supported in part by NHLBI grants HL076259 and HL087823, and NIGM grant GM122940.
2017 Grove Conference Series
This review article is part of the 2017 Grover Conference Series. The American Thoracic Society and the conference organizing committee gratefully acknowledge the education grants provided for the support of this conference by Actelion Pharmaceuticals US, Inc., Gilead Sciences, Inc., and United Therapeutics Corporation. Additionally, the American Thoracic Society is grateful for the support of the Grover Conference by the American Heart Association, the Cardiovascular Medical Research and Education Fund, and the National Institutes of Health.
