Abstract
The pulmonary vasculature plays an important role in many lung pathologies, such as pulmonary arterial hypertension, primary graft dysfunction of lung transplant, and acute respiratory distress syndrome. Therapy for these diseases is quite limited, largely due to dose-limiting side effects of numerous drugs that have been trialed or approved. High doses of drugs targeting the pulmonary vasculature are needed due to the lack of specific affinity of therapeutic compounds to the vasculature. To overcome this problem, the field of targeted drug delivery aims to target drugs to the pulmonary endothelial cells, especially those in pathological regions. The field uses a variety of drug delivery systems (DDSs), ranging from nano-scale drug carriers, such as liposomes, to methods of conjugating drugs to affinity moieites, such as antibodies. These DDSs can deliver small molecule drugs, protein therapeutics, and imaging agents. Here we review targeted drug delivery to the pulmonary endothelium for the treatment of pulmonary diseases. Cautionary notes are made of the risk–benefit ratio and safety—parameters one should keep in mind when developing a translational therapeutic.
Keywords
The pulmonary vasculature is an important target for therapeutic interventions. Pulmonary endothelial cells are implicated in numerous pulmonary diseases, including pulmonary arterial hypertension (PAH), primary graft dysfunction (PGD) of lung transplant, and acute respiratory distress syndrome (ARDS). Targeting drugs to the pulmonary vasculature may be beneficial for the treatment of these and other conditions as it offers a more precise spatiotemporal control of the pharmacological effect.
In addition to the pulmonary endothelium’s important role in numerous diseases, it also has unique features that make it a practical target for drug delivery systems (DDSs) via the intravenous (IV) route. First, the pulmonary endothelium represents ∼25% of the total vascular surface in the body, thus providing an enormouse surface area for binding. 1 Second, the pulmonary vasculature receives the entire first pass of IV-administered drug. Third, it collects the entire cardiac output and does so at lower shear rates than arteries; hydrodynamic conditions aid the binding of targeted drug delivery vectors.1,2
The absence of affinity of most drugs and DDSs to endothelial cells can be overcome by “vascular targeting,” or conjugation of DDS with ligands that bind to the endothelium. This experimental strategy enables delivery to, into, or across endothelial cells.16–21. In this review, we will discuss how such vascular-targeted DDSs have been used to deliver drugs to the pulmonary endothelium for the treatment of animal models that mimic multiple important human lung diseases.
Endothelial determinants for targeting drugs to the pulmonary vasculature
Target determinants for endothelial drug delivery.

PECAM-1, platelet-endothelial cell adhesion molecule 1; ICAM-1, intercellular cell adhesion molecule 1; VCAM-1, vascular cell adhesion molecule; TM, thrombomodulin; ACE, angiotensin-converting enzyme; APP, aminopeptidase P; PV1/Plvap, plasmalemma vesicle associated protein.
Some target determinants useful for vascular targeting are expressed on the endothelium throughout the vasculature. Adhesion molecules platelet-endothelial cell adhesion molecule 1 (PECAM-1) and intercellular adhesion molecule 1 (ICAM-1) are not only expressed on endothelial cells, but they are also constitutively present in other cells accessible to blood (platelets and leukocytes). However, compared to all of these competitor cells, surface levels of PECAM-1 and ICAM-1 are the highest in endothelial cells. While PECAM-1 is mainly located in the inter-endothelial borders,14,40,41 ICAM-1 tends to localize in lipid rafts in the luminal membrane either as a monomer or as an oligomer form. 42 Adhesion molecules are involved in cellular recognition, adhesion, and migration of cells like leukocytes. 43 Notably, inhibition of such functions may be considered favorable during the treatment of some types of inflammation.44–48
The pan-endothelial targets (e.g. PECAM-1) discussed above can be valuable for drug delivery to treat systemic maladies (e.g. sepsis). However, considering the high percentage of total body endothelial surface localized in pulmonary tissue (∼ 25%), and that drugs dosed intravenously first pass through the pulmonary circulation, 1 agents with endothelial affinity primarily accumulate in the lungs after IV administration. This why endothelial target determinants improve lung concentrations of DDSs more than any other organ, even if though such pan-endothelial target determinants are consistently distributed throughout all endothelial cells in the body.49,50
Pathological states, such as inflammatory conditions, also affect the expression levels of some cell adhesion molecules (CAMs) such as ICAM-1 by inducing its synthesis, leading to an increase in its surface expression of approximately twofold in some inflamed types of endothelium 51 and other cell types. 52 Vascular cell adhesion molecule-1 (VCAM-1), P-selectin, and E-selectin, which support early phases of leukocyte adhesion, are sometimes referred to as “inducible” adhesion molecules. 53 Stimulants such as cytokines, oxidants, and abnormal flow trigger P-selectin molecules to translocate from their baseline intracellular position to the cell surface within 10–30 min, 54 and prompt de novo synthesis and surface expression of E-selectin 27 and VCAM-1. 14 DDSs bearing antibodies targeted to these markers can therefore selectively bind to activated endothelium,20,55–59 where in some cases the endothelial determinants such as E-selectin and VCAM-1 are localized more in the arteries and skin microvasculature than in the pulmonary vasculature. 57 This preferred specificity for activated endothelium is especially appealing for visualization of activated endothelium in inflamed areas via delivery of conjugated radioisotopes 60 or ultrasound contrast agents61,62 for imaging applications.
Additional pulmonary specificity can be found in the case of angiotensin-converting enzyme (ACE), which is expressed at the endothelial luminal surface in the pulmonary capillaries at a higher level than in other organs.23,63–67 ACE antibody-conjugated preparations have been found to be promising in directing biotherapeutics and genetic cargos to the pulmonary endothelium in animal studies.31,68–75 Lung visualization using labeled anti-ACE selectively targeting the lungs after IV injection has been reported in rats, mice, cats, primates, and even humans.64,76–78 These studies demonstrate the translational potential of ACE-targeted DDSs. 79
Caveolar epitopes represent another class of endothelial determinant. Caveolae are found in many different types of cells, and are particularly copious in the pulmonary endothelium.33,34 Caveolae are cholesterol-rich domains of cell membrane, decorated on the cytosolic side by the caveolin and cavin family proteins. 35 Caveolae and caveolae-derived endosomes play important roles in subcellular activities such as molecular transport and cell signaling. 80 Extensive studies have been done in applying antibodies and other affinity ligands to target therapeutics to caveolae36,37,39 or to caveolar endosomes in order to cross endothelial cells. 38 Caveolar determinants such as aminopeptidase P (APP)36,39 and plasmalemma vesicle associated protein (PV1 or Plvap) actively accumulate in lungs after IV administration. However, considering the narrow diameter of the caveolar opening (∼ 50 nm), some larger nanocarriers may be unsuitable for caveolar delivery.
Intra- and trans-cellular addressing of drugs within the pulmonary vasculature
In some cases, delivery of drug to the endothelial surface is enough for a therapeutic goal to be reached. However, very often effective therapy may be achieved only when drugs are delivered to specific sub-cellular addresses. 81
The endothelium exerts active non-specific fluid phase uptake via macropinocytosis. 82 The vesicles generated in this process transport compounds, including drugs, present in the blood at high concentrations, but the low efficacy and non-specific nature of this pathway does not meet the requirements for drug targeting. In contrast, uptake of ligands that bind to internalizing receptors is more effective, specific, and controlled than passive fluid phase uptake.
Like the majority of cells, endothelial cells internalize ligands by phagocytosis or receptor-mediated endocytosis, in either clathrin-dependent 83 or clathrin-independent 84 pathways such as caveolar endocytosis.82,85,86 Recent studies on the link between signaling and internalization have demonstrated a vast endocytic network used by cells for endocytosis, sorting, and trafficking of ligand-receptor complexes. 87 Ligand-dependent types of endocytosis have high selectivity to certain cellular receptors and are able to deliver cargoes to distinct destinations.
Target determinants are localized in different domains and clusters in the plasmalemma (Table 1). 88 Thus, PECAM-1 and vascular endothelial cadherin (VE-cadherin) are predominantly localized at the cell–cell border,89,90 while VCAM-1 and ICAM-1 are found in tetraspanin microdomains, specialized types of membrane rafts on apical surface.18,42,91 GP85 presents in the plasmalemma over a thin organelle-free part of the endothelial cell separating alveoli from blood,92,93 whereas APP and Plvap are both found in caveolae. 39 Target localization regulates both the accessibility of target to circulating drug carriers and their fate after anchoring and uptake. 94 For example, endothelial cells internalize selectins via clathrin-mediated endocytosis,95–97 which favors intracellular delivery into endothelial cells of E-selectin-targeted liposomes, 26 drugs,26,98 and genetic materials. 99
Endothelial cells do not internalize unconjugated antibodies to PECAM-1 or ICAM-1, but rapidly internalize multivalent anti-ICAM-1 and anti-PECAM-1 carriers via a non-canonical type of endocytosis. 81 Internalized carriers arrive in lysosomes several hours after uptake, which is slow compared to many classical endocytic pathways that deliver their ligands to lysosomes within 10–20 min.100,101 It has been recognized for a long time that conversion of monovalent or bivalent ligands into multivalent carriers that can engage numerous copies of the receptors enhances internalization. 81 An extensive clustering of receptors eliciting strong endocytic signaling, as well as dissociation of pre-existing clusters and “unnatural” signaling, among other factors, may be involved in the enhanced uptake of multivalent carriers. Although high carrier avidity is viewed as favorable for intracellular delivery, excessively tight binding may be detrimental for the subsequent dissociation of the carrier from the receptors during intracellular trafficking.
The rate of endothelial uptake of drugs and nanocarriers directed to PECAM-1 and ICAM-1 is modulated by the functional status of endothelium, 102 parameters of flow and endothelial adaptation to shear stress,102,103 as well as the size of the nanocarriers.104,105 Furthermore, endothelial internalization of PECAM-1-targeted carriers depends on the selection of anchoring epitopes on the PECAM-1 molecule. 106 Indeed, ligands binding to distinct epitopes of the same anchoring molecules may enter cells differently. This makes selection of ligands facilitating cellular uptake an important goal in drug delivery research.107,108 Using a phage-display library, a series of peptides binding to diverse VCAM-1 epitopes was identified, some of which have shown enhanced uptake. 57 Labeled VCAM-1-binding peptides improved imaging of vascular inflammation in animal models.20,57 Phage display and other high-throughput methods may facilitate selection of internalizable antibodies and their fragments.109–111
Endothelial cells more effectively internalize polyvalent conjugates targeted to ICAM-1 than to PECAM-1, 13 although small (i.e. < 100 nm) PECAM-1-targeted carriers enter the endothelium fairly effectively. 104 Size is generally important in the vascular targeting paradigm. For example, the specificity of pulmonary targeting was shown to be dependent on the size of the carriers; exceeding a sub-micron limit leads to enhanced non-specific mechanical retention in the lungs. 112 Therefore, PECAM-1 and ICAM-1 represent highly unusual endothelial targets providing either surface anchoring or internalization, with the choice controlled by the parameters of the carrier design, i.e. valence of binding. 105 This feature permits targeting of drugs that either need to be retained on the cell surface such as monovalent anti-thrombotic fusion proteins or delivered inside the cell in the form of drug-loaded multivalent nanocarriers. 113
Further, clustering of ICAM-1 leads to activation of sphingomyelinase and subsequent cleavage of sphingomyelin, stimulating endocytosis of anti-ICAM-1-coated carriers in the size range of < 100 to > 1000 nm in diameter. 114 This mechanism does not operate in sphingomyelinase-deficient cells and animals; however, carriers coated with both anti-ICAM-1 and the enzyme, devised to deliver enzyme replacement therapy in Neumann–Pick syndrome, do compensate for the genetic defect and are internalized by cells. 115 Furthermore, co-immobilization of sphingomyelinase with ligands anchoring carriers to transferrin receptor permitted internalization of carriers larger than those normally permitted by clathrin vesicles (< 200 nm). 116
Examples of PECAM-1 and ICAM-1 illustrate the case when endothelial cells internalize nanocarriers coated with normally non-internalizable molecules. In the opposite scenario, coating a nanocarrier with internalizable molecules does not necessarily result in internalization. For example, the uptake of a large, micron-size carrier may exceed the cellular endocytic capacity; formation of such a large vacuole would require prohibitively extensive mobilization of the cell membrane and cytoskeleton. Further, coupling ligands to carriers may impede their interaction with receptors and epitopes localized in invaginations and other domains of the plasmalemma inaccessible to the particles of such size. For example, conjugation of ligands of caveolar epitopes to carriers larger than the diameter of the neck of caveolae (>40–70 nm) abolishes endothelial targeting and transfer. 117
Binding to endothelium may also lead to transport across the cells. Some ligands of receptors involved in endocytosis via clathrin-coated pits, such as transferrin receptor, 118 and caveolae,119–122 such as aminopeptidase P 39 and annexin A1, 38 are capable of crossing the endothelial barrier. These pathways provide an opportunity for trans-endothelial transport of nanocarriers with size suitable for these endocytic vesicles. For example, antibodies to aminopeptidase P undergo fast (within seconds to 1 min) caveolae-dependent transport across the endothelium and stay there for days. 39 However, whether this phenomenon can provide efficient tool for tissue delivery of drugs remains to be investigated. In addition, the potential side effects of engaging caveolar determinants must be better understood in order to define the biomedical utility of this transcellular pathway.123–125 For example, many caveolae localized proteins are critical players in cell cignaling and an interefence with their functioning may cause unwanted consequences. In addition, disease conditions, including inflammation, may affect this pathway.82,117,126–129 It has been shown that anti-ICAM-1 coated nanocarriers (∼100 nm diameter spheres) can be transported across the cellular monolayer without cell damage or disruption of intercellular junctions. 130 Similar to caveolar delivery, ICAM-dependent tissue drug delivery requires further studies.
Effect of pathological factors on vascular targeting
In order to obtain selective delivery to pathological tissues, targeting agents (e.g. monoclonal antibodies and their derivatives) are often utilized that bind to markers that are upregulated in diseased or injured tissues. Typically, targets are upregulated through mechanisms such as synthesis of new protein molecules, mobilization of sequestered intracellular stores, or unmasking of target epitopes.
Delivery of drugs may occur in two settings, prophylactic or therapeutic. Markers that are constitutively expressed in the lung are most suitable for prophylactic delivery (e.g. PECAM-1, ACE, and APP), while molecules that either remain expressed (PECAM-1) 113 or are induced following injury (e.g. VCAM-1 and certain selectins) may find utility in therapeutic interventions and diagnostic imaging.20,57,60,62,99 However, in some cases, targets molecules are shed from the endothelial surface following injury (e.g. ACE or thrombomodulin),22,32,67,131 suggesting that they may not be optimal markers for therapeutic delivery to sites of acute inflammation.
Beyond simple consideration of target expression, pathological changes in tissue physiology may lead to alterations in targeting to the site of injury. Local alterations in physiology may occur either at focal points within a tissue or on a whole-tissue level (less common clinically). One example of a spatially heterogeneous condition is ARDS, which classically appears in patches of the tissue when visualized on a computed tomography (CT) scan.
Recently, our group has developed a mouse model of ARDS wherein injury is induced in a single lobe of the lung, more closely recapitulating the human condition than classical ARDS models that display homogeneous injury throughout the tissue. 132 The impact of injury on sub-tissue distribution of nanocarriers targeted to cell adhesion molecules was measured in order to elucidate mechanisms that could control drug disposition in this injury model. Several mechanisms were evaluated in this model, including hypoxic vasoconstriction (measured by changes in local blood flow), edema (measured by protein leak and tissue weight), and target protein expression (measured by western blot). The injured lobe was observed to have decreased blood flow and increased edema relative to the healthy lobes.
Interestingly, it was found that different targeting strategies had different distribution patterns within the lung and that these could be explained by the various tested mechanisms. For example, untargeted particles preferentially accumulated in the injured lobe, likely due to enhanced vascular leak, while particles targeted to PECAM-1 (no change in expression following injury) were found to accumulate in the healthy lobe, due to the reduced blood flow to the injured lobe. These mechanisms are depicted in Fig. 1. However, ICAM-1 targeted nanocarriers selectively accumulated in the injured lobe, due to a large upregulation of ICAM-1 expression at the injured site. A pharmacokinetic model was developed that considered all of these mechanisms, which was able to make a priori predictions of the sub-tissue distribution of these carriers, based solely on changes in physiology following lung injury.
Impact of pathology on nanocarrier delivery to the inflamed lung. The left panel depicts mechanisms controlling sub-tissue delivery of PECAM-targeted (hypoxic vasoconstriction) and IgG-coated (capillary leak) nanocarriers in the unilateral ARDS mouse model. The top right depicts the localized injury induced in this model and the bottom right shows a semi-physiologic pharmacokinetic model describing sub-tissue nanocarrier disposition in this animal model, which described disposition using a one-compartment model linked to a physiolgic lung model. Within the lung space, nanocarriers were allowed to discribute based on physiologically relevant values to the injury model.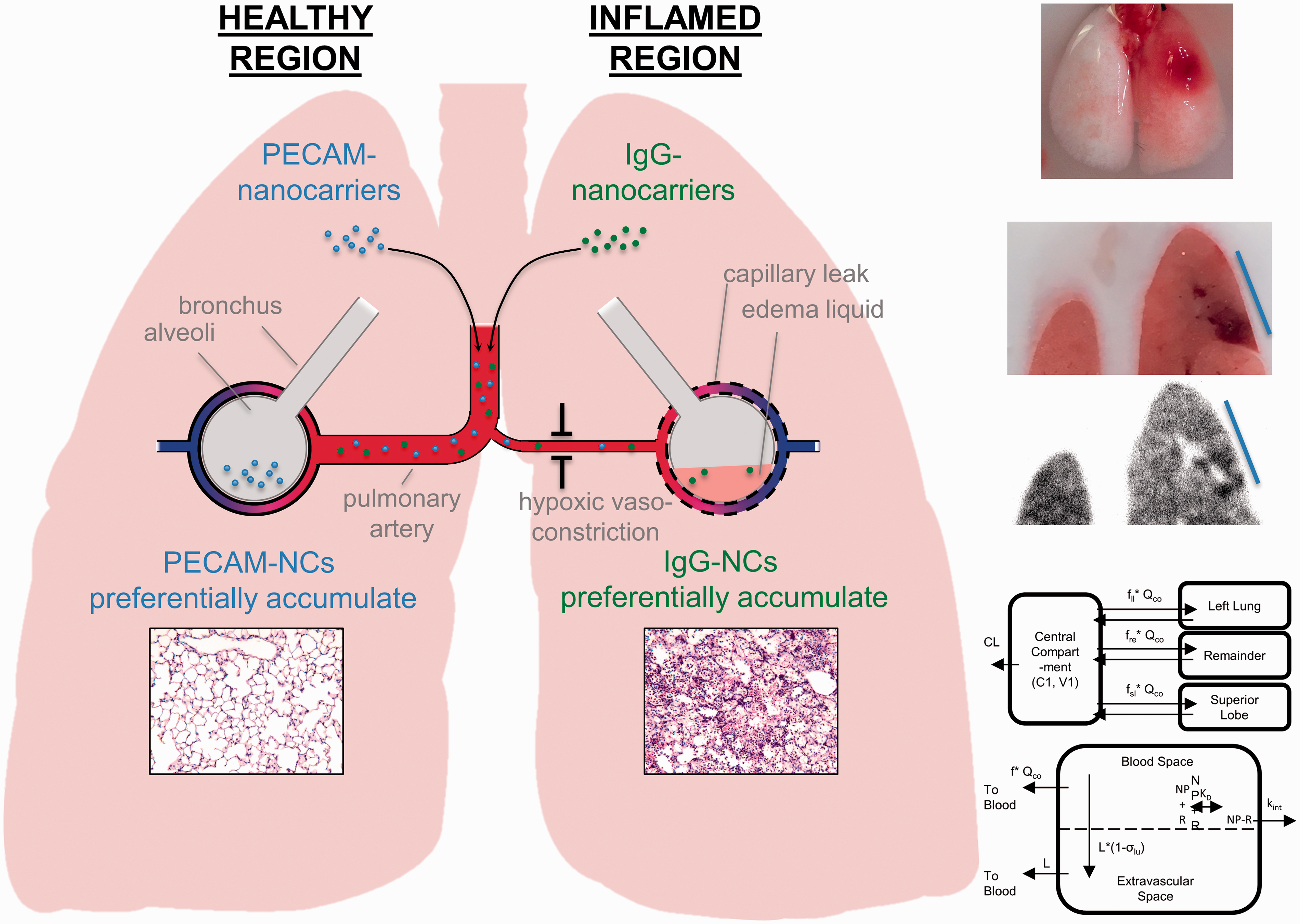
The above example described how in ARDS / acute lung injury (ALI), pathological changes can markedly change how targeted DDSs distribute within the lungs. Numerous other lung pathologies are very likely to also change DDS distribution and efficacy. For example, in PAH, the plexiform lesions of the small arterioles greatly disrupt blood flow, which is very likely to change where DDSs deposit in the pulmonary vascular tree, as compared to normal lungs. Similarly, in pulmonary embolism (PE), the occlusion of the pulmonary arteries by the clot causes numerous vasodilatory changes in the lungs, which may make it harder for DDSs to reach the offending clot. These and numerous other examples illustrate the paramount importance of examining the distribution of DDSs within the lungs of animal models of disease early. Indeed, determining what fraction of a DDS reaches the site of pathology in the lung should be the very first step in development of a DDS for pulmonary diseases.
Targeting antioxidants to the pulmonary endothelium
The disappointing lack of results over the last several decades of antioxidant research, including large-scale clinical trials testing effects of antioxidants and antioxidant enzymes (AOE) catalase and superoxide dismutase (SOD), can be interpreted as a drug delivery problem.133–135 Indeed, data have shown that when antioxidant pharmacokinetics (PK) are improved via chemical modifications using polyethylene glycol (PEG)
136
or PEG-based pluronic
137
or by loading into PEGylated carriers (liposomes
138
or polymeric carriers
139
), the enhanced bioavailability of modified catalase, SOD, or other antioxidants moderately reduced systemic oxidative stress in animals.140,141 Further, SOD and catalase conjugated with either cationic membrane-permeating peptides
142
or heparin-binding peptides enhanced cellular binding and uptake, resulting in modest improved protective effects in animal models of inflammation
143
(Fig. 2). However, none of these non-targeted delivery approaches provided a decisive improvement of antioxidant interventions in controlled animal studies.
Demonstrated functional activities of targeted antioxidant enzymes catalase and superoxide dismutase in vitro and in vivo. LPS, lipopolysaccharide.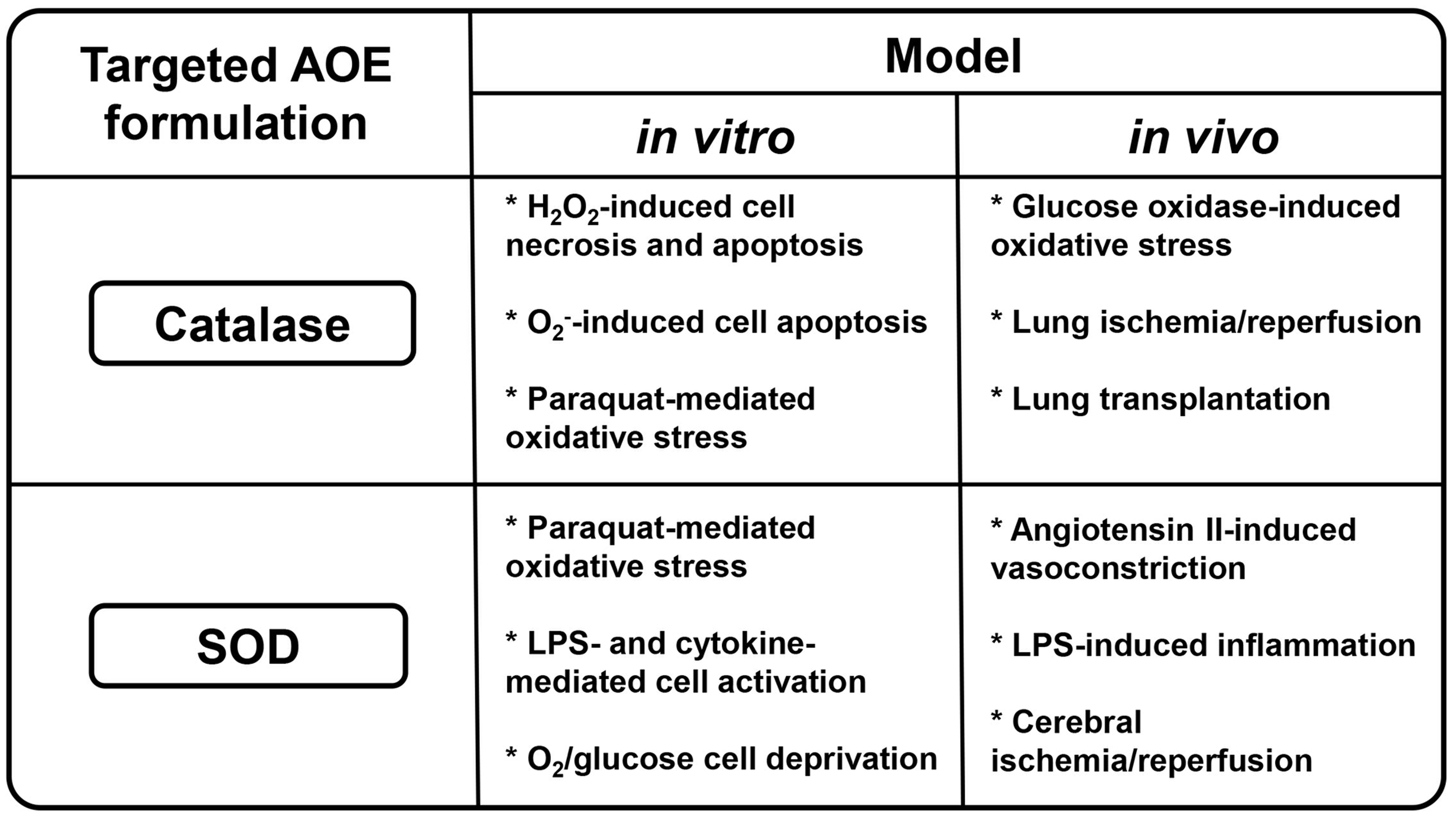
In contrast, AOE conjugated with antibodies to ACE, 70 ICAM-1, 31 and PECAM-1144 but not control IgG specifically bound to the endothelium,13,145,146 and accumulated in the lungs after IV injection in rats, mice, pigs, and dogs.13,31,70 In models of acute oxidative stress, the conjugates protected the perfused lungs in these animals much more effectively than their untargeted counterparts in these species.146–148 Most notably, catalase targeting to pulmonary endothelium via PECAM-1 or ACE was very protective in models of lung transplantation in rats,72,148 mice, 149 and pigs. 150
The benefits of targeted AOE provide specificity to their corresponding reactive oxygen species (ROS) substrates (SOD and catalase degrade superoxide radical and hydrogen peroxide, respectively), while low molecular weight antioxidants mostly lack this specificity. For example, a model of pulmonary ischemia/reperfusion injury showed that targeted catalase, but not SOD, was protective, implicating hydrogen peroxide H2O2 as the chief damaging ROS. 149 In contrast, targeted SOD inhibited vasoconstriction induced by angiotensin II in mice, confirming the key role of superoxide O2.- produced by endothelial NADPH-oxidase (NOX) in depleting the vascular pool of NO, whereas catalase not only failed to attenuate the vasoconstriction effect, but showed some tendency to aggravate it. 149 Furthermore, targeted SOD, but not catalase, inhibited pathological endothelial activation induced by cytokines. 13 PECAM-1-targeted SOD attenuated leukocyte adhesion in cerebral vasculature and reduced the infarction zone in a model of brain ischemia-reperfusion injury. 151
The recent data on anti-inflammatory effects of SOD13,151 demonstrate the importance of intracellular SOD delivery. Because ROS are small, promiscuous species that act without specificity on numerous biological targets, the value of localization within target cells of antioxidants to their therapeutic effects could be underestimated. The range of action of superoxide is on the scale of nanometers, if not angstroms, from their influx site, due to high reactivity and limited membrane diffusion of superoxide. 152 Recent studies show that sub-cellular addressing of SOD is indeed important; PECAM-1-targeted SOD formulations accumulating in endosomes quenched superoxide anion produced in the vesicular lumen by NOX, thereby intercepting this organelle-specific pathological pathway.13,48
The diversity of antioxidant formulations targeted to the pulmonary vasculature includes liposomes and polymeric nanocarriers, in addition to antibody-drug conjugates (Fig. 2). Catalase was found to be protective against oxidative stress in vitro145,147,153 as well as in in vivo models of oxidative stress, lung ischemia/reperfusion, and transplantation.147,149,150 Delivery of SOD was protective in cellular models of oxidative stress and in case of pro-inflammatory endothelila cell activation.13,154 In animal models, SOD may attenuate inflammation, angiotensin II-induced hypertension, and cerebral ischemia/reperfusion.13,151
Liposomes are an established means to deliver antioxidants, protecting them from clearance and deactivation in vivo, and facilitating access to injured or inflamed cells and tissues. 155 Hydrophobic antioxidants can be incorporated within the hydrophobic bilayer (e.g. vitamin E, flavonoids, among many others), 156 while water-soluble antioxidants such as ascorbate, glutathione, and AOE can be encapsulated in the inner aqueous space of liposomes 157 or polymersomes. 158 Cell culture and some animal studies imply that liposomal antioxidants have better pharmacokinetics (PK) and efficacy than free drugs, especially in systemic subtle oxidative stress.159–161 Varying methodology and content of liposomal SOD formulations allows for modulation of the loading efficacy, localization within the liposomal compartments, and enzymatic activity of resultant SOD/liposomes. 162 These studies provided the context for targeting antioxidant liposomes to the pulmonary vasculature.
PECAM-1-targeted liposomes loaded with MJ33, a NOX inhibitor, accumulated in the endothelial cells and inhibited ROS production in cell culture. They provided more potent protective effects than non-targeted counterparts against oxidative stress and inflammation in perfused mouse lungs ex vivo, and in LPS-induced inflammation in mice. 163 Similar results were obtained with a SOD/catalase mimetic EUK-134. Targeted liposomes loaded with EUK-134 bound to endothelial cells in culture and in pulmonary vasculature in mice and provided anti-inflammatory effects in a mouse model of endotoxin-induced lung injury, whereas untargeted IgG/EUK liposomes provided neither delivery of cargo to endothelium nor protection. 164
Furthermore, targeting of AOE encapsulated into a porous milieu permeable to ROS, but impermeable to proteases, has been designed using polymeric nanocarriers based on PEG-PLGA copolymers, allowing access to H2O2 (but not to superoxide), and protecting catalase from proteases. 165 Additionally, porous vesicular polymersomes encapsulating SOD provided access of the enzyme to superoxide, while preventing SOD degradation, and proving effective in a brain injury model. 158 Enzyme PEGylation may also increase protection against proteases, while modulating the molar ratio and size of PEG and PLGA chains in the copolymer controls the shape of nanocarriers, allowing geometries ranging from spherical to filamentous. 166
PECAM-1-targeted PEG-PLGA nanocarriers loaded with catalase provide effective endothelial delivery in vitro and in vivo, and prolonged antioxidant protection of the endothelium. 167 Encapsulation of either catalase or SOD formed by controlled precipitation of magnetic nanoparticles (MNPs) using calcium and oleate provides composite nanocarriers (200–300 nm diameter) containing active catalase or SOD accessible to either H2O2 or superoxide, and protected from proteases. 168 Additionally, in vivo PECAM-1-directed non-polymeric MNPs loaded with SOD or catalase accumulated specifically in the pulmonary endothelium, and catalase-loaded endothelial-targeted particles alleviated pulmonary edema and leukocyte infiltration in a mouse model of endotoxin-induced lung injury, whereas SOD-loaded targeted carriers mitigated LPS-induced lung inflammation. 169
The last two decades have demonstrated significant progress in the formulation of delivery systems carrying antioxidant enzymes, and their applications, to pathologies critically susceptible to oxidative stress including organ transplantation, ischemia-reperfusion, and inflammation. Going forward, testing new target molecules, as well as new delivery systems and the optimization of current platforms, will provide important steps in the translation of targeted antioxidants into the clinical domain, thereby improving management of disease conditions involving this pathological mechanism.
Endothelial targeting of antithrombotic agents
While typically associated with diseases of the systemic circulation, such as myocardial infarction and ischemic stroke, thrombosis and thromboembolism in the pulmonary vasculature are not only a source of direct morbidity and mortality (e.g. in patients with PE), but prominent features of the pathophysiology of nearly all of the lung diseases discussed in this review.170,171 In a landmark study in 1983, Tomashefski et al. used a variety of pre- and post-mortem techniques to examine the pulmonary vessels of 22 patients who died of ARDS, noting thromboemboli in all but one patient and microvascular thrombosis in 19 of 22. Microscopic evidence of acute endothelial injury, even in patients who had survived the early hemorrhagic and exudative phase of the syndrome, suggested local coagulation as a critical and ongoing pathophysiologic event. 172 This process has since been shown to result from both an increase in procoagulant forces (predominantly tissue factor) and failure of endogenous anticoagulant systems.24,173,174 Similarly, histopathologic studies of PAH have shown a high incidence of thrombotic lesions, even in the subset of patients with arteriopathy and plexiform lesions.175,176 As with ARDS, increased expression of tissue factor and loss of key antithrombotic molecules, like thrombomodulin, have been identified as contributors to local coagulation and disease progression.28,177,178
Given the suspected pathophysiologic role of coagulation and, specifically, dysfunction of endogenous antithrombotic mechanisms in lung disease, it is no surprise that a number of efforts have been made to boost these protective pathways pharmacologically. Rather than directly target pulmonary endothelial function, however, most therapeutic programs have focused on systemic infusion of endothelial-derived agents. Among the drugs studied in lung diseases are several small molecules with vasodilatory and antiplatelet activity, such as nitric oxide and prostacyclin (epoprostenol), and biotherapeutics from the three major endogenous anticoagulant pathways, including activated protein C (APC), tissue factor pathway inhibitor, and antithrombin.2,179–183 While some of these therapeutics have found clinical application (e.g. epoprostenol in PAH), the majority of the clinical results have been disappointing and there is increasing consensus that systemic infusion simply may be inadequate to reproduce the activity of highly regulated and localized endothelial systems.
As an alternative, a number of groups have used targeted drug delivery to direct antithrombotic agents to endothelial cells. 184 In some cases, the intention has been localization of therapeutic activity to increase efficacy or diminish the risk of bleeding toxicity, whereas in others, the goal has been to alter the phenotype of the endothelium itself, restoring endogenous anticoagulant and anti-adhesive mechanisms which may have been compromised with the progression of disease. 185 While theoretically attractive, this approach has required new technology to circumvent a significant practical challenge, the rapid internalization of multivalent antibody targeted NPs or protein therapeutics by vascular endothelial cells. To promote retention on the endothelial surface and sustained interaction with the bloodstream, protein cargo has been genetically fused to monovalent affinity ligands, such as single chain variable fragments (scFv), which generally have a lower rate of endocytosis following binding to cell adhesion molecules and other surface determinants.132,186
Our group has pursued delivery of two major classes of antithrombotic proteins to the vascular endothelium. The first is tissue plasminogen activators (tPA), clinically approved for treatment of ischemic stroke and myocardial infarction and recently studied as a means of improving outcome in massive and sub-massive PE. 28 A fusion protein of a single chain fibrinolytic enzyme and a PECAM-1 targeted scFv was found to accumulate in the cerebral vasculature and, when used prophylactically, enhanced reperfusion and reduced BBB disruption following cerebral embolization of fibrin clots. 186 The same therapeutic was also effective in the pulmonary vasculature, demonstrating approximately 2–3 times more fibrinolysis than free enzyme in the setting of venous thromboembolism. 179 However, the apparent need for prophylactic administration limits the practical utility of endothelial-targeted fibrinolytic agents and, while it is possible that vascular targeting may also result in improved efficacy or diminished toxicity after embolic insult, this hypothesis has not been rigorously tested.
The other major application for which scFv targeted fusion proteins have been explored is as a means of augmenting the endothelial protein C (PC) pathway. 181 The key component of this endogenous enzymatic system is the endothelial membrane protein, thrombomodulin (TM), which binds thrombin, changes its enzymatic specificity, and inhibits both coagulation and vascular barrier leak. 180 As mentioned above, the pleiotropic effects of TM, its high level of expression in the pulmonary microvasculature, and its suppression in the presence of disease have led to significant interest in its role in the pathogenesis of lung diseases.24,28,187 Loss of endothelial TM and a second protein, the endothelial protein C receptor (EPCR), which binds protein C and positions it optimally for cleavage by the thrombin–TM complex, results in an imbalance between thrombin and APC, a protease previously approved for the treatment of severe sepsis and studied in a clinical trial of ARDS. 188 While this study was terminated due to apparent lack of efficacy, its authors noted that a low dose was used due to concerns for bleeding risk, the drug’s major toxicity and reason for ultimate withdrawal from the market. As an alternative with lower risk of spontaneous hemorrhage, our group fused TM with the same PECAM-1 specific scFv used for delivery of fibrinolytics and found significant protection in murine models of pulmonary inflammation, hyperoxia, and ischemia/reperfusion injury. 179
This preliminary success motivated further investigation of underlying mechanisms and led to the discovery that scFv/TM fusion protein bound to PECAM-1 does not interact with EPCR in the same way as endogenous TM. 181 The result has been the development of two distinct strategies for augmenting the endothelial protein C pathway, one in which scFv/TM is targeted to ICAM-1, which improves enzymatic partnering with endogenous EPCR, and the other in which two recombinant fusion proteins, scFv/TM and scFv/EPCR, are delivered to adjacent epitopes of PECAM-1, allowing synergistic interaction on the endothelial membrane.181,189 In addition, fusion proteins which incorporate human TM and human specific or species cross-reactive scFv have now been developed.186,190 These agents have allowed confirmation of the antithrombotic effects of scFv/TM in humanized systems, including a recently described microfluidic model of tissue factor-driven, inflammatory thrombosis. These studies not only support the translational prospects of targeted TM, but demonstrate the potential utility of microfluidic models of the endothelial–blood interface and alveolar–capillary unit as tools for testing drug delivery systems in healthy and injured lung vasculature.186,191
Diseases to treat by targeting the pulmonary vasculature
As mentioned above, the pulmonary vasculature plays a significant role in many, if not all, lung diseases. However, only a subset of pulmonary diseases warrants the development of a DDS that targets the pulmonary endothelium. Just a few parameters can be used to evaluate the utility of endothelium-targeted DDSs in a particular disease. 185
First, endothelium-targeted DDSs are not optimal for delivery to the airways. Many lung diseases, most notably asthma, are primarily diseases of the airways. Inhaled delivery to those airways is already sufficient and therefore endothelium-targeted DDSs are not needed for diseases of the airways.
Second, the role of the endothelium in the pathophysiology should be well understood. For example, there is certainly evidence that the endothelium plays a role in the development of COPD, but the mechanisms are uncertain. However, a caveat to this guideline is that even if the endothelium’s role in the pathophysiology is not well understood, endothelium-targeted DDSs could still help by turning the endothelium into a drug depot that elutes to the rest of the parenchyma. Many small molecule drugs diffuse well out of cells, so if the DDS delivers drugs to the endothelium, those drugs could then act on nearby other cell types.
Third, the disease must have a severity and acuity that are compatible with a medication that is IV-delivered. All known endothelium-targeting DDSs require IV injection. IV injections are not practical for most outpatient diseases (e.g. chronic cough), unless the disease is very severe (e.g. PAH). However, for some diseases, it is conceivable that patients would comply with a monthly visit to an infusion center, as is done for many protein therapeutics for rheumatological diseases. Additionally, in select severe diseases like PAH, long-term central lines (e.g. a Hickman catheter) are currently used by some patients and could be used for endothelium-targeted DDSs. But the diseases most amenable to obligate-IV medications are ICU diseases, such as ARDS and PE. In such ICU diseases, the patients almost always already have an IV catheter in place, often in a central vein, making IV infusions facile.
Lung diseases and target regions for therapeutic interventions.

Brief list of targeted formulations used in animal models of ARDS.
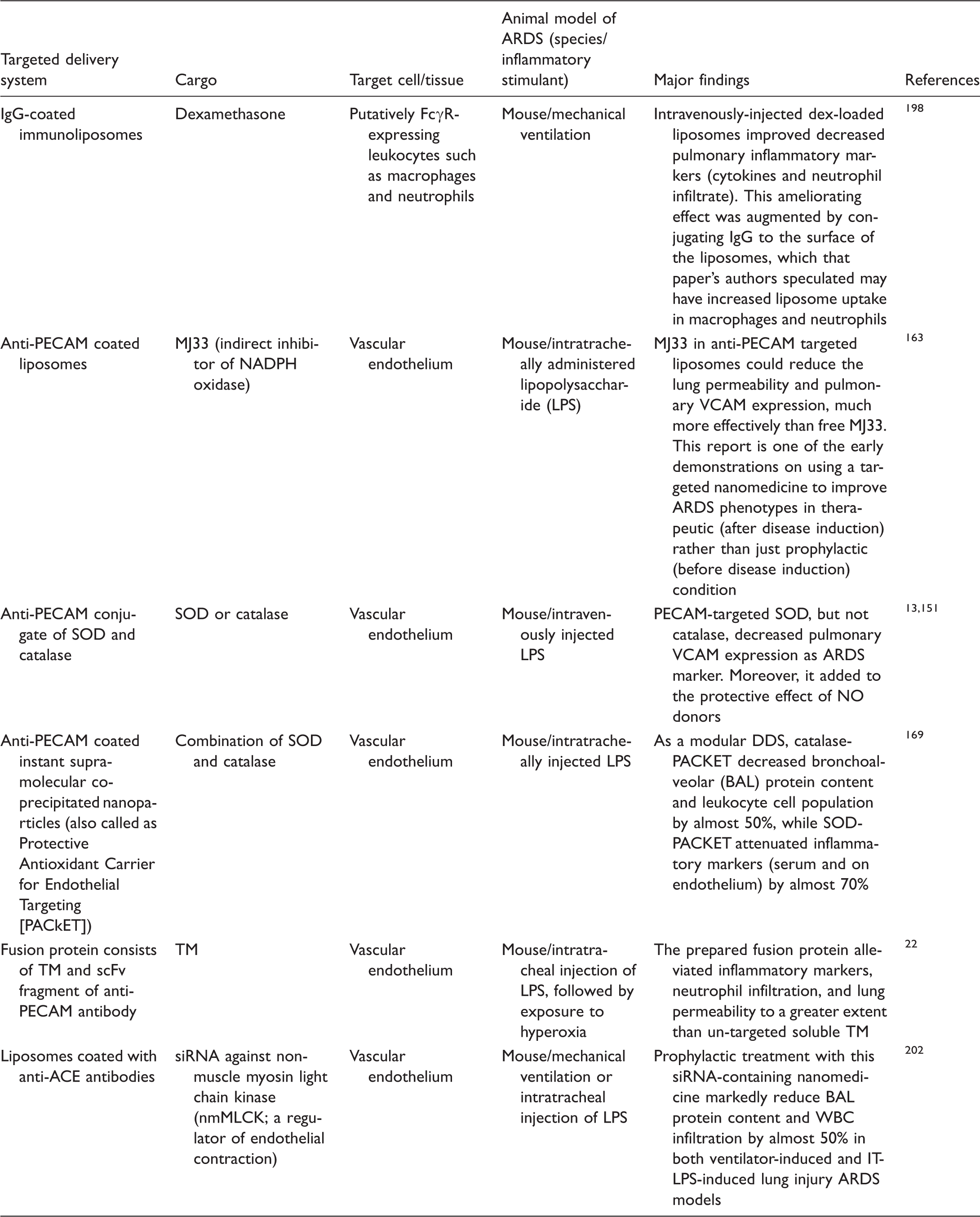
TM, thrombomodulin.
To illustrate the utility of endothelium-targeted DDSs in ARDS, it is helpful to first examine the unmet need in ARDS. ARDS afflicts ∼ 190,000 Americans each year, has a mortality rate of ∼ 40%, and no FDA-approved drugs to treat it. Nearly two dozen drugs have failed in ARDS clinical trials. Why have there been so many failures in ARDS? From a pharmacology perspective, three reasons stand out: (1) ARDS patients are fragile, with multi-system organ dysfunction, so do not tolerate off-target side effects; (2) the inhaled route of drug delivery is challenging because of the layer of liquid filling the alveoli; and (3) the disease is heterogeneous within a population, so targeting a single pathway is unlikely to work on a mixed population.
Endothelium-targeted DDSs seem well suited to these pharmacological challenges. By targeting the drug solely to the flooded alveoli, DDSs could avoid off-target side effects. Additionally, these DDSs avoid the inhaled route, as they are obligate-IV formulations. Finally, the DDSs are capable of carrying multiple cargo drugs, which could act on multiple different signaling pathways simultaneously. A DDS designed to meet these specifications should greatly improve the chances of a successful clinical trial. Several endothelium-targeted DDSs have been designed to meet these specifications. They all involve using three main features: carrier that contains the therapeutic; a lung-targeting moiety (almost always an antibody or fragment thereof); and, of course, the cargo drugs. We summarize each of these three components below.
Multiple carriers have been used to target therapeutics to the lungs of animal models of ARDS. The most common have been liposomes.163,197,198 Liposomes are ∼ 100 nm-diameter lipid bilayers. Liposomes been used in patients as drug carriers since the 1990s, which means that they have a long history of safety and the industrial manufacturing processes have been well worked out. While liposomes have the advantage of longer and broader use, several other drug carriers have been used in ARDS studies, including enzyme–protein conjugates13,151 and polymer NPs. 199 Another very notable carrier design is that of a fusion protein. In a fusion protein, a single chain variable fragment (scFv) of an antibody is genetically fused to a therapeutic protein. One such fusion protein, with an scFv targeting PECAM-1 fused to the anti-thrombotic/anti-inflammatory protein thrombomodulin, showed an ability to prophylactically prevent ARDS phenotypes in a mouse model of ARDS. 22 In choosing a carrier for targeting ARDS, it is best to match the carrier to the cargo therapeutic, while also considering carrier’s safety and manufacturability.
The vast majority of studies have used as their targeting moiety antibodies that bind to endothelial luminal proteins, such as PECAM-1, ICAM-1, APP, and others listed in the sections above. One study, 197 however, used anti-surfactant protein A (anti-SPA) antibodies, which is only expressed on the alveolar epithelium. Unfortunately, that study did not assess the fraction of the DDS that reached the lungs, so it is difficult to compare its targeting capabilities to those of endothelial targets. Indeed, a first step in determining which affinity moiety to employ is a quantitative assessment of the fraction of the DDS that reaches the lungs, preferably the most injured alveoli.
There are many possible cargo drugs for ARDS. For example, the list of >20 drugs that failed in clinical trials, mostly due to off-target side effects, are a reasonable place to start. Additionally, dozens of other drugs have shown efficacy in animal models, but often at doses that are unrealistic in humans. Among the drugs that have shown promise already in endothelium-targeted DDSs in ARDS model are: corticosteroids;197,198 small molecule antioxidants such as N-acetylcysteine, α-tocopherol, MJ33, and EUK-134;163,164,200,201; anti-oxidant enzymes such as catalase and superoxide dismutase;13,151,153 and thrombomodulin. 22 Very intriguingly, nucleic-acid based cargos have also shown promise. For example, siRNA directed against non-muscle myosin light chain kinase was loaded into liposomes coated with anti-ACE antibodies, and when given prophylactically, reduced ARDS-like phenotypes in mice. 202 This proof-of-principle suggests that other genetic cargoes (plasmid DNA, siRNA, shRNA, miRNA, mRNA, etc) might also open a large number of pathways to attack with endothelium-targeted DDSs.
While many of the DDSs described above show promise in ARDS models, much work is to be done. First, most of the studies used the drugs as prophylaxis, not treatment, which is probably unrealistic for ARDS. Second, it is important to use multiple animal models that display severe pathology, not just ones with mild pathology. Finally, it is important to consider toxicology early, as a DDS may shift toxicity from one organ to another. And notably, the above paradigm, as described for ARDS, can be used for the other pulmonary diseases of Table 2.
Cautionary notes: remember Hippocrates
There is no such thing as a perfect targeted therapeutic, especially when facing one of the most sophisticated, complex, sensitive, and important cell types in the body. The aim of vascular targeting in the diseases mentioned here is to improve lung health, rather than the simpler task of targeted drug delivery in cancer, which must only destroy invading cancerous cells. Thus, the standards of safety are different in dealing with cardiovascular, pulmonary, neurological or metabolic complications than for tumor-targeting applications. 203 Therapeutics developed to improve these systemic pathologies are usually more benign than anti-cancer agents; thus, pan-endothelial delivery of antioxidant, anti-inflammatory, or anti-thrombotic agents throughout the vasculature seems to be a suitable option for translation. In addition, physiology plays a major role in this situation, as the target for the vast majority of endothelial targeted nanomedicine targets is the lung, which truly favors the first pass phenomenon.
One of the major concerns in every type of targeting strategy is how non-target cells expressing the ligand of interest could affect or even change the intended therapeutic intervention. As mentioned earlier, most endothelial determinants are ubiquitously expressed throughout the endothelial vasculature of different organs. Moreover, some targets such as CAMs are expressed on other cell types such as epithelial cells or and leukocytes, although mostly at lower protein concentrations.
Another major concern in targeting vascular determinants, especially in systemic disorders, is that the no-harm rule should be carefully followed in terms of targeted cells. Unlike the “find and kill” mission of cancer nanomedicine, in which, an “incidental” toxic effect on the target tumor cell is often cheered, here, endothelial disturbance must be minimized. Moreover, engagement of target determinants by a multivalent carrier presenting antibodies against that target may induce their shedding, internalization, and/or dysfunction. In all the scenarios, there is a chance to induce aggravation of oxidative stress, inflammation, and thrombosis, which should be avoided.
For example, there are several reports on using antibodies against the endothelial glycoprotein thrombomodulin to prepare liposomal formulations targeted to the pulmonary endothelium in vivo.204,205 However, thrombomodulin affects thrombin, and the inhibition of its protective function by engaging it with antibody-functionalized NPs increases the risk of thrombosis and inflammation.180,206 This concern basically makes it impossible to use this endothelial determinant as a suitable target for endothelial-directed DDSs.
Another example is targeting DDSs to ACE and APP, peptidases that cleave mediators including bradykinin. 207 Engagment of DDSs with these peptidases may have consequences such as vascular edema and severe hypotension due to elevation of bradykinin and other signaling peptides. It should be noted that inhibition of angiotensin II production by ACE may be valuable in hypertension and inflammation. Therefore, it is always important to evaluate the impact of using each determinant for nanocarrier targeting in each clinical context.
A common caution with decorating NPs with antibodies is that their unique characteristics may create the chance of activation of complement and other host defense systems in the bloodstream. Complement components and immune cells interact with the Fc fragment of antibodies, leading to rapid clearance from the circulation and immune reaction. As an alternative to antibodies, antibody derivatives called single-chain variable fragments (scFv) can be used as targeting moieties for DDs. scFv retain most of the positive features of antibodies while eliminating Fc-mediated immune responses and clearance mechanisms. However, it should be noted that selective tissue uptake obtained with whole antibodies is usually higher than the one achieved by antibody fragments.
Lastly, we should be aware that proven biocompatibility for each individual components of a DDS does not necessarily translate into a safe DDS. 208 Loading a relatively benign agent into a relatively safe carrier decorated by harmless ligands may generate a combination with pro-inflammatory or adjuvant characteristics. These and other aforementioned cautionary notes are critical in pushing forward the clinical endothelial nanomedicine for pulmonary, cardiovascular, cerebrovascular, and other diseases in need of therapy.
Footnotes
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research was supported by National Heart, Lung, and Blood Institute Grants 1RO1 HL125462-02 (VRM), 1RO1 HL128398-02 (VRM) and RO1 HL126874-01A1 (VRM).
2017 Grover Conference Series
This review article is part of the 2017 Grover Conference Series. The American Thoracic Society and the conference organizing committee gratefully acknowledge the educational grants provided for the support of this conference by Actelion Pharmaceuticals US, Inc., Gilead Sciences, Inc., and United Therapeutics Corporation. Additionally, the American Thoracic Society is grateful for the support of the Grover Conference by the American Heart Association, the Cardiovascular Medical Research and Education Fund, and the National Institutes of Health.
