Abstract
The capacity of existing blood vessels to give rise to new blood vessels via endothelial cell sprouting is called angiogenesis and is a well-studied biologic process. In contrast, little is known about the mechanisms for endothelial cell replacement or regeneration within established blood vessels. Since clear definitions exist for identifying cells with stem and progenitor cell properties in many tissues and organs of the body, several groups have begun to accumulate evidence that endothelial stem and progenitor cells exist within the endothelial intima of existing blood vessels. This paper will review stem and progenitor cell definitions and highlight several recent papers purporting to have identified resident vascular endothelial stem and progenitor cells.
Somatic stem and progenitor cells provide a source of tissue-specific cellular elements that permit appropriate tissue and organ functions through replacement of injured, diseased, and senescent cells in many organ systems throughout the lifespan. 1 Hematopoietic,2,3 intestinal,4,5 skin,6,7 and skeletal muscle stem cells8,9 have been identified and rigorously studied; however, little is known of the cellular and molecular mechanisms that give rise to the homeostatic repair and replacement of vascular endothelial cells. In 1997, Asahara et al. 10 reported on the identification of circulating progenitor cells for the endothelial lineage. These putative endothelial progenitor cells (EPC) were bone marrow-derived cells that displayed an upregulation of “endothelial” cell surface markers and downregulation of “hematopoietic” markers during in vitro culture, suggesting that some hematopoietic stem cells (HSC) displayed the ability to transdifferentiate into EPC to regenerate endothelial cells in vitro.11,12 These putative EPCs also displayed colony-forming activity and were capable of migrating to sites of ischemic injury in vivo in animal models of human disease. Since these putative EPCs were isolated from human blood but participated in neovascularization in the tissues of injured animals, the authors proposed that the cells were engaged in postnatal vasculogenesis as a means to repair the damaged blood vessels. Numerous publications followed where various cell surface markers were identified as enriching for the putative HSCs that could transdifferentiate into EPC subsets to enhance vascular repair13,14 (reviewed in Kovacic et al. 15 ) or could serve as a biomarker for the presence or severity of cardiovascular disease in humans (reviewed in the literature16–19).
Subsequent studies have clarified that those putative EPCs did not possess the capacity to undergo a lineage fate switch (transdifferentiate) from a hematopoietic precursor to a mature endothelial cell. Instead, a series of papers demonstrated that the putative EPCs were in fact events in which labeled donor bone marrow cells either displayed no evidence of plasticity upon rigorous scrutiny,20–22 displayed the host phenotype in tissues following transplantation via spontaneous cell fusion,23,24 were an artifact of host tissue autofluorescence, 25 or that were erroneously attributed to becoming integrated in the endothelial intima at sites of injury, when detailed confocal microscopic analysis determined that donor bone marrow cells were localized in peri-endothelial sites and not integrated as endothelial cells. 26 Subsequently, the putative bone marrow-derived EPCs were shown to be comprised of numerous stages of hematopoietic stem and progenitor cells (HSPC) that can serve paracrine proangiogenic functions to promote vascular repair and replacement through endogenous endothelial cell mechanisms.20,22,26–35 Indeed, these proangiogenic cells could upregulate some “endothelial cell” markers in vitro and thus give the impression they were becoming endothelial cells; however, functional analysis, 36 comparative gene expression profiling,37,38 and analysis of the methylation status of promoters for key known endothelial regulatory genes 39 confirmed that the proangiogenic cells remained more closely aligned to HSPC than mature endothelial cells. Thus, a recent position paper has called for the substitution of the term myeloid angiogenic cells (MAC) for the term EPC when considering the reparative role played by bone marrow hematopoietic-derived cells in the neovascularization process. 31
Some reports have proposed evidence that vascular endothelial cells may also arise from resident vascular progenitor cells. During murine embryogenesis, mesoangioblasts have been identified that emerge from the dorsal aorta and give rise to endothelial, skeletal muscle, bone, cartilage, and dermal cells. 40 The mesoangioblasts display many properties similar to pericytes that are important for controlling the proliferation and differentiation of capillary endothelial cells. Whether these pericytes and mesenchymal stem cells (MSC) within the media and adventitia are resident progenitor cells for all the vascular lineage components has been reviewed on several occasions.41,42 Greiner et al. 43 identified stem cell antigen-1 (Sca-1) expressing precursors upon enzymatic digestion of small murine vessels that displayed potential to form endothelial cells in vitro and the endothelial cells displayed vasculogenic functions. However, the location of these cells within the vasculature was not reported. Zengin et al. 44 isolated progenitor cells residing between the vascular media and adventitial layers of murine arteries and veins that possessed endothelial cell phenotypic features and capillary tube forming potential in vitro. Similar localization of resident angiogenic mesenchymal progenitor cells were identified in human thoracic aortic samples from humans . 45 While interesting, the exact roles played by these resident multi-potent progenitor cells in normal endothelial repair and replacement or following injury has not been pursued or translated into human studies, perhaps due to the requirement for recovery from the host vasculature.
Thus, while some data suggest resident vascular progenitor cells may give rise to endothelial cells (among other lineages), what general evidence has been published that would suggest the endothelial intima may give rise directly to reparative or regenerative activity? Obviously, thousands of papers have been published on the topic of angiogenesis over the past three decades and it has become very clear that the systemic circulation can adapt to requirements for more vasculature or less vasculature to meet homeostatic balance or in response to tumor invasion via this mechanism.46–48 More than four decades ago, several reports highlighted the presence of proliferating endothelial cells during rodent development and that in response to vascular injury, clusters of replicating endothelial cells could be identified in areas of “high turnovers”49,50 (reviewed in detail in Yoder 51 ). In the developing mouse embryo, outgrowth of mesoderm-derived precursors displaying endothelial markers displayed a high capacity for prolonged proliferation and ability to incorporate into developing chick embryonic vasculature, but such cells were not prospectively identified within the embryo, studied at a clonal level, or examined for chromosomal abnormalities. 52 It has also long been known that among all adult murine tissues, the lung vasculature is one of the most readily amenable to use for isolation and cultivation of endothelial cells that possess proliferative potential.53–55 Several publications have highlighted the capacity for the endogenous endothelial cells within the lung vasculature to give rise to replacement endothelial cell progeny that form new blood vessels upon transplantation56,57 or return vascular function to normal following an acute challenge with lipopolysaccharide (LPS). 58 Others have shown that removal of the left lung lobe in a rodent results in compensatory overgrowth of the right lung to rescue lung function, but this lung epithelial expansion is dependent upon endogenous lung vascular endothelial proliferation and vascular expansion.59–61 Likewise, active angiogenesis within the murine skeletal system is required to support osteogenesis. 62 Recently, a novel population of proliferative capillaries within the bone metaphysis (1.77% of total endothelium) was identified that function as a precursor population to mediate normal growth of the bone vasculature, to respond to various stressors or metabolic perturbations to rescue damaged skeletal microvasculature, and were shown to be diminished in concentration with aging concomitant with loss of osteoprogenitor cells. These are just a few examples to illustrate the point that accumulating evidence highlights the resident vascular endothelium as a source of regenerative endothelium during development and in response to injury.
The largely unanswered question is whether sufficient evidence exists that well defined endothelial stem and progenitor cells have been identified in murine tissues and organs. What criteria have been used to define such cells? Have the various putative stem and progenitor cells been scrutinized to identify similarities or differences in their location, gene expression, fates, and responses to injury? This paper will now provide a brief overview of common definitions for somatic stem and progenitor cells and then in the light of these terms, review evidence to support the identification of resident vascular stem and progenitor cells in mouse and man.
Assays to identify endothelial stem and progenitor cells
Somatic stem cells can be simply defined as clonally proliferative, self-renewing cells, which give rise to differentiated cell types in a particular tissue or organ. 1 A somatic stem cell may be multi-potent (giving rise to multiple types of differentiated cells) or unipotent (differentiating into a single lineage of mature cells). In general, somatic stem cells are located within nurturing niches in the tissue or organ for which they generate replacement progeny; for example, intestinal stem cells are present within the intestinal epithelium and skin stem cells reside within the dermis (hematopoietic stem cells are an exception as they reside in the bone marrow but their progeny are distributed throughout the blood and within tissues).2,63–68 Progenitor cells lack self-renewal potential, however, they may clonally expand prior to differentiation into a single lineage of mature cells. Like somatic stem cells, the majority of somatic progenitor cells reside within the tissues for which they provide replacement mature cells.
Multiple assays have been developed to define stem and progenitor cells that reside in different organs and tissues. 1 Stem cells in any tissue must be interrogated for clonal self-renewal. This property is most stringently proven by long-term in vivo persistence with retained capacity for contribution to differentiated progeny. In the murine system, long-term contribution to a particular lineage is best demonstrated through the use of fate mapping strategies (with or without induced perturbations or injuries that require cell replacement). Transplantation assays into primary and secondary recipient hosts are powerful tools to examine clonal self-renewal and long-term contributions to particular cell lineages, but may represent highly stressful and forced expansion of low numbers of transplanted donor stem cells into a system in which endogenous progenitor and mature cells may have been drastically diminished.69–71 Progenitor cells are often measured with colony forming assays in vitro (to prove a precursor product relationship). Stem and progenitor cells may also display distinguishing cell surface markers that can be used to prospectively isolate the cells through use of monoclonal antibodies and flow cytometry or magnetic bead separation. Most recently, stem and progenitor cells from some tissues have become definable by single cell gene expression technologies to permit identification by a unique molecular signature.72–79 Presentation of some selected publications (as examples of detailed approaches to acquire sufficient evidence) identifying putative stem and progenitor cells for the vascular system follows.
To identify stem and progenitor cells for the endothelial lineage, we first need to decide what criteria should be used to define cells belonging to the endothelial lineage. Obviously, there are numerous phenotypic, morphologic, physiologic, genomic, proteomic, and functional parameters that constitute unique and characteristic behaviors of endothelial cells. The point here is that one cannot identify cells of the endothelial lineage by expression of a few cell surface markers or of a few RNA transcripts. For example, when using phenotypic markers to enrich for a stem cell population, functional evidence for enrichment of the particular stem cells must be presented as validation for any of the putative surface markers being highlighted. The best phenotypic markers would be unique and restricted to the particular stem cell being selected; however, this is often not the case and use of a panel of markers can be very useful in discriminating a particular stem cell from progenitor or mature cells within a tissue or organ. Functional evidence for the stem cell should be performed to provide evidence that the putative stem cell directly gives rise to progenitor and mature cells of that tissue or organ (may be conducted by fate mapping studies and/or transplantation as noted above). Transcriptomics and proteomics are increasingly being used at a single cell level to provide novel panels of enriched genes that are expressed by subsets of stem or progenitor cells within the same tissue or organ. 72 Thus, in most instances, to fully define a stem or progenitor cell for the endothelial lineage, one must utilize a panel of phenotypic, functional, physiologic, morphologic, and “omics” information concurrently. A few selected exemplary papers that have applied many of these principles to define endothelial stem and progenitor cells will be presented.
Progenitor cells for the endothelial lineage
Cell surface marker expression.
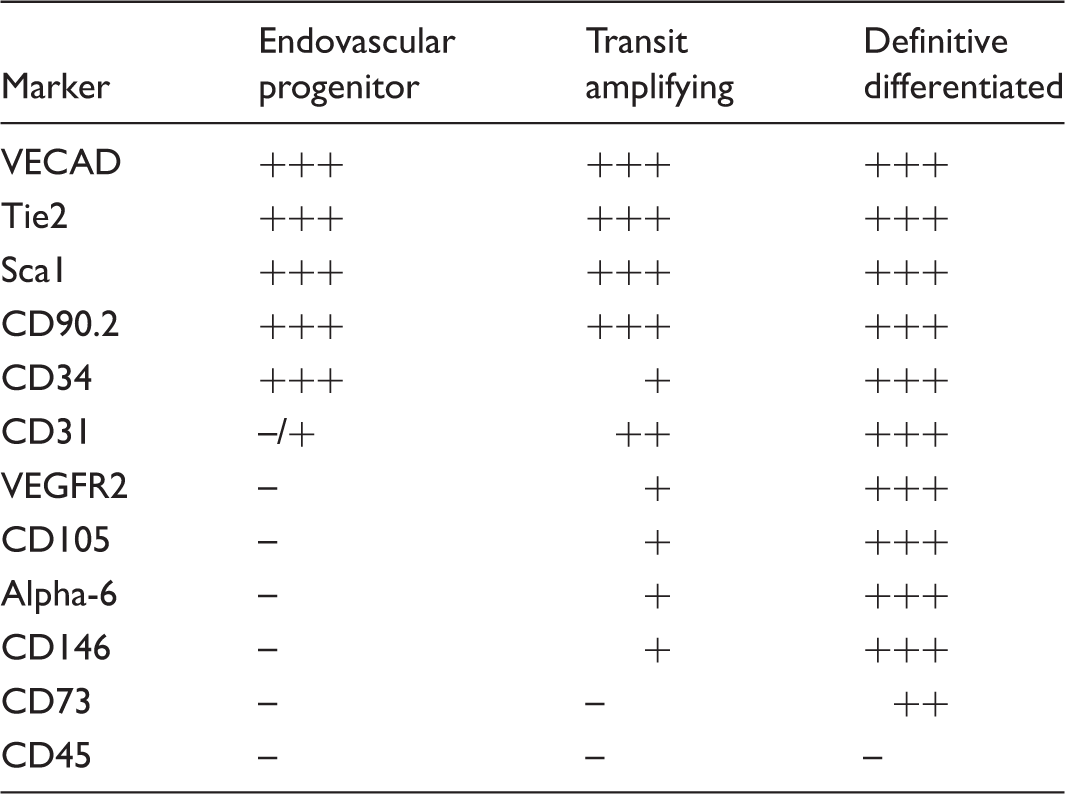
+, positive staining; –, negative staining.
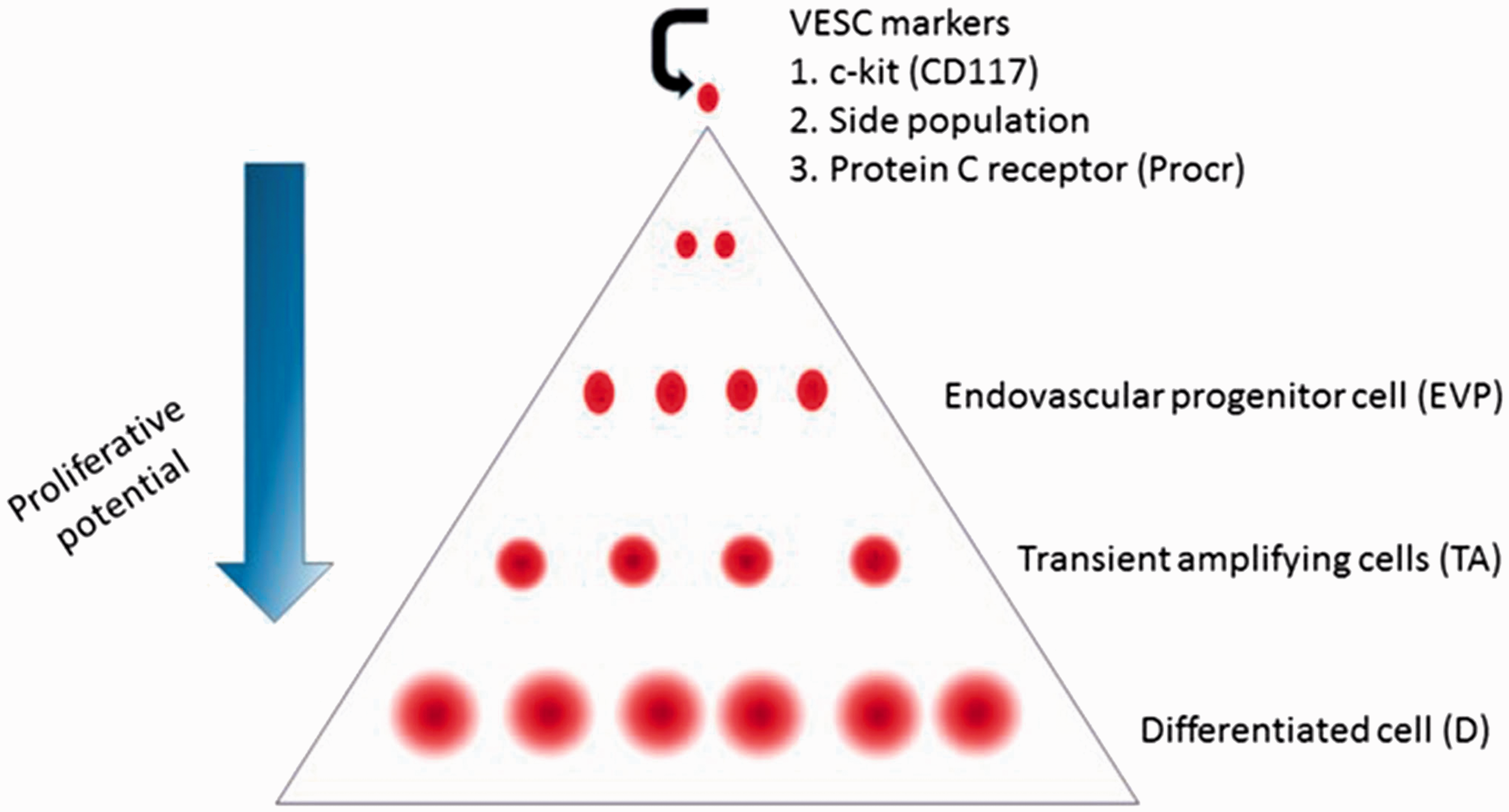
Evidence for a hierarchy of resident VESCs and progenitor cells. VESCs reside in the endothelial intima of blood vessels. Several markers for the VESCs have been proposed.71,72,74 The EVPs give rise to TA cells that produce definitive differentiated (D) cells. 60 VESCs display the greatest proliferative potential while the D cells are non-proliferative.
Evidence for the identification of clonogenic human endothelial progenitor cells (circulating or resident) has been published by several groups.83–86 Analysis of the circulating blood of patients following a sex-mismatched bone marrow transplant indicated that most of the circulating blood outgrowth endothelial cells (BOEC) were derived from the host, but the delayed outgrowth cells displayed the most proliferative cells and were donor derived.
87
Umbilical cord blood was reported to be enriched for clonogenic endothelial colony forming cells (ECFC) that displayed a hierarchy of proliferative potential and in vivo vessel formation compared to adult peripheral blood (Fig. 2).
88
The highly proliferative ECFC from cord blood expressed higher levels of telomerase than the ECFCs cultured from adult peripheral blood cells. Furthermore, resident vascular endothelial cells derived from umbilical veins or human abdominal aorta contained clonogenic ECFCs with vasculogenic potential.
89
Very recently, human-induced pluripotent stem cell (hiPSC)-derived ECFCs have been reported with properties that are similar to umbilical cord blood ECFCs but with some distinct differences in gene expression.
90
At present, it is unclear where the circulating BOECs and ECFCs are derived from; the most plausible source is the vascular endothelial intima, but convincing evidence is lacking to support this assertion. The lack of distinct cell surface markers to prospectively identify the circulating BOEC and ECFC has been and continues to be a significant impairment to further enrichment and development of these cells as a therapy for treating patients suffering from a host of cardiovascular disorders.
Model of a human ECFC hierarchy.
68
High proliferative potential-ECFC (HPP-ECFC) display the highest proliferative potential and self-renew with replating potential. Low proliferative potential-ECFC (LPP-ECFC) form colonies greater in size than endothelial cell clusters but less than HPP-ECFC and do not possess self-renewal potential. Mature differentiated endothelial cells do not divide.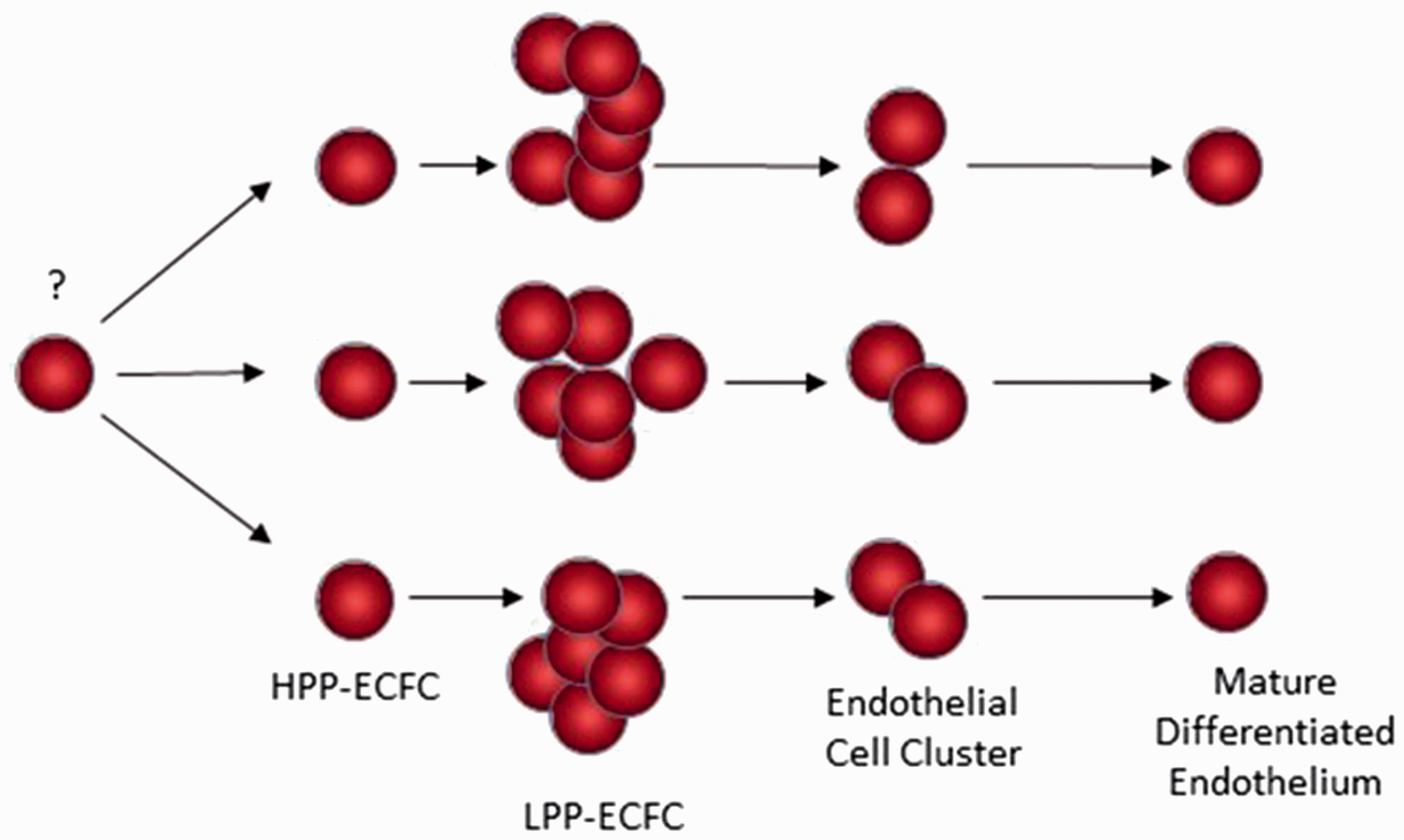
Vascular endothelial stem cells
Fang et al. 91 reported that stem cells for the endothelial lineage could be isolated from lung blood vasculature. Vascular endothelial stem cells (VESC) expressing the phenotype CD31+CD105+Sca-1+CD117+ (devoid of any mature lineage markers for the hematopoietic system) could be isolated from collagenase digested lung tissue. Only the VESCs displayed clonogenic colony-forming activity in vitro at a frequency of approximately six colony-forming units per 1000 isolated lung endothelial cells. When the green fluorescent protein (GFP)-tagged VESCs were suspended in Matrigel and implanted subcutaneously in mice, the donor GFP-expressing VESCs gave rise to donor derived blood vessels. Indeed, when 15 VESC-expressing GFPs were implanted with B16 tumor tissue, GFP-labeled blood vessels were identified in primary, secondary, tertiary, and quarternary tumor implants. Even a single VESC displayed the capacity to form donor blood vessels in vivo in a Matrigel implant. When mice deficient in CD117 expression were examined for endothelial cell colony-forming activity, a significant tenfold reduction in colony formation was identified. In addition, blood vessel density in CD117-deficient mice inoculated with B16 melanoma tissue was less than half the density observed in wild type-mice with the same tumor implants. Thus, the VESCs identified by Fang et al. 91 are marked by CD117 expression (Fig. 1) and loss of CD117 expression causes endothelial cell proliferation and angiogenesis defects. While some flow cytometric estimations of the frequency of the CD117-expressing VESCs in different tissues was reported, no detailed visualization of the precise location of the VESCs in arteries, veins, and capillaries in different tissues was presented. In addition, no fate mapping studies to identify the contributions of the putative VESCs within various vascular beds in homeostatic endothelial turnover was presented.
Stem cells from skin, lung, heart, mammary gland, muscle, and testis have shown evidence for expression of ATP-binding cassette (Abc) transporters that efflux noxious substrates and molecules outside the cells to maintain their viability; 92 thus, Hoechst 33342 DNA binding dye rapidly enters into cells but the presence of the Abc transporters results in efflux of the dye in stem cells causing them to display diminished fluorescence (SP) and permitting their identification and isolation by flow cytometric analysis and sorting. Summer et al. 93 were one of the first groups to demonstrate that adult murine lung tissue displayed a SP (0.3–0.7% of total cells) that appeared stable up through one year of age. SP cells derived from enzyme-digestion of the lung tissue were mostly blood cells (CD45+) but some non-blood cells also stained. A polyclonal antibody raised against an internal peptide sequence for breast cancer resistance protein 1 (Bcrp1; Abcg2) was used to demonstrate that SP cells were Bcrp1+. While smooth muscle cells and some distal epithelial cells expressed Bcrp1, these cells did not display a SP phenotype, suggesting that in these cells, there was no correlation between Bcrp1 expression and function to confer the SP phenotype. More recently, phenotypic lung SP cells identified as MSCs have been isolated that express Abcg2 and these MSC display properties of pericytes that contribute to fibrotic remodeling following injury.94,95 Lung SP cells isolated from embryos at embryonic day (E) 13.5–18.5 or postnatal day (P) 13–55 murine pups were shown to comprise both blood cell (CD45+) and non-blood cell (CD45–) subsets.96,97 The CD45+ lung cells also co-expressed fetal liver kinase 1 (Flk1) but did not express vascular endothelial cadherin (CD144). Both CD45+ and CD45– subsets gave rise to cells displaying phenotypic and some in vitro functional features of endothelial cells. No clonal analysis of ECFC potential, long-term contribution to lung endothelial retention, or capacity for vascular regeneration or repair by these precursor cells was presented.
Naito et al. 98 have also used the Hoechst staining method and have reported the identification of resident vascular endothelial cells within the side-population (SP). Endothelial SP were identified as dormant cells in the steady state, but possessed clonal colony-forming activity, and produced large numbers of mature endothelial progeny when cultured in vitro. When transplanted into experimentally induced ischemic lesions, the endothelial SP cells restored blood flow and reconstituted de novo blood vessels at the site of injection. Although the surface markers of the SP cells was similar to primary capillary endothelial cells, the gene expression pattern of the SP, and main population (MP) that fail to retain the Hoechst dye, was significantly different. The endothelial SP cells failed to express hematopoietic markers, including c-Kit (CD117), and could not be detected in bone marrow (Fig. 1). Bone marrow transplant studies reconstituted the peripheral blood cell lineages, as would be expected, but did not contribute to vascular endothelial SP cells. Use of the Hoechst method fails to permit identification of the putative VESCs within the organ and tissue vasculature during development or after injury and will rely upon further studies to identify novel cell surface markers. Of interest, several unique cell surface markers were identified in the SP cells that may permit prospective isolation of these putative VESCs.
More recently, Yu et al.
99
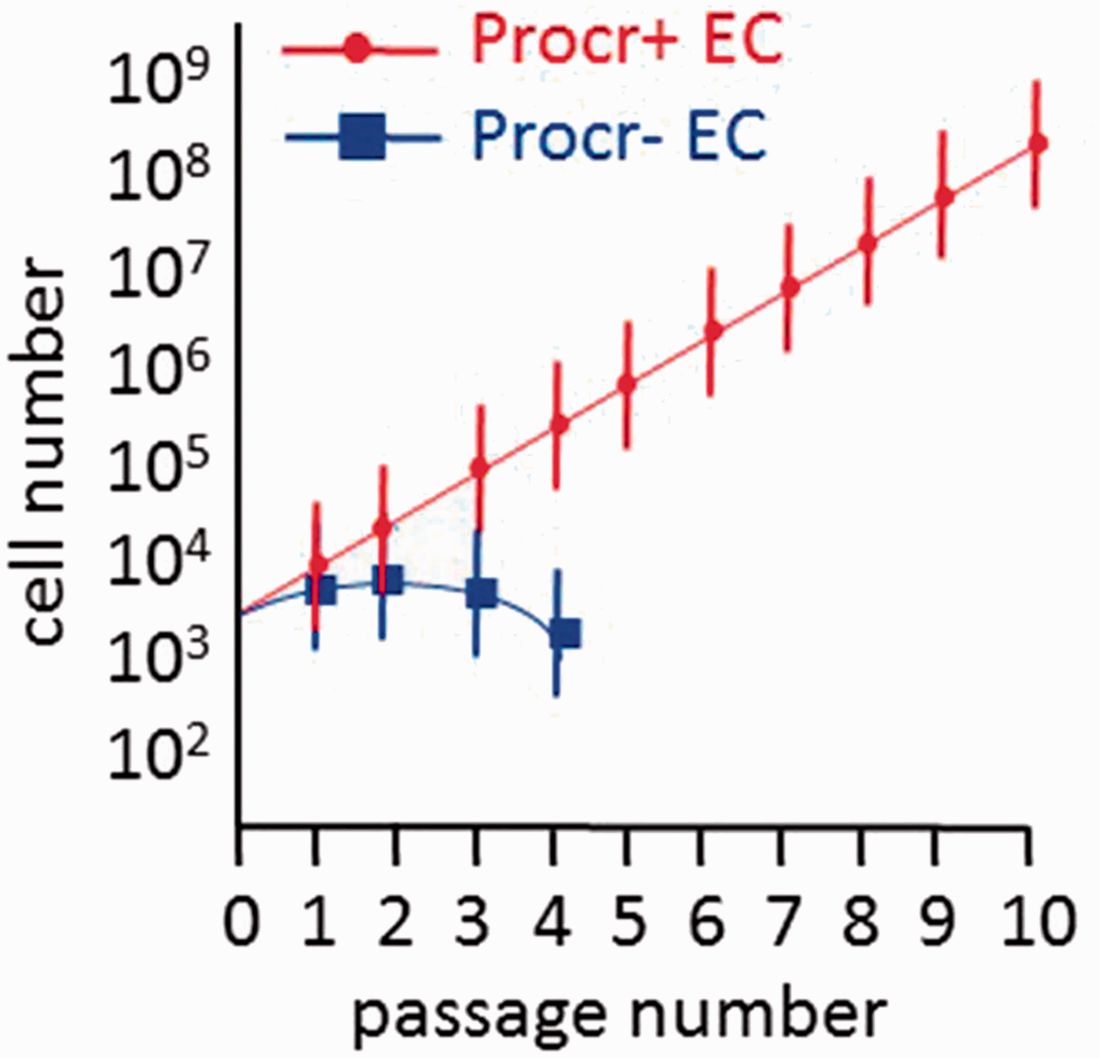
identified protein C receptor (Procr)-expressing endothelial cells as VESCs in the mammary fat pad, skin, and retina. Procr-expressing cells were identified in the tip and stalk cells of the pubertal stage of the mammary fat pad when robust angiogenesis accompanies rapid epithelial growth. In the adult mammary gland, Procr-expressing cells were predominantly found in the stalk cells in areas of angiogenesis. When single-cell suspensions of the mammary gland tissue were prepared and cells exposed to panels of monoclonal antibodies (all blood cells identified and excluded using CD3e, Ly6G/Ly6C, CD11b, Gr1, CD45R/B220, and Ter119) that included CD105 and CD31, approximately 4% of the vascular endothelium expressed Procr. Of interest, while > 85% of the Procr-expressing cells expressed Sca-1, only 2% of the endothelium expressed c-Kit and expression was in the Procr-negative fraction of cells. When Procr-expressing cells isolated from Procr-expressing endothelial cells display the greatest proliferative potential producing progeny through ten passages while the Procr-negative fraction fails to proliferate beyond four passages in vitro
74
.
Conclusions
There is a growing body of work to support the concept that endothelial stem and progenitor cells exist within the endothelial intima of resident tissue vasculature. At present, limited comparisons among the different approaches used by the authors has been accomplished, but some limitations of the present work can be identified. While the work of Patel et al. 80 has shown that endothelial progenitors can be identified by applying stringent criteria, the specific sites of EVP, TA, and D cell localization in organs and tissues at homeostasis (artery, vein, or capillary bed), the contributions of EVP to TA and D cells during homeostasis, differences in the EVP among different organs across the lifespan of the mouse, and determination of whether the EVP represents an endothelial stem cell remain to be addressed. Human endothelial progenitor cells (ECFCs) have been identified;87,88,90 however, no unique identifying markers have permitted prospective isolation of ECFCs from circulating blood or blood vascular endothelium to permit identification of the site of origin of ECFC in humans and determination of whether these cells display stem cell activity for the endothelial lineage. Several papers have published evidence for the presence of resident VESCs in mice; however, the relationship between the unipotent VESC identified by Fang et al. 91 and Naito et al., 98 and the bipotent VESC identified by Yu et al. 99 remains unclear. It is clear that the expression of c-Kit as a marker for VESC differs in these three papers as it is a critical marker in the work of Fang et al., 91 but is not expressed on the SP VESC of Naito et al. 98 or the Procr-expressing VESC of Yu et al. 99 Identification of unique and perhaps more distinguishing characteristics of the VESCs that discriminate these stem cells from progenitor and mature endothelial elements awaits additional study. Finally, no cell surface antigen has yet been reported that can be used to prospectively identify VESCs in mice and man. This is an exciting and emerging theme that will impact our understanding of how the vascular endothelium is organized and replenished throughout the lifespan and may offer new insights into mechanisms of acquired endothelial dysfunction and development of cardiovascular disease.
Footnotes
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
2017 Grover Conference Series
This review article is part of the 2017 Grover Conference Series. The American Thoracic Society and the conference organizing committee gratefully acknowledge the educational grants provided for the support of this conference by Actelion Pharmaceuticals US, Inc., Gilead Sciences, Inc., and United Therapeutics Corporation. Additionally, the American Thoracic Society is grateful for the support of the Grover Conference by the American Heart Association, the Cardiovascular Medical Research and Education Fund, and the National Institutes of Health.
