Abstract
The discovery that fear memories may change upon retrieval, a process referred to as memory reconsolidation, opened avenues to develop a revolutionary new treatment for emotional memory disorders. Reconsolidation is a two-phase process in which retrieval of a memory initiates a transient period of memory destabilization, followed by a protein synthesis-dependent restabilization phase. This reconsolidation window offers unique opportunities for amnesic agents to interfere with the process of memory restabilization, thereby weakening or even erasing the emotional expression from specific fear memories. Here we present four uncontrolled case descriptions of patients with symptoms of posttraumatic stress disorder (PTSD) who received a reconsolidation intervention. The intervention basically involves a brief reactivation of the trauma memory aimed to trigger memory destabilization, followed by the intake of one pill of 40 mg propranolol HCl (i.e. a noradrenergic beta-blocker) that should disrupt the process of memory restabilization. We present three cases who showed a steep decline of fear symptoms after only one or two intervention sessions. To illustrate that the translation from basic science to clinical practice is not self-evident, we also present a description of a noneffective intervention in a relatively complex case. Even though the reconsolidation intervention is very promising, the success of the treatment depends on whether the memory reactivation actually triggers memory reconsolidation. Obviously the uncontrolled observations described here warrant further study in placebo-controlled designs.
Keywords
Introduction
At the turn of this century, a major breakthrough in neuroscience was achieved with the (re)discovery that fear memory is not inevitably permanent (actually this was a rediscovery: post-retrieval transient amnesia was first revealed in the 1960s by Donald Lewis [Lewis et al. 1968]), but can change when retrieved [Nader et al. 2000; Sara, 2000]. Nader and colleagues demonstrated in rats that upon retrieval, consolidated memories may return to a labile state, requiring
In a recent study we translated these laboratory findings on conditioned fear responding to a subclinical double-blind trial in individuals with spider phobia. We showed that a single 40 mg dose of the β-AR blocker propranolol HCl administered directly upon a very short memory reactivation, transformed avoidance behavior into approach behavior in a virtually binary fashion (i.e. spider phobics now fondling our live tarantula): an effect that persisted at least 1 year post-treatment [Soeter and Kindt, 2015b]. Targeting fear memory in spider phobia may be regarded as an endeavor of intermediate clinical complexity, compared to fear-conditioning research in healthy individuals on the one hand, and the more severe anxiety disorders and posttraumatic stress disorder (PTSD) on the other. Trauma memories are typically stronger and broader than fear memories either formed in the laboratory or in individuals with spider phobia, and we know from animal research that stronger and broader memories are relatively resistant to change [Finnie and Nader, 2012]. Nevertheless these findings suggest that we might be on the verge of a breakthrough in reconsolidation-based interventions, although the critical conditions for targeting the complex and pervasive fear memories (i.e. trauma memories) typically encountered in clinical practice are yet unknown.
In sum, pharmacologically-induced amnesia for learned fear has been extensively demonstrated across a wide variety of species, and it clearly outperforms extinction learning: currently the experimental model for exposure as the treatment of choice in anxiety disorders and PTSD [Craske et al. 2014]. The return of fear after cognitive behavioral therapy (CBT)-like interventions can be best explained by the neuroscience literature on fear conditioning and extinction. A consensus has been reached that extinction learning does not erase the original fear memory but instead reflects the formation of a new inhibitory memory, which competes with the earlier formed fear memory [Bouton, 2002]. As a consequence, the fear memory remains intact and may resurface, resulting in a return of fear even after initially successful fear extinction. In contrast, the reconsolidation intervention directly affects the original memory trace and may thereby overcome this potential limitation of extinction learning [Finnie and Nader, 2012; Kindt, 2014]. Nevertheless, clinical observations, pilot findings, and previous studies in our own lab show that the success of reconsolidation interventions is not guaranteed [Bos et al. 2014; Sevenster et al. 2012, 2013, 2014; Wood et al. 2015]. The effect of the intervention depends on whether the memory reactivation actually triggers memory reconsolidation. We observed, among other things, that mere retrieval of the fear memory is not sufficient to induce memory reconsolidation. Only if the retrieval experience contains novel or unexpected information, referred to as prediction error (PE), the memory engram will be destabilized [Pedreira et al. 2004; Morris et al. 2006; Sevenster et al. 2012, 2013, 2014]. Although preliminary evidence in patients with PTSD revealed a reduction in trauma-relevant physiological responding following a reconsolidation intervention [Brunet et al. 2008; Brunet et al. 2011; Poundja et al. 2012], this initial finding could not be replicated in three follow-up trials [Wood et al. 2015]. Of note, these previous clinical trials used script-driven imagery for the reactivation of the trauma memory, while this method has been explicitly developed to trigger retrieval of the trauma memory and not reconsolidation. As such, the design of these previous intervention studies raises several questions with respect to the necessary conditions for a reconsolidation intervention (i.e. PE).
Here we present four case descriptions to illustrate how reconsolidation interventions might be designed in patients with PTSD. We utilize a technique for reactivating the trauma memory that is akin to imaginal exposure [Van Minnen and Arntz, 2004], which also aims to reactivate the trauma memory and violate threat expectancies. Destabilization of fear memory has been hypothetically linked to the violation of threat expectations during retrieval, which, in turn, has been suggested to correlate with PE [Sevenster et al. 2013, 2014]. Upon reactivation however, our reconsolidation intervention directly targets the trauma memory, while the typical prolonged and repeated exposure to trauma memory in imaginal exposure aims to form a new extinction memory that competes with the original trauma memory. Hence, we discontinue reactivation before the threat expectancies decline because we know from fear conditioning studies that repeated or prolonged memory reactivation sessions may form a boundary condition for memory reconsolidation [Lee et al. 2006; Merlo et al. 2014; Sevenster et al. 2014; Suzuki et al. 2004].
General procedure
The general procedure of our reconsolidation intervention in PTSD patients currently involves an online screening, an intake session, one intervention session (or as many as needed to successfully reactivate the trauma memory), and a series of four assessment sessions. In the online screening, patients complete the Posttraumatic Diagnostic Scale (PDS) [Foa et al. 1997] to evaluate the nature and severity of their PTSD symptoms, and the McLean Screening Instrument for Borderline Personality Disorder (MSI-BPD) [Zanarini et al. 2003] to detect the possible presence of a borderline personality disorder (BPD). In addition, trauma exposure is catalogued and patients complete a list of possible contraindications for the use of propranolol.
In the intake session, the study procedures are explained and patients provide written informed consent. Next, trauma memory is explored. Specifically, using the contents of their intrusive symptoms as a guide, the patients’ most painful trauma memories are identified. In the intervention session, these ‘hot spots’ [Ehlers and Clark, 2000; Grey et al. 2001, 2002; Holmes et al. 2005] subsequently serve as the initial focus of the reactivation procedure (see below). After that, the presence of PTSD and possible other DSM-IV Axis I disorders is established using Dutch versions of the Clinician-Administered PTSD Scale (CAPS) [Blake et al. 1995] and the Structured Clinical Interview for DSM-IV Axis I disorders (SCID-I) [First et al. 2002]. In addition, the BPD section of the Structured Clinical Interview for DSM-IV Axis II Personality Disorders (SCID-II) [First et al. 1997] is administered to patients who scored 7 or more on the MSI-BPD in the online screening. Finally, a medical screening is conducted to more definitely rule out possible contraindications for the use of propranolol, including low blood pressure (<90/60 mmHg) or heart rate (<60 bpm), a range of adverse medical conditions (e.g. heart disease, asthma), and the use of other medications that may negatively interact with propranolol (e.g. antidepressants, anti-inflammatory drugs): a complete list of contraindications is available from the authors.
Patients who meet our eligibility criteria, are then included in the study. These criteria include (a) a DSM-IV diagnosis of PTSD, including the occurrence of intrusive experiences, (b) sufficient fluency in Dutch to complete the study procedures, (c) age 18 or older, (d) no concurrent psychological or pharmacological treatment of PTSD symptoms, (e) absence of serious other psychiatric problems that require immediate treatment, (f) absence of BPD, and (g) absence of contraindications for the use of propranolol. In the first intervention session, the baseline assessment is completed (T1, see below) and blood pressure and heart rate are recorded again to ensure the safe administration of propranolol later on. Next, the intervention procedures are briefly reiterated, and the contents and likelihood of patients’ expectations (predictions) regarding the negative consequences of reactivating their most painful trauma memories (e.g. ‘I’ll lose control and go crazy’, ‘I’ll get so angry that I’ll attack somebody’) are made explicit to promote their subsequent disconfirmation (PE) during the reactivation procedure, although it remains elusive whether the PE should be made explicit in order to trigger memory reconsolidation [Coccoz et al. 2013]. Also, patients’ habitual safety behaviors (e.g. distracting oneself) are identified and they are instructed to drop these behaviors during the reactivation procedure.
The actual reactivation procedure is based on regular imaginal exposure procedures [Van Minnen and Arntz, 2004], but is fundamentally different in two ways. First, reactivation is focused on the patients’ hotspots, rather than on their complete trauma narratives. Hence, reliving these hotspots may be embedded in a chronological account of the complete traumatic experience, but this is not imperative. Second, reactivation is terminated as soon as the patients’ distress reaches a maximum (as indicated by subjective units of distress [SUD] ratings). This is done to prevent extinction learning, which underlies the efficacy of prolonged imaginal reliving and has to be ruled out as an alternative explanation of our reactivation procedure. If reactivation of the trauma memory is judged to have been successful, as evidenced by high-end distress ratings, patients’ self-reports on leaving out safety behaviors, and therapist observations, patients’
The assessment sessions take place at the beginning of the first intervention session (T1), and 1 week (T2), 1 month (T3), and 4 months (T4) later. Assessments include the PDS [Foa et al. 1997] as the primary outcome, and the Beck Depression Inventory-II (BDI-II) [Beck et al. 1996], Beck Anxiety Inventory (BAI) [Beck and Steer, 1993], and Posttraumatic Cognitions Inventory (PTCI) [Foa et al. 1999] as secondary outcomes. Of note, T2 is the first outcome assessment and determines if an additional intervention session is needed. Specifically, if patients report no meaningful reduction of their PTSD symptoms at T2, it is explored if and why, in retrospect, reactivation of the trauma memory may have been unsuccessful. If there is reason to believe that reactivation could be optimized, for instance by focusing imaginal reliving on other hot spots or by dropping previously unknown safety behaviors, a second intervention session is offered after the ‘original’ T2 assessment and the first postintervention assessment (the ‘new’ T2) follows 1 week later. This is repeated to a maximum of three intervention sessions in which propranolol is administered. The successful treatments described below (cases 1 to 3) required only one or two intervention sessions, while in the unsuccessful treatment (case 4) a total of three intervention sessions took place over a period of 2 months.
Case descriptions
We here present a selection of case descriptions from an uncontrolled pilot study of the above procedure, which started in June 2013. We obtained baseline and posttest data of 12 patients with PTSD symptoms, from which 2 showed negligible improvement and were considered unsuccessful cases. The remaining 10 patients showed significant improvements. The current selection includes three successful treatments and one unsuccessful treatment, which roughly represent our experiences with this intervention for PTSD to date. Three patients had clinically elevated pretreatment PDS total scores exceeding the PDS cutoff of 18 [Ehring et al. 2007], while one patient (case 2) had a pretreatment PDS total score of 14. Index traumas included suicide of the patient’s mother (case 1), armed robbery (case 2), rape of the patient by her ex-boyfriend (case 3), and violent home invasion robbery (case 4).
All patients were assessed in our department’s outpatient research clinic (UvA PsyPoli) by experienced psychologists with a master’s degree in clinical psychology and postmaster training in CBT. Cases 1, 2 and 3 were treated by the first author (MK) who is a registered healthcare psychologist and an experienced cognitive behavioral therapist. Case 4 was initially treated by a junior clinician, and in a second phase by MK. Due to the early phase of this study, there were a number of irregularities in the data collection. Specifically, the secondary measures (BDI, BAI, and PTCI) were not administered at T2 in case 1 and at T4 in case 4. In case 2, T3 took place 3 months after T1, and it was therefore decided to omit T4. Figures 1 to 4 show the patients’ total and subscale scores on the PDS (primary outcome). Their scores on the BDI, BAI, and PTCI (secondary outcomes) are summarized in Table 1.

PDS total and subscale scores of case 1.
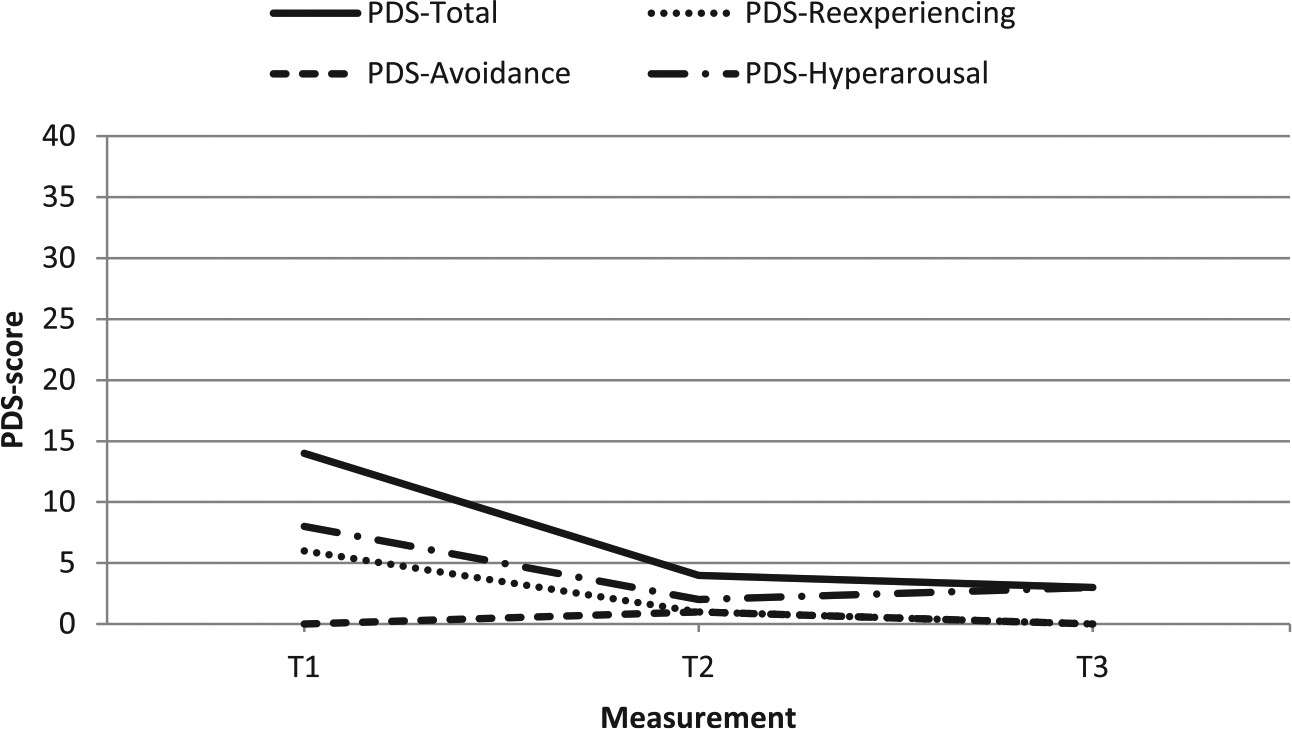
PDS total and subscale scores of case 2.
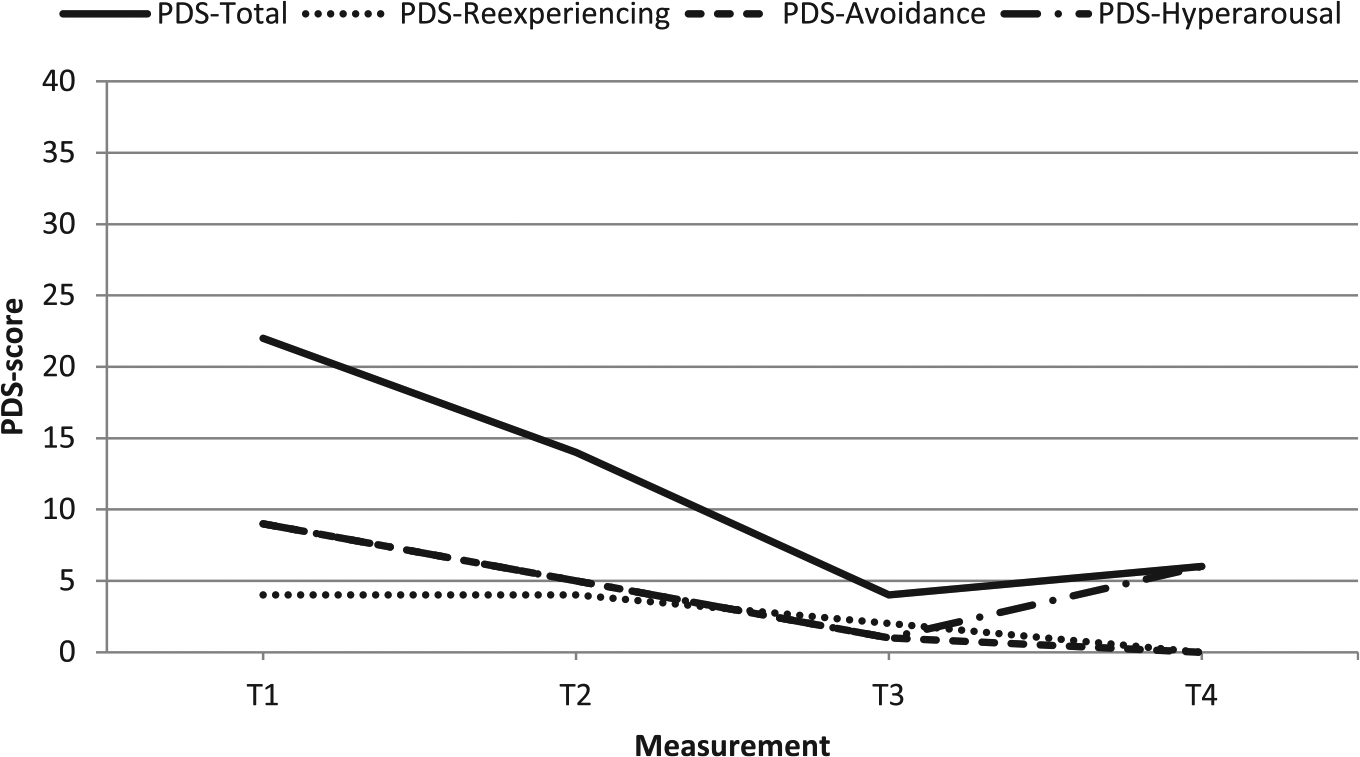
PDS total and subscale scores of case 3.
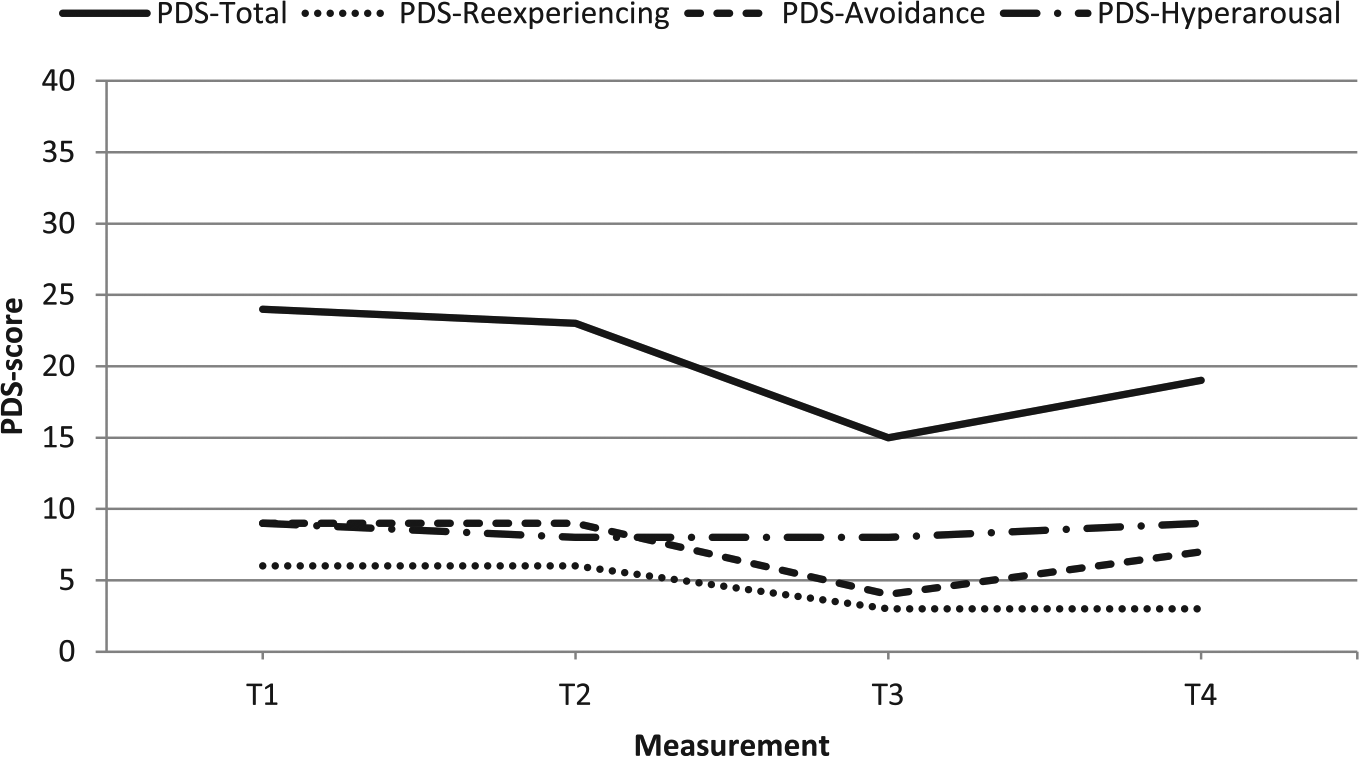
PDS total and subscale scores of case 4.
Patients’ total scores on the BDI, BAI, and PTCI at T1 to T4.
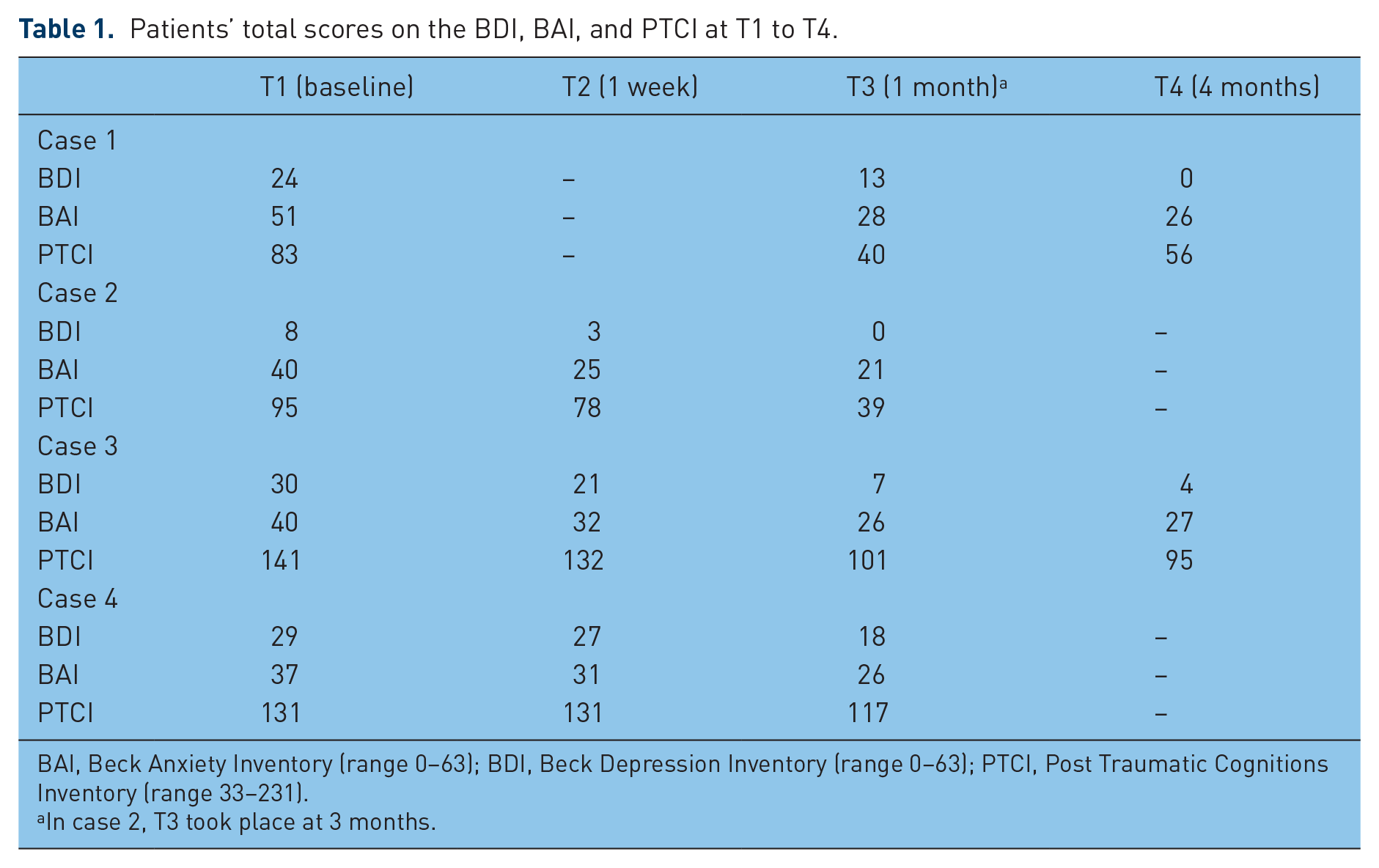
BAI, Beck Anxiety Inventory (range 0−63); BDI, Beck Depression Inventory (range 0−63); PTCI, Post Traumatic Cognitions Inventory (range 33−231).
In case 2, T3 took place at 3 months.
Case 1
Case 1 concerns a 42-year-old woman who self-referred to our research clinic in response to a newspaper advertisement of the present study. She suffered from nightmares and other PTSD symptoms after her mother committed suicide 3 years ago. The suicide occurred in her absence in Germany, and her father brought the news to her over the phone. Her decision to apply for treatment had led to an increase of symptoms in the past month.
At intake, the patient met all diagnostic criteria of PTSD. In addition, she reported to be moderately hindered by a fear of heights. No other disorders were diagnosed, including current or past depressive episodes. She had not received psychological treatment before.
Throughout the intervention session, the patient was continuously in tears. According to her, the processing of the traumatic experience was hindered by her expectation that once she started thinking about it, ‘it would all go wrong’ and she would be overwhelmed by feelings of sadness and grief and never recover again (prediction). Although she acknowledged that this thought was irrational, it prevented her from fully experiencing her feelings of loss, sadness and grief. In daily life, she employed various strategies to avoid these feelings, including distracting herself by thinking of something else or by eating.
Reactivation focused on two intrusive hotspots (i.e. the patient’s memory of her father calling her on the phone to inform her about her mother’s death, and the image of her mother walking up to her to embrace her and then walking away). These two intrusions were reactivated by asking her to relive them, while focusing on her sensory impressions and on the meaning of these experiences to the patient. She was also instructed to drop all her avoidance strategies during reactivation. When her distress ratings reached their peak at 90, she burst out crying and fully experienced the previously avoided emotions. Although overwhelmed by them, this unexpectedly felt as a relief instead of a never-ending sadness (PE). This was followed by the intake of one pill of 40 mg propranolol HCl, as the therapist decided that the reactivation of the fear memory was successful.
As can be seen in Figure 1, 1 week after treatment (T2) the patient’s PDS total score had dropped well below the clinical cutoff of 18, which reflected a reduction of her reexperiencing and avoidance subscale scores. She reported having dropped various avoidance behaviors, and brought her mother’s suicide note and a picture of her mother to the assessment session. In the past week, she had read the note and had looked at the picture for the first time, and this had not led to the emotional breakdown that she had feared so much. Further improvements were observed during the following months, until she reported virtually no PTSD symptoms on the PDS, and not a single PTSD symptom was endorsed on the CAPS at T4. As shown in Table 1, her scores on the secondary outcome measures paralleled the decreasing PDS score until T3, after which the BDI score further decreased to zero at T4, the BAI score remained stable, and the PTCI score slightly increased again.
Interestingly, at T3 the patient indicated that the panic and anxiety that previously surrounded her mother’s suicide was gone, and that she ‘almost missed these feelings, since they had disappeared so suddenly’. Instead, she now experienced sadness and other feelings of mourning, but interpreted these as normal in view of what had happened and, indeed, a sign of progress compared to her previous, predominantly anxious and avoidant state. In the past month, she had discussed their mother’s suicide with her brother and had visited the room in which her mother committed suicide, which according to her would be unthinkable before the treatment. The patient seemed generally content with the treatment, and expressed the wish to receive the same treatment for her fear of heights.
Case 2
Case 2 concerns a 53-year old woman who, with her partner, had been the victim of an armed robbery when travelling in South-Africa 2 years ago. One night, a man entered their private cabin on the hotel grounds and forced them to hand over their valuables. All the time, the patient was held at gunpoint, until the perpetrator left and locked them in the cabin.
At intake, the patient met the reexperiencing and hyperarousal diagnostic criteria of PTSD. Reexperiencing symptoms included intrusive images of the robbery, especially at night, and physiological reactivity in response to trauma-related cues. She described herself as being hyper-alert and suffering from disrupted sleep: she awoke at least once every night due to nightmares or sounds that reminded her of the robbery. Her main avoidance strategy was to suppress her bodily emotional responding to intrusive memories. She could not describe what she actually feared if she had to give up her safety strategies. Exerting control was a habit that she acquired during her childhood; she was simply not used to dwell on intense negative emotions. Hence, her threat expectancies could not be made explicit.
She was one avoidance symptom short of meeting the avoidance diagnostic criterion, and therefore did not receive a formal PTSD diagnosis. As can be seen in Figure 2, her PTSD symptoms were relatively mild (i.e. her pretreatment PDS total score did not exceed the PDS cutoff of 18 and she reported no avoidance symptoms on the PDS avoidance subscale). She admitted to drinking two or three glasses of wine per day, and larger quantities at the weekend. There were no present or past symptoms of depression or other psychiatric diagnoses, and she had not received psychological treatment before. An invitation of a friend to return to South Africa, where he was building a holiday house for them, actually prompted her to apply for treatment.
The reactivation focused on a hotspot memory of the robbery in which she awoke in their hotel cabin in Johannesburg. A burglar wearing a hat, plastic shoes, and dirty and extremely baggy trousers, stood next to her with a gun against her head. She turned her back to him, convinced that this was where her life ended. Although her partner was lying next to her, she could not talk and was overwhelmed by feelings of mental defeat and loneliness. During the reactivation, she was very distressed, cried and felt the intense fear and disgust that she had experienced during the burglary, with distress peak scores of 90. Because the memory reactivation triggered intense emotional feelings that the client had never experienced in daily life when reminded of the traumatic event, the therapist decided that the reactivation was successful and gave her one pill of 40 mg propranolol HCl.
At T2, the patient’s PDS total score had dropped to 4 and her scores on the secondary measures had considerably declined. She reported that she felt very different and quiet. She regained her sound sleep, which was no longer interrupted by nightmares, but she also admitted that she had difficulty to believe that her fear was really gone. At T3, her PDS total score remained low and her scores on the secondary measures showed further decreases. She reported feeling really well. She had travelled to the same city in South-Africa where the robbery had taken place without experiencing any PTSD symptoms or other difficulties. She stated that ‘it was really gone’ and that she felt ‘a lot lighter’.
Case 3
Case 3 concerns a 25-year old female history student who self-referred to the study in response to a posting in the history department. At intake, the patient met all diagnostic criteria of PTSD, as a result of being raped by her then boyfriend 4 years ago. There were no concurrent depressive or other disorders, but she reported a past depressive episode during puberty. Also, she reported three past visual hallucinatory experiences, which she now attributed to the fact that she was going through a particularly stressful period at the time. After further examination, it was decided that these past psychotic symptoms constituted no contraindication for our intervention [Van den Berg et al. 2015; Mueser et al. 2015], but that their possible recurrence should be carefully monitored. Also, the patient reported several BPD symptoms on the BPD section of the SCID-II (including affective instability, feelings of emptiness, and transient, stress-related paranoid ideation and feelings of distrust), but not enough to warrant a BPD diagnosis.
Her treatment history included nine sessions of CBT (3 years before) and nine sessions of Eye-Movement Desensitization and Reprocessing (EMDR) therapy (2 years before), which seemed to have aggravated rather than improved her complaints however and to have ‘destroyed her faith in mental health care’. As a result, she expressed a concern that the present treatment would also worsen her symptoms.
This treatment included two intervention sessions. In the first intervention session, reactivation focused on the rape scene, in particular on the intrusive image of the red door of her room standing open, and the intrusive thought that none of her dorm mates came to her rescue. The patient expected to be overwhelmed by emotions when reactivating these intrusive hotspots. During the reactivation, she reported thinking that she probably deserved the rape and the bad treatment by her ex-boyfriend in general, and felt powerless and suspicious. Her distress ratings reached 70 but because she reported feeling powerless and depressed during the reactivation, it was concluded that her expectations of being overwhelmed by emotions could not have been falsified (no PE), and propranolol was not administered. Instead, a second intervention session was scheduled 1 week later.
At the beginning of the second intervention session, it became clear that feelings of powerlessness and loss of autonomy were the core problem that had hindered the patient’s processing of her traumatic experience. It was therefore attempted to bring about PE by including an imagery rescripting procedure into the reactivation [Arntz, 2012] to induce the feeling of being in control (i.e. contrary to what she had actually experienced). A violation of threat expectancies is supposed to be a necessary condition for reconsolidation, meaning that the magnitude of the outcome or the outcome itself in not being fully predicted (i.e. PE) [Pedreira et al. 2004; Forcato et al. 2009; Lee, 2009; Sevenster et al. 2012, 2013, 2014]. In other words, a mismatch between what is expected (i.e. mental defeat) and what actually occurs triggers memory reconsolidation.
Specifically, a past situation was invoked in which the patient and her boyfriend went to the beach on his motorcycle. Her intention was to have a romantic time, while he was out for sex. This first made her feel powerless, out of control, and very uncomfortable. Then, rescripting started and she was instructed to imagine an incompatible response. Although her distress ratings were similar to the previous session (i.e. 70), this time she pictured herself walking away from the scene. This opposite response gave her a feeling of being in control, safe and relieved (PE), and she subsequently burst out crying. Accordingly, this was followed by the intake of one pill of 40 mg propranolol HCl.
At T2, the patient’s PDS total score had dropped well below the clinical cutoff of 18, reflecting decreased avoidance and hyperarousal subscale scores. Her reexperiencing subscale score did not decrease, but was already low at T1. All three PDS subscale scores further decreased well into the follow up (T3), after which the hyperarousal increased somewhat again (T4).
At T4, the diagnostic criteria of PTSD were no longer met. The patient reported an absence of intrusive symptoms. Instead, she had been feeling well and ‘going with the flow’, and had been able to let go of the memories of her ex-boyfriend. She did report sleeping problems and increased irritability, but these symptoms appeared to be unrelated to her traumatic experience. The patient indeed had been feeling touchy in the past 2 weeks, but thought this resulted from ‘having stood up for herself better than before’. She reported feeling cheerful and enjoying her activities most of the time, and having achieved better study results. Her scores on the secondary measures had gradually decreased until T3, and then largely remained stable from T3 to T4.
Case 4
Case 4 concerns a 20-year old female student who self-referred to our research clinic in response to a newspaper advertisement of the present study. Some 5 years ago, she and her parents became victims of a violent home invasion robbery. Two men entered their home at night, tied up the patient and her parents, and threatened to kill them. A number of physical struggles resulted in both parents receiving gunshots and her father having a fractured skull, but eventually all survived. One perpetrator was soon arrested and sentenced to prison, while the other was still at large at the time of the study.
At intake, the patient met all diagnostic criteria of PTSD. She reported several depressive symptoms, but not enough to warrant a depressive disorder diagnosis. She also recalled three possible depressive episodes in the past, but it was unclear if these were not better conceived of as PTSD symptoms. In addition, the patient reported a number of BPD symptoms (including efforts to avoid abandonment, impulsivity, and chronic feelings of emptiness), but not enough to warrant a BPD diagnosis. Similarly, several symptoms of generalized anxiety were present, but a generalized anxiety diagnosis was postponed. Finally, she met criteria for alcohol abuse and dependency and occasionally used various types of drugs, including cocaine and XTC, but her pattern of using these substances is not unusual for her age group. The patient had received EMDR therapy 5 years ago and a second unspecified treatment 3 years ago, without any substantial effects.
The first intervention session was unsuccessful in that reliving the traumatic event did not trigger sufficiently intense feelings of distress, fear, or sadness. She had two hotspot memories, although the whole experience was extremely threatening and overwhelming. The first hotspot memory that she described was when she awoke in the middle of the night from loud and odd noises. She entered her parents’ bedroom where her father lay down on the ground, moaning in pain and enrolled in a blood-soaked sheet, while her mother was struggling with one of the burglars. Both burglars wore black balaclavas, gloves and huge weapons (AK-47s). One of the burglars held his weapon against her head, while she could see her father lying on the ground. The patient described the scene as ‘a bad dream’. Her other hotspot memory was that she and her mother had to climb up to the attic where they had to lie down and were tied, unable to see each other because it was very dark. They were threatened with death as one of the burglars shot at her mother but missed, and then held his weapon to the patient’s head telling her that she should die. She remembered that ‘all my friends and family passed my mind’s eye because I was convinced that this was my very last moment – this was it’.
Although the patient’s SUD scores increased to 70−80, her distress or fear was not observable for the therapist. Given the high SUD scores, he nevertheless decided to administer 40 mg of propranolol HCl. At 1 week after the first intervention session (T2), the patient’s PDS scores were unchanged. The intervention was therefore repeated, but because the reactivation of her trauma memory was again unsuccessful (i.e. not resulting in observable distress, as in the previous session), no propranolol was administered this time. At 1.5 months later (T3), her PDS total score had dropped to 15, and in an attempt to further improve her symptoms, a third intervention session was held by a different therapist (MK). This time the reactivation of her trauma memory triggered SUD scores of 70. Because the patient again expressed little emotion when reliving the trauma, it remained unclear for the therapist if the fear memory reactivation had been successful. Given the considerably elevated SUD scores however, one pill of 40 mg propranolol HCl was administered. Nevertheless the treatment appeared unsuccessful: at T4, the patient still reported fears in her daily life and her PDS total score had increased to (just) above the clinical cutoff of 18. Her secondary outcome scores showed a roughly similar pattern, with little or no changes from T1 to T2, and minor drops from T2 to T3.
We have no definitive explanation of why our intervention failed to improve these patient’s symptoms. Her baseline PDS total score of 24 was within the range of the scores of the other patients with successful treatments (14−34), which suggests that the lack of success cannot be attributed to extremely high or low pretreatment symptom severity. One explanation is that reactivation of the patient’s trauma memory was incomplete or otherwise unsuccessful. Certain personality characteristics or the patient’s elevated substance use are two factors that may have prevented the full reactivation of her trauma memory. Of note, both therapists noted that the patient, despite elevated self-reported distress ratings and considerable efforts of both patient and therapists, displayed little emotion when reliving the trauma and appeared to try to keep control by rationalizing her experiences. She also suggested that the treatment setting was not sufficiently threatening to mimic the fears and panic that she was experiencing in her daily life, because the daylight and the presence of a therapist might have served as safety signals. We suggested the possibility of another memory reactivation in her home where the robbery took place, but the patient was not very keen on trying this. Her greatest fear was that her trauma memories would trigger panic, and that she might lose control and eventually go crazy. She also confided to the therapist that she had actually never experienced sadness, grief or other negative emotions when talking about the traumatic event, either in a therapeutic or in a private context.
Discussion
Although we cannot rule out that nonspecific treatment mechanisms (e.g. therapist attention and expectations) underlie the uncontrolled observations described in this article, the magnitude, speed, and robustness of the observed improvements are remarkable at the very least. All three successfully treated patients continued to improve well beyond the actual intervention. This is especially remarkable in view of the fact that these effects were achieved after only one or two intervention sessions. It bears mentioning that this is less than even the most efficient empirically supported PTSD treatments to date, such as trauma-focused CBT and EMDR [Bisson et al. 2007; Bradley et al. 2005; Seidler and Wagner, 2006], or Writing Therapy [Van Emmerik et al. 2013].
We also presented a patient (case 4) for whom the reconsolidation intervention was not successful. Even though it looks very promising, the success of the intervention depends on whether the memory reactivation actually triggers memory reconsolidation. We observed in our fear-conditioning studies that mere retrieval of the fear memory is not sufficient to induce its labilization and subsequent reconsolidation [Sevenster et al. 2012, 2013, 2014]. The clinical implication is that even if patients experience high levels of distress, this is not necessarily an indication that their fear memory is destabilized. In other words, fear expression during memory reactivation is not informative on whether the memory trace enters a labile phase [Ben Mamou et al. 2006]. Notwithstanding our new insights on PE as a prerequisite to trigger memory reconsolidation, no objective criterion is yet available to determine the optimal degree of PE in clinical practice. Of note, the patient in case 4 presented with a relatively complex clinical picture. Another explanation for the lack of effect for case 4 is therefore that the reconsolidation intervention is exclusively designed to target unduly intense fears, while PTSD is a complex disorder with a broad range of other negative emotions, which may have dominated this patient’s clinical picture. Also, our clinical impression was that certain temperamental or personality characteristics (e.g. experiential avoidance) may have further hindered her successful treatment, although we have no formal diagnostic data on this.
CBT for anxiety and related disorders is still the treatment of choice in clinical practice [Butler et al. 2006; Craske et al. 2014], but there are many patients who do not profit from CBT or who experience a relapse even after initially successful treatment [Hofmann and Smits, 2008; Loerinc et al. 2015]. The relatively good short-term outcomes of CBT for anxiety disorders (i.e. 6−12 months following the start of therapy) are no guarantee of good long-term outcomes. The long-term course of anxiety disorders, regardless of diagnostic type and active treatment, strongly fluctuates with a tendency towards chronicity [Durham et al. 2012]. Only about 40% of patients achieve sustained recovery in the sense of no longer meeting diagnostic criteria for an anxiety disorder and seeking little or no treatment for anxiety over the follow-up period, whereas the majority of patients (60%) show relapse [Durham et al. 2012]. Although the memory reactivation seems procedurally similar to imaginal exposure, including a violation of threat expectation [Craske et al. 2014], it should be much shorter than traditional exposure techniques in order to prevent the formation of a new inhibitory memory [Bos et al. 2012; Lee et al. 2006]. If the exposure is too long, the amnesic agent (i.e. propranolol) may interfere with the formation of the extinction memory instead of targeting the fear memory itself. Apparently, the window of opportunity to target emotional memory with amnesic agents is small: it is preceded and followed by phases that leave the original memory unaffected [Merlo et al. 2014; Sevenster et al. 2013, 2014].
The litmus test for the reconsolidation intervention for PTSD and other complex disorders though is whether the fear-reducing effects will persist in the long run, in larger samples, and in controlled trials. Of note, the procedures described here are being continuously developed as our pilot program progresses towards this aim. Until then, we warn against moving too fast to expensive and time-consuming randomized controlled trials without further pilot testing of these deceptively easy procedures, and against prematurely discarding CBT-like interventions as a well-established treatment of choice in PTSD.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest
The authors declare that there is no conflict of interest.
