Abstract
Strong evidence supports the existence of a discontinuation syndrome following the withdrawal of antidepressant medication, particularly second-generation antidepressants. The syndrome is a common phenomenon and guidance as to best avoid the symptoms is essential for both practitioners and patients. The current study reviewed the available literature on the best methods of discontinuation for antidepressants in order to avoid or prevent the occurrence of any unpleasant side effects associated with antidepressant withdrawal. Accordingly, an electronic search of the PubMed/MedLine database and Google Scholar was conducted to find relevant literature published within the last 10 years. From this, 18 related articles were identified; five clinical studies, one case series, one consensus panel’s recommendations and 11 literature reviews. Of the articles reviewed there is a general consensus as to tapering the drug slowly over a period of weeks or months. Also, in those patients who experience severe symptoms the drug should be reinstated and discontinued more gradually. The discontinuation syndrome does not occur as frequently or severely with longer-acting agents such as fluoxetine and therefore it is recommended that switching to this drug prior to withdrawal may be advisable. The articles reviewed also emphasize the need for patient education and reassurance throughout the discontinuation process. One in particular adds that cognitive behavioural therapy may be a useful tool in easing the patients’ distress. However, this review highlights the lack of controlled data to support the available guidelines. Furthermore, the guidance which is available is somewhat conflicting. Research approaches should address this issue as well as develop appropriate methods of withdrawal for specific drugs.
Introduction
Depressive disorders are currently estimated to affect 350 million people worldwide with approximately 1 in 20 people reporting an episode of depression each year [Marcus et al. 2012]. Antidepressant medication is a primary treatment option for depression as well as for many anxiety disorders and, according to Spence and colleagues, between 1998 and 2012, there was a 165% increase recorded in the prescribing of antidepressant drugs in England [Spence et al. 2014].
Antidepressants have been available for over 50 years with iproniazid being the first drug to be used in the clinical treatment of depression following the discovery of its psychoactive properties during the search for potential pharmacological treatments for tuberculosis in 1952 [Lieberman, 2003]. Iproniazid and related compounds reduced the breakdown of the monoamines noradrenaline, serotonin and dopamine by inhibiting the enzyme monoamine oxidase: hence the term, monoamine oxidase inhibitors (MAOIs) [Lieberman, 2003]. Around the same time, molecular modifications to the phenothiazines resulted in the first tricyclic antidepressant (TCA), imipramine, which blocked the reuptake of noradrenaline and serotonin in the synapse extending their bioavailability [Lieberman, 2003]. The MAOIs and TCAs are now regarded as the first-generation of antidepressant medication and are no longer the drugs of choice in the treatment of depression due to safety and toxicity concerns [Gartlehner et al. 2011]. Over the last three decades, second-generation antidepressants, including selective serotonin reuptake inhibitors (SSRIs) and more recently selective serotonin and noradrenaline reuptake inhibitors (SNRIs), have become the frontline pharmacological treatment for depression [Gartlehner et al. 2011]. These drugs have comparable efficacy, but lower toxicity in overdose and less troublesome side effects than TCAs and MAOIs [Bitter et al. 2011].
Despite having a superior side-effect profile, second-generation antidepressants have been reported to be associated with a discontinuation syndrome upon withdrawal [Bitter et al. 2011]. In a comparison between the withdrawal reactions of patients treated with benzodiazepines and antidepressant medication for panic disorder, Offidani and colleagues found both classes of drugs to be associated with the same type of problem upon discontinuation [Offidani et al. 2013]. They also suggest that most of the newer antidepressant medications used for anxiety disorders have ‘similar, if not more pronounced’ dependence problems than benzodiazepines, despite the latter being used less and less often in the treatment of anxiety for this precise safety concern. In 1997, Zajecka and colleagues defined the SSRI discontinuation syndrome as a cluster of symptoms following the discontinuation of a SSRI, not due to other factors [Zajecka et al. 1997]. These symptoms typically include; dizziness, disturbance of balance, headache, nausea, insomnia and vivid dreams [Renoir, 2013]. Others can include paraesthesia, ‘electric-shock’-like sensations, depersonalization and irritability, although there have been some reported cases of discontinuation leading to visual and auditory hallucinations [Yasui-Furugori and Kaneko, 2011] or even resembling a stroke [Reeves et al. 2003]. Discontinuation symptoms can last between 1 and 2 weeks, are usually mild, and rapidly disappear upon readministration of the drug [Bitter et al. 2011]. In 2000, Black and colleagues identified 53 different symptoms within the condition (of which dizziness was the most common) and proposed a set of diagnostic criteria for the SSRI discontinuation syndrome that requires two or more of the described symptoms developing within a week of drug withdrawal [Black et al. 2000]. Haddad and Anderson provide a more detailed description of the primary SSRI discontinuation syndrome, dividing symptoms into six subgroups (sensory symptoms, disequilibrium, general somatic symptoms, affective symptoms, gastrointestinal symptoms and sleep disturbance) and differentiating from rarer symptoms such as mania and extra-pyramidal syndromes [Haddad and Anderson, 2007]. In 2013, Renoir stated that the existence of a discontinuation syndrome had been confirmed by a number of well-controlled studies [Renoir, 2013]. The syndrome is believed to be dependent on the elimination half-life of the administered drug and the patient’s rate of metabolism [Bitter et al. 2011], occurring most frequently following the withdrawal of agents with shorter half-lives [Sheldon, 2006].
A discontinuation syndrome can present a number of challenges not only due to the unpleasant side effects experienced by the patient but in addition the emergence of such symptoms may be mistaken for a relapse of the underlying condition, a physical disorder or possibly side effects of a new antidepressant if a switch was made during treatment [Haddad and Anderson, 2007].
A particular concern is expectant mothers. Given the prevalence of depression in reproductive-age women, the prevalence of antidepressant use in this population, and the frequency of unplanned pregnancies, many studies on discontinuation have involved this group [Cohen et al. 2006]. Clinically this presents a problem as women with histories of even highly recurrent depressive illness are likely to discontinue antidepressant use during attempts to conceive or after conception. Cohen and colleagues found that 68% of the women who discontinued antidepressant treatment proximate to conception relapsed during pregnancy; of these, approximately 50% relapsed within the first trimester and 90% by the end of the second trimester. Also 60% of the women who discontinued antidepressant treatment in this study at the beginning of pregnancy reintroduced antidepressant therapy during the pregnancy.
Another concern is the neonate, as a discontinuation syndrome has also been detected in a small percentage of infants exposed to antidepressants
The elderly are another group which require specific guidance about antidepressant treatment and discontinuation as depression is the most common mental health disorder affecting this age group and yet most research is conducted on younger populations [Wiese, 2011]. Without geriatric-specific guidance it may be difficult to discern the extent of problems with discontinuation of some antidepressant medication.
Understanding the particular pharmacology of different antidepressant drugs can help explain the symptoms which arise upon discontinuation [Howland, 2010]. Baldessarini and colleagues hypothesized that illness following discontinuation of psychotropic drugs represents a response to long-term physiological adaptation of cerebral neural systems to the pharmacodynamic actions of the agents involved. The authors, however, distinguish the complex of physiological, autonomic and sensory responses often observed in the first days after discontinuing antidepressants, particularly short-acting serotonergic antidepressants. Instead they emphasize that such reactions arise rapidly, are transient and may reflect manifestations of drug withdrawal effects [Baldessarini et al. 2010]. They also add that illness latency after discontinuing antidepressants was not related to duration of treatment or dose [Baldessarini et al. 2010]. Other studies dispute this, however, with Blier and Tremblay stating that the rate at which SSRI treatment is terminated and the duration of treatment appear to be key factors in predicting discontinuation symptoms [Blier and Tremblay, 2006]. They suggest that SSRI discontinuation symptoms may arise from the rapid decrease in serotonin (5-HT) availability when treatment ends abruptly but also note that the discontinuation syndrome may not be mediated exclusively through 5-HT receptors; they propose that the noradrenaline and the cholinergic systems also play a key role [Blier and Tremblay, 2006].
Some reports claim that some novel antidepressant drugs, such as agomelatine which possesses agonist properties at the melatonin MT1 and MT2 receptors and which acts as an antagonist at the 5-HT3 receptor, do not exhibit a discontinuation syndrome upon withdrawal despite having a relatively short half-life [Green, 2011]. Understanding the pharmacology of agents such as these may provide insight, although further studies are required [Green, 2011].
Although there remains some debate as to the biological mechanisms underlying the antidepressant discontinuation syndrome, there is substantial agreement that it can occur following the withdrawal of any antidepressant and is a common phenomenon amongst a wide range of antidepressants including TCAs, MAOIs, and SSRIs, particularly with more-potent and shorter-acting SSRIs such as paroxetine and SNRIs such as venlafaxine [Tartakovsky, 2011]. Studies have shown that this withdrawal reaction is a genuine syndrome experienced at least by some patients and therefore does present a clinical concern. Due to the soaring prescription rates of drugs such as these and the prevalence of depression globally, guidance on the treatment of this disorder is necessary, especially for discontinuation, as adverse effects appear to be a common phenomenon experienced during drug withdrawal. According to Ogle and Akkerman, at present the literature available as well as the package insert guidance is vague and somewhat generic [Ogle and Akkerman, 2013]. As a result, the current study reviews the literature on:.
methods of discontinuation to examine the guidance for both healthcare professionals and patients; and
the evidence base upon which these guidelines rest.
The study will focus on the second-generation antidepressants, which are of particular concern due to the number and severity of reported cases of a discontinuation syndrome.
Methods
For this review an electronic search of the PubMed/MedLine database and Google Scholar was completed using the search terms: antidepressant, discontinuation, syndrome, withdrawal, methods, guidance, controlled, trial, clinical study, SSRI/SNRI and tapering. Articles were limited to those in English, those which were based upon human studies or reports and those which have been published within the last 10 years. The rationale for restricting the search to within the last decade was to bring the readers up to date on the most current research. The electronic databases were last searched in May 2015. In addition to this, manual searches of reference lists in relevant reviews were also completed to supplement the electronic search. Of the 26 articles identified as potentially providing guidance on specific methods of antidepressant discontinuation from the electronic search, eight were excluded upon review because of insufficient relevance.
Results
The electronic search identified 18 peer-reviewed publications containing guidelines for antidepressant discontinuation. Of the 18 research articles, five were clinical studies (two randomized controlled trials, two retrospective analyses and one observational cohort study) [Tint et al. 2008; Montgomery et al. 2004; Baldwin et al. 2007; Himei and Okamura, 2006; van Geffen et al. 2005], one was a single case series, one was a consensus panel’s recommendations and 11 were comprehensive literature reviews (see Table 1).
Peer-reviewed publications identified through database search.
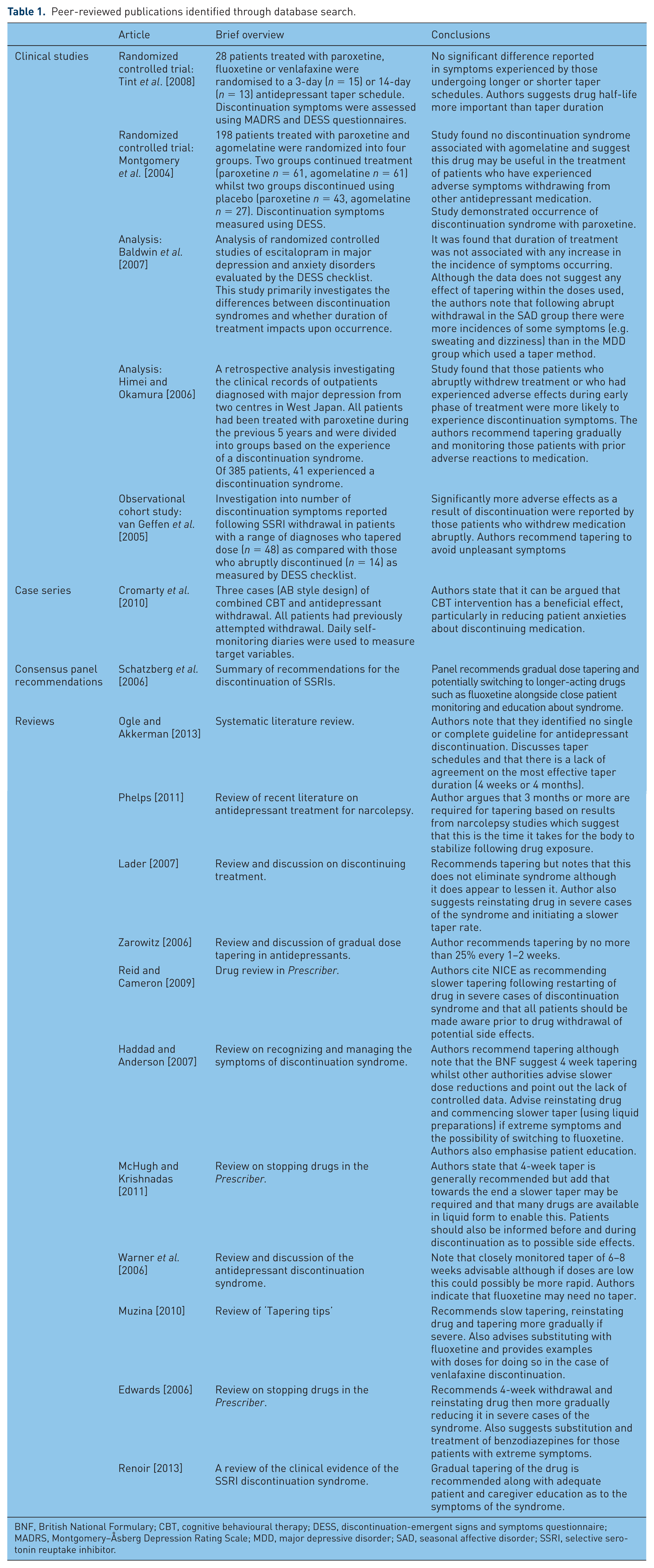
BNF, British National Formulary; CBT, cognitive behavioural therapy; DESS, discontinuation-emergent signs and symptoms questionnaire; MADRS, Montgomery–Åsberg Depression Rating Scale; MDD, major depressive disorder; SAD, seasonal affective disorder; SSRI, selective serotonin reuptake inhibitor.
Overview
A review of this literature shows a general consensus towards tapering the dose of the drug over time, although the taper rates recommended vary somewhat between the articles reviewed. For instance, two of the articles suggest that reducing the dosage by 25% per week is sufficient to avoid discontinuation symptoms [McHugh and Krishnadas, 2011; Edwards, 2006] whilst another more cautiously recommends tapering over 6-8 weeks [Warner et al. 2006]. Phelps nevertheless proposes even longer rates of gradual dose reduction, adducing evidence from narcolepsy studies which show 3 months as being necessary for cataplexy rates to return to baseline [Phelps, 2011]. The author argues that this period is required for the body to ‘normalize’ during discontinuation and recommend 4 months in order to reduce relapse rates and symptoms associated with drug withdrawal [Phelps, 2011]. Many of the guidance articles reviewed state explicitly that there is conflicting opinion as to the optimum duration of gradual dose reduction [Haddad and Anderson, 2007; Ogle and Akkerman, 2013] and the evidence base for tapering antidepressants is weak. Of the five clinical studies reviewed, only two [Himei and Okamura, 2006; van Geffen et al. 2005] recommend tapering the drug over time as a result of findings that abruptly withdrawing medication significantly increases the likelihood of a discontinuation syndrome. Only one randomized control trial [Tint et al. 2008] investigates the effects of tapering schedules, however, with the authors reporting no significant difference between a 3-day and 14-day taper rate. Nevertheless, the compared taper schedules are relatively short in this study and sample size is small.
Tapering schedules
Most articles reviewed agree that tapering is unnecessary for patients who have been taking an antidepressant for 4 weeks or less as this is insufficient time to develop a withdrawal reaction [Ogle and Akkerman, 2013; Haddad and Anderson, 2007; Edwards, 2006]. They also agree that if discontinuation symptoms are severe, the drug should be reintroduced and a slower taper initiated [Ogle and Akkerman, 2013; Lader, 2007; Zarowitz, 2006; Schatzberg et al. 2006; Reid and Cameron, 2009; Warner et al. 2006; Edwards, 2006]. Baldwin and colleagues argue that duration of treatment has no association with incidence of discontinuation syndrome [Baldwin et al. 2007] and two of the reviewed publications suggest that the half-life of the drug plays a more pivotal role than the taper rate [Tint et al. 2008; Montgomery et al. 2004]. They also suggest that for antidepressants with shorter half-lives, such as venlafaxine and paroxetine, a more gradual dose reduction would be advisable as a result of the associated severe discontinuation syndrome [Tint
Alternative management
Only three of the studies reviewed provide alternative advice for discontinuing antidepressants when symptoms are severe as opposed to implementing an even more gradual rate of dose reduction. For instance, Renoir suggests that patients experiencing particularly adverse side effects may benefit from a short course of symptomatic treatment with a benzodiazepine [Renoir, 2013]. Haddad and Anderson likewise advocate the use of benzodiazepines for those suffering with insomnia, whilst adding that antimuscarinic agents may be useful in ameliorating the gastrointestinal symptoms associated with TCA withdrawal, and antipsychotic treatment can be given to those patients experiencing withdrawal mania [Haddad and Anderson, 2007].
Cromarty and colleagues detail the effects of cognitive behavioural therapy (CBT) throughout the discontinuation process from experience of a single case series and found that it may be of benefit. CBT could be potentially useful in shifting the patients’ self-beliefs that discontinuation symptoms are a sign they cannot cope without the medication to a more positive understanding that it is a common and temporary stage associated with drug withdrawal [Cromarty et al. 2010]. This study has limitations however, and more studies are necessary as to the potential benefits of CBT as an adjunctive therapy with gradual dose tapering during discontinuation.
Need for education
The majority of the reviewed literature concur that the education of both clinician and patient is key to the process of drug discontinuation [Ogle and Akkerman, 2013; van Geffen et al. 2005; Schatzberg et al. 2006; Haddad and Anderson, 2007; Reid and Cameron, 2009; McHugh and Krishnadas, 2011; Warner et al. 2006; Muzina, 2010]. Haddad and Anderson, in particular, highlight the need for information regarding discontinuation symptoms to be discussed with the patient before they even begin treatment [Haddad and Anderson, 2007]. Patient reassurance that side effects will be short-lived and self-limiting [Zarowitz, 2006] and do not indicate dependence on the drug [Ogle and Akkerman, 2013] is also of vital importance. van Geffen and colleagues stress this as patients who had reported a lack of knowledge of discontinuation symptoms experienced greater adverse effects during withdrawal [van Geffen et al. 2005]. Three of the articles [Ogle and Akkerman, 2013; Tint
Panel recommendations
Of the articles reviewed, the consensus panel recommendations [Schatzberg et al. 2006] were the most comprehensive in providing guidance for antidepressant discontinuation. They review management strategies formulated by a previous panel which met in 1997 [Schatzberg et al. 1997]. In this panel, four specific guidelines were proposed for SSRI discontinuation: reassuring the patient; reintroducing the drug and tapering at a slower rate for severe cases; all drugs (with the possible exception of fluoxetine) should be slowly tapered to reduce the incidence of a discontinuation syndrome; and initially prescribing or switching to drugs with a longer half-life (such as fluoxetine). The 2006 panel mostly reiterated this advice but added some clinically significant points such as close monitoring of patient during and after discontinuation with clinicians available for reassurance or questions during this period. They also add the importance patient education of the syndrome as well as the education of any caregivers involved.
Another set of guidelines covers all of the treatment of depression [Cleare et al. 2015]. It is the official document of the British Association of Psychopharmacology (BAP). In the section on stopping antidepressant treatment (pp. 504–505), the experts state that in a minority of cases the withdrawal symptoms can be severe and last several weeks with the potential for misdiagnosis as relapse: ‘It is presumed that tapering is an effective strategy to minimise discontinuation symptoms but there is a lack of evidence about this or the optimal rate of taper.’.
Discussion
Despite a plethora of research detailing the existence and manifestation of a discontinuation syndrome following antidepressant withdrawal, the comprehensive literature review identified only 18 articles which provided explicit guidelines on how best to discontinue antidepressant medication in order to avoid unpleasant side effects. Many of the reviewed articles also comment on the lack of guidance available, with McHugh and Krishnadas highlighting the lack of controlled data as to the effectiveness of tapering, the duration by which this should occur or the lowest dose recommended prior to treatment termination [McHugh and Krishnadas, 2011]. Likewise, Warner and colleagues [Warner et al. 2006] also add that there are no ‘clear, validated tapering recommendations’ and Edwards [Edwards, 2006] describes antidepressant tapering as more of ‘an art than science’ due to the lack of any data to support a definitive tapering procedure. Ogle and Akkerman also note that there are few, if any, studies which describe appropriate discontinuation methods for specific antidepressant drugs and the data which are available are taken from limited controlled trials and drug manufacturers’ studies [Ogle and Akkerman, 2013].
As well as there being a lack of guidance in general, the available literature comes with its own limitations, putting into question whether or not the advice available is even reliable. For instance, of the articles reviewed in the current study only five are clinical studies [Tint et al. 2008; Montgomery et al. 2004; Baldwin et al. 2007; Himei and Okamura, 2006; van Geffen et al. 2005] of which none have substantial sample sizes. This presents a real concern in that the guidance which is available rests upon a weak evidence base from clinical trials. Similarly, all five studies rely upon self-report measures such as the DESS to measure discontinuation symptoms. The DESS, or discontinuation-emergent signs and symptoms questionnaire, is a 43-item clinician-rated or patient-completed checklist developed by Rosenbaum and colleagues in 1998 to assess the number of adverse side effects reported in the literature [Rosenbaum et al. 1998]. According to Lader, the DESS is lengthy, which restricts its use in some research and clinical settings but it remains the scale recognized by most regulatory agencies [Lader, 2007]. Self-report measures often possess validity problems as information may be wrongly remembered or biased. Similar to the controlled trials reviewed, the case series [Cromarty et al. 2010] is limited in that it reports on a small amount of data, only three cases. They also note that a full experimental design was not used in the study and that the variables measured are defined based on the participants’ perception of them which, much like self-report measures, creates validity issues. The majority of the identified literature were reviews and although these can be useful in collating the available information and providing guidance based upon cumulative findings, reviews are unable to provide any empirical evidence for such recommendations or add any further findings to what is already known. Consequently, it is not only the general lack of guidance but also the quality of the data available that causes concern.
Although there are few studies available, the guidance they provide does possess substantial face validity. From the available literature there is a general consensus that the best method is to taper the drug slowly in order to avoid discontinuation symptoms. At present, the most recent antidepressant guidelines advise this method and recommend a minimum period of a 4-week taper following long-term treatment, preferably over months for a planned withdrawal of antidepressant medication [Cleare et al. 2015]. However, as highlighted, some debate remains as to the optimum taper schedule implemented. McHugh and Krishnadas add that individuals vary in their propensity to experience discontinuation symptoms and there should be no time pressure on the tapering period when an antidepressant is being terminated altogether [McHugh and Krishnadas, 2011]. Despite this, the question of methods of discontinuation will remain an ongoing issue with the release of novel agents for the treatment of depression and information for both practitioner and patient alike needs to be made available.
Currently a number of websites such as WebMD and Harvard Health offer advice to patients considering or presently undergoing drug withdrawal. But information is general and at times contradictory: for example, the duration that a drug should be tapered and the proportion of people likely to experience the syndrome vary between websites. Likewise, whilst WebMD quotes the National Institutes of Health in saying that antidepressants are not ‘habit-forming’ [WebMD, 2014], the charity Mind advises that some drugs do have the potential to be addictive as some are used as street drugs (e.g. the MAOI tranylcypromine) [Mind, 2014]. Haddad and Anderson reiterate that there is ‘no evidence that patients crave antidepressants once they have stopped them’ in general [Haddad and Anderson, 2007], however some rarely prescribed drugs, most markedly tranylcypromine, can create dependence. According to Haw and Stubbs, of the patient information leaflets available on antidepressants, not all contain a warning or explanation of the symptoms of the discontinuation syndrome or why it is best not to withdraw these medications abruptly and without the supervision of a medical professional [Haw and Stubbs, 2010]. This information should be available and adequate, as noted by van Geffen and colleagues, patients feel less distress from the symptoms they experience when they have been made aware of them and their self-limiting nature [van Geffen et al. 2005].
As mentioned previously, specific guidance also needs to be made available for cases in which there is particular concern such as pregnancy and treatment of the elderly. Of the articles reviewed, only one discusses discontinuation in people over the age of 65 years [Zarowitz, 2006]. Nor do any of the articles reviewed provide advice as to discontinuation methods in expectant mothers despite the extensive literature which details the concerns that this poses for both mother and child. One study found some tentative evidence for a dose effect for antidepressants and the risk of neonatal discontinuation symptoms [Galbally et al. 2009]: this suggests that dose rather than drug half-life and placental passage may be more critical in determining risk. In cases such as these the practitioner should explain the risk/benefit ratio to the patient and discuss it so that informed decisions can be made as to treatment continuation or withdrawal. For instance, it may be advisable in certain cases to maintain antidepressant treatment at low doses for those older patients who would find discontinuation particularly troublesome, whilst mothers who chose to continue treatment during pregnancy may choose to refrain from breastfeeding as this along with exposure
Along with providing guidelines and advice, certain measures should be taken in order to avoid or prevent discontinuation symptoms. Most importantly, the selection of patients and choice of antidepressant could reduce the numbers of people experiencing the syndrome. Many of the reviewed studies suggest that fluoxetine requires no taper and is associated with relatively few symptoms on discontinuation. Likewise newer agents such as agomelatine, have been reported to have no associated discontinuation syndrome and therefore patients may benefit from treatment or even switching to these drugs upon withdrawal [Montgomery et al. 2004]. Smeraldi and Delmonte warn, however, that when switching from fluvoxamine to agomelatine the inhibition of CYP 450 1A2 and 2C9 by fluvoxamine can increase agomelatine levels if prescribed simultaneously [Smeraldi and Delmonte, 2013]: a 3-day washout period is preferable to avoid this. McAllister-Williams and colleagues also warn that the first drug would need to be withdrawn gradually to avoid symptoms recurring but that this can take place once agomelatine treatment has begun, in cases other than with fluvoxamine [McAllister-Williams et al. 2010]. Tapering can also be facilitated by liquid formulations for precision in very gradual dose reductions, whilst tapering strips are now available for some antidepressants, including paroxetine, in which each strip contains a slightly lower dose on each consecutive day [Groot, 2013]. Another potential method of avoiding unnecessary discomfort during discontinuation may come from the use of specialist nurses that have been trained in antidepressant discontinuation. This strategy has been trialled previously for benzodiazepine withdrawal, with one study in particular reporting that, after a period of one year, two thirds of patients had successfully ceased taking the medication [Lopez-Peig et al. 2012]. Finally, treatment should also be kept as short as possible with the aim of complete discontinuation.
The current study reviews the literature available on the best methods of discontinuation for antidepressant medication. The study focuses upon the newer second-generation antidepressants due to the proportion and severity of the associated discontinuation syndrome. The review stresses the lack of guidance currently available to both practitioners and patients, particularly the lack of controlled data to inform this guidance. On the whole, more adequate guidelines for tapering and discontinuation need to be made freely available, with particular attention given to topics such as discontinuation in pregnancy and old age. Also, appropriate methods for specific agents, especially those such as paroxetine which are reportedly more likely to present with severe symptoms, are needed to reduce the current clinical difficulties. The present study is limited in that as a review it cannot add any new information and wider searching of databases may identify research which might have been unknowingly omitted from this review.
Footnotes
Acknowledgements
Professor Malcolm Lader was the supervisor of Emma Wilson.
Conflict of interest statement
The authors declare that there is no conflict of interest.
Funding
This review was supported by a student grant to Emma Wilson by the Department of Neuroscience, Institute of Psychiatry, Psychology and Neuroscience, King’s College London.
