Abstract
Objective:
This study was designed to explore the efficacy and tolerability of oral paliperidone extended release (ER) in a sample of patients who were switched to flexible doses within the crucial first 5 years after receiving a diagnosis of schizophrenia.
Methods:
Patients were recruited from 23 countries. Adults with nonacute but symptomatic schizophrenia, previously unsuccessfully treated with other oral antipsychotics, were transitioned to paliperidone ER (3–12 mg/day) and prospectively treated for up to 6 months. The primary efficacy outcome for patients switching for the main reason of lack of efficacy with their previous antipsychotic was at least 20% improvement in Positive and Negative Syndrome Scale (PANSS) total scores. For patients switching for other main reasons, such as lack of tolerability, compliance or ‘other’, the primary outcome was non-inferiority in efficacy compared with the previous oral antipsychotic.
Results:
For patients switching for the main reason of lack of efficacy, 63.1% achieved an improvement of at least 20% in PANSS total scores from baseline to endpoint. For each reason for switching other than lack of efficacy, efficacy maintenance after switching to paliperidone ER was confirmed. Statistically significant improvement in patient functioning from baseline to endpoint, as assessed by the Personal and Social Performance scale, was observed (p < 0.0001). Treatment satisfaction with prior antipsychotic treatment at baseline was rated ‘good’ to ‘very good’ by 16.8% of patients, and at endpoint by 66.0% of patients treated with paliperidone ER. Paliperidone ER was generally well tolerated, with frequently reported treatment-emergent adverse events being insomnia, anxiety and somnolence.
Conclusions:
Flexibly dosed paliperidone ER was associated with clinically relevant symptomatic and functional improvement in recently diagnosed patients with non-acute schizophrenia previously unsuccessfully treated with other oral antipsychotics.
Introduction
Early treatment of patients with schizophrenia may be particularly important. The initial course of the disease is generally considered to be most amenable to intervention, with symptoms becoming more stable after 5 years [Lieberman et al. 2001; McGorry et al. 2008; Rosen and Garety, 2005]. Indeed, when compared with patients with chronic disease, a higher proportion of patients recently diagnosed with schizophrenia were hospitalized, with length of stay being longer and healthcare costs being higher [Nicholl et al. 2010]. Targeting treatments to the first 2–5 years of illness may optimize achieving desirable outcomes [McGorry et al. 2008]. In addition, data from two observational studies reported that patients with recently diagnosed schizophrenia (⩽3 years) might be more responsive to treatment than those with more long-standing disease [Dubois et al. 2014].
Paliperidone extended release (ER) is effective in the management of schizophrenia; both short-term and long-term efficacy and safety of paliperidone ER have been demonstrated in randomized controlled trials in patients with schizophrenia. Paliperidone ER, an oral second-generation atypical antipsychotic, uses an innovative osmotic controlled-release oral delivery system (OROS® osmotic technology, Alza Pharmaceuticals, Palo Alto,California) in order to achieve minimal peak to trough fluctuations over 24 h with once-daily dosing, and to decrease steady-state drug concentrations in the body [Conley et al. 2006]. Short-term efficacy and safety were demonstrated by analyzing pooled data from three 6-week randomized controlled clinical trials treating patients with acute schizophrenia with fixed doses of paliperidone ER versus placebo [Davidson et al. 2007; Kane et al. 2007; Marder et al. 2007; Meltzer et al. 2008]. These patients experienced significant improvements in psychotic symptoms, disease severity, and patient functioning for all paliperidone ER doses tested, as well as good safety and tolerability [Meltzer et al. 2008]. Maintenance of good long-term efficacy and tolerability was shown using pooled data from three 52-week, open-label, long-term extensions of randomized, controlled clinical trials treating acute schizophrenia with paliperidone ER [Emsley et al. 2008]. The most commonly reported treatment-emergent adverse events (TEAEs) were insomnia and headache. Weight increased by a mean of 1.1 kg at endpoint.
Studies of long-term outcomes suggest that patients with recently diagnosed schizophrenia may benefit more from treatment than patients with a longer duration of disease. A post hoc analysis of data from a 1-year study treating stable patients with risperidone long-acting injectable (25 mg or 50 mg every 2 weeks) compared outcomes in a small cohort of patients with non-acute schizophrenia diagnosed within 3 years of study enrolment (N = 57) versus those patients diagnosed for more than 3 years (N = 266) [Macfadden et al. 2010]. Patients more recently diagnosed with schizophrenia showed a trend toward lower relapse (10.5% versus 21.8%; p = 0.053), and significantly better improvement in psychotic symptoms as assessed by Positive and Negative Syndrome Scale [PANSS; mean ± standard deviation (SD): PANSS total score change −10.2 ± 2.0 versus −3.8 ± 0.9; p = 0.004] and Clinical Global Impressions, Severity Scale (CGI-S; mean ± SD: CGI-S score −0.5 ± 0.1 versus −0.2 ± 0.1; p = 0.002). Another post hoc analysis of data pooled from three double-blind trials followed by 1-year open-label extensions compared outcomes after switching to paliperidone ER in 259 patients diagnosed within 3 years of enrolment and 925 patients diagnosed for more than 3 years [Canuso et al. 2010]. Patients in this sample had active symptoms at enrolment with mean baseline PANSS total scores of around 92–94. At endpoint from the open-label treatment, patients more recently diagnosed with schizophrenia improved significantly by PANSS total score (mean ± SD: −32.3 ± 1.5 versus −26.7 ± 0.9; p = 0.001) and Personal and Social Performance (PSP) scale [Morosini et al. 2000] total score (mean ± SD: 18.8 ± 1.2 versus 14.7 ± 0.7; p = 0.003).
Information on treatment outcomes for specific patient groups with paliperidone ER in the real world rather than clinical trial setting, however, is limited. A recent 6-month prospective interventional study used a real-world design to explore the use of paliperidone ER in 1812 patients with nonacute schizophrenia, previously treated unsuccessfully with other oral antipsychotic medications [Schreiner et al. 2014]. This flexible-dose study supported results from previous randomized controlled trials demonstrating treatment response, tolerability and safety of paliperidone ER under conditions of routine clinical practice. As recent research findings have suggested a higher treatment response and different side-effect profile in patients with schizophrenia recently diagnosed with their disease, the current analysis explores 6-month treatment response, safety and tolerability data, patient-reported outcomes, and predictors of response in a subset of patients from this larger study, specifically the subset of patients who were recently diagnosed with schizophrenia.
Methods
This study explored patients with non-acute schizophrenia previously unsuccessfully treated with another oral antipsychotic, who had been diagnosed with schizophrenia within 5 years. This group was part of a larger study (N = 1812) which has been published previously [Schreiner et al. 2014].
This study was conducted in Belgium, Bulgaria, Croatia, Denmark, Finland, France, Germany, Greece, Hungary, Israel, Italy, Latvia, Lithuania, Poland, Portugal, Russia, Serbia, Spain, Sweden, Switzerland, Turkey, The Netherlands and the United Kingdom from April 2007 to January 2009. The study was performed in accordance with the guidelines of the International Conference on Harmonization for Good Clinical Practice, and the study protocol was approved by Independent Ethics Committees. Prior to study enrolment, all potential participants provided written informed consent.
Patients
Eligible patients were inpatients or outpatients aged at least 18 years, with a diagnosis of schizophrenia according to the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV) or a related disorder that was treated with an antipsychotic. All patients were diagnosed with a psychotic disorder within the preceding 5 years. Schizophrenia was considered to be non-acute when treated with an oral antipsychotic and the patient experienced a change in CGI-S score of 1 or less during the 4 weeks before enrolment. Patients were required to have previously received an adequate, that is, therapeutic dose of any other oral antipsychotic for a sufficient period of time (at least 1 month) prior to enrolment, per investigator judgment. Patients were excluded if they had any of the following: known hypersensitivity to paliperidone ER or risperidone; had been treated with clozapine or a long-acting injectable antipsychotic during the preceding 3 months; significant medical illness; tardive dyskinesia; neuroleptic malignant syndrome; high risk for adverse events (AEs) or self-harm; or substance dependence over the past 6 months (however, substance abuse was allowed). If patients had been treated with an adequate dosage of an appropriate oral antipsychotic for an adequate period of time, previous antipsychotic treatment could be considered unsuccessful due to various causes, including lack of efficacy, tolerability or safety issues, or lack of compliance.
Treatment
Patients were flexibly dosed with oral paliperidone ER tablets (3–12 mg/day) with a recommended starting dose of 6 mg once daily. Most patients were transitioned to an effective dose of paliperidone ER without titration and were treated for up to 6 months.
Other antipsychotics prescribed for the treatment of schizophrenia were not allowed during the entire study. Previous antipsychotics had to be discontinued or tapered off over a maximum of 4 weeks based on the clinical situation and investigator’s decision. Some concomitant medications were permitted during this study. Antipsychotics and other psychotropic medication administered prior to enrolment for conditions other than schizophrenia, such as sleep induction or sedation, could be continued during the trial if a stable dose was maintained. Benzodiazepines were allowed as rescue medication during the trial for periods of up to 10 consecutive days. Benztropine mesylate or biperidene up to 4 mg/day, or trihexyphenidyl up to 10 mg/day were permitted for the treatment of extrapyramidal symptoms, with the need for anticholinergic medication to be evaluated by the investigator on an ongoing basis.
Outcome measures
Assessments of efficacy, and safety and tolerability were made at baseline and treatment weeks 4, 8, 13 and 26 (or endpoint).
Efficacy assessments
The primary efficacy outcome was based on the main reason for transitioning to paliperidone ER. For patients switching for the main reason of lack of efficacy with a previous oral antipsychotic, the primary efficacy outcome was an improvement in PANSS total score of at least 20% [Kay et al. 1987] from baseline to endpoint. These patients were termed responders. For patients switching for main reasons other than lack of efficacy, the primary efficacy outcome was the shift in PANSS total score from baseline to endpoint. Non-inferiority was defined as a difference of no more than 5 points at endpoint versus baseline on the PANSS total score. Schuirmann’s one-sided test was used to confirm non-inferiority.
The following additional efficacy measures were assessed at baseline and treatment week 26 (or endpoint): PANSS subscale and Marder factor [Marder et al. 1997] scores; CGI-S scores [Guy, 1976]; and PSP scores [Morosini et al. 2000]. The CGI-S scores measure symptom severity on a scale from 0 to 6: ‘normal’ (0); ‘borderline ill’ (1); ‘mildly ill’ (2); ‘moderately ill’ (3); ‘markedly ill’ (4); ‘severely ill’ (5); and ‘extremely ill’ (6). The PSP scale is a clinician-reported measure of severity of personal and social dysfunction which was developed as an improvement upon the Social and Occupational Functioning Assessment Scale (SOFAS), and the Global Assessment of Functioning (GAF) scale. It is a 100-point single-item rating scale based on the assessment of the functioning of patients in four distinct domains (socially useful activities; personal and social relationships; self-care; and disturbing and aggressive behaviours). Patient satisfaction with previous antipsychotic treatment at baseline and with paliperidone ER at endpoint was assessed using a 5-point scale: ‘very poor’ (5); ‘poor’ (4); ‘moderate’ (3); ‘good’ (2); and ‘very good’ (1).
Safety and tolerability
TEAEs were recorded throughout the study. Extrapyramidal Symptom Rating Scale (ESRS) scores [Chouinard and Margolese, 2005] were assessed at baseline and treatment weeks 4, 8, 13 and 26 (or endpoint). Body weight was measured and body mass index (BMI) was calculated at baseline and at treatment weeks 13 and 26 (or endpoint). Sleep quality and daytime drowsiness over the previous 7 days were scored using an 11-point ordinal scale. Sleep scores ranged from ‘very badly’ (0) to ‘very well’ (10); daytime drowsiness ranged from ‘not at all’ (0) to ‘all the time’ (10).
Statistical analysis
Unless stated otherwise, descriptive results of continuous/ordinal variables are presented as mean ± SD. Patients receiving at least one dose of paliperidone ER and having at least one post-treatment assessment were included in the efficacy and safety analyses of the intent-to-treat population. Patient demographics, efficacy, treatment satisfaction and safety parameters were assessed using descriptive statistics. Primary efficacy was assessed by estimating the 95% confidence intervals (CIs) for treatment response. Within-group changes versus baseline were evaluated using the two-tailed Wilcoxon signed-rank test (α = 0.05). For 76–80% of patients, data were available for baseline and week 26, and for 20–24% the analysis reflected last observation carried forward (LOCF) data for endpoint only.
For the predictor analyses of treatment response, we used a more stringent criterion (also called clinical response), that is, a decrease in the PANSS total score from baseline to endpoint of at least 20% and a decrease in CGI-S score of at least one point. For the analysis of explanatory variables for clinical response, a stepwise logistic regression was used, taking into account age, sex, BMI, diagnosis and duration of schizophrenia, number of prior hospitalizations in the previous 12 months, main reason for switching to paliperidone ER, previous antipsychotic, baseline psychotic symptoms assessed by PANSS score, disease severity assessed by CGI-S score, and functional status assessed by PSP score. Country of origin was included in all models to correct for possible nonclinical predictors, such as clinical settings, dosing, titration and concomitant medication. First, country and all baseline explanatory variables were included in the model one at a time and then separately; a stepwise-forward selection method in logistic regression analysis was used including all baseline explanatory variables to obtain an initial set of significant explanatory variables at the 10% level, correcting for potential country effects. Second, a stepwise-forward selection method was used including country and the initial set of significant explanatory variables in order to obtain a reduced model. Third, the nonsignificant explanatory variables were included in the reduced model (including country) and checked for significance at the 10% level. If necessary, the second and third steps were repeated to obtain the final model (including country).
Results
Patients
A total of 719 patients were screened: 3 patients who were screened were not enrolled into the study as they failed to meet the inclusion criteria, and 3 additional patients did not receive paliperidone ER (2 patients withdrew their consent after enrolment and 1 patient decided not to start the study treatment). Consequently, 713 patients were enrolled in the study and treated with paliperidone ER (Figure 1). Patients were predominantly male and had paranoid subtype of schizophrenia (Table 1). Four patients had a diagnosis other than schizophrenia (1 each with bipolar disorder, coenestopathic, pseudoneuroticism and schizophrenia simplex). Although the selection criterion was less than 5 years since diagnosis, interestingly the actual mean ± SD time was only 2.3 ± 1.7 years. The main reason for switching to paliperidone ER was most commonly due to lack of efficacy (54.3%) or tolerability issues (29.9%) with the previous oral antipsychotic. At baseline, most patients were using a single antipsychotic medication (83.3%), 11.5% were using more than one antipsychotic, and 5.2% did not use an antipsychotic before baseline, which reflects a major protocol deviation. The most common previous oral antipsychotics were risperidone (41.1%), olanzapine (21.2%), quetiapine (10.1%), haloperidol (9.0%) and aripiprazole (8.8%).

Patient disposition.
Baseline characteristics.
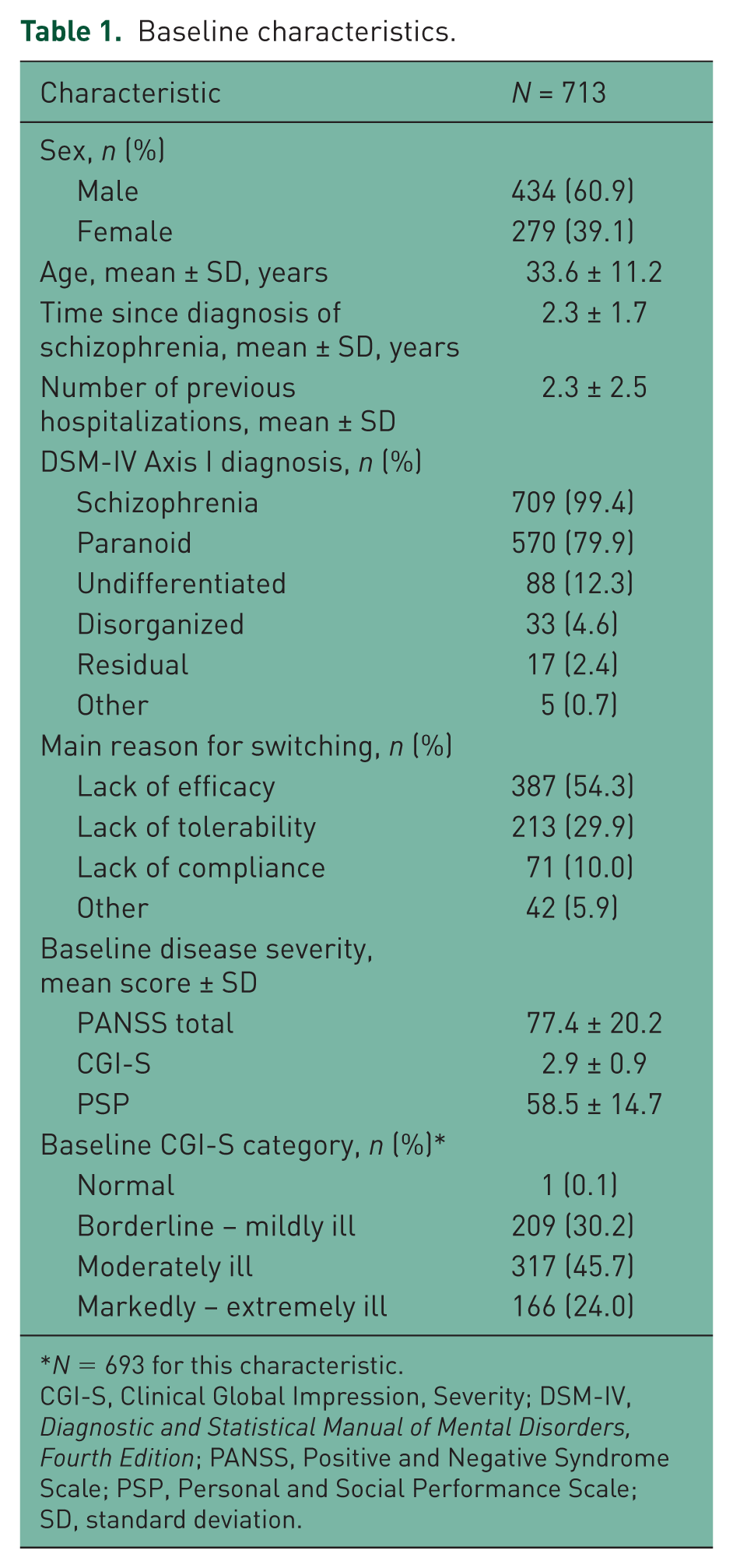
N = 693 for this characteristic.
CGI-S, Clinical Global Impression, Severity; DSM-IV, Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; PANSS, Positive and Negative Syndrome Scale; PSP, Personal and Social Performance Scale; SD, standard deviation.
For recently diagnosed patients, the mean ± SD initial paliperidone ER dose was 5.2 ± 1.9 mg/day (median: 6 mg/day), with a mean ± SD average dose of 6.8 ± 2.5 mg/day during the study (median: 6 mg/day) and mean mode ± SD dose of 7.0 ± 2.9 mg/day (median: 6 mg/day). Mean average paliperidone ER dose for patients switching for reasons other than lack of efficacy was 6.2–6.3 mg/day, which was slightly lower compared with patients switching for the reason of lack of efficacy (average dose: 7.2 mg/day). Mean ± SD duration of exposure was 149.6 ± 58.7 days, with an increase in dosing occurring for 417 patients (58.5%) and a decrease for 139 patients (19.5%) during the study.
Efficacy
Efficacy data were available for 693 patients. For patients who switched due to the main reason of lack of efficacy (n = 377), the primary efficacy outcome, an improvement in PANSS total score of at least 20% from baseline to endpoint, occurred in 63.1% of patients (95% CI 58.0–68.0). For patients switching for main reasons other than lack of efficacy, the primary efficacy outcome was non-inferiority in efficacy, defined as a difference of no more than 5 points in mean change from baseline at endpoint in PANSS total score. Mean ± SD baseline PANSS total scores were 83.6 ± 18.5 for patients switching due to lack of efficacy (n = 377), 66.1 ± 17.0 for patients switching due to lack of tolerability (n = 209), 80.6 ± 20.8 for lack of compliance (n = 67), and 72.7 ± 23.9 for ‘other’ reasons (n = 40). Mean ± SD changes from baseline to endpoint were −8.9 ± 18.2 for patients switching for the main reason of lack of tolerability, −18.4 ± 20.7 for lack of compliance, and −11.3 ± 14.2 for ‘other’ reasons. Schuirmann’s one-sided test confirmed non-inferiority to within the specified equivalence bounds for each group (p < 0.0001).
Mean improvement in PANSS total scores, as well as PANSS subscales and Marder factors, from baseline to endpoint for the entire recently diagnosed population was statistically significant and clinically relevant (Table 2). For each of the subgroups based on main reason for switching, mean baseline to endpoint changes for PANSS total, subscale and Marder factor scores were significant (all p ⩽ 0.0001, except for the ‘uncontrolled hostility/excitement’ score, which was p = 0.0028 for ‘other’ reason for switching and which was not statistically significant for patients switching due to lack of tolerability).
Mean Positive and Negative Syndrome Scale (PANSS) scores at baseline and endpoint for all patients (N = 693).

All values are mean ± standard deviation.
p < 0.0001; change in PANSS scores (from baseline to endpoint) tested with the two-tailed Wilcoxon signed-rank test.
Based on CGI-S categories, 30.3% of patients were ‘normal’ to ‘borderline – mildly ill’ at baseline; this percentage increased to 56.3% at endpoint [Figure 2(a)]. CGI-S scores at baseline cor-responded to ‘moderately ill’ (mean ± SD: 2.9 ± 0.9). Baseline to endpoint improvement in CGI-S scores (mean ± SD: −0.6 ± 1.1) was statistically significant (p < 0.0001), with a CGI-S score at endpoint corresponding to ‘mildly ill’ (mean ± SD: 2.4 ± 1.2). Baseline to endpoint improvement in CGI-S scores was statistically significant for each subgroup based on main reason for switching (p ⩽ 0.0001, except for ‘other’ reason for switching, which was p = 0.0191).

Secondary efficacy measures at baseline and endpoint: Clinical Global Impression, Severity categories (a); Personal and Social Performance (PSP) scale categories (b); and treatment satisfaction (c). ER, extended release.
Among the 660 patients with both baseline and endpoint data for the PSP scale, mean ± SD total PSP scale score improved from 58.6 ± 14.5 at baseline to 65.9 ± 15.7 at endpoint (p < 0.0001). Improvements were also statistically significant at both 13- and 26-week assessments (p < 0.0001). Baseline to endpoint improvements in PSP scale scores were statistically significant for each subgroup based on main reason for switching (p ⩽ 0.0001, except for ‘other’ reason for switching, which was p = 0.0265). At baseline, only 17.7% of patients showed a mild degree of difficulty in functioning; this was increased to 39.8% at endpoint [Figure 2(b)]. At baseline, 5.2% of patients functioned so poorly that they required intensive supervision; this was reduced to 3.5% at endpoint [Figure 2(b)].
For the total population, mean ± SD treatment satisfaction scores were 3.2 ± 0.8 (representing moderate satisfaction) with the prior antipsychotics at baseline and 2.3 ± 1.0 (representing good satisfaction) with paliperidone ER at endpoint. Treatment satisfaction with prior antipsychotic treatment at baseline was rated ‘good’ to ‘very good’ by 16.8% of patients and at endpoint by 66.0% of patients treated with paliperidone ER [Figure 2(c)]. Proportions of patients who rated treatment satisfaction with prior antipsychotic treatment ‘good’ to ‘very good’ were lower for patients who switched due to lack of efficacy compared with patients who switched due to reasons other than lack of efficacy (with prior antipsychotic at baseline: 14.7% versus 19.4%; with paliperidone ER at endpoint: 60.2% versus 73.1%).
Improvements in quality of sleep and daytime drowsiness were significant at each assessment and at endpoint (p < 0.0001) (Figure 3). Improvement in sleep quality from baseline to endpoint was statistically significant for patients switching due to lack of efficacy (p < 0.0001) and lack of compliance (p = 0.0003). Reduction in daytime drowsiness from baseline to endpoint was statistically significant for patients switching due to lack of efficacy, lack of tolerability and lack of compliance (p ⩽ 0.0007).
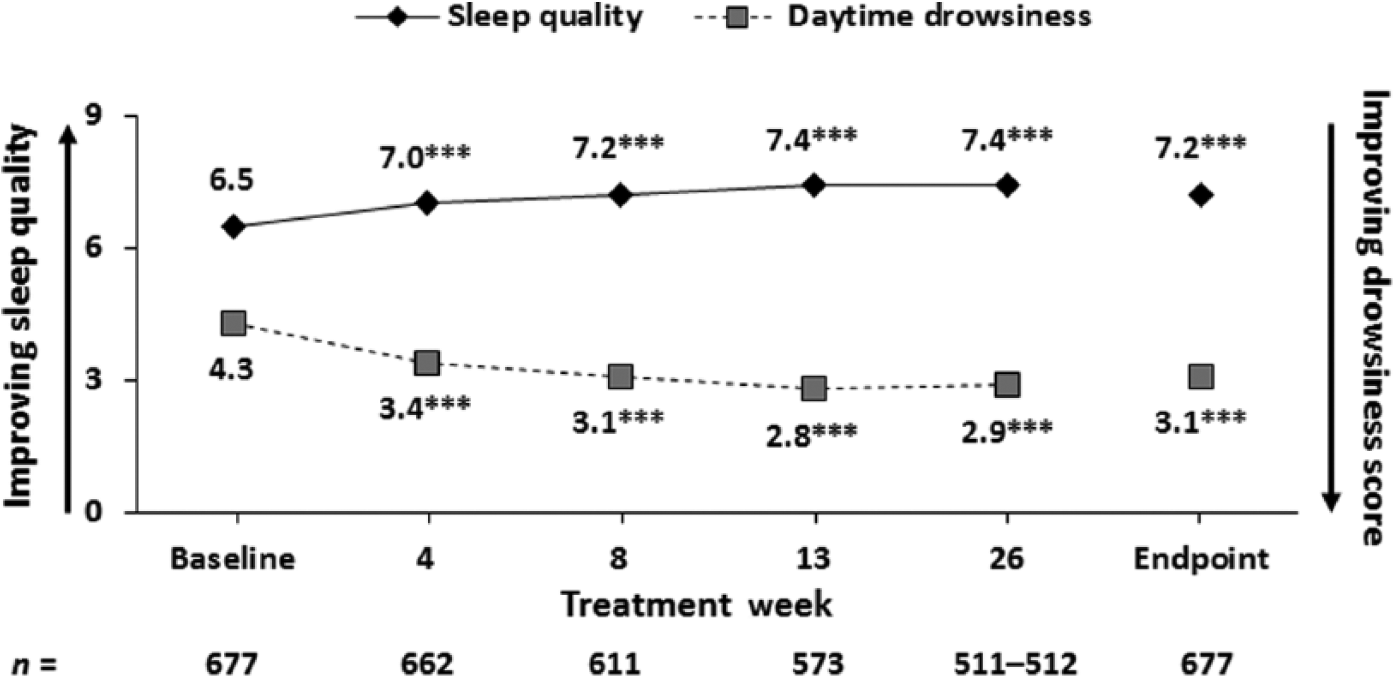
Sleep quality and daytime drowsiness.
Predictor analysis
Clinical response (defined as a decrease in PANSS total score from baseline to endpoint of at least 20% plus a decrease in CGI-S score of at least one point) occurred for 295 patients (42.6%). Baseline CGI-S score was a significant predictor of clinical response (odds ratio 1.465; 95% CI 1.204–1.783; p < 0.001) (Table 3). There was a trend for the type of schizophrenia and the main reason for switching to paliperidone ER to also be predictors of clinical response (p = 0.0543 and p = 0.0764, respectively).
Important clinical predictors of clinical response based on logistic regression after stepwise modeling.*

Country of origin was included in the model to correct for possible nonclinical predictors, like clinical settings, dosing, titration, and concomitant medication.
CGI-S, Clinical Global Impression, Severity; CI, confidence interval.
Safety and tolerability
Safety data were available for 712 treated patients, and 413 patients (58.0%) reported experiencing at least 1 TEAE (Table 4). Paliperidone ER was generally well tolerated. Serious TEAEs were experienced by 59 patients (8.3%); the most common serious TEAEs were psychotic disorder (n = 16; 2.2%), schizophrenia (n = 14; 2.0%) and anxiety (n = 8; 1.1%). TEAEs occurring in at least 5% of patients were insomnia, anxiety and somnolence.
Treatment-emergent adverse events (TEAEs).

Values are presented as n (%).
Most common were psychotic disorder (2.2%), schizophrenia (2.0%) and anxiety (1.1%).
Percentages are based on the total number of TEAEs (n = 1116).
At baseline, a total of 33 potentially prolactin-related AEs were reported in 30 (4.2%) patients with their previous oral antipsychotic: amenorrhea (n = 13); erectile dysfunction (n = 5); sexual dysfunction (n = 5); galactorrhea (n = 3); erectile libido decreased/libido disorder/loss of libido/abnormal orgasm (n = 2); ejaculation failure (n = 2); and gynecomastia, dysmenorrhea and breast discharge (n = 1 each). Hyperprolactinemia or increased blood serum prolactin levels were reported in 13 (1.8%) patients at baseline.
During the study, 50 different potentially prolactin-related TEAEs were reported in 45 (6.3%) patients: amenorrhea (n = 13); galactorrhea (n = 13); libido disorder/decreased libido/anorgasmia/orgasm abnormal (n = 7); erectile dysfunction (n = 7); sexual dysfunction (n = 5); menstrual disorder (n = 2); and breast discharge/gynecomastia/oligomenorrhea (n = 1 each). In 14 patients (2.0%), elevated serum prolactin levels were reported.
Extrapyramidal symptoms, as measured by the ESRS, improved significantly at each assessment and endpoint (p < 0.0001) (Figure 4). Baseline to endpoint improvement in total ESRS scores was statistically significant for subgroups switching for the main reasons of lack of efficacy and lack of tolerability (p < 0.0001).

Extrapyramidal symptoms as measured by mean Extrapyramidal Symptom Rating Scale (ESRS) total scores. Note: decreasing ESRS scores reflect improvement in extrapyramidal symptoms.
Baseline and endpoint body weight and BMI were recorded for 648 patients. For the total population, mean ± SD baseline weight and BMI were 79.4 ± 17.9 kg and 26.6 ± 5.3 kg/m2, respectively. Mean ± SD weight and BMI increased, respectively, by: 0.7 ± 3.8 kg and 0.3 ± 1.3 kg/m2 at week 13; 1.0 ± 5.1 kg and 0.4 ± 1.7 kg/m2 at week 26; and 0.9 ± 4.8 kg and 0.3 ± 1.6 kg/m2 at endpoint. Increases for both weight and BMI were statistically significant (p < 0.0001), but not considered clinically relevant at each assessment and endpoint.
Increases in body weight from baseline to endpoint were statistically significant, although not considered clinically relevant, for patients who switched from monotherapy quetiapine or risperidone (Figure 5). Notably, although not statistically significant, patients who switched from olanzapine monotherapy showed a decrease in body weight from baseline to endpoint.
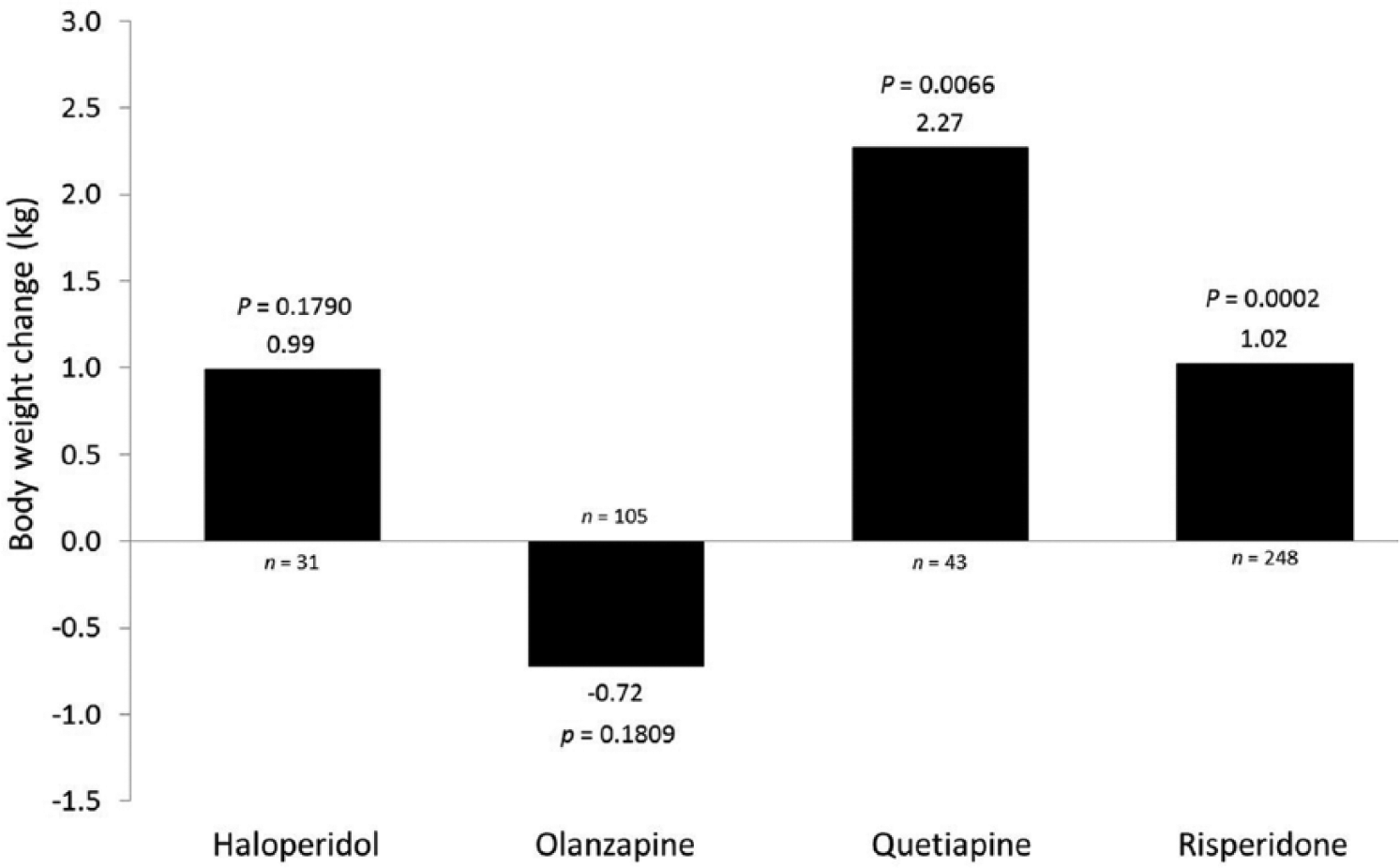
Change in bodyweight from baseline to endpoint by previous oral antipsychotic medication.
A clinically relevant weight change (⩾7%) from baseline to endpoint occurred in 85 patients (13.1%) of the total population. In patients switching from haloperidol monotherapy, a clinically relevant weight change was observed in 22.6%. The proportions of patients switching from monotherapy with olanzapine, quetiapine or risperidone with relevant weight change (⩾7%) were 9.5%, 14.0% and 11.7%, respectively.
For the total population, statistically significant, although mostly not clinically relevant, body weight increases were observed from baseline to endpoint for all patients with a baseline BMI of less than 25 kg/m2 (Figure 6). For patients with a baseline BMI of at least 30 kg/m2, no significant weight increases were observed.

Change in bodyweight from baseline to endpoint by baseline body mass index (BMI) category.
Discussion
Paliperidone ER is an effective antipsychotic treatment for patients recently diagnosed with schizophrenia. A majority of patients experienced a clinically relevant improvement in psychotic symptoms. The observed improvement in symptom severity is in line with previous data showing that improvement after switching antipsychotic therapy may be greater among patients with greater baseline impairment [Möller et al. 2005]. Also, the improvements in symptom severity, including positive and negative symptoms, observed here are consistent with data from randomized controlled trials [Meltzer et al. 2008; Turkoz et al. 2011]. In this context, it would be interesting to know whether consistent, once-daily, oral intake of an effective and well-tolerated antipsychotic medication can contribute to long-term efficacy and relapse prevention [Emsley et al. 2011]. Personal functioning and patient satisfaction showed improvement compared with prior antipsychotic treatment. This is especially important for younger patients because impaired personal and social functioning can negatively affect their education and social development. Furthermore, patient satisfaction with treatment is an important predictor for adherence to antipsychotic medication [Liu-Seifert et al. 2007].
Paliperidone ER was generally well tolerated in patients with recently diagnosed illness. Given the less sedating properties of paliperidone ER compared with many other second-generation antipsychotics, including oral risperidone [Jones et al. 2010; Luthringer et al. 2007; Turkoz et al. 2011], combining paliperidone ER temporarily with sedating comedication and allowing for an adequate cross-titration when switching from other, in particular, sedating antipsychotics [Schreiner et al. 2014; Stahl, 2008] may help to further improve tolerability. ESRS scores showed statistically significant improvement after switching to paliperidone ER, which could result from both the pharmacokinetic and pharmacodynamic profile of paliperidone ER [Conley et al. 2006; Ereshefsky and Mascarenas, 2003; Marchese et al. 2010; Turkoz et al. 2008]. The improvements in daytime drowsiness and sleep quality are consistent with data from a randomized controlled study comparing paliperidone ER and placebo [Luthringer et al. 2007]. The clinically relevant (⩾7%) change in bodyweight, observed in our study in a minority of patients who switched to paliperidone ER, supports data from a recent post hoc analysis that shows similar long-term tolerability with paliperidone ER among patients with either recently diagnosed schizophrenia (⩽5 years) or with chronic illness (>5 years) [Sliwa et al. 2012].
Efficacy outcomes in this study were similar to results from a post hoc assessment of a small sample of 57 patients who were diagnosed within 3 years with schizophrenia or schizoaffective disorder with stable symptoms [Macfadden et al. 2010]. These patients were treated with risperidone long-acting injectable and showed greater improvement in mean total PANSS and CGI-S scores than 266 patients who had been diagnosed more than 3 years previously. Improvements were more substantial in another post hoc analysis of patients with active symptoms switching to paliperidone ER [Canuso et al. 2010]; however, baseline impairments were also substantially greater in this population compared with the current sample with stable illness.
The results of the predictor analysis, indicating that patients with higher baseline disease severity are more likely to respond to treatment, are in line with other studies in patients with acute schizophrenia [Heres et al. 2014] and in patients with first-episode schizophrenia [Crespo-Facorro et al. 2007; Tabatabaee et al. 2008; Zhang et al. 2014]. These data conflict with a previously published analysis of drug-naive patients with schizophrenia in whom higher baseline CGI-S scores were a predictor of clinical non-response [Nordon et al. 2014]. However, mean baseline CGI-S score in that study was considerably higher (4.7) than in the present study (2.9). A few other studies have also either reported higher baseline disease severity predicted clinical non-response [Perkins et al. 2004] or no effect [Brousse et al. 2010].
The main limitations of this study are the open-label treatment of patients with paliperidone ER, the absence of a comparator group and the fact that this is a secondary analysis. Another limitation is the relatively short duration of the study (up to 6 months). Although the data do not provide head-to-head comparisons between treatments with different antipsychotics, the data do suggest that patients who have experienced failure in the form of lack of efficacy with other antipsychotics could still exhibit improvement with paliperidone ER. At the same time, for patients who needed to switch antipsychotics for other reasons, such as lack of tolerability, the significant result is that the patients maintained their previous improvement as assessed by PANSS and CGI-S scores.
Unlike earlier post hoc analyses comparing outcomes in patients with recent-onset versus more-established disease [Canuso et al. 2010; Macfadden et al. 2010], the current study only included patients with recent-onset schizophrenia requiring an antipsychotic. As a result of the importance of treating schizophrenia early, future studies may wish to compare very long-term outcomes among patients who had been treated when they still had more-recent-onset schizophrenia, and those with established disease who had started treatment later in the disease process.
In conclusion, flexibly dosed paliperidone ER treatment for up to 6 months was generally well tolerated, and associated with meaningful clinical response in non-acute patients recently diagnosed with schizophrenia who had been previously unsuccessfully treated with other oral antipsychotics. Specifically, for patients switching for the main reason of lack of efficacy, more than half of patients achieved an improvement in PANSS total scores of at least 20% from baseline to endpoint, and for each reason for switching other than lack of efficacy, maintenance of efficacy after switching to paliperidone ER was confirmed. Even more, patients who were switched for reasons other than lack of efficacy also demonstrated a statistically significant and meaningful improvement in clinical symptoms.
Footnotes
Acknowledgements
The authors would like to thank Pim Dekker, PhD, from Excerpta Medica for providing writing and editorial support.
Funding
The study, writing, and editorial support were funded by Janssen Pharmaceutical Companies of Johnson & Johnson in EMEA.
Conflict of interest statement
L. Helldin has no conflicts of interest. J. Peuskens has been a consultant for, received grants and/or research support and honoraria from, and been on the speakers’ bureaus and/or advisory boards of the following companies: AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Janssen, Lundbeck and Pfizer. R. Vauth has received funding for research, advisory board membership and sponsored lectures in the last 3 years from Janssen-Cilag, Otsuka, Lundbeck, Eli-Lilly and Swiss National Science Foundation. E. Sacchetti has received funding for consultancy, research, advisory board membership and sponsored lectures in the past 3 years from Lombardy Region, Italian Ministry of Education, University and Research, Angelini, AstraZeneca, Eli-Lilly, IMS Consulting Group, Innovapharma, Lundbeck, Janssen-Cilag, Otsuka, Pfizer, Roche, Rottapharm, Servier and Takeda. H. bij de Weg has no conflicts of interest. H. Herken has no conflicts of interest. M. Lahaye is a member of the Medical Affairs EMEA department of, and is employed by, Janssen-Cilag BV, The Netherlands. A. Schreiner is a full-time employee of Janssen-Cilag, Germany, and a shareholder of Johnson & Johnson.
