Abstract
Researchers have documented biases in attention and memory in depressed and dysphoric individuals. Several studies have examined these biases among previously depressed individuals, and while there is evidence that attention and memory biases persist in remitted depression, the findings are not consistent. One limitation of previous research is that few studies have used a stress or negative mood induction (MI) to activate the cognitive vulnerability posited to underlie attention and memory biases. The present study used a free-viewing eye-tracking paradigm to assess previously depressed participants’ attention biases for positive and negative words before and after a sad MI. Memory biases were assessed using tests of incidental recognition. Only participants who were successfully mood-induced were included in the analyses. Unlike previously depressed participants, never depressed participants exhibited attention and memory biases that favored positive over neutral words, both before and after the sad MI, suggesting a protective bias that is maintained in a sad mood state. After the sad MI, previously depressed participants had smaller attention biases for positive words and smaller memory biases for negative words compared to never depressed participants. The findings are generally supportive of the notion that cognitive vulnerability is maintained to some extent in remitted depression and can be influenced by a sad mood.
According to Beck’s (1967) cognitive model, biases in attention and memory reflect a deep-seated cognitive vulnerability to depression. When underlying depressive schemas are activated, vulnerable individuals attend to and process information in a way that prioritizes negative over neutral and positive information. Biased processing of emotional information is thought to increase risk for depression by increasing negative mood and thought content and interfering with effective emotion regulation (Beck, 1979; Clark & Beck, 1999). Consistent with Beck’s model and subsequent theories of the role of cognitive biases in depression (e.g., Everaert et al., 2012; Ingram, 1984; Joormann & Vanderlind, 2014; Teasdale, 1988), researchers have found strong support for depression-related biases in attention, memory, and other cognitive processes (see Gotlib & Joormann, 2010; LeMoult & Gotlib, 2019, for reviews). Relative to non-depressed individuals, depressed and dysphoric individuals attend to negative stimuli more and to positive stimuli less (Armstrong & Olatunji, 2012; Huang et al., 2023; Suslow et al., 2020), take longer to disengage from negative stimuli (Sanchez et al., 2013; Sanchez et al., 2017; Sears et al., 2010; but see Allard & Yaroslavsky, 2019) and have better memory for negative stimuli and poorer memory for positive stimuli (Bogie et al., 2019; Everaert et al., 2022). Depressed and dysphoric individuals also recall autobiographical memories with reduced specificity (i.e., overgeneral autobiographical memory; Liu et al., 2013; Weiss-Cowie et al., 2023) and are slower to recall autobiographical memories in response to positive cue words (Gupta & Kar, 2012).
An important but understudied phenomenon is the role of cognitive biases in maintaining vulnerability outside of an active depressive episode. Depression has a high relapse rate, and many individuals with depression experience multiple episodes (Burcusa & Iacono, 2007; Solomon et al., 2000). According to cognitive models, vulnerability persists in a dormant state when an individual recovers from a depressive episode and is no longer symptomatic (Beck, 1967, 1979; Scher et al., 2005). Stress or negative mood states can trigger the activation of depressive schemas and corresponding information processing biases in previously depressed individuals, including attention and memory biases, with consequences that may ultimately lead to a relapse of depression.
In contrast to the extensive literature on attention and memory biases in currently depressed individuals, fewer studies have examined these biases among previously depressed individuals. Overall, the research on attention biases indicates that biases persist beyond remission from an active depressive episode (see Shamai-Leshem et al., 2022, for a meta-analysis), but the findings are not consistent. Some studies have found that previously depressed individuals exhibit increased attention to sad or negative stimuli compared to non-depressed individuals (Joormann & Gotlib, 2007; Newman et al., 2019; Newman & Sears, 2015; Soltani et al., 2015), whereas others have not observed a group difference for negative biases (Isaac et al., 2014; Li et al., 2016; Sears et al., 2011). Some studies have reported decreased attention to positive stimuli among previously depressed individuals relative to non-depressed individuals (Joormann & Gotlib, 2007; Li et al., 2016; Newman et al., 2019; Sears et al., 2011; Soltani et al., 2015), whereas others have found no differences for positive biases (Elgersma et al., 2018; Isaac et al., 2014; Woody et al., 2016). There are inconsistencies even within studies. For example, Newman et al. (2019) found that previously depressed women exhibited the characteristic attention biases for negative and positive naturalistic images but not for sad and happy face images, in contrast to findings indicating attention biases for both naturalistic and face images in currently depressed samples (Suslow et al., 2020). Thus, although there is some evidence for the persistence of attention biases in remitted depression, the biases appear to be weaker and less consistent relative to the attention biases observed in current depression.
The findings of studies examining memory biases in previously depressed samples have also been mixed (see Everaert et al., 2022, for a meta-analysis). Consistent with theories of persistent cognitive vulnerability in remitted depression, some studies have found that previously depressed individuals recall more negative words and fewer positive words than never depressed individuals (Kircanski et al., 2013; Romero et al., 2014). Previously depressed individuals also exhibit overgeneral autobiographical memory relative to never depressed individuals (Hallford et al., 2022), although the magnitude of the effect is about half that for currently depressed individuals (Weiss-Cowie et al., 2023). However, other studies have observed memory biases among previously depressed individuals for stimuli of one emotional valence (either positive or negative) but not the other. For example, Fernandez et al. (2022) found that previously depressed individuals had smaller memory biases for positive words than never depressed individuals but did not differ in their biases for negative words. In contrast, Cerny et al. (2019) found that previously depressed individuals had larger memory biases for negative words but did not differ from never depressed individuals in their biases for positive words. Two other studies reported no evidence of any valence-specific memory biases among previously depressed individuals (Bogie et al., 2019; Sears et al., 2011).
A limitation of previous research on attention and memory biases in remitted depression is that few studies have used a stress or negative mood induction (MI) to activate the vulnerability that is hypothesized to remain dormant outside of an active depressive episode. When previously depressed individuals participate in a research study, their baseline mood states and levels of recent or ongoing stress will naturally vary. As such, the extent to which their cognitive vulnerability is naturally activated is unknown and is likely to vary within and across samples. Without an experimental manipulation of mood to systematically activate cognitive vulnerability, heterogeneity in the extent to which cognitive vulnerability is activated is likely to produce corresponding variability in the extent to which memory and attention biases will be exhibited. This heterogeneity may, in part, explain the less robust biases and inconsistent findings observed in the literature on remitted depression. In a small number of early studies that used MIs with previously depressed samples, the findings generally supported Beck’s (1967) diathesis-stress hypothesis of cognitive vulnerability (see Scher et al., 2005, for a review). That is, previously depressed individuals, relative to never depressed individuals, were found to exhibit negatively biased cognition following a negative (or sad) MI or naturalistic stressor, but not when in a neutral mood state. However, most of these studies used self-report measures of cognitive content rather than behavioral measures of cognitive processing biases.
Recent meta-analyses of attention and memory biases in remitted depression highlight the limited scope of this literature and the consequent challenges for the diathesis-stress hypothesis of cognitive vulnerability. A meta-analysis of attention biases found that previously depressed individuals have larger biases for dysphoric stimuli and smaller biases for positive stimuli relative to never depressed individuals, and that the use of a MI did not moderate the magnitude of the differences in these biases (Shamai-Leshem et al., 2022). However, only four studies using MIs were available for the moderation analysis (Fritzsche et al., 2010; Newman & Sears, 2015; Platt et al., 2022; Zvielli et al., 2016) and the type of MI and analysis decisions (e.g., including all participants or only those for whom the MI was effective) varied across these studies. Two of the studies used eye-tracking measures of attention (Newman & Sears, 2015; Platt et al., 2022), which are a reliable method for measuring attention biases (Lazarov et al., 2016; Sears et al., 2019; Skinner et al., 2018; Waechter et al., 2014), whereas the others used response time-based measures that often have poor psychometric properties (Waechter et al., 2014, 2015). A meta-analysis of memory biases in previously depressed individuals found that although the use of a MI was not a significant moderator of effect size, there was a significant pooled effect for studies with a MI but not for studies without a MI (Everaert et al., 2022). This outcome suggests that memory biases in previously depressed individuals may only occur following a mood or stress induction (Everaert et al., 2022). However, this analysis was also based on a small number of studies (with only seven of those studies using a MI) and aggregated across disparate effects (e.g., positive and negative biases; between-subject and within-subject comparisons). Ultimately, the fact that few studies have examined attention and memory biases in previously depressed individuals, particularly with MIs, underscores the need for additional research (Shamai-Leshem et al., 2022). The present study contributes to this literature by examining the effects of a sad MI on both attention and memory biases in a sample of previously depressed individuals.
Whereas some studies have used MIs as a prime, measuring attention or memory biases following the MI (e.g., Kircanski et al., 2013; Vrijsen et al., 2014), MIs can also be employed as an experimental manipulation to evaluate differences in biases in a negative versus neutral mood state. This can be accomplished by using between-subjects designs or within-subjects designs. For example, Newman and Sears (2015) used a between-subjects design, with previously depressed and never depressed women randomly assigned to either a sad or neutral MI group, with attention to emotional images measured using a free-viewing eye-tracking paradigm. They found that never depressed participants in the sad MI group attended to positive images significantly more than never depressed participants in the neutral MI group, whereas for previously depressed participants there was no difference between the sad and neutral MI groups in their attention to positive images. The researchers hypothesized that the never depressed participants’ mood-incongruent attention (i.e., increased attention to positive information while in a sad mood state) reflected a protective mood repair mechanism that was absent or diminished among previously depressed participants and that the lack of this protective attention bias could contribute to relapse vulnerability.
MI studies using a within-subjects design can provide a more direct test of the hypothesis that previously depressed individuals possess a latent cognitive vulnerability that can be activated by negative mood. In these studies, an individual’s attention to emotional stimuli is measured before and after a negative MI, with the pre- versus post-MI differences in the allocation of attention used to index the effects of the induced mood state. The effects of a MI on memory can be assessed by comparing an individual’s recall or recognition of emotional stimuli presented before and after a MI. Within-subjects designs allow for stronger causal inferences and more sensitive tests of the effects of mood on attention and memory, yet few MI studies have used such designs, and none have examined mood-induced changes in both attention and memory in previously depressed individuals. A recent study using a free-viewing eye-tracking task found that a sad MI produced no changes in sustained attention to sad or happy faces in a sample of unselected adults (Hertz-Palmor et al., 2023). Two other studies that also used free-viewing eye-tracking tasks with unselected adult samples observed mood-incongruent increases in attention to positive faces (Sanchez et al., 2014) and images (Speirs et al., 2018) following a sad MI. Sanchez et al. further reported that increased attention to positive faces following the MI predicted mood recovery at the end of the study session, consistent with the affect regulation explanation of mood-incongruent attention to positive information (Nashiro et al., 2012; Reed et al., 2014). These studies did not include previously depressed individuals, however, and thus it was not possible to evaluate whether previously depressed individuals lack the mood-incongruent protective biases observed in these studies. Similarly, studies have shown that non-depressed individuals recall happy memories following a sad MI, which leads to mood repair (Joormann & Siemer, 2004; Josephson, 1996), but these studies did not include previously depressed individuals and thus could not determine whether they lack these mood-incongruent memory biases.
The Present Study
To understand the nature of enduring cognitive vulnerability in remitted depressed states, further studies are needed that compare attention and memory biases in previously depressed individuals in and outside of a negative mood state. In the present study, previously depressed and never depressed women viewed displays of positive, negative, and neutral words for 8-s while their eye movements were tracked and recorded. Following a distraction task, they completed an incidental (unexpected) recognition memory test for the words presented during the free-viewing eye-tracking task. Participants then watched a video to induce a sad mood, followed by a second eye-tracking task, a different distraction task, and an incidental recognition memory test for the words presented during the second eye-tracking task. Given that, as discussed earlier, we assumed that previously depressed participants would naturally vary in their baseline activation of cognitive vulnerability, we did not hypothesize specific differences in attention and memory biases between previously and never depressed participants before the sad MI, while the participants were in their baseline mood state. Our hypotheses were as follows: (1) for previously depressed participants there would be a significant increase in attention and memory biases for negative words after the sad MI (i.e., a within-group difference in biases), consistent with activation of latent cognitive vulnerability and mood-congruent information processing; (2) for never depressed participants there would be a significant increase in attention and memory biases for positive words after the sad MI (a within-group difference in biases), in line with previous findings of mood-incongruent information processing following negative MI in non-depressed and unselected samples (Joormann & Siemer, 2004; Josephson, 1996; Newman & Sears, 2015; Sanchez et al., 2014; Speirs et al., 2018), which are suggestive of a protective mood repair mechanism; (3) in a sad mood state, previously depressed participants would have larger attention and memory biases for negative words relative to never depressed participants (i.e., a between-group difference in biases after the sad MI); and (4) in a sad mood state, previously depressed participants would have smaller attention and memory biases for positive words relative to never depressed participants (i.e., a between-group difference in biases after the sad MI).
Method
Participant Recruitment and Eligibility
The study was reviewed and approved by an institutional research ethics board (REB14-1692). All participants provided informed consent. Details on participant recruitment are reported in Fernandez et al. (2022). 1 Only female participants were recruited, which controlled for potential sex and gender differences in attention and memory for emotional stimuli, as well as differences in emotional responses to the sad MI. Participants were recruited from the community through flyers, advertisements on the university’s research website, a participant database, and an annual women’s show. Prospective participants completed a phone screen interview that included selected modules from the Structured Clinical Interview for the DSM-5 (SCID-5-RV; First et al., 2015) to assess for inclusion and exclusion criteria. Eligible participants were invited for a laboratory visit. The SCID-5-RV was used to assess for past and previous Major Depressive Disorder (MDD) to determine a participant’s group membership. Participants in the previously depressed group met the diagnostic criteria for past, but not current (over the past month) MDD. Participants in the never depressed group had no current or previous history of MDD. General exclusion criteria included the presence of current or previous psychosis, current or previous mania, and current substance use disorder. Participants received a $25.00 (CAN) gift card for their laboratory visit.
Measures
The Structured Clinical Interview for DSM-5 (SCID-5-RV)
The SCID-5-RV (First et al., 2015) is a semi-structured interview that includes diagnostic modules to assess for mental disorders according to criteria outlined in the DSM-5 (APA, 2013). The SCID-5-RV was administered by a doctoral-level clinical psychology student and undergraduate research assistants trained by one of the principal investigators (a registered psychologist). Only the relevant modules to assess for the presence or absence of current and lifetime MDD, psychosis, mania, and substance use were administered.
The Patient Health Questionnaire (PHQ-9)
The PHQ-9 (Spitzer et al., 1999) is a 9-item self-report questionnaire consistent with the DSM-5 diagnostic criteria for depression. The PHQ-9 assesses for depressive symptom severity and functional impairment (e.g., “Over the last 2 weeks, how often have you been bothered by any of the following problems?”). Items are rated from zero (“Not at all”) to three (“Nearly every day”). Total scores range from 0 to 27, where scores of 5–9 indicate minimal symptoms of depression, scores of 10–14 indicate mild depression, scores of 15–19 indicate moderately severe depression, and scores greater than 20 indicate severe depression. The PHQ-9 can be used to assess lifetime history of depression by modifying the item instructions (e.g., “For the 2 weeks in your life that you were the most blue, sad, or depressed, how often were you bothered by any of the following problems?” (PHQ-9L; Cannon et al., 2007). Both the current (PHQ-9) and lifetime (PHQ-9L) versions were used in this study. The PHQ-9 is a reliable and valid measure of depression severity (Kroenke et al., 2001). For the current sample, Cronbach’s alpha was .79 for the PHQ-9 and .95 for the PHQ-9L.
The Beck Depression Inventory-II (BDI-II)
The BDI-II (Beck et al., 1996) was used to assess depressive symptom severity over the past 2 weeks. The BDI-II is a widely used 21-item self-report questionnaire that assesses emotional, physiological, motivational, and cognitive symptoms of depression. Items are rated from zero to three, with higher values corresponding to greater symptom severity. Total scores range from 0 to 63, where scores of 0–13 indicate minimal symptoms of depression, scores of 14–19 indicate mild depression, scores of 20–28 indicate moderately severe depression, and scores of 29–63 indicate severe depression. For the current sample, Cronbach’s alpha was .90.
Mood Ratings
Participant’s moods were assessed at seven different time points during the study, as described in the Procedure section, using a visual analog mood scale (VAMS; Luria, 1975). The VAMS consists of a 100 mm horizontal line with endpoints labeled “very sad” and “very happy”; participants indicated their current mood by placing a dash on the horizontal line. The VAMS was scored from 0 to 100, determined by measuring (in mm) the distance from the left side of the scale (labeled “very sad”) to the participants’ rating. Lower VAMS ratings therefore reflect stronger feelings of sadness.
Demographics Inventory
The demographics inventory included questions about age, ethnicity, marital status, previous episodes of depression, experiences with psychotherapy, and recent changes in mood.
Apparatus for Eye Tracking
Eye movements were recorded using an EyeLink 1000 eye-tracking system (SR Research Ltd., Mississauga, Ontario), which uses infrared video-based tracking technology. The system has a 1000 Hz sampling rate and a temporal resolution of 2 ms. The average gaze error is less than 0.5 degrees of visual angle. Words were shown on a 24-inch LED monitor positioned 60 cm away from the participant. To increase tracking accuracy, participants rested their chin on a chin rest to minimize head movements while they viewed the words. Eye tracking data was processed using the EyeLink Data Viewer analysis software (SR Research, v. 4.4.1) to filter for blinks and other artifacts. The software excluded brief fixations (<100 ms) recorded immediately before and after a blink detection, which excluded blink events from the total fixation time calculation. All other fixations with a duration of less than 100 ms were merged with nearby fixations. The software was used to calculate total fixation times (the sum of all individual fixation durations) for positive, negative, and neutral words for each of the 25 test trials presented before and after the sad MI. Each participant’s mean total fixation times for positive, negative, and neutral words presented before and after the sad MI were used in the calculation of attention biases reported below. Two previously depressed participants were excluded from all analyses due to calibration issues that resulted in poor eye-tracking data.
Eye Tracking Stimuli
The stimuli consisted of 200 words, divided into positive (50 words), negative (50 words), and neutral (100 words) categories. Examples of negative, positive, and neutral words are “inferior,” “thankful,” and “inverted,” respectively. Words were taken from the English Lexicon Project (Balota et al., 2007), which provides measures of printed frequency and other psycholinguistic variables. As described in Fernandez et al. (2022), these words were chosen using valence ratings collected from female undergraduate students prior to the study, who rated words on a scale from +5 (very positive) to −5 (very negative), with 0 representing “neutral.” For the 200 words chosen for this study, the mean valence ratings of the positive, negative, and neutral words were 3.2, −3.3, and 0.3, respectively.
The 200 words were divided into two eye-tracking tasks, one administered while the participant was in a neutral (baseline) mood and the other following the sad MI. Each eye-tracking task consisted of 25 test trials, with each trial consisting of one negative word, one positive word, and two neutral words. There were also ten filler trials consisting of four neutral words. The ten filler trials were included to reduce participants’ expectation that there would be valenced words in each display and to reduce their conspicuousness. The order in which the 35 trials were presented was randomly determined for each participant. The order in which the two sets of 35 trials were presented (before or after the sad MI) was counterbalanced across participants. The four words shown during a trial were randomly allocated to the four quadrants of the display. Reading times for words are affected by word length and printed frequency (Kuperman et al., 2024), and these characteristics will vary among randomly selected words of different valences. To control for such differences, the words in each trial were preselected to be identical in length and similar in printed frequency. To help participants differentiate the words presented in the two eye-tracking tasks for the subsequent memory tests, for one of the eye-tracking tasks the words were presented in a white font on a dark background, and for the other task the words were presented in a yellow font on a dark background (counterbalanced across participants).
Mood Induction Stimuli
The MI procedure used brief video clips to induce a sad mood. Previous research has shown that videos are the most effective MI stimuli in terms of the magnitude and persistence of the mood change created (Kuijsters et al., 2016; Westermann et al., 1996). Two different videos were used. The video “Otto’s Story” (Haldenwang, 2012; 7 min 57 s in duration), which narrates the story of a young boy who dies of brain cancer, was shown before the second eye-tracking task. This video has been used in two previous studies and was shown to successfully induce a sad mood in approximately 80% of participants (Frayn et al., 2016; Speirs et al., 2018). The second video, “Ol’ Boy” (Siew, 2013; 6 min 48 s in duration), which documents the story of an animal shelter’s unsuccessful attempt to save an abandoned and malnourished dog, was shown immediately after the second eye-tracking task. This video was used by Speirs et al. (2018) and successfully induced a sad mood in approximately 60% of participants. The first video was shown to participants to induce a sad mood before the second eye-tracking task; the second video was shown after the second eye-tracking task as a “booster” to prolong the feelings of sadness so that participants would still be experiencing sadness during the second recognition memory test.
Recognition Memory Tests
Participants completed two recognition memory tests: the first after the first eye-tracking task (before the sad MI) and the second after the second eye-tracking task (after the sad MI). A recognition test was used, as opposed to a recall test, because recall tests carry a greater cognitive load with respect to the retrieval of information and are thus more susceptible to the influence of motivation and executive functioning ability (Howe & Malone, 2011). Participants were not previously informed about either test so that they were unexpected. For both tests, participants viewed words one at a time on a computer display and selected a response option corresponding to their memory of the word: “sure old,” “guess old,” “sure new,” or “guess new” (similar to the procedure used by Roediger & McDermott, 1995). These options capture recollection- and familiarity-based retrieval processes (Tulving, 1985), which both contribute to performance on recognition memory tests (Yonelinas et al., 2010). The “sure old” and “sure new” response options captured recollection-based retrieval or “remembering,” whereas the “guess old” and “guess new” response options captured familiarity-based retrieval or “knowing” in the absence of conscious recollection. Correct recognitions were defined as the sum of “sure old” and “guess old” responses to old words to incorporate both types of retrieval.
Each recognition memory test included all the negative and positive words presented during the preceding eye-tracking task (25 positive words and 25 negative words) and half of the neutral words (25 words, which were preselected). These were the “old” words. In addition, 75 “new” words (25 positive, 25 negative, and 25 neutral words) that were not shown during the eye-tracking task were included in each memory test. The new words were matched with the old words for printed frequency, word length, and valence to increase the difficulty of the task. The order in which the old and new words were presented was randomized for each participant.
Computation of Attention and Memory Biases
Attention and memory bias indices were computed for each participant and used as dependent variables in the analyses reported below. We computed these indices in the same manner as Koster et al. (2010) and Fernandez et al. (2022). For the attention biases, a bias was defined as the mean difference in total fixation time between positive/negative words and neutral words (as there were two neutral words presented on each trial, the mean total fixation time for neutral words was based on the total fixation times to both neutral words). An attention bias greater than zero indicated that, on average, a participant attended to positive/negative words more than neutral words during the 8-s presentations, whereas a bias less than zero indicated that positive/negative words were attended to less than neutral words. Table 3 shows the mean attention biases for positive and negative words for never depressed and previously depressed participants before and after the sad MI.
Each participant’s correct recognition data was used to calculate a memory bias index. The bias for positive words was calculated as the difference (in %) between the percentage of correct recognitions for positive words (the sum of correct “sure old” and “guess old” responses) and the percentage of correct recognitions for neutral words. Thus, a bias greater than zero indicated that a participant had better recognition for positive words than neutral words, whereas a bias less than zero indicated that a participant had poorer recognition for positive words than neutral words. Memory biases for negative words were calculated as the difference in correct recognition between negative and neutral words and interpreted in the same manner. Memory biases were calculated for positive and negative words shown before and after the sad MI. 2
Procedure
Participants were provided with written and spoken instructions at the beginning of the lab session. Figure 1 shows an outline of the procedure. Participants began by completing the demographics inventory and rating their current mood using the VAMS (Time 1 mood rating). After a brief calibration procedure, participants began the first eye-tracking task. The eye-tracking task began with two practice trials to familiarize participants with the displays and procedure. These were followed by 35 trials (25 test trials and 10 filler trials) presented in a random order. Participants fixated on a white dot in the center of the display to ensure that their gaze was focused at the same location before the start of each trial; the display of words was triggered after a stable 3-s fixation was registered at this center location. Each display of four words was presented for 8 seconds. Participants were instructed to view the words in any order they wished (a free-viewing paradigm) and their eye gaze was tracked and recorded throughout the 8-s presentation. Participants were not informed that their memory for the words would be tested later. Overview of Study Procedure
After participants finished the first eye-tracking task they were asked to complete a 7-min distraction task, which involved watching an instructional video (how to change the brakes in a car). Participants were instructed to pay close attention to the video because they would be tested on the material later in the session. Following this distraction task, participants completed the first recognition memory test. Participants then completed another distraction task (Raven’s Matrices; Raven, 1958) for 12 min. This task was intended to reduce participants’ memory of the words in the first eye-tracking displays. After the second distraction task was completed, participants were told that the first half of the lab visit was finished and that the second half of the visit would be similar to the first (they would complete an eye-tracking task and watch a video); however, they were told that their memory for the words shown during the eye-tracking task would not be tested and that instead their memory for the instructional video would be tested. These directions were intended to prevent participants from anticipating a memory test for the words shown during the second eye-tracking task.
Participants then completed their Time 2 mood rating and watched the first sad video (“Otto’s Story”; Haldenwang, 2012). Participants were instructed to imagine themselves in a similar situation and to allow themselves to feel any emotions that arose. After they watched the video, they rated their mood again (Time 3 rating). Participants then completed the second eye-tracking task and rated their mood again (Time 4 rating). Participants then watched the second sad video (“Ol’ Boy”; Siew, 2013). After watching the second sad video they rated their mood again (Time 5 rating) and then completed the second recognition memory test (for the words presented during the second eye-tracking task). After the memory test, participants rated their mood again (Time 6 rating), watched a positive film clip (a comedic scene from the movie When Harry Met Sally; Reiner, 1989), and rated their mood a final time (Time 7 rating). At the end of the session participants were asked whether they expected the second recognition memory test and rated their expectation using a scale from 0 (I did not expect the memory test) to 3 (I expected the memory test). Few participants (7.6%) expected the second memory test, and sensitivity analyses indicated that the results were unchanged when these participants’ data were excluded. The total participation time was between 90 and 120 min.
Participant Characteristics
Given that the study design was based on the premise that latent attention and memory biases would be activated only when participants were in a dysphoric mood state, the analyses included only the participants who were successfully mood-induced. Excluding participants who were not mood-induced also increased confidence that post-MI changes in attention and memory biases were due to the sad MI (Rottenberg et al., 2018). A successful sad MI was defined as at least a 20% decrease in the VAMS ratings from pre- to post-MI (Time 2 vs. Time 3). Of the 48 never depressed participants, 34 were successfully mood induced (72.9%), and of the 57 previously depressed participants, 45 were successfully mood induced (82.4%), χ2(1) = 0.92, p = .337. Statistical power analyses indicated that this sample of 79 mood-induced participants (34 never depressed and 45 previously depressed) was sufficient to detect within-group and between-group differences in attention and memory biases. 3
Participant Characteristics and Psychological Measures for the Never Depressed and Previously Depressed Groups

Note. BDI-II = Beck Depression Inventory-II scores. PHQ-9 = Patient Health Questionnaire-9 scores. PHQ-9 Current = percentage of participants classified as depressed based on Patient Health Questionnaire-9 scores. PHQ-9 Lifetime = percentage of participants classified as having been previously depressed based on Patient Health Questionnaire-9 Lifetime scores. Standard deviations in parentheses. ES = effect size; Cohen’s d for t-tests and Phi coefficient for chi-square tests.
Results
Statistical analyses were carried out using the Statistical Package for the Social Sciences (SPSS, version 29; IBM Corp, 2023). An alpha level of 5% was used for all statistical tests unless otherwise noted.
Mood Rating Data
VAMS Mood Ratings for Never Depressed and Previously Depressed Participants
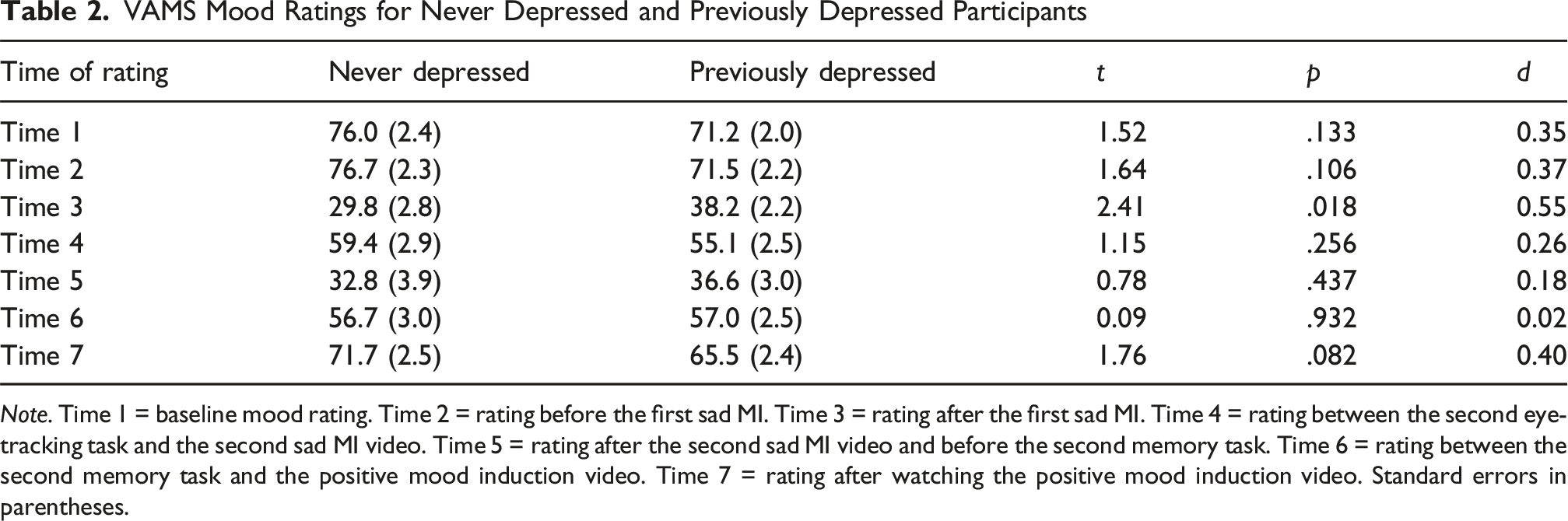
Note. Time 1 = baseline mood rating. Time 2 = rating before the first sad MI. Time 3 = rating after the first sad MI. Time 4 = rating between the second eye-tracking task and the second sad MI video. Time 5 = rating after the second sad MI video and before the second memory task. Time 6 = rating between the second memory task and the positive mood induction video. Time 7 = rating after watching the positive mood induction video. Standard errors in parentheses.
The main effect of depression group was not significant, F(1, 77) = 0.22, p = .641, partial η2 = .00, but there was a significant interaction between depression group and mood rating time, F(6, 462) = 3.33, p = .003, partial η2 = .04. We used independent samples t-tests to test for between-group differences in the mood ratings (using an alpha of 5% to reduce the Type II error rate, given that we did not want to overlook a genuine group difference in the VAMS ratings). These indicated that the groups differed only in their Time 3 mood ratings (after the first sad MI); specifically, never depressed participants had lower mood ratings (M = 29.8) than previously depressed participants (M = 38.2) at Time 3, t(77) = 2.41, p = .018, d = 0.55. This suggests that the first sad MI was more effective for never depressed participants, producing a larger decrease in mood. This was confirmed by comparing the percentage decrease in VAMS ratings between Time 2 and Time 3. For never depressed participants the mean VAMS percentage change was −58.7% (SD = 23.3), whereas for previously depressed participants the mean percentage change was −45.8% (SD = 19.5), t(77) = 2.67, p = .009, d = 0.61. Larger decreases in mood were expected to lead to larger changes in attention and memory biases, and to take this group difference into account we used analysis of covariance (ANCOVA) when comparing never depressed and previously depressed participant’s post-MI attention and memory biases, controlling for VAMS percentage change.
Within-Group Comparisons of Attention Biases
Positive and Negative Attention Biases (in ms) and Positive and Negative Memory Biases (in %), Before and After the Sad Mood Induction
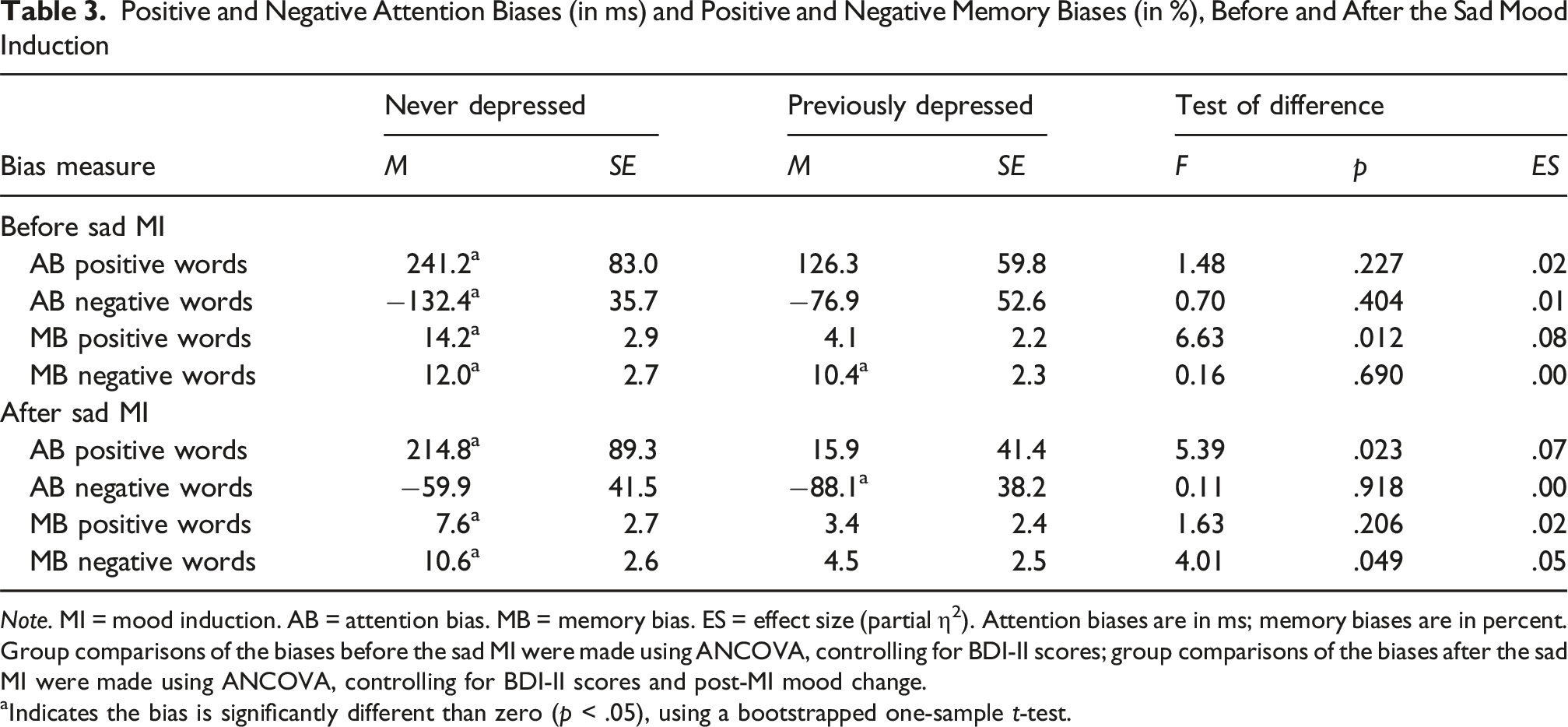
Note. MI = mood induction. AB = attention bias. MB = memory bias. ES = effect size (partial η2). Attention biases are in ms; memory biases are in percent. Group comparisons of the biases before the sad MI were made using ANCOVA, controlling for BDI-II scores; group comparisons of the biases after the sad MI were made using ANCOVA, controlling for BDI-II scores and post-MI mood change.
aIndicates the bias is significantly different than zero (p < .05), using a bootstrapped one-sample t-test.
For never depressed participants, there was a significant attention bias for positive words before the sad MI (241.2 ms), t(33) = 2.91, p = .016, d = 0.50, and after the sad MI (214.8 ms), t(33) = 2.41, p = .047, d = 0.41, and these biases did not differ from each other, F(1, 32) = 0.01, p = .960, partial η2 = .001. These biases were greater than zero, which indicated that never depressed participants attended to positive words more than neutral words before and after the MI. For negative words, never depressed participants had a significant attention bias before the sad MI (−132.4 ms), t(33) = 3.71, p < .001, d = 0.64, but not after the sad MI (−59.9 ms), t(33) = 1.44, p = .159, d = 0.25. However, these biases did not differ from each other, F(1, 32) = 2.69, p = .111, partial η2 = .08. 4 The bias for negative words before the sad MI was less than zero, which indicated that never depressed participants attended to negative words less than neutral words.
For previously depressed participants, there was no attention bias for positive words before the sad MI (126.3 ms), t(44) = 2.11, p = .070, d = 0.32, or after the sad MI (15.9 ms), t(44) = 0.39, p = .706, d = 0.06, and these biases did not differ significantly, F(1, 43) = 1.09, p = .302, partial η2 = .03. Thus, unlike never depressed participants, previously depressed participants did not attend to positive words more than neutral words either before or after the sad MI. For negative words, there was no attention bias before the sad MI (−76.9 ms), t(44) = 1.46, p = .164, d = 0.22, whereas there was a significant bias after the sad MI (−88.1 ms), t(44) = 2.30, p = .035, d = 0.34. However, these biases did not differ, F(1, 43) = 1.21, p = .278, partial η2 = .03. The bias for negative words after the sad MI was less than zero, which indicated that previously depressed participants attended to negative words less than neutral words.
Within-Group Comparisons of Memory Biases
The mean memory biases for positive and negative words are listed in Table 3 and were analyzed in the same manner as the attention biases. For never depressed participants, there was a bias for positive words before the MI (14.2%), t(33) = 4.85, p < .001, d = 0.83, and after the MI (7.6%), t(33) = 2.84, p = .008, d = 0.49, and these biases did not differ significantly, F(1, 32) = 2.98, p = .094, partial η2 = .09. The biases were greater than zero, which indicated that never depressed participants had better recognition for positive words than neutral words, both before and after the MI. For negative words there was also a bias before the MI (12.0%), t(33) = 4.52, p < .001, d = 0.78, and after the MI (10.6%), t(33) = 4.14, p < .001, d = 0.71, which did not differ significantly, F(1, 32) = 0.53, p = .474, partial η2 = .02. Thus, never depressed participants also had better recognition for negative words than neutral words before and after the MI.
For previously depressed participants, there was no memory bias for positive words before the MI (4.1%), t(44) = 1.88, p = .067, d = 0.28, or after the MI (3.4%), t(44) = 1.41, p = .166, d = 0.21, and no significant difference between these biases, F(1, 43) = 1.08, p = .304, partial η2 = .03. Thus, unlike never depressed participants, previously depressed participants did not have better recognition for positive words than neutral words. For negative words, there was a bias before the MI (10.4%), t(44) = 4.45, p < .001, d = 0.66, but not after the MI (4.5%), t(44) = 1.81, p = .077, d = 0.27, and these biases differed significantly, F(1, 43) = 5.05, p = .030, partial η2 = .11. The bias for negative words before the sad MI was greater than zero, which indicated that previously depressed participants had better recognition for negative words than neutral words.
Between-Group Comparisons of Attention and Memory Biases
Between-group comparisons of the attention and memory biases before the sad MI were conducted using ANCOVA, controlling for BDI-II scores, given that the groups differed in their BDI-II scores. As shown in Table 3, never depressed and previously depressed participants did not differ significantly in their attention biases for positive or negative words. There was no group difference in the memory biases for negative words, whereas the groups did differ in their memory biases for positive words, F(1, 76) = 6.63, p = .012, partial η2 = .08. Never depressed participants had a significantly larger memory bias for positive words than previously depressed participants before the sad MI (14.2% vs. 4.1%, respectively).
Table 3 also shows group comparisons of the attention and memory biases after the sad MI. These biases were compared using ANCOVA, controlling for BDI-II scores and VAMS percentage change (as the MI was more effective for never depressed participants). The groups differed in their attention biases for positive words, with never depressed participants having a significantly larger bias (214.8 ms) than previously depressed participants (15.9 ms) after the MI, F(1, 75) = 5.39, p = .023, partial η2 = .07. There was no group difference in the attention biases for negative words. Comparisons of the memory biases showed that the groups did not differ in their biases for positive words, whereas for negative words never depressed participants had a significantly larger bias than previously depressed participants after the sad MI (10.6% vs. 4.5%), F(1, 75) = 4.01, p = .049, partial η2 = .05.
Moderation of Attention and Memory Biases by MI Efficacy
An alternative approach to analyzing the post-MI biases is to examine how the attention and memory biases were affected by the efficacy of the sad MI, instead of controlling for these differences via ANCOVA. To do so, we conducted multiple regression analyses, in which the post-MI bias was the dependent variable and depression group (never depressed, previously depressed) was the categorical predictor variable. Mean-centered values for percentage VAMS change (pre- to post-MI) was the moderator variable, and BDI-II scores were used as a covariate to control for the group difference in these scores. The key statistical test was the interaction between depression group and percentage VAMS change: a significant interaction would indicate that the effect of mood change on a bias was not the same for never depressed and previously depressed participants. These analyses were carried out using PROCESS (version 4.3 for SPSS; Hayes, 2022), which provides follow-up tests of significant moderation effects.
Analyzing the post-MI attention and memory biases in this fashion revealed one significant interaction between depression group and percentage VAMS change. Specifically, in the analysis of the attention biases for positive words, the overall regression model was significant, R = .36, F(4, 74) = 2.72, p = .036, accounting for 12.8% of the variance, and the interaction was significant, F(1, 74) = 5.08, p = .027, accounting for 6.0% of the variance. The nature of this interaction can be seen in Figure 2, which shows the association between attention biases for positive words and percentage VAMS change, across three different levels of VAMS change (at the mean, −51%; one SD below the mean, −29%; and one SD above the mean, −73%), with larger percentages reflecting larger shifts in mood post-MI, for never depressed and previously depressed participants. For never depressed participants, larger VAMS percentage changes post-MI were negatively associated with attention biases, t(33) = 2.20, p = .031. That is, for never depressed participants who were more affected by the sad MI, attention biases for positive words were smaller, which suggests that larger shifts in mood were associated with decreases in attention to positive words (relative to neutral words) post-MI (a mood-congruent effect). In contrast, for previously depressed participants, equivalent shifts in mood were not associated with decreases in attention to positive words post-MI, as there was no association between VAMS percentage change and attention bias for positive words, t(44) = 1.02, p = .312. This outcome indicates that, unlike never depressed participants, previously depressed participants’ attention to positive words was not affected by the degree of mood change experienced after the sad MI. Association Between Attention Biases for Positive Words and Percentage VAMS Change for Never Depressed and Previously Depressed Participants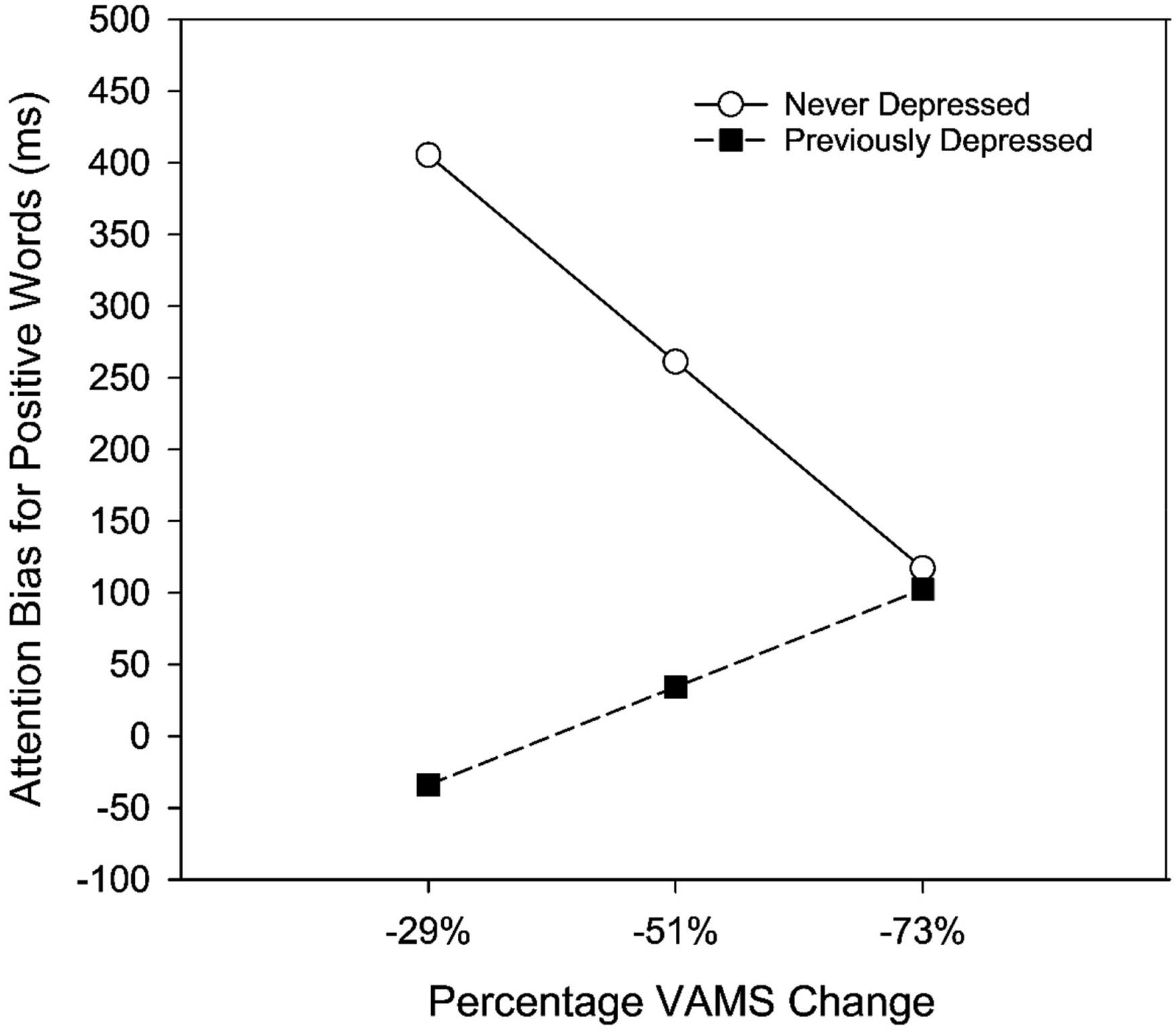
Discussion
A core tenet of cognitive models of depression is that a latent cognitive vulnerability persists following the remission of depression and can be reactivated by stress or negative mood, leading to negatively biased information processing. To evaluate this assumption, we assessed attention and memory biases in previously depressed and never depressed individuals before and after a sad MI. Contrary to the study hypotheses, previously depressed participants did not show an increase in attention and memory biases for negative words when in a sad mood state relative to baseline, as would be expected due to activation of cognitive vulnerability. Instead, previously depressed participants had smaller memory biases for negative words when in a sad mood state compared to baseline and exhibited no changes on any other bias measure. Also contrary to hypotheses, never depressed participants did not show an increase in attention and memory biases for positive words following the sad MI, as would be expected due to a protective mood repair mechanism. Instead, never depressed participants exhibited biases in attention and memory favoring positive over neutral words both before and after the sad MI, suggesting a maintenance of positive biases in a sad mood state. However, never depressed participants who were more affected by the sad MI had smaller attention biases for positive words after the MI (a mood-congruent effect). The hypothesized group differences in attention and memory biases between previously and never depressed participants following the MI were only weakly supported. As hypothesized, when in a sad mood state, previously depressed participants had significantly smaller attention biases for positive words compared to never depressed participants. However, contrary to hypotheses, there was no group difference in attention biases for negative words or in memory biases for positive words following the MI, and previously depressed participants had smaller (not larger) memory biases for negative words than never depressed participants following the MI. Thus, while the results revealed differences between previously depressed and never depressed participants in their pre- and post-MI biases and in the way those biases were affected by the MI, the pattern of findings is more complicated than anticipated.
Within-Group Differences in Attention and Memory Biases
Never depressed participants exhibited attention and memory biases that favored positive over neutral words, and these biases were similar in magnitude both before and after the sad MI. Thus, although never depressed participants did not show the hypothesized increase in positive attention and memory biases in a sad mood state, they did have positive biases overall that were maintained in a sad mood state. In contrast, previously depressed participants did not attend more to positive words or have better memory for positive words, relative to neutral words, either before or after the MI. A similar pattern of findings has been observed in previous studies comparing non-depressed and depression-vulnerable (both currently depressed and previously depressed) samples and is thought to reflect the existence of protective biases among non-depressed individuals and the lack of such protective biases among depression-vulnerable individuals (Gotlib et al., 1988; Li et al., 2016; McCabe & Gotlib, 1995; Newman et al., 2019; Soltani et al., 2015). Additional support for this idea comes from a study by Thoern et al. (2016), which found that larger attentional biases for happy faces were associated with higher resilience to stress in a nonclinical sample. Thus, our findings are consistent with the existence of general protective biases among never depressed individuals that favor the processing of positive stimuli regardless of mood state, rather than a specific mood repair mechanism.
Our hypothesis of mood-incongruent effects on attention and memory biases among the never depressed participants was based on the findings of previous studies that induced negative mood states. For example, both Newman and Sears (2015) and Speirs et al. (2018) found that non-depressed individuals increased their attention to positive images after experiencing a sad MI (as did Isaacowitz et al., 2008, although only for their group of older adults). The critical difference between these previous studies and the present one is likely the use of images as stimuli. With images, a participant can increase their attention to positive images (images of smiling babies, happy couples, friendly dogs, etc.) after a sad MI in an effort to repair their mood. By contrast, increasing attention to positive words is probably much less effective at counteracting a sad mood than increasing attention to positive images given the greater intensity and potency of emotional information in images (e.g., Bayer & Schacht, 2014; Beall & Herbert, 2008). Although the use of positive words as stimuli may have eliminated a mood-incongruent effect on attention among never depressed participants, the maintenance of attention on positive words following the sad MI may still reflect an adaptive bias with benefits for mood repair, a bias that was absent among previously depressed participants.
Similarly, although the never depressed participants did not show an increase in positive memory biases when in a sad mood compared to baseline, they had positive memory biases (i.e., superior memory for positive words compared to neutral words) both before and after the sad MI. This contrasts with the previously depressed participants, who had similar memory for positive and neutral words (i.e., no positive memory bias) both before and after the sad MI. A few studies have found that non-depressed participants tend to recall happy autobiographical memories when induced to feel a sad mood, and that recall of positive memories leads to mood repair (Joormann & Siemer, 2004; Josephson, 1996). As we suggest above regarding attention to positive words, recalling positive words is likely a less natural and effective strategy for repairing negative mood than recalling happy autobiographical memories. Future studies should compare cued recall of autobiographical memories following a sad MI in never depressed and previously depressed individuals. Overall, the consistent group differences in positive attention and memory biases both before and after the sad MI are consistent with the hypothesis that the absence of protective cognitive biases among previously depressed individuals may contribute to relapse vulnerability (Armstrong & Olatunji, 2012; Duque & Vázquez, 2015).
While the never depressed participants generally maintained their positive attention biases in the sad mood state, there was a significant inverse association between the extent of mood change from pre- to post-MI and attention biases for positive words following the MI (Figure 2). That is, never depressed participants who experienced larger shifts in mood (i.e., for whom the sad MI was more effective) had smaller attention biases for positive words after the sad MI. This was the case for the never depressed participants only; for the previously depressed participants the extent of mood change was unrelated to post-MI attention biases. This outcome suggests that strong negative mood states can diminish the positive attention bias typically observed in never depressed individuals. Although this finding was not hypothesized, it makes sense that mood-incongruent (i.e., positive) cognitive biases may not be adaptive in highly negative mood states. Thus, it may be that non-depressed individuals have positive biases in euthymic and milder negative mood states but mood-congruent biases in stronger negative mood states. While our results provide preliminary evidence that intensity of mood may moderate the effects of induced mood states on attention biases, experimental manipulations of mood intensity would provide stronger evidence. Future studies should investigate the effects of negative mood states of varying intensity on attention and memory biases for emotional stimuli, and in turn, the association between such biases and the extent of mood repair, among both healthy and depression-vulnerable individuals. Such studies could be conducted using laboratory MI procedures or in response to naturally occurring stressors.
While never depressed participants exhibited significant memory biases favoring both positive and negative words at baseline, previously depressed participants exhibited significant memory biases only for negative words at baseline. Nevertheless, these results are largely consistent with previous research that shows that unselected samples have enhanced memory for emotional versus neutral stimuli (e.g., Adelman & Estes, 2013; Kousta et al., 2009; Monkman et al., 2025; Ridout et al., 2003; see Murphy & Isaacowitz, 2008, for a review). It has been suggested that superior memory for emotionally salient (and negative, especially) events has evolutionary benefits and may be mediated by involvement of the amygdala (Buchanan & Adolphs, 2002). It is notable that never depressed and previously depressed participants had similar memory biases for negative words at baseline (12.0% vs. 10.4%). which makes the large difference in their memory biases for positive words (14.2% vs. 4.1%) all the more conspicious.
Between-Group Differences in Attention and Memory Biases
In a baseline mood state, previously depressed participants had a significantly smaller memory bias for positive words, but a similar memory bias for negative words compared to never depressed participants. For attention biases, the comparisons between the never depressed and previously depressed groups at baseline indicated small but non-significant differences for positive and negative words (partial η2 = .02 and .01, respectively). Thus, the attention biases favoring positive words and disfavoring negative words were weaker (non-significantly) for previously depressed participants compared to never depressed participants. Recall that we did not hypothesize significant differences between the groups at baseline, given that we expected natural variability in the extent to which cognitive vulnerability would be activated among previously depressed individuals in a baseline mood state. Nonetheless, activation or partial activation of cognitive vulnerability among at least a subset of the previously depressed sample may have led to these small and inconsistent group differences in attention and memory biases at baseline.
In a sad mood state, previously depressed participants had significantly smaller attention biases for positive words and significantly smaller memory biases for negative words compared to never depressed participants. The smaller attention biases for positive words among previously depressed individuals aligned with the study hypotheses. As noted earlier, never depressed participants maintained preferential attention to positive words in a sad mood state, whereas for previously depressed participants there was a tendency to decrease their attention to positive words in a sad mood state. Thus, although never depressed participants had an attention bias favoring positive over neutral words before and after the MI, and previously depressed participants had no attention bias for positive words before or after the MI, the between-groups difference was only large enough to be statistically significant in the sad mood state. Thus, these results are partially consistent with Beck’s (1967) theory that cognitive vulnerability may be reactivated among remitted depressed individuals by negative mood states, leading to depressogenic information processing. On the other hand, it is unclear why memory biases for negative words were smaller following the MI compared to baseline for previously depressed participants. One possibility is that the MI was not sufficiently potent to activate cognitive vulnerability in the previously depressed participants, a possibility that is consistent with the overall weak support for the hypothesized mood-congruent biases among the previously depressed participants in the sad mood state in this study. If their cognitive vulnerability was not sufficiently activated, the reduced memory biases for negative words exhibited by previously depressed participants in the sad mood state may have functioned as an adaptive mood repair mechanism consistent with their euthymic state. However, given that this finding was unexpected and contrary to hypotheses, we are cautious in proposing potential explanations until it is replicated in future research.
Study Strengths, Limitations, Challenges, and Directions for Future Research
One distinguishing feature of the present study is the use of word stimuli to measure attention and memory biases, which is both a strength and a limitation. Previous studies of attention biases, including those with previously depressed samples, have typically used face images and naturalistic images that include people (see Shamai-Leshem et al., 2022, for a review). Such stimuli implicate social information processing, which may be influenced not only by depression but also by social anxiety, a common comorbidity of depression (Heinrichs & Hofmann, 2001; LeMoult & Joormann, 2012). Word stimuli are less influenced by social processes and therefore have an advantage over image stimuli in the study of depression-specific biases. Word stimuli are also easier to match on multiple dimensions (printed frequency, length, valence, color, brightness) and can therefore enhance experimental control. On the other hand, words have many other dimensions to consider when matching; for example, many words have more than one meaning (e.g., bank, stamp, and fair), and the meanings can be of different valences (e.g., date, pass, club, and battery). Semantic ambiguity can affect reading times (Haro & Ferré, 2018; Piercey & Joordens, 2000; Siakaluk et al., 2007) and should be controlled when using word stimuli, as it was in our study. In addition, as noted, words are less potent emotional stimuli relative to images (Bayer & Schacht, 2014; Beall & Herbert, 2008), which likely reduces the magnitude of attention biases that can be observed and limits the effectiveness of using attention to counteract an induced sad mood.
Another strength of this study is the measurement of attention and memory biases before and after the sad MI to permit direct testing of changes in biases in both previously depressed and never depressed groups separately, in addition to testing for between-group differences in biases at baseline and following the MI. Moreover, we evaluated the success of the sad MI across participants, and for the statistical analyses we included only those who met an a priori definition of success (i.e., a minimum 20% decrease in VAMS ratings pre- to post-MI). This analytic decision was important given the evidence that a substantial percentage of individuals do not respond to MI procedures (Gillies & Dozois, 2021), as well as the observation that non-response rates can differ between clinical groups (Rottenberg et al., 2018). Examination of the success of the sad MI across participants also allowed us to control for the extent of mood change in the analyses and, separately, to test the extent of mood change as a moderator of the between-group differences in post-MI biases. These design and analytic features increased the statistical conclusion validity of the study, as we were able to conduct a more direct and specific test of the effect of induced sad mood on attention and memory biases among previously depressed and never depressed individuals.
A limitation of the study is that some participants may have expected the second memory test and, if so, they may have attended to the words presented after the sad MI differently than participants who did not have this expectation. We employed several design features to prevent and evaluate this possibility. Specifically, participants were told that they would not have their memory tested for the words shown during the second eye-tracking task and would instead have their memory tested for the instructional video that they watched earlier in the session. At the end of the study, participants were also asked to rate the extent to which they expected the second memory test, and these ratings indicated that few participants (7.6%) expected the second memory test. In addition, as noted, the results were similar when these participants were included or excluded from the analyses. Nonetheless, it is possible that some participants may have expected the second memory test and failed to report this, whether due to reporting bias or lack of conscious awareness of their expectations. Of course, one could employ a fully between-groups design to eliminate this possibility (i.e., random assignment to either the neutral or sad MI, with only one assessment of attention and memory biases), but this would also eliminate many of the advantages of the within-subjects MI design.
Another challenge already noted is the potential variation in the level of cognitive vulnerability among previously depressed participants and in the extent to which that vulnerability was activated at baseline. Previously depressed samples are heterogeneous with respect to various clinical characteristics, including number of prior depressive episodes, duration of remission, and severity of residual symptoms, and this heterogeneity may reflect and/or influence heterogeneity in cognitive vulnerability. We did not have experimental control over participants’ baseline mood state. Thus, there was likely natural variation in participants’ mood states when they entered the study, as well as in their experience of recent stressors or negative life events. Differential activation of cognitive vulnerability among the previously depressed sample at baseline may have obscured some of the effects of the sad MI on biases, as well as affected comparisons between the previously depressed and never depressed groups at baseline. We attempted to mitigate this issue by controlling for depression symptom severity (BDI-II scores) in the analyses. Future studies may alternatively address this issue by using additional eligibility criteria (e.g., minimal depression symptoms, specific range of remission duration, absence of recent stress) to recruit more homogeneous previously depressed samples. Of course, most any strategy to reduce variability in the level and activation of cognitive vulnerability among previously depressed individuals would also limit the generalizability of the study findings.
Although the study sample size was adequately powered to detect medium effects (and was larger than the sample sizes of most studies that have examined the effects of a MI on attention and/or memory biases in previously depressed samples; see Everaert et al., 2022; Shamai-Leshem et al., 2022, for reviews), it is possible that some of the null effects observed were due to inadequate power. For example, previously depressed participants had smaller attention biases for positive words after the sad MI compared to before the MI (d = .26), and although this difference was not statistically significant, the direction of the effect was consistent with the hypothesis that previously depressed participants would attend less to positive stimuli when in a sad mood state. The previously depressed sample was adequately powered to detect effects slightly smaller than medium-sized within-group differences (d = 0.43 or larger). However, it is possible that for previously depressed individuals, changes in attention biases due to induced sadness are genuinely small effects (∼d = .20), particularly when using word stimuli, in which case much larger samples would be required to detect such effects. Moreover, limitations of laboratory-based MI procedures could contribute to this dilemma. Typical laboratory-based MIs produce effects on mood that are limited in potency and duration (Gillies & Dozois, 2021). We attempted to mitigate this issue by using video clips for MI stimuli and by including only participants in the analyses for whom the MI was effective. Nonetheless, the effects of a laboratory-based MI on attention and memory biases among previously depressed individuals will typically be far less potent than the effects of naturally occurring sad moods and real-life stressors. Our MI may not have produced a strong enough sad mood to activate cognitive vulnerability among the previously depressed participants, which could account for the weak evidence of mood-congruent changes in their biases as well as the unexpected mood-incongruent change in their memory biases for negative words.
To address these issues, future studies could employ alternative sad MI procedures designed to produce larger and/or longer-lasting effects (e.g., recall of sad memories; Gillies & Dozois, 2021), strategies to boost or prolong MI effects during the measurement of biases (e.g., interspersing or incorporating MI stimuli into the attention and memory tasks), and observational research designs to examine the effect of naturally occurring life stress on attention and memory biases. Longitudinal research designs that follow previously depressed participants over time would provide a strong test of attention and memory biases as risk factors for relapse (e.g., Beevers & Carver, 2003; Newman et al., 2019; Ruhe et al., 2019; Woody et al., 2016). Biases, life stress, and depression symptoms could be assessed repeatedly to examine whether depressogenic attention and memory biases covary with life stress, consistent with activation of cognitive vulnerability, and whether stress-activated biases predict increased likelihood of relapse.
Finally, the decision to recruit a female sample was based on sex and gender differences reported in the depression literature (e.g., general prevalence, etiology, and course), as well as differences in the processing of emotional stimuli (Donges et al., 2012; Kessler et al., 1993; Montagne et al., 2005; Piccinelli & Wilkinson, 2000). This decision limited the generalizability of the results but eliminated variability in the attention and memory data due to sex and gender differences related to cognition in depression. Recruiting an all-female sample also eliminated potential sex and gender differences in emotional responses to the sad MI (e.g., Fernández et al., 2012; Schaefer et al., 2010). Despite these advantages, future studies should aim to recruit mixed-gender samples when investigating attention and memory biases in remitted depression, because sex and gender may be important moderators of the extent to which cognitive vulnerability is activated by stress or negative mood.
Conclusions
This study evaluated the diathesis-stress component of Beck’s (1967) cognitive model of depression through an experimental test of a sad MI on attention and memory biases in previously depressed and never depressed individuals. The results did not support the hypothesis that previously depressed participants would have larger attention and memory biases for negative words and smaller attention and memory biases for positive words in a sad mood state compared to a baseline mood state. Instead, previously depressed participants had a smaller memory bias for negative words post-MI and no significant changes on the other bias measures. However, previously depressed participants did show a non-significant reduction in attention biases for positive words from pre- to post-MI, consistent with the hypothesized direction of effect. In general, never depressed participants exhibited protective attention and memory biases that favored positive stimuli and disfavored negative stimuli relative to neutral stimuli in both a baseline and a sad mood state. In contrast, previously depressed participants generally lacked these protective biases and, compared to never depressed participants, had significantly smaller memory biases for positive words in a baseline mood state and significantly smaller attention biases for positive words in a sad mood state. Overall, the pattern of effects is generally supportive of the notion that cognitive vulnerability is maintained, perhaps in an attenuated form, following remission from depression, and can be influenced by negative mood. Future research that employs larger sample sizes powered to detect small effects, more potent MI procedures, and naturalistic longitudinal designs will be necessary to further elucidate the role of attention and memory biases in maintaining vulnerability to depression in previously depressed samples.
Footnotes
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by research grants from the Canadian Institutes of Health Research (grant number MOP-136988-2014) and the Natural Sciences and Engineering Research Council of Canada (grant number RGPIN 04326-2018).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
