Abstract
The overlap of Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) and Stevens-Johnson syndrome (SJS) caused by antituberculosis drugs represents an extremely rare event. This situation can manifest between 2 and 8 weeks after the first exposure to the medication. The overlap of these conditions can lead to atypical clinical manifestations, thus complicating the early diagnosis and the implementation of early treatment. This report describes the case of a patient who developed the DRESS/SJS overlap 35 days after starting antituberculosis treatment. The patient experienced severe skin and systemic involvement, a situation that required her admission and monitoring in the intensive care unit. From our experience with this case, we conclude the importance of an accurate and timely diagnosis using validated scoring systems such as RegiSCAR to confirm the clinical diagnosis of DRESS/SJS and ALDEN to assess the likelihood of drug causality. Timely intervention with corticosteroids plays a key role in moderating the exaggerated immune response, helping to alleviate dermatological symptoms and prevent long-term organ damage. In addition, the availability of safe therapeutic alternatives for tuberculosis treatment allows for more effective and safer management in these patients.
Plain language summary
Why are we talking about this? When a person starts tuberculosis treatment with certain medications, there is a small chance they could develop two serious skin conditions at the same time: DRESS syndrome and Stevens-Johnson syndrome (SJS). Although extremely rare, these conditions can be very dangerous and challenging to manage, especially if not identified early.
What happened in this case? In this report, we present the case of a patient who developed both conditions about a month after starting tuberculosis treatment. These problems severely affected the patient’s skin and also caused damage to other organs, requiring intensive care in the hospital.
What did we learn from this case? This case highlights the importance of making an early and accurate diagnosis. Tools like the RegiSCAR and ALDEN scoring systems are very helpful for quickly identifying these reactions. We also learned that starting the appropriate treatment as soon as possible is essential to prevent complications. In cases like this, it is crucial to consider safer treatment options for tuberculosis when severe reactions occur.
Why is this important? This case reminds us that, while these reactions are very rare, it is essential for doctors to be prepared to identify and manage them appropriately. It also emphasizes the need to adapt tuberculosis treatment to ensure patient safety without compromising its effectiveness.
Keywords
Introduction
Overlapping cases of Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) syndrome and Stevens-Johnson syndrome (SJS) represent rare and severe cutaneous adverse reactions. The mortality associated with SJS ranges from 4.8% to 5.7%, while in DRESS it ranges from 10% to 20%.1–4 Both conditions primarily arise from exposure to specific drugs, with antiepileptics and antibiotics being the most commonly implicated agents. 5 Although the occurrence of these conditions induced by antituberculosis drugs (ATDs) is less common, their frequency may increase in areas with a high tuberculosis burden or in patients with HIV coinfection.6–8
DRESS syndrome typically manifests 2–8 weeks after initial drug exposure, featuring a broad range of skin lesions that can cover over 50% of the body. It is accompanied by symptoms such as fever, lymphadenopathy, eosinophilia, and damage to internal organs. 9 In contrast, SJS typically manifests within the first 4 weeks of exposure and is characterized by erythematous macules, blisters, skin peeling, and erosions, predominantly involving the oral, conjunctival, and genital mucosa, with less than 10% of the total body surface area affected.10,11 It can also present respiratory symptoms, fever, dysphagia, ocular discomfort, and damage to internal organs, similar to those seen in DRESS syndrome. 12
The overlapping nature of both DRESS and SJS syndromes presents significant challenges due to their similar clinical presentations and the ambiguity surrounding their pathogenic mechanisms, complicating both diagnosis and treatment. Additionally, SJS and toxic epidermal necrolysis are closely related conditions, often considered part of a disease continuum, distinguished by the extent of skin detachment. Within this context, we present the case of a female patient who developed an overlapping DRESS/SJS reaction following the use of ATDs.
The reporting of this study conforms to the CARE checklist. 13
Case report
A 24-year-old woman from the coast of Peru was diagnosed with pulmonary tuberculosis, confirmed by sputum smear microscopy and a GeneXpert test, which showed sensitivity to rifampin. She is currently undergoing treatment with isoniazid, rifampin, pyrazinamide, and ethambutol. The patient has no relevant medical history or known allergies. Figure 1 displays the chronology of the disease.

Summary of the patient’s medical history.
On day 35 of her treatment, she presented with general malaise, fever, and macular lesions on the extremities. Despite discontinuing the medication for 5 days, her symptoms persisted, including gastrointestinal problems and further extension of the dermal lesions, leading her to seek emergency care in June 2023.
Upon admission, the patient presented with altered vital signs, including hypotension (blood pressure: 80/50 mmHg), tachycardia (heart rate: 115 beats/min), tachypnea (respiratory rate: 24 breaths/min), and fever (temperature: 39°C). The physical examination revealed jaundice, erythematous skin lesions on the extremities, abdomen, and chest, some evolving into blisters, bilateral conjunctivitis, and ulcerative lesions on the lips, along with cervical and axillary lymphadenopathy, and crackles in the left lung. Laboratory tests revealed anemia with a hemoglobin level of 8.5 g/dL (normal range: 12–16 g/dL), leukocytosis with a white blood cell count of 23,200/mm3 (normal range: 4000–10,000/mm³), a total lymphocyte count of 11,400 cells/mm3 with the presence of atypical lymphocytes, and eosinophilia with an eosinophil count of 2523/mm3 (normal range: 0–500/mm³). Serologies for HIV, syphilis, Human T-cell Lymphotropic Virus (HTLV), and hepatitis B and C viruses were negative. Due to the suspicion of DRESS syndrome, treatment with hydrocortisone 100 mg IV three times a day was initiated, and the patient was admitted to the pulmonology department.
On the third day of hospitalization, the patient developed hepatic and renal failure, evidenced by elevated total bilirubin levels (3.2 mg/dL, normal range: 0.1–1.2 mg/dL), ALT (322 U/L, normal range: 7–56 U/L), ALP (730 U/L, normal range: 44–147 U/L), INR (1.8, normal range: 0.8–1.2), and creatinine (3.84 mg/dL, normal range: 0.6–1.2 mg/dL). The patient was mildly somnolent, responsive to stimuli, and presented with oliguria (480 mL in 24 h). By the sixth day, she exhibited desquamation, pruritus, edema of the lips and eyelids, and painful ulcerative lesions in the mouth, accompanied by dysphonia, dysphagia, and respiratory failure (pH: 7.36; pCO2: 44 mmHg; PO2: 58 mmHg; PaO2/FiO2 ratio: 276), requiring the placement of a nasogastric tube and the use of supplemental oxygen (FiO2: 36%; Figure 2). Due to the severity of the DRESS syndrome, she was transferred to the ICU and treated with methylprednisolone (1 mg/kg/day) and chlorphenamine. Considering a score of 11 points on the RegiSCAR classification system, the patient’s clinical features, a 9-point evaluation on the Algorithm for Drug Causality for Epidermal Necrolysis (ALDEN; Supplemental Table S1), and the histopathological findings from the skin biopsy, which revealed orthohyperkeratosis and evidence of confluent apoptotic necrosis of keratinocytes in the epidermis, along with a perivascular infiltrate in the dermis consisting of lymphocytes, histiocytes, and some eosinophils, as well as red blood cell extravasation, interstitial edema, and foci of melanocytic pigment (Figure 3), it was concluded that this is a case of DRESS/SJS overlap.
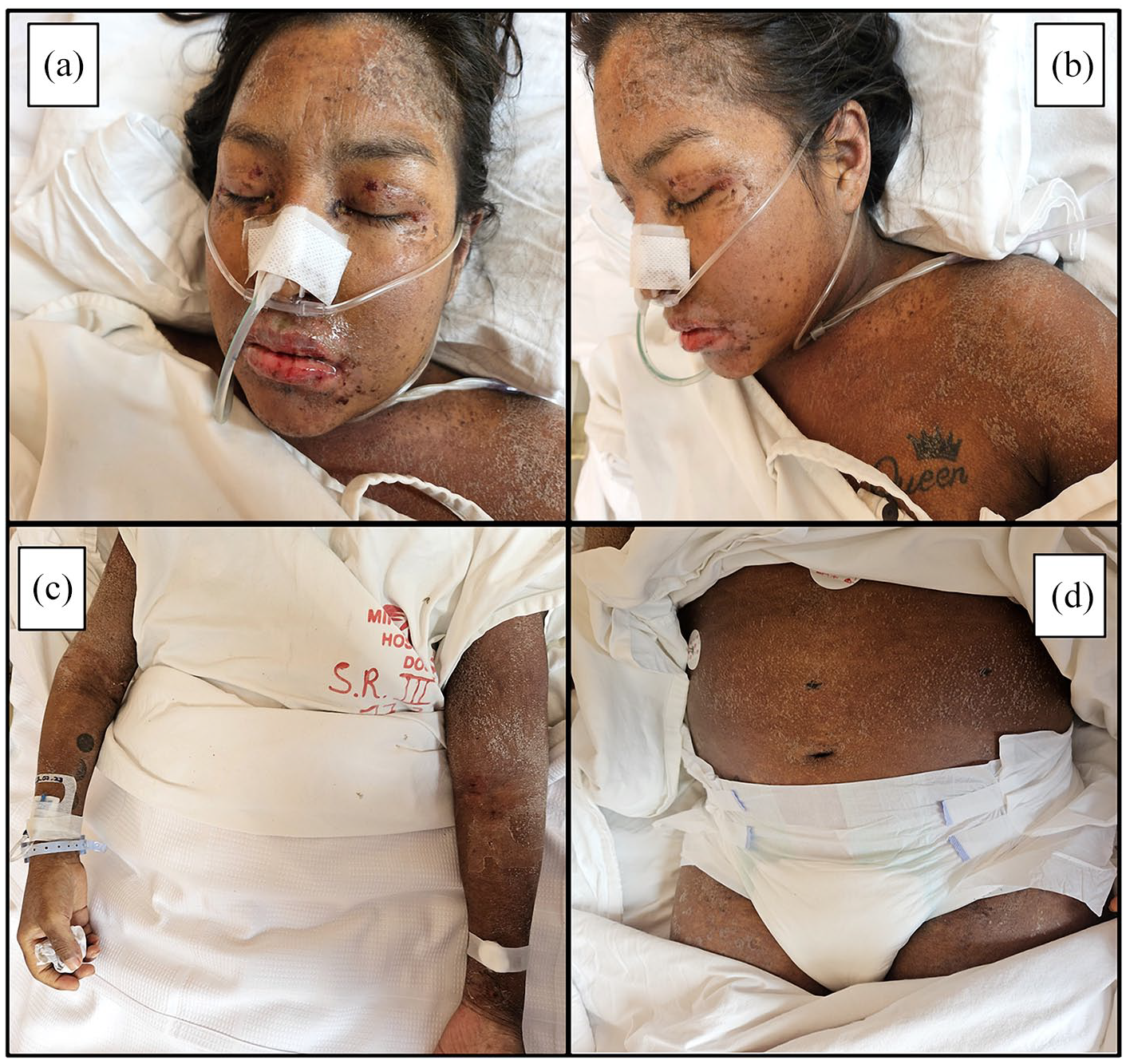
Desquamation occurred on the forehead, cheeks, and nasolabial region, accompanied by edema on the face, especially on the lips, where erosive areas were also covered by crusts (a, b). Desquamation, along with residual hyperpigmentation, was observed on the extremities and abdomen (c, d).

Depicts a skin biopsy (H&E staining). Orthokeratosis and the epidermis exhibited signs of sudden necrosis, associated with multiple apoptotic keratinocytes (black arrow). The dermis showed a mild inflammatory infiltrate, composed of lymphocytes and eosinophils, along with scattered foci of melanin pigment (white arrow).
On her 10th day of hospitalization, the patient had clinically improved, with normalization of liver and renal enzymes, allowing her to return to the pulmonology service. On the 42nd day of hospitalization, she resumed her antituberculosis therapy with a modified regimen approved by the National Committee for Retreatment Evaluation of Peru, which included medications such as Levofloxacin, Linezolid, Bedaquiline, Amikacin, Clofazimine, and Cycloserine. These ATDs were introduced using a challenge protocol, where each drug was administered individually, and an additional drug was added every 4–5 days to complete the regimen, to identify the specific drug in case of an adverse reaction. After 70 days of hospitalization, the patient was discharged without any cutaneous adverse reactions. Follow-up showed that the skin lesions had resolved, and she had good tolerance to the treatment, although she had developed progressive alopecia (Figure 4), which led to her being referred to dermatology for evaluation.
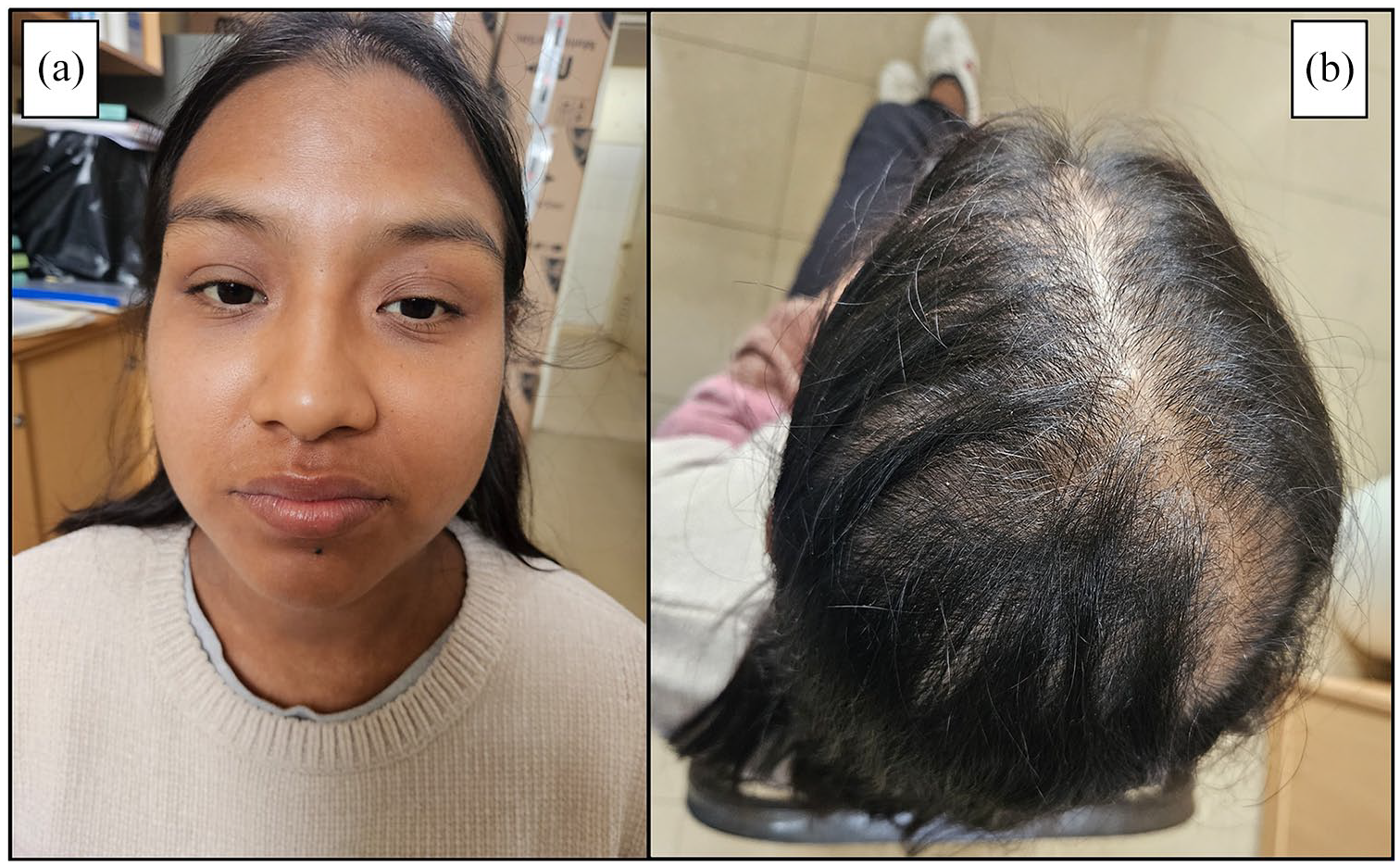
It showed the total recovery of the cutaneous lesions on the face attributed to the DRESS/SJS superimposition (a). Grade II-1 alopecia was observed according to the Ludwig scale, affecting the crown region and extending toward the left side of the occipital region (b).
Discussion
Serious adverse reactions associated with systemic drugs, specifically those that trigger DRESS syndrome or SJS, have an incidence rate ranging from 0.1 to 6 cases per million people.9,14 The overlap of DRESS/SJS is extremely rare; a study published by Bouvresse et al. reported that it occurs in only 2.1% of cases. 15 To date, approximately seven cases have been reported worldwide, primarily associated with allopurinol, antiepileptics such as phenobarbital and oxcarbazepine, non-steroidal anti-inflammatory drugs, and antiparasitic agents such as benznidazole (Supplemental Tables S2 and S3).9,14,16–20 However, this would be the first reported case of DRESS/SJS overlap caused by ATDs. Although standard tuberculosis treatment regimens include multiple drugs with significant potential drug interactions, the frequency of overlap reactions induced by these medications is extremely low. Unlike SJS, DRESS syndrome has been reported more frequently, with rifampin, isoniazid, and ethambutol identified as the primary causative agents in approximately 17.5%–65% of cases.7,21–23 Furthermore, a study conducted by Sim et al. indicates that over 48% of cases are caused by a combination of two or more first-line medications. 24
In the treatment of TB, identifying ATDs that cause severe adverse reactions is crucial. This is because desensitization methods with proven efficacy have been developed, capable of reintegrating these drugs into the therapeutic regimen with a success rate exceeding 62% in patients affected by DRESS syndrome.25,26 However, SJS, only one successful case in the desensitization process has been documented. This was reported in a study by Callado et al., involving a 6-year-old male patient. 27 This finding underscores the significance of such strategies for the reuse of ATDs, which are essential to optimizing treatment efficacy and enhancing patient adherence. Moreover, it is essential to distinguish between desensitization and sequential oral rechallenge. Desensitization aims to induce sustained tolerance to the offending drug, making it a more complex process and less suitable in critical situations. In contrast, sequential oral rechallenge is better documented in cases of severe adverse drug reactions caused by ATDs. 28 This approach allows for the rapid and safe identification of the offending drug through the progressive and controlled introduction of medications, significantly reducing the time required to determine the cause of the reaction. Although this strategy could have been considered in this case to continue using the essential drugs in the regimen, the severity of the patient’s clinical condition and multisystem involvement led to prioritizing their safety and opting for an alternative therapeutic approach. Despite this, a review of the existing literature does not yield sufficient evidence of successful outcomes in cases with overlapping DRESS/SJS. In this context, the World Health Organization recommends several alternative ATDs, including quinolones, aminoglycosides, bedaquiline, cycloserine, and linezolid, which are associated with a risk of severe skin reactions of less than 9%.7,29 This strategy emphasizes the necessity of customizing antituberculosis therapy to meet the individual needs of the patient, aiming to minimize the risks of severe adverse reactions.
The diagnosis of DRESS syndrome in our patient was confirmed using the RegiSCAR criteria, a widely validated tool for assessing severity and confirming cases of DRESS. 30 Simultaneously, the suspicion of SJS was supported by the ALDEN score, which indicated a high probability of drug causality.31,32 Although the histopathological analysis and clinical features supported the coexistence of both conditions, it is crucial to highlight the importance of using these two evaluation tools in combination to ensure an accurate diagnosis of DRESS/SJS overlap. This overlap represents a significant clinical challenge due to the similarity in their presentations and the variability in both cutaneous and systemic manifestations. In clinical management, careful and continuous observation of cutaneous manifestations, such as the development of blisters, mucosal erosions, and the progression of the rash, is critical, as these symptoms can rapidly worsen in both conditions. Likewise, systemic involvement, including hepatic, renal, and pulmonary dysfunction, must be closely monitored, as it can directly impact the patient’s prognosis.1,4 The occurrence of alopecia in our patient as a late manifestation was likely a consequence of telogen effluvium, a relatively uncommon sequela in severe drug reactions. 31 According to the publication by Lee et al., a prevalence of approximately 5.4% of alopecia has been reported in patients with DRESS syndrome, with an expected recovery of hair loss within 6 months. 33
The overlap of DRESS and SJS in this case may be driven by shared immune mechanisms, particularly involving the activation of T-cells and subsequent immune dysregulation. Both syndromes are thought to be initiated by drug-specific immune responses, with DRESS characterized by a broader systemic immune activation, including eosinophilia and multi-organ involvement, while SJS primarily affects the skin and mucous membranes. 34 A key factor in this overlap could be the differential activation of cytotoxic T-cells, which are responsible for inducing keratinocyte apoptosis in SJS. In contrast, DRESS involves a more systemic inflammatory response, often linked to cytokine release, which can still cause significant cutaneous and organ damage. 35 The immune activation observed in both syndromes may explain the simultaneous appearance of DRESS and SJS in this patient, suggesting a convergence of immune pathways that drive both keratinocyte apoptosis (as in SJS) and systemic inflammation (as in DRESS).
In addition, genetic polymorphisms related to the major histocompatibility complex and variations in drug-metabolizing enzymes, such as CYP2B6, CYP2E1, and NAT2, may contribute to this overlap when administering ATDs.36,37 These genetic variations can impair the body’s ability to efficiently eliminate drug metabolites, leading to their accumulation. These metabolites can act as haptens, binding to host proteins and forming neoantigens that interact with Major Histocompatibility Complex (MHC) molecules, triggering an exaggerated immune response mediated by T-cells. 38 This mechanism highlights the complexity of drug-induced immune reactions, emphasizing the interplay between genetic factors, drug metabolism, immune system dynamics, and the crucial role of corticosteroids in managing such severe syndromes. Understanding these overlapping immune pathways is essential for optimizing treatment strategies and minimizing long-term damage.
Conclusion
The overlap of DRESS and SJS induced by ATDs represents an exceptionally rare and clinically complex phenomenon. This case highlights the critical importance of prompt and accurate diagnosis through validated scoring systems such as RegiSCAR and ALDEN. Early intervention with corticosteroids plays a pivotal role in modulating the heightened immune response characteristic of these syndromes, alleviating dermatological manifestations, and mitigating the risk of long-term organ damage. Furthermore, the availability of safer therapeutic alternatives for tuberculosis treatment ensures more effective and secure management for affected patients.
Supplemental Material
sj-docx-1-taw-10.1177_20420986241312484 – Supplemental material for Overlapping of DRESS and Stevens-Johnson syndrome due to first-line antituberculosis drugs: a case report
Supplemental material, sj-docx-1-taw-10.1177_20420986241312484 for Overlapping of DRESS and Stevens-Johnson syndrome due to first-line antituberculosis drugs: a case report by Cristian Morán-Mariños, Felix Llanos-Tejada, Rebeca Huamani-Llantoy, Capriny Bernal-Turpo, Kimberly López-Pilco, Alex Ventura-Leon and Renato Casanova-Mendoza in Therapeutic Advances in Drug Safety
Supplemental Material
sj-docx-2-taw-10.1177_20420986241312484 – Supplemental material for Overlapping of DRESS and Stevens-Johnson syndrome due to first-line antituberculosis drugs: a case report
Supplemental material, sj-docx-2-taw-10.1177_20420986241312484 for Overlapping of DRESS and Stevens-Johnson syndrome due to first-line antituberculosis drugs: a case report by Cristian Morán-Mariños, Felix Llanos-Tejada, Rebeca Huamani-Llantoy, Capriny Bernal-Turpo, Kimberly López-Pilco, Alex Ventura-Leon and Renato Casanova-Mendoza in Therapeutic Advances in Drug Safety
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
