Abstract
Background
Because guanine-based herpes simplex virus thymidine kinase inhibitors are not orally available, we synthesized various 6-deoxy prodrugs of these compounds and evaluated them with regard to solubility in water, oral bioavailability, and efficacy to prevent herpes simplex virus-1 reactivation from latency in a mouse model.
Methods
Organic synthesis was used to prepare compounds, High Performance Liquid Chromatography (HPLC) to analyze hydrolytic conversion, Mass Spectrometry (MS) to measure oral bioavailability, and mouse latent infection and induced reactivation to evaluate the efficacy of a specific prodrug.
Results
Aqueous solubilities of prodrugs were improved, oxidation of prodrugs by animal cytosols occurred in vitro, and oral absorption of the optimal prodrug sacrovir™ (6-deoxy-
Conclusions
Ad libitum oral delivery of sacrovir™ was effective in suppressing herpes simplex virus-1 reactivation in ocularly infected latent mice as measured by the numbers of mice shedding infectious virus at the ocular surface, numbers of trigeminal ganglia positive for infectious virus, number of corneas that had detectable infectious virus, and herpes simplex virus-1 genome copy numbers in trigeminal ganglia following reactivation. These results demonstrate the statistically significant effect of the prodrug on suppressing herpes simplex virus-1 reactivation in vivo.
Introduction
Drugs currently used for human herpes simplex virus (HSV) infections are nucleoside (“acycloguanosine”) analogs, such as acyclovir, its prodrug valcyclovir (Valtrex®), the prodrug famciclovir (Famvir®), as well as the pyrophosphate analog foscarnet (Figure 1). Although these drugs are effective in treating HSV infections during the symptomatic and infectious replicative stages, they are only partially effective in suppressing reactivation of the viruses from the latent state in neurons.1,2 In fact, there is no “cure” for herpes virus latency, and despite treatment with current therapeutics both symptomatic and asymptomatic recurrent shedding and infection occur. This represents a significant weakness of current therapies as infectious virus is unwittingly transmitted via mucosal membranes to partners. This is problematic with ocular infections by HSV-1 and genital infections with HSV-2. The latter infects the genitalia of both sexes and can be transmitted to sex partners even in the absence of active disease.
Antiherpes drugs.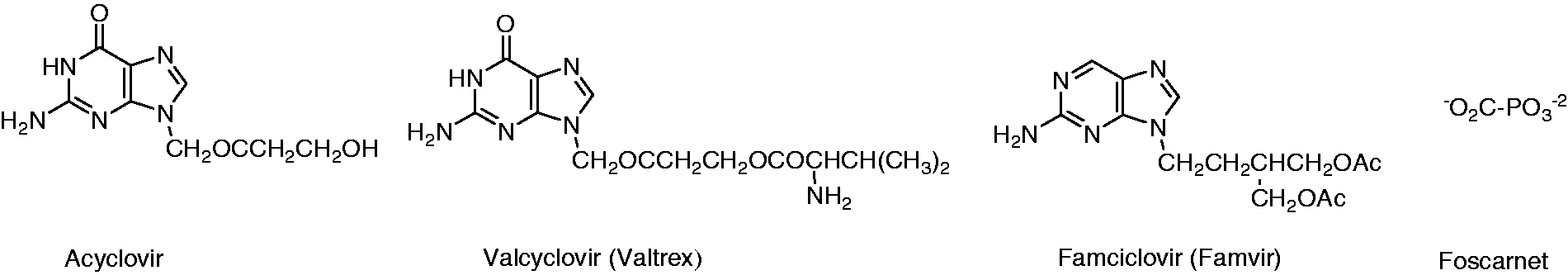
Thus, in order to control the reactivation of the virus, especially in immunocompromised patients where development of drug resistant variants to acyclonucleoside drugs has become common, we3–5 and others6,7 have developed several families of inhibitors of HSV thymidine kinase (TK) whose expression is required for reactivation of virus from the latent state in neurons. Interestingly, we showed that both 2-(phenylamino)-6-oxopurines such as the 9-(4-hydroxybutyl) derivative HBPG and N2-[3-(trifluoromethyl)phenyl]guanine, HSV thymidine kinase inhibitors and prodrugs.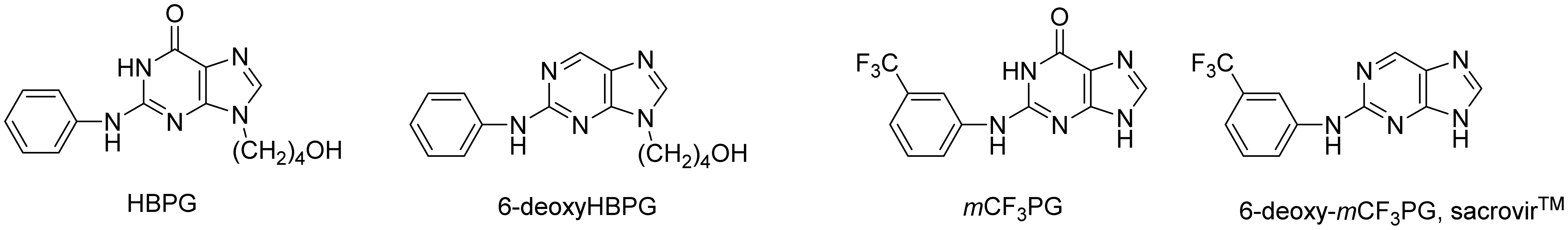
The marketed drug famciclovir (Figure 3) undergoes both ester cleavage and oxidation to provide effective plasma levels of the drug penciclovir.
12
In addition, various nontoxic adjuvants (facilitators) have been developed to increase water solubility of poorly soluble compounds and, in some cases, enhance their oral absorption. In this paper we, therefore, describe synthesis of 6-deoxyguanines corresponding to the active TK inhibitors, their oxidative conversion to the ultimate drugs by incubation in animal cytosols, their water solubility, and their oral absorption and conversion, alone and in combination with various facilitators, by mice. While preliminary results
13
indicated that 6-deoxyHBPG was not oxidized by cytosols, 6-deoxy- Metabolism of famciclovir.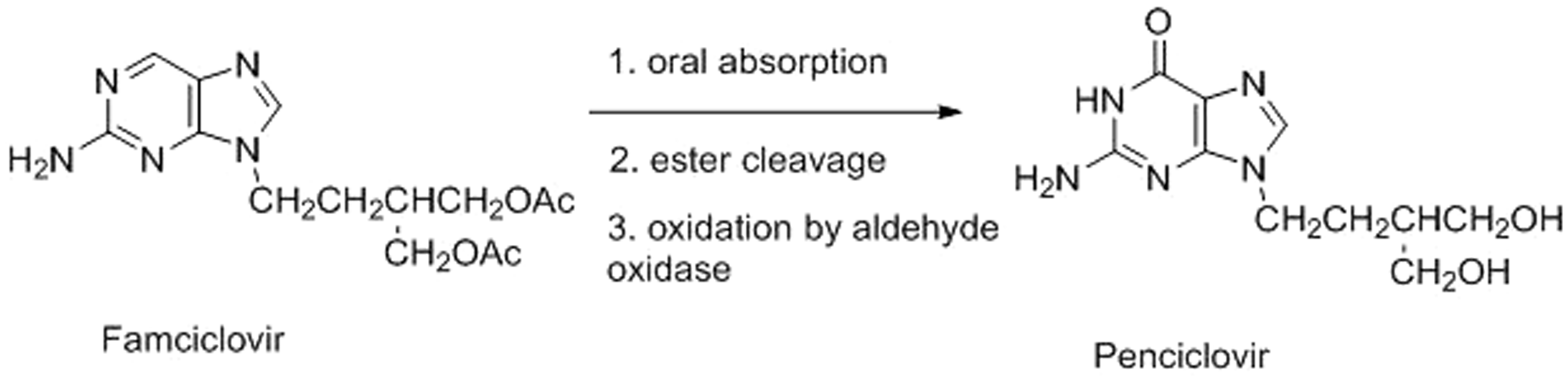
Materials and methods
General
All new compounds were characterized by 1H NMR,
13
C NMR, LC–MS, and HPLC analyses (see Supplementary Material for details of syntheses). HBPG and
Cytosol incubations
Animal cytosols were pooled samples from liver (Bioreclamation Inc., Westbury, NY). Test compounds (50 µM) were incubated at 37°C in mixtures containing 1 mg/ml cytosolic proteins in phosphate buffer (pH 7.4) in glass vials. At various times, aliquots of the incubation mixture were removed and mixed with 2 volumes of acetonitrile, centrifuged at 13,000 × g, the supernatants filtered through 10 k cutoff centrifugation filters, and analyzed by LC–MS. Standard curves were generated from authentic prodrugs and oxidation products.
Solubility
Aqueous solubility was determined at 25°C by stirring an excess of compounds in water or water containing various adjuvants overnight, filtering and analysis by HPLC with UV quantitation of the filtrate. Comparison with a standard curve in each case allowed calculation of concentration. Adjuvants included variable percentages of Soluplus®, a polyvinyl caprolactam–polyvinyl acetate–polyethylene glycol graft copolymer, 10% Solutol® HS 15, a polyoxy 15-hydroxystearate, and 10% Kollidon® (Povidone), polyvinylpyrrolidone of avg. MW 10,000.
Oral bioavailability studies
Bolus
Sacrovir (12 mg) was dissolved with sonication in solutions of 1, 5, and 10% Soluplus in deionized water (2 ml). Swiss Webster mice (avg wt 28.7 g) were given these solutions at 10 ml/kg orally via gavage. Animals were anesthetized with isoflurane at 20 min postdosing, and blood was removed by cardiac puncture and placed in heparinized tubes on ice. Animals were then sacrificed by CO2 inhalation and double pneumothorax. Blood samples were centrifuged at 1500 × g for 5 min at rt, and plasma was drawn off and frozen at −70°C until processed.
In drinking water
Sacrovir (186 mg) was dissolved in 10 ml of 10% aqueous Soluplus with stirring, and this suspension was added to 90 ml of deionized water. This solution containing 1.86 mg/ml of sacrovir in 1% aqueous Soluplus and 1% Soluplus alone were provided as the sole source of drinking water to groups of five mice ad libitum. Fresh solutions were prepared each day. Animal weights and water consumption volumes were measured each day. After the end of the experiment, animals were anesthetized with isoflurane and exsanguinated by cardiac puncture. Blood was processed as above, and LC–MS was used to quantitate prodrug or drug concentrations in plasma.
Effects of sacrovir on HSV-1 reactivation
Corneas of ketamine/xylazine-anesthetized seven-week-old female BALB/c mice (Charles River Laboratories) were scarified bilaterally in a cross-hatch pattern and infected topically with a 3 µl drop containing 25,000 PFU/eye of wild-type HSV-1 McKrae strain. Animals were injected intraperitoneally with 200 µl normal human serum to increase survivability. At days 3 and 5 postinfection, the efficiency of infection was assessed in each eye by fluorescent slit-lamp biomicroscopy and by detection of infectious virus in ocular swabs. To assess complete HSV-1 latency, at both 4 and 5 weeks postinfection, ocular swabs were cultured on Vero cells and tested negative for infectious virus. At greater than 40 days postinfection, surviving mice were randomly assigned into treatment groups: (1) control; normal drinking water; (2) 1% Soluplus; or (3) sacrovir (1.86 mg/ml) in 1% Soluplus. Fresh solutions were prepared each day and provided ad libitum as the sole source of drinking water for each group for two days prior to initiating HSV-1 reactivation by hyperthermic stress as described previously. 14 Following hyperthermic stress-induced reactivation, mice were dried, returned to their cages, and provided food and water containing freshly prepared treatments. At 24 h postreactivation, animals were humanely euthanized and assessed for the presence of infectious virus in paired ocular swabs, paired eviscerated trigeminal ganglia (TG), and individually excised cornealscleral buttons. The presence of infectious virus in each sample was determined by coculture on CV-1 cells. Samples that showed no HSV-1-mediated cytopathic effect at day 7 were scored as negative. In a parallel study, individual TGs were removed, eviscerated in ATL buffer (Qiagen), and frozen until processed for DNA extraction.
Quantification of HSV-1 genomic viral loads in TG
HSV-1 genome copy number in TG was determined by quantitative real-time PCR of the UL30 DNA polymerase gene. UL30 primers and PCR reaction conditions were as previously published. 14 Total DNA was extracted from individually isolated TG using DNeasy columns (Qiagen) and quantified spectrophotometrically. Target genomes in 150 ng of DNA were amplified and detected using BioRad IQ SYBR Green Supermix. Samples were assayed on a BioRad CFX96 in 96-well plates relative to a standard curve with a plasmid containing the HSV-1 UL30 gene. The number of UL30 gene copies in each sample was determined against the standard curve, and the number of viral genomes per TG was calculated based on the total DNA extracted from each TG. Data were plotted in Graphpad and statistical significance between all groups was determined by one-way ANOVA with subsequent Tukey’s multiple comparisons posttest.
Results
Syntheses
Prodrugs
6-DeoxyHBPG was prepared as shown in Figure 4. Details of this and other new syntheses are in Supplementary material.
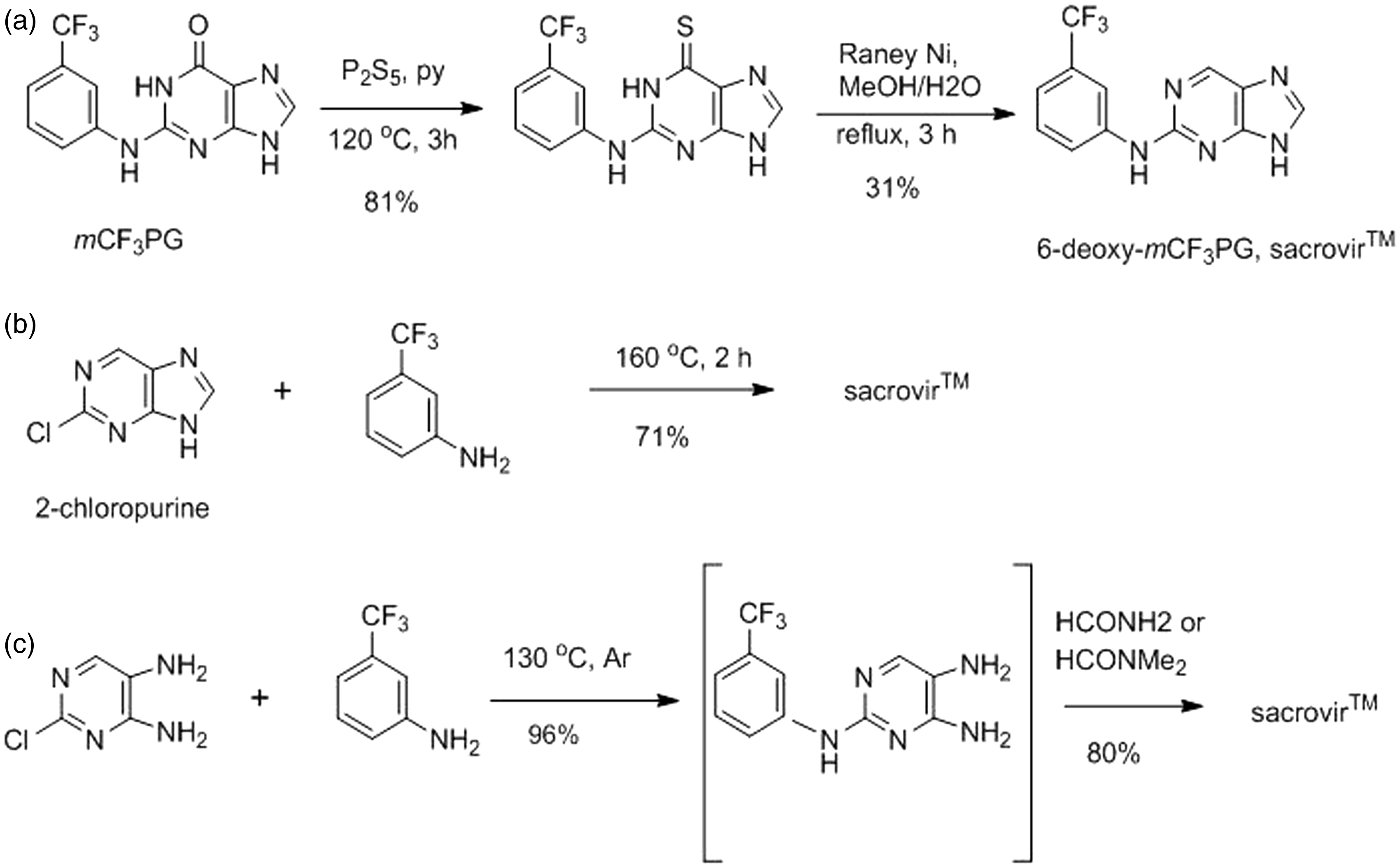
6-Deoxy-
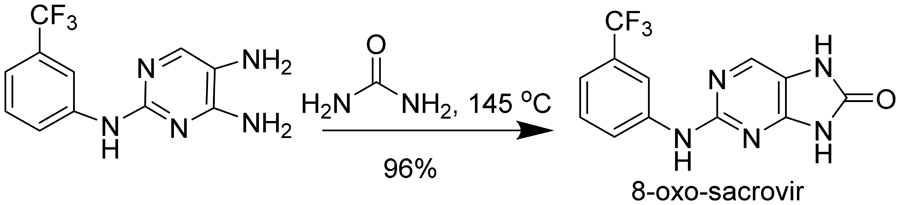
In order to determine the identity of the second oxidation product of sacrovir™, the authentic 8-oxo analog was prepared from the pyrimidine intermediate in 96% yield as summarized:
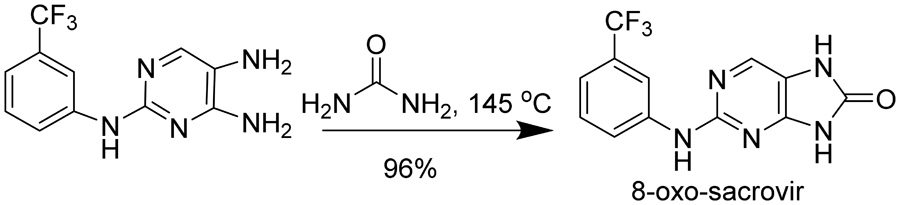
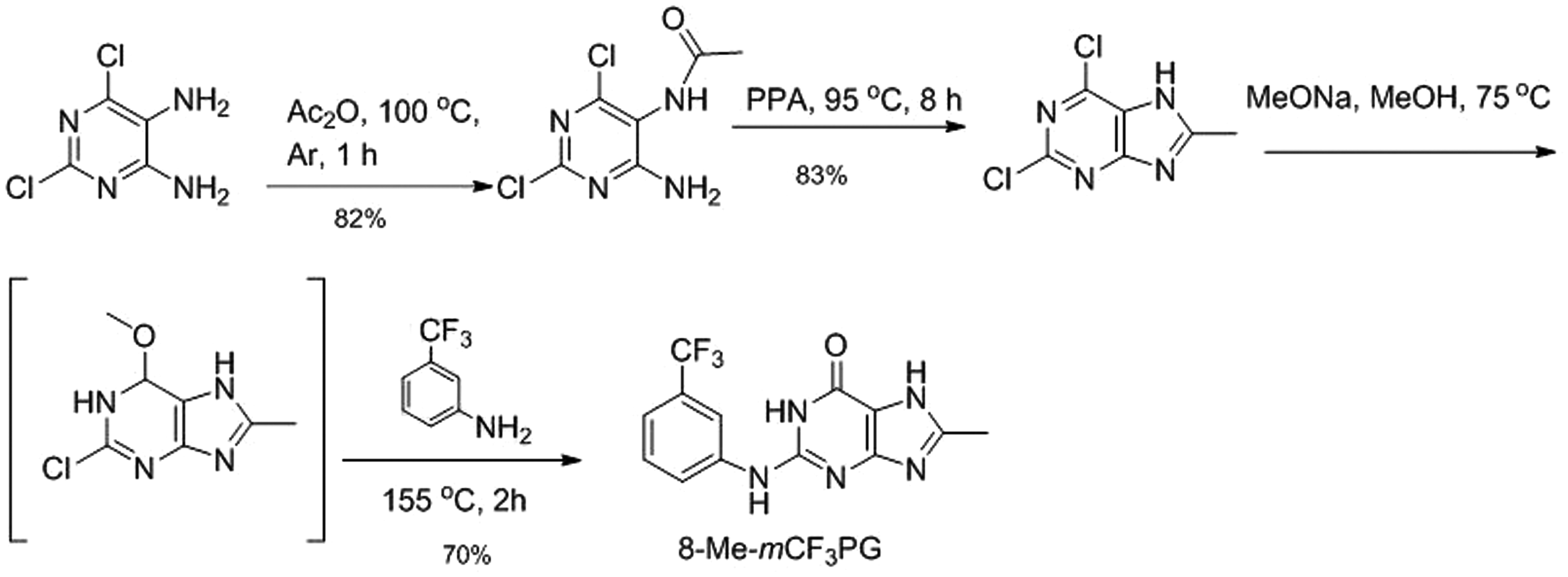
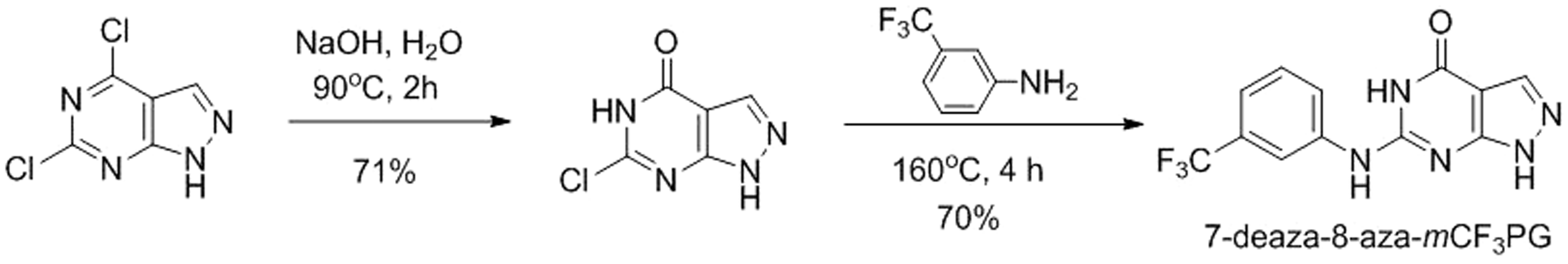
Because of the uncertainty in in vivo conversion of sacrovir, we chose to evaluate cellular oxidation of several 8-blocked forms of this compound as potential prodrugs and the corresponding guanines as TK inhibitors. Synthesis of 6-deoxy-8-aza-
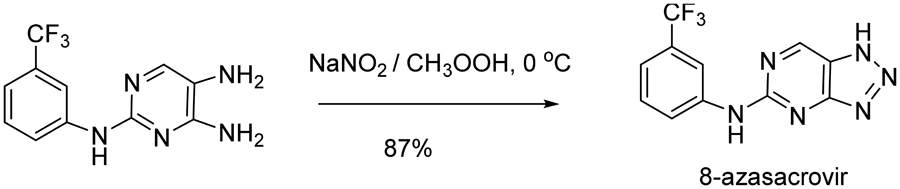
TK inhibitors
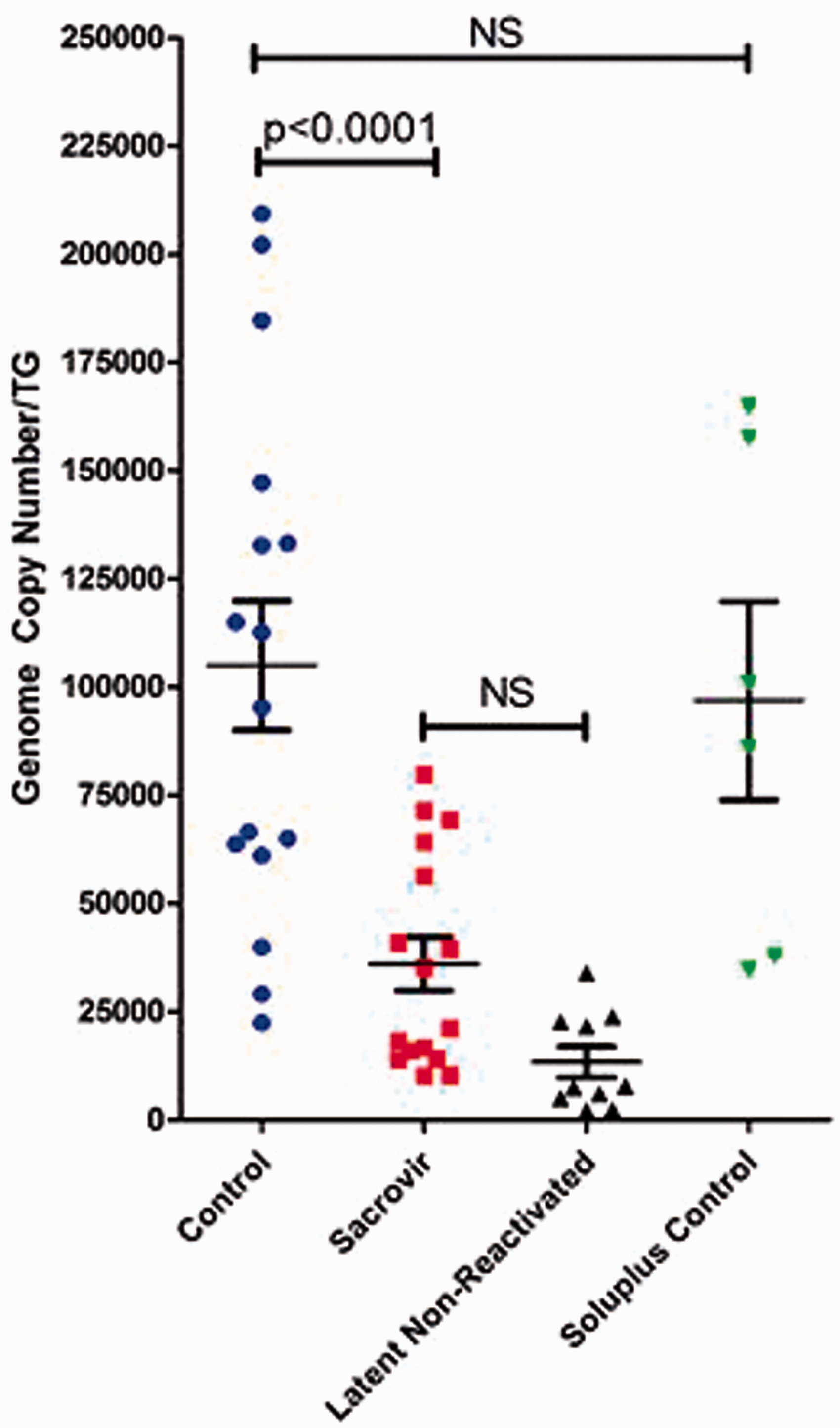
HBPG and Synthesis of 6-deoxy-HBPG. Synthesis methods for 6-deoxy- Synthesis of 8-methyl- Synthesis of 7-deaza-8-aza- HSV-1-specific genome copies in trigeminal ganglia. NS: not significant.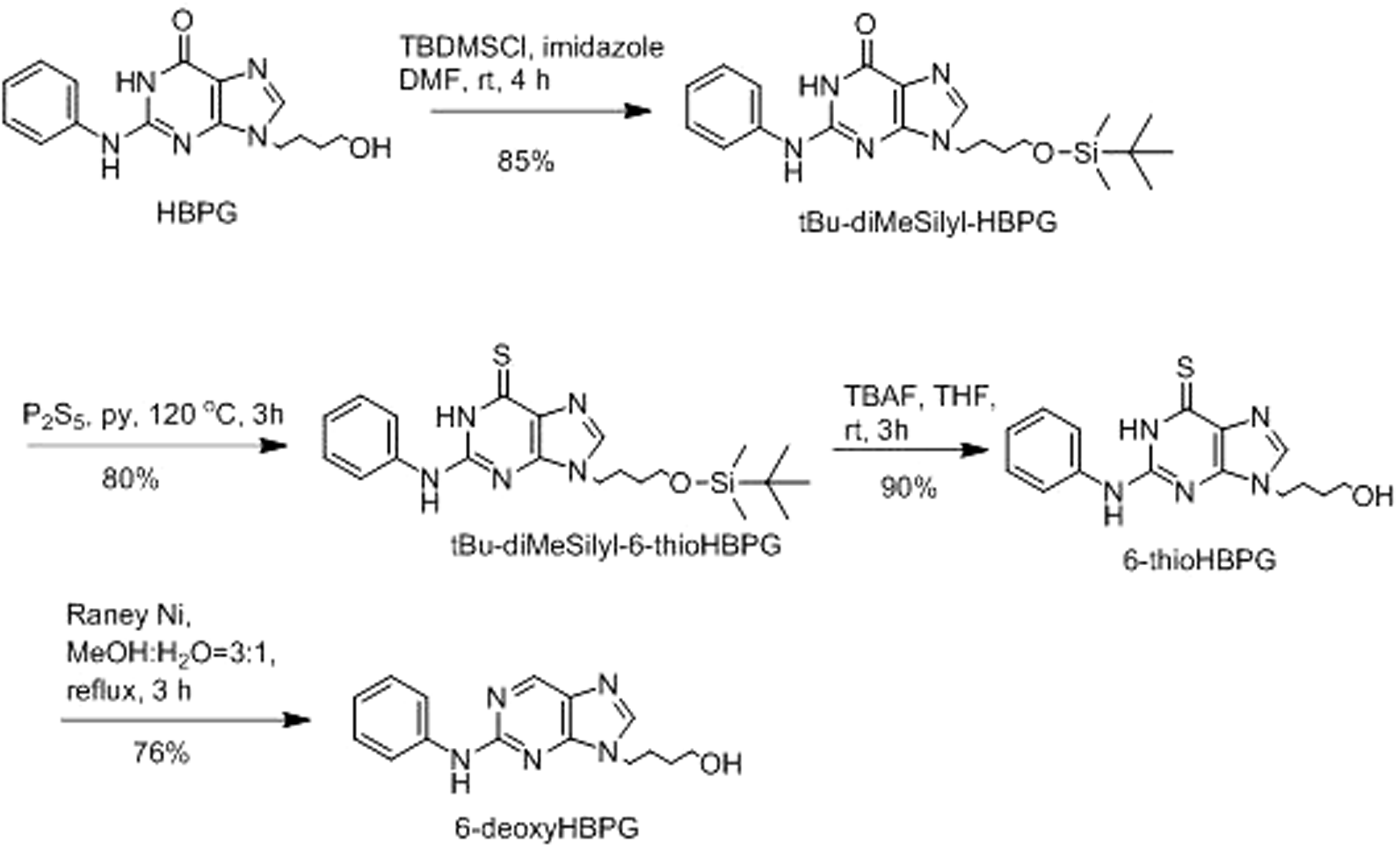
8-Aza-
Enzyme inhibition
Recombinant HSV TKs were cloned, expressed, purified, and assayed as described.
5
Briefly, the enzymes with and without test compounds were assayed in the presence of Km concentrations of substrate (thymidine, 1 and 2 µM for HSV-1 and HSV-2 TKs, respectively).
5
8-Methyl-
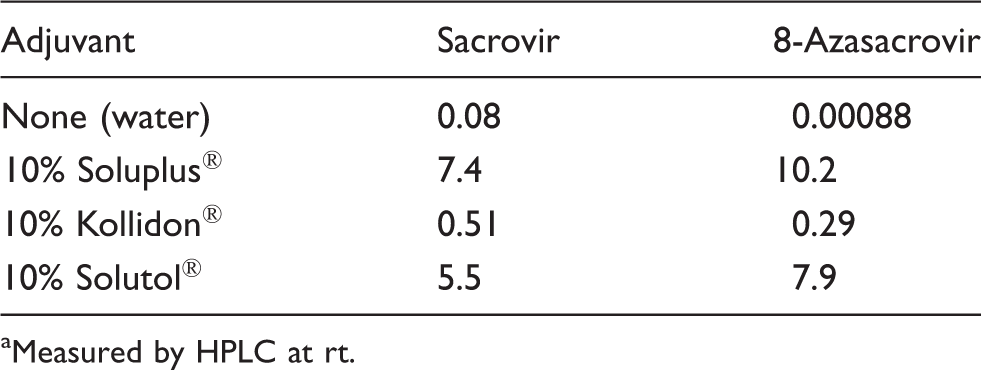
Solubility of sacrovir and 8-azasacrovir
Oxidation by animal cytosols
Oxidation of prodrugs by animal cytosols. a
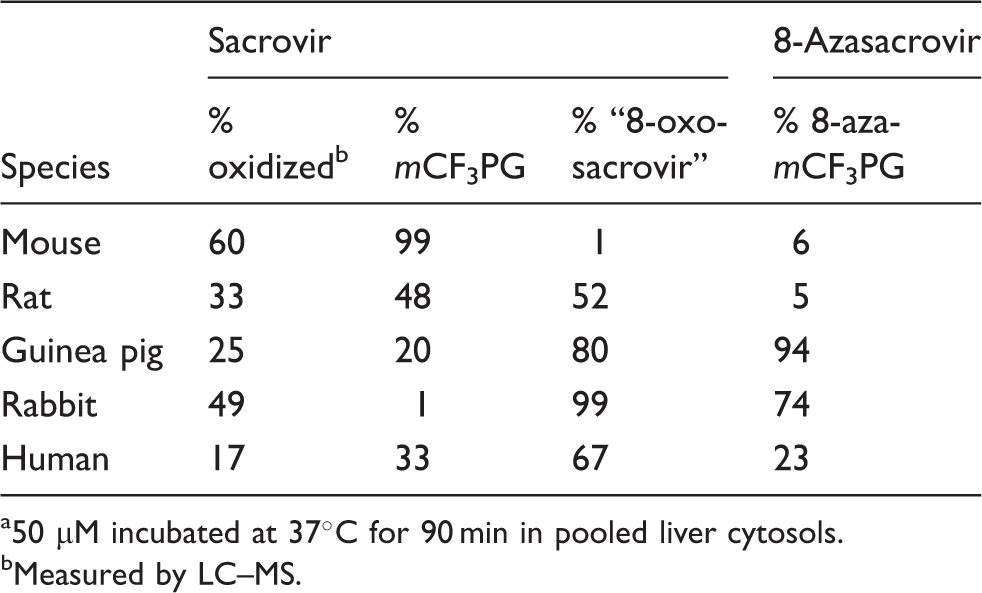
50 µM incubated at 37°C for 90 min in pooled liver cytosols.
Measured by LC–MS.
Absorption and bioavailability of oral sacrovir in mice
Bolus dosing by gavage
Plasma concentration of
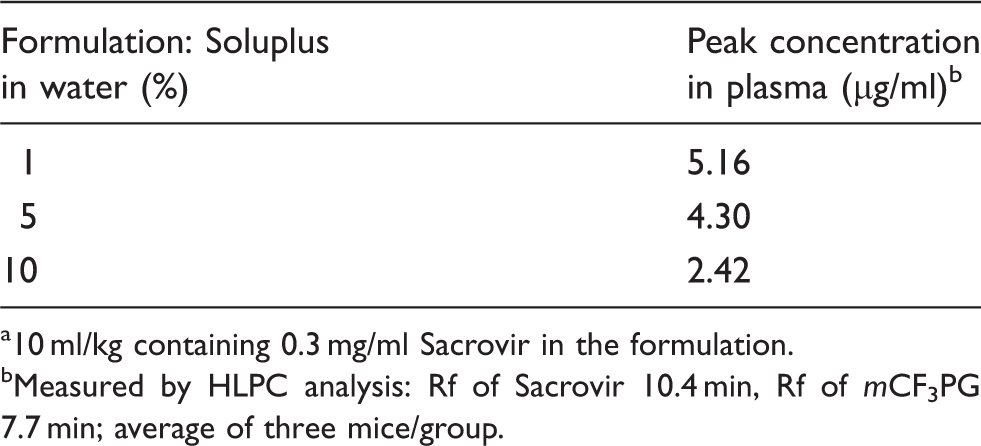

10 ml/kg containing 0.3 mg/ml Sacrovir in the formulation.
Measured by HLPC analysis: Rf of Sacrovir 10.4 min, Rf of
In drinking water
Consumption of sacrovir in drinking water by mice. a

“Water” or formulation in water was available to groups of five mice ad libitum.
By LC–MS of plasma after ca. five days.
Effect of sacrovir on HSV-1 reactivation from latently infected mice
Effect of treatments on HSV-1 reactivation in mice.
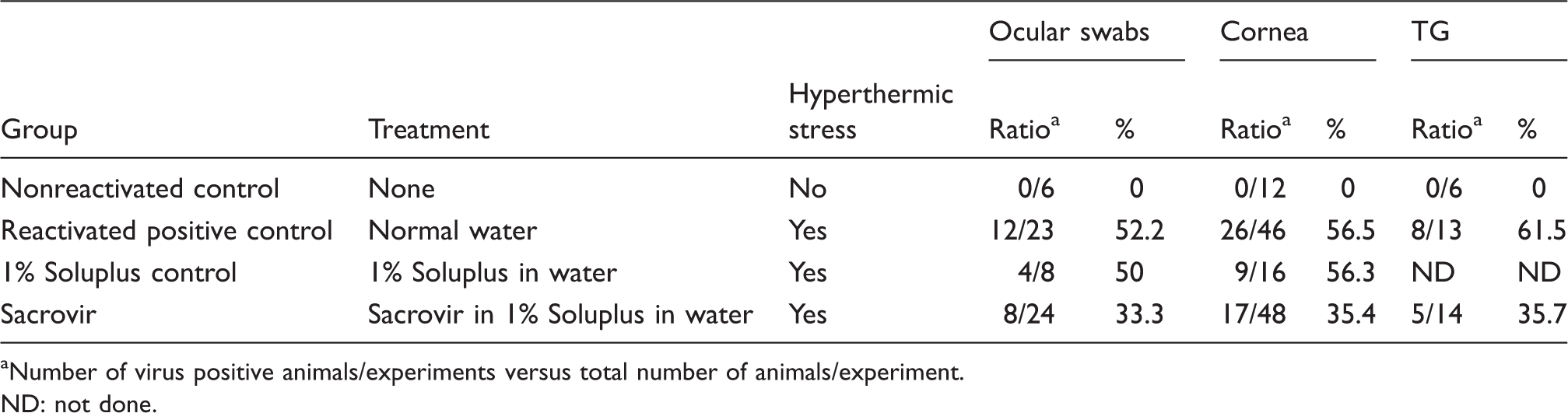

Number of virus positive animals/experiments versus total number of animals/experiment.
ND: not done.
In a parallel study, HSV-1 genomic viral loads within the TG were quantitatively determined by RT-PCR of individually isolated TGs from reactivated and nonreactivated animals under the various treatment conditions. 14 The HSV-1 genomic viral load from individual TG isolates and the mean of each treatment group are shown in Figure 8. In nonreactivated TGs, HSV-1 genomic viral loads ranged from 2103 to 23,777 copies per TG with an average of 13,282. In reactivated positive controls, the TG averaged 104,983 copies per TG and ranged from 22,386 to 184,617 copies per TG. Control treatment with the 1% Soluplus adjuvant alone did not differ significantly from positive controls: a viral load range from 34,556 to 164,712 copies per TG, resulting in an average genomic viral load 96,853. By contrast, sacrovir treatment reduced the overall average genomic viral load in heat-stress reactivated animals to 36,012 copies per TG with a range of 10,150–79,690 copies per TG.
These results demonstrate that sacrovir is absorbed chronically by mice and converted to
Discussion
6-DeoxyHBPG, i.e. 2-phenylamino-9-(4-hydroxybutyl)purine, was not oxidized to HBPG by animal cytosols nor was it orally absorbed in mice (results not shown) and was not studied further. 6-Deoxy-
Sacrovir was soluble in 1–10% Soluplus (Table 3) and readily absorbed orally in 1% Soluplus in water. It was also important, in order to deliver drug consistently to animals, to measure the acceptability of sacrovir and Soluplus by mice. Both sacrovir in 1% aqueous Soluplus and 1% aqueous Soluplus alone were accepted by mice in the drinking water for five days, the length of the reactivation experiment (Table 4). The “dose” of sacrovir was ca. 368 mg/kg/day. Soluplus® is the graft copolymer polyvinyl caprolactam–polyvinyl acetate–polyethylene glycol, and it is used either in aqueous solution or by hot-melt extrusion to enhance solubility of poorly soluble compounds. 18 It often increases oral absorption of drugs at pharmacologically acceptable levels. It is stated by the manufacturer to be “virtually non-toxic after a single ingestion.” It also did not affect the consumption of drinking water by mice, both in the absence and presence of sacrovir (Table 4). Soluplus represents the best adjuvant to increase the oral absorption of sacrovir and related compounds, at least among those reported herein (and others unpublished).
Ad libitum oral delivery of sacrovir albeit at a lower “dose” than expected was effective in suppressing HSV-1 reactivation in ocularly infected latent mice as measured by four parameters: (1) percentage of mice shedding infectious virus at the ocular surface, (2) percentage of TG positive for infectious virus, (3) number of corneas that had detectable infectious virus, and (4) HSV-1 genome copy numbers in TG following reactivation. The first three are summarized in Table 5, and the genome copy number data are summarized in Figure 8, demonstrating the statistically significant effect of the prodrug on suppressing HSV-1 reactivation in vivo.
Footnotes
Acknowledgements
This work is dedicated to the memory of Dr James Hill, LSU Eye Center, New Orleans, LA.
Declaration of conflicting interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors were supported, in part, by SBIR grant 1 R43 AI100300-01 from the National Institutes of Health (to GEW) and by FIRB grant 2BAU011.SR4.001 (to FF). LS was supported by a fellowship provided by Regione Lombardia, Project ID 13810040.
Supplementary Material
Supplementary material includes details of synthesis and characterization of all new compounds.