Abstract
Bleach (sodium hypochlorite, NaOCl) ingestion is highly toxic and can lead to severe complications, including oesophagitis, mediastinitis, and upper airway oedema. We present a case of a 28-year-old male with no prior medical history who intentionally ingested an unknown volume of 3.2% NaOCl in a suicide attempt. The patient presented with haematemesis, chest pain, and epigastric pain. Initial assessment revealed tachycardia and atrial fibrillation (AF) with a heart rate of 135–150 bpm. Nasoendoscopy showed mild upper airway oedema, while oesophagogastroduodenoscopy (OGD) revealed severe oesophagitis with a small distal tear. A CT scan confirmed acute oesophagitis with mediastinitis. The patient was managed with intravenous fentanyl, amiodarone for AF, pantoprazole, dexamethasone, and broad-spectrum antibiotics. He was admitted to the High Dependency ward for close monitoring, and his AF converted to sinus rhythm within 24 hours. Psychiatric evaluation diagnosed an acute stress reaction with bereavement, with a background of possible psychosis. The patient was discharged on day 5 with no further complications. This case highlights the rare occurrence of AF in a patient with mediastinitis and oesophagitis secondary to bleach ingestion without oesophageal perforation. Prompt supportive care, close monitoring, and psychiatric evaluation are crucial in managing such cases. This report underscores the importance of considering AF as a potential complication in patients with mediastinitis following bleach ingestion.
Introduction
Bleach, also known as sodium hypochlorite (NaOCl), is highly toxic and can cause serious health effects if ingested in large amounts. 1 We present a case of NaOCl ingestion with acute oesophagitis with mediastinitis.
Case summary
A 28-year-old male with no past medical history was brought in by paramedics for haematemesis after an intentional ingestion of an unknown volume of bleach (NaOCl 3.2%), as part of a suicide attempt. He complained of chest and epigastric pain. There was no co-ingestion of any other drugs or alcohol.
He was tachycardic on presentation with a heart rate of 135. Blood pressure and oxygen saturations were normal. Clinical examination revealed a patent airway with throat injection and epigastric tenderness with no associated peritonism. The cardiorespiratory exam was normal. An electrocardiogram (ECG) done showed atrial fibrillation (AF) with a telemetry rate ranging from 130 to 150 (Figure 1). A chest radiograph done was normal and venous blood gas did not reveal any acidosis. Bloods including full blood count, renal panel with extended electrolytes and thyroid function test did not reveal any abnormalities.
He was given titrated doses of intravenous (IV) fentanyl for analgesia. His AF was managed with IV amiodarone 150 mg, administered over 30 min. IV Pantoprazole was administered for potential oesophagitis and gastritis. IV dexamethasone 4 mg was administered to suppress airway inflammation. Nasoendoscopy performed by ENT doctors in the Emergency Department revealed oedema over the posterior soft palate margin, epiglottis, and bilateral arytenoids, obscuring the posterior third of the vocal cords. The endoscopic impression was mild upper airway oedema with no immediate airway concern.
An urgent Oesophagogastroduodenoscopy (OGD) revealed severe oesophagitis with multiple areas of erythema, with a small tear at the distal oesophagus. Due to concerns of aggravating the tear, the procedure was abandoned, and an urgent computer tomography (CT) scan of the thorax and abdomen was performed. The CT showed a long segment of diffuse mural oedema and thickening of the oesophagus with surrounding mediastinal soft tissue stranding, in keeping with acute oesophagitis with mediastinitis (Figure 2).
He was admitted to High Dependency ward for close airway monitoring. He was empirically covered with broad spectrum intravenous antibiotics. He was kept nil by mouth for the first 24 h and thereafter was gradually started on clear fluid as tolerated. His AF converted to sinus rhythm within 24 h of admission (Figure 3). Psychiatric consult was obtained inpatient, and he was diagnosed with a suicide attempt due to acute stress reaction with bereavement. This is on a background of possible previously diagnosed psychosis. The patient remained well during the hospital stay and was discharged on day 5 of admission.
Discussion
A review of the literature showed few case reports describing oesophageal perforation and mediastinitis as complications of bleach ingestion. Two case reports has described AF with chlorine inhalation,2,11 and one case report described a patient with AF due to a perforated esophagus after bleach ingestion.3,4 To our knowledge there are no reports describing AF in a patient with mediastinitis with esophagitis without perforation, as happened in our case.
NaOCl ingestion has been known to cause significant tissue damage and inflammation, leading to severe complications such as oesophagitis, mediastinitis, and upper airway oedema.5–7 Therefore, it is important to provide prompt and appropriate management to prevent further damage.
In managing NaOCl ingestion, there is minimal evidence to support decontamination efforts. Gastric lavage is contraindicated due to risk of aspiration and has not shown benefit. 1 There is a reported case of mediastinitis and oesophageal stenosis secondary to gastric lavage being performed on patient who ingested NaOCl.5,8
The primary approach to treating NaOCl poisoning is by providing supportive care that addresses the symptoms. Patients with symptoms should be closely monitored for any respiratory or cardiovascular issues that may arise. In cases where there is a significant respiratory compromise, it may be necessary to perform early intubation and provide mechanical ventilation to the patient. 1 It is important to closely monitor the acid-base status, pulse oximetry, serum electrolytes, and fluid balance for any irregularities in patients with NaOCl poisoning. If there is a presence of metabolic acidosis, some authors recommend administering sodium bicarbonate as a potential treatment option. 9 There is no role for enhanced elimination in the treatment of NaOCl ingestion based on literature.
NaOCl ingestion can provoke atrial fibrillation through multiple converging mechanisms. Caustic injury from hypochlorite and its conversion to hypochlorous acid can perforate the oesophagus, leading to pericardial inflammation; observational data indicate pericarditis can trigger atrial fibrillation and flutter in up to 10 % of cases. 10 Hypochlorous acid and chlorine gas also act as powerful oxidants, causing oxidative stress and sympathetic activation, both of which lower arrhythmia thresholds. 11 Furthermore, systemic inflammation and sepsis from mediastinal contamination amplify these effects, as high myeloperoxidase and hypochlorous acid levels correlate with new-onset atrial fibrillation in septic patients. 12 Autonomic dysregulation due to pain, stress and inflammatory ganglion irritation further promotes atrial arrhythmogenicity. 13 Together, these pathways explain why severe bleach ingestion, though uncommon, can precipitate atrial fibrillation and underscore the need for prompt assessment of metabolic, inflammatory and structural complications alongside standard arrhythmia management.
Patients who present with intentional bleach ingestion should be thoroughly evaluated for any associated medical and psychiatric conditions,1,7 as well as any co-ingestion of other substances. These patients may require close monitoring and management in a high-dependency setting. They may also require early or late endoscopy to evaluate for oesophageal complications such as oesophageal stenosis. 5
In cases where there is concern about exacerbating tissue damage, procedures such as OGD should be performed with caution or deferred, and alternative diagnostic methods should be considered.
Prompt psychiatric evaluation and management are crucial in patients presenting with intentional bleach ingestion,1,7 as these patients may be at increased risk of suicide and require appropriate follow-up and support. ECG showing atrial fibrillation with rapid ventricular rate. CT thorax image shows diffurse mural oedema and thickening of the oesophagus with surrouding soft tissue stranding (yellow arrow) in keeping with acute oesophagitis with mediastinitis. Repeat ECG showing sinus rhythm. This was done about 12 h from ECG in Figure 1.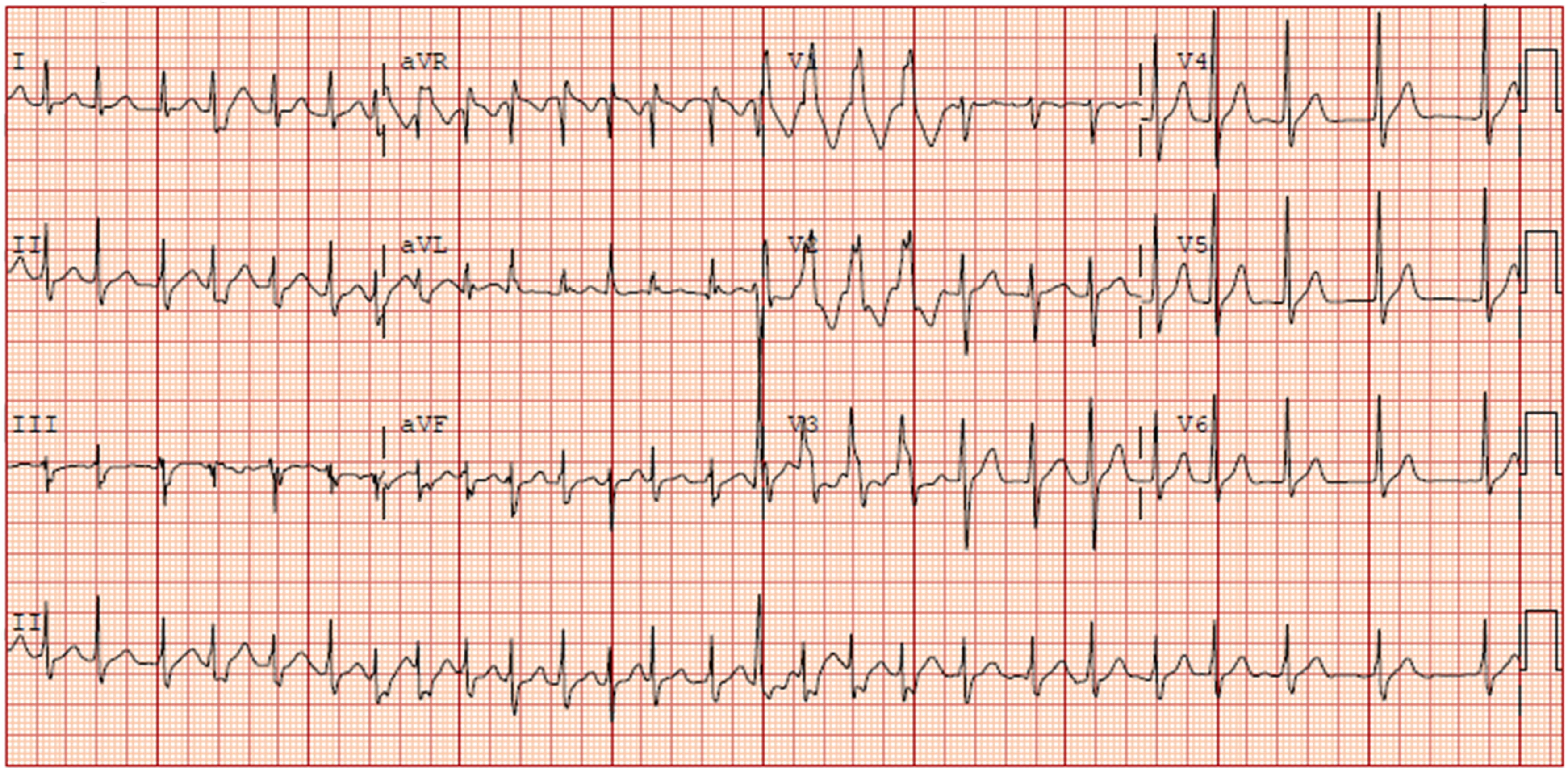


Conclusion
We present a unique case of bleach ingestion, where the patient suffered oeosphagitis without perforation, mediastinitis and atrial fibrillation as a complication of the ingestion.
Footnotes
Ethical considerations
Changi General Hospital does not require ethical approval for reporting individual cases.
Consent to participate
A written consent was obtained from the patient for the purpose of writing and publishing this case report.
Author contributions
Frist author wrote the first draft of the manuscript. Second author reviewed and edited the manuscript and approved the final version of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Data Availability Statement
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study.
