Abstract
Background
The use of telepractice as an alternate method of delivering healthcare to people increased significantly after COVID-19 became a global pandemic.
Objectives
This study aimed to identify factors contributing to the accelerated adoption of telepractice during COVID-19 in Singapore. It also sought to examine whether there are differences in the perspectives of staff in nursing facilities and caregivers in personal homes towards telepractice.
Methods
A cross-sectional mixed method design was used. A survey with 20 items was adapted from the Telehealth Usability Questionnaire and translated into Mandarin. Anonymous responses were obtained from 70 patients and caregivers who had received speech therapy services via telepractice from a restructured hospital before and/or during Singapore’s Circuit Breaker period. Analyses were conducted using descriptive statistics and content analysis.
Results
Sociodemographic variables of age, gender, education level and language preference did not impact user satisfaction and the likelihood of using telepractice again. Service-related factors were more influential. Participants chose to use telepractice as it saved travelling time (24.0%), was easy to use (19.3%), improved healthcare access (17.5%) and reduced waiting time (17.5%). Although all respondents expressed satisfaction in telepractice, 35.5% from personal homes and 37.5% from nursing facilities were not keen to use it again. Amongst caregivers, 26.7% from personal homes and 37.5% from nursing facilities preferred not to continue telepractice use. Technical and logistical disruptions and the lack of ‘personal touch’ were contributing factors.
Conclusion
Improving technological infrastructure, providing training for users and developing guidelines would help sustain telepractice as a form of service delivery beyond COVID-19.
Introduction
Telepractice refers to the provision of speech therapy services remotely, predominantly over the Internet via video-conferencing platforms. 1 Speech therapy services are uniquely suited to telepractice delivery because of the audio-visual nature of clinical interactions and techniques. 2 The American Speech-Language-Hearing Association recognised telepractice as an appropriate form of service delivery in year 2005, 1 with the service shown to have similar efficacy to conventional in-clinic sessions. 3 However, the adoption of telepractice as an alternative to physical consultations pre-COVID-19 has been limited, particularly in Asia.
Although a conference and cross-institutional discussions were held in year 2019 in Singapore to encourage the development of telepractice, there was no strong push for services to be delivered online. So telepractice remained provided by a handful of therapists for selected clients. Convenience sampling of 114 speech therapists in Singapore from May to July 2020 revealed 78.4% of therapists believed in-person therapy is of better quality than telepractice. 4 Survey findings perceived therapists to lack resources to support telepractice while clients might lack access to technology. A similar study in Hong Kong also showed telepractice being regarded as less effective than face-to-face sessions. 5
The coronavirus disease (COVID-19) proved to be a formidable disruptor impacting healthcare and economic systems worldwide. Governments’ directives to limit virus transmission inadvertently restricted many from accessing services in healthcare facilities. In Singapore, the government implemented a ‘Circuit Breaker’ period from 7 April to 1 June 2020, followed by a gradated re-opening plan. During this period, safe-distancing measures and work-from-home policies were implemented. 6 Non-essential face-to-face services such as outpatient appointments for non-life-threatening health conditions were deferred. To enable continuity of care, many healthcare providers including speech therapists started offering video-conferencing services online.
Sociodemographic factors
The first aim of this study was to investigate the influence of sociodemographic factors on the adoption of telepractice in Singapore. The impact of these factors on digital health services have been inconsistent. Some studies report no consistent nor strong impact of age, gender, education level and preferred language on the uptake of telepractice. 7 Others indicate that older persons might be less receptive to telepractice than younger persons. Older persons, defined as people aged 60 or 65 and above, 8 tended to value service attitudes and ‘personal touch’ which are more easily experienced in face-to-face sessions.9,10 In contrast, younger and more highly educated respondents were more receptive to adopting telepractice due to the perceived ease of use and language or technological literacy.9,10 A ‘gender gap’ was also identified where females, especially in low- and middle-income countries in South-East Asia, were less inclined to adopt new technology.11,12 Other studies, however, showed women in developed countries being willing to use telehealth 13 with high satisfaction rates reported, 14 possibly because access to healthcare was maintained whilst they juggle multiple responsibilities like work, household and childcare. 15 To date, no study has investigated how sociodemographic factors influence the adoption of telepractice in a cosmopolitan country in Asia like Singapore.
Service-related factors
The second aim of the study was to evaluate the impact of service-related factors on telepractice use. According to the Unified Theory of Acceptance and Use of Technology (UTAUT), 16 adoption and end-user acceptance of technology are influenced by four factors: 1. Performance expectancy, meaning how the technology enhances the quality of life performance; 2. Effort expectancy, which refers to the ease of use and convenience of the technology; 3. Social influence, which includes the views of important others towards the use of technology and 4. Facilitating conditions, which refers to an individual’s belief that organisational and technical infrastructure exists. Given that treatment effectiveness, convenience, accessibility and cost-effectiveness correlated strongly with the satisfaction and use of digital health services in Korea and China,17, 9 this study also sought to establish if service-related factors were influential in Singapore.
Caregiver perspectives
The third aim of the study was to compare the perspectives of staff caregivers at nursing facilities towards telepractice to that of caregivers from personal homes. COVID-19 has been found to cause a significant increase in associated mortality in nursing home residents compared to the surrounding communities. 18 During Singapore’s Circuit Breaker, nursing home residents and staff could not leave the home while external therapists could not enter to provide services. Many nursing homes began supporting video calls between residents and families, and some participated in telepractice sessions. A pre-COVID-19 survey suggested that telehealth usage amongst nursing staff may be impacted by reduced confidence, or lack of knowledge and skills.19,20 It is not clear if the physical constraints imposed by COVID-19 and the push to telehealth services have changed the perceptions of nursing staff.
In all, this study aimed to: 1. Investigate the impact of sociodemographic factors (i.e. age, gender, education level and language preference) on the adoption of telepractice 2. Evaluate the impact of service-related factors on users’ attitudes towards telepractice 3. Assess if there are differences in the perspectives of staff in nursing facilities and caregivers in personal homes towards telepractice
Methods
Study design
A cross-sectional mixed methods design was used. This retrospective study was recognised by the Institutional Review Board as a quality improvement project which did not require ethics approval.
Setting and participants
Tan Tock Seng Hospital is a multi-disciplinary tertiary hospital, serving a resident population of 1.4 million persons in Singapore. 21 Telepractice services were started in December 2018 by a few speech therapists for patients with Parkinson’s Disease to conveniently access Lee Silverman Voice Treatment LOUD (LSVT-LOUD) programme. LSVT-LOUD is an evidence-based protocol that aims to make a person’s voice loud and speech clear. To achieve optimal therapeutic intensity, patients attend hourly sessions, 4 days a week, for 4 weeks. 22 Such schedules can be challenging for patients with Parkinson’s disease, as they may face reduced mobility and have difficulty making frequent hospital visits. The initial platform used for telepractice was Vidyo, before moving on to Zoom.
With the constraints imposed by the COVID-19 outbreak, telepractice became an obvious method for continuing therapy. The speech therapy department at Tan Tock Seng Hospital re-designed processes and provided training so all speech therapists could deliver telepractice services. The suitability criteria for patients were expanded with the creation of a risk stratification matrix to help therapists determine patients’ suitability. These efforts resulted in the percentage of outpatients seen via telepractice increasing from less than 5% pre-COVID-19 to 48% in April 2020 and 89% in May 2020.
The study was conducted from April 2020 to September 2020. Patients and caregivers who received outpatient communication and swallowing services at the acute hospital and an offsite rehabilitation centre via telepractice before and/or during the Circuit Breaker period were recruited. The first patient had used the service in September 2019 while the last patient was seen on 1 June 2020. A subset of these participants were patients and staff from nursing facilities in Singapore. There was no difference in the recruitment process for participants from personal homes and nursing facilities.
All participants provided consent for telepractice and had an internet-enabled electronic device with Zoom Application downloaded. Participants also had a stable internet connection and food, drinks and utensils prepared if the session was meant to be a swallow review. Caregivers were present if patients could not manage the session independently. All sessions were encrypted by the Integrated Health Information Systems, Singapore’s HealthTech agency.
Development of questionnaire
An online questionnaire (Appendix A) containing 20 items was developed via Google Forms. Google Forms was used as it is familiar to most internet users in Singapore. The questionnaire was adapted from the Telehealth Usability Questionnaire (TUQ, 23) by including 7-point Likert scales and tailoring the questions to suit the local pandemic context. The adapted questionnaire was also translated into Mandarin, a language commonly used in Singapore. Six domains, namely usefulness, ease of use, interface quality, interaction quality, reliability and satisfaction, were used to measure usability in the TUQ and the adapted questionnaire.
The definitions of each domain are: 1. Usefulness – the effectiveness and efficacy of the telehealth system in delivering clinical outcomes comparable to in-person healthcare service 2. Ease of use – the amount of effort it takes to learn and use the telehealth system 3. Interface quality – the quality of the user interface, ease of navigation and an overall impression of the interaction between the user and the technology system 4. Interaction quality – the subjective perception users have when interacting with the clinician via the telehealth system, including audio-visual quality 5. Reliability – how easily a user can recover from technical errors while using the telehealth system 6. Satisfaction – the level of comfort, satisfaction and willingness of caregivers and patients to continue using the telehealth system
Administration of questionnaire
Online survey links were created and included in appointment emails to patients and/or their caregivers. Phone calls, conducted in English or Mandarin, were done by a therapy assistant after telepractice sessions to remind participants to complete the questionnaire. If participants expressed difficulties completing the questionnaire online, the survey would be administered via the call where the therapy assistant would read the questions and options aloud before recording participants’ responses. Participation was voluntary and the data collected was anonymous.
Data/statistical analyses
Participants’ responses were organised using Excel 2016 software and data analyses focused on specific questions in the questionnaire. The primary analyses for patient satisfaction and continued use of telepractice were derived from Q8 and Q17, respectively. Responses of ‘strongly dissatisfied’, ‘dissatisfied’, ‘somewhat dissatisfied’ were grouped wholly as dissatisfied, while ‘strongly satisfied’, ‘satisfied’, and ‘somewhat satisfied’ were grouped wholly as satisfied. ‘Neutral’ was regarded as neither satisfied nor dissatisfied. The quantitative responses and sociodemographic data collected were analysed using chi-square tests. Where the assumptions for chi-square were not met, the Fisher’s exact test with p value calculated by Monte Carlo simulation was used. A p value of 0.05 was considered statistically significant.
Content analyses were performed on Q15 and Q18. Categories for service-related factors such as ‘COVID-19 restrictions, safety concerns, ease of use, improved access to healthcare, lack of ‘personal touch’, ‘technical and logistical disruptions’ were identified. These categories were coded and analysed using the IBM Statistical Package for Social Sciences Statistics software version 27.0. 24
Results
Sociodemographic characteristics of participants
84 patients were seen via telepractice from September 2019 to 1st June 2020. Of these, 2 declined, 2 passed away, 2 were overseas and 4 were uncontactable. Another 4 were not contacted as challenging interactions were noted between healthcare professionals and the patients and/or their caregivers. Of the 70 respondents who completed the questionnaire, 47 were patients and 23 were caregivers who were either family members, helpers, or staff nurses from nursing facilities.
Sociodemographic characteristics of participants in personal homes.

Sociodemographic characteristics of participants in nursing facilities.
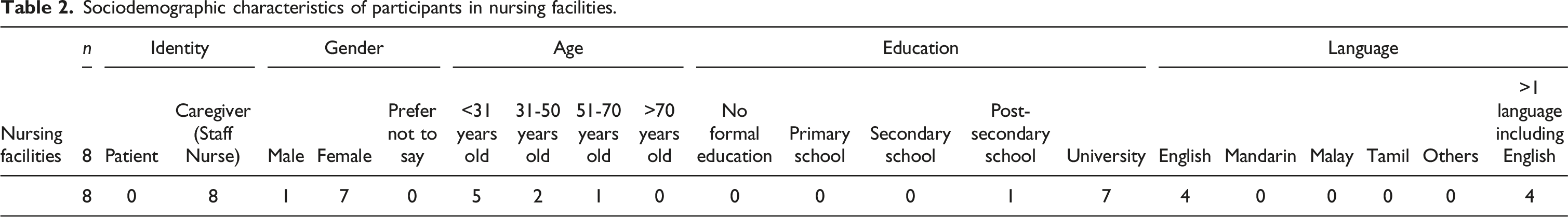
Impact of sociodemographic factors
All respondents expressed that they were satisfied with the telepractice service. Of the 62 respondents from personal homes, 19 indicated that they were very satisfied, 27 were satisfied, 15 were somewhat satisfied and 1 was neutral. Of the 8 respondents from nursing facilities, 1 was very satisfied, 6 were satisfied, 1 was somewhat satisfied.
Regarding the continued use of telepractice, 40 respondents from personal homes would use telepractice again while 22 would not. 5 out of 8 respondents from nursing facilities would use telepractice again while 3 would not.
Age
The chi-square test of independence showed no significant association between age and the willingness to use telepractice again X2 (1, N = 62) = 0.64, p = 1.000.
Gender
The chi-square test of independence showed no significant association between gender and the willingness to use telepractice again X2 (1, N = 61) = 0.15, p = 0.789. One case was disregarded from the analysis as the respondent had declined to report gender.
Education level
The chi-square test of independence could not be used as the minimum expected count was not met. Fisher’s Exact Test found no significant association between education level and the willingness to use telepractice again (2-sided p = 0.307).
Preferred language
Similarly, conditions for the chi-square test were not met. Fisher’s Exact Test found no significant association between preferred language and the willingness to use telepractice again (2-sided p = 0.673).
Impact of service-related factors
171 responses were obtained for why participants chose telepractice. Each respondent could select multiple choices. The most popular reasons for choosing telepractice were that it saved travelling time (n = 41, 24.0%) and was easy to use (n = 33, 19.3%). Some respondents felt it improved access to healthcare (n = 30, 17.5%) with less time spent waiting for registration or transportation (n = 30, 17.5%). Some also felt that telepractice saved money (n = 15, 8.8%).
10.5% of the responses (n = 18) reflected COVID-19 as a factor influencing their choice to use telepractice. Of these, 6/18 (33.3%) responses involved COVID-19 restrictions where in-person sessions were not allowed for non-essential services while 7/18 (38.9%) responses expressed safety concerns. The remainder (5/18, 27.8%) did not specify. One advocate, whose loved one was having cancer, favoured telepractice as it minimised trips to the hospital and physical contact with others.
Participants were similarly afforded multiple choices for their reasons as to whether or not they would use telepractice again. 88 responses were obtained. 73.9% (n = 65) were positive responses while 26.1% (n = 23) were negative responses. Similar themes of convenience, improved access, safety and ease of use were highlighted as positive reasons for continued use. The top negative reasons included respondents’ preference for ‘personal touch’ during face-to-face visits (n = 10, 11.4%) and having reduced confidence and technical know-how in navigating video-conferencing technology (n = 4, 4.5%). The technological limitations experienced involved disruptions due to unstable internet connections, difficulty reading due to poor video quality, or therapy materials not being sent beforehand.
A small group of responders also opined about the lack of medical subsidies for telepractice, given that it was still a relatively new service that had not been approved for national subventions then (n = 4, 4.5%). No adverse events were reported.
Caregivers’ survey
The third aim of the study was to examine whether caregivers in nursing facilities perceived telepractice differently from caregivers in personal homes. All caregivers were reportedly satisfied with the service (n = 23, 100%). Most respondents rated that they would use the service again (n = 19, 82.6%). Based on Fisher’s Exact Test for small samples, there was no significant association between caregiver location and satisfaction with telepractice (2-sided p = 1.000) and the likelihood of using it again (2-sided p = 0.103).
Amongst the 26 responses from caregivers in personal homes who would use telepractice again, the top reasons for choosing telepractice were that it saved travelling time (n = 8, 30.8%), was easy to use (n = 4, 15.4%) and it reduced waiting time (n = 5, 19.2%). 3 out of 8 caregivers from the nursing facilities also agreed that telepractice saved time travelling and waiting.
37.5% (3/8) of caregivers from the nursing facilities said they would not use the service again, compared to 26.7% (4/15) of caregivers from personal homes. Of these, 2 out of the 3 caregivers from nursing facilities indicated a preference for face-to-face sessions. The nursing staff felt that they ‘can get more precise information from in-person sessions’ and ‘it is better for the therapist to interact with the patient in person’. In-person visits were also seen as an ‘opportunity for the resident to go out’. Similarly, 2 out of 4 caregivers from personal homes preferred in-person sessions as they ‘want the patient to be properly assessed by the therapist’ and they ‘can better see the therapist’s effort or feedback, more personal touch’. Although the remaining 2 out of 4 caregivers from personal homes were hesitant to use telepractice again due to cost issues, caregivers from nursing facilities cited technological and logistical reasons. One indicated that their ‘resident was hard of hearing and cannot hear well through digital means’, and ‘the clinician cannot see well from the video so staff had to repeat multiple times’. Another said that staff ‘need to set up many things but busy, has many other things to do’.
Discussion
Sociodemographic factors
Age, gender, education level and language preference did not impact user satisfaction and the likelihood of continued use. Although younger respondents with higher education levels have increased receptivity to telepractice,9,10 technological literacy and language familiarity may not have been an issue for the participants surveyed. Most of the patients surveyed cited English as a preferred language and had received at least secondary school education, while most caregivers had received up to tertiary education. High smartphone penetration rates in Singapore 25 and the exposure to high-technology devices may mean more adults can easily navigate the telepractice systems or have caregivers who can provide technical support.
Service-related factors
On the other hand, service-related factors such as convenience, improved access, safety and ease of use associated positively with participants’ satisfaction and the likelihood of continued use. These findings match the UTAUT 16 where technologies perceived as useful26,9 and requiring low-effort commitment27,28 are more likely to be adopted. Cost was a recurring concern for some respondents, who indicated they would not use the service again. These respondents expressed keenness for government subventions, which by the time of writing, have been rolled out to support telehealth. Their responses align with prior findings that high costs can be a barrier to telepractice adoption. 7
Although all respondents expressed satisfaction with telepractice, 35.5% (22/62) from personal homes and 37.5% (3/8) from nursing facilities were not keen to continue telepractice. This disparity between satisfaction and interest in continued use finds support in Orlando’s systematic review 29 where in-person appointments were preferred even though telehealth was a satisfactory option. Respondents from those studies and our research highlighted challenges in rapport building and unfamiliarity in technological aspects of telehealth as factors influencing their choice. One way to address these issues is to establish a hybrid model of service where some sessions are done face-to-face while other sessions are done via telepractice. Solution guides to commonly experienced issues could be provided to all users beforehand. This way, the patient receives benefits from both methods and the clinician-patient relationship is preserved. 30
Telepractice in nursing facilities
Despite the convenient access telepractice provided to nursing staff and patients 31 during the Circuit Breaker period, 37.5% (3/8) of caregivers from nursing facilities were not keen to continue telepractice, compared to 26.7% (4/15) of caregivers from personal homes. This finding was not unexpected given previous research had suggested reduced expertise in telehealth may lower telepractice usage amongst nursing staff19,20 Social, technical and logistical challenges were cited as reasons to discontinue telepractice. This outcome aligns with findings from a recent article 32 where overseas nursing home staff felt that telehealth could worsen social isolation for patients and increase staff burden if technological infrastructure and training were lacking.
Another reason why nursing staff in our study may prefer physical consultations could be because telepractice was introduced to nursing facilities only during the Circuit Breaker period. The quick roll-out allowed minimal time to establish processes. Other than their usual duties, nurses now have to solve IT-related problems via trial and error during telepractice. Moreover, the caregiver to patient ratio is much higher in nursing facilities than in personal homes, so staff may not have dedicated time to set up and troubleshoot.
The adoption of telehealth during the pandemic has been reported to be quicker in nursing homes that were already using the service before COVID-19. 32 Given that having experienced tech-savvy caregivers encourage successful adoption and implementation of telehealth,33–35 nursing staff could be provided with the necessary training for telepractice. Risk management protocols and guidelines delineating job roles during telepractice could also be created with nursing staff, so staff and patients feel assured of the care delivered.
Limitations and future directions
One limitation of this study is its short duration and small non-randomised sample size, with most of the data coming from one tertiary hospital in Singapore that provides adult outpatient speech therapy services. The survey did not compare users who used telepractice with those who declined telepractice as the focus of the initiative was to assess users’ satisfaction. Unfortunately, the restricted sampling made it challenging to obtain a well-balanced perspective of patients and caregivers towards telepractice. Second, the cultural validity and reliability of the survey on the population sampled could not be established. Although the questions were adapted from TUQ, TUQ’s validation study was conducted on participants from the University of Pittsburgh, where most participants were Caucasians and had at least college and above education. 23 Third, qualitative input obtained were limited in response length. More in-depth qualitative responses could be obtained in future to facilitate the transition towards technology-enabled care.
Conclusion
Telepractice has come a long way. We envision that telepractice will continue as a service delivery option post-COVID-19, particularly as the population age and the caregiving workforce shrinks. Our findings indicate that having good logistical and technological infrastructure, adequate training and developing guidelines, would help telepractice remain a sustainable alternative for delivering healthcare.
Footnotes
Acknowledgments
The authors thank all colleagues, patients and caregivers from the Speech Therapy Department and Rehabilitatio n Centre at Tan Tock Seng Hospital, as well as the Nursing Homes in Singapore for supporting this telepractice effort. We would like to specially acknowledg e: (1) Head of Department and Principal Speech Therapist Zenne T'ng Kuan Chen for supporting the initiative. (2) Principal Speech Therapist Ng Seok Kheng for encouraging the developmen t of the work. (3) Principal Speech Therapist Kwong Seh Ling for her guidance and for vetting the manuscript. (4) Senior Therapy Assistant Cheok Bee Khim for calling the patients and caregivers for data collection.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Appendix
Video consultation patient feedback survey (English/Mandarin)

| S/N | Question | Options |
|---|---|---|
| 1 | Are you您是 | • Patient病患 |
| • Caregiver看护者 | ||
| 2 | Gender性别 | • Male男性 |
| • Female女性 | ||
| • Prefer not to say不想透露 | ||
| 3 | Age range年龄层 | • < 31 |
| • 31-50 | ||
| • 51-70 | ||
| • > 70 | ||
| 4 | Highest education level attained最高学历 | • No formal education无正式教育 |
| • Primary school小学 | ||
| • Secondary school中学 | ||
| • Post-secondary education中学以上的教育和培训 | ||
| • University大学 | ||
| 5 | Preferred language(s) (tick all that applies) | • English英语 |
| 常用语言(请在所有适当的选项中打勾) | • Mandarin华语 | |
| • Malay马来语 | ||
| • Tamil淡米尔语 | ||
| • Others其他:___________ | ||
| 6 | When did you use video consultation with your clinician? (tick all that applies) | • Before COVID-19 Circuit Breaker (before 7th April 2020) |
| 请问您在哪段期间使用线上视讯的医疗服务?(请在所有适当的选项中打勾) | 2019冠状病毒阻断期前 (2020年4月7日前) | |
| • During COVID-19 Circuit Breaker (7th April – 1st June 2020) |
||
| • After COVID-19 Circuit Breaker (after 1st June 2020) |
||
| 7 | What type of service did you receive via video consultation? (tick all that applies) | • Communication发音,语言,咬字 |
| 请问您在线上视讯获得哪项医疗服务?(请在所有适当的选项中打勾) | • Swallowing 吞咽 | |
| • Others 其他:_________ | ||
| Satisfaction 满意程度 | ||
| 8 | Overall, how satisfied are you with the video consultation sessions? | • Very satisfied非常满意 |
| 总体来说,您对线上视讯的医疗服务感到满意吗? | • Satisfied满意 | |
| • Somewhat satisfied有点满意 | ||
| • Neutral中立 | ||
| • Somewhat unsatisfied不太满意 | ||
| • Unsatisfied不满意 | ||
| • Very unsatisfied非常不满意 | ||
| Ease of Use使用方便 | ||
| 9 | The video consultation system was simple to use | • Strongly agree非常同意 |
| 线上视讯系统简单易用 | • Agree同意 | |
| • Somewhat agree有点同意 | ||
| • Neutral中立 | ||
| • Somewhat disagree不太同意 | ||
| • Disagree不同意 | ||
| • Strongly disagree强烈反对 | ||
| Reliability可靠性 | ||
| 10 | The sessions provided over video consultation are as effective as in-person visits |
• Strongly agree非常同意 |
| 11 | I felt comfortable communicating to the clinician via video consultation |
• Strongly agree非常同意 |
| 12 | I felt my privacy is protected during video consultation |
• Strongly agree非常同意 |
| Interface & Interaction Quality界面和互动质量 | ||
| 13 | I could hear the clinician clearly |
• Strongly agree非常同意 |
| 14 | I could see the clinician clearly |
• Strongly agree非常同意 |
| Usefulness有用性 | ||
| 15 | What were your reason (s) for choosing video consultation? (tick all that applies) |
• Ease of use容易使用 |
| Use of Video Consultation in the Future未来使用线上视讯服务 | ||
| 16 | Video consultation sessions are as value-for-money as in-person visits |
• Strongly agree非常同意 |
| 17 | Will you use video consultation again after COVID-19 circuit breaker? | • Yes会 |
| 2019冠状病毒阻断期后, 您是否会继续使用线上视讯的医疗服务? | • No不会 | |
| 18 | Please share why you would/would not use video consultation again | |
| 请分享您为什么会/不会再次使用线上视讯的医疗服务 | ||
| 19 | Would you recommend video consultation to someone else? | • Yes 会 |
| 您会不会向他人介绍使用线上视讯的医疗服务? | • No 不会 | |
| 20 | Please provide any additional comments or feedback for our video consultation service | |
| 请对我们的线上视讯的医疗服务提供任何评论或反馈 | ||
