Abstract
Evidence has emerged that pregnant women who contract coronavirus disease 2019 (Covid-19) are at increased risk of certain forms of severe illness as well as complications requiring intensive care unit admission and resultant mortality. Teleconsultations can facilitate continuing care for obstetric patients during the Covid-19 pandemic while reducing their risk of exposure to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). In this short report, we share our experience in the provision of teleconsultations for ambulatory obstetric anaesthesia patients in our high-risk obstetric anaesthesia clinic during the Covid-19 pandemic. Appropriate labour analgesia or anaesthesia plans were able to be formulated and communicated to the patients by teleconsultation, resulting in no delay or compromise in their peripartum care. Both patients and clinicians reported satisfaction with the teleconsultation process and outcome. The considerations and challenges in setting up a teleconsultation service as well as the factors in favour of teleconsultation are also explored.
Keywords
Introduction
We share our experience in the provision of teleconsultations for ambulatory obstetric anaesthesia patients during the coronavirus disease 2019 (Covid-19) pandemic. Our institution serves as a referral centre for parturients with multiple comorbidities. The high-risk obstetric anaesthesia clinic sees parturients with comorbidities who are co-managed by internal medicine specialists in partnership with the obstetricians. These patients are referred by the obstetricians for anaesthesia assessment as part of multidisciplinary care. The goals of the clinic are the discovery of anaesthetic issues, optimisation of comorbidities as well as planning of labour analgesia and anaesthetic options. It also includes patient counselling and communication of plans to the rest of the multidisciplinary team.
Teleconsultations for delivery of essential medical services
Since the onset of the Covid-19 pandemic, there have been over 42 million cases globally (as of 26 October 2020). The national ‘disease outbreak response system condition’ was raised to ‘orange’ on 7 February 2020 indicating severe disease with limited community spread. 1 This was further escalated to a nationwide ‘circuit breaker’ lockdown from 7 April to 1 June, which imposed strict control measures. Local health authorities mandated the postponement of all non-essential surgeries and outpatient consultations. 2 These were defined as medical services that if not provided or performed would result in significant or rapid deterioration of the patient’s medical condition, and potentially threaten their health and wellbeing. Local health authorities also mandated that medical services that were suitable for teleconsultations be delivered remotely. 3
Evidence has emerged that pregnant women with Covid-19 are at increased risk of certain forms of severe illness as well as complications requiring intensive care unit (ICU) admission and resultant mortality.4,5 Furthermore, vertical transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has been reported. 6 To maintain our high-risk patients’ antenatal care and minimise their risk of exposure to SARS-CoV-2, we explored teleconsultations as an adjunct option for patients referred to our obstetric anaesthesia clinic. These teleconsultations are defined as the interactions between remote healthcare professionals and patients using information and communications technology to provide direct patient care. 7
Setting up teleconsultations in obstetric anaesthesia clinic
A teleconsultation workflow was created with approval from the institution’s medical board (Figure 1). Support was enlisted from the obstetrics and gynaecology department for this new initiative. Three clinicians underwent training on an online course addressing the use, limitations and implementation of a teleconsultation service. Locally, the provision of teleconsultations does not require licensing but is allowed for specific use cases within a regulatory sandbox to develop new models of care provision. 8 To address patient privacy concerns, we utilised a secure video conferencing software (Zoom version 5.2.0, 2020) with end-to-end encryption to prevent interception of data. This was installed on an authorised hospital laptop with only authorised personnel having access rights to the Zoom account used for patient care. No patient data were stored on the laptop and the recording function of the software was disabled. Access to the session was password controlled and circulated only to invited patients. A waiting room function controlled access into the video session to prevent the inadvertent entry of other patients into an ongoing teleconsultation.
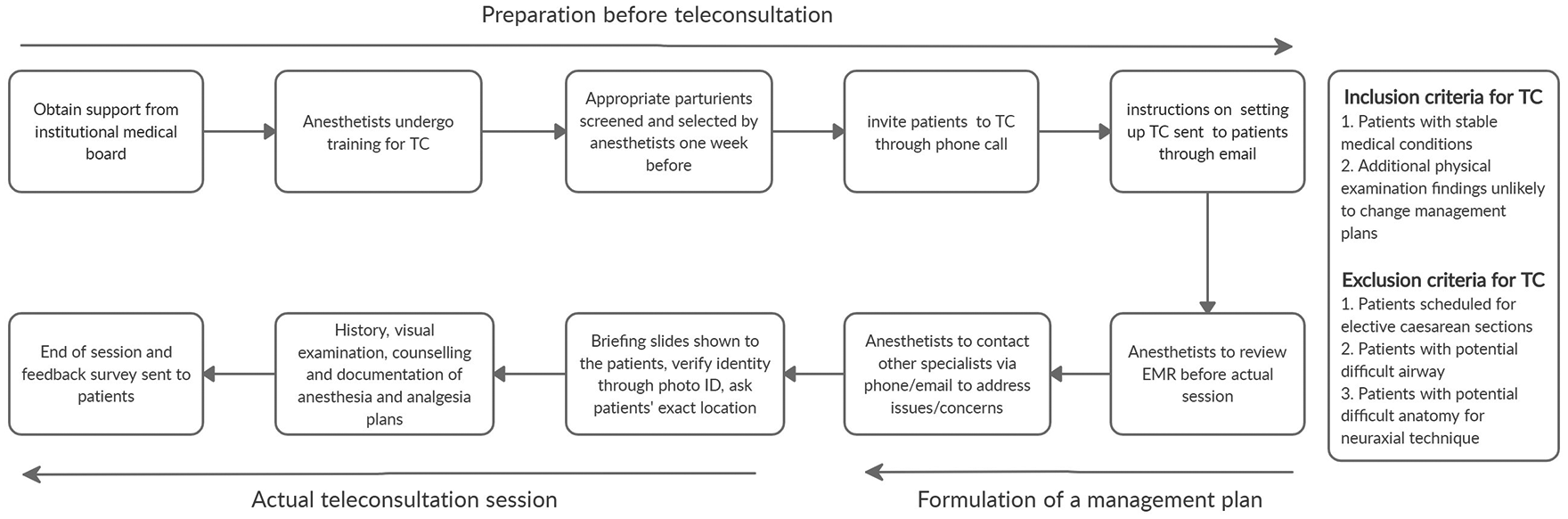
Teleconsultation workflow for high-risk obstetric anaesthesia clinic. Inclusion and exclusion criteria for teleconsultation.
Teleconsultation criteria included patients with stable comorbidities in whom the physical examination was unlikely to add additional information that would affect the formulation of labour analgesia or anaesthesia plans. Suitable candidates were screened by anaesthetists one week prior to the session. Suitable patients were invited for a teleconsultation and informed that the consultation charges would be the same as for physical consultation. Patients were excluded if they were scheduled for elective caesarean sections, as their physical presence would be needed for consent taking and blood investigations. Patients with a history of a difficult airway or medical conditions that predispose them to it were excluded. Patients with medical conditions that predispose to difficult neuraxial anaesthesia such as moderate to severe scoliosis or prior spinal instrumentation were also excluded (Figure 1). A summary of the medical conditions of the nine patients seen through teleconsultation is presented (Table 1).
Summary of patients reviewed by teleconsultation in obstetric anaesthesia clinic.

Conduct of teleconsultations
At the start of the teleconsultation, a briefing slide was shown to patients on its benefits and limitations as well as the option for a physical consult. To ensure medical care is provided for the right patient and the correct medical history is referred to, each patient’s identity was verified at the start by asking for their government-issued photo identification document to be displayed. The current exact location of the patient was asked so that emergency services could be directed if emergent medical care was required during the consultation. Patients’ electronic medical records (EMRs) were at hand during teleconsultations.
A thorough and comprehensive history was taken, recognising the inability to carry out an in-person examination. The examination is limited to what is seen and heard during the teleconsultation. Detailed history taking and attention were paid to acute symptoms warranting early medical attention. There was also a low threshold to arrange for a physical consultation if a physical examination was deemed necessary to add information that would change the anaesthetic or labour analgesia plan.
After assessment, the patient is counselled on the labour analgesia options and anaesthetic plan. This was recorded in the patients’ EMR for communication with the obstetric team. Further queries or new issues discovered during teleconsultation were communicated to the obstetric team via email. An electronic medical certificate (e-MC) was issued if required, which could be forwarded to employers. A short messaging text is sent containing a unique link to access the e-MC which is verifiable from a government repository website. 9 This eliminates the need to mail out the physical medical certificate to teleconsultation patients which potentially could be lost during the process. Among the nine patients who underwent teleconsultations, the duration varied from 30 to 40 minutes. We also issued an electronic feedback survey to patients and clinicians on their satisfaction with teleconsultation.
Benefits and shortcomings of teleconsultations
Teleconsultation is becoming an essential tool in healthcare delivery. The present pandemic has fastened its development due to social distancing requirements to minimise the spread of disease. Systematic reviews have demonstrated the use of teleconsultations in preoperative assessment and diagnosis to be both feasible and useful.10–12 Traditionally, the advantages of teleconsultation include convenience, time and cost savings. 13 During this pandemic, it has the added advantage of reducing the usage of limited personal protective equipment and reducing exposure risk to SARS-CoV-2 for parturients, a population vulnerable to more severe forms of Covid-19 and its complications (Figure 2). The factors in favour of physical consultations and teleconsultations respectively are presented (Figure 2).

Factors favouring teleconsultation and physical consultation in high-risk obstetric anaesthesia clinic.
Barriers to implementing of teleconsultation service
Barriers to the adoption of teleconsultation occur at three levels: the patient, the healthcare provider and the institution. Institutional support for teleconsultation is vital by encouraging clinicians to receive training, deploying resources for its actualisation and support from referring specialties.
A reason quoted by patients for not preferring teleconsultation is the desire to see a physician in person. This does not apply to our high-risk obstetric patients as they remain on regular follow-up with obstetricians for check-ups and scans despite the current pandemic due to the time-sensitive nature of pregnancy. The patient–physician relationship is the foundation for the delivery of therapeutic care and has traditionally been developed by face-to-face meetings. It is debated if this relationship is cultivated in telemedicine in which there is no physical encounter. However, evidence suggests that telemedicine provides comparable health outcomes when compared with face-to-face consultations without compromising the patient–physician relationship. Other common patient barriers are language barriers and unfamiliarity with mobile technology that supports teleconsultation.
Physicians may fear that teleconsultation could result in errors in diagnosis or inadequate data quality. Schoen et al. showed that a pre-anaesthetic teleconsultation evaluation is as reliable as those conducted in-person. 12 Data collected from teleconsultations were found to be adequate in making a diagnosis and forming a treatment plan. Experience in our institution supports the findings from previous studies. Appropriate labour analgesia or anaesthesia plans were able to be formulated and communicated to the patients by teleconsultation, resulting in no delay or compromise in their peripartum care. Furthermore, no changes to the formulated anaesthesia or labour analgesia plans were required during delivery. Moreover, teleconsultation does not prevent effective communication between anaesthetists and other specialists in providing multidisciplinary care.
Aids to teleconsultation service
Information can be communicated to patients by modalities other than video conferencing to enhance the teleconsultation consultation. Methods that could be incorporated include the sharing of electronic pamphlets and videos as well as phone applications offering search functions to a library of common patient concerns. These aid in patient understanding and allow the teleconsultation to focus on patient assessment and clarification of questions.
Quality assurance and legal issues
As teleconsultation is a new modality of care, standards should be followed to ensure patients receive the same level of care as if they had seen the anaesthesiologist in person. These include ensuring regulatory guidelines are followed as well as the conduct of ongoing audits and feedback to ensure standards of care are adhered to.
Surveys sent to both patients and clinicians found high degrees of satisfaction with the teleconsultation process. Clinicians were satisfied with the history taking, visual examination and patient counselling processes by teleconsultation. Patients were satisfied with their teleconsultations and did not feel their care was inferior to a physical consultation. The convenience was appreciated as they could consult from the comfort of their own home or workplace, avoiding the loss of time from work and caregiving. Patients were also keen for possible future teleconsultation sessions. Both clinicians and patients were satisfied with the audio and visual quality as well as the ease of use of the video-consultation software. None of the patients required a follow-up physical consultation for further assessment or required a change of the plans formulated from teleconsultation.
Legal issues unique to telemedicine may arise. Clinicians have to abide by local regulatory guidelines when providing telemedicine services. Patients should be informed of the nature, limitations and alternatives of remote telemedicine with clear documentation of consent for teleconsultations. Data privacy issues are a concern and robust security measures to protect the medical data collected by teleconsultation are essential. Clinicians delivering teleconsultations have to ensure the same quality of care as in-person care and outcomes should be audited. Clinicians should ensure they are qualified to deliver telemedicine services by being trained in the use of communication platforms and are able to obtain adequate patient information for care.
Conclusion
As healthcare technology rapidly evolves, teleconsultation will become a growing trend in medicine for properly selected patients, especially in the current Covid-19 pandemic. We believe the key factors for successful teleconsultations involve adequate prior preparation including technical resources, patient consent and education as well as training of staff. Proper patient selection criteria for teleconsultation are also crucial. More importantly, teleconsultation should not prevent the continuous communication between the multidisciplinary team managing the high-risk parturient. Despite the current small number of patients on trial for this service, its use should be explored further for more suitable patients to benefit from teleconsultation.
Footnotes
Acknowledgements
The author(s) acknowledge the support from the preoperative evaluation clinic nurses and administrative staff as well as Francine Tu from the obstetrics and gynaecology clinic. Special thanks to Yasar Arafat for his technical support.
Authors’ contributions
Leonard Loh, Yingke He and Un Sam Mok conceived the idea for the paper. Leonard Loh and Yingke He drafted and revised the paper. Kai Lee Ng and Hairil Rizal Abdullah helped to revise the paper.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Not applicable
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Not applicable
