Abstract
Gossypiboma is defined as mass of cotton matrix which is left in the body after surgical procedure. It is a rare complication detected after surgical procedure. This condition is under reported because of medicolegal implications. We hereby report three cases of gossypiboma encountered in clinical practice. The preoperative diagnosis of a foreign body was made in two cases. However, in one case it was misdiagnosed as a hydatid cyst.
Keywords
Introduction
Gossypiboma or textiloma are the terms used for the cotton or woven fabric left in the body cavity during surgical intervention. The first description of gossypiboma was reported by Wilson in 1884. 1 It is most frequently diagnosed in the intra-abdominal cavity and is also reported in the thorax, extremities, breast and central nervous system (CNS). The retained intra-abdominal surgical sponge results in inflammatory reaction and abscess formation. The other response may be in the form of an aseptic fibrotic reaction forming mass. It is always considered in the differential diagnosis of any patients presenting with a painful abdomen, infection or mass, and in those that have a history of laparotomy in the past. A computerized tomography ultrasound (CT) scan is diagnostic in these cases; sometimes, it may be misdiagnosed as a haematoma, neoplastic lesion or hydatid disease. Indeed, with the introduction of surgical timeouts, operating room protocols and technology (barcoded surgical sponges and scanning systems), the risk of retained foreign bodies has reduced over time. The diagnosis of gossypiboma may cause embarrassment, humiliation, loss of job and medicolegal suits. 2 We report three cases of gossypiboma, two following gynaecological procedures and one after a cholecystectomy, which was misdiagnosed as a hydatid cyst.
Clinical series
Case 1
A 42-year-old woman presented with a history of on-and-off bleeding and serous discharge per vaginum from one year. She underwent total abdominal hysterectomy for uterine fibroid at another medical facility in 2015. At presentation, vital signs were normal. Ultrasound (USG) abdomen suspected complex inflammatory mass in the supravesical region. Contrast enhanced computed tomography (CECT) whole abdomen showed a large, well-defined, thick-walled, heterogeneous intra-peritoneal mass measuring 10 × 9 × 6 cm in the infraumbilical midline region with internal air loculi, suggestive of abscess formation (Figure 1). On laparotomy, an intra-abdominal globular mass of size 12 × 12 cm was present posterior to urinary bladder. Upon manipulation, it revealed a surgical mop surrounded by pus, adhered to the adjacent structure (Figure 1). The surgical mop was torn into pieces during its removal, and pus sent for culture and sensitivity. Normal saline lavage of the pelvis was performed. Patient made an uneventful recovery and was discharged on post-operative day (POD) 9.
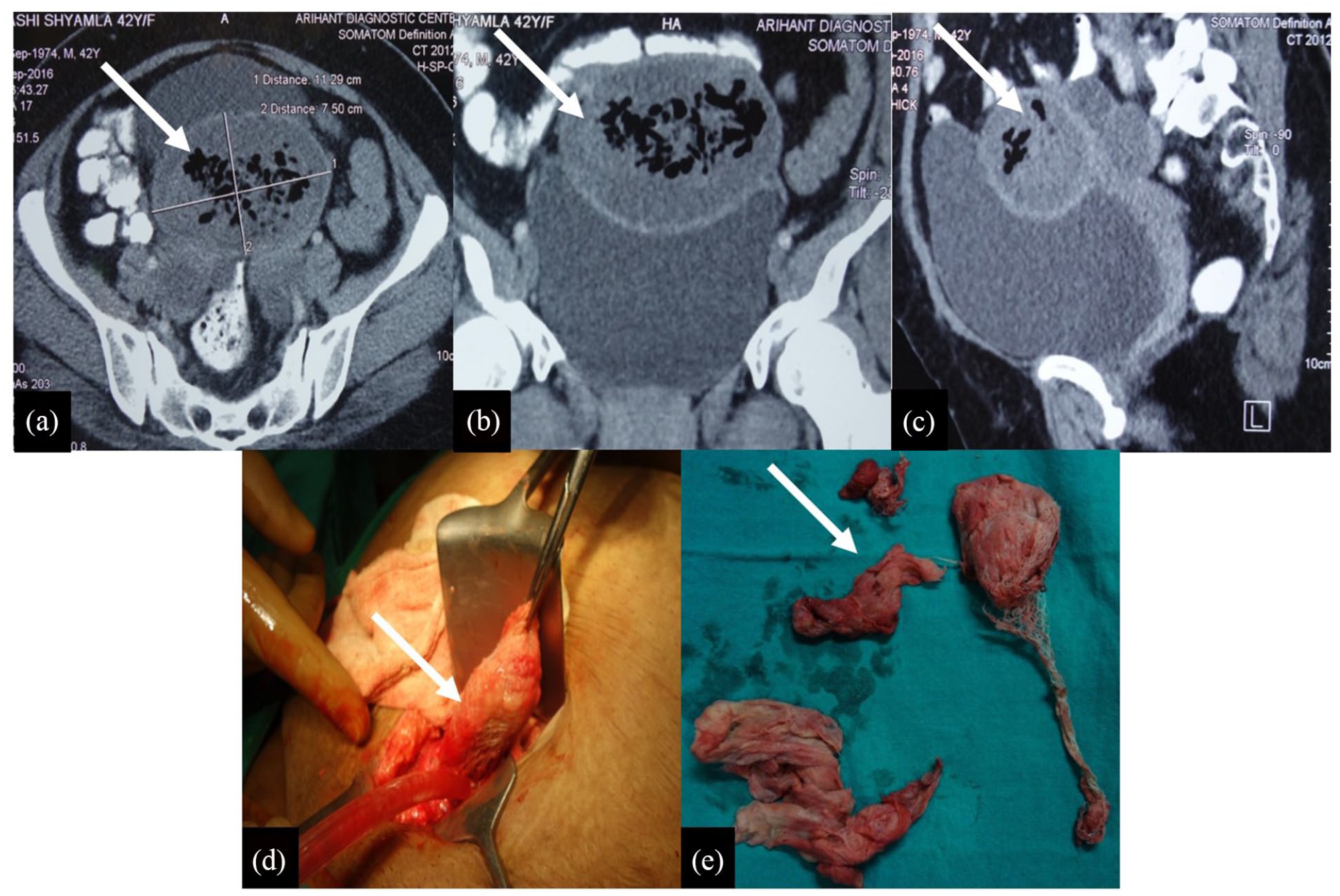
Axial (a), coronal (b) and sagittal (c) reformation of contrast-enhanced CT scan of pelvis showing a well-defined, thick-walled, heterogeneous intra-peritoneal space occupying lesion (white arrow) in the infraumbilical midline region with internal air loculi, mimicking abscess formation. (d) Operative photograph of the surgical mop being removed during laparotomy. (e) Removed pieces of surgical mop.
Case 2
A 72-year-old male presented with heaviness and discomfort in right upper abdomen from the last four years, without any history of fever, vomiting and co-morbidity. He underwent open cholecystectomy in 2008 at another hospital. At presentation, vital signs were normal and per abdomen examination revealed a firm lump measuring 6 × 6 cm in right hypochondrium, which was non tender without any local rise in temperature. USG abdomen showed the possibility of an intra-peritoneal hydatid cyst in right hypochondrium. CECT abdomen showed an intra-peritoneal complex cystic lesion in right hypochondrium with internal lamellated membrane mimicking a hydatid cyst (Figure 2). IgG and IgM Immunoglobulin G and Immunoglobulin MA lower (uterine) segment Caesarean section were negative for Echinococcus granulosus. On exploratory laparotomy, a capsulated surgical mop measuring 17 × 16 cm was present in the peritoneal cavity in right subhepatic region, which was densely adhered to the inferior surface of the right lobe of the liver, omentum and adjacent bowel, with purulent material inside the capsule (Figure 2). Pus was sent for culture and sensitivity, which was reported sterile after 48 hours. Patient responded well post-operatively, orally allowed on day 1 and discharged on POD 5.
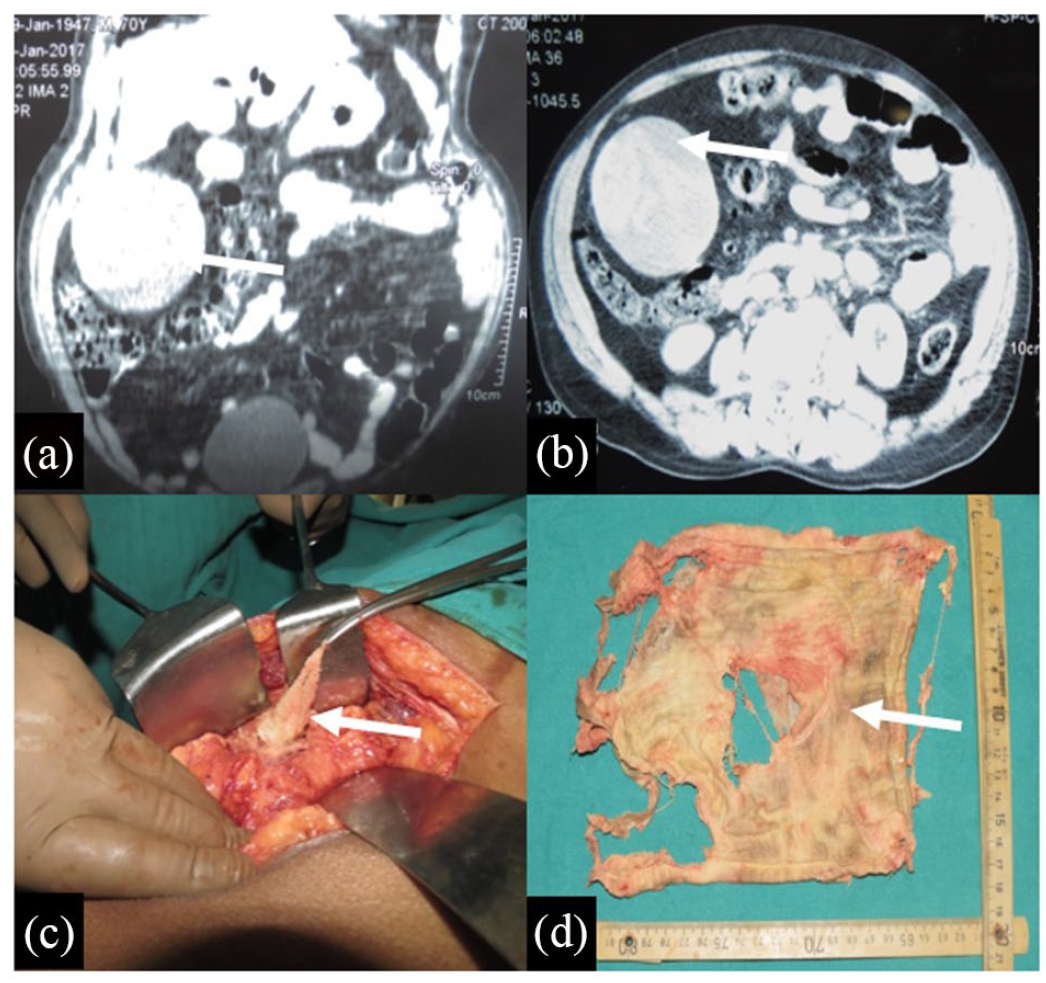
Axial (a), coronal (b) reformation of contrast-enhanced CT scan of pelvis showing a well-defined, thin-walled, heterogeneous intra-peritoneal space occupying lesion (white arrow) in right lumbar region, with wavy hyper-density, mimicking hydatid cyst. (c) Operative photograph of the surgical mop being removed during laparotomy. (d) Removed pieces of surgical mop.
Case 3
A 30-year-old female presented to the surgical outpatient department with complaint of pain in lower abdomen and purulent discharge from incision site from three months following lower segment caesarian section (LSCS), which was performed in another medical setup four months back. At presentation, vital signs were stable, and on abdominal examination, a sinus tract was present in the lower part of incision, with an underlying lump measuring 10 × 8 cm in the infraumbilical region, which had a smooth surface, was irreducible and mobile side to side, and cough impulse was absent. USG pelvis showed complex heterogeneous mass. CECT abdomen was carried out, which showed a relatively well-defined, thick-walled, air-trapped lesion noted in the posterior aspect of uterine fossa, suggestive of a foreign body; posteriorly, the lesion seemed to be communicating anteriorly – lesion abuts uterus, but fat planes are well maintained (Figure 3). Exploratory laparotomy was performed and, intra-operatively, a 10 × 8 cm surgical mop was present posterior to bladder, which was adhered to the posterior surface of the uterus and the rectal wall. The surgical mop was surrounded by foul-smelling pus, and was removed (Figure 3). Patient made an uneventful recovery.
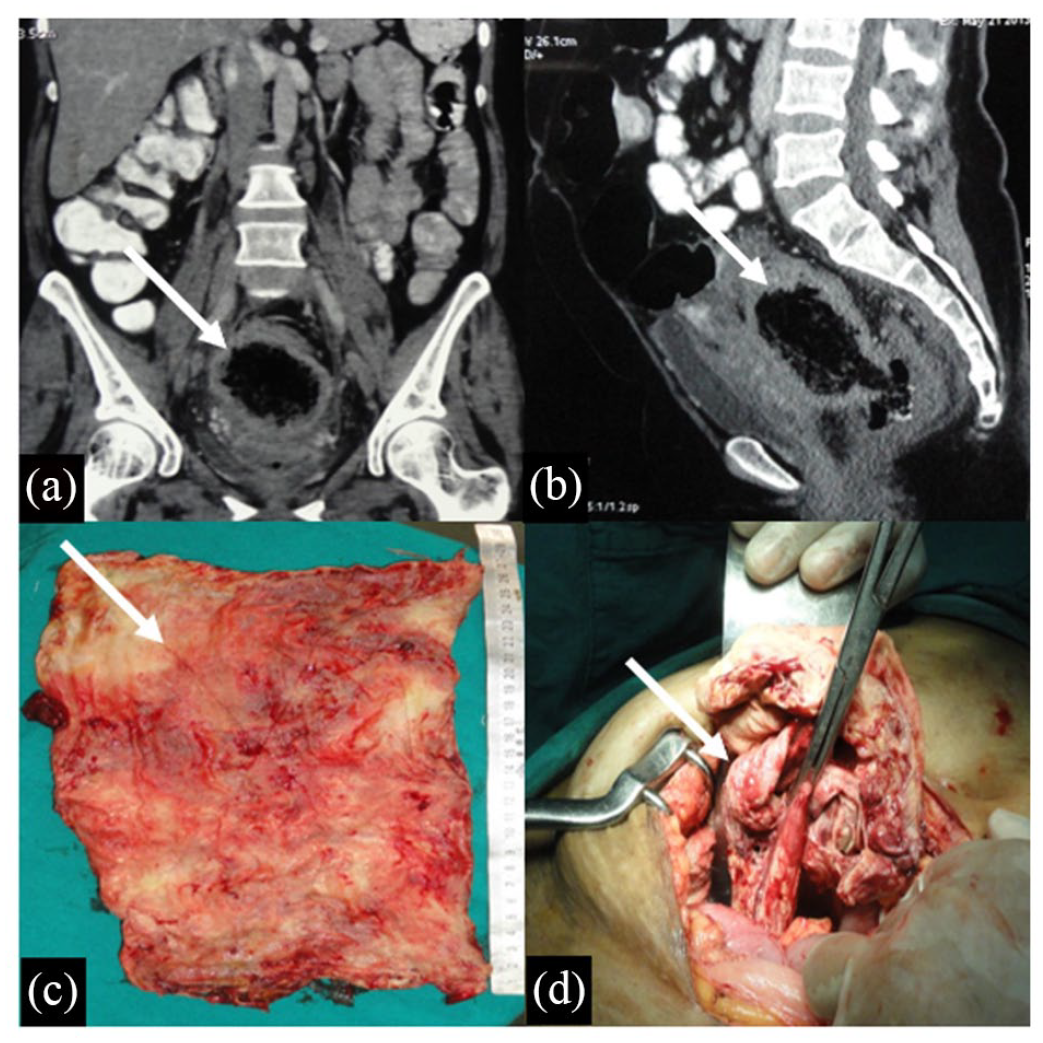
Coronal (a) and sagittal (b) reformation of contrast-enhanced CT scan of pelvis showing a well-defined, heterogeneous pelvic space occupying lesion (white arrow) in retro vesical region, with dirty air density intermixed with fluid and soft tissue density, mimicking extraluminal faecal matter. (c) Operative photograph of the surgical mop being removed during laparotomy. (d) Removed pieces of surgical mop.
Discussion
The term “gossypiboma” originates from the Latin word “gossypium” (meaning cotton) and the Swahili word “boma” (meaning place of concealment). The word “Textiloma” originates from the Latin word “textiles” (weave in) and the Greek word “oma” meaning disease, tumour or swelling. It is difficult to estimate the exact incidence of gossypiboma in clinical practice as they are under reported. However, it is reported with a frequency of one in 100–5000 for all surgical interventions and one in 1000–1500 intra-abdominal operations. 3 The leftover foreign body after surgical procedure has medicolegal implications and can result in mental agony, embarrassment, humiliation, huge monetary compensation, and even loss of job and imprisonment for the operating surgeons. At the same time, such negligence increases morbidity and mortality in patients, on top of financial loss.
Gossypiboma is most common in the intra-abdominal cavity, but is also reported in the thorax, extremities and breast. They are detected following intra-abdominal, cardiovascular, breast, orthopaedic and neurosurgical procedure. 4 The cotton pads that are left may remain silent for years. The body responds in two ways: exudative or aseptic fibrinous reaction. The exudative form occurs in the early post-operative period, and may lead to abscess formation. The aseptic fibrinous response towards a foreign body results in adhesion formation and encapsulation, leading to the development of mass.
The clinical presentation may be acute or subacute. 5 The diagnosis of gossypiboma is difficult as it is usually present with non-specific symptoms like fever, pain, pus discharge, rectal bleeding, diarrhoea and weight loss. Sometimes mass may be palpable. However, it is mostly misdiagnosed because of a low index of suspicion. These gossypiboma remain silent in the body. However, the extrusion of cotton material can occur through the fistulous tract or migration internally into the intestinal lumen, rectum, vagina or bladder. In acute presentation, it has a septic course and abscess formation occurs. In chronic or delayed presentation, encapsulation and adhesions occurs. In other rare courses, the foreign body may have transmural migration, leading to bowel obstruction or the passage of such a foreign body through the anus, which is also reported in literature.
The post-operative detection of a retained mop/sponge is difficult to detect by radiological imaging unless they have radiological markers. However, these markers may get distorted by folding, twisting or disintegration with time. Gossypiboma may be misdiagnosed as haematoma, abscess, granulomatous or neoplastic lesions. Radiographs may show a characteristic whorl-like pattern, fine opacities with mottled air densities or fistula formation. Ultrasound may show well-defined mass with wavy internal echo, hypoechoic ring and posterior acoustic shadow. The images on ultrasound may be cystic or solid. The cystic lesion has a zigzag echogenic bundle, while solid-type lesions have complex mass with hyper and hypoechoic pattern. As in our cases, heterogeneous mass was detected on ultrasound when a surgical mop was left after a lower segment caesarean section, and there was a possibility of intra-peritoneal hydatid cyst disease localized in the right hypochondrium when open cholecystectomy was done with right subcostal incision and surgical sponge left during surgery. Enzyme-linked immunosorbent assay for hydatid disease (IgG and IgM) was negative in our case, and previous ultrasound before cholecystectomy detecting cholelithiasis showed no evidence of any cystic lesion, ruling out the possibility of hydatid disease, although capsulated lesion was in favour of hydatid disease. Preoperative diagnosis of hydatid is essential to manage intra-operatively to prevent uncontrolled spillage after capsule rupture and leading to hydatid dissemination. Ultrasound was in favour of complex inflamed supravesical mass when surgical sponge was left after total abdominal hysterectomy for uterine fibroid.
CT scan is the investigation of choice in detecting these foreign bodies and associated complications. The most characteristic feature for gossypiboma is the spongiform pattern with gas bubbles. 6 The presence of a wavy-striped, high-density pattern represents the sponge. The radio marker strips in the sponge may appear as thin metallic density. In our case, a surgical sponge left after open cholecystectomy through right subcostal incision was misdiagnosed as hydatid disease. In two other cases of our series, pelvic surgery was done, leading to a retained foreign body, but CT scan was not confirmatory, with only findings of collection, thickened wall and well-defined heterogeneous mass. Wall calcification can also be observed. In chronic cases, calcification may occur along the cotton fibres, giving the appearance of a calcified reticulate rind sign. Few reports have described the magnetic resonance imaging findings of gossypiboma. It appears as hypointense on T1-weighted images and hyperintense on T2 images. The presence of well-defined, capsulated soft tissue mass with a whorled pattern on T2-weighted image is characteristic. 7
Explorative laparotomy and removal of surgical sponge may sometimes be difficult because of adhesions to the adjacent structures or fistula formation with the small/large bowel. 8 In few patients, perforation or fistula may be closed. In the presence of adhesions, perforation may be missed and lead to faecal fistula in the post-operative period. Gawande et al. described the three significant risk factors for the retained foreign body as emergency surgery, unexpected change in operation and body mass index. 3
The emergency surgical procedure increases the risk of retained foreign body by nine times. In order to prevent such an act of negligence, many countries have enacted the rule of counting the instruments and textile materials that are used during surgical procedure. Sponges with radio-opaque markers are mandatory and radiographic screening may be done in patients with difference in counts. Data sharing is not applicable to this article, as no data sets were generated or analysed during the current study. It is difficult to diagnose a retained sponge by radiographic studies in the absence of a radio-opaque marker. 9 Patient safety is the prime concern of the healthcare system. The personnel involved in the operative procedure should be aware of such a potential error. Teamwork and communication are important in preventing these errors. Barcodes may be used, and a scanner would count the sponges. An electronic chip may be embedded in the sponges and identified at the end of the surgical procedure by the use of an electronic article surveillance system using magneto mechanical technology or radiofrequency identification (RFID) microchip by handheld scanner. 10
Gossypibomas are usually preventable. Many risk factors have been identified over the years. Training of the entire surgical team, with a special emphasis on the safety protocols and an increased awareness of the possibility and the devastating consequences of this problem are crucial in preventing this embarrassing situation. Systems should be brought into place for better communication between all members of the operating team. The newer advances such as barcoding and RFID tagging of sponges may help in early identification and timely rectification in the near future, but it is always a combined, concerted, co-ordinated and complex team effort by the entire surgical team which ensures nothing is left behind after surgical intervention.
Conclusion
Gossypiboma is an avoidable but not an uncommon condition today, despite various preventive measures. It may be misdiagnosed because of a low index of suspicion. CT scan is the investigation of choice for detecting such a foreign body and its complications. Few patients remain asymptomatic; however, others may have non-specific presentations. Preventive measures should be applied with the barcoding and RFID tagging of sponges. Awareness about the missing sponges and communication among healthcare personnel of the surgical team is essential to prevent a catastrophe like gossypiboma.
Footnotes
Authors’ contributions
PK and PS acquired the data and drafted the manuscript with input of concept and design; SKT, AV and AKK reviewed the manuscript and drafted the final version. All authors approved the manuscript to be submitted.
Availability of data and materials
Data sharing is not applicable to this article, as no data sets were generated or analysed during the current study.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval was given by the Ethical Review Committee, Institute of Medical Sciences, Banaras Hindu University, Varanasi, India.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Informed consent was given for all cases included in the study.
