Abstract
Background:
Community-based audiology service is new to the Singapore’s health-care landscape. Cases deemed unsuitable to remain under audiologists’ management in the community are referred to ear, nose and throat (ENT) specialists.
Objectives:
Analysis of the clinical profiles for these referred cases revealed the local community burden of otological and auditory conditions.
Methods:
This was a retrospective, cross-sectional pilot study. Clinical records of 375 patients who were seen by audiologists at a community-based mobile hearing clinic (MHC) and warranted ENT specialist referrals were extracted for descriptive analysis.
Results:
A total of 83.73% (n=314) of patients attended their ENT appointments as advised by audiologists. Most patients (57.07%, n=234) had one condition diagnosed by the ENT specialist. One patient had four ENT conditions. Twenty-two types of otological conditions were diagnosed. Chronic suppurative otitis media, otitis externa, impacted cerumen and otitis media with effusion made up the four most frequently seen conditions in this subgroup. Twelve types of auditory conditions were diagnosed, with asymmetrical hearing loss topping the list. Sixteen types of other ENT conditions were diagnosed. Four incidental findings of vestibular schwannoma were reported.
Conclusion:
Many of the otological conditions diagnosed were chronic. Auditory conditions were predominantly hearing loss. Yet, they were found unnoticed or untreated by patients at the time of their visit to the MHC. This community-based audiology clinic had a catalytic effect on promoting timely or even early otological/hearing diagnosis and treatment. Understanding the prevailing ENT conditions of our wider population indicates the potential for growing community-based hearing health-care provision.
Introduction
The provision of health-care services is constantly evolving to meet the changing demands. An ongoing shift is the decentralising of health-care provision from the traditional hospital-centric model to one that is integrated into the community. This can be done by placing the health-care service provision in the community, by a virtual care modal such as telehealth or even by blending the two. Such types of health-care provision shall henceforth be termed the ‘community-based health-care provision model’.
The community-based health-care provision model has been well received in sparsely populated yet geographically large places in a number of ways. First, it has reduced costs for patients in terms of the monetary outlay that can be incurred when attending a medical appointment. 1 Second, it has reduced intangible opportunity costs such as time consumed and work missed.2,3 Three, it has increased convenience of access4,5 which encourages attendance 6 and reduces defaulter rates. This further translates to maximising the potential of available resources and minimising its wastage. Four, it has led to shorter wait times and earlier interventions, where any, which is made possible due to the cascade of effects from the first three points. These benefits were possible because fundamentally, community-based health-care provision such as telehealth 7 and teleaudiology 8 are able to achieve equivalent outcomes as the standard care model or better – such as earlier detection of hearing loss with no drop-out from follow-ups. 9
Singapore is not a sparsely populated or geographically large place. It is a city state, which makes it the exact opposite: densely populated and geographically small. Population density as at 1 July 2019 was 8291.9 people per square kilometre. 10 As a comparison, that of Malaysia and Australia stood at 97.2 and 3.3 people per square kilometre, respectively. 10 Actual proximity to a health-care provider may be smaller in terms of distance, but a higher population density places higher demand on the health-care providers in the locality. The ratio of residents aged 20–64 years old supporting residents aged ⩾65 years has lessened over the years, falling from 10.5 to 7.4 from 1990 to 2010 and standing at 4.5 in 2019. 11 Health-care provision needs to grow with the growing elderly population, and transform to meet the changing demands. 12
In Singapore, visiting the tertiary hospitals is one way of accessing audiology services. The existing health-care model requires residents first to obtain a specialist referral appointment via one of the 20 polyclinics found island-wide. Polyclinics provide primary care at subsidized rates. Only upon completion of consultation with the ear, nose and throat (ENT) specialist doctor at the ENT specialist outpatient clinic (SOC) can an audiology service appointment be issued. This means a twofold wait time: first, for the ENT SOC appointment and, second, for the audiology service appointment. This is a gap that can be tackled by bringing audiology services into the community.
Delivering the conventionally hospital-based audiology service in the community setting is unprecedented locally. In 2015, the National University Hospital (NUH) audiology team piloted a new hearing health-care model by establishing the research phase mobile hearing clinic (MHC). Fronted by audiologists, it offered diagnostic hearing assessment and hearing aid services to a selected group of adult patients (aged ⩾40 years) in a community setting. The diagnostic hearing assessment comprised video otoscopy, tympanometry and pure-tone audiometry (PTA). The two-year research phase of the MHC yielded very positive outcomes. In particular, 72% of patients reported that without the community-based MHC, they would never have gone for audiology services in hospital on their own accord. 13 Following the conclusion of the research phase, the MHC was officially rolled out as a community audiology service to adult patients aged ⩾21 years across Singapore.
Patients presenting with hearing loss that is symmetrical and age-related (i.e. presbycusis) are deemed appropriate to remain under the management of an audiologist at the community level. So, they do not require ENT referrals. Referrals to ENT specialists in SOC were advised according to the evidence-based guidelines (Figure 1) provided by the Ministry of Health. 14 This new community hearing care model marks the advent of audiologists being the primary contact point of patients attending audiology services. This study evaluated and reported on the clinical profiles of patients who were seen at the MHC and warranted ENT specialist referrals. This information provides an insight into the community burden of otological and auditory conditions in Singapore.
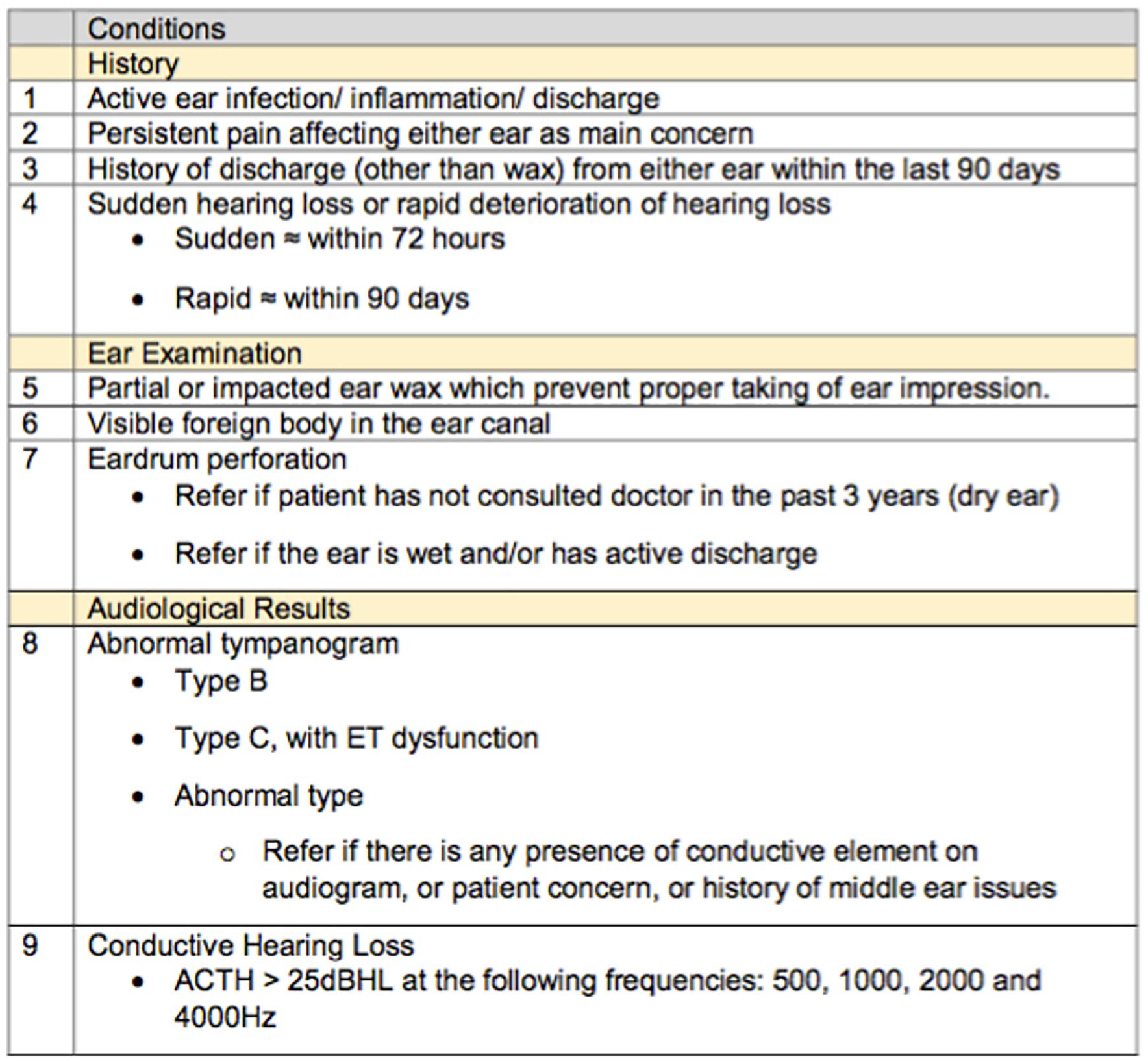
Evidence-based guidelines provided by the Ministry of Health for referrals to ear, nose and throat specialists doctors in specialist outpatient clinics.
Methods
The clinical records of 375 patients who were first seen by MHC audiologists and then referred to NUH ENT SOC between 1 November 2017 and 15 November 2018 were extracted for descriptive analysis. All of these patients fulfilled the aforementioned evidence-based referral guidelines (Figure 1). Patients came to the MHC by one of three routes: (a) the screening route – patients were advised to pursue diagnostic hearing assessment by virtue of unfavourable hearing screening results; (b) the GP route – patients were advised to pursue diagnostic hearing assessment by their polyclinic general practitioner (GP), either due to the patient’s self-reported hearing issue or from the GP’s own bedside assessment of the patient’s hearing; or (c) the walk-in route – patients visited MHC of their own volition to have their hearing checked.
Data extracted included age, sex, referral sources, conditions diagnosed by ENT specialists, where any, and pure-tone averages. A pure-tone average of 500, 1000, 2000 and 4000 Hz in the better ear (PTABE) was used for analysis. A pure-tone average >40 dBHL is considered to be disabling hearing loss for adults. 15 None of the patients were active hearing aid users at the time of the MHC consult. The data collected contained no patient identifiers and had no impact on any treatment or follow-up. Anonymity and confidentiality were maintained.
Results
Demographics
The demographics of the sample population (n=375) are presented in Table 1. Sex distribution was relatively equal. Age distribution was more elderly-centric, with the 65- to 69-year-old age group making up slightly more than a quarter of the sample (28.80%, n=108).
Demographics.
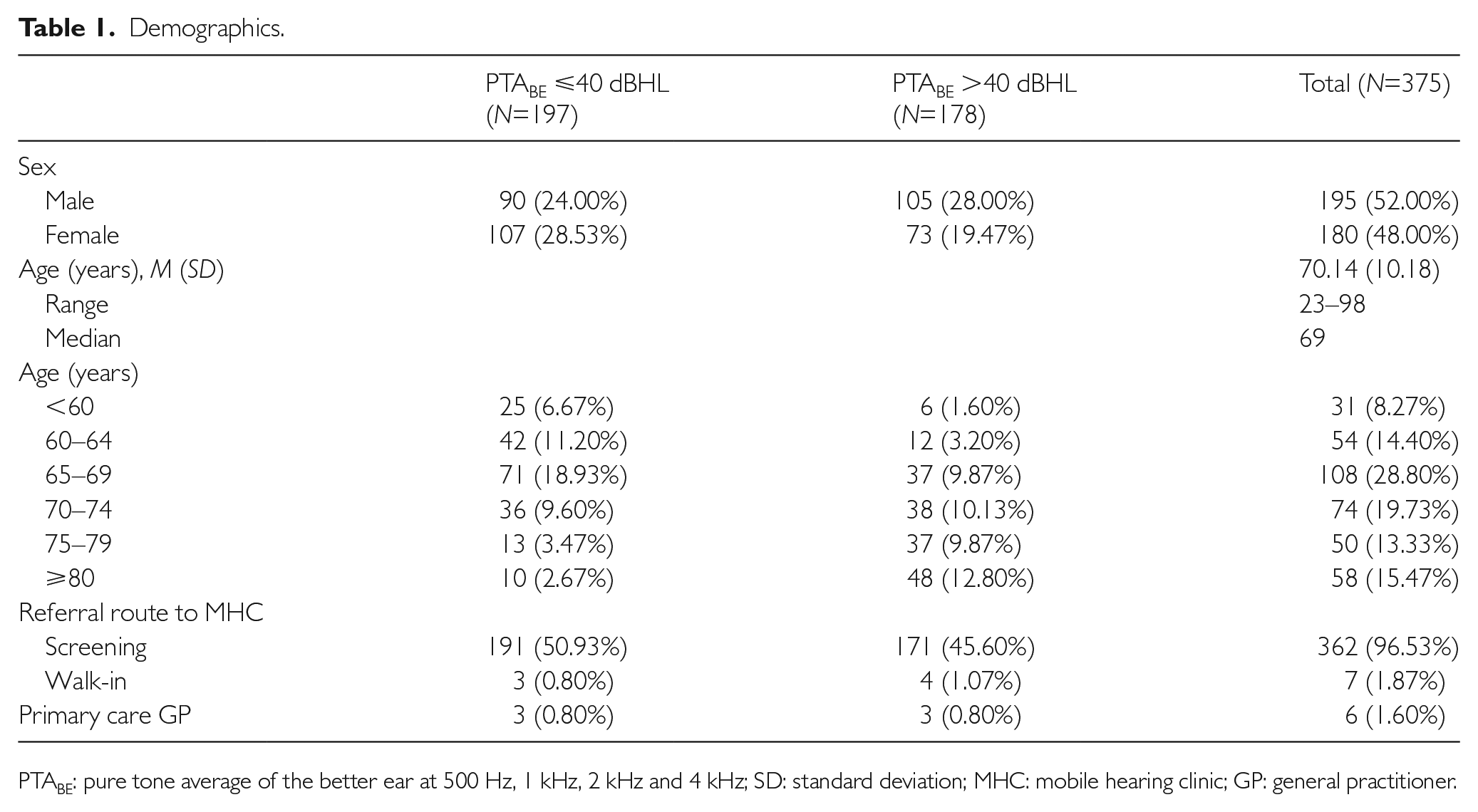
PTABE: pure tone average of the better ear at 500 Hz, 1 kHz, 2 kHz and 4 kHz; SD: standard deviation; MHC: mobile hearing clinic; GP: general practitioner.
Attendance at ENT SOC via the MHC
The attendance ratio is reflected by referral routes and age groups and is presented in Table 2. The majority of the sample came to the MHC via screening (n=362), and 83.70% (n=303) of them turned up for their ENT SOC appointment. There were fewer referred to the MHC via walk-in (n=7) and GP routes (n=6), but the latter had full attendance to ENT SOC. Overall, all age groups except those aged <60 years had an ENT SOC attendance rate >75%.
Attendance to ENT SOC by age group and by referral route to MHC.

ENT: ear, nose and throat specialist outpatient clinic appointment.
Number of ENT conditions diagnosed in each patient
Of the 375 patients referred from MHC to NUH ENT SOC, 314 turned up for their ENT appointment. Of these, the majority had just one condition diagnosed. Others had two to four conditions diagnosed. Table 3 shows the breakdown in sample by the number of ENT conditions diagnosed.
Number of ENT conditions diagnosed in each patient.

Frequency of ENT conditions diagnosed
Conditions diagnosed by ENT specialists are presented by frequency and type in Table 4. The total number of diagnosed conditions exceeds the sample population because each patient can have more than one diagnosis on the basis of having two ears. It is also possible for one ear to have more than one condition diagnosed, for instance otitis externa with underlying presbycusis.
Frequency of ENT conditions diagnosed by ENT specialist doctors.
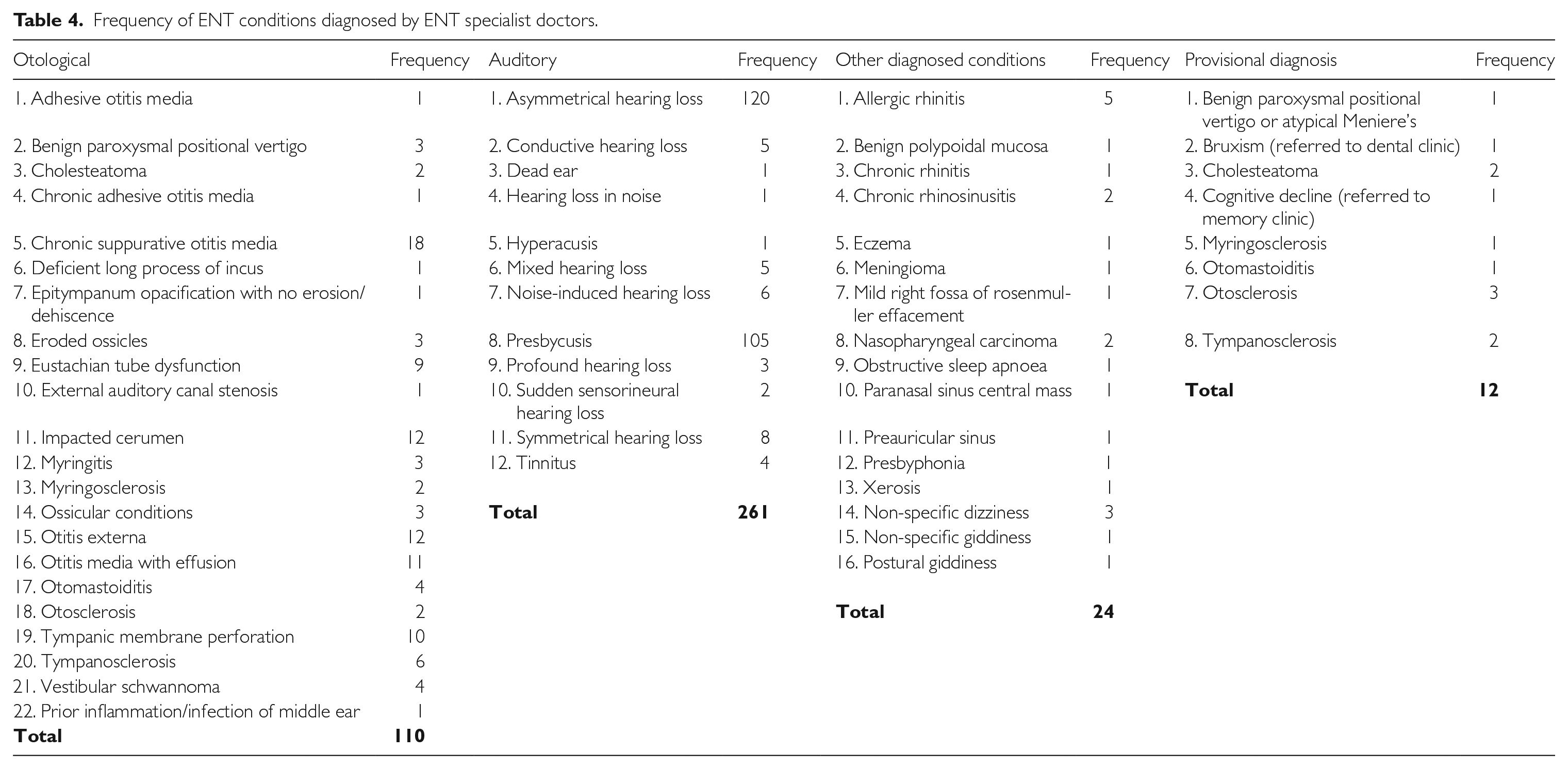
In the interests of accuracy, conditions that were provisionally diagnosed at the time of data collection remained as is. At the time of data collection, there were 12 provisional diagnoses, two of which were referred to other disciplines, with incidental findings of bruxism and cognitive decline pending further investigations. There were also non-otological ENT conditions (n=19), with allergic rhinitis (n=5) being the most common.
Discussion
Almost half the sample population (n=178; 47.47%) had a PTABE >40 dBHL. This is not surprising, as elderly patients aged ⩾60 years made up the majority of the studied population, and the prevalence of hearing loss doubles with every decade of age. 16 There were more males (n=105) than females (n=73) with a PTABE >40 dBHL, which again is in agreement with the finding of age-related hearing loss being more prevalent in men than women <80 years of age. 16 Males could have had more noise exposure compared to females17,18 in part due to greater male representation in sectors with higher noise exposure, such as production, manufacturing and construction. 19 The ages of the elderly men in the sample also corresponded with the induction into uniformed services enlistment when the National Service (Amendment) Bill was passed in parliament in 1967, suggesting the possibility of firearms noise exposure. These sources of noise exposure could have predisposed the males in the sample to noise-induced hearing loss. However, it is unlikely to have skewed the sex representation, as hearing decline with and without prior noise exposure was not found to be significantly different. 20
The overall attendance rate at the ENT SOC referred from the MHC was 83.73%, which is considered fairly high, given that this is a novel health-care model fronted by allied health professionals (audiologists). Attendance at ENT SOC appointments was highest via the GP route (100%), followed by the screening route (83.70%). The lowest attendance rate was seen for the walk-in route (71.43%). Not many could understand the importance of ear and hearing health without prior advice from health-care professionals. 21 A health-care professional’s input can wield perceptible influence on the health-seeking behaviour of individuals. This is even more marked in Asian countries such as Singapore, where the decision-making process tends to be more doctor-centric 22 than it is in non-Asian countries. Such an influence is especially important for hearing loss – a health domain well known for stigmatisation. The stigma can stem from perceived public stigma23,24 and/or self-stigma. 25 Many hearing loss sufferers exercise voluntary inattention by trying to hide their hearing loss. 26 Some even develop voluntary denial about having hearing loss. 25 These maladaptive behaviours diminish self-esteem and self-efficacy, 25 and in no way do the pressing needs for managing the conditions get appropriately addressed. These factors are demonstrated by the study’s sample population, which had no active hearing aid users, despite almost half of them having a PTABE >40 dBHL.
Every patient who attended an ENT SOC appointment (n=314) had at least one or more condition diagnosed. One patient had four conditions diagnosed: myringitis, otitis externa, allergic rhinitis and Eustachian tube dysfunction. There were 22 types of otological conditions that were diagnosed 110 times (Table 4). The top four conditions in the subgroup – chronic suppurative otitis media (16.36%), otitis externa (10.90%), impacted cerumen (10.90%) and otitis media with effusion (10.00%) – are surgically or medically treatable. Chronic discharging ears can lead to moderate conductive hearing loss, 26 which may or may not be reversible after treatment. Impacted cerumen and otitis media were also identified as acquired causes of hearing loss by the World Health Organization. 15 If left untreated, chronic otitis media can lead to profound hearing loss and even intracranial complications. 27
In a retrospective analysis of otological diagnoses from the US nationwide Emergency Department (ED) system from 2009 to 2011, suppurative and unspecified otitis media made up the biggest diagnostic category for adults (32.4% of 3,126,562 adults) followed by external ear disorder (28.8%). 28 In another study that analysed the most common otolaryngological diseases treated for 1067 patients in the ED of a hospital in Brazil over a one-year period, 29 upper respiratory tract infection (24.55%), acute rhinosinusitis (16.21%) and tonsillitis (16.25%) were more frequently diagnosed. Otological conditions such as cerumen (6.93%), acute otitis media (6.84%), acute otitis externa (5.81%) and secretory otitis media (2.34%) were comparatively fewer. These studies analysed ENT conditions diagnosed in an emergency setting. The nature of the emergency setting accounts for the higher acuity of the conditions seen compared to this study which is reflective of the community-specific ENT burden. It underpins the prevalence of untreated chronic ENT conditions in the larger community.
There were 120 (29.48%) cases of asymmetrical hearing loss reported in this study. One case was certain about the cause of the asymmetry (hit on the ear during childhood). Five cases with mild asymmetry at a single frequency were offered serial PTA monitoring. A further 114 cases were advised for further investigations by the ENT specialists, with the explanations were duly communicated. Preferring to monitor emerged as the most frequently documented reason (where available) among the 80 who declined further investigations. Thirty-one attended the radiological appointments, of whom 29 had no abnormalities detected on magnetic resonance imaging (MRI) and two had no abnormalities detected on computed tomography (CT) done due to conditions precluding MRI. Three defaulted on their radiologic appointments, as they changed their minds, preferring to monitor instead.
Asymmetrical hearing loss can manifest as a symptom of active disease, such as in vestibular schwannoma (VS). Four diagnosed cases of VS presented with asymmetrical hearing loss and other related symptoms. All their presenting symptoms were not counted as individual diagnoses in Table 4 because they were manifestations of the active disease (VS). The suggested incidence of VS is approximately 13 per million people per year. 30 It is not possible to calculate incidence from this study’s sampling, although picking up four cases of VS (1.07% of 375) from this small and very specific sample is remarkable. This could do with previously undiagnosed tumours being diagnosed at this point in time 31 by virtue of the audiology service being made available and accessible in the community. It could also be the result of this study’s subject sampling: This study has population heavily weighted to the elderly,32–34 as opposed to studies of the general population that incidence or prevalence are derived from.
The screening programme that the screening route patients went through before being referred for diagnostic hearing assessment at the MHC targeted the elderly aged ⩾60 years. Those found to have unhealthy hearing conditions during screening were seen by the MHC audiologists, who brought diagnostic hearing assessment and other audiology services to the patients right at the heart of their communities. Had these patients not been seen, the otological and auditory conditions would have been neither identified nor managed. Audiologists are therefore befitting as the community’s primary contact point of patients with hearing issues and hearing losses.
The MHC had served to bridge the gap between untreated ENT conditions in the community and conventional health-care providers, which is typically not equipped with the facilities, equipment or allied health professionals to conduct diagnostic hearing assessment in the primary-care setting. It has a catalytic effect in promoting timely, or even early, diagnosis and treatment. This is important, as the risk of significant conditions remaining unaddressed appears potentially higher in the community. 4 Whether by screening, GP or walk-in route, the MHC was the right channel for residents to learn about their conditions and to receive the audiological solutions or medical attention that they needed.
Limitations
This is the first study reporting the otological and auditory profiles of a group of patients who received audiology care in a community setting. It comes with a few limitations because of the nature of the study. First, the sample size was small and came from only one hospital. This may suggest that any form of locality-specific ENT burden in different communities cannot be ruled out. However, Singapore has a small land area, consistent infrastructure across the city state and fairly uniform weather throughout the year. These characteristics may reduce the likelihood of locality-specific ENT burdens across Singapore. Second, there was no statistical significance found with statistical tests such as the t-test or chi-square test of significance. Only descriptive analysis of the data was presented, but descriptive analysis has its merit: it has high descriptive potential, analytical simplicity and is low in cost. 29 Moreover, the data were neither self-reported nor survey based but built upon formal medical diagnosis conferred by ENT specialists, therefore lending rigor to the descriptive analysis.
Conclusion
This study provided an insight into the burden of otological and auditory conditions of the wider population by sampling a slice of the community. The majority of the otological conditions found were chronic. The auditory conditions were predominantly hearing loss. While these conditions are not acute, some of them can be symptomatic and yet were still found to be untreated or unnoticed by the patients at the time of their visit to the MHC. Being situated in the community puts the MHC in the right place to capture these patients who are either knowingly or unknowingly suffering in silence. They can then be directed to the appropriate channels for the needed audiological solutions or medical attention. With hearing loss fast becoming a front runner in the global burden of disease, 23 public awareness and early interventions are more important now than ever. Understanding the prevailing ENT conditions of the wider population can guide the long-term planning of health-care provision, public education, early intervention and preventive care. It can also help to shape future policymaking to benefit those who need help the most. In the shorter term, it emphasises the need for growing community-based hearing health-care provision.
Footnotes
Acknowledgements
We would like to thank colleagues who were part of the MHC team at the time of writing (Chiang Weichen Win, Gan Ruling, Lee Sing Yin, Lim Zhen Han and Then Tze Kang) and the brainchild of MHC’s research phase who laid the foundations for the current community audiology service (Chong Sheue Lih). We would also like to thank the Head of Department (A/Prof Loh Woei Shyang) for maintaining and growing the community audiology service.
Authors’ contributions
Z.H.L. researched the literature, conceived the study, obtained ethical approval and collected and analysed the data. Y.P.S. was involved in the cleaning of the anonymous clinical data. Author 1 drafted and revised the manuscript. J.H.Y.L. streamlined the study design, interpreted the data, critically revised the drafts and gave final approval of the version to be published.
Availability of data and materials
The data generated and analysed during the study are available from the corresponding author.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
Ethical approval for this study was obtained from National Healthcare Group (NHG) Domain Specific Review Board (DSRB; study reference number 2018/01340).
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed consent
This study required the collection of existing data. There was no research activity involving any human subjects. Therefore, informed consent was not and could not be sought. The information collected was not sensitive in nature, did not contain patient identifiers and was derived from standard clinically indicated procedures.
