Abstract
Coronavirus disease 2019 (COVID-19) can lead to coagulation activation and venous thromoembolism (VTE), with an incidence of around 25–27%. Patients admitted to the intensive care unit (ICU) are at highest risk. There are not many studies reporting its incidence in non-ICU patients. A large number of COVID-19 patients in Singapore, with symptoms ranging from mild to moderate, have been admitted to either Community Care Facilities (CCF) or in general wards of Public Healthcare Institutions (PHI). In case there is a surge of COVID-19 patients, there is a possibility that general wards in PHIs may need to admit an increasing numbers of acutely ill patients, with only the critical ones being admitted to ICU. The incidence of VTE in non-ICU patients is not exactly known and its detection in these patients is challenging. Thus, the healthcare staff managing these patients at the CCFs and general wards at the PHIs should be vigilant and monitor these patients for development of signs and symptoms of deep vein thrombosis, as well as trend D-dimer level. An algorithm for a potential approach to manage VTE in non-ICU COVID-19 patients is described. A prospective study is needed to establish the incidence of VTE in non-ICU patients in Singapore and the predictive value of D-dimer levels to detect this risk, as well as a therapeutic protocol to initiate appropriate pharmacological thromboprophylaxis in these patients.
Introduction
Out of the total 29,812 COVID-19 patients in Singapore up to 21 May 2020, the majority have been admitted at Community Care Facilities (CCF) and general wards of Public Healthcare Institutions (PHI). Few patients have required admission to Intensive care Units (ICU). Coronavirus disease 2019 (COVID-19) can lead to coagulation activation and venous thromoembolism (VTE), which comprises macro-vascular thrombosis such as deep vein thrombosis (DVT) and pulmonary embolism (PE), and also micro-vascular thrombosis. Older, bedbound patients and those with underlying medical conditions such as sepsis, malignancy, recent surgery, patients requiring ICU admission and those with a previous history of VTE are at a higher risk.
Text
The incidence of VTE in COVID-19 patients is not definitely established, but recently published studies have reported an incidence rate of 25–27%. 1 Klok et al. reported a higher incidence of VTE in COVID-19 patients admitted to ICU. 2 Acute PE was detected on computed tomography (CT) pulmonary angiography in 23% patients with severe COVID-19. 3 The increasing reports of VTE in ICU patients in recent studies may also be due to increased screening in these high-risk patients.
But there are not many studies reporting the incidence of DVT in non-ICU COVID-19 patients. A study reported that out of the total number of non-ICU COVID-19 patients who had signs of DVT, 50% of them were detected to be positive on Doppler compression ultrasound scan, with the thrombus most frequently detected in the iliac-femoral-popliteal veins. 4 Two single-center studies have reported a 3% and 6% risk of VTE, respectively, in patients admitted to the ward. This risk is higher compared with non-COVID-19 patients who are hospitalized in the wards.5,6
Three CCF centers have been set up in Singapore, at D’Resort, Singapore EXPO and Changi Exhibition Centre. A fourth CCF is being set up at Tanjong Pagar Terminal. They were initially designed to accommodate recovering COVID-19 patients, but they subsequently started to take in COVID-19-positive patients with relatively mild symptoms. Also, after release of the circuit breaker, in case there is a surge of COVID-19 patients, there is a possibility that general wards in PHIs may need to admit increasing numbers of acutely ill patients, with the critical ones being admitted to ICU. The detection of PE and DVT may be challenging in non-ICU COVID-19 patients. The exact incidence of VTE in this group of patients is not known. Some of these patients already suffer from shortness of breath due to COVID-19, occasionally associated with borderline low oxygen saturation, thus suspecting a diagnosis of PE may be more difficult. Moreover, doctors are primarily focusing on the respiratory symptoms, and hence systematic examination of the lower limbs for signs of DVT is often overlooked. Therefore, healthcare staff managing these patients at the CCFs and general wards at the PHIs should be vigilant and monitor these patients for development of signs and symptoms of VTE (e.g. DVT and PE).
To date, there is no clear pathogenesis of VTE in COVID-19 patients. Cytokine storm in COVID-19 can lead to stimulation of pro-coagulant factors such as D-dimer, which is a widely used but non-specific biomarker to diagnose VTE. COVID-19 may cause elevated D-dimer levels not only due to hypercoagulability, but also because of inflammation, infection and advanced age. 7 D-dimer is elevated in many patients at the time of admission, with one study reporting that 68% of hospitalized COVID-19 patients had elevated D-dimer levels. 8 Patients who died from COVID-19 had higher D-dimer level on admission as compared with those who survived. 9 This may suggest that increased activation of the coagulation cascade may co-relate with severe disease. Elevated D-dimer level cannot eliminate the presence of VTE in this group of patients, nor does its level at presentation co-relate with the future development of VTE. 10
The exact relationship between D-dimer level and COVID-19, and the change in level during disease progression, is not fully studied. Cui et al. showed a D-dimer cut-off value of >1.5 µg/ml had a sensitivity of 85%, a specificity of 88.5%, and a negative predictive value of 94.7% to predict VTE. 1 Another study reported that a D-dimer cut-off value of 1.57 µg/ml had a sensitivity of 95.7%, specificity of 29.3%, positive predictive value of 19% and negative predictive value of 97.5% to rule out asymptomatic DVT. The prevalence of DVT was 3.8%, 10.5% and 25.8%, when D-dimer was categorized into the range of 1.0–1.8 µg/ml, 1.801–2.65 µg/ml and >2.65 µg/ml, respectively. 11
Current international guidelines recommend thromboprophylaxis with low-molecular-weight heparin (LMWH) or unfractionated heparin for ICU patients with confirmed VTE, or those who are at a higher risk of developing VTE. 12 A study by Klok et al. recommends pharmacological thromboprophylaxis for all COVID-19 patients admitted to the ICU. 2 Some studies recommend administration of prophylactic dose of LMWH in all hospitalized COVID-19 patients. 13
Due to patient surge during this pandemic, an increasing number of acutely ill patients may be admitted in the non-ICU setting. As these patients may at higher risk of developing VTE as compared with the low-risk patients, they may need to be initiated on prophylactic thromboprophylaxis, even in the absence of confirmed VTE at the time of admission. When to initiate anticoagulation remains controversial. For now, these decisions must be made on a case-by-case basis, considering the risk of VTE. Rather than treating all COVID-19 patients in non-ICU setting with prophylactic anticoagulation, these patients should maintain adequate hydration and they should also be encouraged to mobilize and perform static exercises. In patients without risk factors for hemorrhage, thromboprophylaxis may be reasonable for those with a baseline D-dimer level >1.5 µg/ml. Healthcare staff at CCFs and in general wards of the hospitals should regularly monitor patients for development of signs and symptoms of DVT, as well as D-dimer level trend. If there is a clinical suspicion of a patient developing VTE or a rising D-dimer level, the patient should be promptly referred to the hospital for Doppler ultrasound scan for DVT or CT pulmonary angiography for PE (Figure 1). This will aid early diagnosis, initiate anticoagulation and avoid complications.
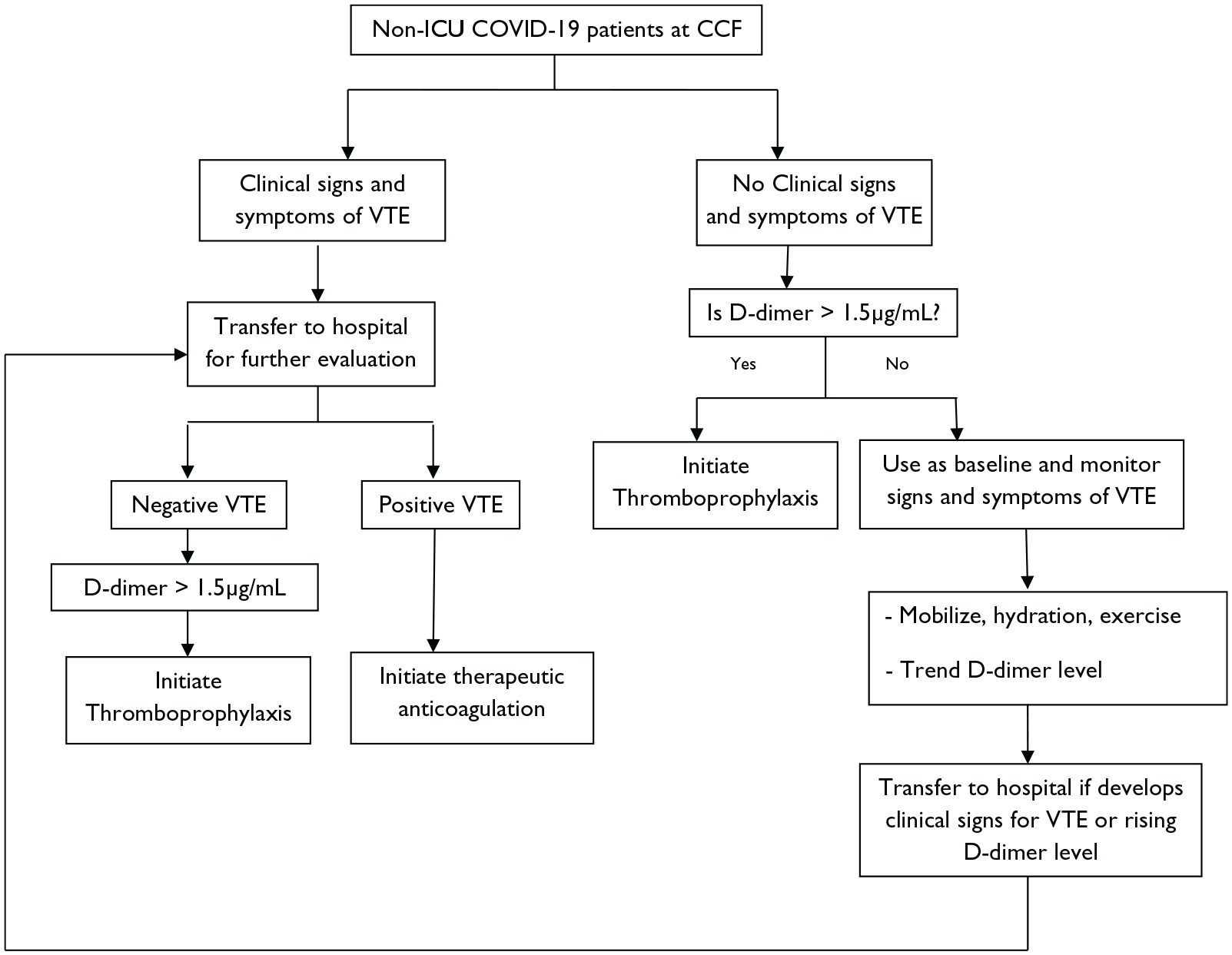
Algorithm for a potential approach to managing VTE in non-ICU COVID-19 patients at CCF.
Conclusion
Looking at the scarcity of data regarding the risk of VTE in non-ICU patients to date, and given that the majority of patients are currently being admitted in non-ICU setting in Singapore, a higher cut-off level for D-dimer might be necessary for the diagnosis of VTE in non-ICU COVID-19 patients. It is also reasonable to conclude that anticoagulation should not be initiated only based on the D-dimer level; but a high index of suspicion, combined with frequent examination for signs and symptoms of VTE and a rise in D-dimer level, may suggest the need to initiate thromboprophylaxis. A prospective study is needed to establish the incidence of VTE in non-ICU patients in Singapore and the predictive value of D-dimer levels to detect this risk, as well as a therapeutic protocol to initiate appropriate pharmacological thromboprophylaxis in these patients.
Footnotes
Acknowledgements
None.
Author contribution
SP conceived the idea for the manuscript and also contributed to the writing and editing of the review.
Availability of data
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study.
Ethical approval
Not applicable.
Informed Consent
Not applicable.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Not applicable.
Meeting
This manuscript has not been presented in abstract form at any meeting.
