Abstract
Here, we describe the case of a 67-year-old man who had been under surveillance for solitary pulmonary nodule for two years and was diagnosed with malignancy via electro-navigational bronchoscopy (ENB). Surveillance computed tomography scan of the thorax showed annual growth increments of the pulmonary nodule. In view of his Brock score showing a 35% probability of malignancy, the patient was subjected to ENB, and metastatic adenocarcinoma from the gastrointestinal tract was diagnosed. ENB was done using a machine on loan from Veran Medical Technologies. The procedure was successful, with no immediate or long-term complications. The diagnosis following histopathological examination was adenocarcinoma, and he was subsequently referred to our oncology unit for further management.
Introduction
Electro-navigational bronchoscopy (ENB) is a novel diagnostic tool, with a high positive yield of up to 94% sensitivity in tissue sampling of peripherally located solitary pulmonary nodules. Even though it is currently not readily available in Malaysia due to cost, lack of facilities and expert personnel to carry out the ENB, current evidence shows that not only does it give a higher yield, it is also among the safest method available to interventional pulmonologists in targeting solitary pulmonary nodules. This case report showcases the safety and successful biopsy of solitary pulmonary nodules via ENB in our local community, and it serves as a benchmark to guide future development in the field of interventional pulmonology in Malaysia.
Case presentation
A 67-year-old man with underlying co-morbidities, including type 2 diabetes mellitus, hypertension and ischaemic heart disease, had been under follow-up at our respiratory clinic for a solitary right upper-lobe lung nodule since 2015. The nodule was picked up incidentally from a computed tomography (CT) scan of the thorax that was done to investigate the cause for his slightly raised estimated systolic pulmonary arterial pressure (eSPAP). He was asymptomatic.
A chest radiograph (Figure 1) did not reveal any nodules. However, from his yearly CT surveillance scans (Figure 2(a) and (b)), it could be seen that the nodule was slowly increasing in size. The increase from 2015 to 2016 was small, and the decision for delaying tissue sampling was made in view of him being asymptomatic and the slow growth of the nodule. A further CT scan of the thorax in 2017 (Figure 2(c)) showed a spiculated lesion with associated surrounding reticulation in the anterior segment of right upper lobe, measuring 1.0 cm×1.4 cm. The Brock University cancer prediction equation was calculated, which showed that the probability of cancer was 34.82%. The 2017 Fleischner Society Pulmonary Nodule Follow Up and Guidelines suggest that either the nodule should be followedd up with a CT scan or positron emission tomography (PET) CT scan in three months or tissue sampling should be undertaken.
Chest X-ray showing normal findings.

Serial computed tomography scan of the thorax. Coronal views in (a) 2015, (b) 2016 and (c) 2017 showing a spiculated nodule in the anterior segment of the right upper lobe measuring 1.0 cm×1.4 cm.
The decision was made to undertake tissue sampling due to the high suspicion of malignancy. Because of the location of the nodule, tissue sampling was planned to be done using ENB. A virtual airway leading towards the suspicious right upper-lobe lung nodule was constructed from inspiratory and expiratory CT images, giving the bronchoscopists a clear view for a successful procedure. After a negative study from a flexible bronchoscope, a transbronchial lung biopsy was attempted under the guidance of ENB via bronchoscopy with a 2.8 mm working channel.
No immediate and late complications were seen. The tissue sample taken was reported as metastatic adenocarcinoma from the gastrointestinal tract, as immunohistochemical staining revealed strong positivity for cytokeratin 20 and was negative for cytokeratin 7 and thyroid transcription factor 1. The patient was referred to our oncology unit for chemotherapy and further follow-up.
Discussion
Among the novel diagnostic tools in the field of interventional pulmonology is navigational bronchoscopy. It has been gaining approval as the tool of choice in the diagnosis of peripheral and/or solitary lung nodules. Two forms of navigational bronchoscopy are available: ENB and virtual bronchoscopic navigation (VBN). In general, ENB has five components and needs three stages to be carried out. The five components are a low-dose electromagnetic field created around the patient, software creating a three-dimensional (3D) virtual airway, a sensor device, a display interface and a working channel. 1 The three stages required are planning, navigation and biopsy. Once a 3D route to the lesion has been planned using CT images, a bronchoscope is navigated to the targeted lobe after linking the virtual fiducial registration point. A needle biopsy is then advanced until it reaches the targeted lesion. 2 To date, two different commercially available systems exist that uses ENB: (a) the SpiNDrive (Veran Medical Technologies, Inc., St. Louis, MO) that is able to ‘track’ instruments and thus improves the accuracy, and (b) superDimension ENB (Medtronic, Minneapolis, MN) which is widely used.
VBN displays 3D images of the tracheobronchial trees that are matched with actual images. The bronchoscope is then advanced to the targeted lesion. To date, VBN technology is carried out using the aptly named LungPoint® VBN System from Bronchus Technologies, Inc. (Mountain View, CA). 3
There are different modalities available to be utilised in tissue sampling of solitary lung nodules, each with their own advantages and disadvantages. These include transthoracic percutaneous CT-guided lung biopsy, ultrathin (outer diameter of 3 mm) bronchoscopy and radial endobronchial ultrasound (EBUS). CT-guided transthoracic biopsy has an overall sensitivity of up to 82%. 4 However, it needs an accessible window for core needle insertion, and the rate of complications may also be as high as 30%. 5 On the other hand, EBUS has a sensitivity of up to 77% in the hands of an experienced operator. 6 However, Eberhardt et al. reported a decrease in diagnostic yield for lesions <20 mm. 7 Ultrathin bronchoscopy is capable of reaching up to the eighth generation of the bronchi. However, it requires a very experienced bronchoscopist, and it is not available in most places. Table 1 summarises the sensitivity of the different diagnostic modalities.
Sensitivity of different diagnostic modalities for pulmonary lesions.

CT: computed tomography; EBUS: endobronchial ultrasound.
The diagnostic yield of ENB (Table 2) has been reported, with a wide range of sensitivity from 59% to 94%.8–14 This could be explained by different selection criteria and protocols in the studies. Several factors have been recognised to improve the yield from ENB. The presence of a positive bronchus sign on CT images as shown by Brownback et al., 9 use of rapid on-site cytopathological examination 10 combined with EBUS and PET scan improved the success rate of biopsy.11–13 In a study by Eberhardt et al., 13 there appears a non-significant trend towards an increase in the diagnosis of lesions in the right middle lobe, and Chen et al. 14 further note that lesions in the lower lobes are much more challenging to be sampled from.
Diagnostic yield of ENB.
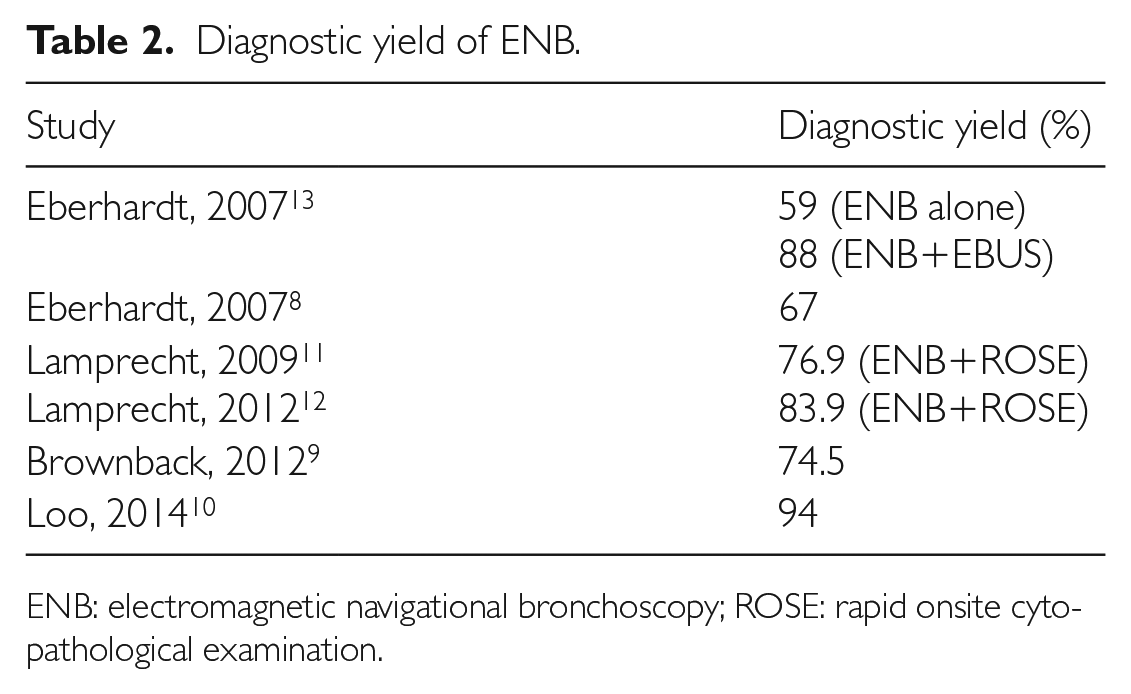
ENB: electromagnetic navigational bronchoscopy; ROSE: rapid onsite cytopathological examination.
Conclusion
ENB is a safe procedure with high positive yield in sampling of peripherally located solitary pulmonary nodule. Due to its specificity and safety profile, a serious effort should be made so that ENB is made readily available in most centres. This includes training of the operators, reducing the cost and preparing the facilities with the infrastructures and equipment needed. ENB is one of the modalities available in tissue sampling, however, it is not superior and does not render other modalities obsolete. Rather, a careful selection and individually tailored based on size, location and feasibility should be considered to get the best outcome for tissue sampling.
Footnotes
Acknowledgements
The authors would like to thank all participants for their involvement and cooperation during the procedure. We are also grateful to Veran Medical Technologie, Inc., for loaning us an ENB.
Authors’ contributions
F.A.H. and A.S.M. were both involved in the literature review, data collection, data analysis and paper write-up.
Availability of data and materials
The data sheets generated and analysed during the study are available
Ethical approval
non applicable.
Informed consent
Written informed consent was obtained from the patient.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
