Abstract
Introduction:
Nurses are among the largest potential users of electronic medical record (EMR) systems in health care settings. Yet little is known about their perceptions and confidence toward using such systems. This study explored nurses’ perceptions toward and confidence in using the EMR system. Predictors for confidence status in using the system among nurses were postulated.
Methods:
A cross-sectional survey design was used. A sample of 169 nurses were recruited from a general governmental university hospital in Muscat, Oman.
Results:
Most of study participants did not have prior experience with EMR systems elsewhere. About half (52.1%) perceived that they were confident in using the system. A logistic regression model showed nurses who (a) had six or more years of experience in using the system, (b) perceived that their suggestions regarding improving the system were taken into consideration by the system managing team, (c) perceived that the changes introduced in the system were important to their work, and (d) perceived that the information retrieved through the system was updated, to be more likely confident in using the system.
Discussion:
When customizing the EMR system, the informatics team that manages the system is invited to more consider suggestions for improvement that are raised by nurses. More training on the system is suggested to increase confidence among nurses who had little experience in using the system. In order to enhance the preparation of future nurses with contemporary technology-driven health care practices, nursing schools officials are encouraged to include general computer information technology training into nursing curricula.
Introduction
Electronic medical record (EMR) systems have been available in health care settings for several years, with usage of the system increasing worldwide.1–4 The potential to improve patient care outcomes, health care providers’ performance, and reimbursement activities have been the core motives for using such computerized clinical systems.4–6 Incorporating evidenced-based practice tools into the EMR system may promote decision making at the point of care and improve health care quality. 7
As more options and functionalities within the EMR system for managing patient information become available, there are rising expectations that health care practice could be either helped or hindered by such systems.8,9 Understanding human-technology interactions helps overcome barriers to use, as well as maximize available resources in the name of providing high-quality care.
Little is known about perceptions of health care providers, including nurses, toward the use of EMR systems and their level of confidence in using these systems. Given that nurses are the largest group of potential users of EMR systems in health care settings, it is therefore important to understand nurses’ interactions with EMR systems and the ensuing impact on nurses’ activities and routines.10,11 Internationally, insufficient studies1,3,7,8,11–27 have examined the effects of EMR use among nurses. Among those carried out, conflicting findings have been found.
Nurses’ acceptance of the EMR system is necessary for the integration of the EMR system with patient-centered nursing care activities. 27 Not surprisingly, such an acceptance of the system by nurses depends on nurses’ perceptions of possible benefits that EMR use brings to the quality of health care. 24
EMR use by nurses requires effectiveness and efficiency in order to improve or achieve quality health care for patients. Effectiveness is achieved when EMR use assists nurses in achieving accuracy and completeness in their health care activities. Efficiency refers to resources expended in relation to the accuracy and completeness with which nurses achieve such activities. Rose et al. 14 conducted two independent ethnographic qualitative studies to validate the EMR’s effectiveness and efficiency. The authors found that customizing the EMR system was key to the usability of the EMR system.
In a study by Eley et al., 12 the authors found that increasing age was positively correlated with lower confidence level in using the EMR system. In a descriptive phenomenological study conducted by Kossman and Scheidenhelm, 13 nurses who worked on medical-surgical floors and intensive care units believed that EMR use made them more organized. This belief came about because the EMR provided task lists and computerized charting, which made them less dependent on memory or written notes.
A study by Gonzalez et al. 24 found that nurses did not think positively of the EMR system. This was because nurses were not sure of a reduction in time required to document nursing care, despite use of the EMR system, whereas, some studies supported the notion that EMR use significantly deceases nurses’ documentation time and increases time spent in direct patient care.2,3,8,16,21 Bosman et al. 2 compared documentation time between two groups of nurses utilizing paper- and EMR-based systems and found a 30% reduction in patient documentation time in the group using the EMR system. Donati et al. 3 similarly found nurses take less time recording data utilizing an EMR system compared to using paper. In a study by Lambooij et al., 8 nurses considered the EMR system easy to use and aligned with their clinical routines, allowing less time between patient encounters and entry of clinical data.
In a systematic review, Gephart et al. 23 examined nurses’ experiences of unintended consequences arising from switching to an EMR system. Although the nurses experienced changes in workflow, faced continuous adaptation to meet patients’ needs when dealing with imperfect EMR systems, and encountered difficulty accessing patient information, they were still unwilling to revert to paper records. Similarly, Tubaishat 26 evaluated an EMR system use among nurses in Jordan and found them to favor EMR use over paper-based medical record systems. Moreover, nurses were satisfied with the EMR system and agreed that it supported the provision of high-quality care.
EMR use should enable all health care providers, including nurses, to view pertinent data quickly so that accurate decisions can be made both in life-threatening and non-life-threatening situations. As such, its use is crucial to providing safe and quality care measures. 28 EMR use facilitates nurses’ documentation of more specific topics such as patient education, the need for restraints, and assessment of pain. 16 EMR should also enable nurses to prevent errors, since error messages pop up in the event of errors.
Some organizational factors may affect EMR use. These include whether there are sufficient numbers of terminals (which reduces or eliminate wait time), and also significantly affects the use of the EMR system. 29 Eley et al. 12 found that access to computers was the main barrier faced by nurses to EMR use in the workplace. Limited training on how to use the EMR system also decreases the confidence of its usage among nurses, and thus, affects quality of care provided. In addition, quality of patient care decreases with EMR use when less time is spent at the patient’s bedside, and its accompanying loss of personalized care. 29
Schenk et al. 25 explored the perceptions and confidence of nurses toward EMR use. They found nurses to believe the EMR system did not improve patient care, leading to low confidence in using the EMR system.
Confidence in using the EMR system is a prerequisite to optimum use of the data in the system; as well as eliciting data. Nurses who use the EMR may feel that they are unable to acquire and maintain a mental overview of their cases merely by viewing electronic records. For instance, some nurses may feel insecure about identifying emerging health problems of their cases merely by clicking through the different EMR system’s screens. These nurses would be at a high risk of performing medical errors. 30 It is hence important to consider nurses’ perceptions about the EMR system and the level of confidence they have concerning the system. This assists in identifying positive steps to influence EMR use; it also helps rectify misinformation.
Hence, understanding how EMR use among nurses affects them is imperative and vital. 10 In Oman, no studies have been conducted to understand nurses’ and other health care providers’ perceptions on EMR use, as well as their confidence levels regarding EMR use.
This study was thus carried out to answer the following research questions: (1) What are the perceptions of nurses toward the EMR system? (2) What is the level of confidence of the nurses in using the EMR system among nurses? (3) What are the relationships between the variables in the study, and level of confidence in EMR use? (4) What are the predictors for nurses to feel confident in EMR use?
Methods
Design
A cross-sectional survey design was used.
Setting and sample
Participants were nurses who worked at a general governmental university hospital in Muscat, Oman. Using a comprehensive list that contained all practicing nurses at the hospital (
The inclusion criteria for participation were: (a) employment in the participating hospital for at least three months to allow for time to have experience using the EMR system, (b) use of the EMR system as part of routine duties at the work unit, (c) the ability to read and write the English language, and (d) provision of informed consent for participation.
Nurses who met the inclusion criteria were invited to participate on a voluntary basis between March and October 2014. Anonymity and confidentiality of the responses were ensured. Before making the decision to participate, the objectives, nature and risks of the study were explained verbally. The consent forms were collected, indicating agreement to participate. As per the approved study protocol, additional blank copies of the consent form were provided to each individual to keep for their records. The forms had complete contact details of the principal investigator and institutional review board for research. As a token of appreciation, each participant was given an 8 GB flash drive.
Measurements
The participants completed a standardized self-administered questionnaire that elicited data regarding sociodemographic, clinical, information technology experiences, and perceptions toward the EMR system, together with perceived level of confidence in using the system.
Perceptions about EMR usage by nurses were assessed using a standardized 17-question instrument, with a five-point Likert response rating. Specifically, the participants were given five response options for each item: “strongly disagree,” “disagree,” “do not know,” “agree” and “strongly agree.” 31 The perceptions covered several aspects pertinent to the EMR system: system development, nature of support provided for nurses; characteristics and quality of the system, adaptation of the system to nursing work routines, quality of electronic documentation, as well as the impact of system use both on nurses and the hospital. The instrument developed by Oroviogoicoechea et al. 31 had well-established face- and- construct validities. It had also high internal consistency, with a Cronbach’s alpha of 0.93. In this study, the Cronbach’s alpha was 0.91.
The perceived level of confidence in using the system was assessed using a single question “How confident are you in using the EMR system?” with a Likert scale ranging from “0” (not at all confident) to “10” (extremely confident).”
Ethical considerations
The study protocol was approved by the research and ethics committee at a governmental school of nursing, and the institutional review board for research at the research site.
Data management and analysis
Data files were built and analyzed using the IBM SPSS program. Frequencies and percentages were populated for categorical variables. Means, standard deviations, minimums, maximums and medians were calculated for each continuous variable. When needed, the continuous variables were dichotomized at the median score to create “high” and “little and low” groups.32–34 Multivariate logistic regression with Wald forward selection was carried out to identify independent predictors associated with the dependent variable, i.e. the level of confidence in using the EMR system (with high vs. little and low confidence status). Logistic regression analyses with odds ratios (ORs), with 95% confidence intervals (CIs), were calculated. All the two-tailed statistical analyses were conducted with a
Results
Sociodemographic characteristics
The participants’ mean experience in nursing was 15.95 years (± 8.72), and the mean number of years in EMR usage was 5.93 (± 2.40). Other sociodemographic characteristics of the study population are given in Table 1.
Sociodemographic characteristics of study participants.

Information technology experiences
A vast majority of the study participants (92.3%) reported owning a personal computer or a laptop (Table 2). Slightly more than half of them (54%) indicated daily internet use outside the hospital, with only 1.8% of the individuals indicating the complete absence of internet use outside the hospital. About three-quarters of the participants (75.1%) indicated no prior experience with EMR systems. When asked if they had been contacted to provide suggestions for customization or configuration of specific parts of the current EMR system, about one-fifth of the participants (20.7%) answered “yes” (Table 2). About twice as many nurses indicated having undergone computer training compared to those without (Figure 1).
Information technology experience of study participants.

EMR: electronic medical record.
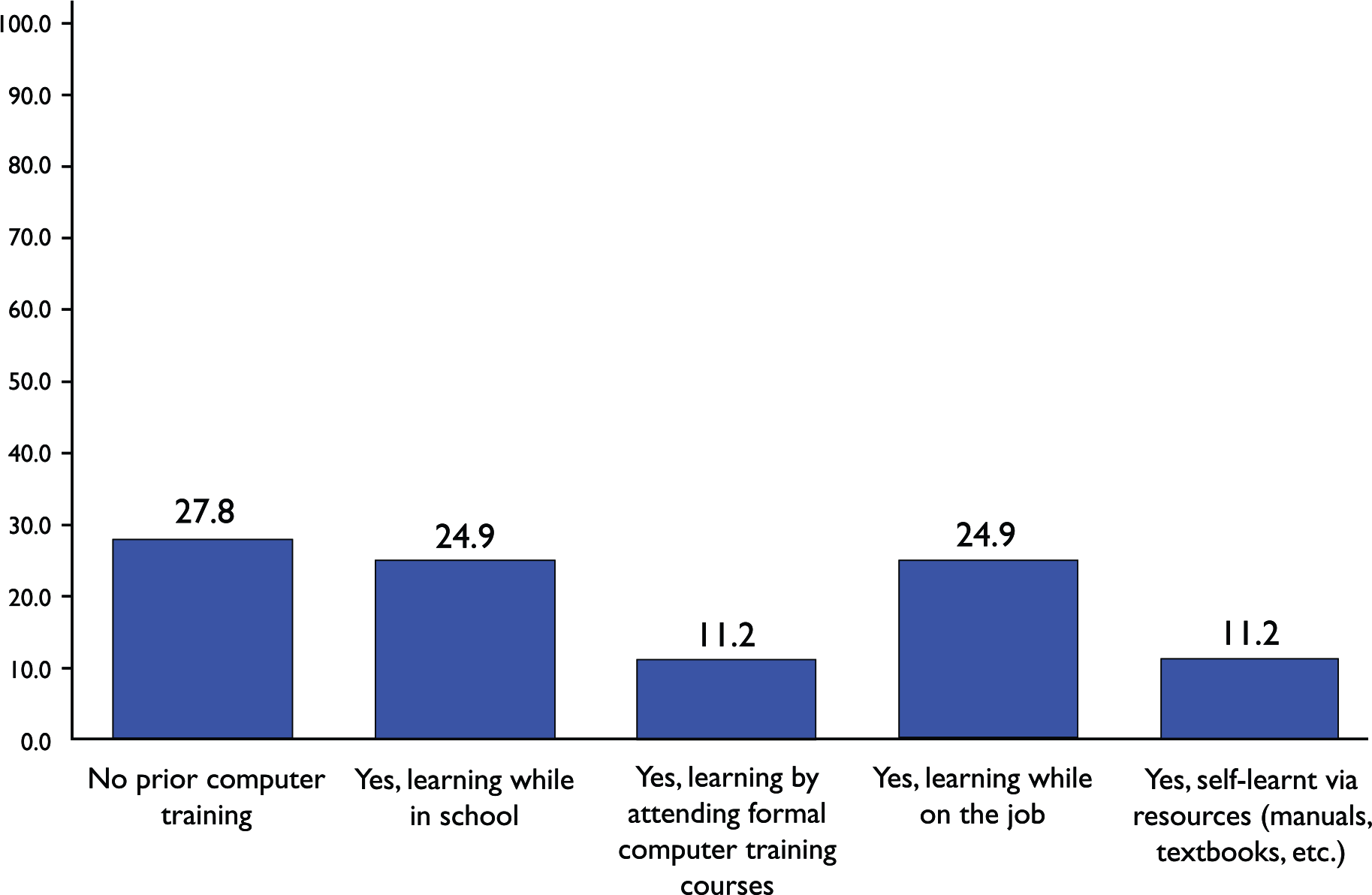
Modes through which participants underwent computer training.
Perceptions toward the use of the EMR system
Two positive perceptions of EMR indicated by the highest proportion of participants (97.0%) were the notions that the data entered into the EMR were important for patient care and that EMR is integrated into their daily work (Table 3). Conversely, the lowest proportion of individuals perceived that their suggestions for improvement were taken into account (60.4%) and that the EMR developers understood their problems (71.0%). The mean Likert score for reported confidence in using the EMR system was 8.49±1.22 (range 4.0–10.0; median = 9.0). Approximately half of the participants indicated confidence in using the EMR system (Figure 2).
Study participants’ perceptions toward use of an EMR system.
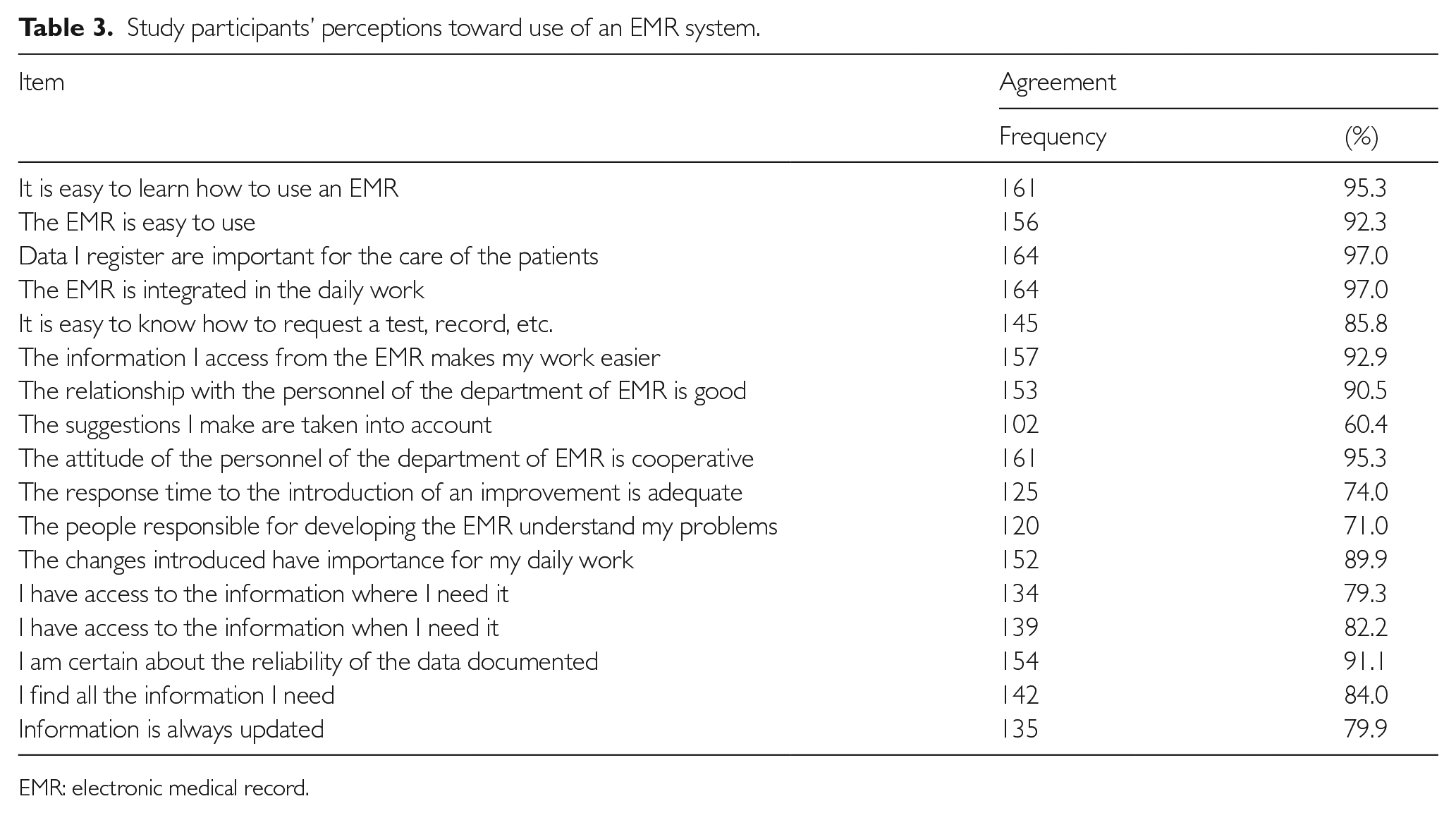
EMR: electronic medical record.
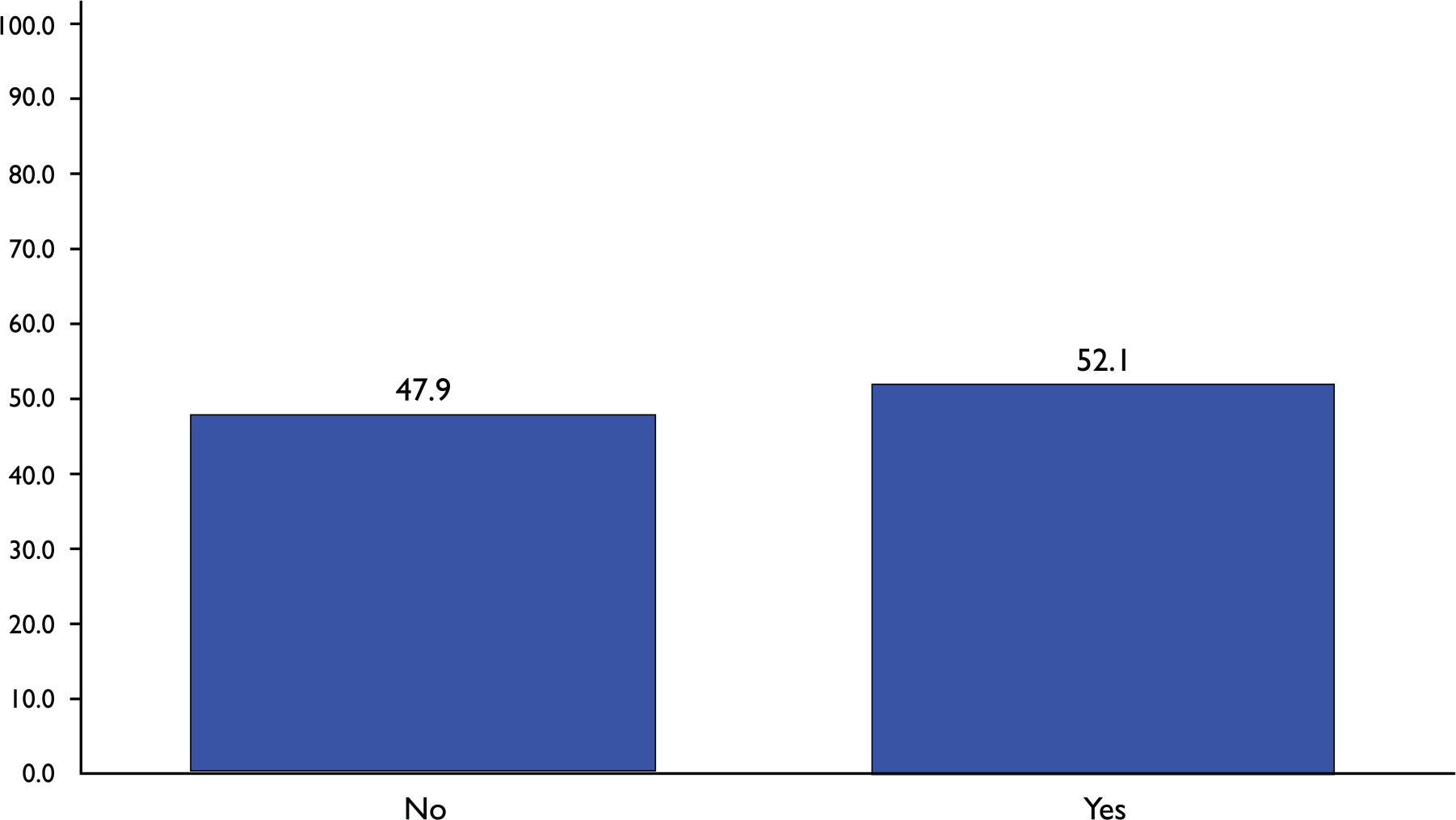
Self-assessment of confidence in using electronic medical records as indicated by study participants.
Predictors of confidence in using the EMR system
The logistic regression model was statistically significantly able to estimate the confidence of nurses in using the EMR system with high sensitivity (73.4%,
Multivariate logistic regression of variables and confidence in using an EMR as a dependent variable a .
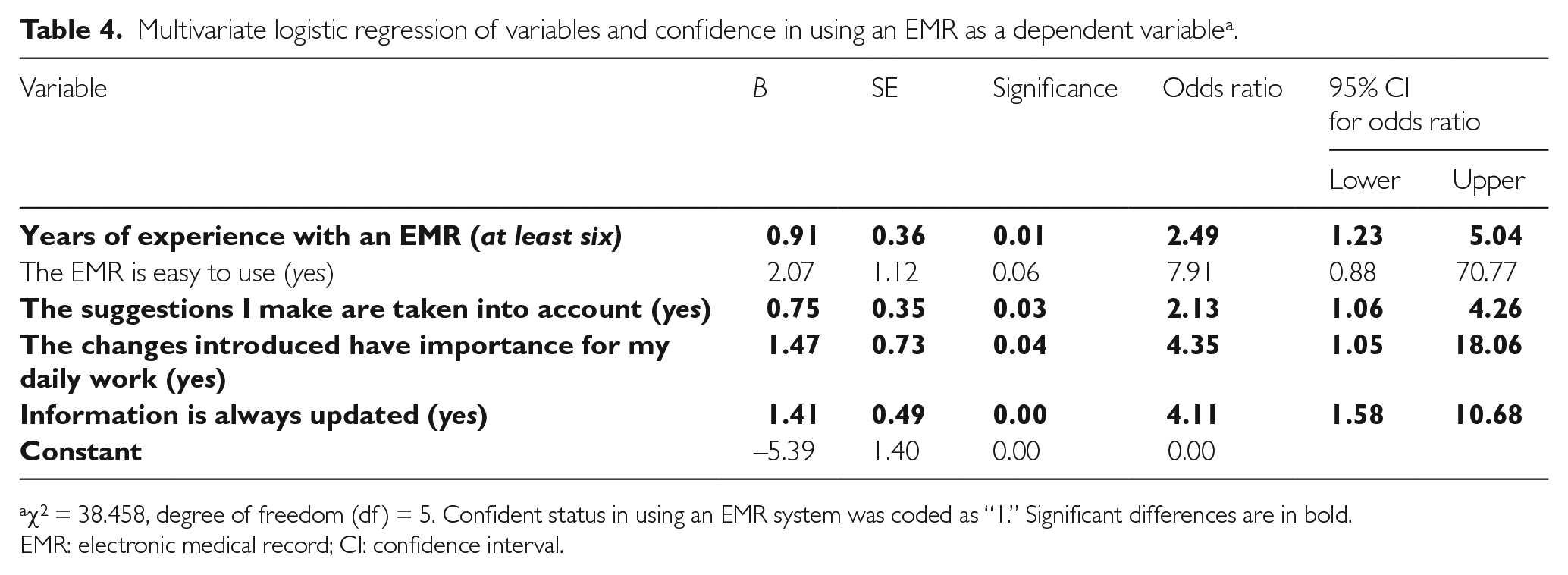
EMR: electronic medical record; CI: confidence interval.
Discussion
In this study, it was observed that three-quarters of the participants lacked prior experience with an EMR system, and that approximately one-quarter of them received computer training while on the job, highlights the point that limited training on how to use the EMR system could be considered a barrier that prevents nurses from effectively using the system. Inadequate education and training on using the EMR system have also been reported in other studies,15,16 with nurses also indicating that the difficulty of receiving technological support was a significant barrier to use of the EMR system. 15
It should also be noted that approximately one-quarter of the study participants had no computer training. This may affect their abilities to competently use the EMR system, and influence the quality of their interaction with the system while providing nursing care. Nurses should be able to demonstrate the following when dealing with information systems: basic familiarity with the use of computers, basic competence with computer software applications for creating and sharing professional documents, and electronic communication tools.9,35–38 In this regard, further studies exploring the effects of limited computer literacy among nurses on quality nursing care provision are needed.
It was noted that almost all the study participants perceived the importance of the data entered into the system in providing optimal care for the patients. A large majority (97%) also considered EMR systems to be integrated in their daily work routine. Ideally, EMR systems should support nurses’ activities and routines, and decrease interruption to the normal workflow of nurses. These results are consistent with those of Yontz et al., 27 who found that perioperative nurses considered the EMR system to be beneficial, improved nursing documentation, did not add to the nursing workload or eliminate any nursing jobs. The acceptance of the EMR system is influenced by several factors, such as the perceived usefulness of the system by nurses, along with nurses’ perceptions of the system’s ease of use. 19
The study nurses were least positive about aspects of their feedback on improvements to the EMR system, namely the suggestions that they had made had been considered, the EMR developers understanding their problems, and an acceptable response time in rolling out improvements in the system (Table 3). The results also indicate that nurses were likely to display confidence in using the system when they perceived that suggestions they made were taken into account. It is important to consider the opinions of nursing staff on the EMR systems as they are the end-users of the system.10,13,23,39 The nurses should be encouraged to speak up and acknowledge workflow changes that do not support work efficiency or could threaten patient safety. 23 Involvement of nurses in EMR system modeling was found to be influential to EMR usage. 14 The ability of nurses to customize the system would add to the desirability of system usage. Further, the team responsible for the operation of the EMR can help nurses by improving the system via customization, which would aid in raising quality of care provided to the public.
One predictor for high confidence in EMR use is at least six years of experience in using the system. It is perplexing that it needs six years to feel confident about using the EMR system. A qualitative study of nurses with fewer years of system usage can likely provide insight to this problem. Lack of organizational training and support to nurses while using the system could lead to disruptive workflow. 15 Training and ongoing support can be revisited for newly employed nursing staff. The training should be provided regardless of previous exposure to EMR systems.
Another predictor for nurses’ high confidence was perception of how updated the patient information in the EMR system was. If nurses perceive the data stored in the EMR system as updated, they had more confidence in using the system. Having access to up-to-date patient records is important, as it affects the reliability of hospital care. Previous studies13,14 have highlighted the impact of organization of data for practicing nurses. If an EMR system has updated and necessary clinical data, it will be helpful to improve the quality of patient care, 40 and similarly improve patient safety.11,41
Conclusions and implications
This study provides unique knowledge about Omani nurses’ perceptions toward the use of the EMR system, and the confidence level they possess while using such systems. While about three-quarters of the study participants did not have prior experience with an EMR system, approximately half of the individuals considered themselves as confident in using the system while rendering nursing care services to patients.
In general, while the findings show that nurses perceive the EMR system positively, areas for improvement are still being indicated. The data in the EMR system are also seen as important in supporting nurses in providing care to patients and regarded as integrated with routine clinical nursing work. The informatics team that manages the system is thus invited to consider nursing suggestions and feedback when making customizations and changes to the system.
Several factors have been found to increase the likelihood of developing high confidence in using the EMR system. Nurses are highly confident end users of the EMR system when: (1) they have at least six years of experience in using the EMR system, (2) they perceive that their suggestions about system improvements are taken into consideration by the informatics team that manages the system, (3) they perceive that changes introduced into the system are important to their nursing practice, and (4) they perceive that the information retrieved through the system had been updated.
Systematic training of nursing staff about the features and capabilities of the EMR system is highly encouraged. Training opportunities, especially for the users who have not attended computer and information technology courses, may enable nurses to more effectively and efficiently use the EMR system.
There is a need for continual engagement with nurses during EMR implementation. 23 EMR managing teams and policy-makers are invited to involve nurses during system evaluation and remodeling endeavors. Collecting feedback from nurses regarding the system will not only make the workflow easier for nurses, but also would support the varied efforts of providing quality care for patients.
In our present-day scenario where the health care industry is strongly supported by modern technology, further research is needed to understand the potential effects of limited computer literacy on quality nursing care. This research can also help us better understand the feelings and experiences of nurses with little experience of the EMR system, who were found to have low confidence in using the system. Nursing school officials are advised to include general computer and information technology contents in nursing curricula. Further, a dedicated nursing informatics course is recommended.9,35–38
Limitations
This study suffers from a number of limitations. Causal relationships between study variables cannot be inferred because of the cross-sectional nature of the study. Further, this study relies on self-reporting. Thus, the external validity of the study findings might be subject to social desirability and recall bias. This could have been ameliorated by the use of an anonymized random sampling method, used to recruit study participants.
Footnotes
Declaration of Conflicting Interests
The author declares that there is no conflict of interest.
Funding
This work was funded through the Dean’s Fund, College of Nursing at Sultan Qaboos University, Oman.
