Abstract
Background:
Different health care systems impact on medical education.
Objective:
We aim to describe the differences and similarities in the perceptions of pediatric residents on education in professionalism and communication skills across two countries.
Methods:
We conducted a cross-sectional survey of pediatric residents in the United States and Singapore. A 108-item written questionnaire on perceptions regarding education in communication/professionalism was administered. A five-point Likert scale was used for each attribute in the survey. Quantitative analysis was performed using chi-square test.
Results:
Response rate was 65.9% (89/135). In the domain of professionalism, residents from both countries ranked shared decision making as the most important attribute (Singapore vs. USA: 26/50 (52.0%) vs. 19/39 (48.7%),
Conclusions:
This investigation demonstrates more differences in the perception of how communication is taught compared to professionalism across two countries. Barriers and promoters to teaching were similar across these two countries, with role modeling being an important approach to teaching communication and professionalism across both countries.
Keywords
Introduction
Effective communication and professionalism are essential qualities of all physicians. In recognition of the importance of these areas as cornerstones of medical practice, communication and professionalism have been incorporated as key domains of competence for residency education by the Accreditation Council for Graduate Medical Education (ACGME) in the United States, and also internationally through the development of the ACGME – International (ACGME-I).1,2 In addition, the Royal College of Paediatrics and Child Health in the United Kingdom place similar importance on the evaluation of the competency of residents and trainees in the areas of communication and professionalism in their post-graduate professional examinations. 3
Previous studies have examined the perceptions of residents on the training provided for communication and professionalism in their respective specialties, as well as perceptions of their own professionalism.4–7 These investigations have all been conducted within a single medical system, geographical region, or country. These prior studies do not address differences and the variable structure of medical and educational systems (such as duty hour restrictions and other factors) that are likely to impact the teaching of communication and professionalism within different specialties.8,9 Furthermore, facilitating factors, and preferred teaching methods are likely to be different across countries.
To investigate the potential differences in the perceptions of pediatric residents’ in the teaching of communication and professionalism across different cultures, we conducted a cross-sectional survey of pediatric residents in United States and Singapore. Singapore adopted the ACGME-I accreditation system in 2010, and residents are assessed in a manner similar to the structure in the United States across the six domains of competence outlined by ACGME based on ACGME-I requirements. However, the educational systems, and health care systems are different in these two countries. We hypothesized that there would be differences in the perceptions of pediatric residents on preferred methods, barriers and facilitators in learning professionalism and communication across countries.
Methods
Study design and participants
Duke Children’s Hospital is a tertiary referral hospital located in Durham, North Carolina, United States, and KK Women’s and Children’s Hospital (KKH) is large tertiary hospital in Singapore. Prior to 2010, pediatric training in Singapore modeled closely after the United Kingdom; however, since 2010, Singapore has embarked on the pediatric residency program structure as accredited by the ACGME-I. This study was approved by the Institutional Review Boards at both institutions.
We designed our survey utilizing components from previously published assessment tools.4,7,8 A conceptual framework for this survey focused on attention and motivation as outlined in Bandura’s social learning. 10 The objectives of the adapted survey were to investigate the importance of the various attributes of communication and professionalism, preferred teaching methods and perceived barriers and promoters for teaching these domains of competencies. Because each individual previous assessment tool did not allow us to achieve our aims, we have to incorporate various survey elements from each. We adapted the statements so that it will be applicable to pediatric residents. In addition, we added teaching methods that were specifically available in both institutions. During the design stage, we piloted the survey with 8 fellows and registrars at Duke Children’s Hospital and KKH for feedback and refinement of the questions. Our final cross-sectional survey consisted of 108-item written questionnaire.
After development, the survey was distributed using REDCap (Research Electronic Data Capture) to all trainees in the pediatric programs at these two hospitals, and data were collected in the REDCap Database. 11 We included residents from the combined medicine-pediatric residency program in the United States. There is currently no such combined residency program in Singapore. In total, 135 surveys were sent electronically, 73 to Duke and 62 to KKH.
Data collection methods
We collected pertinent demographics of the respondents which included age, gender, location of medical school, year of graduation, and year of residency. For each specific communication skill and professionalism attribute, we asked residents to rate the importance of that particular attribute using a five-point Likert scale (1 = not at all important, 5 = extremely important). In addition, respondents were asked to choose the three most important attributes in the domains of professionalism (13 attributes) and communication (16 attributes). Residents were also asked about his/her perception of the best methods in teaching these two areas. This characterization of the best teaching method was specified to include all options, regardless of whether this method was used in their current program. Barriers and promoters in facilitating the learning of these two domains were also identified. The respondents were also asked to list the three most important teaching methods, barriers, and promoters.
Data analysis
We analyzed our data using Stata 12.1. To measure the internal consistency of the attributes within the professionalism and communication domain in the final data, we calculated the Cronbach’s alpha coefficient. We summarized responses in the Likert scale questions in medians and interquartile ranges. Categorical variables were summarized with counts and percentages. In comparing data between the two geographical regions, we utilized the chi-square test for categorical variables. Statistical significance was taken as
Results
The total number of responses was 89 (65.9%) with response rates of 53.4% and 80.6% from Duke and KKH, respectively. The median age of respondents was 29 (interquartile range: 28, 30) years; 18/89 (20.2%) of respondents were male. Majority of respondents (55/89 (62.8%)) graduated after the year 2010. Internal consistency of the attributes within the domain of professionalism (
The majority of our respondents ranked all the attributes of professionalism and communication as moderately to very important (Table 1). No attributes were considered to be redundant or unimportant. Residents from both countries ranked shared decision making, competency, and compassion/empathy as the three most important attributes of professionalism. In the domain of communication, however, there were differences in the perceptions of the three most important attributes between the two countries. Compared with only eight (20.5%) residents from the United States, residents from Singapore considered dealing with the difficult families and patients (30 (60%)) as one of the most important attributes of communication.
Ranking of professionalism and communication attributes (
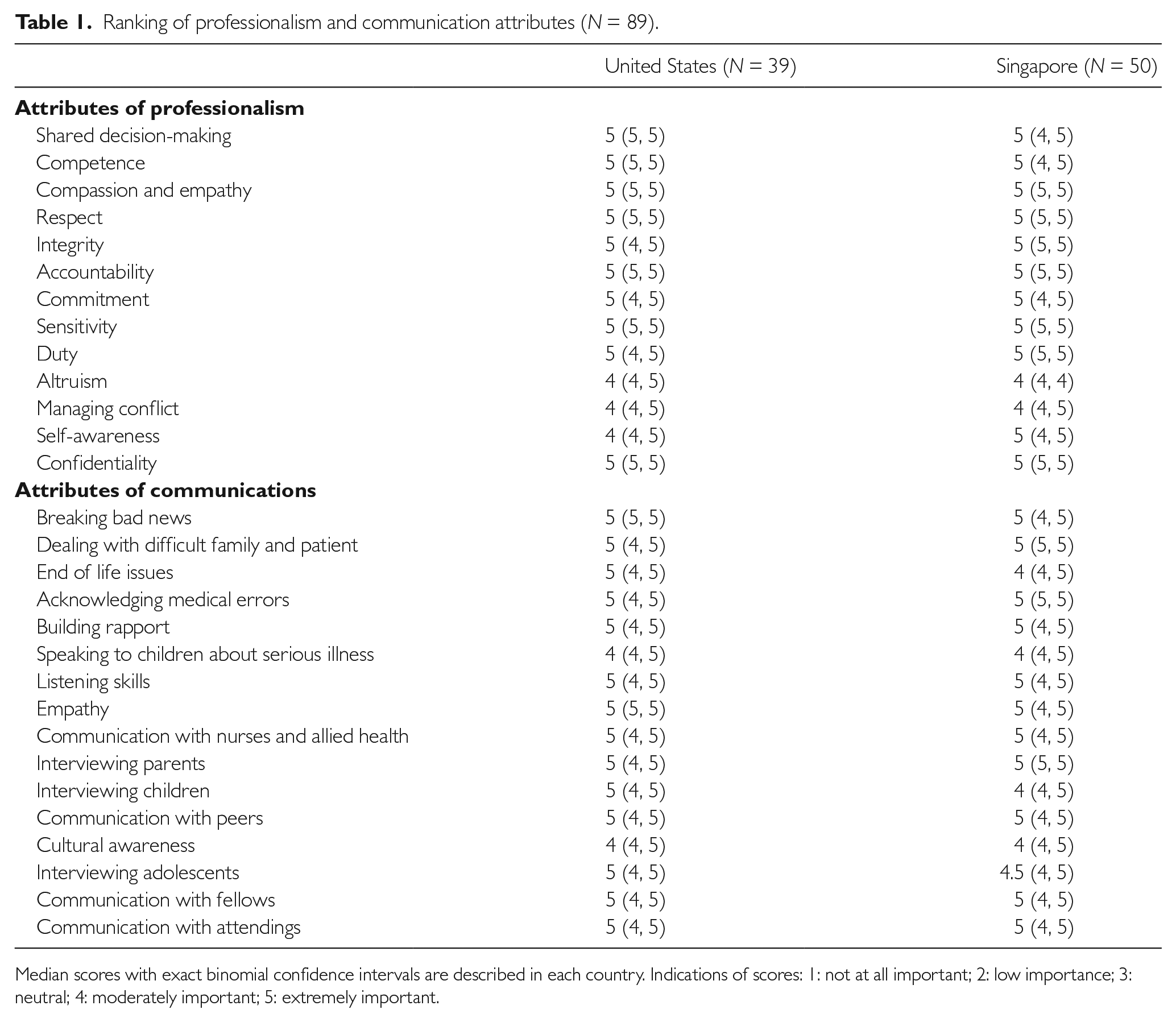
Median scores with exact binomial confidence intervals are described in each country. Indications of scores: 1: not at all important; 2: low importance; 3: neutral; 4: moderately important; 5: extremely important.
Role modeling by attendings, direct observation and feedback, and role modeling by fellows or registrars were the three methods perceived to be most effective in teaching professionalism in both countries (Table 2). In addition, among residents in Singapore, high fidelity simulation was tied as third most effective technique with role modeling by fellows or registrars. For communication, the two methods for teaching communication perceived as most effective in both countries were direct observation with feedback and role modeling by attendings (Table 2). When asked to select the three most important tools for teaching communication, there was a significant difference in the perception of standardized patients as a teaching tool between the two centers (United States vs. Singapore: 7.7% vs. 40%,
Ranking of methods for teaching professionalism and communication as perceived by residents (

Median scores with exact binomial confidence intervals are described in each country. Indications of scores: 1: not at all important; 2: low importance; 3: neutral; 4: moderately important; 5: extremely important.
Residents from both countries perceived the top three barriers to teaching of professionalism and communication similarly (Table 3). The top three barriers were high workload, time constraints, and fatigue. Residents from Singapore, however, cited culture within the department as a significant barrier to the teaching of professionalism and communication as compared to residents from the United States (30.0% vs. 0.0%,
Number of respondents listing the barriers and promoters as one of the three most important in teaching professionalism and communication.

Note: In the setting of multiple testing, a
Discussion
Our study demonstrates similarities in the perception of professionalism and communication across countries. Similarly, the teaching methods that were perceived as most effective were similar in the domain of professionalism but differed for communication. Residents from both countries cited common barriers in learning these two competencies, but the choice of most important promoters of teaching of these competencies were in a different order between the two countries.
It is interesting that residents from different cultural backgrounds and medical systems placed similar emphasis on professionalism attributes as compared to communication. Professionalism is defined as commitment to carrying out responsibilities, adherence to ethical principles, and sensitivity to a diverse patient population, 12 and these data suggest that this definition appears to be viewed consistently across cultural and geographic boundaries. The similarity in assessment of the attributes of professionalism has also been demonstrated in a previous investigation within a single country involving residents from five different specialties that utilized a focus-group methodology. 13 Similar to our findings, the study demonstrated that professionalism is most crucial as it relates to the doctor–patient relationship. Across different medical systems and countries, physicians are generally held to the same code of conduct and, based on our data, these expectations appear to cross cultural lines. Thus, it is not surprising that residents from both countries ranked the top three attributes of professionalism in a similar manner, since the definition of a good physician appears to hold true regardless of location or background. In addition to similar cultural framework, these similarities may also be explained by the need to achieve ACGME milestones and adhere to specific guidelines in both centers.
We found that there was a difference in the perception of the use of standardized patients in communication training in both institutions. One possible explanation for this difference is the methods used in teaching this competency in both institutions. In KKH, residents are required to attend a communication course (held quarterly) that utilizes standardized patients to teach effective communication principles. Standardized patients are not used in this manner to teach communication at Duke Children’s Hospital. In both countries, role modeling was perceived as the most important and effective method to teach both competencies. This method is often “taught” by a faculty without the faculty knowing or having an explicit intent to teach. 14 The importance of role modeling in this manner to teach professionalism is not unique to pediatrics. This approach has been previously demonstrated in other specialties including both surgery and intensive care.15,16 Furthermore, a systematic review that included 43 studies in medical education reported that role modeling and personal reflections that are guided by faculty members were widely considered to be the most effective methods for teaching professionalism. 17 When combining our data with the findings from prior studies, an important element of faculty development for both senior and junior staff should be an understanding of the impact of their behavior and importance of role modeling on trainees. The behavior of senior members in front of junior staff likely has a tremendous impact on residents’ learning of both professionalism and communication. Thus, senior staff and faculty members need to model desirable behaviors, especially given that in the academic environment, they are almost always being watched by learners, even when they are not explicitly teaching.
However, residents should be cognizant that they should not imitate their seniors or peers without being critical. Blindly following a role model may not fully maximize the educational value of role modeling. 18 Indeed, by leveraging on positive role models that are available, residency programs should consider equipping their junior staff with skills that enable them to critically appraise the pros and cons of the observed behavior. For example, instead of telling the residents that there is a right and wrong way of breaking bad news, residents should be encouraged to discuss different communication techniques that they have observed, critically appraise the various approaches and feel empowered to choose for themselves the styles and approaches that they like best.
Across both countries, the barriers to learning these competencies were strikingly similar. High workload and time constraints potentially limit the time available for residents to self-reflect on professionalism issues that may arise during daily work or patient encounters. Furthermore, these barriers potentially limit the time that is required to have a meaningful communication session with a patient and their family. Innovative ways to manage these two barriers are required to ensure that residents have sufficient clinical exposure, while they are also simultaneously able to reflect and seek feedback on their communication skills and professional behaviors in these encounters. Duty hour regulations, which are currently imposed in both countries, can be a double-edged sword with regard to this issue. In a previous survey of 169 residents (internal and family medicine) from three centers, respondents felt that while duty hour restrictions addressed the issue of fatigue, they limited the continuity of care and accountability to both patients and colleagues. 8 While duty hours will likely remain limited for the foreseeable future, it is imperative that training programs allow time for residents to both self-reflect on these important competencies, while they work to balance continuity of patient care and clinical exposure.
Further investigation of the barriers to learning professionalism and communication reveals an important noticeable difference in what is perceived as a barrier in one country that is not present in the other. Culture within the department was cited as fourth most common barrier in Singapore, with none of the residents from the United States citing this barrier (15/50 vs. 0/39,
While there are a number of strengths, this investigation is not without limitations. Limitations of our study included only involving respondents from one center in each country. There may be variability across institutions within both of these countries. Furthermore, we only involved residents from one specialty. Our sample from a single specialty from two centers may limit the generalizability of our findings to some degree, but these data provide an interesting first step in addressing important issues. Our survey did not include any free text or qualitative data that could potentially be used to illuminate further discussion. Although we presented the Cronbach’s alpha value for the attributes in the two domains in our study, this value should be interpreted in the context of the limited number of respondent that we had in our study. To our knowledge, this is the first study to examine the differences between two centers in two distinct countries, geographical regions, and cultural systems that have adopted a similar residency training program structure. Instead of focusing on a single area, our study examined two important domains of competence that are considered vital by the ACGME and ACGME-I that should easily cross both cultural and geographic boundaries.
Conclusion
Our study demonstrated that there are slightly more differences in the perception of the importance of the various attributes of the domain of communication than professionalism. We found that similar barriers exist within two distinct cultures in learning these competencies. Our study demonstrated common findings, both in terms of the importance of role modeling and direct observation in both cultures and the identification of fatigue, workload, and time constraints as barriers, further emphasizing the importance of these aspects of medical education. This investigation also highlights important differences that exist between cultures with similarly structured residency training systems. As programs expand and become more global, a stratified approach to education with attention to cultural differences should be considered in the training of these important foundations of pediatrics and the practice of medicine.
Footnotes
Acknowledgements
The authors acknowledge all the pediatric residents at Duke Children’s Hospital and KK Women’s and Children’s Hospital who took time to complete this survey.
Declaration of Conflicting Interests
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
