Abstract
Unintended arterial cannulation and injection of drugs may result in ischaemia and tissue necrosis. Various methods used to differentiate accidental arterial from intravenous cannulation have their own shortcomings. Here we present the case of a 13-year-old girl having an elective procedure under general anaesthesia and the challenges faced in distinguishing suspected intra-arterial cannulation from what was indeed an intravenous cannulation. We recommend the use of an open-ended saline-filled ‘T’ connector–syringe system and pressure transduction as the methods of choice to identify and confirm, respectively, a suspected arterial cannulation during anaesthesia.
Background
Unintended arterial cannulation during anaesthesia and injection of certain drugs can result in local ischaemia and tissue necrosis. Various methods used to differentiate accidental arterial from intravenous (IV) cannulation have their own shortcomings. A novice anaesthetist, in particular, might not only be unaware of serious consequences of an inadvertent arterial cannulation but also the methods to detect and confirm the same. Here we present the case of a 13-year-old girl presenting for an elective procedure and the challenges faced in distinguishing suspected intra-arterial cannulation from what was indeed IV cannulation. We discuss and recommend easy and reliable methods for early detection and differentiation between arterial and venous cannulation in an anaesthetised patient.
Case presentation
A healthy 13-year-old girl presented for bilateral inferior turbinate sub-mucous diathermy. Standard monitoring was established, with the blood pressure (BP) cuff on the left arm. A 22G IV cannula was inserted into a vessel on the dorsum of the right hand between the third and fourth metacarpals. Patient was pre-oxygenated and induced with propofol, fentanyl and atracurium and intubated. Anaesthesia was maintained on pressure controlled ventilation and sevoflurane/air/oxygen mixture. Hartmann’s infusion was commenced using a standard IV tubing connection attached to the patient via a three-way tap and a 100 cm IV extension line, without any infusion pumps.
Within a couple of minutes, a significant backflow was noticed on the IV tubing. A brisk backflow of bright blood was noted when the cannula was opened to air. Suspecting arterial cannulation, another IV cannula was inserted on the dorsum of the left hand, with the BP cuff repositioning on the left leg. Blood sample taken from the first cannula analysed using I-STAT (Abbot, Transmedic) showed a
In recovery, blood gas analysis using the I-STAT on the samples from the right hand dorsum and right ankle cannulae with the patient breathing room air, showed
Discussion
It is not only vital to differentiate unintended arterial cannulation from venous cannulation early during anaesthesia but also important to know how to make this distinction. Unintended arterial cannulation has been reported many times during anaesthesia.1–3 Clinical clues and methods used to identify and confirm unintended arterial cannulation during anaesthesia are presence of backflow of pulsatile bright-red blood, pain on injection and/or blanching distal to site of injection, blood gas analysis and pressure transduction. However, most of these methods have their own shortcomings.
On one hand, brisk backflow of bright-red blood will not be seen when a deliberate attempt is made to prevent backflow to assist capping of the cannula. On the other hand, a patient who is anaesthetised, paralysed and ventilated on high FiO2 might have a backflow of brisk bright blood even from an IV cannula, though not pulsatile. Hence the first point to note is that ‘pulsatile’ backflow is to be looked for to identify arterial cannulation ‘early’ during anaesthesia in most suspected cases, except in a small group of patients such as severely hypotensive patients or paediatric patients with cyanotic heart disease. Technically, it can be difficult to identify pulsations with the naked eye when a cannula is left open to air has a brisk backflow. A simple effective solution is to connect a saline filled ‘T’ connector to the cannula connected to a 2 ml syringe barrel at the other end held vertically (Figure 1). The blood flows from the artery into the cannula, then into the ‘T’ connector and forms a pulsatile meniscus at the 2 ml syringe barrel unlike in venous cannulation (Figure 2). This helps us detect the ‘pulsatile backflow’ without spillage and identify an arterial cannulation, early. In adults where larger bore 15 cm extension tubing with a three-way tap is routinely connected to IV cannulae, it can be used as a manometer by holding it vertically exposed to atmospheric pressure. A syringe barrel is used to prevent spillage and provide a wider meniscus to aid observation. In case of adults with large bore cannulae, a larger syringe barrel or a longer extension such as 30 cm tubing connected to a three-way tap could also be used to detect the pulsatile meniscus and prevent spillage. A very small chance of negative venous pressure causing aspiration of air into the tubing should be borne in mind.
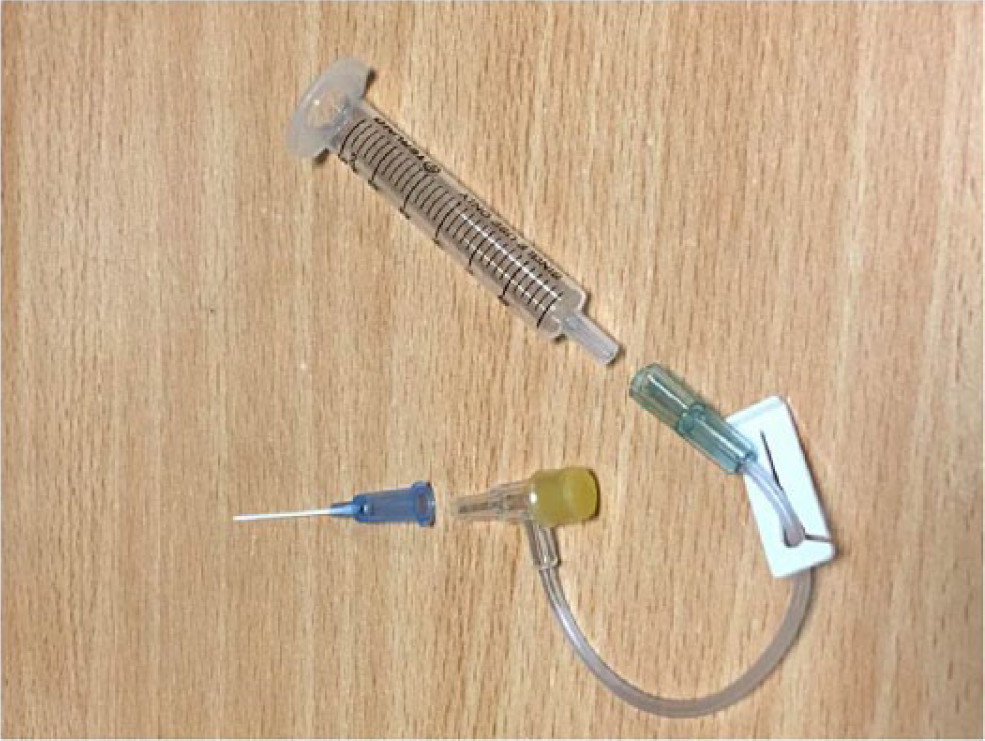
Components of the ‘T’ connector–syringe barrel system.

‘T’ connector–syringe barrel system connected to a cannula demonstrating meniscus formed by the backflow of blood.
Pain on injection may indicate intra-arterial injection fairly late in the process of identification, as the drugs would have been already administered. The most commonly used induction agent propofol, causes pain even on IV injection. Moreover, most children induced with inhalational techniques and patients who are already anaesthetised cannot report pain on injection of drugs. Hence, pain on injection cannot be used for early identification of unintended intra-arterial cannulation during anaesthesia.
In patients who are anaesthetised, paralysed, intubated and ventilated, blood gas analysis can be performed quickly. However, on comparing peripheral venous and arterial oxygen partial pressures, though PvO2 is less than PaO2, there is a high variability in the difference between the two values (PaO2 − PvO2 ), depending on the vasodilatation in the patient, due to inhalational anaesthetic agents and other factors during anaesthesia.4,5 Peripheral venous
It might be challenging to pick up pulsations of very small superficial vessels that vaso-constrict secondary to stimulation due to needle puncture; 6 hence ultrasound guidance is less effective in detecting inadvertent arterial cannulation of small vessels during anaesthesia.
Invasive BP monitoring is the gold standard to measure BP. As long as the transducer system is free of air bubbles and kinks, connected to appropriate extensions and the vessel is patent, a pulsatile arterial pressure wave often provides definitive confirmation of arterial cannulation, even in hypotensive, hypoxic patients and paediatric patients with cyanotic heart disease. Hence arterial pressure waveform is the most reliable method for differentiation of arterial and venous cannulation during anaesthesia.
In our case, we suspected arterial cannulations in both hands, though uncommon, due to backflow of blood into infusion lines followed by brisk backflow of bright-red blood on uncapping the cannulae. It was not recognised immediately after cannulation as the backflow was deliberately prevented using manual pressure on the vessel proximal to the tip of the cannula, to aid IV tubing connection. We did not look for pulsatility as the backflow was very brisk and bright red in colour, probably due to high FiO2. Our FiO2 was still on the way down from 100% at induction to the set value of 30%, with low flows of less than 1 litre per minute when we took our first sample for blood gas analysis. We also did not see any blanching on flushing them with 2 ml of saline. We initially chose to perform blood gas analysis instead of pressure transduction, to save time. We also used two different I-STAT blood gas analysers to ensure that the results were not spurious due to I-STAT defects. We used saphenous venous sample as baseline instead of taking an arterial sample. Since the blood gas results were not confirmatory, we pressure transduced the cannulae. There were no arterial pressure waveforms on transducing the cannulae and hence we concluded that the cannulae were all IV. Subsequent blood gas analysis of samples obtained from cannulae in the dorsum of the hands and ankle confirmed our inference.
Learning points
We conclude that during anaesthesia, it is vital to:
identify and confirm suspected intra-arterial cannulation ‘early’ prior to injecting drugs to avoid ischaemia and tissue necrosis;
use appropriate methods to distinguish arterial and venous cannulation.
We recommend the use of:
an open-ended saline-filled ‘T’ connector–syringe system for early identification of intra-arterial cannulation, in most patients;
pressure transduction as the modality of choice for confirming suspected unintended arterial cannulation during anaesthesia.
Footnotes
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
