Abstract
Brachioplasty is a common procedure performed by plastic surgeons, with type II brachioplasty being the most regularly performed procedure in the clinic. This study evaluates patient satisfaction after mini-incision brachioplasty using a five-question survey. We administered the survey to 26 patients six months after they had undergone mini-incision brachioplasty to correct type II deformity. Most of the patients considered the improvement by surgery acceptable (53.8%), while 84.6% reported a decrease of at least two clothing sizes post-surgery. More than half (57.7%) were satisfied with body symmetry following surgery, while 69.2% accepted the resultant scar. However, only 30.8% would recommend this type of operation without reservations. The results of this study indicate that adequate patient education prior to mini-incision brachioplasty is key to optimal patient satisfaction.
Introduction
Body contouring is a rapidly growing field in plastic surgery. In 2015, nearly 400,000 patients underwent body contouring procedures in the US alone, with an almost 5000% increase in the number of upper arm lifts performed in the last 15 years. 1 Multiple techniques for brachioplasty have been described singly, or combined with liposuction since 1954.2,3
Patient satisfaction can be used to assess the quality of care. Recent publications on patient satisfaction after cosmetic surgery have shown that the majority of patients are satisfied with the outcome of the operation. 4
The purpose of this study was to evaluate patient satisfaction after undergoing mini-incision brachioplasty combined with liposuction.
Methods
This study included 26 patients who underwent bilateral mini-incision brachioplasty. The operations were conducted from June 2012 to December 2014. On average, the follow-up period was 14 months (range 6–24 months).
Patient selection
Selected patients presented with moderate excess skin and fullness of the upper arms (Type II). Patients with comorbid conditions, fullness of upper arm only (Type I) or with fullness of upper arm combined with severe redundancy of skin (Type III) were excluded from the study.
Patients were shown the exact location of the axillary scar. The terms “hairline,” and “fades away” were never mentioned to the patients. Informed consent was obtained from all patients involved in the study. Consent for photography was obtained separately.
Surgical procedure
Preoperative marking was carried out with the arm in adduction (Figure 1). The anterior point was marked in the anterior axillary fold. The posterior point was marked in the posterior axillary fold.2,5 The arm was then elevated 90°, and the two points connected. The redundancy of the lower part of the arm was grasped towards the axilla. The point that made the best contouring was marked as the apex for the triangle of excision. The same was done for the other arm.
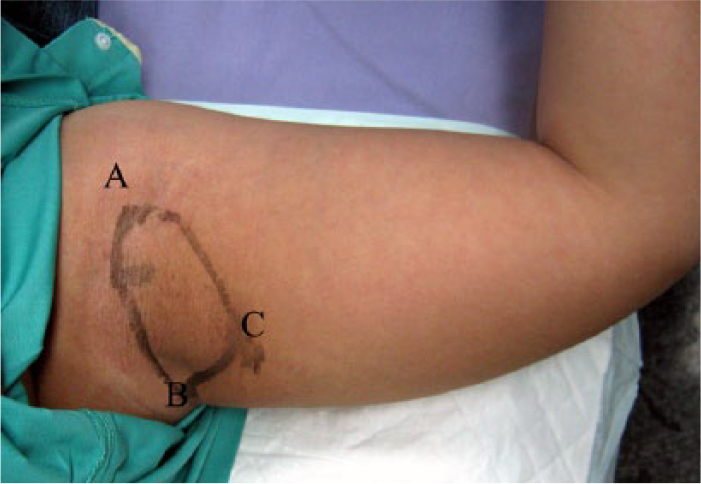
Surgical markings.
Under general anesthesia, the patient was laid supine, and her arms were placed behind her head to expose both axillae. Liposuction with the tumescent technique was first carried out. This involved an injection with lactated Ringer’s, mixed with adrenaline at a ratio of 1:250,000, followed by aspiration, which was completed when there was an adequate redundancy sufficient for wound closure with minimal tension. The central part of the triangle base was excised together with the apex, and the key suture to contour the arm made. Excisions above and below the suture were carried out. If the proposed incision was cut from the start, this could result in a dog ear that would extend beyond the marked anterior and posterior points, and the scar would be visible. An area of fat, including the lymphatic system, was retained in all cases. The wound was closed in two layers without a drain, and a garment was applied on the lower half of the circumference of each upper arm.
Postoperative care
The patients were instructed to change the plaster garment every week for four weeks. Antibiotics were given in the first five days, and the sutures were removed 10 days after the surgery.
Patient outcome study
Patients were interviewed six months after their surgery
The delay between the surgery date and the patient interview was to allow the initial postoperative enthusiasm to dissipate, and for the patients’ normal activities to resume before they were questioned. Multiple attempts were made to contact each patient by the last-known home address and telephone numbers. The interviews were conducted by nurses in the clinic to minimize bias. Following previous studies,6–8 patients were asked the following five questions (scores provided in brackets after responses):
Did you think the surgery has provided improvement over the long term?
No (0); Yes, but it was not worth the time or recovery effort (1); Yes, it was worth the time and recovery effort (2).
Has your clothing size changed after the surgery?
No (0); Yes, a decrease of 1–2 sizes (1); Yes, a decrease of 3–4 sizes (2).
Do you consider the results of the surgery to be symmetrical?
No, the results were not acceptable (0); No, but the results were acceptable (1); Yes (2).
How would you consider to the appearance of the surgery scar?
Very prominent and not acceptable (0); Prominent but acceptable (1); Not prominent (2).
Would you recommend this operation to others?
No (0); Yes, with some concern (1); Unconditionally, yes (2).
Results
The 26 respondents were female, with a mean age of 34.8 years (range 21–52). Nearly half of the patients indicated that they would recommend the operation to others with some concern. The highest patient satisfaction occurred with teachers and the lowest recorded with students. This was statistically significant (Table 1). Between housewives and teachers, and students and health professionals, the difference in drop in garment size was statistically significant. In a comparison of patients by occupation type, there was no significant difference in their perception of post-surgery satisfaction, particularly when it came to scar formation and recommending the operation to others.
Patient satisfaction scores grouped by occupation.

15 cells (100.0%) have expected count less than 5. The minimum expected count is 0.08.
The standardized statistic is 0.271.
However, patients who had obtained information regarding the procedure from friends before the operation were more likely to recommend the operation to others at a statistically significant level.
Although the relationship between the preoperative information source and satisfaction was not statistically significant, patients who had obtained information about the procedure from friends showed a higher percentage of satisfaction. Otherwise, there were no significant differences between preoperative information sources and postoperative changes in garment size, perceived postoperative symmetry and satisfaction with scar formation.
Clinical results
The pre- and postoperative results of some of our cases are shown in Figures 2 and 3. These figures show the postoperative reduction in arm circumference, the discreetly located scar with its symmetry and neat healing.

Patient with type II brachioplasty: (a) preoperative, anterior view; (b) preoperative, posterior view; (c) liposuction; (d) postoperative, anterior view; and (e) postoperative, posterior view.

Patient showing type II brachioplasty: (a) preoperative, anterior view; (b) preoperative, posterior view; (c) anterior scar on right arm; (d) anterior scar on left arm; (e) postoperative, anterior view; and (f) postoperative, posterior view.
Surgical complications
None of the patients required blood transfusions or hospitalization for the management of surgical complications. There were also neither seroma nor wound disruptions, except for one case where the wound closed in a T-shape due to bad design.
Discussion
Before this study, there were no surveys specifically addressing patient satisfaction post-brachioplasty. This questionnaire was crafted using questions drawn from published articles in the field of body contouring surgery, as well as patient remarks.6–9 The survey participants all agreed that the survey questions were clear and unambiguous.
Patient satisfaction was highest among teachers and housewives, and lowest among physicians, health professionals and students. These results are influenced by social factors that were not investigated in this study (e.g. lifestyle and individual personalities of the patients). In general, the patients were satisfied with the surgical outcomes. A minority of patients who were completely dissatisfied with the outcome had expectations set too high, and were overly obsessed with the desired outcome. The patients obtained information about the procedure preoperatively from the following three sources, with nearly equal frequency: the Internet, the media and friends. Those who obtained information from friends took less time in preoperative consultation and showed the highest satisfaction scores.
This study was limited by the small number of patients surveyed. It is also likely that the interval between the operation and the administration of the survey could have influenced the outcome, given that the contour of the arm changes with subsequent weight gain/loss. 10
While the results obtained in this study are preliminary in nature, they suggest that to ensure optimal patient satisfaction, physicians should furnish patients with the operative details in full, and conduct an in-depth discussion of scar appearance. In this discussion, it would be helpful to show patients pre- and post-operation augmentation photographs of past patients.
Footnotes
Declaration of conflicting interests
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
