Abstract
Introduction:
Although cervical cancer is the 10th most common cancer among females in Singapore, it is a vaccine-preventable cancer. Human papillomavirus vaccines combined with regular Pap (papillomavirus) smears have been shown to reduce the mortality and morbidity associated with cervical cancer. We assessed the knowledge and attitudes towards cervical cancer, human papillomavirus and its vaccination amongst pre-university female students and assessed if a short educational presentation can improve this knowledge and acceptability of the vaccine.
Methods:
A cohort survey was carried out amongst 150 female students at Hwa Chong Junior College via questionnaires administered anonymously. Standardized educational presentations were carried out followed by post intervention questionnaires.
Results:
Almost all the students were aged between 15 and 19 years old (99.3%). At baseline, only 29% and 27% of the students had ever heard of human papillomavirus and its vaccines respectively. The most common source of information cited was from a family member or a friend (22.5%). Only 4% had been administered the human papillomavirus vaccine. Mean knowledge scores significantly improved from 4.95 to 8.61 out of 10 after the intervention. Of those who did not have the vaccine, only 31.3% were willing to consider the human papillomavirus vaccine pre-intervention, with a statistically significant improvement to 51.4% post intervention.
Conclusion:
Low awareness about human papillomavirus, its relationship to cervical cancer and its prevention is common, even amongst well-educated students. Most of them obtained the information from family and/or friends. A short educational presentation was able to improve the knowledge scores, and improve the acceptability of the human papillomavirus vaccine.
Introduction
Cervical cancer is the fourth most common cancer in females globally. 1 Nevertheless, it is one of the few cancers which is preventable by vaccination. It is known that persistent human papillomavirus (HPV) infection causes the eventual development of cervical cancer. 2 In particular, HPV subtypes 16 and 18 are responsible for about 70% of cases. A prophylactic vaccine against these HPV subtypes would be an effective preventive measure to reduce the burden of cervical cancer. 3 Since 2009, the World Health Organization has recommended that the HPV vaccine be included in national immunization programs. 4 HPV vaccination has been incorporated nationally into school vaccination programs in countries such as Australia, United States, United Kingdom and Denmark.
In Singapore, cervical cancer is the 10th most common cancer in women, making up about 3.1% of reported cancers from 2010–2014. 5 The incidence of cervical cancer and its mortality rate have been declining in Singapore since the introduction of opportunistic Pap smear screening from the 1980s and the implementation of the national cervical cancer screening program (Cervical Screen Singapore) in 2004. Nevertheless, 1005 new cases of cervical cancer were diagnosed in Singapore from 2010–2014, accounting for 357 deaths. 5
There are currently two vaccines, Cervarix and Gardasil, available in Singapore from 2007 and 2006 respectively. Trials of both vaccines have shown more than 90% efficacy in preventing CIN 2, CIN 3, and adenocarcinoma-in-situ caused by HPV-16 or HPV-18, 6 and has been shown to be cost-effective in lowering the burden of HPV-related diseases. 7 It is recommended to females 9–26 years of age.8,9 The HPV vaccines have been included in Singapore’s National Immunization Schedule since 2010, but vaccination is not compulsory, and is not routinely offered to eligible girls.
A study in 2009 showed Singaporean women’s knowledge of HPV infection was poor, with only 20% having heard of it. However, attitudes towards HPV vaccination were generally positive, 10 despite the low HPV uptake rate of 8.8% in a study done among nurses. 11
To encourage its uptake, our government allowed the use of Medisave (a national compulsory saving scheme) to pay for HPV vaccination with effect from November 2010. However, it is unclear if this has improved the uptake of the vaccine to date. There is a need to raise awareness in women at a younger age about HPV, its effects and the benefits of HPV vaccination if we are to further reduce the incidence and severity of cervical cancer.
We aimed to explore the knowledge and attitude towards HPV vaccine with respect to cervical cancer prevention in a group of pre-university female students in Singapore, and see if a simple standardized 10 minute presentation can improve their knowledge and acceptance of the vaccine.
Materials and methods
The study was approved by the SingHealth Centralized Institutional Review Board. It was conducted at a typical public pre-university education center in the central area of Singapore with students typically aged 15–19 years old. We obtained approval from the education center’s administrators to do the study and recruitment on site.
The eligibility criteria were female students aged 15–26 years attending the education center. Students of this age range are beginning to make independent decisions regarding their own health. They are also within the target population for HPV vaccines. Team members approached groups of students for recruitment in March 2014. The students were ensured confidentiality, and informed of their right not to participate. Verbal informed consent was obtained before administering the questionnaires in English.
Participants first completed an anonymous self-administered questionnaire (Appendix 1). They then viewed a presentation consisting of standardized education slides on an electronic tablet by trained team members, and were given time to address any queries they may have. The educational slides presented basic facts about cervical cancer, HPV, the role of the HPV vaccine in preventing cervical cancer, the recommended eligibility for the vaccine, Medisave eligibility and the role of Pap smear in screening for cervical cancer. A post-education questionnaire (Appendix 2) was then administered to evaluate the impact of the education session on the students’ knowledge and attitudes with regard to cervical cancer vaccination and screening. No discussion was allowed between participants in the filling in of both questionnaires. Each member was trained to stick to the standardized presentation slides in an objective manner and not offer personal opinions, nor use persuasion to influence the participants. No vaccine was promoted over another. Each session lasted approximately 10 minutes. The questionnaires were labeled with a unique number and no personal identifiers were collected.
Statistical analysis
Data analysis was performed with SPSS version 22.0. McNemar’s paired test was used to compare the knowledge scores before and after the intervention. The paired-t test (two-tailed) was used to assess the acceptability of the HPV vaccine, based on the sample population who had not been vaccinated, and the proportion that responded ‘yes’ to the question on whether they would take up the vaccine or not.
Results
All 150 female students approached agreed to participate. The population surveyed was largely in the 15–19 year old age group (99.3%). Baseline data showed that only 29.3% of the participants were aware of the existence of the HPV virus and 26.7% of them had heard of the HPV vaccine. Only 4.0% surveyed were already vaccinated against HPV.
Out of the 26.7% who had heard of the HPV vaccine, the most common source of information stated was from a family member or friend (22.5%). Some learnt about it from clinics (15.0%), but few indicated that they learnt about it from the media such as the newspaper, television, radio, or even from the Health Promotion Board ((HPB) a national organization for health education and promotion). About one-third of the participants (32.5%) did not provide an answer to this question.
Ten questions were asked before and after the presentation (Appendix 2) to assess the gain in knowledge in the participants (Table 1). The questions covered knowledge about HPV, its vaccine and Pap smears.
Proportion of students who answered correctly before and after the educational intervention.

HPV: human papillomavirus; Pap: papillomavirus.
There was a statistically significant improvement in mean test scores (Table 2). All questions shown in Table 1 showed significant improvement, except the question on the symptoms of HPV infection, and the candidates of the Pap smear. This showed that a short educational session was able to raise the awareness and knowledge of the students in most aspects with regards to HPV, its vaccine and Pap smears.
Mean test scores (maximum 10).

The importance of any intervention is not only to improve the knowledge of the participants, but to also change their attitude. This correspondence was displayed in the significant improvement in responses towards receiving the HPV vaccination after the educational intervention (Table 3).
Distribution of responses towards receiving the HPV vaccination amongst 144 female students who have not had the HPV vaccine.

HPV: human papillomavirus.
Our survey revealed six students (4.0%) who were already vaccinated against HPV. Amongst the 144 who were not vaccinated, approximately one-third (31.3%) indicated that they were willing to be vaccinated at baseline, while 63.9% of them were ambivalent (‘maybe’). After the educational presentation, there was a significant improvement. More than half (51.4%) stated that they wanted to be vaccinated (two-tailed paired t-test, p<0.05; Table 3), and the proportion of those who remained ambivalent fell to 47.2%.
Out of the five participants (3.5%) who were not willing to be vaccinated at the start, some of the reasons given were ‘too expensive’, ‘too troublesome’ and ‘not likely to catch virus’, while two gave ‘no sexual exposure’ as their reason. The number of participants not willing to go for the vaccine dropped to one (0.7%; who stated ‘no sexual exposure’ as the reason) after the intervention. It was interesting to note that our simple presentation was able to influence a change in the decisions of four out of five female students who initially rejected the vaccine.
Discussion
We achieved a good response rate with almost all students answering all the questions. Despite the vaccine being available in Singapore from 2006–2007, low awareness about HPV (29.3%) and its vaccine (26.7%) was found to be prevalent. This corresponded to the 2009 study done in Singapore amongst nurses. 11 This was particularly noteworthy since the recruitment population comprised students of one of the top pre-university education centers in Singapore. More studies of the general population should be carried out to ascertain if an even lower rate of awareness is present.
The largest source of information about HPV vaccination cited by the participants was family members and friends rather than healthcare professionals, HPB or the media. This large knowledge–information gap, even amongst these well-educated students, shows that much can and should be done in terms of public health education and outreach. The acceptability of the vaccine was moderate (31.3%) at baseline, with most being ambivalent, with a few rejecting the vaccine (3.5%). This indicates a prime potential to educate and reach out to these young women.
The use of a short standardized educational presentation on an electronic tablet was effective in raising the knowledge scores in this cohort of the female students from a mean of 4.95 to 8.61 out of a total of 10. Accurate knowledge is important to dispel any myth or misconception about cervical cancer, HPV and its vaccine. This is especially important since our study showed that the most common source of information was family and friends, and not official sources. Also, an improved and validated educational system and questionnaire could be used, particularly with regard to education towards symptoms of HPV infection and the candidate profiles for Pap smears. These were the two questions out of the 10 in the questionnaire which did not show a statistically significant improvement.
Our study also demonstrated that as knowledge improved, so did the acceptability of HPV vaccine. More expressed willingness to consider the vaccine (from 31.3% to 51.4%) and fewer rejected it (from 3.5% to 0.7%) after the intervention. However, we acknowledge that the expression of acceptability may not translate to the actual uptake of the vaccine. Future studies should include a follow-up where participants are contacted and assessed on the actual uptake.
Although the sample size was small (N=150), it was enough to demonstrate the effectiveness of a short, simple educational presentation. However, larger studies with more heterogeneous demographics should be carried out in order to be able to clearly identify solutions to implement for health promotion.
Other limitations of this study included convenience sampling, unvalidated questionnaires and limited sampling consisting of students from only one educational center.
Conclusion
A low awareness and acceptability of the HPV vaccine was shown to be prevalent amongst pre-university female students in Singapore. A simple educational intervention was able to improve these. The information gained from this study can be used to plan further, larger studies on effective population-based health education strategies targeting a wider population of young adolescent females in Singapore, and improve the uptake of this potentially life-saving vaccine.
Footnotes
Appendix 1. Pre questionnaire on human papillomavirus (HPV) vaccine and cervical cancer prevention
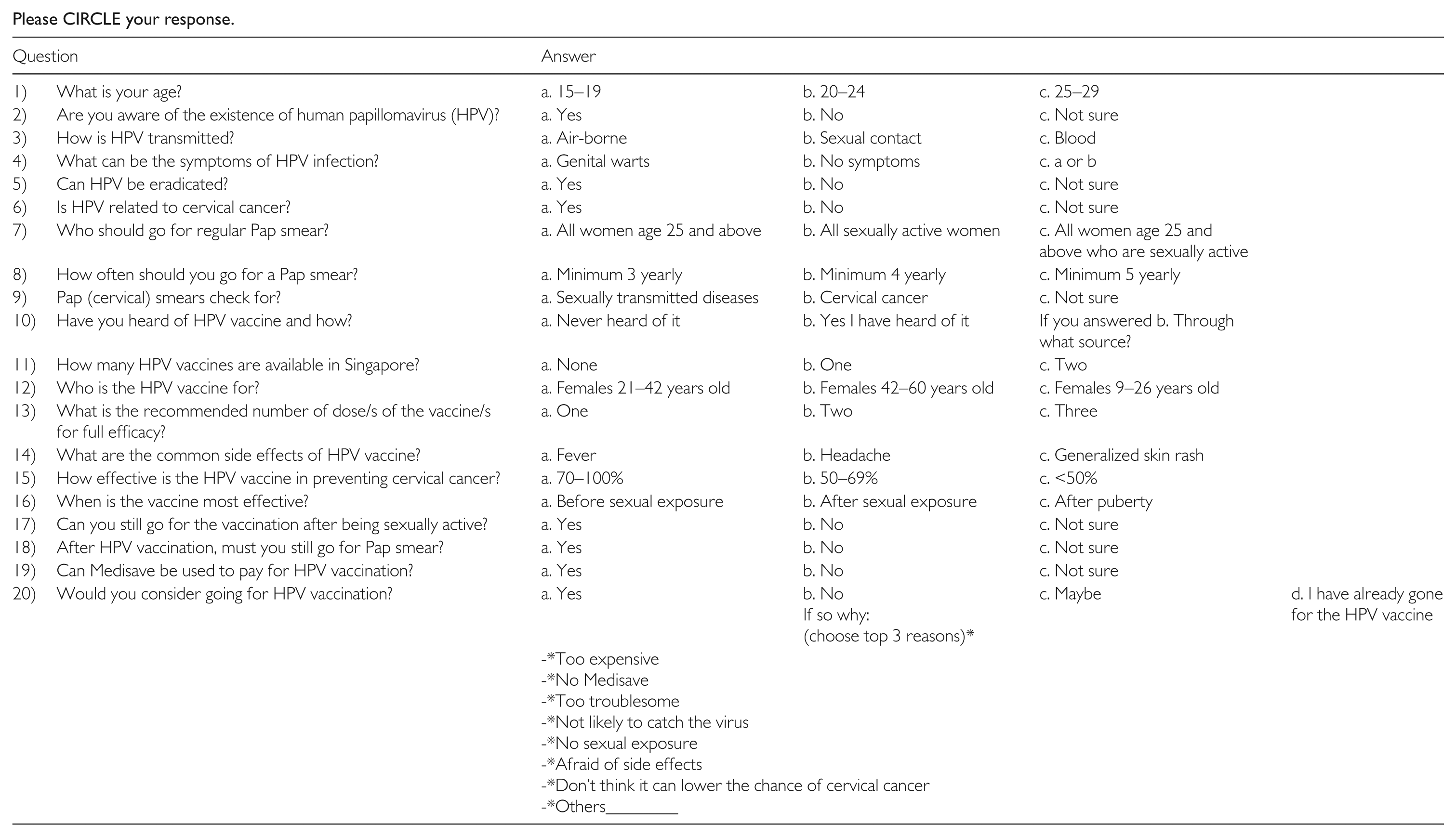
Please CIRCLE your response.
| Question | Answer | |||
|---|---|---|---|---|
| 1) What is your age? | a. 15–19 | b. 20–24 | c. 25–29 | |
| 2) Are you aware of the existence of human papillomavirus (HPV)? | a. Yes | b. No | c. Not sure | |
| 3) How is HPV transmitted? | a. Air-borne | b. Sexual contact | c. Blood | |
| 4) What can be the symptoms of HPV infection? | a. Genital warts | b. No symptoms | c. a or b | |
| 5) Can HPV be eradicated? | a. Yes | b. No | c. Not sure | |
| 6) Is HPV related to cervical cancer? | a. Yes | b. No | c. Not sure | |
| 7) Who should go for regular Pap smear? | a. All women age 25 and above | b. All sexually active women | c. All women age 25 and above who are sexually active | |
| 8) How often should you go for a Pap smear? | a. Minimum 3 yearly | b. Minimum 4 yearly | c. Minimum 5 yearly | |
| 9) Pap (cervical) smears check for? | a. Sexually transmitted diseases | b. Cervical cancer | c. Not sure | |
| 10) Have you heard of HPV vaccine and how? | a. Never heard of it | b. Yes I have heard of it | If you answered b. Through what source? | |
| 11) How many HPV vaccines are available in Singapore? | a. None | b. One | c. Two | |
| 12) Who is the HPV vaccine for? | a. Females 21–42 years old | b. Females 42–60 years old | c. Females 9–26 years old | |
| 13) What is the recommended number of dose/s of the vaccine/s for full efficacy? | a. One | b. Two | c. Three | |
| 14) What are the common side effects of HPV vaccine? | a. Fever | b. Headache | c. Generalized skin rash | |
| 15) How effective is the HPV vaccine in preventing cervical cancer? | a. 70–100% | b. 50–69% | c. <50% | |
| 16) When is the vaccine most effective? | a. Before sexual exposure | b. After sexual exposure | c. After puberty | |
| 17) Can you still go for the vaccination after being sexually active? | a. Yes | b. No | c. Not sure | |
| 18) After HPV vaccination, must you still go for Pap smear? | a. Yes | b. No | c. Not sure | |
| 19) Can Medisave be used to pay for HPV vaccination? | a. Yes | b. No | c. Not sure | |
| 20) Would you consider going for HPV vaccination? | a. Yes | b. No |
c. Maybe | d. I have already gone for the HPV vaccine |
| -*Too expensive |
||||
Appendix 2. Post questionnaire
Dear students, thank you for listening to our talk on the human papillomavirus (HPV) and cervical cancer. We hope that you have benefitted from the lecture and would like to find out how much you have learnt. Please take about five minutes to read through and answer the questions. Thank you for your time and participation.
Acknowledgements
We thank Hwa Chong Junior College (HCJC) for their kind collaboration for this study. Tokens of appreciation (without any company logo) were provided by MSK and Merk pharmaceuticals. The biostatistician is Ms Eileen Koh Yi Ling, from SingHealth Polyclinics Research Department.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This work was supported by SingHealth Family Medicine Residency.
