Abstract
Background:
Pain alters the neuromuscular activation and results in altered movement adaptations. A new exercise prescription method proposes that we can restore the neuromuscular control by rehabilitating the deficient neural drive through Pilates exercises. This is done by identifying the postural control deficits using single-leg tests such as hopping, half squats and heel raises. The aim of this study was to find out if this method of prescribing exercises results in clinically relevant outcomes.
Methods:
Fifteen patients with chronic non-specific low back pain with unilateral musculoskeletal pain were recruited. Following consent, all patients were randomly assigned either to perform gym or Pilates-based individualised exercises once weekly for six weeks. The primary outcome was to measure the pain intensity using a 0–10 numerical rating scale. The secondary outcome measures were: the global perceived effect scale (GPE; 0–10), the patient-specific functional scale (PSFS; the patient-generated measure of disability) and the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC; the condition-specific measure of disability).
Results:
There were statistically significant differences noted after intervention within the control group in the numerical rating scale (P=0.041), GPE (P=0.024), PSFS (P=0.039) and within the experimental group in the WOMAC (P=0.008), GPE (P=0.007) and PSFS (P=0.007). However, as there were clinically significant baseline differences, the within-group difference could be due to regression to the mean. There were no statistically significant results between the two groups after intervention.
Conclusion:
This new prescription method for Pilates-based exercises may improve disability and global perception of recovery. However, the outcomes are not different from a regular gym-based exercise programme.
Background
Created and taught by Joseph Pilates in the early 20th century, Pilates exercises were introduced to the performing arts community. Pilates exercises involve full-body movements to train motor control with coordination between body and mind. The exercises are based on principles such as centering, concentration, control, precision, fluidity of movements and breathing.1–4 Research to date has found some justification that Pilates exercises help lessen pain and disability5–7 by targeting underlying aberrant neuromuscular control.5–7
However, a recent systematic review rejects the superiority of Pilates-based exercises to other forms of exercises. 8 In a recent review, Hodges suggests that some of the existing tools of rehabilitation that require an overhaul could be those related to the training of motor control or movement strategy. 9 In the light of proposals to overhaul the motor-control training strategies surfacing in the literature, a new method of exercise prescription has been proposed. This new method suggests restoring the neuromuscular control by facilitating the deficient neural drive through Pilates-based exercises.10,11 It was recently tested on those who had long term unilateral musculoskeletal disorders,10,11 and successfully demonstrated its validity and reliability. The assessment process of this new method involves finding the side (or leg) with dynamic postural stability deficits (PSDs) using simple single-leg tests such as rebound hops, half squats and heel raises. After the side or leg with a dynamic PSD has been established, an individual-specific set of Pilates-based exercises is prescribed to improve the deficit.
This study aims to find out if treating dynamic PSDs identified with this method can improve pain and disability among people with chronic non-specific low back pain and unilateral musculoskeletal disorders.
Methods
Research design
This study was conducted as a randomised pilot trial, enlisting participants with chronic non-specific low back pain, along with unilateral musculoskeletal injuries.
Blinding
This was a double-blinded randomised pilot trial. The participants were randomly assigned to one of two types of exercises. Different physiotherapists conducted the control and experimental group exercises. These physiotherapists were also blinded to data collection during the first and final visits.
Sample size
A sample size determination is study-specific. With a 15% drop-out rate taken into consideration, we decided to use a sample size of 40 for this study. This conclusion was reached after taking into consideration the studies by Tulloch et al. 10 and Ross and Guskiewicz. 12 In those studies, 35 participants were required to detect a 15% difference in their time to stabilisation (TTS) measurements. It was calculated by assuming two-sided alpha at 0.05 and power at 0.8.
Inclusion and exclusion criteria
Participants were included if they had musculoskeletal injuries in only one of their lower limbs, along with chronic non-specific low back pain, were able to do rebound hopping on the affected lower limb and were aged 18–75 years. Participants were excluded if they had: (a) incurred lower-limb injuries within the last six weeks; (b) undergone surgery within the last 12 weeks; (c) ligament reconstruction or any surgery done on the affected lower limb within the last six months; (d) fractures to their lower limbs within the last 12 months; (e) any neurological condition; (f) any inflammatory joint conditions or lower back disorders, vestibular conditions, malignant conditions, or (g) any cognitive and/or visual impairments.
Study procedures
This study was conducted at the outpatient physiotherapy clinic at Changi General Hospital in Singapore, using participants screened for eligibility. Following consent, a total of 40 participants were screened for inclusion and exclusion criteria. They were then randomly assigned to one of two types of exercises using a sealed envelope. One group was assigned individualised Pilates-based exercises, the other general gym-based exercises. The participants attended weekly exercise classes for six times in six consecutive weeks.
Outcome measures
The participants were required to record the primary and secondary outcome measures during their first and the final visit. The primary outcome was to measure the pain intensity using a 0–10 numerical rating scale (NRS). The secondary outcome was measured with the global perceived effect scale (GPE; 0–10), the patient-specific functional scale (PSFS) and Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) scores.
Interventions
The participants in the experimental group performed individualised Pilates exercises as prescribed by Pilates-trained physiotherapists.10,11 The side (or leg) with dynamic PSDs was identified by asking the participants to perform five repetitions each of single-leg tests such as single-leg hops (SLH), single-leg (SL) half squats and single-leg heel raises (SHR) on both legs.
Self-reported participant effort was measured using a 0–10 scoring system similar to the PSFS, with 0 being unable to perform the test and 10 being able to perform the test perfectly without perceiving any difficulty. The poor-performing side during the tests between the left and right side was identified as the perceived PSD side by the participants and documented. The participant’s PSD side was verified by the observation of the physiotherapist assigned to watch for their pelvic and overall stability while performing the tests. Standardised verbal instructions were given to avoid bias. The dynamic PSD side (as confirmed by the physiotherapist) was then used to categorise patients as having flexion or extension bias to prescribe the individualized Pilates exercises.10,11
The physiotherapist prescribed participants in the control group gym-based exercises, as per their needs. A combination of strengthening, flexibility and balance training exercises was performed using gym equipment such as the leg press, foam roller, wobble board and stationary bicycle. The exercises sessions in both groups lasted for half an hour each session, once per week, for six consecutive weeks.
Statistical analyses
All statistical tests were performed using SPSS 23.0.0.0 (SPSS Inc., USA). The data were checked for normality prior to the analyses. The non-parametric tests were performed to find differences at baseline before the intervention. 13 The pre to post-exercise changes within the control and experimental groups were analysed using the Wilcoxon signed-rank test. The level of statistical significance was set at P<0.05. The differences between the control and experimental groups were analysed using analysis of covariance (ANCOVA) as there were baseline differences between the groups. 14

Study protocol.
Results
A visual inspection of data distribution was carried out with box-and-whisker plots on the patient demographic data, as well as the outcome measures at baseline. There were a few outliers noted in the distribution; however, as there was only a small sample size (n=15), the baseline characteristics have been presented as median (interquartile range) in the Table 1.
Baseline characteristics.
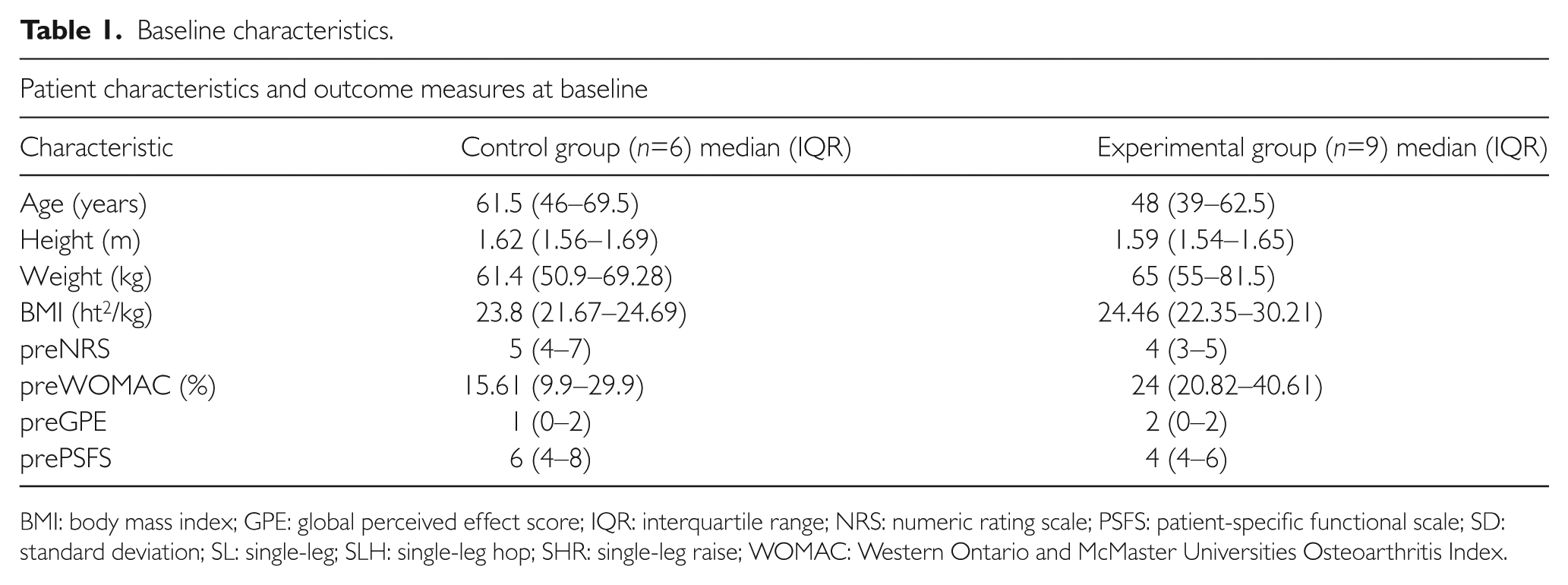
BMI: body mass index; GPE: global perceived effect score; IQR: interquartile range; NRS: numeric rating scale; PSFS: patient-specific functional scale; SD: standard deviation; SL: single-leg; SLH: single-leg hop; SHR: single-leg raise; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index.
The non-parametric tests showed no statistically significant differences at the baseline for all the outcome measures (Table 2). However, there were clinically significant differences between the control and the experimental groups in WOMAC and PSFS (Table 2).
Outcome measures at baseline.
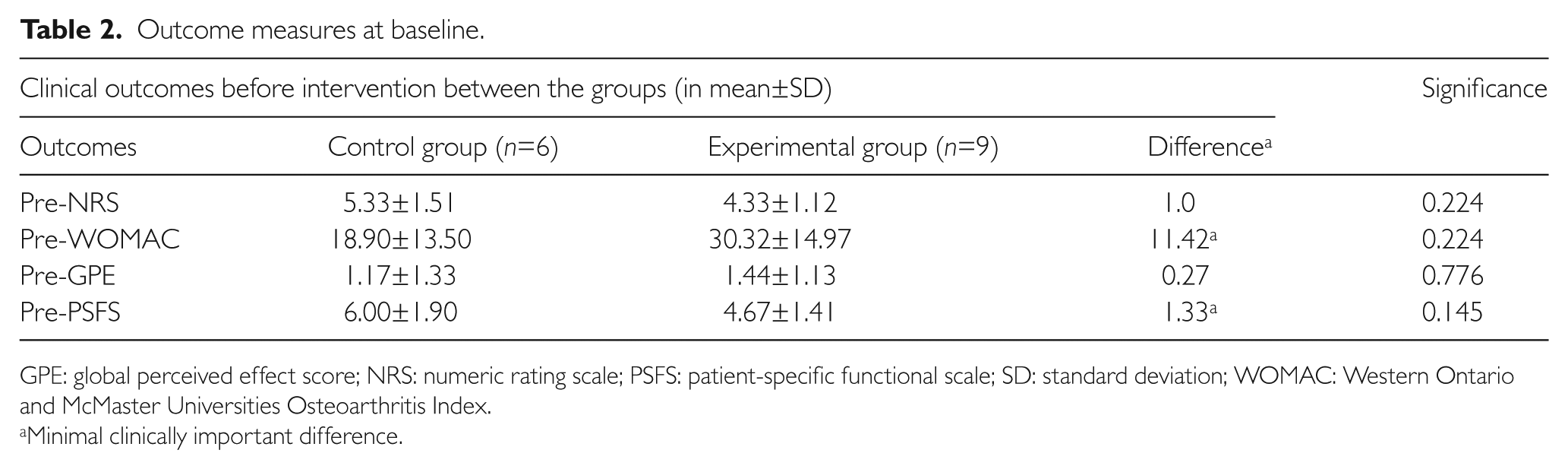
GPE: global perceived effect score; NRS: numeric rating scale; PSFS: patient-specific functional scale; SD: standard deviation; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index.
Minimal clinically important difference.
As there were clinically significant differences in WOMAC and PSFS scores at the baseline, an ANCOVA was performed to find the differences between the groups after the intervention. 14 All outcome measures met the assumptions needed for ANCOVA, including the homogeneity of regression. The ANCOVA was performed on all the outcome measures separately to test the null hypothesis that the error variance of the dependent variable (see Table 3) is equal across the groups. There were no statistically significant differences between the groups after the intervention (Table 3).
Between-group difference after the intervention.

GPE: global perceived effect score; NRS: numeric rating scale; PSFS: patient-specific functional scale; SD: standard deviation; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index.
The outcomes of all different tests (NRS, WOMAC, GPE and PSFS) within the two groups were compared before and after intervention using the Wilcoxon signed rank test. There were statistically significant differences noted after intervention within the control group in the NRS, GPE and PSFS outcomes (Table 4). There were also statistically significant differences noted after intervention within experimental group in the WOMAC, GPE and PSFS outcomes (Table 4).
Clinical outcomes: within-group differences.

GPE: global perceived effect score; NRS: numeric rating scale; PSFS: patient-specific functional scale; SD: standard deviation; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index.
Significance.
Where applicable, Spearman or Pearson correlation coefficients were computed (Table 5) to find the relationship between the disability scores (pre-WOMAC, pre-PSFS) and the single-leg tests (pre-SHR, pre-SLH, pre-SL half squat) that were used to decide the side of PSDs.10,11,15 There was no correlation between the disability scores and the single-leg tests.
Relationship between disability and single-leg tests.

PSFS: patient-specific functional scale; SL: single-leg; SLH: single-leg hop; SHR: single-leg raise; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index.
Correlation is significant at the 0.05 level (two-tailed).
Correlation is significant at the 0.01 level (two-tailed).
Discussion
Based on the scores in Table 4, the study has shown that the new method 10 of prescribing a six-week regime of individualised Pilates-based exercises to patients with unilateral musculoskeletal pain and chronic low back pain is effective in reducing disability, and in improving global perception of recovery. To our knowledge, this is the first study to show the effectiveness of this new method, which aims to identify and treat dynamic PSDs.10,11
This is consistent with a recent meta-analysis, which suggests that an exercise programme that aims to improve coordination/stabilisation and strength/resistance can have a significant effect on reducing symptoms in chronic low back pain. 16
This study hoped to investigate if the tailored prescription of Pilates-based exercises was more effective than the gym-based exercises. The findings show that the participants in the control group who performed gym-based exercises for six weeks had a significant decrease in pain scores (NRS) and disability (PSFS), as well as a significant increase in global perception of recovery (GPE) (Table 4). In fact, there were no statistically significant differences between the Pilates-based exercises and the gym-based exercises after the six-week period (Table 3).
There are a few possible reasons for this. The significant changes in the participants who performed gym-based exercises could have been due to a real increase in strength and coordination, as mentioned in the meta-analysis. 16 Another reason is that there were clinically significant differences between the experimental and control groups in WOMAC and PSFS at baseline (Table 2). Such differences at baseline could have balanced out the results between the two groups after the intervention. The lack of difference between the groups could also have been due to the small sample size. A similar trial with a larger sample size, without baseline differences, and with a control arm is required to verify this finding.
In this new method of exercise prescription, 10 it is proposed that the dynamic PSDs can be detected using single-leg tests such as SHR, SLH and SL half squats, scored on a self-reported performance rating scale (0–10).10,11,15 The physiotherapist decides on the side/leg that has dynamic PSDs using a 0–10 score rating (0 being unable to perform; 10 being no difficulty at all) the participants identified. If the self-reported scores were low on one side compared to the other, the side with the lower score was determined as the side/or leg with dynamic PSDs. We wanted to find if the self-reported performance score from the single-leg tests (thought to represent dynamic PSDs) had any association with the patient’s actual disability. If such an association exists, this new method will be useful in detecting and treating PSDs that occur with disability.
In our study, analyses were performed to identify if there are any relationships between the self-rated single-leg tests (SHR, SLH, SL half squats) used to detect dynamic PSDs and the outcome measures used to identify disability (PSFS, WOMAC). There was no correlation noted between the self-rated scores from the single-leg tests and the disability scores (Table 5). These results show that the performance on the single-leg tests is not related to the patient’s disability status. Despite this, the therapists in this study were able to identify the PSDs using this new method of exercise prescription.
The findings in this study were consistent with previous reports of a lack of association between self-reported stability deficits and their functional performance.15,17 It is still premature to dismiss the stability deficits detected by the new method of exercise prescription as it could hold a potential scope for rehabilitation. It could be that the outcome measures used in this study to identify disability did not detect the neural drive deficits that were thought to be the cause of such self-reported PSDs. As of now, we understand that the new method does not reflect the disability as measured using the PSFS and WOMAC. Future research should also focus on refining the assessment process and its diagnostic accuracy.
Limitations
There were a few limitations in this study. A statistically significant difference in the experimental group between the pre and post values could have been because of regression to the mean. 18 Hence, it is important to exercise caution when interpreting the data.
The other limitations in this study were drop-outs, a small sample size, and interviewer bias that was likely to have affected the data collection. Although a 15% drop-out rate was factored in during the sample size estimation, there turned out to be more drop-outs than expected. The most common reasons for participants dropping out were compensation issues, and the preference for doing either gym-based exercises or a combination of gym and Pilates-based exercises. The patients were attracted to the new exercise equipment in the gym, and wanted to try it out, in the hopes it would improve their condition better. The drop-outs and no-shows are some of the practical challenges of research in a clinical setting. In this study, the missing data due to drop-outs could have resulted in spurious statistically significant results in the pre to post data analyses within the groups. 19
In addition, the physiotherapists could have been biased in determining the injured side as the side with dynamic PSDs, resulting in interviewer bias. The new method’s test procedures were however standardised to reduce this bias. Questionnaire bias could have occurred in this study from the outcome measure (WOMAC) as it comprised questions to measure disability. The flaws in the questions or varying interpretation of the questions might have led to differences in accuracy between the groups that were compared. The outcomes including PSFS and GPE required participants to recall and report their condition. This could have led to recall biases during data collection. Measures were taken to standardise the outcome measurements in order to reduce these biases.
Footnotes
Conflict of interests
None declared.
Funding
This study was funded by the Changi Health Fund from Changi General Hospital, Singapore.
