Abstract
Introduction:
The widespread shortage of nurses has been exacerbated by an ageing workforce. Though skilled and productive, older nurses are more vulnerable to the physical and mental demands of nursing. Hence, this review was performed to determine the existing evidence on challenges faced by older nurses, factors which promote or deter retirement and strategies that could help in their retention. The results of this review would help with the implementation of age-friendly initiatives to enable older nurses to work longer, while simultaneously allowing institutions to maintain high-quality nursing care.
Methods:
A search was done using three databases, namely MEDLINE, the Nursing and Allied Health Literature (CINAHL) and PsycINFO. Primary studies and reviews published between 2004 and 2015 were retrieved. Keywords used were ‘older nurses’, ‘retirement’, ‘re-employment’ and ‘retention’.
Results:
Articles retrieved were mainly qualitative studies. A few quantitative surveys and reviews were reported. The definition of older nurses was inconsistent across the literature. Personal health concerns and limitations, computerisation and shift work were common challenges faced by older nurses, while monetary factors, health and workload were consistent themes on early retirement. Financial reasons were also identified as factors associated with retention, along with flexible schedules. Almost all strategies suggested in the literature for retaining older nurses lacked empirical testing.
Conclusion:
The ageing process may render certain tasks less desirable and more challenging for the older nurses. Employers could pay attention to the needs of an older workforce through improved workplace practices and being familiar with factors associated with early retirement and retention.
Introduction
In many countries around the world, there is growing concern about the shortage of nurses, a phenomenon that is exacerbated by an ageing population. 1 The average age of the working nurse in Australia, Canada and the United Kingdom was reported to be mid-to-late-40s, with 30–40% being over the age of 50. 2 In the United States, at least 40% of the nurses in the workforce are expected to be more than 50 years of age by the year 2020. 3 The average age of registered nurses in Singapore was reported to be 37 years old in the year 2013, 4 with only 16% being 45 years old or older. However, with Singapore being one of Asia’s fastest ageing populations, we can reasonably expect the nursing workforce to become older in the near future. According to published statistics on the labour force in Singapore, the proportion of workers aged 60 and above has increased from 3.7% in 2004 to 9.3% in 2013, and further increased to 10.3% in 2014. 5
The need for an age-friendly working environment is pertinent in nursing. Nursing involves shift work, physical care, frequently missed breaks and interaction with very ill patients, notwithstanding the need for critical thinking skills and technical skills to care for complex patient populations. Ageing is known to be related to reductions in aerobic power, muscular strength and endurance, reaction speed, acuity of the senses, sleep disturbance and increased risk of chronic disease. More significantly, older healthcare workers are known to suffer from back pain, other musculo skeletal disorders and stress-related mood disorders. 6 Although older nurses are more vulnerable, there are also many advantages to retaining them. Older nurses are known to be the most skilled and productive employees. They have a wealth of life experience, superior communication skills, dedication and loyalty, take fewer sick days and are less inclined to consider working abroad. 1
This review was performed to determine the existing evidence based on specific challenges faced by older nurses, factors that promote or deter retirement and strategies that could help in their retention. Results of this review would help to inform the implementation of age-friendly initiatives which would enable older nurses to work longer, while at the same time allow institutions to maintain high-quality nursing care.
Method
A search for articles describing challenges faced by older nurses, and strategies to retain them, was carried out in January 2015 and repeated in June 2015. The search strategy included all types of studies (both quantitative and qualitative), as well as reviews. Three electronic databases were used: MEDLINE, Nursing and Allied Health Literature (CINAHL) and PsycINFO. Keywords used for the search were ‘older nurses’ AND the terms ‘retirement’ OR ‘re-employment’ OR ‘retention’. Given rapid changes in the healthcare industry, only articles published within the last ten years (2004–2015) were included.
Results
A total of 20 journal articles were used in this review. Most of the published articles described the conduct of qualitative studies (
Challenges faced by older nurses
Older nurses reported facing specific challenges in their workplaces, although it was unclear whether these challenges were associated with the ageing process or changes in the general work environment. By their mid-40s, older nurses might start to experience sensory limitations related to vision and hearing acuity and risk contracting chronic illness. Some reported current or recent weight problems, most commonly weight gain.7,8 Henceforth, personal health concerns and limitations are common issues faced by older nurses.2,8 Older nurses also tend to report more physical pain; some indicated chronic neck, shoulder or back pain, while others suffered from pain associated with musculoskeletal disorders or arthritis. 8 Chronic pain conditions were reported to be aggravated by normal nursing duties. 7
In a study looking specifically at age-related changes and challenges at work, older healthcare workers (nurses and allied health professionals) working in hospital settings reported that reading medication and manual handling had become more challenging (Table 1). 6 Older workers also narrated that shift work had become increasingly more tiring,6,7 rapid computerisation was challenging and working with computers was associated with physical discomfort (Table 1). 6
Challenges faced by older nurses.

Factors associated with early retirement
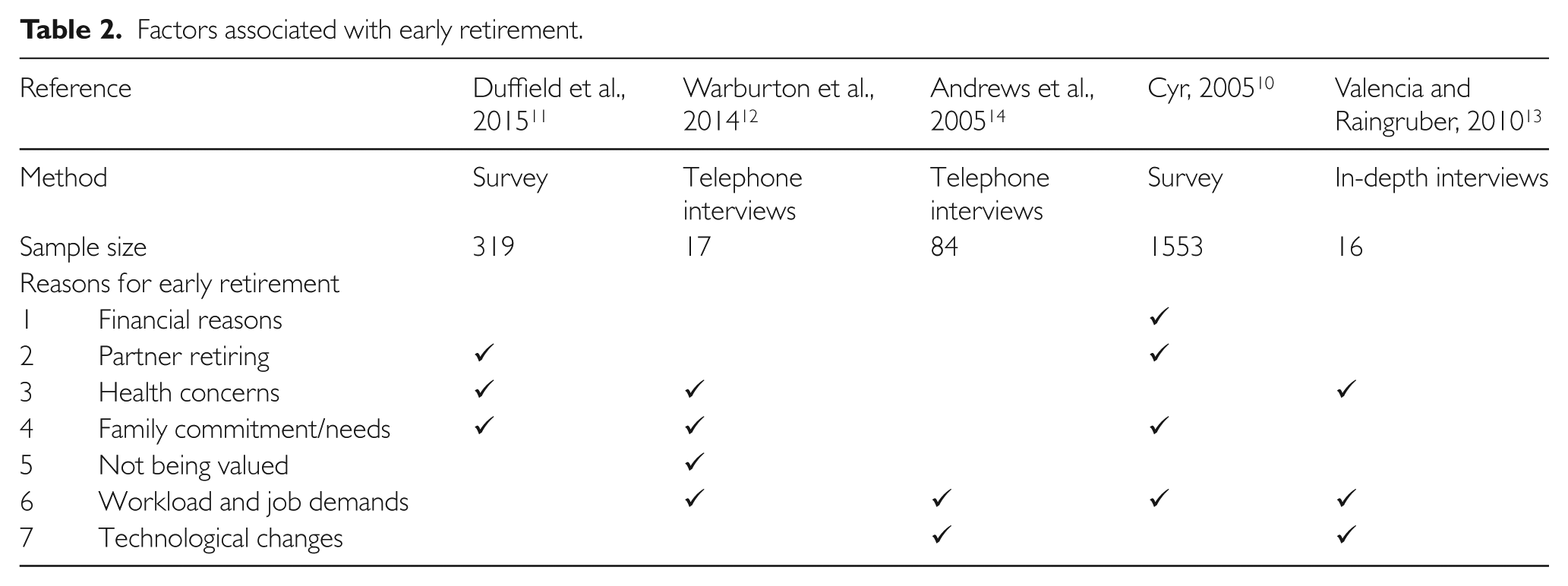
Older nurses are leaving the workforce primarily for financial reasons. Nurses tend to retire early if they perceive that they have attained financial security 10 for their post-retirement years. In a study on older Australian nurses’ intention to leave the workforce, 11 respondents reported ‘financial security’, ‘maximum superannuation benefits reached’ and ‘optimal taxation situation’ as key financial considerations for leaving the workforce (Table 2). Other reasons include health concerns (age related or work-load related) and family situations (partner retiring or need to care for children or sick relatives) as summarised in Table 2.10–12 Smaller studies12,13 echoed the same concerns, with older nurses reporting that health concerns or issues, heavy work demands or changes in the work place prompted them to leave the workforce. Other ‘push’ factors, such as not being valued for providing high-quality care in a resource-constrained work environment was also mentioned. 12 Other negative aspects of work which lead to older nurses leaving include rapid technological changes which impacted on older nurses’ practice competence, and job stress in relation to heavy workloads and decreased physical and mental stamina.13,14
Factors associated with early retirement.
Factors associated with retention
A literature review 15 which included 38 papers published between 1998 and 2007 reported that older nurses valued being recognised for their expertise and work, and preferred managers who are professional, demonstrate integrity and empower others. They preferred direct involvement in decision-making and being able to make an impact on patient care through greater empowerment and autonomy. Despite the common misconception, older nurses do appreciate ongoing professional development opportunities. They wanted to continue to learn and to be able to keep up with changes, especially technological advances. Older nurses also wanted a reduction in workload, to be reassigned to less physically demanding jobs and to have access to flexible work arrangements. Adequate compensation for years of experience, knowledge and responsibility would also entice older nurses to work longer. 15
Financial consideration was a key factor which prompted nurses to continue working. 16 Older nurses working in their late 50s and early 60s have been found to continue to work in order not to compromise their financial situation in the future or to finance the post-retirement lifestyle they desired.12,13
Another commonly identified reason for older nurses to stay in the nursing workforce is patient contact and interpersonal relationships, which they found enjoyable and rewarding. 12 Satisfaction with daily work and being valued by senior management had also been reported as reasons for older nurses to stay longer in nursing.12,16 Support of co-workers and being able to work particular days or reduced hours (work flexibility) also positively impacts on nurses’ decision to continue working. Older nurses also valued being able to continue to learn and to develop themselves professionally. 12
In a large-scale survey study undertaken in 2004, 16 but published seven years later, older workers in the healthcare sector were also more likely to think that they can work until 65 years of age or beyond if the work is deemed not too physically and mentally demanding and their own health status is good (Table 3). On the other hand, they are more likely to want to work to 65 years or beyond if they consider work to be an important part of their life and because of personal economic incentives. The decisions of life partners and close friends to retire or continue to work past 65 years also had a strong influence on older workers’ belief that they can and want to work beyond 65 years (Table 3). 16
Factors associated with retention.
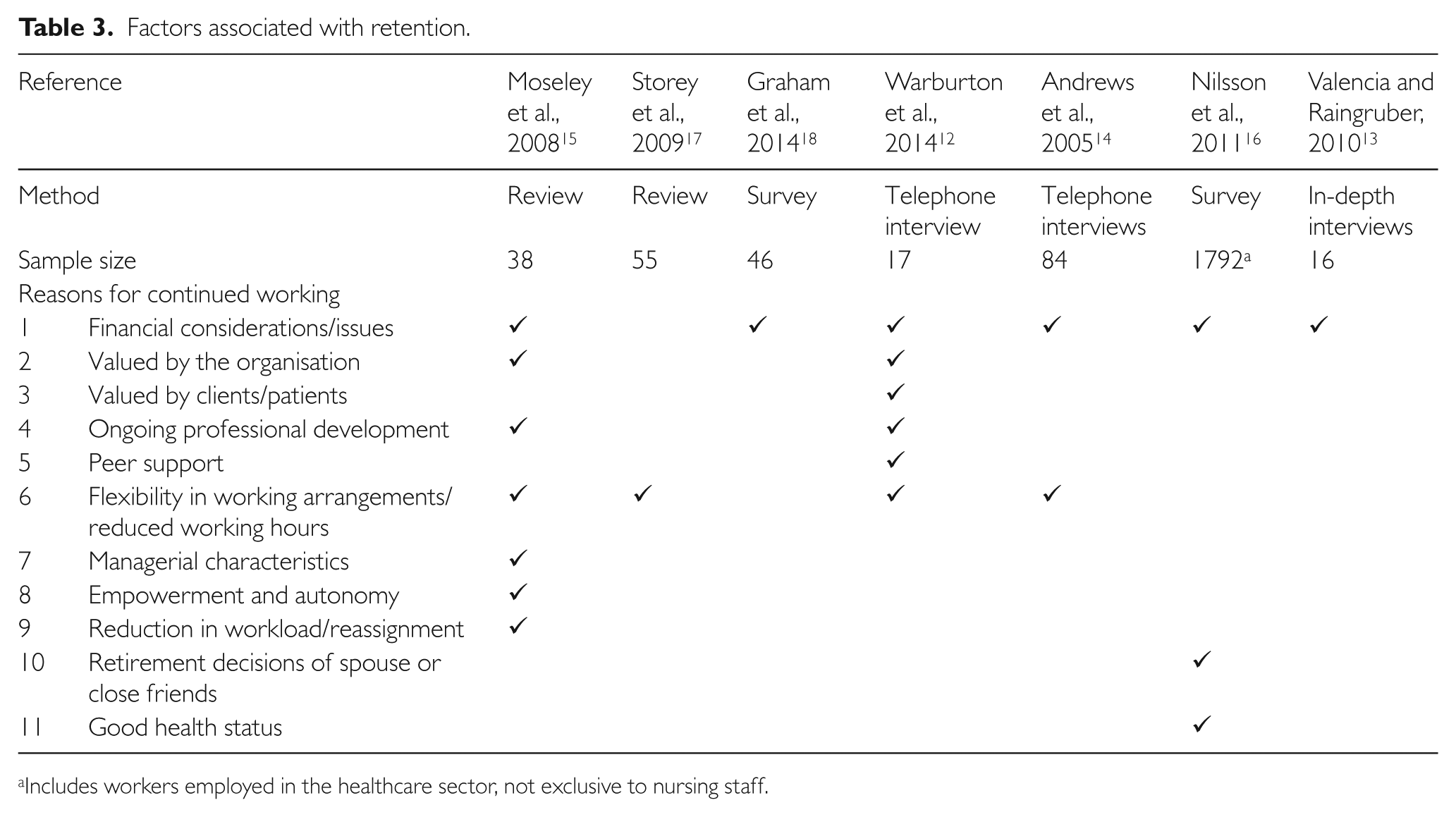
Includes workers employed in the healthcare sector, not exclusive to nursing staff.
Strategies for retaining older nurses
As summarised by Fitzgerald 2 , in order to effectively retain older nurses, the practice environment needs to be ergonomically redesigned to save physical energy and prevent musculoskeletal injuries; human resources practices need to be more flexible, allowing for phased-in retirement plans, flexible scheduling, education and training, as well as alternative or redesigned roles (Table 4).
Strategies to retain older nurses.

Many older nurses favoured flexible working arrangements, citing reasons such as family commitments, health-related reasons or fatigue, and the desire to travel or have more time for themselves. 19 Flexible working arrangements could take the form of job sharing (typically two people performing part-time work normally undertaken by one person working full time), shorter shifts, casual hours or part-time when they are nearing retirement or if they wish to re-join nursing after retirement.2,14 Flexible working arrangements were also reported as the number one priority in enabling older nurses to manage both their home and work caregiving responsibilities. 20 In a large-scale survey involving 1553 nurses, it was found that 78% of the respondents would contemplate working part-time or per diem work (Table 4). 10 The study also found that financial incentives and giving ideal hourly rates would motivate nurses to stay in the profession rather than to retire. 10 However, the study involved younger nurses (51% less than 46 years old), who might not have given enough thought to the issue of retirement. 10 On the other hand, availability of flexible working arrangements alone might not be enough. A greater intention to remain may also be related to how fair and supportive older nurses perceived their immediate supervisor to be. 21
In all three review articles,2,8,22 authors had advocated for improvements to the physical environment of the workplace in order to retain older nurses. In particular, authors called for ergonomically correct designs and equipment to support safe patient handling, 22 and use of devices such as ceiling lifters. 8 Other recommendations include decentralisation to reduce walking distances, adequate lighting, non-slip floor surfaces and provision of respite rooms. 8
A survey study by Wray et al. 23 demonstrated that older nurses reported less access to continuing professional development activities when compared to their younger colleagues. Justifying the need for continual education and training for older nurses, Cohen 22 argued that the lack of education opportunities may lead to the onset of employee boredom and indifference toward the job, hence increasing the chances of job disengagement among older nurses. In another longitudinal study, 24 availability of training and development practices was linked to the intention to remain with the organisation.
Older nurses expressed a need to be respected and recognised for their expertise and credited when they do a good job. Acknowledgement of work done was reported to have a major influence on workplace commitment. 19 Cohen advocated for a culture where older nurses are recognised and respected, and ‘the knowledge, experience and perspective of older nurses are appreciated’. 22
Various authors2,22 also wrote of the need to redesign jobs for older nurses or offer job rotation opportunities (Table 4). For example, older nurses usually have a greater amount of experience in clinical nursing. As such, they can take the role of consultants for nurses with lesser experience, mentors to help new nurses where they can offer experiential assistance, or as instructors for new nurses. 2
In a telephone interview with 15 managers with responsibility for nursing workforces, Leese et al. reported the implementation of other strategies such as career breaks (sabbaticals from six months up to five years with guaranteed return to the same or a similar post) and support for returners (training and development) and nurses who had dependents (carer leave of 5–7 days a year; provision of advisory services). 25 However, the study did not include older nurses themselves and hence perceived usefulness of the strategies were only from the point of view of managers.
In general, strategies, as outlined above, were narrated by respondents to surveys or authors themselves and perceived to be useful or effective. Except for the longitudinal study by Armstrong-Stassen and Schlosser, 21 the rest of the above-mentioned studies did not involve empirical testing to evaluate the effectiveness of such retention strategies.
Only one other empirical study was found through our literature review. The empirical study 26 evaluated the effectiveness of a caring-based programme (given dedicated time to reflect and focus on caring relationships with oneself, work colleagues as well as patients) among older nurses. It was reported that such strategies could improve work engagement and assist older nurses to remain in direct patient care.
Limitations
This review did not include articles published in non-English languages, which might have provided valuable information about nursing workforce from Asian cultures that are more relevant to our Singapore context. We also did not review grey literature, which might have provided more detailed or emerging insights.
Conclusion
Given the increase in demand for healthcare services, coupled with an ageing workforce, the retention of older nurses is extremely important in the local healthcare industry. This review has summarised key challenges that older nurses may face. In particular, the ageing process may render certain tasks less desirable and more challenging for the older nurses. However, these challenges can be overcome through better work practices, which pay attention to the needs of an older workforce. It is also important for nurse leaders and human resource practitioners to be familiar with factors associated with early retirement and retention, such that appropriate strategies can be implemented so that more nurses not only ‘can’ but also ‘want to’ work beyond 65.
Footnotes
Conflict of interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
