Abstract
This is a review on talus osteochondritis dissecans and talus osteochondral lesions. A majority of the osteochondral lesions are associated with trauma while the cause of pure osteochondritis dissecans is still much discussed with a possible cause being repetitive microtraumas associated with vascular disturbances causing subchondral bone necrosis and disability. Symptomatic nondisplaced osteochondral lesions can often be treated conservatively in children and adolescents while such treatment is less successful in adults. Surgical treatment is indicated when there is an unstable cartilage fragment. There are a large number of different operative technique options with no number one technique to be recommended. Most techniques have been presented in level II to IV studies with a low number of patients with short follow ups and few randomized comparisons exist. The actual situation in treating osteochondral lesions in the ankle is presented and discussed.
Introduction
Osteochondral lesions of the talus (OLT) are frequent after acute ankle trauma. A subset of osteochondral lesions of the talus is osteochondritis dissecans. A general problem regarding ankle OCD is that this entity is not clearly defined. In a lot of articles, the term used for the same lesion varied from osteochondral lesions (OCL), osteochondral fractures (OCF), flake fractures, or transtalar dome fractures, and so on. Other terms are such as acute or traumatic and chronic or non-traumatic OCD. In addition, there is no clear differentiation between juvenile osteochondritis dissecans (JOCD) and adult osteochondritis dissecans (AOCD).1-13
When describing treatment of OLT, OCD is also included as the treatment choices are more or less the same for both types of lesions. The majority of articles reporting on OLT subsequently include also OCD. However, the easiest is to use the term osteochondritis dissecans (OCD) when describing the most often seen nontraumatic lesions in children or adolescents and to use the term osteochondral fractures in patients with trauma, including both the cartilage and the subchondral bone most often seen in adults. 13
Epidemiology and Etiology
Incidence
Coltart 14 in 1951 was the first to report on the incidence of osteochondral talar lesions. Overlooking 25,000 fractures he found a frequency of 0.09% of osteochondral lesions, including OCD-cases. In a recent study, Kessler et al 15 reported an overall incidence of 4.6/100,000 for OCD-cases in children and adolescents between 6 and 19 years. The age dependent incidence ranged from zero for children aged 2 to 5 years, 1.1/100,000 in patients aged between 6 and 11 years. The highest incidence with 6.8/100,000 was shown in children and adolescents aged between 12 and 19 years. Furthermore, a multivariate logistic regression analysis exhibited in male patients aged between 12 and 19 years showed a 6.9 times increased risk for the development of an OCD lesion compared with females. In children and adolescents, 22.9% of the patients needed surgery. 16
The incidence of talar OLT lesions following an ankle distortion has been reported to be up to 6.5%. 17 Almost all these lesions were preceded by a trauma (sprain or fracture).1,2,17-22
Berndt and Harty 18 demonstrated the trauma cause experimentally already in 1951. Further analyses seem to be unreliable due to the differently used terms osteochondritis, osteochondral, talar dome, and transchondral fractures where sometimes it was a pure osteochondral trauma lesion and sometimes an OCD lesion.
Location
A few studies have shown that the majority of lesions (53%-58%).23-26 are located at the medial talar rim occurring in the middle third in the anterior-posterior direction. A minor percentage are seen at the lateral talar rim (total 34%-42%),23-25 occurring mostly (25.7%) in the middle third in the anterior-posterior direction. Only a small percentage is found in the central third of the talus. 25 The rate of coexisting talar and tibial lesions is up to 35%. 27
Symptomatic lesions are most often located in the mid-third of the lateral talar dome and to a lesser extent in the mid-third of the medial talar rim. 26 Only a few are found in the center of the talus. The authors speculate that these findings support the theory of a mechanical induction of OCD lesions at the talus.
Morphology
Recent morphological analyses using data obtained from high-resolution magnetic resonance imaging (MRI) 28 revealed that 2 out of 5 morphological criteria (malleolar width and length of the trochlear arc) were significantly different in idiopathic OCD and traumatic OLT-lesions when compared with healthy controls. 28 Another morphological investigation on predisposing factors for talar osteochondral lesions (OLT) using 3-dimensional computed tomography (CT) images 29 showed that the medial malleolar area and the medial malleolar volume was significantly smaller and that the anterior opening angle of the talus was significantly larger in 19 patients with medial OLT in comparison with 19 healthy controls. 29 In addition, an MRI analysis of patients who suffered from tibial shaft fractures showed in 37% concomitant occult talar lesions up to 12 months postoperatively. 30
Biomechanics
Biomechanical studies have shown that at the ankle joint forces occurring at heel rise during stance phase were found to be 3.9 to 5.0 times body weight.31,32
The average tibiotalar contact area has been estimated to be 4.4 cm2, SD 1.21. 33 Accordingly, the pressure during the stance phase can be calculated to be 650 N/cm2. During running this load may increase multiple times. 22
Furthermore, in a cadaver study mimicking either supination or pronation ankle sprains, Bruns and Rosenbach 34 were able to demonstrate that the contact areas moved from the center of the talus toward the medial rim in supination or toward the lateral rim in pronation. But this study was a static one without considering that the real load might be distinctly higher owing to the dynamics of the trauma with impulse loading.
An analysis of biomechanical characteristics of the cartilage layer in different areas in the ankle joint 35 shows that tibial cartilage is stiffer (1.19 MPa) than talar cartilage (1.06 MPa). The softest cartilage is found in the posterolateral (0.92 MPa) and in the posteromedial talus (0.92 MPa). The anterior and posterior regions of the lateral and medial sites of the tibia are found to be 18% to 37% stiffer than the corresponding sites of the talus.
Both, Simon
When mimicking osteochondral lesions in a cadaver study, it was found that the peak rim stress depends on the size of the defect. 38 As an example, an osteochondral autograft transplant (OAT) procedure could restore contact biomechanics at the talar rim. 39
Clinically, bone bruises could be seen in posttraumatic MRI at the medial talar border after anterior fibulotalar and fibulocalcanear ligament tears. Thus, these findings had been discussed as a probable precursor of a talar OLT. 40
Metabolic Influence
Bruns
Diagnostics
As for OLC/OCD at the knee joint or elbow joint44,45 symptoms of OCL/OCD lesions are not specific and often vague. Most of the patients report on a diffuse ankle pain, probably in combination with swelling or blocking. There are no typical clinical signs in any joint. Thus, the diagnostic procedure should include a plain x-ray examination of the ankle using the anterior-posterior and lateral view and probably the mortice view (20° inner rotation of the leg using a course of beam) as a first examination. But, for an advanced diagnosis CT scans or MRI scans are in use to visualize the lesion 3-dimensionally. There are advantages and disadvantages for all diagnostic procedures such as radiation dose for CT, but a good visualization of the bony part of the lesion. In cases without any or with minor changes in the x-rays, MRI might be better to show bone marrow probably exhibiting a bone marrow edema as an initial stage of the lesion. Furthermore, with MRI the status of the cartilage can be visualized.46-49 Some authors are using the technetium-99m methylene diphosphonate single photon emission CT (SPECT).50,51 This procedure combines this sensitivity with the superior anatomical detail of CT, enabling better localization of pathological uptake and evaluation of associated structural changes.
There are some comparative studies: Mintz
Verhagen
Yasui
Regarding the imaging techniques for follow-up examinations there are no clear recommendations. Imaging techniques such as radiographs, CT scans and MRI scans have been used inconsistently. Most often radiographs and CT scans have been used for follow-ups, and in a minor frequency MRIs have been used. 47
Treatment Options and Results
Scientifically there are almost no comparative prospectively randomized studies elaborating clear recommendations depending on the age of the patient and stage of the disease both regarding pure OCDs and osteochondral traumatic lesions. Most of those articles are level III or level IV studies. There are only a few level-I and level-II studies.57-62
Conservative Treatment
In initial stages with intact articular cartilage, it is thought that conservative treatment is indicated.1,3,6,7,9,10,22,63 Although there are no precise protocols for conservative strategies, it is generally accepted that such therapies should be the first choice, particularly in patients with JOCD.10,64,65
Conservative treatment includes10,64-66 the following:
Rest
Cast/brace immobilization
Restriction from weight bearing
Use of nonsteroidal anti-inflammatory drugs (NSAIDs)
Based on few published data, it would seem that conservative therapy in JOCD, adult OCD (AOCD), and OLT patients should be limited to a period of about 6 months with a tendency toward earlier surgical treatment in adult patients. In one study on JOCD, it was found that after 6 months only 16% of the patients’ lesions had completely healed. A further 6 percent, who still experienced some pain following immobilization, required surgery and 42% had to undergo surgery owing to unhealed lesions and pain. In contrast, 46% had no symptoms, but as could be seen in radiographs, had still persistent lesions. 10
Letts
However, from several studies it is obvious that clinical and radiographic results do not always correlate, meaning that even in symptomless patients, changes are still radiographically detectable.12,64-66
Surprisingly good results have been observed for so-called stage-V lesions. Such lesions exhibited subchondral cysts in 35 ankles of 34 patients. After an average of 38 months of conservative treatment, 9 JOCD patients exhibited a lower rate of excellent or good results (33%) compared with the adult patients (62%).
5
It was also observed that there was no correlation between size of the lesion and the clinical outcome and that lateral lesions did better than medial ones and that there was no significant development of osteoarthritis. Verhagen
Whether extracorporeal shockwave therapy (ESWT) can help in a conservative set-up is still under evaluation.
67
Others used intraoperative ESWT to improve healing after implantation of bone marrow aspirate concentrate (BMAC) or for postoperative pain relief after arthroscopic microfractures (MFX).
68
Regarding factors possibly predicting the result of conservative treatment in JOCD, Heyse
From the 2017 International Consensus Meeting on Cartilage Repair of the Ankle, the consensus for an optimal protocol for conservative management of an acute nondisplaced osteochondral lesion of the ankle is
Immobilization for 4 to 6 weeks with touchdown weightbearing.
NSAIDs could be used in cases of significant pain and swelling.
Medium strong evidence for the use an injection of a biological product in the form of concentrated bone marrow aspirate or platelet-rich plasma if there is no improvement in symptoms after 4 to 6 weeks. 70
Surgical Therapy
Debridement, Bone Marrow Stimulations (BMS), and BMS-Augmented AMIC Repair
In the late 20th century, several articles have been published on arthroscopic treatment of OCD/OLT with shaving and debridement of the defects and/or drilling and MFX. The results have mostly been good to excellent.2,6-8,12,13,20,21 In 3 systematic reviews, comparing different surgical procedures, it was shown that the highest average success rate of nonreconstructive techniques was reached by excision, curettage, and drilling (85%, 9 85%, 11 and 86% 25 ; followed by excision and curettage (78%, 9 77%, 11 and 78% 25 ). The lowest success rate was reported for excision only (38%, 9 54%, 11 and 38%. 25 On the basis of these findings, it was summarized that conservative treatment or surgical excision alone is not to be recommended for talar OCL/OCD.9,11,25
Furthermore, owing to great diversity in the articles and variability in treatment results, no definitive conclusions could be drawn.
Transchondral drilling is not without complications; anterograde trans-osseous drilling can initiate iatrogenic bone cysts and produces drill holes to the cartilage.
71
In the authors’ experience, the use of a hand-driven awl used in a retrograde manner can avoid transchondral drilling, drill heat and thus does not negatively affect the osseous tissue. Similar recommendations were made in a review article analyzing 29 studies about a combined therapy including arthroscopic debridement and MFX.
72
Results from 295 patients who had undergone this treatment were monitored and, in 80%, the results were either good or excellent. However, all 29 publications are level-IV studies describing several techniques, mostly applied arthroscopically, without differentiation of OCL from talar dome fractures or OCD. Goh
The main problem with drilling or any other perforation procedures of the subchondral bone (SCB) is that synovial fluid may penetrate into the SCB resulting in destruction and/or development of subchondral bone cysts owing to its osteolytic potential.22,74 This is in accordance with findings described for the etiopathology of SCB cysts.74-77
Furthermore, degradation of the SCB following MFX has been reported.
78
With an MRI-follow-up using a new SCB health score evaluating different criteria such as the amount of edema, subchondral cyst diameter, and qualitative and thickness changes in the SCB, Shimozono
Seow
A comparison of the arthroscopic LDFF procedure with arthroscopic BMS exhibited after one year no clinical differences. However, the authors found that the SCB plate was restored significantly superior after arthroscopic LDFF compared with arthroscopic BMS and suggested that LDFF leads to a lower rate of ankle osteoarthritis and thus a better long-term outcome. In contrast, it is well-known that BMS will results in a rate of ankle osteoarthritis in 33% to 34%. 82 However, many lesions are not able to be treated by LDFF procedures as the osteochondral fragments often are necrotic at time of surgery.
Zengerink
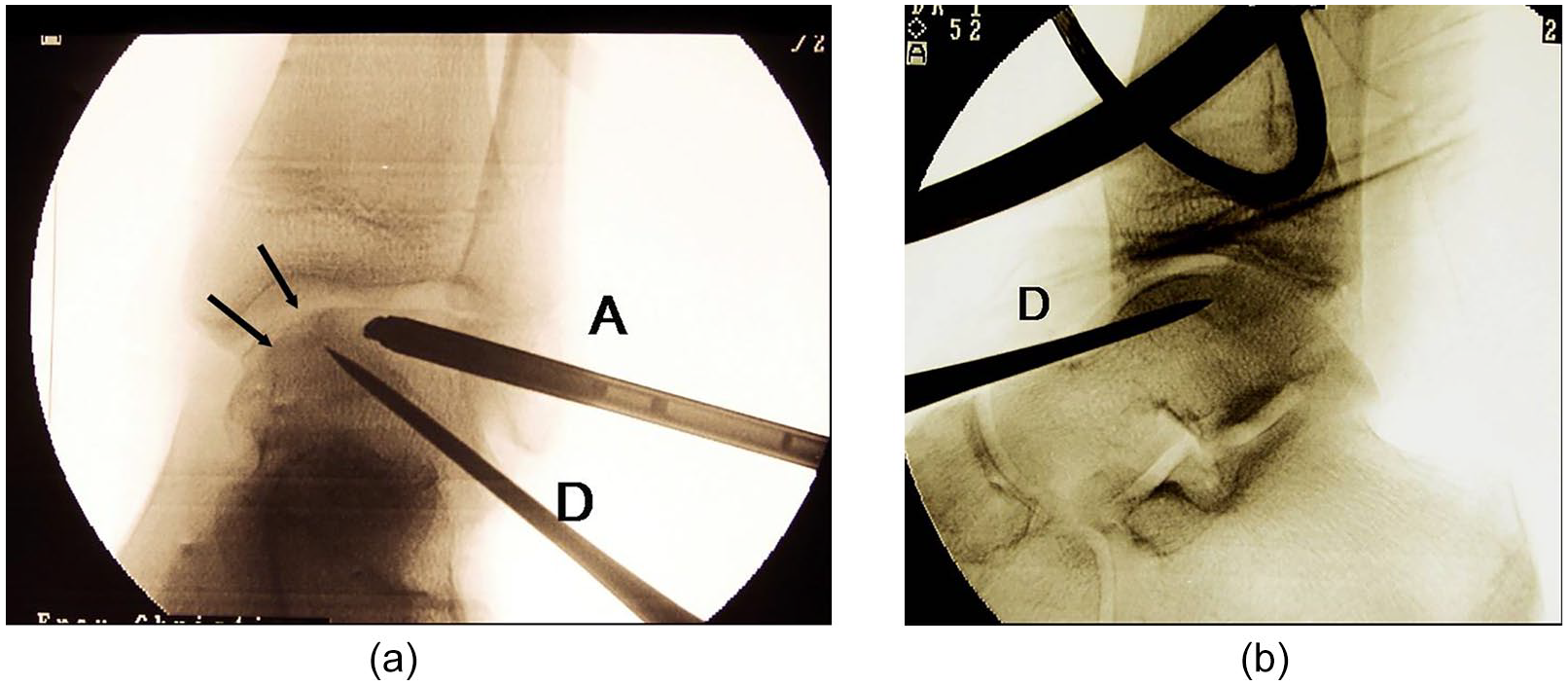
(
Evidence for Bone Marrow Stimulations
Zwingmann
In another study, the best overall success rate, independent of the stages but in correlation to the different surgical techniques was found to be 84% for transplantation procedures, 82% for fragment refixation, 76% for BMS/MFX, and 71% for only debridement. 11
In a study including 130 patients with OLT treated with arthroscopic debridement and drilling/MFX, Cuttica
Ramponi
Another systematic review BMS/MFX demonstrated once more the rather disappointing scientific situation. Yasui
In a most recent second systematic review on BMS, Toale
Based on this medium strong evidence and high international consensus, BMS can be considered for the surgical treatment of full-thickness chondral or osteochondral lesions that have failed conservative treatment in lesions <10 mm in diameter and <5 mm in depth. 93
Few reports on the time for return to sports exist but in 1 article an average return to play length of 15 ± 4 weeks in athletes treated with BMS has been reported. 94
More Complex OLT Repair Methods
Advanced cases such as stage IV or cystic lesions and those with severe damage to the cartilage are treated with more advanced surgical techniques such as osteoarticular transplants (OATS) ( Fig. 2a-d )/mosaicplasty or autologous chondrocyte implantation (ACI). In general, related to the 2017 consensus meeting, 93 defects larger than 10 mm in diameter and with a depth >5 mm are not suitable for BMS. Such lesions need a more direct filling at the time of surgery. The alternatives presented augment, in different ways, either as BMS with a porous scaffold inducing the repair with chondrogenic cells or a fill of the defect with an osteochondral full tissue. There is no evidence that there are different indications for those treatment alternatives but very large loss of bone needs osteochondral allografting.
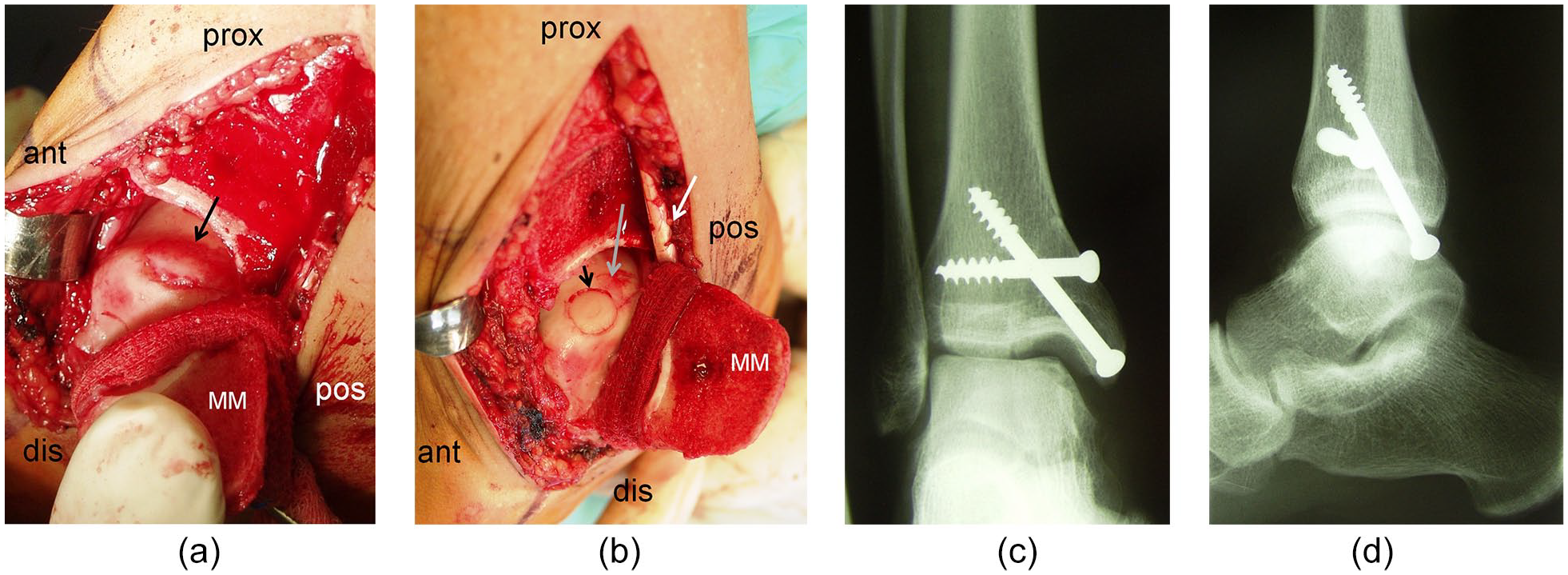
(
Autologous Chondrocyte Implantation (ACI)
There are several papers reporting good and excellent results for different generations of ACI in the treatment of OCL/OCD lesion.95-102 In all these level IV studies, there was a distinct and significant postoperative improvement detectable.
Recently, Erickson
With the third- and fourth-generation ACI, no lesion containment is needed. From the International Consensus Meeting in 2017, a high consensus and evidence was found that ACI can be considered in primary or revision procedures for large lesions greater than 1 cm2, with or without cysts, including shoulder lesions. 106 Normally, return to sports after ACI procedures in the knee is depending on type of sport and similar is for ACI for osteochondral ankle lesions with a mean return around 12 months postsurgery.
Osteo(chondral) Transplantation
Osteochondral Autograft Transplantation System (OATS) and Mosaicplasty
Several publications are reporting on OATS and/or mosaicplasty for the treatment of OLT or OCD in the talus. In some articles, both terms OATS and mosaicplasty are used synonymously. 107
However, there is an important technical difference between them: While with OATS using a technique with graft implantation in an overlapping manner filling up the defect completely instead in mosaicplasties, the osteochondral grafts are implanted side by side leaving clefts between them. These clefts allow the synovial fluid to penetrate into the SCB until fibrous tissue will have filled up the clefts with scar tissue ingrowing from the SCB. Thus, the osteolytic character of the synovial fluid may be harmful to the SCB including the transplanted grafts.22,75-77
Hangody
Baltzer and Arnold
115
achieved good and excellent results in almost all 43 patients including 22 patients with OCD lesions. Their results were depending on the size of the graft—the smaller the graft the better. Woelfle
Two of the most important biomechanical criteria for osteochondral reconstructive procedures seems to be restoration of the contact area and pressure distribution. Studies have shown that both mosaicplasty 108 and OATS could fulfill such criteria. 39
Park
A systematic review of 11 studies on 500 ankles with OCL treated with OAT 118 exhibited, at a mean 62.8 months’ follow-up, an excellent or good result in 87.4% of the patients. Thirty-one patients (6.2%) underwent reoperations and 5 ankles (1.0%) were regarded as failed. Donor site morbidity was observed in 18 patients (3.6%) at final follow-up. 118
A meta-analysis on donor site morbidity being a specific problem after OAT and mosaicplasty exhibited a donor site morbidity ranging from 6.7% to 10.8%. In larger groups (
The use of autologous transplants taken from the injured talus itself has, to our knowledge, been first reported in 2002.
120
The authors used transplants from the talus itself, thus avoiding the more invasive technique of harvesting grafts from the intact knee joint. A significant postoperative improvement was seen after 2 years in all 12 patients. This was confirmed by Kreuz
Regarding OAT/mosaicplasty, in rare cases where a lesion is located in the anterior third of the talus and an osteotomy is not necessary, it can be done arthroscopically. 123 However, this is technically demanding since the transplants have to be placed vertically and flush with the healthy surrounding cartilage.
The combination of autologous osteochondral transplants taken from the ipsilateral knee joint with cancellous allografts has been used in 15 patients suffering from OCL/OCD accompanied by SCB cysts >15 mm). 124 After 12 months, the VAS (visual analogue scale) score exhibited a distinct pain reduction and an increased AOFAS (American Orthopaedic Foot and Ankle Society) score. The radiolucent area of the cysts disappeared on the plain radiographs in all cases. 124
The return to sports has been found to be rather high. Nguyen
Bone Grafts Alone Without Cartilage Layer
A transplantation procedure using only cortical-cancellous bone grafts without any cartilage layer resulted in 46% failures (6 of 13 patients). Five of the 7 remaining patients were still suffering from mild to moderate pain at a mean follow-up of 52 months.
128
Struckmann
There exist acceptable evidence and high consensus that cancellous bone grafting is the preferred method of treatment in cases of subchondral bone marrow lesions of the ankle. There is no evidence for or against bone void substitutes. 129 Bone grafting can be utilized in lesions with large subchondral cysts, as well as in cases with large and/or deep lesions with or without subchondral cysts ( Fig. 3 ). For cystic lesions, bulk bone transplantation (e.g., osteochondral autograft/allograft) should be considered. 127 The rate of return to preinjury level of sports was 79% for patients after bone marrow stimulation, 72% for patients after autograft transplantation, and 69% for patients after autologous chondrocyte implantation.
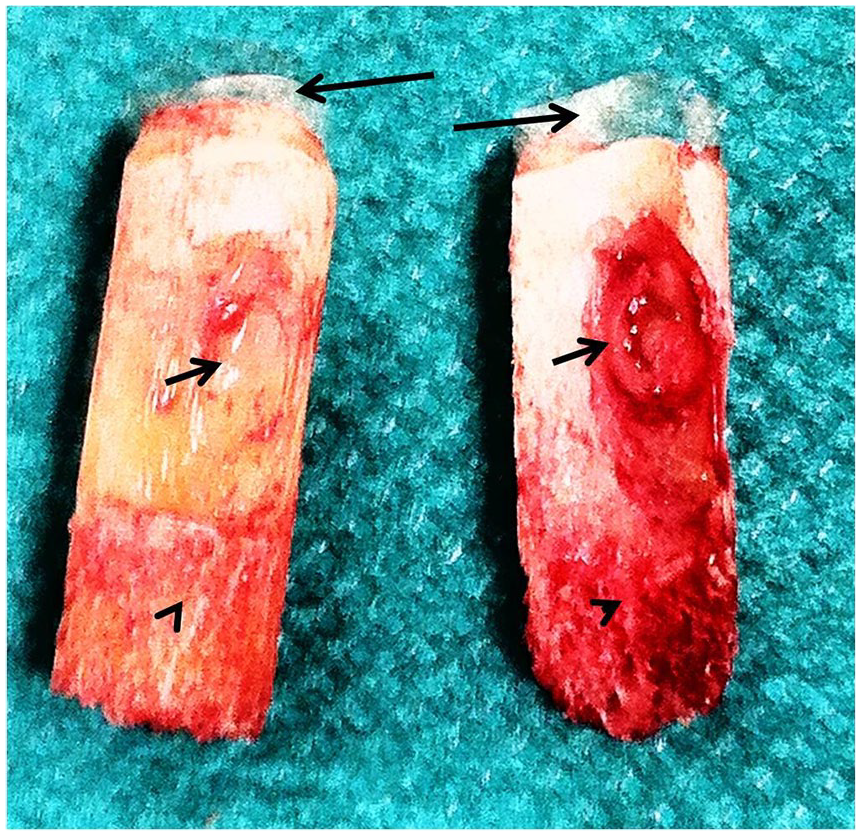
Osteochondral explants of a cystic osteochondritis dissecans (OCD) lesion of the talus (long black arrows = damaged cartilage on the top of the explants; short black arrows = the cystic subchondral lesion, arrowheads = subchondral normal bone).
Osteochondral Allografts
Osteochondral allografts for repair of OCL/OCD have been used since many years.130-132 But, as for as other repair techniques the level of evidence and the methodological quality is low.131,132 Almost all reports are level IV or even level V. In principle, the problem is immunogenicity. 132 While chondrocytes embedded in extracellular matrix were believed to be immunologically privileged the bony part is even more at risk, particularly without any immunological matching and without immunosuppression.132,133
There are different kinds of allografts, such as
bipolar allografts
bulk transplants
small osteochondral allografts.
There is no clear definition of bulk/structural transplants versus small allografts and their size, whereas bipolar allografts seem to be not appropriate for treatment of OCL/OCD-lesions. Mulholland and Gross
129
were the first to present a paper on osteochondral allografts used for talar osteochondral lesions. A longer follow-up was presented in 2001 by Gross
In a retrospective study, El-Rashidy
Adams
In contrast to above statements, Orr
Van Tienderen
Comparison of allografts with OAT has been reported twice: In a prospective randomized level II study on 20 patients who had received OAT were compared with 20 patients treated with allografts.
142
At final follow-up, no patient who had received OAT developed ankle degenerative changes or knee complications while one of the allograft patients developed symptoms of asymptomatic arthritis. The mean Foot and Ankle Ability Measure score of the 16 patients (exclusion of 4 patients) who had received osteochondral allograft plugs could be followed up increased from 55.2 preoperatively to 80.7 at the time of final follow-up. The postoperative score was lower than after OAT, but statistically not significant (
Consensus and some evidence exist that bulk osteochondral allograft transplant can be considered in uncontained/shoulder lesions or lesions that cannot be addressed with an osteochondral autograft. There is strong evidence and consensus for the use of fresh, nonfrozen allografts in the ankle. No special reports on the return to sport after ankle osteochondral allografts have so far been published. 144
Extracellular Matrix Allografts and Particulated Juvenile Cartilage Allografts
Extracellular matrix cartilage allografts (ECMA) and particulate juvenile cartilage allografts (PJCA) are relatively new biologics that may improve the quality of cartilage repair. ECMA are developed from allogenic cartilage and contain extracellular matrix that is native to articular cartilage, including key components such as type II collagen, proteoglycans, and cartilaginous growth factors. 145
PJCA consist of pieces of fresh juvenile cartilage allografts containing vital cells within their native extracellular matrix. Fibrin glue is used to secure PJCA inside the lesion. Several experimental studies on PJCA have already been published but only a couple reporting on its clinical application. 146
ECMA
In contrast to PJCA, there exist several preclinical studies on ECMA147-151) but, to our knowledge, only 1 clinical report 152 exists. This prospective study evaluated the intermediate-term results of operatively treated primary OCL with a size of 1.5 cm2 or smaller with arthroscopic excision, MFX combined with ECM in a level III study. 151 After a maximal follow-up of 19 months, ECMA resulted in a high rate of improvement in ankle function and pain.
PJCA
Saltzman
Up to now there are at least 5 additional articles on this particular allogenic transplantation procedure and 1 further retrospective study.153-158
A comparative study on PJCA in combination with BMAC versus patients treated with MFX only has been performed by Karnovsky
Dekker
In another study, 46 patients with critical-size OCLs (≥6 mm widest diameter) were arthroscopically treated with a mixture of PJCA and BMAC.
156
Factors associated with outcomes were lesion size and hypertrophy. An increasing lesion size was associated with a decreased clinical score and hypertrophy was accompanied with a higher postoperative pain score. In twenty-two patients who received a postoperative MRI, the reparative tissue still exhibited only fibrocartilage. This is in accordance with results reported by Karnovsky
Another analysis on PJCA has most recently been given by Heida
A second systematic review on PJCA has been published by Aldawsari
Biologics: Scaffolds, Platelet-Rich Plasma (PRP), and Bone Marrow Aspirate Concentrate (BMAC)
Osteochondral scaffolds
Apart from the aforementioned AMIC procedure, there are many scaffolds with different biochemical characteristics in use. In 2017, Shimozono
In another systematic review on the clinical evidence of articles reporting on the AMIC procedure in different joints Gao
The use of biomimetic collagen scaffolds has been reported in 2 articles: Christensen
McGoldrick
The addition of a scaffold to a bone marrow stimulation (e.g., matrix-augmented bone marrow stimulation) can be considered in the following cases:
Primary and revision cases with lesions >1 cm2
Cases in which a 1-step procedure is to be used
In cases where an additional bone grafting may be needed. 106
Platelet-rich plasma
PRP is an autologous product of concentrated blood plasma that contains at least twice of the normal platelet concentration in blood and contains of several growth factors and cytokines166-169 and is produced with a bedside procedure concentrating PRP from autologous blood samples for individual use. Thus, the concentration is differing from individual to individual. PRP contains different growth-factors such as transforming growth factor-β1 (TGF-β1), fibroblast growth factor (FGF), epidermal growth factor (EGF), platelet-derived growth factor (PDGF), and vascular endothelial growth factor (VEGF).166-170 These factors are capable for the proliferation of chondrocytes in a porcine model 171 and human PRP stimulates migration and chondrogenic proliferation of subchondral progenitor cells. 172
In addition, PRP has also been used in orthopedic surgery with the purpose to improving the healing process in different tissues such as tendons, bone, and cartilage or musculoskeletal disorders either as a single agent or as an adjunct in combination with BMAC.173-180
Regarding the role of PRP in cartilage repair of talar OCL the diversity of clinical studies is confusing and similar to other reports on talar cartilage repair: Most of these studies are level IV studies with a limited scientific value: In 2015, Guney
For treatment of larger subchondral cystic OCL/OCD lesions (so-called Hepple-V-lesions), Gu
In a recent systematic review, Yausep
The International Consensus Group did not make any analysis on the use of PRP for different repairs of ankle osteochondral lesions and there is no consensus or strong evidence that an augmentation of PRP to different repair procedures will speed up return to play. 106
BMAC
Friedenstein
BMAC has been proven for cartilage repair in different combinations with scaffolds and/or PRP.
In 2009, Giannini
Four-year clinical results had been reported from the same institution in 2013.
186
Forty-nine patients exhibited a significant improvement 24 months postoperatively followed by a significant decrease in the AOFAS between 24 and 48 months with a direct correlation between clinical and MRI results followed by mid-term results.
186
Buda
A combination of OAT and BMAC has been analyzed by Kennedy and Murawski 188 in 72 patients treated. After a mean follow-up time of 28.02 months, the authors had found a significant improvement in the FAOS-score as well as in the SF-20 scores. But 3 patients exhibited a donor-site morbidity. Unfortunately, the authors did not compare these patients with those treated with OAT only to evaluate the influence of BMAC on OATS. A comparison of BMAC (40 patients) versus ACI (40 patients) 105 exhibited similar results in both groups without any statistically significant differences at 48 months. But the authors preferred bone marrow–derived cells over ACI for the single step procedure, owing the patients’ comfort and lower costs.
A case-control study reported by Hanon
Most recently, Vannini
In a prospective study, Murphy
The use of BMAC in juvenile patients suffering from JOCD has first been studied by Pagliazzi
The International Consensus Group did not make any analysis on the use of BMAC for different ankle osteochondral lesions and there is not yet any consensus or strong evidence that a BMAC procedure for ankle lesions will speed up return to play.
Mini-Metallic Implants
A relatively new method is implantation of metallic substitutes to treat OCD-lesions in failed previous surgeries. Van Bergen
Currently, there are at least 4 mid-term follow-up studies on implantation of hemi-caps as a salvage procedure after failed previous interventions in the ankle joint available on 10 to 38 patients.196-199 Three groups reported on a rather large number of revision surgeries with a revision rate up to 70% 196 and/or high rate of unsatisfied or only moderately satisfied patients (8 of 12, 66%). 199 Only 2 groups with rather large cohorts of 31 patients 198 and 38 patients 197 reported on good clinical results, but a large rate of additional surgeries, 42% 198 and 55.3%. 197 Nevertheless, 77% patients regained their sports activities postoperatively after 4.1 months (SD, ±3). 197
In contrast, 2 groups stated that “metal resurfacing might not be considered a definitely valid alternative for treatment of OCDs after failed previous surgery” 199 and “that implantation of the Hemi CAP® as a salvage procedure for OCDs of the talus is challenging and does not consistently lead to good clinical results.” 196
An alternative mini-metal implant might be the Episealer (Episurf AB, Stockholm, Sweden). It is a custom-made patient-specific resurfacing implant developed for local cartilage repair first for the knee in clinical use. For the ankle joint now CE-marked implants exist for the ankle but still not any clinical results. It aims to treat patients suffering from pain and reduced mobility due to focal cartilage lesions and underlying bone damage. 200
Long-Term Follow-ups
Long-term results with a minimum of 5 years follow-up up to 20 years including palliative and reconstructive procedures are numerous.20,63,89,95,96,108,112,201-209
There is only 1 article on exclusively conservative treatment in a reasonable number of 22 patients with 24 OCL out of initially 48 that have been reexamined after 14 years (range, 11-20 years). 201 Regarding pain 75% reported pain reduction and 13% each an unchanged or increased pain, 73% of the patients showed no progression of ankle osteoarthritis and 27% progression by one grade. Another article described a rate of good results (42%) after conservative treatment of the initial OCD stages and, later, surgical removal of the lesions (33%). They stated that the longer the symptoms persisted, the worse the results. 9
Comparison of long-term results after surgical therapies is difficult owing to the different used procedures and the lack of studies comparing different surgical strategies prospectively. In older publications authors report only on excision and drilling.20,63,89,204-206 After excision and drilling most of the reports with long-term results mentioned an excellent or good outcome is achieved in between 65% and 88% of the patients after removal of the lesion plus a BMS.20,63,89,204-206
In 2013 and 2016 there were 2 article207,208 reporting exclusively on arthroscopic debridement and BMS. Van Bergen
They found that in 76% of 93 reexamined patients continued participating in sports at final follow-up but did not reach the level before surgery.
More recently, there are more long-term results on reconstructive procedures such as ACL/MACI95,96,202 or OATS/mosaicplasty108,112 available. Giannini
Regarding autologous osteochondral transplantation either OATS or mosaicplasty there are three reports with rather different results. While Hangody
In contrast, Valderrabano
Comorbidities
Little is known about comorbidities of talar OLTs. Since ankle instability with supination and/or pronation sprain is supposed to be an important etiological factor in talar OCD lesions, in principle, it should be considered to treat any ankle instability as well. Lee
Discussion and Conclusion
Treatment of an OLT (OCD/OCL) depends mainly on the symptoms, the location of the lesion, and the imaging evaluation. Patients with medial or lateral lesions and radiographic findings that reveal no detached osteochondral fragment may be treated conservatively. Conservative treatment in these patients includes immobilization of the limb in a brace and reduced weightbearing for up to 3 months. Patients with lesions and signs of a partially or completely detached fragment even if still “
However, based on the available literature, one may summarize the following treatment alternatives without any ranking:
Conservative treatment could be the choice for small, stable osteochondral lesions
Operative treatment when conservative treatment has failed
A healthy osteochondral fragment may be refixated either retro- or antegrade
A necrotic osteochondral fragment is excised and for small defects BMS may be used
For larger and deeper lesions more complex surgeries are used where the treatment choice is up to the surgeon’s preference
Medium sized and deep lesions may be treated with osteochondral autografts, BMAC, AMIC, particulated auto- or allografts, or ACI
Large sized and deep lesions with bone grafts, osteochondral allografts
Failed biological repairs could be candidates for mini-metal implants
Augmentation of graft alternatives may be done with PRP.
In summary, the scientific situation is still poor as more than 90% of the articles published on talar OCL are level III and IV studies. Thus, regarding the scientific value and consequently on the impact on the clinical application of any particular decision is arbitrary and not scientifically based. Furthermore, the evaluation of preoperative status and the postoperative results per se is under debate. Servlet
Footnotes
Acknowledgments and Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
