Abstract
Background:
Cervical spinal cord injury (CSCI) often results in respiratory muscle weakness, requiring prolonged mechanical ventilation and tracheostomy. However, the frequency and timing of ventilator-weaning milestones after acute hospitalization are not well described. This study assessed the rates and timing of daytime ventilator weaning, liberation from invasive ventilator support, and decannulation among adults with CSCI managed under a standardized weaning protocol at a rehabilitation center, and the associations of weaning milestones with discharge disposition.
Methods:
We retrospectively analyzed data from adults with CSCI admitted to the University of Utah Craig H. Neilsen Rehabilitation Hospital between 2015 and 2022. All subjects required continuous mechanical ventilation via tracheostomy upon admission and underwent a standardized ventilator weaning protocol. We tracked the time to reach key ventilator-weaning milestones—daytime wean, liberation from invasive mechanical ventilation, and decannulation—and categorized discharge destinations based on required respiratory support intensity. Predictors of milestone achievement and discharge outcomes were assessed using Fine-Gray competing-risk and proportional odds logistic regression models.
Results:
Among 39 subjects, 76% were weaned from daytime ventilator support (median day 20), 62% were liberated from invasive ventilatory support (median day 23), and 48% were decannulated (median day 36) by discharge. Subjects with lower-level injuries (C5–C8) were more likely to achieve further weaning and decannulation compared with those with high-level injuries (C1–C4) (odds ratio [OR] 5.54 [1.51–20.38]). Increasing age was associated with discharge to more intensive care settings (OR 0.68 per decade [0.48–0.95]). Decannulated subjects had higher odds of being discharged home (OR 22.84 [2.84–183.57]). No significant differences in weaning status based on discharge disposition were observed.
Conclusions:
Most subjects with CSCI initially on continuous mechanical ventilation achieved partial or full ventilatory independence during rehabilitation, although these milestones were often reached several weeks into their stay.
This is a visual representation of the abstract.
Keywords
Introduction
Half of spinal cord injuries (SCI) occur in the cervical spine (CSCI), 1 often causing weakness of the respiratory muscles and impaired ventilatory function. 2 Consequently, many persons with CSCI require chronic ventilatory support. Tracheostomies are performed in up to 75% of individuals with CSCI.3,4 Many clinicians perceive that patients with CSCI at the C4 level or above cannot be liberated from mechanical ventilation because of the anatomic innervation of the diaphragm arising from C3, C4, and C5 nerve roots.5–11 This belief may contribute to delayed or absent weaning attempts. However, persistent ventilator dependence among patients with SCI has been associated with lower quality of life, higher mortality rate, and more frequent hospitalizations. 12 Thus, identifying additional individuals with CSCI who could be liberated from mechanical ventilatory support might improve outcomes.
Prior studies examining guided weaning and predictors of success report ranges of 45% to 85%.11,13,14 A meta-analysis evaluating weaning outcomes among individuals with SCI in both ICU and in-patient rehabilitation settings reported an 85% rate of liberation from mechanical ventilation in in-patient rehab and decannulation rates ranging from 25% to 100%. 11 Despite these encouraging rates, subject categorization by injury level was not possible, limiting insight into outcomes specifically for those with CSCI. Although existing reports have evaluated overall ventilator liberation rates among individuals with SCI, these reports have lacked granular descriptions of the weaning time course, baseline covariates, and ultimate disposition. The absence of this information limits the ability of clinicians to provide guidance to patients or benchmark their program’s performance. Thus, we sought to describe liberation from ventilation rates, time to weaning milestones, and discharge disposition among adults with CSCI at a single center with standardized weaning protocols.
QUICK LOOK
Current knowledge
Individuals with cervical spinal cord injury (CSCI) frequently require tracheostomy and long-term mechanical ventilation because of respiratory muscle weakness. Successful ventilator liberation and tracheostomy decannulation are possible, especially in structured in-patient rehabilitation settings.
What this paper contributes to our knowledge
In this single-center retrospective study of adults with CSCI admitted to in-patient rehabilitation on continuous mechanical ventilation, 74% weaned from daytime support, 59% achieved liberation from invasive ventilation, and 46% were decannulated. Subjects with lower cervical injuries (C5–C8) had significantly higher odds of liberating and decannulation than those with higher-level injuries. Decannulation was strongly associated with discharge to home, whereas older age predicted discharge to more resource-intensive care. These findings highlight the potential for ventilator liberation, even among individuals with high-level CSCI.
Methods
This was a health record–based retrospective cohort study of adults with SCI who were admitted to the University of Utah Rehabilitation Unit, now known as the University of Utah Neilsen Rehabilitation Hospital, between 2015 and 2020. The study was exempted by the University of Utah Institutional Review Board (IRB #00153003).
Screening for inclusion was performed by a single reviewer (C.F.), who reviewed documentation of both pre-rehabilitation and rehabilitation hospital courses. Potentially eligible patients were identified by a health records search for any mention of “trach,” “tracheostomy,” “ventilator,” “mechanical ventilation,” “spinal cord injury,” “SCI,” or usage of the mechanical ventilator documentation flowsheet. Individuals were eligible for inclusion if they were at least 18 years old at the time of injury, had a diagnosis of CSCI, had a tracheostomy, and were receiving continuous mechanical ventilation at the time of admission. Patients who had completed weaning milestones before admission (eg, daytime or nighttime weaning) were excluded.
Extraction of data elements for included subjects was performed in duplicate (C.F. and either P.C., W.T., or J.B.). Respiratory data and weaning information were obtained from respiratory flowsheets, which were documented during the subject’s admission. Owing to the wide range of injury levels and American Spinal Injury Association scores, injury levels were divided into high (C1–C4) versus low (C5–C8) and motor complete versus motor incomplete.
Care for all individuals with CSCI who require mechanical ventilatory support, including the study subjects, was standardized in the following manner. Physical therapy, occupational therapy, and/or speech therapy were delivered 3 h daily for 5 days out of the week or 15 h spread over 7 days. Management of ventilators was coordinated between physical medicine and rehab physicians, a pulmonologist, and respiratory therapists. Upon admission to rehabilitation, subjects were placed on pressure control intermittent mandatory ventilation (PC-IMV), and their ability to generate adequate tidal volumes (8–12 mL/kg of ideal body weight) was assessed by reducing the set breathing frequency and evaluated for the capacity to maintain adequate tidal volumes and subject comfort. If subjects were unable to maintain adequate tidal volumes with pressure support ventilation, a breathing frequency was added to maintain 10–12 breaths/min with tidal volumes equaling 8–12 mL/kg of ideal body weight. Subjects were then weaned to pressure support based on comfort and tidal volumes. Following the transition to pressure support, subjects were removed from the ventilator and supported with a tracheostomy mask. If subjects tolerated the tracheostomy mask, they underwent ventilator-free time with Passy Muir valve, followed by capping trials. Daily ventilator-free time was adjusted according to subjects’ comfort, tidal volumes, and oxygenation. An arterial blood gas (ABG) was obtained on admission and upon signs of clinical changes to assist in ventilatory weaning. Decannulation was considered if the tracheostomy tube remained capped for 24 h with an ABG demonstrating adequate ventilation. The secretion management protocol includes routine mechanical insufflation-exsufflation and suctioning. Mechanical in-exsufflation was performed 4 times per day as needed by respiratory therapy and trained caregivers or family members. Respiratory comorbidities such as asthma, COPD, and pulmonary embolism were treated with the standard of care during the weaning process with the assistance of a pulmonologist.
For the purpose of the article, we use the following definitions. Weaning refers to the gradual reduction of the intensity and invasiveness of respiratory support. “Daytime wean” refers to the absence of invasive ventilation via tracheostomy during daytime hours (≈07:00–19:00). “Liberation from invasive mechanical ventilation” refers to going the entire (24 h) day without invasive ventilation. Decannulation refers to tracheostomy tube removal without reinsertion.
Three sets of outcomes were considered. First, ventilator-weaning outcomes were operationalized as an ordinal variable from most respiratory support to least: “Fully Ventilator Dependent,” “Daytime Wean,” “Liberated from Invasive Mechanical Ventilation,” and “Decannulated” before subjects were discharged from rehabilitation. Noninvasive ventilation (such as NIV via the oral or nasal route) was permitted and assessed separately. The day on which the milestone first occurred was extracted from respiratory therapy notes. Similarly, discharge location was treated as an ordinal variable ordered from most resource-intensive to least: long-term acute care hospital (LTAC), skilled nursing facility, home with home health, or home without home health services (home). Last, death during follow-up was identified via notification of death in the subjects’ medical records.
Proportional odds logistic regression was used to model independent associations between age, higher versus lower injury level, complete versus partial injury severity, and the ordinal weaning outcome at discharge. A second proportional odds logistic regression with the same predictors modeled discharge location. These predictors were chosen based on hypothesized clinical importance without stepwise selection.
The time to first occurrence of each weaning milestone was quantified using subdistribution hazards regression (Fine-Gray) with death or discharge counted as competing events, 15 adjusting for the same covariates. Rehabilitation admission was taken as time 0. We report subdistribution hazard ratios (SHR), with SHR values > 1 indicating a higher cumulative probability of achieving each weaning milestone by a given timepoint. Thus, for all models, odds ratios (OR) and hazard ratios above 1 represent a higher chance of a more desirable outcome (a higher likelihood of more independence, a higher likelihood of less resource-intensive disposition, and a higher cumulative probability of achieving each weaning milestone, respectively).
Kaplan–Meier survival analyses with log-rank tests were used to assess for unadjusted associations between discharge location and risk of death and for discharge ventilator-weaning status and risk of death.
No imputation was performed, as the missing data rate was <5% for all utilized variables. Statistical analyses were performed using Stata version 18 (StataCorp, College Station, Texas). Code for statistical analyses is available at https://github.com/reblocke/NRH-SCI-Vent.
Results
Of 237 reviewed records mentioning one of the key words, 39 subjects met the inclusion criteria and were analyzed (Fig. 1). Median age was 43 (interquartile range [IQR] 28–59) years, 77% were male, and subjects were admitted to in-patient rehabilitation at a median of 17 (IQR 13–25) days after their injury. Median days from injury to initial intubation was 0 (IQR 0–4), and tracheostomy occurred a median of 7 days (IQR 4–9) after intubation. C4 (n = 15), C5 (n = 9), and AIS A (n = 28) injuries were most common (Table 1). Median stay in in-patient rehabilitation was 64 days (IQR 56–76). No subjects died during their rehabilitation stay.
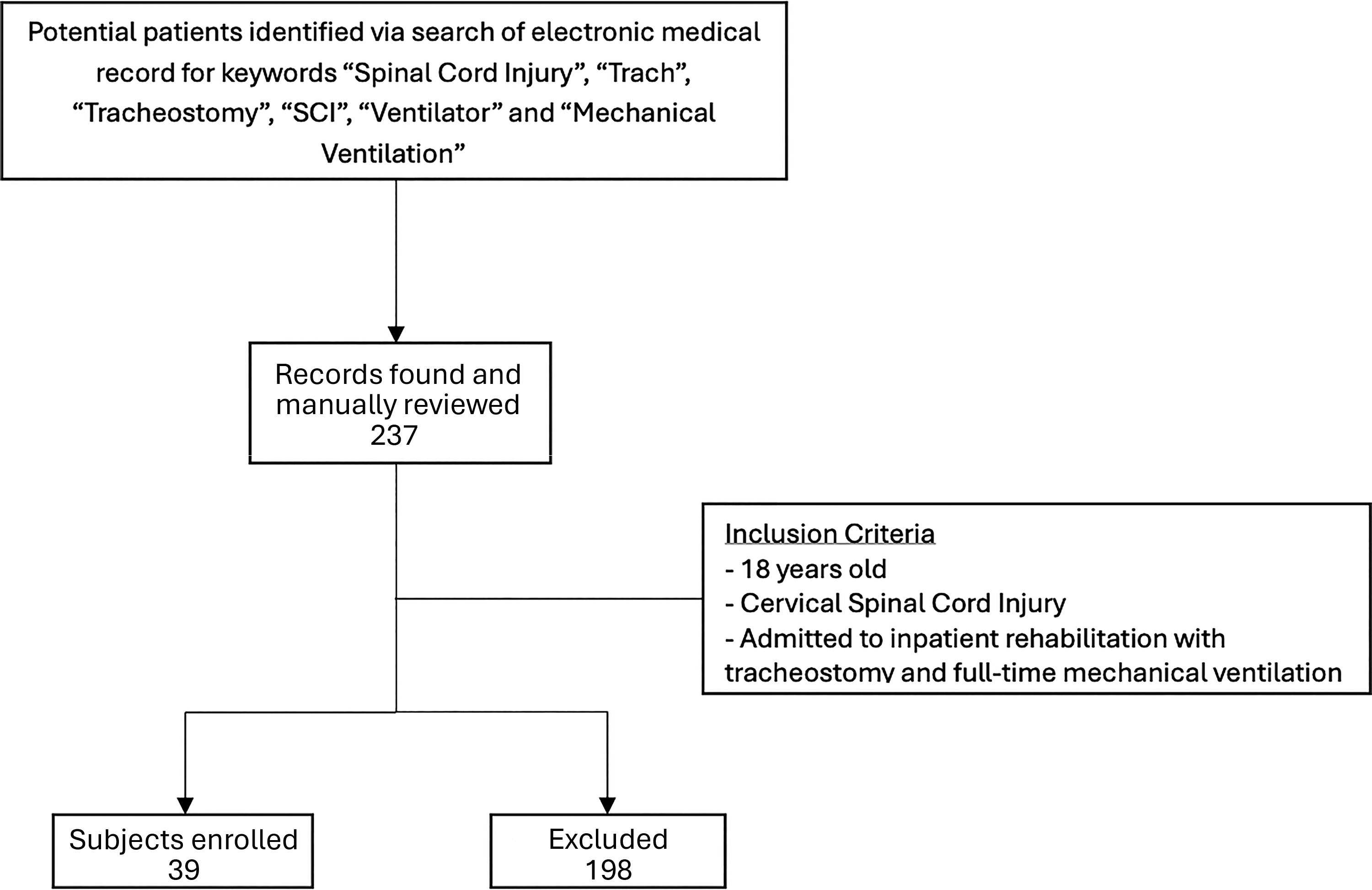
Flow chart. Of 237 medical record hits (2015–2022), 198 records were excluded through manual review (inadequate injury level, no continuous mechanical ventilation, or prior weaning). The final study cohort included 39 adult subjects with a cervical spinal cord injury who received continuous mechanical ventilation via tracheostomy at admission to rehabilitation.
Preadmission course and baseline variables
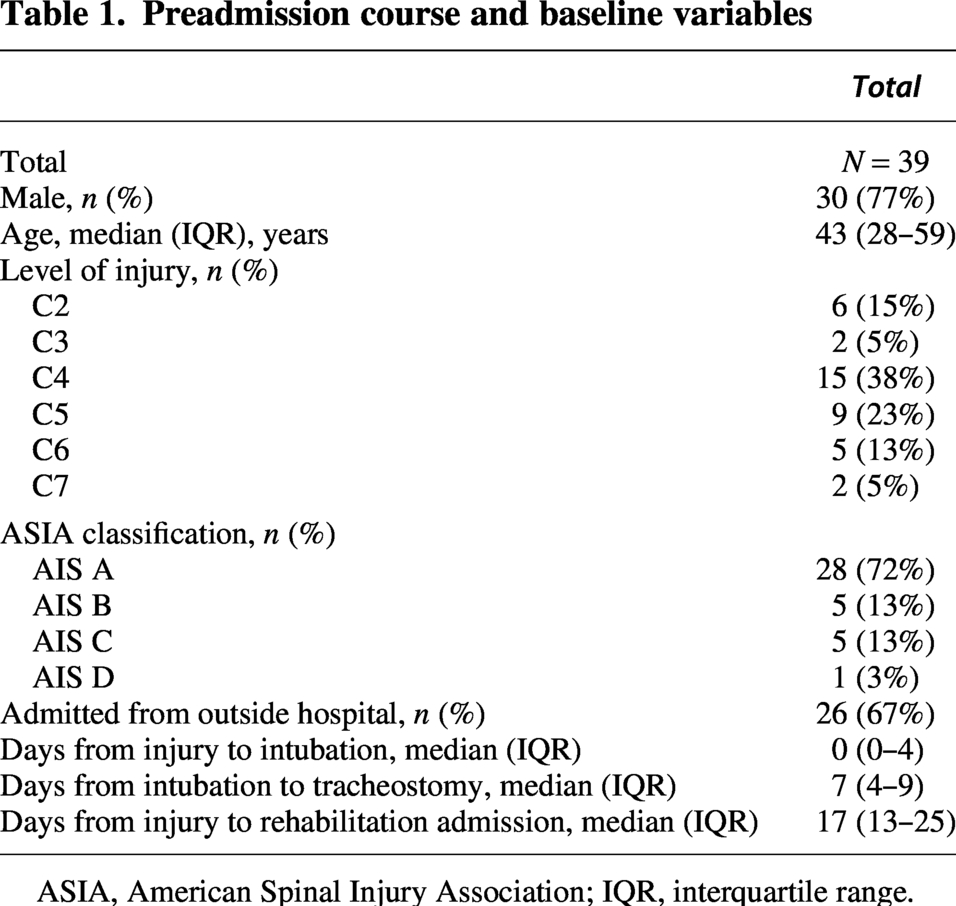
ASIA, American Spinal Injury Association; IQR, interquartile range.
By the time of discharge from in-patient rehabilitation, 74% (n = 29) of subjects who were continuously ventilated upon rehabilitation admission were weaned from daytime ventilator support (at median rehabilitation day 20), 59% (n = 23) were liberated from invasive ventilator support (median day 23), and 46% (n = 18) were decannulated (median day 36; Fig. 2). In the subdistribution hazards regression, subjects with low SCI had a higher cumulative incidence of weaning during the day (SHR 3.21, 95% CI 1.43–7.15, P = .004), liberation from invasive ventilation (SHR 2.31, 95% CI 1.04–5.12, P = .04), and decannulation (SHR 3.18, 95% CI 1.23–8.22, P = .02) by discharge (Supplementary Figure S1). Low (compared with high) spinal cord injury was associated with a 5.54 (1.51–20.4, P = .01) higher odds of more ventilatory independence at discharge (Fig. 3). Other predictors (age and complete vs partial motor impairment) were not independent predictors of weaning milestone achievement.
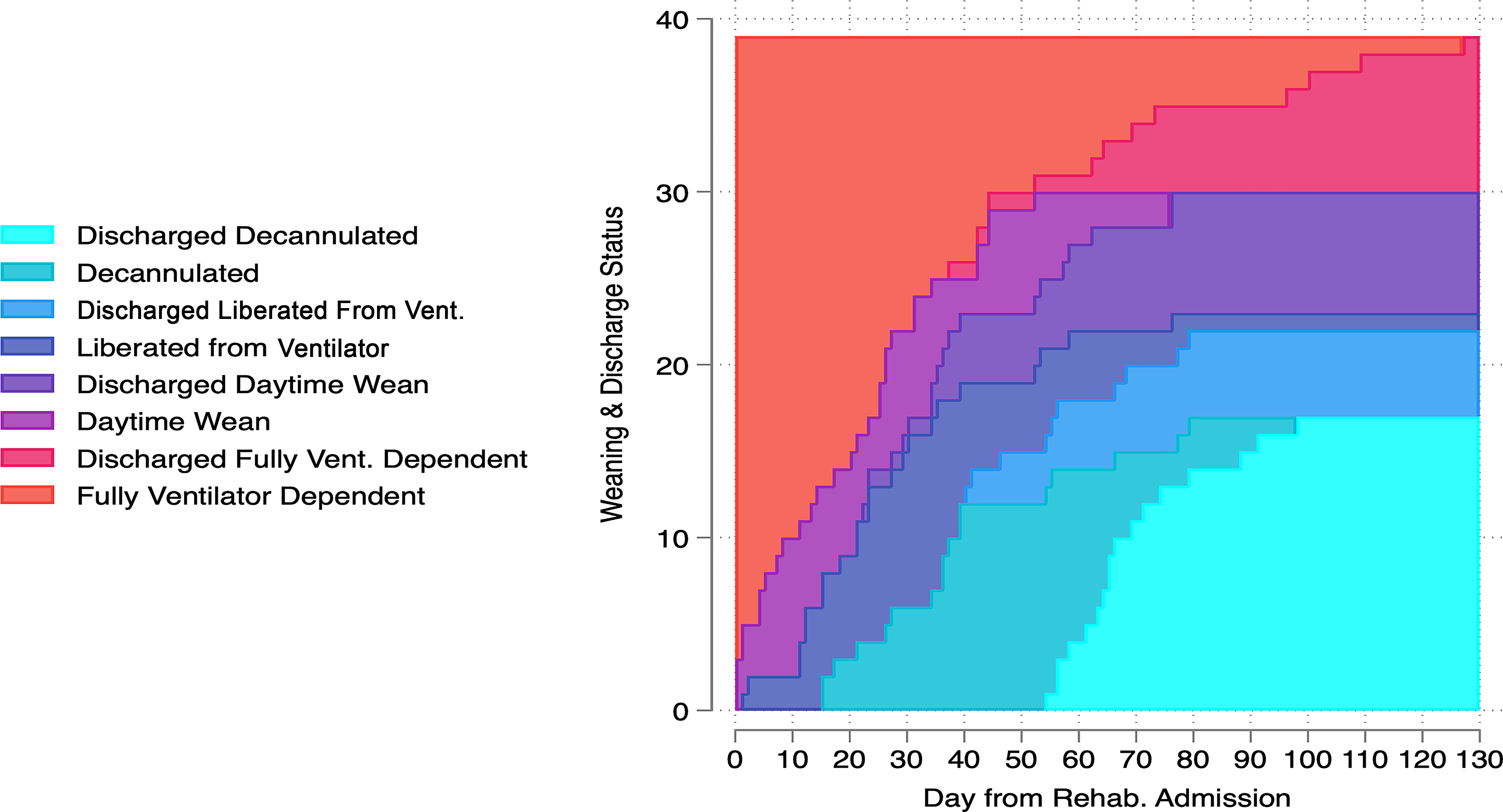
Time course of ventilator-weaning milestones. Stacked panel plot illustrating the daily proportion of cohort members occupying 1 of 8 mutually exclusive categories of discharge status and first ventilator-weaning milestone achievement: In-patient: 24-h ventilator-dependent, daytime-weaned, liberated from invasive mechanical ventilation, or decannulated; Discharged: 24-h ventilator-dependent, daytime-weaned, liberated from invasive mechanical ventilation, or decannulated. Subjects transition from the “in-patient” to “discharged” categories on their rehabilitation discharge date, and they transition between ventilator milestone categories on the first day that each milestone is achieved.
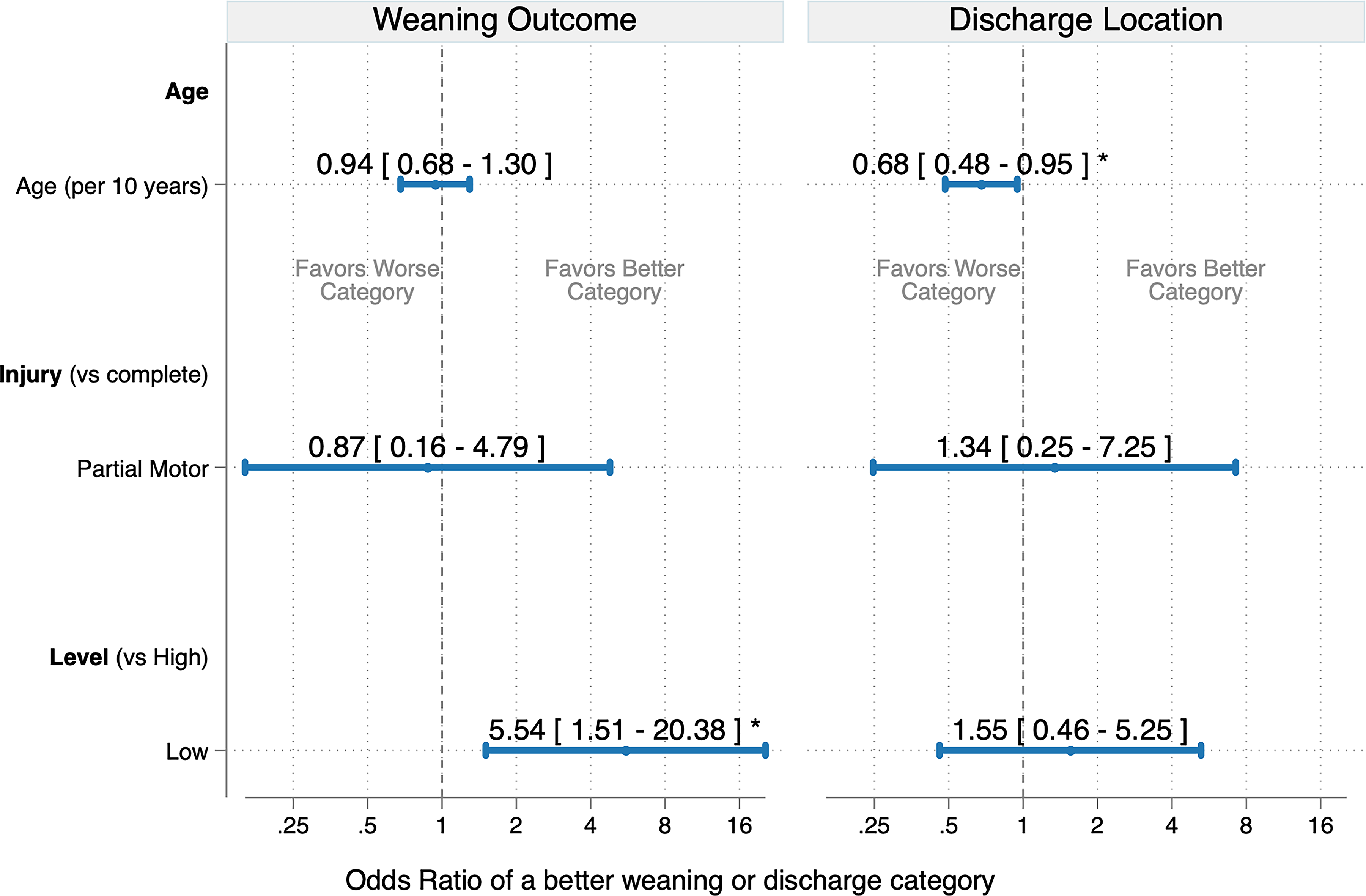
Predictors of weaning milestone achievement and discharge destination. Proportional odds ratios (OR) and 95% confidence intervals show the independent association of age (per decade), injury level (high = C4 or above, low = C5 and below), and motor completeness with ventilator weaning (left) and discharge destination (right). Weaning categories ascend from 24-h ventilator dependence, weaned during day, liberated from invasive mechanical ventilation, to decannulated. Discharge categories ascend from long-term acute care facility, skilled nursing facility, home with home health, to home independently. OR > 1 indicate a greater odds of a more desirable outcome (more weaning milestones achieved, less resource-intensive discharge). *P < .05.
Independent discharge to home occurred in 18% (n = 7) of subjects, 18% (n = 7) discharged home with home health, 46% (n = 18) discharged to a skilled nursing facility, and 18% (n = 7) discharged to an LTAC facility. Low (compared with high) spinal cord injury was not independently associated with discharge level of care (OR 1.55 for less resource-intensive discharge category, 0.46–5.25, P = .48), but older subjects tended to discharge to more resource-intensive care settings (OR 0.68 per decade, 0.48–.95, P = .02). Among the subgroup with high cervical injuries (C1–4, n = 23), 47% (n = 11) were able to liberate from invasive ventilatory support, 30% (n = 7) were decannulated, and 26% (n = 6) were discharged to home (with or without home health).
After accounting for age, decannulation was independently associated with a more independent home discharge with proportional OR 22.84 (2.84–183.57, P = .003) as compared with 24-h ventilator dependence. Other weaning milestones were not associated with higher odds of independent home discharge (Supplementary Figure S2).
When evaluating mortality, 10 of 39 subjects (26%) died at a median time of 382 days from rehabilitation admission. Survivors had a median follow-up of 1,101 days. Discharge location predicted time-to-mortality (log-rank P = .038) but discharge ventilator support did not (log-rank P = .37; Supplementary Figure S3).
Discussion
In this retrospective cohort of subjects with CSCI who required continuous mechanical ventilation via tracheostomy upon admission to in-patient rehabilitation, we found that a majority (74%) were able to achieve at least partial ventilatory independence. Nearly two-thirds achieved liberation from invasive ventilation, and almost half were decannulated by discharge from rehabilitation. Notably, even among those with high-level CSCI (C1–C4), we observed significant weaning potential: Half were fully weaned, and one-third were decannulated. These findings challenge common perceptions that patients with high-level CSCI are “unweanable” and reinforce the importance of not prematurely concluding that ventilator dependence is permanent.5–11
We evaluated to see if early SCI classifications, level, and completeness could have been inaccurate because of confounding factors such as inexperience from outside providers performing exams, subject factors such as sedation, and inadequate subject participation. We found that 62% of SCI classifications did not change with our exam. The subjects that were reclassified to a higher or lower level did not have a significant impact on their ability to wean, although they are a small subset of the sample, which could limit analysis. Importantly, many subjects achieved weaning milestones after prolonged rehabilitation stays, often around or beyond the third week. This underscores the need for patience in weaning efforts and cautions against using early weaning failures—such as ICU outcomes or initial ventilator dependence at admission—as predictors of final ventilator status. Indeed, our findings suggest that early inability to wean does not preclude eventual success, particularly when patients are managed under a consistent and progressive weaning protocol. 7
Decannulation was strongly associated with discharge to home settings. However, weaning status itself was not significantly associated with discharge location in unadjusted analyses, suggesting that nonclinical factors (eg, social support, insurance, geography) may also heavily influence discharge disposition. Even after controlling for weaning milestones, older age predicted discharge to more resource-intensive settings such as skilled nursing facility or LTAC, perhaps reflecting overall frailty.
Our results suggest that rehabilitation protocols should anticipate and accommodate prolonged and systematic attempts at weaning, particularly in patients with high-level injuries, and that discharge planning should not be based solely on early weaning outcomes. 8 The variability in ventilator liberation success across institutions reported in prior studies may in part reflect differences in how long patients are supported during rehabilitation and how aggressively weaning is pursued postacute care.
Our small sample size at a single in-patient rehabilitation center may limit generalizability and limit the ability to adjust for multiple potential confounders affecting weaning and discharge outcomes. Additionally, the retrospective design prevented accounting for factors not routinely recorded in medical records. For example, we are limited in our ability to assess the degree of adherence to weaning protocols, as this information was not reliably extractable from the chart review. Although our chart review process involved reviewing collected data for accuracy because of the retrospective nature of our study, we were unable to verify initial charting accuracy. Owing to inconsistencies in documentation, we were unable to reliably ascertain initiation of noninvasive ventilation following decannulation. Last, factors influencing which patients are admitted to in-patient rehabilitation may vary between health systems and thus may limit generalizability.
Future research should aim to standardize an evidence-based approach to ventilator weaning and tracheostomy decannulation. Additional efforts are needed to evaluate the long-term outcomes of individuals who successfully wean following extended in-patient rehabilitation, including rates of hospitalization, respiratory complications, and survival. Furthermore, interventions aimed at standardizing weaning practices and optimizing discharge planning could improve outcomes and reduce biases in care allocation.
Conclusions
This single-center retrospective study demonstrates that a high percentage of CSCI subjects who required continuous mechanical ventilation upon admission to in-patient rehabilitation were ultimately weaned, including many with high cervical injuries. Importantly, successful liberation from mechanical ventilation often occurred after extended rehabilitation, and prior weaning failures did not reliably predict final outcomes. These findings highlight the need for ongoing, protocol-driven weaning efforts and caution against premature assumptions about a patient’s potential for ventilator liberation. Discharge decisions and care planning should be informed by this potential, not early weaning status alone. Our results support using these data to guide families and clinicians toward more informed, optimistic, and individualized treatment planning for individuals with severe CSCI.
Footnotes
Author Disclosure Statement
Dr. Fenger has no relationships to disclose. Dr. Locke discloses an equity interest in Mountain Biometrics, Inc. (a startup applying time series machine learning on wearable biomedical sensor data, unrelated to the current article). Dr. Barker has no relationships to disclose. Dr. Tang has no relationships to disclose. Dr. Creveling has no relationships to disclose. Ms. Foster-Palmer has no relationships to disclose. Dr. Flis has no relationships to disclose. Dr. Park has no relationships to disclose. Dr. Rosenbluth has no relationships to disclose. Dr. Brown discloses consulting fees from Breas Medical and Baxter.
Funding Information
This research was supported by the National Institutes of Health under Ruth L. Kirschstein National Research Service Award 5T32HL105321 from the NIH, the American Thoracic Society ASPIRE Fellowship, and the Intermountain Foundation, awarded to Dr. Locke.
