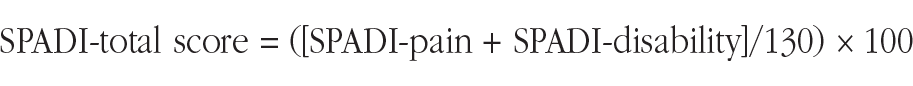Abstract
Background:
Although exercise interventions are recommended in the management of subacromial pain syndrome (SPS), there is a lack of data regarding the exercises focusing on the principal biomechanical deficiencies that cause symptoms.
Hypothesis:
Utilizing progressive scapula retraction exercises (SRE) and glenohumeral rotation exercises (GRE) in the scapula stabilization program may lead to more reduction in symptoms and greater acromiohumeral distance (AHD) values.
Study Design:
A double-blind, randomized controlled trial.
Level of Evidence:
Level 2.
Methods:
A total of 33 patients were assigned randomly to either SRE or SRE+GRE. Both groups received a 12-week supervised rehabilitation program, including manual therapy and exercises (stretching and progressive scapula stabilization exercises). In addition, the SRE+GRE group performed GRE exercises at gradual elevation angles. From 12 to 24 weeks, patients performed exercise programs less frequently (3 times per week). Disability (shoulder pain and disability index [SPADI]), AHD (at 5 active abduction angles), pain intensity (visual analogue scale [VAS]), and patient satisfaction were recorded at baseline, 12 weeks, and 24 weeks. A total of 16 healthy individuals were recruited as a control group to compare AHD values. Data were analyzed using mixed model analyses of variance.
Results:
A statistically significant group-by-time interaction was found for AHD values (F4,92 = 6.38; P = 0.001), a significant group-by-time interaction for SPADI-disability (F1,33 = 5.148; P = 0.01), SPADI-total (F1,32 = 4.172; P = 0.03), and for pain during activity (F2,62 = 3.204; P = 0.05). However, no significant group-by-time interaction for SPADI-pain (F1,33 = 0.533; P = 0.48), for pain at rest (F1,31 < 0.001; P = 0.99), and at night (F1,32 = 2.166; P = 0.15). Yet, a significant time effect was observed.
Conclusion:
Progressive SRE and GRE in the scapula stabilization program lessens symptoms and improves AHD values in patients with SPS. Moreover, this program could preserve outcomes and further increase AHD when applied less frequently.
Clinical Relevance:
Utilizing SRE and GRE in the scapula stabilization program at gradual shoulder abduction angles provides better rehabilitation outcomes.
Subacromial pain syndrome (SPS) is a common cause of shoulder pain and dysfunction.14,36 The condition results from soft tissue compression within the subacromial space when the arm is elevated.25,36 The lack of coordination or alterations in the activation patterns of the scapulothoracic and glenohumeral muscles may lead to abnormal subacromial space narrowing in patients with SPS while performing shoulder activities.4,25,26,33 Specifically, this theory is affected by 2 main biomechanical factors. First, a changed force-couple relationship between periscapular muscles could cause the scapula to be less upwardly rotated, posteriorly tilted, and more internally rotated and a decreased acromial elevation.4,25,34 Second, a decreased rotator cuff coactivation could contribute to excessive superior humeral migration.25,26 In light of the deficits mentioned above, preventing abnormal subacromial space narrowing could be considered an important rehabilitation goal for SPS and should be focused on.
Rehabilitation of SPS requires a multimodal approach, and exercises are a fundamental part of rehabilitation regimens.1,4,14,15,17,23,24,28,29,31,33,40 Scapula stabilization exercises have yielded favorable results on symptoms in recent studies; however, those exercises’ effect on acromiohumeral distance (AHD)–which is used to estimate subacromial space width–is still limited.7,15,17,22,24,30,31,40 Therefore, exercises targeting the principal deficiency could be an option to provide better rehabilitation outcomes.23,29,31 When considering the dynamic nature of the subacromial space, tailoring scapula stabilization and glenohumeral rotational exercises (GRE) at gradual elevation angles may be a replication of the daily living shoulder activities. It might help to retrain movement control while performing shoulder activities, thereby leading to improved functionality and greater AHD values. Thus, the program could minimize reinjury risk, and the patient could safely return to daily living activities.
To date, the efficacy of scapula retraction exercises (SRE) with GRE at gradual shoulder positions during the scapula stabilization program has never been investigated in patients with SPS. Therefore, the aim of this study was two fold. First, we aimed to investigate the effect of SRE with or without GRE at gradual shoulder elevation angles in the scapula stabilization program on symptoms. Second, we aimed to examine the AHD values between the patients with SPS and healthy controls at 5 shoulder abduction positions and identify whether the patients with SPS demonstrated a decreased AHD. We hypothesized that utilizing progressive SRE with GRE in the scapula stabilization program would lead to more functional improvement and pain reduction. We further hypothesized that a decreased AHD at varying shoulder abduction angles would be observed in patients with SPS at baseline. However, utilizing SRE and GRE would increase AHD at all shoulder positions.
Methods
Study Design and Randomization
This double-blind, randomized controlled trial was conducted with concealed allocation and blinding. The study protocol was approved by Hacettepe University Institutional Review Board (KA18-0018) and was registered prospectively at the www.ClinicalTrials.gov website (NCT03494192). Written and informed participant consent was obtained, and CONSORT statements were followed.
Participants were recruited at the Faculty of Physical Therapy and Rehabilitation, Hacettepe University, Ankara, for a 6-month duration. Potential candidates were diagnosed by an orthopaedic surgeon. AHD measurements were obtained by the same radiologist. Baseline outcome assessments were recorded by an experienced therapist. The assessors remained the same throughout the study and were blind to group allocation. Patients were also blind to group allocations; they knew that they were given an intervention but did not know the differences between them. After baseline assessment, patients were allocated randomly to 2 experimental groups (scapula retraction exercise group [SRE] or scapula retraction + glenohumeral rotational exercise group [SRE+GRE]). According to the 1:1 distribution randomization algorithm, a statistician generated a computer-based randomization sequence placed in sequentially numbered, opaque, sealed envelopes stored in a locked box. All patients were treated by the same therapist.
Participants
A total of 33 patients were included. Eligibility criteria were as follows: 18 to 45 years of age (Neer Stage I and II), primary complaint of anterolateral shoulder pain lasting at least 6 weeks, a painful arc in active flexion or abduction, positive Neer Sign or Hawkin’s Kennedy test, a pain when resisting humeral external rotation (ER) or abduction, not receiving any nonsteroidal anti-inflammatory drugs, or any shoulder treatment (including physical therapy and corticosteroid injection). Exclusion criteria were as follows: history of any shoulder, cervical, or thoracic trauma (or surgery) and type-III acromion. In addition, 16 healthy participants who were screened using the provocation test by the orthopaedic surgeon (age, hand-dominancy, and sex-matched) were included as a control group (CG) for AHD normative data.
Interventions
Patients received up to 20 supervised rehabilitation sessions over a 12-week period (at a frequency of twice a week for the first 8 weeks, and once a week from the 8 to 12 weeks). After 12 weeks, patients proceeded to a reduced exercise program until 6 months.
The rehabilitation program consisted of manual therapy (applied by a therapist) and supervised exercise programs. Manual therapy consisted of soft tissue mobilizations (ie, posterior shoulder complex, long head of the biceps brachii, and anterolateral shoulder region) and joint mobilizations (ie, glenohumeral and acromioclavicular joint) to enhance shoulder arthrokinematics and reduce symptoms.13,28,37 The exercise program is described in Table A1 (available in the online version of this article).1,23,28,40 Scapula stabilization exercises were performed by coactivating the core musculature to achieve more periscapular muscular activity. 5 We determined the proper elastic band resistance before exercise administration using Borg CR10 scale. 27 Elastic band resistance was assessed every week. The previous load was maintained if the patients could not perform a greater load. The exercise progression was checked with weekly sessions (proceeding to the next intensity level), and exercises were reviewed and corrected if needed. When proper control of the exercises was achieved with supervision, the exercises were advised as home exercises. Patients were instructed to perform the exercises in front of a mirror to check their postural alignment and prevent undesired movements. Patients were given an exercise brochure and a self-check list to enhance compliance.
The exercise program included the same exercises for each group as well as the same progression. To retrain appropriate control of movement during shoulder elevation, SRE progressed through 5 phases. Phases were graded according to resistance level applied on the shoulder and shoulder elevation angles. For instance, in phase 1, patients performed 10 repetitions of SRE in a standing position (with the arm at 0° of abduction and the elbow at 90° of flexion) using an elastic band. Once patients could perform all repetitions without pain and reach adequate movement control, they progressed to the next phase. In phase 2, they performed 15 repetitions with the arm at 0° of abduction and 10 repetitions with the arm at 30° of shoulder abduction. In phases 3-5, patients were instructed to continue the same progression with the shoulder at 45°, 60°, and 90° of shoulder abduction.
The distinction of the exercises for the SRE+GRE group was the inclusion of the gradual glenohumeral ER and internal rotational exercises, and bilateral ER with SRE. Patients followed the same progression phases as described above for GRE. Patients were instructed to perform the GRE with the coactivation of the core and periscapular musculatures.
When patients completed the 12 weeks, they were asked to perform their exercise program (according to group allocation) until 6 months (Table 2, available online). During this period, the therapist made biweekly phone-call appointments to ask about patients’ symptoms and whether they performed their exercises.
Outcome Measures
Outcomes were recorded at baseline, 12 weeks, and 6 months. The primary outcome was the shoulder pain and disability index (SPADI) for disability status, and the secondary outcomes were the visual analogue scale (VAS) for pain severity, AHD measurements (0°, 30°, 45°, 60°, and 90° of shoulder abduction) and patient satisfaction level. In addition, demographic characteristics of the participants (ie, age, sex, symptom duration, and dominant shoulder) were recorded.
Disability status was assessed using the SPADI designed to measure shoulder-specific disability status. 43 The questionnaire is scored on a 100-point scale, where 0 represents “no disabilities” and 100 represents “extreme disabilities.” 43 The SPADI contains 13 items that assess mainly 2 domains: a 5-item subscale that measures pain severity (SPADI-Pain) and an 8-item subscale (SPADI-Disability) that measures disability. 43 SPADI with 10 points change is defined as the minimal clinically important difference (MCID). 32 The total score (SPADI-Total) was calculated as follows:
Pain severity (at rest, during shoulder activity, and at night) was measured using a 100-mm VAS that consisted of a 100-mm straight line with end-points defining pain intensity. 11 Patients were asked to mark the pain level that corresponds to their pain intensity on the line between “0 = no pain” and “100 = the worst pain imaginable” (MCID = 14 mm). 38
AHD measurements were obtained from the symptomatic shoulders of the patients and dominant shoulders of the CG. AHD was measured using real-time ultrasonography (US) equipment (Siemens Acuson S2000, Siemens Medical Systems), with a 6.5 to 13 MHz linear transducer. Measurements were taken at 0°, 30°, 45°, 60°, and 90° of shoulder abduction in the coronal plane. AHD was defined as the shortest linear distance between the head of the humerus and the inferior edge of the acromion (in millimeters). To standardize positioning, participants stood upright with their feet positioned shoulder-width apart and elbows flexed at 90° with the thumb pointing upwards. The US transducer was placed along the lateral aspect of the acromion, in line with the longitudinal axis of the humerus to visualize the shortest linear distance between the humerus and the acromion. 9 First, we measured the AHD at 0° of shoulder abduction in the coronal plane. Participants then moved the shoulder to 30°, 45°, 60°, and 90° of active shoulder abduction, and we recorded the AHD at each shoulder position. Three consecutive real-time US images were obtained for each arm position, and the mean value was used for data analysis. We used a standard goniometer and a wooden bar to measure and monitor the degrees of abduction (Figure 1). In addition, we calculated the intrarater between-day reliability of the AHD measurements. Testing was repeated on 2 separate occasions (7 days apart) at each shoulder position. The mean of these measurements was used to determine the reliability of the radiologist.
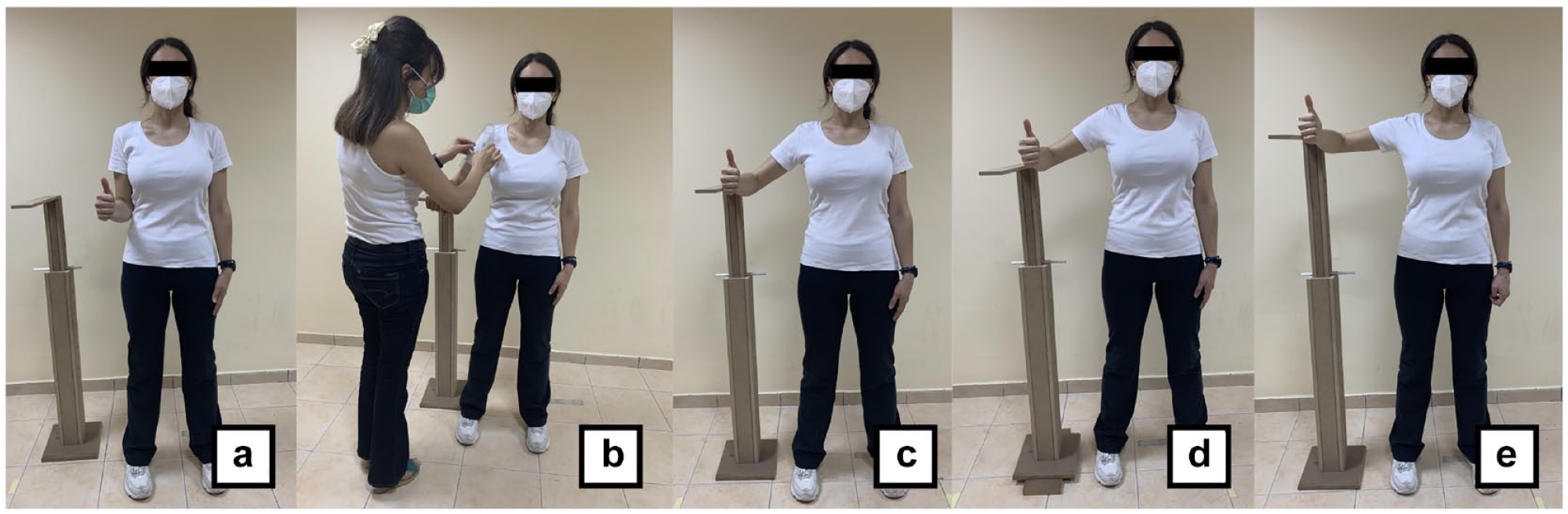
Participant positionings at 5 shoulder abduction angles during AHD measurements. (a) At 0° of shoulder abduction. (b) At 30° of shoulder abduction. (c) At 45° of shoulder abduction. (d) At 60° of shoulder abduction. (e) At 90° of shoulder abduction. AHD, acromiohumeral distance.
Patient satisfaction was evaluated by using the single assessment numeric evaluation rating, which is determined by the patient’s response to the following question: How would you rate your shoulder today as a percentage of normal (0% to 100% scale with 100% being normal). 39 Patients were asked to respond to the question considering their shoulder condition throughout the rehabilitation program. Patient satisfaction was assessed 2 times (at 12 weeks and at 6 months).
Sample Size Calculation
The sample size was calculated using the G*Power for Mac (Version 3.1.9.6; University of Dusseldorf) to detect the smallest significant difference in disability status. The sample size was estimated as follows: (1) the MCID of 10-points based on the SPADI (SD = 7.4), (2) significance level of 5%, (3) power of 80%, (4) a 15% drop-out.32,44 Finally, the required sample size was 16 patients per group.32,44
Statistical Analyses
Statistical analyses were conducted with SPSS (Version 22 for Mac; SPSS Inc.). The Kolmogorov-Smirnov test was used to assess the normality and homogeneity of the variance. One-way analysis of variance (ANOVA) was used to compare demographic characteristics and mean values of the pain intensity and SPADI at baseline. Independent samples t test was used to compare symptom duration and patient satisfaction. Then, a 2-way ANOVA with a mix-design (group [SRE group and SRE+GRE group] × time [baseline, 12 weeks, and 6 months]) was used the investigate the effectiveness of SRE with or without GRE on SPADI and VAS. Lastly, a 3-way ANOVA with mix-design (group [SRE group, SRE+GRE group, and CG] × time [baseline, 12 weeks, and 6 months] × shoulder position [0°, 30°, 45°, 60°, and 90° of shoulder abduction]) was used to evaluate the effectiveness of the rehabilitation programs on AHD. When a significant interaction term was present, a post hoc Bonferroni test was performed. The significance level was set at 0.05.
As with the AHD measurements, intraclass correlation coefficients (ICC2,3) with corresponding 95% CI were used to compare the average of 2 measures from each time interval. 41 The error of AHD measurement was calculated using the standard error of measurement (SEM) and minimal detectable change (MDC) with 95% CIs (MDC95%): SEM = (SD × √1 - ICC), MDC95% = SEM × 1.96 × √2. 6
Results
A total of 58 potential candidates were assessed for eligibility between August 2018 and February 2021; 24 patients who did not meet the eligibility criteria were excluded. The flow diagram of the participants is presented in Figure 2. All groups showed similar demographic characteristics (P > 0.05; Table 1) and mean values of the pain intensity and SPADI scores at baseline (P > 0.05; Table 2). According to the self-check diary, the exercise adherence rate was excellent (92.5%) and did not differ between groups.
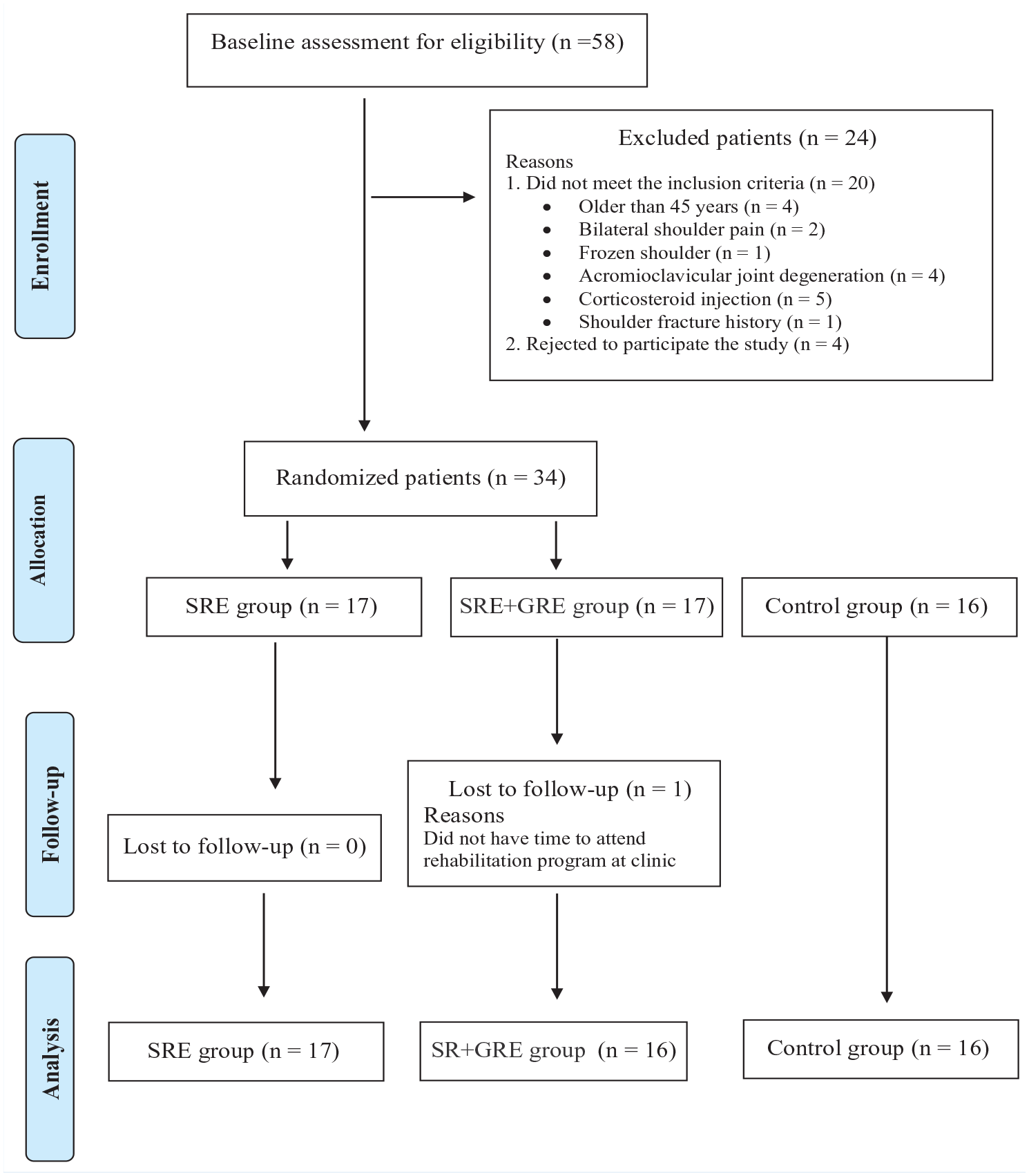
CONSORT flowchart of participants. CONSORT, consolidated standards of reporting trials; SRE, scapula retraction exercise group; SRE+GRE, scapula retraction + glenohumeral rotational exercise group.
Demographic characteristics of the participants at baseline a
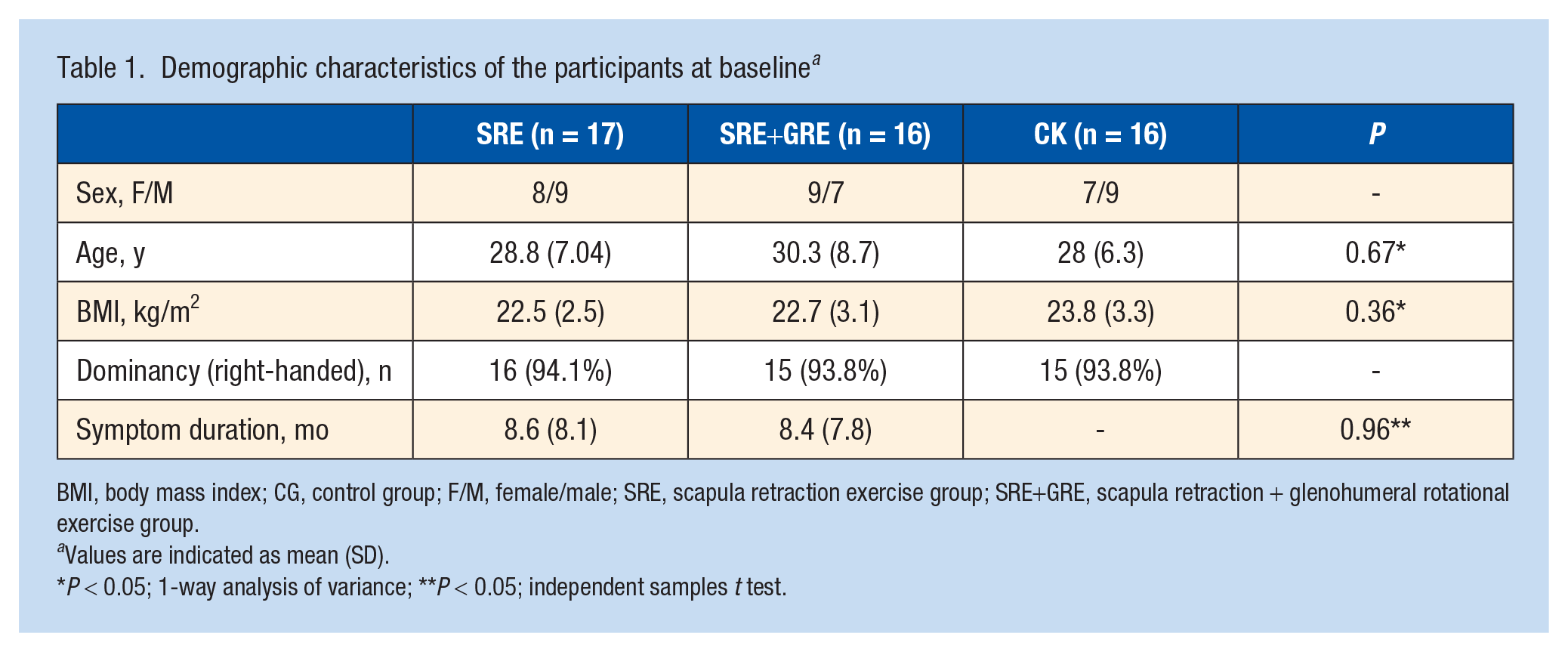
BMI, body mass index; CG, control group; F/M, female/male; SRE, scapula retraction exercise group; SRE+GRE, scapula retraction + glenohumeral rotational exercise group.
Values are indicated as mean (SD).
P < 0.05; 1-way analysis of variance; **P < 0.05; independent samples t test.
Mean values of the SPADI and pain intensity according to VAS (including within-group changes) and mean differences of the SPADI and VAS with 95% CIs between groups at baseline, 12 weeks, and 6 months a
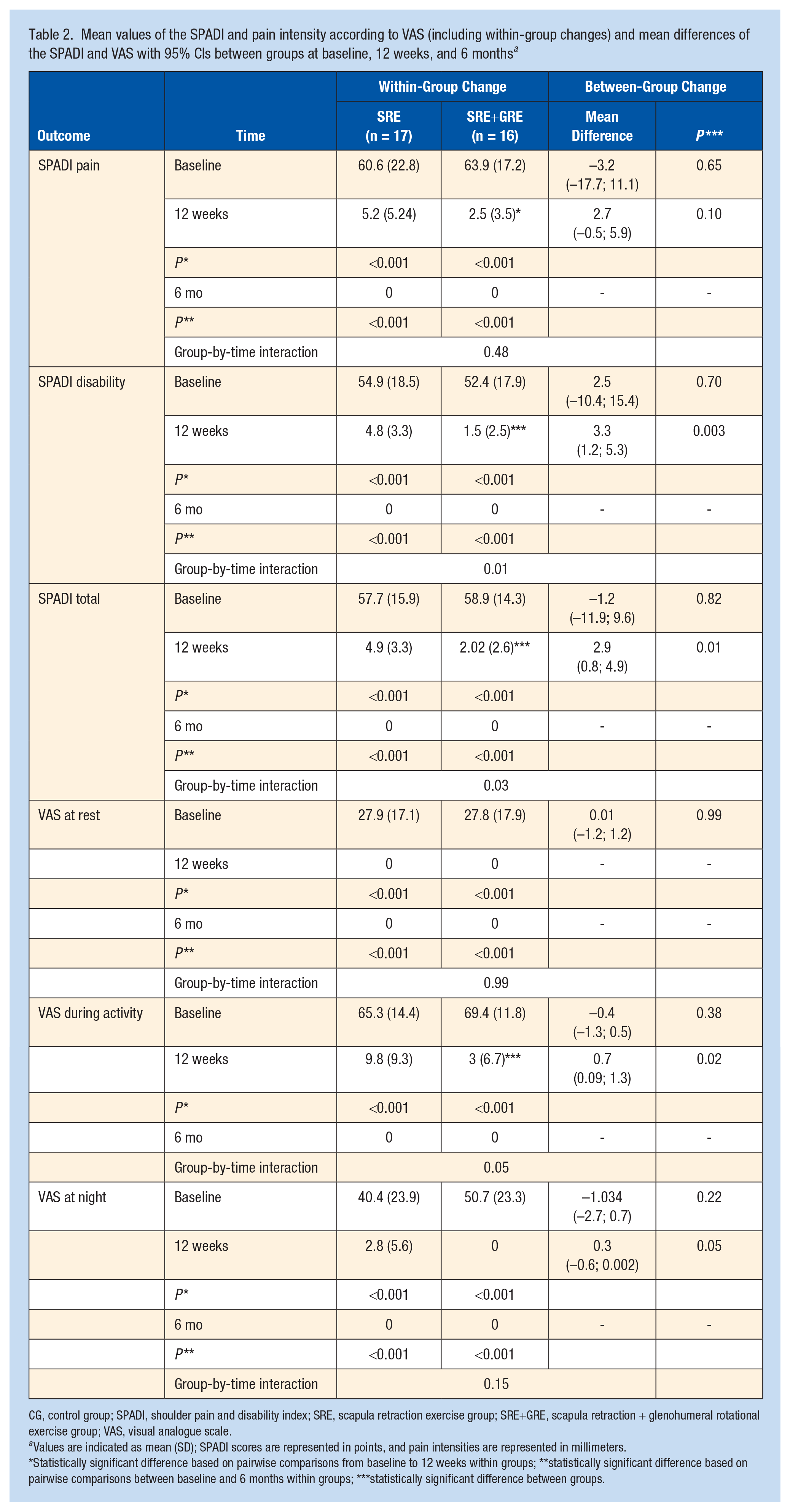
CG, control group; SPADI, shoulder pain and disability index; SRE, scapula retraction exercise group; SRE+GRE, scapula retraction + glenohumeral rotational exercise group; VAS, visual analogue scale.
Values are indicated as mean (SD); SPADI scores are represented in points, and pain intensities are represented in millimeters.
Statistically significant difference based on pairwise comparisons from baseline to 12 weeks within groups; **statistically significant difference based on pairwise comparisons between baseline and 6 months within groups; ***statistically significant difference between groups.
For functionality (Table 2), there was no significant group-by-time interaction for SPADI-pain (F1,33 = 0.533; P = 0.48). However, a significant main time effect was found. SPADI-pain was improved at 12 weeks (P < 0.001) and 6 months (P < 0.001). There was a significant group-by-time interaction for SPADI-disability (F1,33 = 5.148; P = 0.01) and SPADI-total (F1,32 = 4.172; P = 0.03). Pairwise comparisons revealed that the SRE+GRE group showed lower SPADI-disability (P = 0.003) and SPADI-total (P = 0.01). For pain intensity (Table 2), there was no significant group-by-time interaction for pain at rest (F1,31 = <0.001; P = 0.99) and at night (F1,32 = 2.166; P = 0.15). Yet, a significant main time effect was found (at rest: F1,31 = 83.393; P < 0.001; at night: F1,32 = 121.22; P < 0.001). The pain at rest and night decreased at 12 weeks (P < 0.001; P < 0.001; respectively) and at 6 months (P < 0.001; P < 0.001; respectively). However, a significant group-by-time interaction was found for pain during activity (F2,62 = 3.204; P = 0.05). Pairwise comparisons revealed that less activity pain was recorded in favor of the SRE+GRE group (P = 0.02).
The mean AHD values and SDs of all participants are reported in Figure 3. There was no significant group-by-time-by angle interaction found for all angles (F16,368 = 0.942; P = 0.40). However, a statistically significant main angle effect was observed (F4,183 = 3.271; P = 0.01), showing that the AHD reduced when the shoulder was abducted. For all participants, the reduction in AHD was significant between 0° and 30° (P = 0.03, mean change = 1.56 mm; 95% CI: 0.7, 3.1), between 0° and 45° (P < 0.001, mean change = 2.97 mm; 95% CI: 2.4, 3.6), and between 0° and 60° (P < 0.001, mean change = 3.3 mm; 95% CI: 2.7, 3.9). A statistically significant group-by-time interaction was found for the AHD values (F4,92 = 6.38; P = 0.001). At baseline, the decrease in AHD was greater in the intervention groups compared with CG at all elevation angles (Table 3). Intervention groups demonstrated increased AHD values over time (except 0° of shoulder abduction in the SRE group) (Figure 3). Pairwise comparisons demonstrated that larger AHD values were observed in the SRE+GRE group than in the SRE group at all elevation angles at 12 weeks and 6 months (Table 3). Moreover, greater AHD values were found in the SRE+GRE group than in the CG (except 60° of shoulder abduction) at 6 months. In addition, test-retest analysis of the AHD measurement revealed an excellent reliability and acceptable measurement error (Table 4).
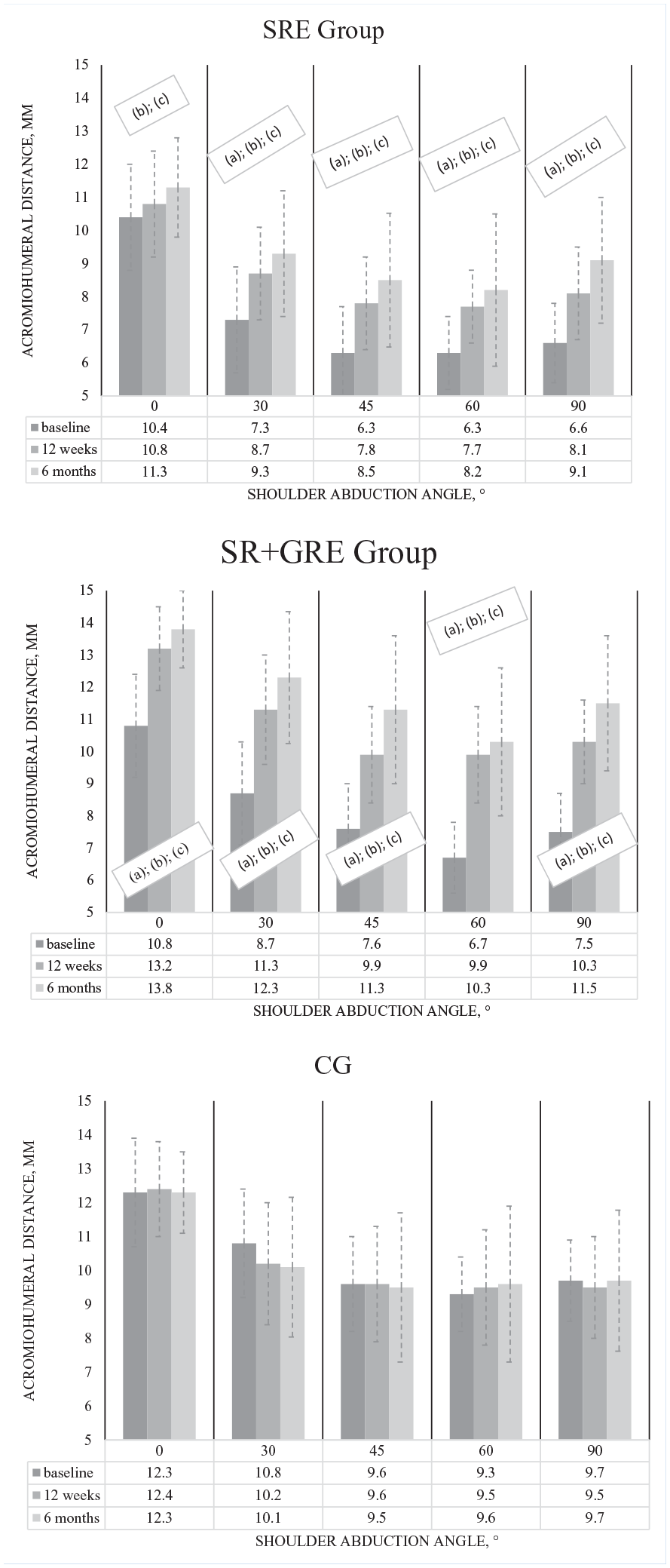
Measures of the AHD according to time (within groups) for the SRE, SRE+GRE, and CG at 0°, 30°, 45°, 60°, and 90° of abduction. Values are mean (SD) AHD (mm). *Statistically significant difference based on pairwise comparisons from baseline to 12 weeks within groups; **statistically significant difference based on pairwise comparisons from baseline to 6 months within groups; ***statistically significant difference based on pairwise comparisons from 12 weeks to 6 months within groups. AHD, acromiohumeral distance; CG, control group; SRE, scapula retraction exercise group; SRE+GRE, scapula retraction + glenohumeral rotational exercise group.
Mean differences in AHD values with 95% CIs between groups at baseline, 12 weeks, and 6 months a
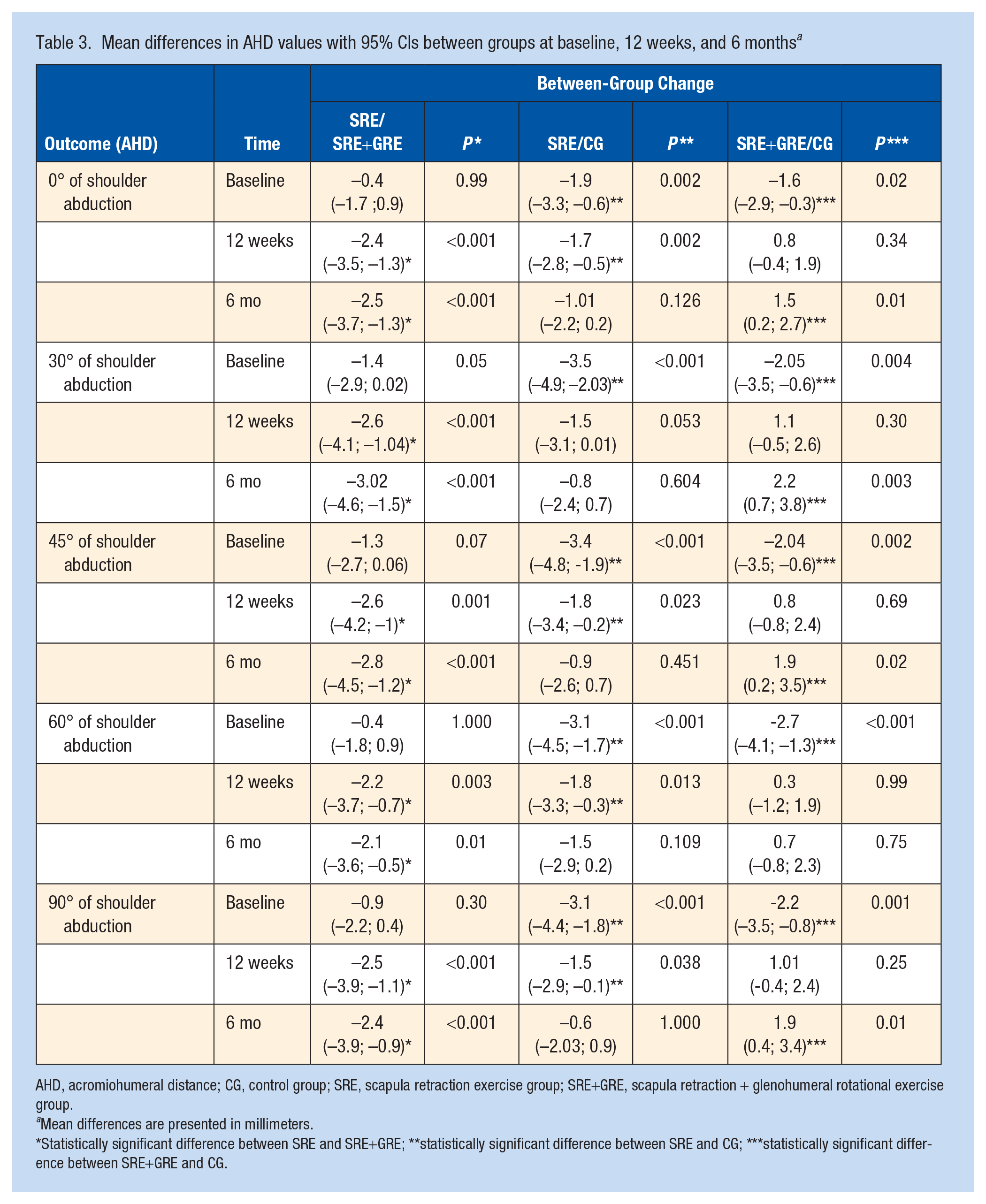
AHD, acromiohumeral distance; CG, control group; SRE, scapula retraction exercise group; SRE+GRE, scapula retraction + glenohumeral rotational exercise group.
Mean differences are presented in millimeters.
Statistically significant difference between SRE and SRE+GRE; **statistically significant difference between SRE and CG; ***statistically significant difference between SRE+GRE and CG.
Between-day reliability (ICC), SEM and MDC with 95% CI, and CV% of AHD measurements a
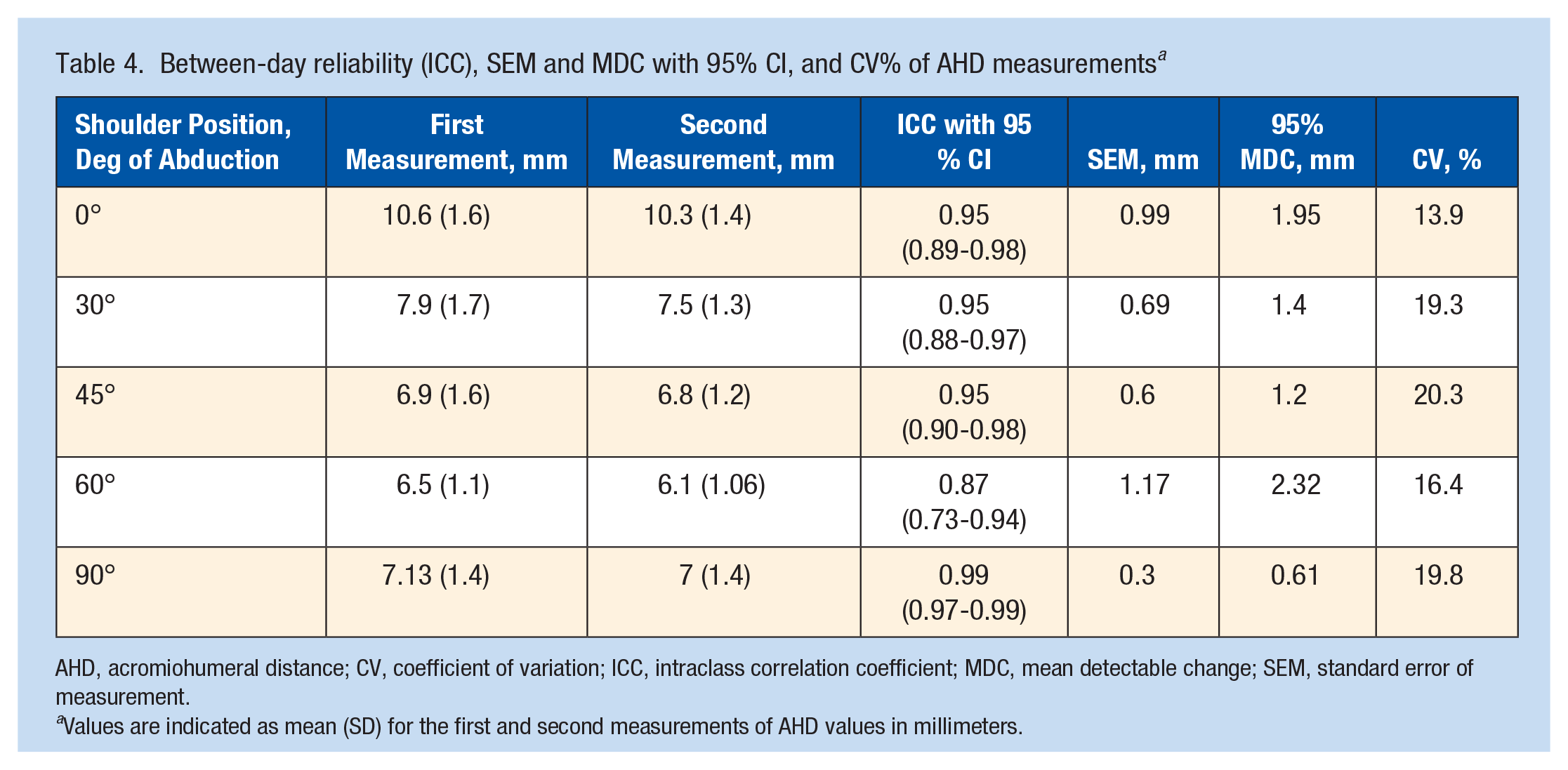
AHD, acromiohumeral distance; CV, coefficient of variation; ICC, intraclass correlation coefficient; MDC, mean detectable change; SEM, standard error of measurement.
Values are indicated as mean (SD) for the first and second measurements of AHD values in millimeters.
For patient satisfaction, there was no statistically significant difference observed at 12 weeks (P = 0.17). Moreover, satisfaction levels reached 100% in both groups at 6 months.
Discussion
The findings of this study support our primary hypothesis that utilizing SRE and GRE with a gradual progression in the scapula stabilization program was effective in patients with SPS at 12-week and 6-month follow-ups. However, group differences were not higher than the MCID. Moreover, our secondary hypothesis confirmed that patients with SPS showed narrower AHD values than the CG at baseline. Applying SRE and GRE together demonstrated greater AHD values. However, we found similar patient satisfaction levels. Patient satisfaction was expected to reach higher levels when their symptoms were relieved.
To our knowledge, this is the first randomized controlled trial interpreting the 12-week intensive rehabilitation program with a gradual progression and a reduced exercise program until 6 months in patients with SPS. Recent systematic reviews and meta-analyses have indicated that physiotherapy approaches consisting of manual therapy and exercises present positive rehabilitation outcomes.7,15,28 However, no consensus has yet determined which exercise program is superior.1,4,14,15,29,31,33 Furthermore, there were no thoughts regarding how to maintain rehabilitation outcomes or whether exercises should proceed as a reduced exercise program. In the present study, we chose scapula stabilization exercises from the exercises that demonstrated higher muscle activities based on previous electromyography studies.3,8,12,18,21,22 Exercises were performed intensively for the first 12 weeks. Then, the reduced exercise program was advised from 12 weeks to 6 months. In addition, we targeted applying SRE and GRE to retrain appropriate movement control–starting with the lowest elevation angle and proceeding to higher angles. Our main reasoning for performing SRE and GRE together at gradual elevation angles was the effect of scapular and rotator cuff muscles on subacromial space width during arm activities. The main contribution of this study (further to previous studies interpreting functional improvements and pain reduction) is that exercises targeting the principal deficiencies in patients with SPS provide greater AHD values. Previous studies have well documented that an important synergistic relationship between scapular stabilizers and the glenohumeral rotators is associated with the width of the subacromial space.10,24,34 This intimate relationship is also considered a stabilizer and mover. 10 While scapular muscles produce scapular upward rotation and retraction (the combination of the posterior tilt and ER), it also supports the glenohumeral movements. The main mechanism behind our finding could be explained by applying SRE and GRE step-by-step may improve the stabilizer and mover relationship of those muscles, thereby increasing AHD values.
Although AHD values increased in all patients compared with baseline, the AHD values of the SRE+GRE groups were greater than those of the SRE group (not CG) at 12 weeks. Studies investigating the effect of the exercises on AHD in patients with SPS have demonstrated conflicting results.4,33 One study investigating the coactivation approach in patients with SPS reported that the AHD did not differ. 4 However, another study investigating movement-oriented exercises reported an increased AHD. 33 Their methodological differences may cause a contradiction because their exercise programs and total intervention durations differed from our study. They followed a 6-week rehabilitation program and measured AHD at 3 shoulder positions. However, we followed the rehabilitation program for a 6-month duration and measured AHD at 5 active shoulder positions at 12 weeks and 6 months. In addition, we selected the gradual shoulder elevation angles while performing exercises that were similar to positions preferred during AHD measurements. Thus, we suggest clinicians focus on the exercises that prevent biomechanical deficits causing subacromial space narrowing if they aim to improve AHD.
The present study demonstrated a more pronounced widening of AHD in the SRE+GRE group at 6 months (higher than CG). Since manual therapy did not apply from 12 weeks to 6 months, increased AHD values may be a real effect of the exercises. The findings of this study support our premise that exercise selection should focus on maintaining subacromial space would be beneficial in patients with SPS. Previous studies have demonstrated the initial effect of exercises on AHD.17,19,35,42 According to their findings, SRE at different shoulder abduction positions, isometric pulldown exercise, and GRE increased AHD.17,19,35,42 To add to previous findings, our main contribution is that applying those exercises over the long term could increase the AHD in patients with SPS. Since the GRE was the only difference between groups in exercise selection, the additional effect of these exercises may have improved AHD values in our study. The main mechanisms behind the improvements can be explained as follows. The first is the depressor effect of the rotator cuff muscles on the humeral head. Typically, the deltoid has the largest elevator moment, requiring inferior counterbalance to prevent excessive subacromial space narrowing.28-30 The rotator cuff muscles are the most capable of actively reversing superior migration of the humeral head against the deltoid muscle activity. 16 Improving the force-coupling relationship between the rotator cuff and deltoid muscles utilizing progressive GRE increases the AHD. Another mechanism is the contribution rate of the stabilizer and mover relationship between the scapula and humerus during dynamic movements. Although concurrent movement of the scapula and humerus maintains the AHD, the relative contribution of the scapular and rotator cuff muscles to AHD differs. 10 In particular, superior migration of the humerus, rather than the inferior movement of the acromion (by means of scapular downward rotation and protraction), is the more dominant mechanism creating reductions in subacromial space. 10 Consequently, improving conscious control of the rotator cuff muscles at gradual shoulder abduction angles could provide more biomechanical benefits for maintaining subacromial space. Therefore, our results suggest that gradual SRE and GRE exercises in the scapula stabilization program could further increase AHD values in patients with SPS.
In this study, patient satisfaction was similar. These findings demonstrate that the satisfaction rate may be more related to the perceived impact of the residual symptoms or limitations of daily life. The results of the satisfaction surveys do not always associate with the objective outcomes achieved by the rehabilitation in question because patient factors influence satisfaction. A recent study reported that subjective tools (eg, VAS score, function score) were the most significant factor influencing patient satisfaction, rather than objective tools. 2 In our findings, patient overall expectation of pain-free shoulder function was restored after rehabilitation; they could be satisfied. In contrast, improvements in AHD values have been beyond the patients’ understanding and expectations. Therefore, similar symptom regression may explain the similar patient satisfaction rates in our study.
Limitations
This study has major limitations. First, caution is necessary when interpreting AHD improvements between groups, particularly considering that MCID values have not yet been calculated in patients with SPS. Besides, one must take into consideration that MCID values depend on the characteristics of the selected patients in clinical research. The smallest difference in AHD measurements that would be clinically meaningful to patients’ symptoms is still unknown. For this reason, we conducted our reproducibility analysis. As mentioned in the Methods section, we interpreted our clinical meaningfulness, calculating minimum detectable changes (MDCs) with 95% CIs. MDCs are often used to interpret the size of between-group effects (which can be detected objectively as true change outside of the measurement error). 20 In our study, changes in AHD values were interpreted in relation to MDCs. The group differences were found to be greater than the calculated MDCs values. Therefore, we could say that the group differences were a real change (not due to random measurement error) and demonstrated a clinically meaningful difference between groups. Although these differences may relieve the symptoms, they will not give information regarding any change in AHD width, which leads to a minimal clinically important change in the patient’s symptoms. Therefore, the meaningful AHD–the amount needed to change patient symptoms and shoulder function–must be calculated in further studies. Second, we did not include the scapula stabilization group only as a CG since the scapula retraction exercise is part of the scapula stabilization exercise program. Finally, the scapula stabilization program did not include specific thoracic exercises that may have affected AHD values. Future studies are needed to examine whether thoracic exercises affect the AHD.
Conclusion
This double-blind, randomized controlled trial provides evidence that exercises focusing on primary deficits are beneficial in terms of improvements in AHD values in patients with SPS. Furthermore, adding SRE and GRE gradually to the scapula stabilization program was shown to be superior to the scapula stabilization program alone for decreasing pain during activity, SPADI-disability, and SPADI-total. Therefore, we recommend adding progressive scapular and rotator cuff exercises into exercise programs as a safe and efficient measure. Future studies are needed to examine whether this proposed exercise program is efficient in maintaining AHD values in the long term.
Supplemental Material
sj-docx-1-sph-10.1177_19417381231155190 – Supplemental material for Utilizing Scapula Retraction Exercises With or Without Glenohumeral Rotational Exercises With a Gradual Progression for Subacromial Pain Syndrome
Supplemental material, sj-docx-1-sph-10.1177_19417381231155190 for Utilizing Scapula Retraction Exercises With or Without Glenohumeral Rotational Exercises With a Gradual Progression for Subacromial Pain Syndrome by Leyla Eraslan, Ozan Yar, Fatma Bilge Ergen, Gazi Huri and Irem Duzgun in Sports Health: A Multidisciplinary Approach
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.