Abstract
Background
Hallux valgus is a common condition with a complex etiology resulting in numerous treatment options. Recurrence of the deformity can occur following correction. Surgical technique and possibly also postoperative care play a role in reducing recurrence rates. This article highlights a postoperative surgical dressing technique which allows for semirigid support during the immediate postoperative period.
Methods
A wooden tongue depressor placed along the medial border of the hallux comprises the primary support for the dressing. The rigidity of the tongue depressor allows for the hallux to be drawn toward the depressor, encouraging neutral alignment of the hallux. Dressings are removed 2 weeks postoperatively, with new dressings applied in similar fashion and maintained in place until 6 weeks postoperatively.
Results
Based upon our observations, our surgical dressing technique provides sufficient support following hallux valgus correction surgery while being straightforward to replicate without the need for frequent dressing changes. The dressing materials are of negligible cost and are typically readily available. No associated wound complications have been observed.
Conclusions
We present an easily replicable and affordable option for postoperative hallux valgus correction surgical dressings.
Levels of Evidence:
Level V: Expert Opinion
“The overall goals of postoperative care following hallux valgus correction include pain management, bony and soft-tissue healing, and maintenance of the achieved alignment correction.”
Introduction
Hallux valgus is a common foot deformity affecting the first ray, with an estimated prevalence ranging from 23% to 35.7% of the population. 1 The severity of hallux valgus can be classified by measuring certain radiographic angles, including the hallux valgus angle, first and second intermetatarsal angle, and distal metatarsal articular angle. Surgical treatment options for this condition are extensive due to the complex etiology of hallux valgus. 2 Osseous abnormalities as well as soft-tissue imbalances are important to recognize and address in treatment. Recurrence rates are not insignificant; factors such as anatomic predisposition, noncompliance, certain medical comorbidities (eg, rheumatoid arthritis, Ehlers-Danlos, neuromuscular disorders), and poor surgical technique have been found to be associated with a higher risk of recurrence. 3 As the pendulum swings toward allowing earlier postoperative weightbearing, postoperative care (eg, immobilization, surgical dressings) potentially plays a larger role in patients’ outcomes.
The overall goals of postoperative care following hallux valgus correction include pain management, bony and soft-tissue healing, and maintenance of the achieved alignment correction. 4 However, no consensus exists with regard to postoperative care. The general agreement is in favor of utilizing a dressing that provides some degree of immobilization. 4 Typical postoperative bunion dressings are comprised of soft gauze folded between the first and second toes to maintain the corrected alignment of the great toe. While research investigating the outcomes after use of varying postoperative dressings is limited, some studies have found no difference in patient-reported outcomes, complications such as hallux valgus recurrence or nonunion, and/or radiographic parameters with the use of less restrictive postoperative dressings.5 -8 The postoperative dressing technique we describe uses semirigid support in the form of a splint, without being overly constrictive.
Technique
Materials required include non-adherent dressing (we prefer Xeroform), dry gauze, 2-inch gauze bandage, 2-inch cast padding, 1 wooden tongue depressor, and a 2-inch elastic bandage, all sterile. Once the incisions are closed, the foot is cleaned with normal saline-soaked laparotomy sponges and dried, and then a strip of non-adherent dressing is applied over the incisions, followed by dry gauze. The gauze is overwrapped with cast padding extending from the hallux and forefoot to just past the ankle, approximately 2 layers thick with 50% overlap between layers. The tongue depressor is then placed centered over the medial aspect of the hallux, ensuring that the distal aspect of the tongue depressor spans the distal phalanx (Figure 1). The proximal end of the tongue depressor often reaches to approximately the level of the midtarsal joints. The tongue depressor is secured in place with 2-inch gauze bandage in the following manner: several layers (typically 3) of gauze bandage are wrapped over the tongue depressor around the base of the foot proximal to the metatarsophalangeal joints, then the gauze bandage is advanced distally between the first and second toes, gently pulling the hallux toward the tongue depressor using at least 3 layers of gauze bandage (Figures 2-4). The remnant gauze bandage is wrapped evenly around the remainder of the foot and ankle. It is important to pass the gauze bandage at least once around the ankle to reduce the risk of slippage of the bandages. Further cast padding can be placed around the foot and ankle, followed by the 2-inch elastic bandage, ensuring that the elastic bandage passes around the hallux at least twice in similar fashion to the gauze bandage to further secure the hallux to the tongue depressor (Figure 5). A postoperative forefoot-offloading shoe is then applied.
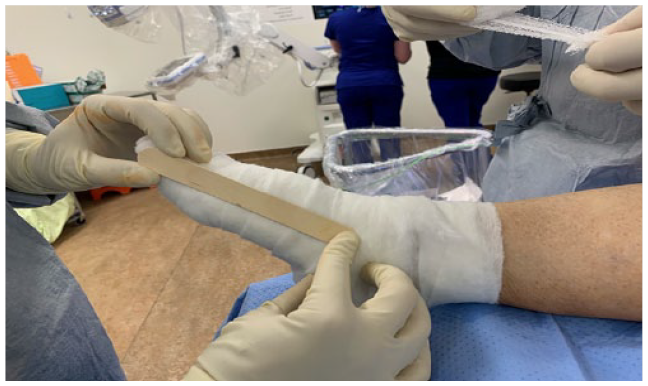
Demonstration of appropriate placement of the tongue depressor during application of the postoperative dressings.
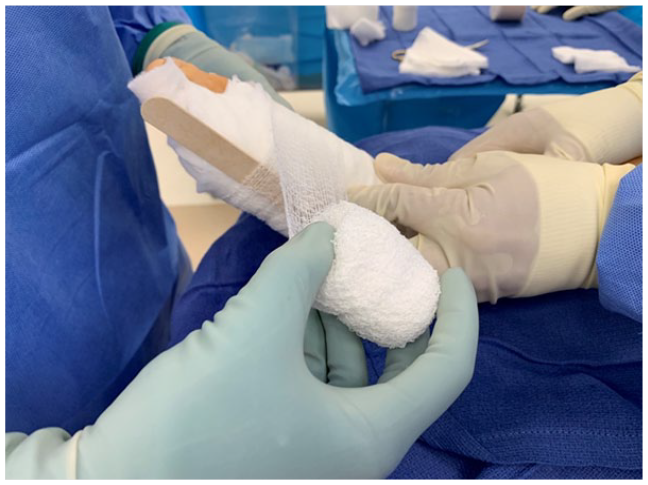
Initial securement of the tongue depressor along the medial aspect of the hallux with gauze wrap.
Demonstration of pulling the hallux gently towards the tongue depressor with gauze bandage.
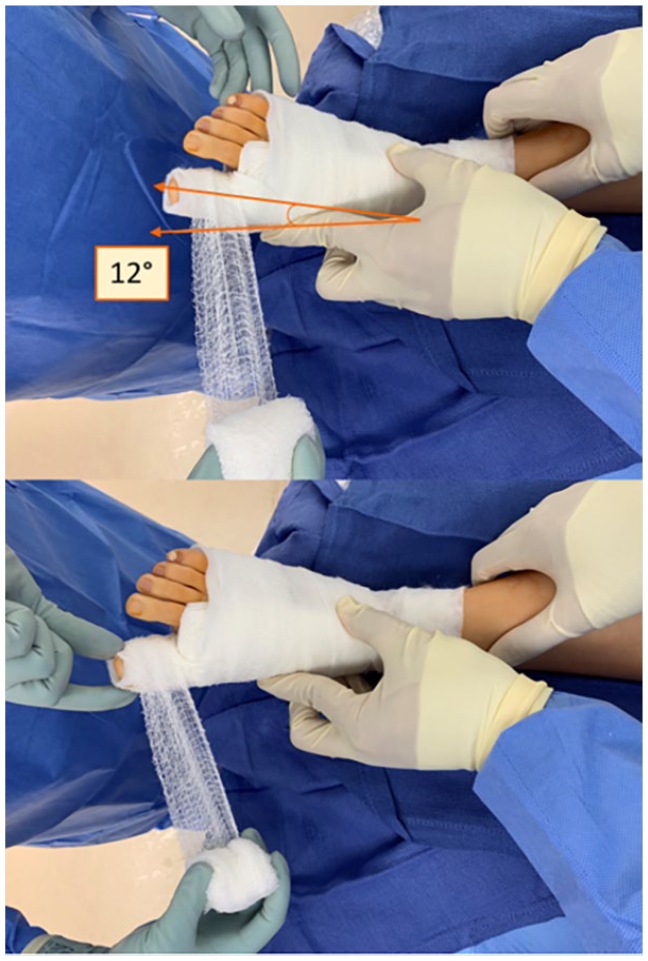
Representation of the additional correction achievable by securing the hallux to the tongue depressor with gauze bandage.
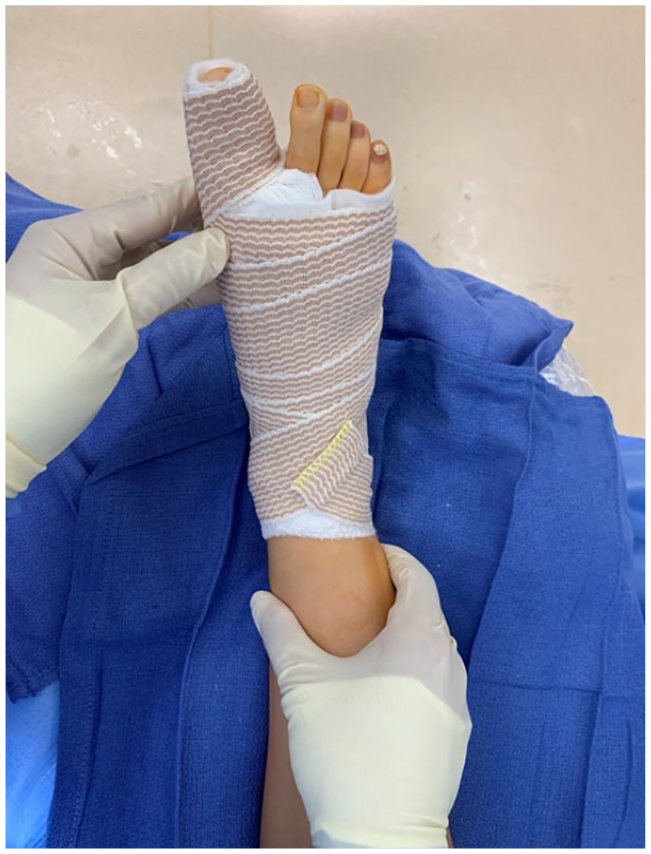
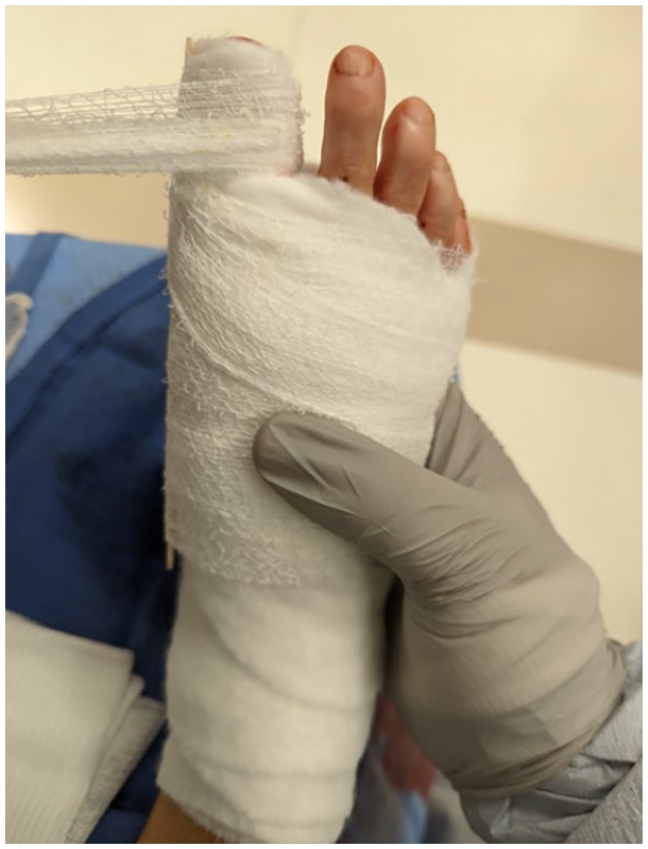
Completed surgical dressing.
The patient keeps this surgical dressing intact until the first follow-up appointment scheduled at 2 weeks postoperatively. We typically remove sutures at the initial follow-up visit, apply reinforced adhesive skin closure strips (Steri-Strip) to the incisions, and place new surgical dressings in similar fashion to the intraoperative dressings, but without the nonadherent dressing layer. These new dressings stay in place until the subsequent follow-up visit at 6 weeks postoperatively. The postoperative forefoot-offloading shoe is used for 6 weeks total and then the patient is allowed to progress to weightbearing as tolerated in a regular shoe. This technique is indicated for all hallux valgus correction procedures, regardless of the preoperative deformity severity or the type of procedure performed to achieve correction (including but not limited to minimally invasive techniques, open Chevron osteotomies, and Lapidus procedures). Having a concomitant lesser toe procedure (eg, hammertoe correction) is not considered a contraindication.
Discussion
Advantages of the described technique include the following:
The tongue depressor serves as a splint for rigid support along the medial aspect of the foot that pulls the hallux out of valgus while preventing the hallux from being pulled into excessive varus (ie, allows for neutral positioning of the toe). This method provides more support than gauze alone, but is less restrictive than a cast, which has not demonstrated additional benefit or decreased complication rates in the current literature.4,5,7 In addition, complication rates (eg, nonunion) have been found to be similar among various degrees of restrictive postoperative dressings when evaluated.4 -7
The tongue depressor is of negligible cost and is easy to obtain.
In the setting of concurrent second-toe correction surgery (eg, for hammertoe correction), the hallux is pulled to the tongue depressor, with minimal padding required within the first webspace. Thus, there is minimized risk of displacement of the second toe, compared to techniques which rely on a space-occupying material (eg, foam, gauze) within the first webspace.
Frequent dressing changes are not required with this technique, with only one dressing change performed at the 2-week postoperative clinic visit. In comparison, more time-intensive dressing techniques such as weekly spica taping of the hallux have not been found to significantly affect postoperative (radiographic) results (compared with the use of a postoperative foam toe separator). 8
It is important to ensure proper padding underneath the tongue depressor to prevent development of pressure wounds. In our experience, the gauze provides ample padding, and in the past 5 years that we have been using this technique, we have not yet encountered a patient with pressure wounds. Limitations of this technique include the potential for the tongue depressor to change in position between dressing changes if not adequately secured, which may negatively affect the maintenance of correction achieved. Increasing the frequency of postoperative visits could mitigate this possibility, but would be more labor- and time-intensive.
Future Directions
In the near future, we plan to examine the impact of our technique by performing a prospective cohort study measuring the intraoperative angles (hallux valgus, first and second intermetatarsal, and with or without distal metatarsal articular angle) pre- and post-application of surgical dressings at 2 weeks postoperatively and when the dressings are definitively discontinued at 6 weeks postoperatively.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable, because this article does not contain any studies with human or animal subjects.
Informed Consent
Not applicable, because this article does not contain any studies with human or animal subjects.
Trial Registration
Not applicable, because this article does not contain any clinical trials.
