Abstract
Nonalcoholic fatty liver disease (NAFLD), characterized by excessive liver fat accumulation, is a common liver disease linked to obesity, insulin resistance, and metabolic dysfunction. The lack of effective treatments against NAFLD has led to an increasing focus on alternative and natural remedies. Essential oils, extracted from a variety of plants, have drawn interest due to their high content of active compounds and potential functions to support liver health. Ginger essential oil, known for its anti-inflammatory, antioxidant, and cholesterol-lowering properties, promotes antioxidant enzymes and ameliorates liver fat accumulation in mice model of NAFLD. Nigella sativa oil with its diverse array of bioactive components, mitigates fatty liver by lowering tumor necrosis factor-alpha, malonaldehyde (MDA), and plasma lipids in vivo and in human trials that could contribute to NAFLD management. Garlic oil, rich in organosulfur compounds, has shown potential benefits in modulating oxidative stress and inflammation associated with NAFLD. Similarly, essential oils from turmeric, pepper, patchouli, and basil reduced lipid accumulation and inflammation and enhanced lipid metabolism in animal models of NAFLD. These findings underscore the use of essential oils as complementary medicines for NAFLD, opening avenues for further research and clinical applications.
Introduction
Nonalcoholic fatty liver disease (NAFLD), marked by the deposition of excessive triglycerides (TG) in the liver, has emerged as a major health concern, affecting nearly 30% of the global population.1,2 This liver condition is generally diagnosed among people with no history of unrestricted alcohol consumption. 3 Recently, the term “metabolic dysfunction-associated fatty liver disease (MAFLD)” has been proposed as an alternative to NAFLD to designate fatty liver diseases associated with metabolic dysfunction for an easy diagnosis of the disease. 4 While alcohol is absent from the scenario, the etiology of NAFLD is intricately woven into the fabric of modern lifestyles and obesity epidemic. 5 NAFLD encompasses a spectrum of liver conditions, ranging from benign hepatic steatosis to more severe forms that include nonalchoholic steatohepatitis (NAHS), fibrosis, and cirrhosis. 6 Advanced fibrosis and cirrhosis in NAFLD are correlated with the increasing liver-specific as well as the overall mortality throughout the world. 7
A number of factors are considered to be involved in the pathogenesis of NAFLD. Overconsumption of high calories and fructose leads to the accumulation of saturated fats in adipose tissues, which are then released into liver as free fatty acids (FFA) and deposited as TG and cholesterols in the hepatocytes. 8 De novo lipogenesis, which is regulated by sterol regulatory binding protein-1c (SREBP-1c) and carbohydrate response element binding protein (ChREBP), is the central mechanism behind fatty acid deposition in liver. 9 The overproduction of SREBP-1c under high insulin signaling leads to the increased expression of several genes involved in lipogenesis, including AMP-activated protein kinase α, fatty acid synthase (FAS), and phosphoinositide-3 kinase (PI3 K).10,11 This, in turn, leads to an increased influx of fatty acids into the liver, where they are converted into TGs and stored in. The accumulation of TGs inside the cytoplasm of hepatocytes is the emblem of NAFLD. 12
The absence of specific pharmacological interventions has prompted researchers to explore alternative and complementary approaches to manage NAFLD. Lifestyle modifications, such as healthy diets and regular exercise, remain crucial components of managing and preventing NAFLD. 13 Essential oils, derived from a diverse array of plant sources, such as ginger, orange, garlic, Artemesia argyi, and basil have garnered attention for their prospective therapeutic actions against NAFLD.14–17 This review aims to provide a comprehensive analysis of the current state of knowledge regarding the use of essential oils as a potential intervention against NAFLD. By discussing the findings from preclinical and clinical studies with reference to the underlying molecular mechanisms and highlighting potential challenges, this review aims to contribute to our understanding of the roles of essential oils in the treatment and management of NAFLD. As we delve into the intricate interactions between essential oils and hepatic metabolism, this exploration may unveil novel avenues for therapeutic development and pave the way for future research aimed at addressing this pressing public health issue.
Pathophysiology and Molecular Landscape of NAFLD
Nonalcoholic fatty liver disease comprises a spectrum of liver disorders, encompassing conditions in which fat builds up in the liver cells. 18 A combination of genetic, environmental, and metabolic factors is involved in the pathogenesis of NAFLD, causing the development and progression of hepatic steatosis or fatty liver, leading to more severe conditions such as NAHS, fibrosis, cirrhosis, and even hepatocellular carcinoma. 19 A central feature in the pathophysiology of NAFLD is insulin resistance, which plays a critical role in the development and progression of hepatic steatosis. 20 Insulin resistance leads to impaired insulin signaling in hepatocytes, adipocytes, and peripheral tissues and the activation of SREBP-1c and ChREBP (Figure 1). The activation of SREBP-1 and ChREBP occurs through 2 major pathways, namely PI3K and protein kinase B, promoting increased lipolysis in adipose tissue and excessive generation and release of FFAs into the blood flow. 21 The liver, in turn, takes up these FFAs and converts them into TG, contributing to the accumulation of fat within hepatocytes. 22

Pathophysiology and molecular landscape of nonalcoholic fatty liver disease (NAFLD). Created with www.biorendercom.
The augmented buildup of TGs within hepatocytes can trigger oxidative stress, creating an imbalance between the generation of reactive oxygen species and the antioxidant defense mechanisms by depleting the antioxidant enzymes. 23 Oxidative stress activates inflammatory responses, recruiting immune cells to the liver and initiating a release of inflammatory cytokines, such as tumor necrosis factor-alpha (TNF-α), interleukin-6 (IL-6), and IL-1β through cytochrome P450 2E1 (CYP2E1)-mediated pathway. 24 This inflammation along with dysregulated lipid metabolism is the principal characteristic of NAFLD. 25 Mitochondrial dysfunction and the uncontrolled lipid droplet formation and turnover within hepatocytes lead to the intracellular retention of TGs. 26 Simultaneously, de novo lipogenesis, the process of synthesizing fatty acids utilizing precursors from nonlipid sources, is upregulated in NAFLD, which further intensifies the hepatic lipid accumulation. 27
The interplay between the liver and adipose tissue is fundamental to the pathophysiology of NAFLD. Adipose tissue dysfunction, as seen in obesity, results in altered secretion of adipokines and cytokines. 28 Increased release of pro-inflammatory cytokines, such as TNF-α and IL-6 further amplifies the inflammatory cascade in the liver, promoting NAHS progression. 29 In addition, genetic predisposition significantly contributes to the NAFLD susceptibility among individuals. In particular, polymorphisms in genes, such as peroxisome proliferator-activated receptors (PPAR), SREBP, and TNF-α involved in lipid metabolism, insulin signaling, and inflammation may influence an individual's risk of developing NAFLD and its progression to more severe stages. 30 Furthermore, dysbiosis of gastrointestinal microflora leading to dysregulated appetite signaling, reduced short-chain fatty acid production, and suppressed bile acid metabolism is considered an important factor in the pathogenesis of NAFLD (Figure 1). 31 Understanding these molecular mechanisms provides a foundation for developing targeted therapies aimed at specific pathways involved in the progression of NAFLD. Research in this field is ongoing, with the ultimate objective of identifying effective interventions to prevent and treat NAFLD. Recently, essential oils from various sources have shown remarkable effects against NAFLD progression, underscoring the potential of essential oils as an alternative therapy in mitigating NAFLD.
Essential Oils in the Treatment and Management of NAFLD
Essential oils have historically been used as natural therapeutics against numerous diseases. 32 Essential oils, derived from various plants through distillation or cold pressing, are intricate blend of volatile compounds, including alcohols, aldehydes, esters, ethers, ketones, and terpenoids generated during the secondary metabolism of the plant raw material. 33 Essential oils have demonstrated anti-inflammatory, antioxidant, hepatoprotective, and lipid-lowering effects in preclinical and clinical studies, which are largely attributed to the presence of bioactive compounds, including terpenes, phenolics, and flavonoids (Figure 2).34,35 The use of essential oils in addressing metabolic NAFLD is an area of continuing research. Essential oils, such as ginger, garlic, and Nigella sativa oils, have shown promising effects in reversing NAFLD through modulating lipid metabolism, de novo lipogenesis, oxidative stress, and hepatic inflammation (Table 1).
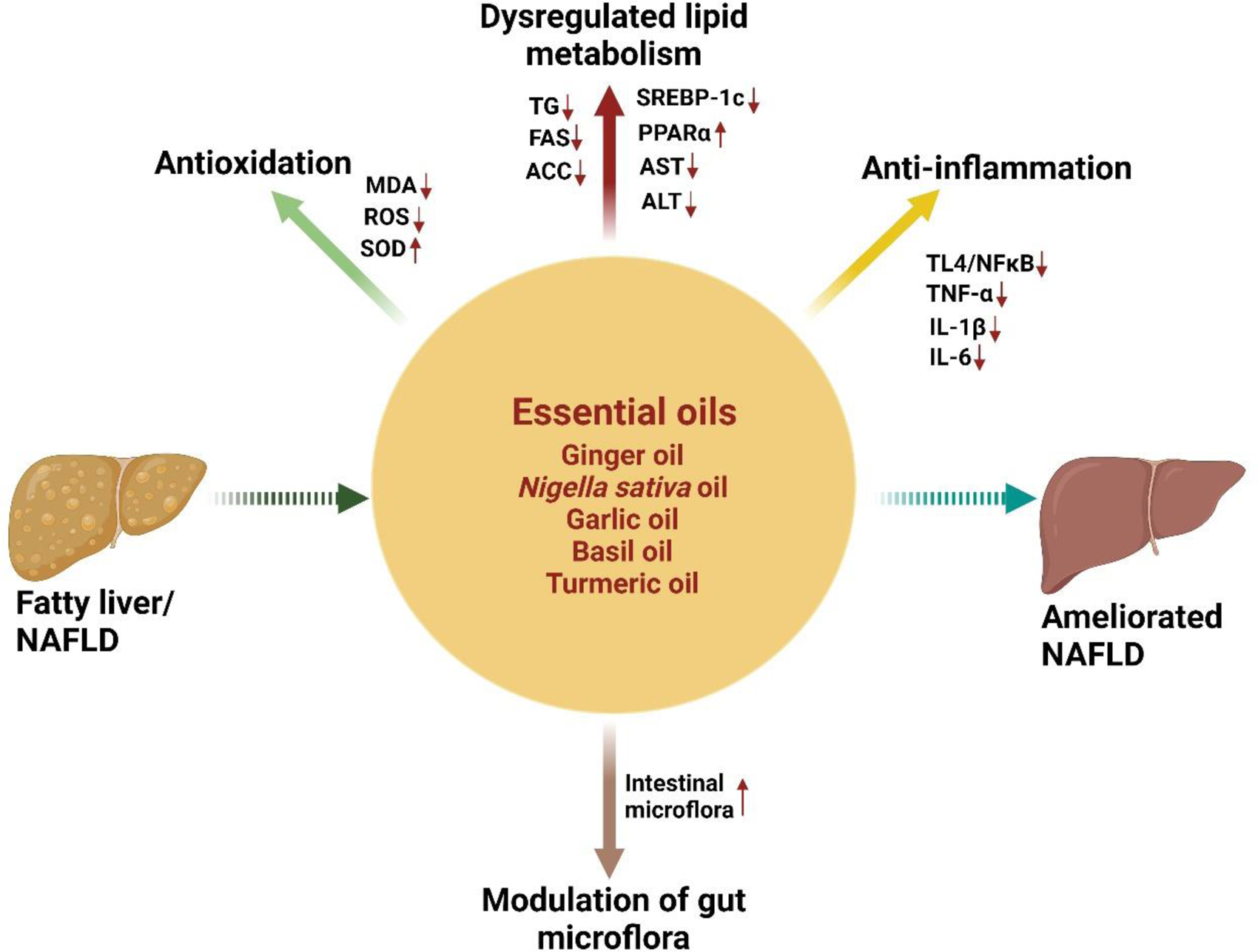
Ameliorating effects of essential oils against nonalcoholic fatty liver disease (NAFLD). Created with www.biorendercom.
Effects of Essential Oils on Nonalcoholic Fatty Liver Disease (NAFLD).

Abbreviations: FFA, free fatty acids; TG, triglycerides; TNF-α, tumor necrosis factor-alpha; PPAR, peroxisome proliferator-activated receptor; ALT, aminotransferase; LDL-C, low-density lipoprotein cholesterol; HDL-C, high-density lipoprotein cholesterol; SOD, superoxide dismutase.
Ginger Essential oil
The root of Gingiber officinale, commonly known as ginger, is one of the most widely used spices around the world. For centuries, ginger has been used as a “miracle medicine” to treat a wide range of illnesses, including diabetes, cancer, inflammation, and gastrointestinal disorders. 47 Recent clinical trials on patients with type II diabetes and hyperlipidemia highlighted the potential effects of ginger in reducing insulin resistance and serum triglyceride (TG) concentration. 48 Ginger essential oil (GEO), abundant in gingerol, shogaol, zingerone, β-bisabolene, and other bioactive compounds, is renowned for its remarkable antioxidative, anti-inflammatory, and cholesterol-lowering properties. 49 GEO hindered the progression of NAHS by reducing plasma alanine aminotransferase (ALT) level, enhancing antioxidant catalase, glutathione, and glutathione reductase levels, and lowering hepatic pro-inflammatory cytokine levels. 50 GEO also mitigated hepatic inflammation by modulating the NLR family pyrine domain-containing 3 inflammasome and LPS/Toll-like receptor 4 signaling pathways. 36 Furthermore, GEO promoted the increase of favorable bacterial populations while reducing the harmful bacteria associated with NAHS. In a follow-up study, GEO demonstrated hepatoprotective effects against high-fat diet-induced NAFLD in obese mice by inhibiting lipid biosynthesis and oxidative stress. 37 In particular, GEO suppressed the expression of SREBP-1c, FAS, and cytochrome P450 2E1 (CYP2E1) in mice. Further preclinical and clinical studies are needed to better understand the specific mechanisms and optimal dosage for the potential therapeutic use of GEO in addressing NAFLD.
Nigella sativa Seed Oil
Nigella sativa, commonly known as black seed or black cumin, has rich historical and cultural significance as a medicinal plant. Apart from its culinary applications across diverse cultures, Nigella sativa possesses numerous bioactive compounds with demonstrated anti-inflammatory, antioxidant, and hepatoprotective activities. 51 Nigella sativa seed oil (NSO), containing thymoquinone, thymohydroquinone, and flavonoids, is renowned for its pharmaceutical properties against various chronic diseases. 52 A number of clinical investigations have specifically highlighted the favorable effects of NSO against insulin resistance and diabetes mellitus.53,54 Explorations into the impact of NSO on NAFLD reveal a multifaceted influence on the progression and management of this deadly liver condition. 55 An in vivo study by Al-Okbi and colleagues suggest that NSO could serve as an effective supplement against inflammatory fatty liver by reducing TNF-α, MDA, and plasma lipids. 38 Recent results from a randomized controlled trial further underscore the efficacy of NSO in enhancing liver health by mitigating steatosis and reducing liver injury in individuals with NAFLD. 39 Notably, NSO's influence extends to blood lipid profiles, marked by a significant reduction in TG, low-density lipoprotein cholesterol (LDL-C), and an increase in high-density lipoprotein cholesterol (HDL-C) levels among NAFLD patients. This compelling evidence suggests that NSO holds promise as an effective therapeutic intervention for patients with NAFLD.
Garlic Essential Oil
Garlic, celebrated for its medicinal properties, has attracted unprecedented research attention due to its rich bioactive profile pharmacological functions. Renowned for their anti-inflammatory, antioxidant, anticancer, and various health-promoting attributes, both garlic and its bioactive constituents play significant roles in the management of chronic diseases. Numerous preclinical and clinical investigations indicate that garlic supplements can reduce the incidence and severity of NAFLD by modulating oxidative stress, hepatic inflammation, and hepatic steatosis.56–58 Garlic essential oil (GO) emerges as a novel therapeutic tool with potential benefits in preventing cancer, alleviating oxidative damage and inflammation, preserving liver health, and reducing blood sugar levels. 59 Previous research underscores the promising effects of organosulfur compounds derived from GO, such as diallyl disulfide and diallyl trisulfide, in addressing the multifaceted challenges presented by NAFLD. 60 Lai et al reported that GO and its active compound DAD exhibited anti-NAFLD effects in obese mice by regulating key enzymes and molecules involved in lipid synthesis and metabolism, including SREBP-1c, acetyl-CoA carboxylase, FAS, and PPAR-α. 40 The authors propose that GO and DAD offer protection against lipid accumulation, inflammation, and oxidative stress in obese mice with NAFLD. In another rodent study, the use of single clove garlic oil demonstrated significant effects in enhancing oxidative status by increasing the activity of superoxide dismutase antioxidant enzymes and suppressing pro-inflammatory cytokines, such as TNF-α, IL-6, and IL-1β in high-fat diet-induced hepatic steatosis in rats. 41 These results underscore the potential therapeutic benefits of GO in addressing oxidative stress and inflammation associated with NAFLD.
Others
While essential oils are often emphasized for their aromatic and therapeutic properties, their prospective roles in addressing the challenges of NAFLD are being continually investigated. The body of evidence supporting the utilization of essential oils as a possible remedy for NAFLD is expanding, suggesting a promising avenue for further exploration and discovering therapeutic applications in preventing NAFLD.
Turmeric, a spice derived from the Curcuma longa plant, has a long history of medicinal use for its anti-inflammatory and antioxidative properties. Growing body of research outcomes suggest that the active compound in turmeric, known as curcumin, may exert beneficial effects in inhibiting the progression of NAFLD. 61 Notably, supplementing turmeric essential oil (TO) to rats with NAHS, resulted in the reduction of lipid weight, a decline in hepatic TG, and the activation of PPAR-α associated with lipid metabolism. These outcomes suggest that TO exerts inhibitory actions on liver fat accumulation in NAHS by enhancing the lipid metabolism. 45
Amomi fructus, derived from the seeds of Amomum villosum, has shown beneficial effects in addressing NAFLD. Amomi fructus exhibits anti-inflammatory and antioxidant properties that may mitigate liver damage associated with NAFLD. Volatile oil from A fructus (VOAV) inhibited endogenous lipid synthesis and lipid buildup in the liver by reducing TG, TC, FFA, and LDL-C levels in rats. In addition, VOAV adjusted microflora, reduced inflammation by boosting zona occludens and occludin, and suppressed the TLR4/NF-κB pathway, making it a compelling candidate for further investigation as a natural intervention against NAFLD. 46
Patchouli oil, due to the high content of sesquiterpenes and flavonoids demonstrated therapeutic effects against hepatic steatosis by counteracting hepatic lipid accumulation in rats. 62 These results suggest a possible role of PO in mitigating the underlying factors associated with NAFLD, including hepatic inflammation and oxidative stress.
Peppermint oil (PPO), derived from the Menta piperita plant, demonstrated therapeutic benefits in mitigating NAFLD. According to the results from a randomized control trial, PPO could ameliorate NAFLD by lowering liver enzymes, including ALT, AST, and MDA levels, indicating its antioxidative functions in reversing NAFLD. 63
Basil essential oil (BO) and its active compounds, such as eugenol, and flavonoids have well-known therapeutic implications in improving liver health. 64 Administering BO slowed NAHS progression in a rat model of NAFLD with a special reference to gut-liver axis. 42 Remarkably, BO reduced the levels of total cholesterol, TGs, and low-density lipoprotein cholesterol. Therefore, modulating gut-liver axis in combating NAFLD using essential oils deserves further investigations.
Conclusion
Essential oils from ginger, Nigella sativa, garlic, and others are endowed with bioactive compounds and have therapeutic implications against NAFLD. The multifaceted biological functions of essential oils, including antioxidant, immunomodulatory, and hepatoprotective effects, highlight their potential to mitigate the progression of NAFLD. However, the current evidence on the benefits of essential oils in counteracting NAFLD is rather limited, necessitating future investigations with well-designed methodologies. For now, essential oils could be suggested as adjunctive therapies for the prevention and management of NAFLD alongside lifestyle modifications, dietary changes, and medication. Further research and clinical studies are warranted to elucidate the specific mechanisms and optimal formulations for integrating essential oils into preventive or therapeutic strategies for NAFLD.
Footnotes
Author Contributions
Conceptualization, MAM, RJK, and TK; Formal analysis, JY; Funding acquisition, JY; Investigation, MAM and RJK; Validation, JY and TK; Writing – original draft, MAM and RJK; Writing – review & editing, SMS, TK & JY. Validation: JHC. All authors have read and approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by a National Research Foundation of Korea (NRF) grant funded by the Korean government (MSIT) (NRF-2022R1F1A1074769; RJK) and 2023 research grant from Pusan National University Yangsan Hospital. The funding bodies did not have a role in the design of the study and collection, analysis, and interpretation of data and in writing the manuscript.
