Abstract
Aim:
We compared biochemical and clinical data of individuals with type 2 diabetes (T2D) who opted for only teleconsultation (ie, no in-person visit at all), hybrid visits (combining home blood tests and in-person consultation), and fully in-person visits (both tests and consultation in person) at a tertiary care diabetes center.
Methods:
In this observational cohort study, we retrieved demographic, anthropometric, and biochemical data of 8197 individuals with T2D who sought diabetes care between 2021 and 2023 (384 participants with only teleconsultations, 721 with hybrid visits, and 7092 with fully in-person visits) from the electronic medical records of a chain of tertiary diabetes care centers across India.
Results:
Individuals who opted for teleconsultation had a shorter duration of diabetes compared with those who opted for hybrid or fully in-person visits. Although participants who opted for a teleconsultation had better glycemic and lipid control at baseline, those who underwent hybrid and in-person visits showed greater improvements in fasting plasma glucose, glycated hemoglobin (A1c), and LDL cholesterol (LDL-C) during follow-up. Improvements in overall ABC target achievement (
Conclusion:
While teleconsultation is a useful complement to in-person visits, the latter results in better glycemic and lipid control, perhaps due to more effective engagement with the diabetes care team.
Introduction
Diabetes mellitus affects more than 500 million individuals worldwide, more than 100 million of whom reside in India.1,2 Type 2 diabetes (T2D) usually occurs at younger ages and lower levels of obesity among Asian Indians.3-5 Management of diabetes entails frequent follow-up with health care providers to enable assessment of the level of metabolic control and timely changes in the treatment regimen so that chronic organ- and life-threatening complications can be prevented. Unfortunately, individuals with diabetes are often unable to adhere to the follow-up schedule on account of factors such as lack of time, distance and finances. This is particularly so in countries like India, where the majority of patients with diabetes reside in rural areas. Moreover, health care facilities and providers are mostly located in cities and towns. This leads to suboptimal follow-up, poorly controlled diabetes and increased risk of complications as shown by the ICMR INDIAB study where only 7% of patients achieved the ABC (ie,
The advent of telemedicine has, therefore, offered new hope to individuals with diabetes, enabling them to access quality health care without leaving their homes. The term Telemedicine refers to the delivery of health care services using communication technology to exchange information for diagnosis, treatment, disease prevention, research, and the continuing education of health care providers. 7 Telephone or videoconference-based teleconsultations offer an effective alternative to traditional face-to-face consultations. They have the potential to provide timely and cost-effective interventions remotely, thereby enhancing health care accessibility. 8 Telephone or video consultations can potentially reduce access costs 9 and limit the transmission of infectious agents, 10 albeit with the caveat that the quality of care may be compromised if not implemented appropriately. In India, on March 25, 2020, during the COVID-19 pandemic, the Ministry of Health & Family Welfare recognized telemedicine and established the country’s telemedicine policy guidelines. 11
A comprehensive meta-analysis on the effectiveness of telemedicine interventions in T2D has highlighted the potential benefits of telemedicine in reducing HbA1c levels and improving overall diabetes management. 12 Earlier studies have emphasized the potential benefits of telemedicine in improving patient outcomes, increasing access to care, and enhancing patient engagement.13-15 As telemedicine continues to evolve, it is likely to play an increasingly important role in the management of diabetes and other chronic conditions. However, notwithstanding the myriad benefits of teleconsultation, many individuals still prefer to visit medical centers for in-person consultations as they need the personal touch of their physicians. There is little data from developing countries like India on the effectiveness of telemedicine for diabetes control, and how it compares with traditional in-person consultation. This study aimed to compare the impact of teleconsultation (no in-person visits) versus hybrid visits (combining in-person testing and teleconsultation) or fully in-person (tests and consultation visit) on clinical and metabolic parameters in patients with T2D at a tertiary care diabetes center in India.
Methods and Data Collection
For this observational cohort study, we retrieved demographic, anthropometric, and biochemical data of 8197 individuals with T2D who sought diabetes care between 2021 and 2023, from the electronic medical records of a chain of tertiary diabetes care centers across India. We excluded other types of diabetes (type 1 diabetes, gestational diabetes mellitus, fibro calculous diabetes mellitus, secondary diabetes, etc.) from the data set. We included only those diagnosed with T2D per standard diagnostic criteria and definitions and confirmed by a physician. We categorized individuals with T2D into three groups as follows: participants who had only teleconsultation (ie, no in-person visit at all), (n = 384); those who had hybrid visits (combining home blood tests and in-person consultation), (n = 721) and those who had fully in-person visits (both tests and consultation) (n = 7092). Figure 1 shows the study flowchart. Follow-up data for each category were acquired for further analysis and comparisons to determine which group showed better outcomes. Overall, the follow-up data were available in 43% (n = 3494, 6.0% in teleconsultation, 56.2% in hybrid, and 43.2% in in-person consultations) with a mean follow-up duration of 0.5 ± 0.4 years (1.6 ± 0.6 years for teleconsultation, 0.7 ± 0.4 years for hybrid and 0.6 ± 0.3 years for in-person visit consultations).

Study flowchart.
Teleconsultation
Patients who opted for teleconsultation never visited the center for anthropometric or clinical evaluations during the study duration. The follow-up consultations with the health care providers were also conducted remotely. The flow of patient care through teleconsultation was as follows: The patient contacted the diabetes center through digital or nondigital medium and they were referred to the dietitian/diabetes educator, who accessed the patient’s electronic records. After reviewing the patient’s history, the dietitian followed standard recommendations/guidelines to order tests and scheduled an appointment for home blood collection. The consultant could review or modify the ordered tests before blood collection based on specific patient complaints. Trained phlebotomists collected biospecimens at the patient’s doorstep, and the samples were labeled using barcoded labels for identification. Anthropometric measurements and blood pressure (BP) were also recorded at home. All biospecimens were brought to the central laboratory for processing. Data on anthropometry and BP were entered into the electronic medical records. Once blood reports were generated, they were shared with the patient and automatically linked to their electronic medical records. After teleconsultations were scheduled, the consultants viewed the reports online and contacted patients through audio and video calls (arranged according to the patient’s preference). Calls typically lasted for five to ten minutes. The final prescription was electronically sent and medicines were delivered to the patient’s doorstep wherever necessary. 10
Hybrid Visit
Diabetes management appointments that involved a mix of both in-person visits and teleconsultations were considered hybrid visits. In such cases, the patients physically visited the health care facility for tests or evaluations related to diabetes and later had a follow-up consultation with the doctor through audio and video calls at their convenience. Alternatively, they could opt for home blood collection and tests and see the provider in person. This approach allows for diabetes education and counseling by a diabetes educator/dietitian, during their in-person visit to the center giving the patients flexibility in reaching out to the health care team.
In-Person Visits
This is the traditional model where patients visit the center for blood tests and clinical evaluation and then have in-person consultations with the doctor.
Following the registration process at the center, patients were initially assessed by the dietitian or diabetes educator, who collected a comprehensive medical history, including information on presenting symptoms, previous illnesses, dietary habits, family history of diabetes, current medications, and any surgical procedures that may have been performed.
The patient was examined in detail by a doctor and relevant tests were ordered. The patient could then proceed for cardiac, eye, and foot evaluations as needed. Consultations with concerned specialists (cardiologists, ophthalmologists, surgeons etc.) were also available. The patients received counseling and education on diet by diabetes educators/dietitians. Exercise and stress management sessions were also provided by trained personnel. These were followed by the final diabetes consultations, which took anywhere between 10 to 30 minutes. Once a final prescription was generated, patient had the option of buying medications. Before leaving the clinic, the next follow-up visit date was fixed.
Clinical evaluations are detailed below: Height was measured in centimeters using a stadiometer and weight was measured using a traditional spring balance and recorded to the nearest 0.1 kg. Body mass index (BMI) was calculated using the formula: weight (kg)/height squared (m2). Blood pressure was recorded in the resting seated position in the right arm using a mercury sphygmomanometer and rounded off to the nearest two mmHg. Two readings were taken five minutes apart and the mean of the two readings was used.10,16
A fasting blood sample was collected following an overnight fast of no less than eight hours. Participants with a previously confirmed diabetes diagnosis were provided with a standard breakfast, 90 minutes after which a venous blood sample was taken for the postprandial glucose measurement. Biochemical assays were performed at the main center as well as branch laboratories, which undergo regular standardization with the Central Lab through stringent quality control tests. 10 Plasma glucose was estimated by the glucose oxidase method, serum cholesterol by cholesterol oxidase and peroxidase (CHOD-PAP) method, triglycerides by glycerol phosphate oxidase-peroxidase-amidopyrine (GPO-PAP) method, HDL cholesterol by direct Immunoinhibition, and low-density lipoprotein cholesterol was calculated using the Friedewald equation. All analyses were carried out on Beckman Coulter AU2700 (Fullerton, CA) biochemistry analyzer. Glycated hemoglobin (HbA1c) was estimated by high-performance liquid chromatography using the Variant II Turbo (Bio-Rad, Hercules, CA). The fasting and stimulated (post-breakfast) C-peptide levels were estimated by chemiluminescence method on a Siemens ADVIA lentaur XPT immunoassay analyzer at the time of first registration at the center.10,16
Definitions
Diabetes
Diabetes was defined when the fasting plasma glucose (FPG) level was ≥ 126 mg/dL (7.0 mmol/l) and/or 2-h post-load glucose level ≥ 200 mg/dL (11.1 mmol/l), 17 or if there was a physician-treated or a self-reported diagnosis of diabetes or if the individual was on medications for diabetes.
Type 2 Diabetes
Type 2 diabetes (T2D) was diagnosed based on the absence of ketosis, absence of pancreatic calculi (on abdominal radiograph), and response to oral hypoglycemic agents (OHA) for more than two years. 16
Obesity Classification
Underweight if BMI <18.5 kg/m2; Normal if BMI was 18.5 to 22.9 kg/m2, Overweight if BMI was ≥23.0 to 24.9 kg/m2 and Obese if BMI was ≥25.0 kg/m2. 18
Glycemic Targets
Good control if glycated hemoglobin was ≤7.0%, Fair control if between 7.0 to 7.9%, and Poor control if ≥8.0%. 19
Hypertension
Subjects with self-reported hypertension and on drugs for hypertension and those who had a systolic BP of ≥140mmHg and/or diastolic BP of ≥90mmHg 20 were considered to have hypertension.
Dyslipidemia
Dyslipidemia was considered to be present if any of the following were present.
Hypercholesterolemia
If serum cholesterol levels were ≥5.12 mmol/dL (200 mg/dL) or the patient was under drug treatment for hypercholesterolemia. 21
Hypertriglyceridemia
If serum triglyceride levels were ≥1.69 mmol/l (150 mg/dL) or if under drug treatment for hypertriglyceridemia. 21
Low High-Density Lipoprotein Cholesterol (HDL-C)
If (HDL-C) levels were <1.02 mmol/l (40 mg/dL) for men and <1.28 mmol/l (50 mg/dL) for women. 21
ABC control was defined as the proportion of individuals meeting glycemic (
Given the de-identified data, the study was exempted from formal review by the Institutional Ethics Committee. Only participants who had provided written informed consent to use anonymized medical data were included in the study.
Statistical Analysis
Descriptive analysis was done for continuous and categorical variables. Continuous variables were expressed as mean with standard deviation. Categorical variables were expressed as proportions. One-way ANOVA was used to compare groups for continuous variables, the chi-square test was used for categorical variables. Paired t-test was done to compare the baseline and follow-up data and p-values < 0.05 were considered statistically significant. Statistical analysis was done using IBM SPSS Statistics 27 Version.
Results
Baseline clinical and biochemical details of individuals with T2D who had teleconsultation, hybrid visits, and in-person visits are presented in Table 1. Individuals who opted for teleconsultation had a shorter duration of diabetes compared with those who opted for hybrid visits or in-person visits. Weight was significantly higher and HbA1c, total cholesterol, and LDL cholesterol were significantly lower among the teleconsultation group compared with the hybrid and in-person visit groups. Those who opted for teleconsultation were more likely to reside in Chennai city (as opposed to the rest of Tamil Nadu or India). Individuals who opted for teleconsultation had better glycemic control at baseline. While the prevalence of hypercholesterolemia was significantly less in the only teleconsultation group, there were no significant differences in the prevalence of hypertension between groups. The frequency of patient interactions for teleconsultation and in-person visits was similar with most individuals visiting once in six months.
Baseline Clinical and Biochemical Details of Individuals With Type 2 Diabetes Who Had Teleconsultation, Hybrid Visits, and In-Person Visits at a Tertiary Care Diabetes Center.
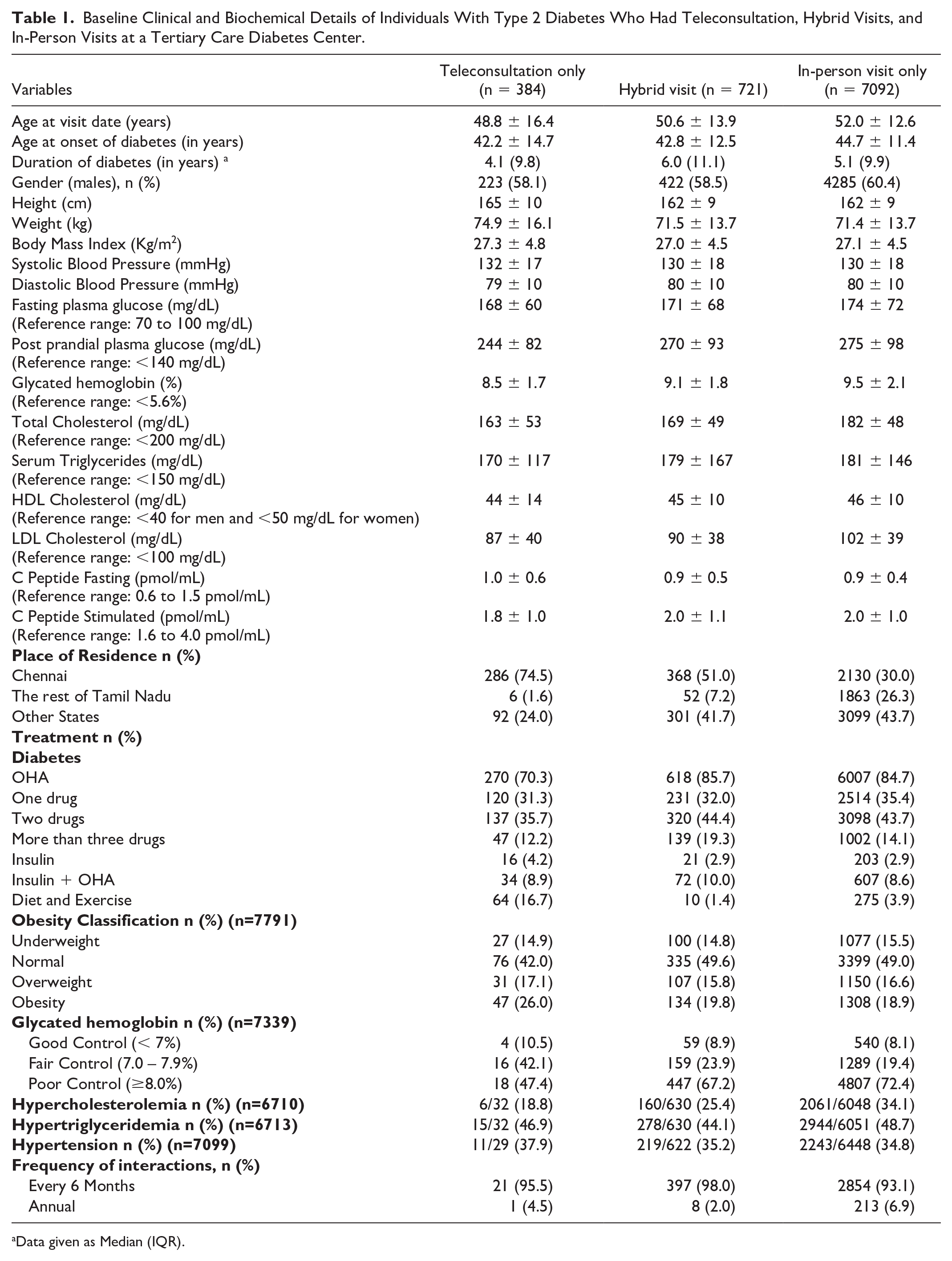
Data given as Median (IQR).
Figure 2 presents the age group-wise distribution of the study participants. It is seen that younger individuals were more likely to opt for teleconsultation whereas hybrid and in-person visits were more common in older age groups.
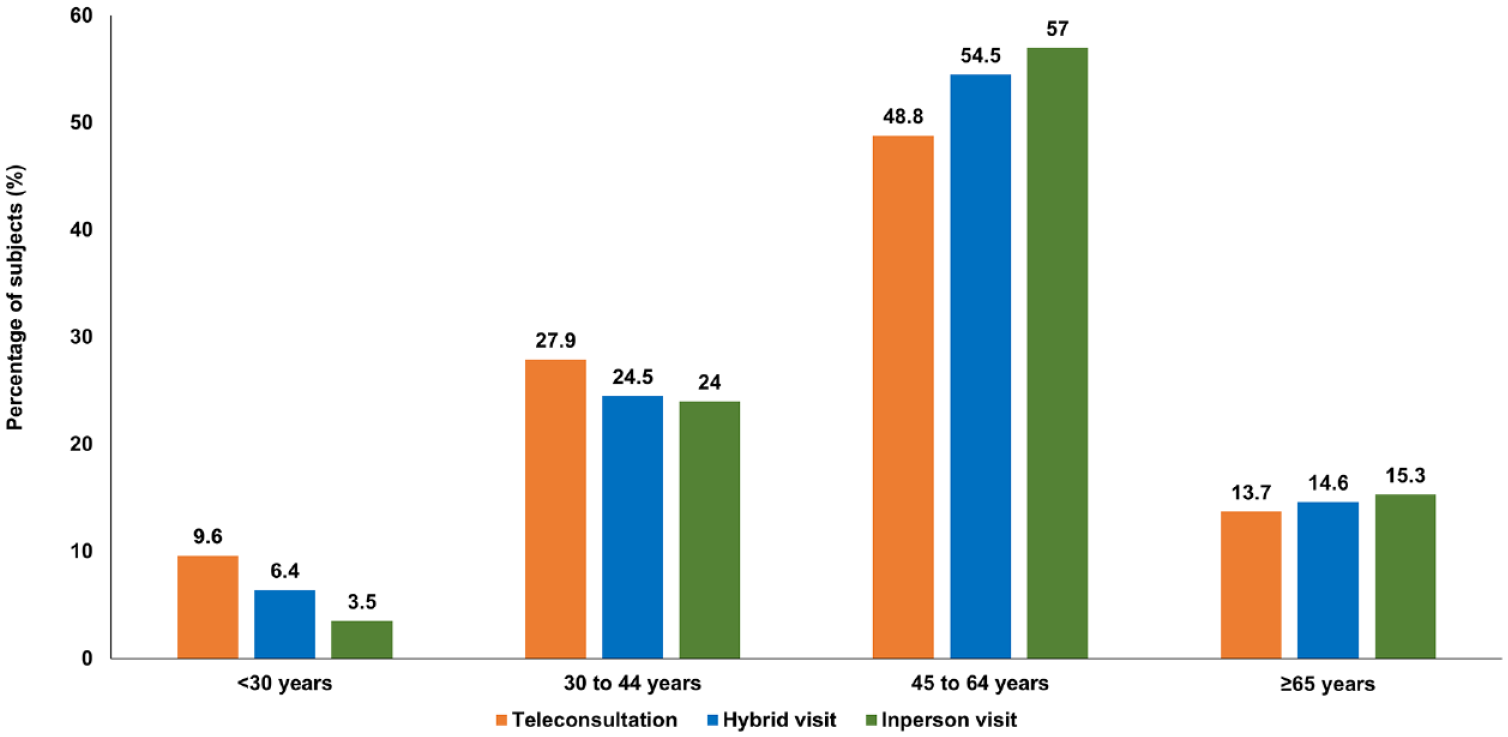
Age group-wise distribution of study participants.
Figure 3 shows the follow-up data of individuals who opted for the three different modes of treatment. Compared with those who had teleconsultation alone, participants who underwent hybrid visits and in-person visits showed greater improvement in mean fasting plasma glucose levels (P < .05) and HbA1c levels (P < .05) after the follow-up. Furthermore, a significantly greater reduction was observed in total cholesterol (P < .05) and LDL cholesterol (P < .05) among individuals who had hybrid visits and in-person visits. Those who opted for teleconsultation alone did not demonstrate any significant reduction in biochemical parameters when compared with the other two groups.
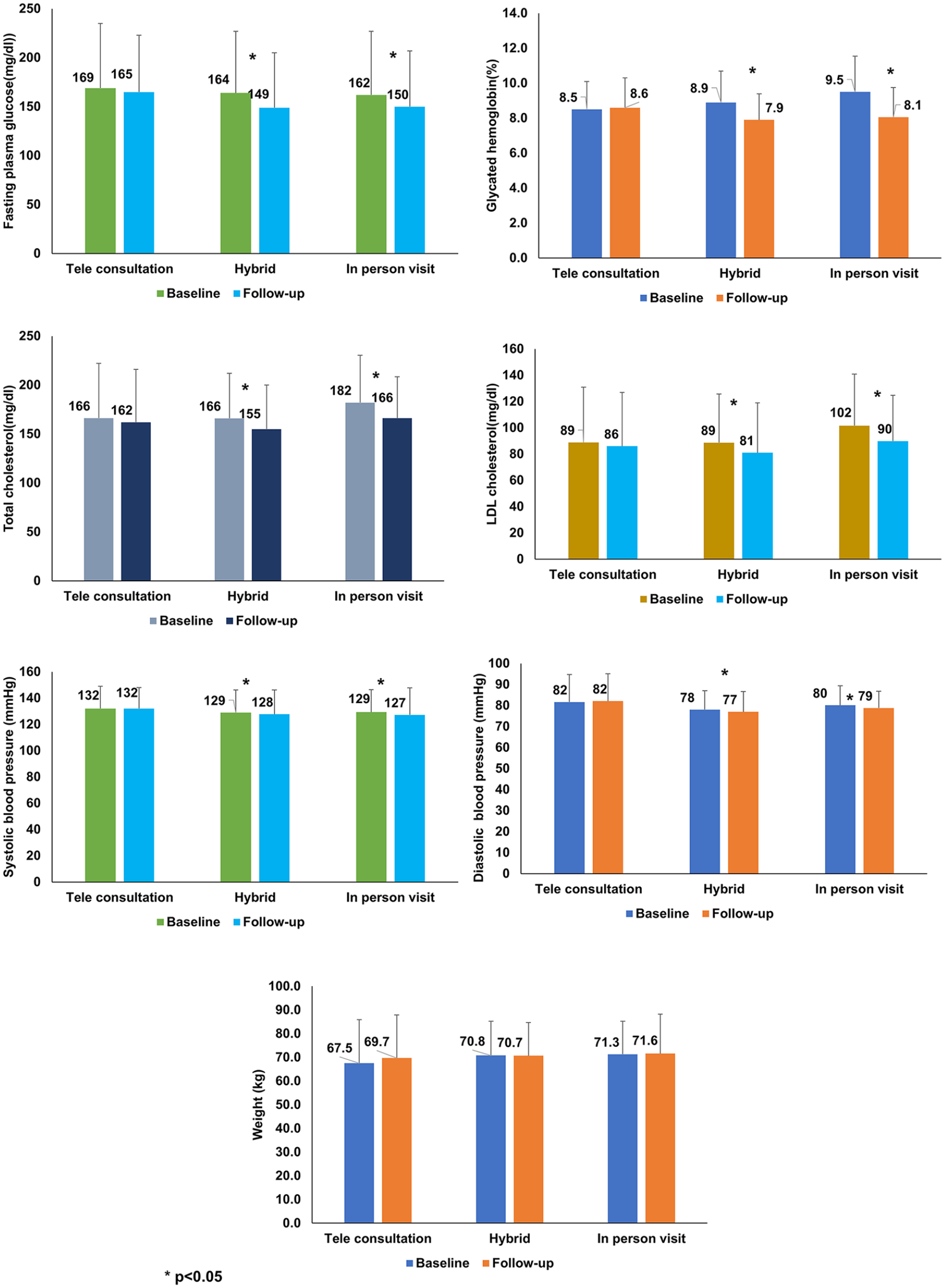
Mean biochemical parameters of baseline and follow-up visits of participants among teleconsultation, hybrid visits and in-person visits.
Figure 4 shows the proportion of individuals in each group who achieved
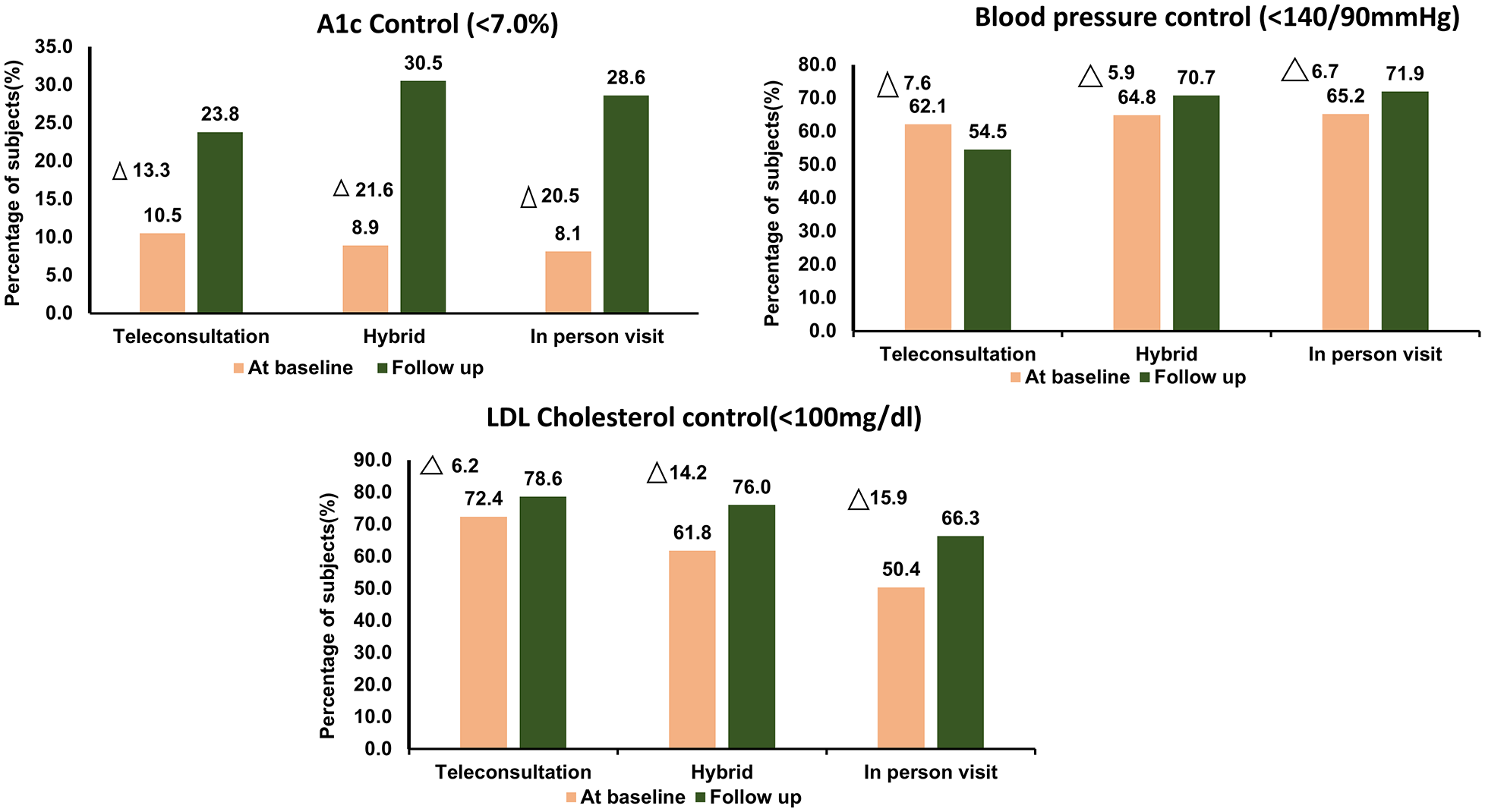
ABC control of study participants.
Discussion
Telemedicine has several advantages over conventional in-person care, especially concerning cost and time. However, until recently, its widespread adoption in India was limited as it was not legalized. In early 2020, the Government of India introduced guidelines for the safe and effective use of telemedicine in India, thanks to the COVID-19 pandemic, at which time access to in-person consultations was difficult or impossible. Telemedicine uptake saw a sharp rise during this period, although some patients still said they preferred in-person consultation. 10
We undertook this study after the COVID-19 pandemic subsided, to compare teleconsultations, hybrid visits (combining both in-person and teleconsultation), and in-person visits for individuals with T2D in our (predominantly outpatient) clinic. Our results show that teleconsultation provides a viable treatment option for those who are well-controlled or have milder forms of T2D. However, for those who have comorbidities or complications, and a longer duration of diabetes, while teleconsultation can be an add-on modality, in-person visits appear to provide better control and achievement of the ABC goals of diabetes management.
In our study, teleconsultation visits were predominantly chosen by individuals in younger age groups, likely due to their higher level of tech-savviness. Conversely, the elderly tended to prefer in-person visits. This preference among the elderly could stem from various factors such as the desire for social interaction during clinic visits, difficulties in using advanced technology (smartphones), more comprehensive clinical evaluations and access to specialists, more time spent with providers to clarify doubts, or simply resistance to change in their established routine for clinic visits.10,22,23
A multisite qualitative study examining telehealth experiences among older adults found that older patients, particularly those with low socioeconomic status, limited health knowledge, hearing impairment, or non-English proficiency, encountered greater challenges with telehealth interactions. 10 To encourage greater adoption of telemedicine among the elderly in the future, efforts should be made to improve internet connectivity, provide education about the advantages of technology, and develop user-friendly applications. In this context, it is worth noting that the mean age of the participants in our study was above 30 years. Had we included younger age groups, the preference for teleconsultation would likely have been greater.
It is also interesting to note that individuals who opted for in-person visits had poorer glycemic control and higher cholesterol levels at baseline compared with those who had teleconsultation or hybrid visits. The symptoms arising from high blood glucose levels could likely have prompted these individuals to choose in-person visits over teleconsultation, despite the inconveniences associated with the former. In contrast, follow-up visit data revealed that participants who had in-person visits and hybrid visits demonstrated better control of glucose and cholesterol levels compared with those who opted for teleconsultation. This raises the possibility that the evaluations and interventions undertaken during teleconsultation, might not be as effective as those following an in-person visit.
The impact of teleconsultation may be compromised due to the inability of the physician to physically examine the patient and assess clinical features and symptom intensity, such as pallor and edema. It should also be noted that video consultation was opted for, by a smaller number of participants. Even though video calls have been reported to be an effective tool for diabetes management, they require a high-quality internet connection, as well as considerations of confidentiality and convenient scheduling at both ends. 24 A cross-sectional study conducted by Abanemai et al 25 found that Saudi Arabian individuals with diabetes expressed a high level of satisfaction with virtual care, particularly females, and it was associated with good adherence to diabetes medication.
At present, it appears that teleconsultations can be a valuable tool for managing chronic conditions such as diabetes, but it is unlikely to completely replace in-person consultations. As suggested by Haimi, 26 issues concerning data security, technical obstacles, and regulatory impediments are some of the concerns that must be addressed during teleconsultations. While technology is advancing rapidly, there is a need for further innovations to ensure that patients from low socioeconomic backgrounds have access to telemedicine services. Despite these challenges, the importance of utilizing telemedicine cannot be overlooked, especially in the context of pandemics like COVID-19 where minimizing the risk of exposure is of utmost importance. 23 While in-person visits are preferred for precise diagnosis, examination, and treatment, telemedicine is favored for its lower costs, infection prevention benefits, and time-saving aspects. 15 Despite several limitations, telemedicine interventions hold promise for diabetes care. Implementing rigorous and ongoing training for intervention teams, securing funding to reduce the cost of telemedicine care, and developing standardized telemedicine systems can accelerate the widespread adoption of telemedicine in diabetes care.27,28
A patient’s socioeconomic status (SES) can significantly influence their choice of consultation method, whether in-person, teleconsultation, or a hybrid of both. Key factors that play a role include access, literacy, convenience, and cost. Patients with lower SES often face challenges in accessing telehealth due to limited access to internet, smartphones, or computers, making in-person visits more appealing. 29 In contrast, higher SES patients typically have better access to technology and are more comfortable using digital health care platforms. While teleconsultations can be more convenient for lower-income patients by eliminating transportation costs, lack of access to necessary devices often forces them to opt for in-person visits. Additionally, health care costs, insurance coverage, and trust in face-to-face care further influence consultation choices. Patients with lower SES and lower health literacy may prefer in-person visits for clearer explanations, while those with higher SES, with more flexible work schedules, often feel comfortable with telehealth due to familiarity with digital tools.26,30
The study’s strength lies in its large sample size and the availability of data from branches in eight states across India. Teleconsultation data were meticulously identified using unique identification numbers assigned to patients at the time of registration, along with information on their mode of calls. However, the study has several limitations, including the short follow-up period, and the low percentage of telemedicine participants with follow-up data. The number of audio consultations was also more than video consultations.
Ultimately it is the choice of individuals with T2D to opt for in-person visits or the choice of teleconsultations (audio versus video) based on their personal preference and medical conditions. Although teleconsultation is a convenient and inexpensive way of managing patients with chronic disease, it needs to be supplemented with regular follow-up and in-person visits whenever necessary to achieve consistent outcomes. In resource-limited settings, telemedicine appears to be a suitable treatment option for those with well-controlled milder forms of diabetes while those who have comorbid conditions might need in-person visits.
Footnotes
Abbreviations
T2D, Type 2 diabetes; ABC,
Author Contributions
RMA conceived the study and was involved in the execution of the work. SJ and SG retrieved data for the analysis. SR and AA did the statistical analysis of the study, wrote the first draft of the article, and made revisions wherever necessary. RMA, RHA, SKR, RU, GP, and VM gave valuable scientific comments and revised the drafts of the article. All authors read the final draft of the article and approved it.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Human and Animal Rights
All procedures followed were by the ethical standards of the responsible committee on human experimentation and with the Helsinki Declaration of 1975, as revised in 2013.
