Abstract

Asteroid hyalosis (AH) is a rare condition in which small, yellow-white spherical particles known as asteroid bodies are present within the vitreous body. Population-based epidemiological and autopsy studies have found a low prevalence of AH, ranging 0.8%-1.2%; association of AH with systemic diseases such as diabetes mellitus (DM) has been proposed but is not well established. Although AH fills the vitreous body with opaque structures, it generally has a minor impact on vision; even in severe cases that render fundus examination impossible, vision is often unaffected. However, its presence may preclude diabetic retinopathy (DR) assessment. 1
The Xavante is a large indigenous group living in Mato Grosso State, Central Brazil, which remained a genetically isolated population, 2 retaining their own complex social organization and cultural values. The Xavante reached a demographic nadir in the late 1950s, but experienced a marked populational increase in the last decades, with the demarcation of their lands, health programs, and establishment of peaceful contacts with non-Indians. 2 Traditionally hunter-gatherers, the Xavantes recently became more sedentary with the demarcation of reserves; they also underwent important dietary changes. As a result, and also probably due to genetic predisposition, DM is now epidemic among them.3,4 In this setting, ophthalmological examination was offered at two Xavante Reserves in January 2020, primarily for DR screening. Villages were selected due to operational conditions in order to optimize field work. Due to the scarcity of ocular health professionals in the region, there was a demand for routine ocular examination even for individuals without diabetes; a total of 158 individuals (59.5% with diabetes) underwent retinal photographs with a handheld smartphone-based device (Eyer, Phelcom Technologies, São Carlos, Brazil).
In the Sangradouro/Volta Grande Reserve (total estimated adult population: 623), 82 individuals from one village were examined; in the São Marcos Reserve (total estimated adult population: 1588), 3 76 individuals from 6 villages were examined. Overall, AH was detected in 17 individuals, a 10.7% frequency rate. Five patients had bilateral AH, and 12 had DM (70.6%); AH distribution among individuals with and without diabetes was not different (chi-square test, P = .417); age (Student’s t-test, P = .533) and gender (chi-square test, P = .579) were not different among groups with and without AH either. Interestingly, many of the individuals with AH were clearly family related (Figure 1). The finding of an abnormally high frequency of AH in this population, in which every village may correspond to one or some extended family units, 5 and its “cluster” distribution in limited geographic areas point to a familial component of inheritance.
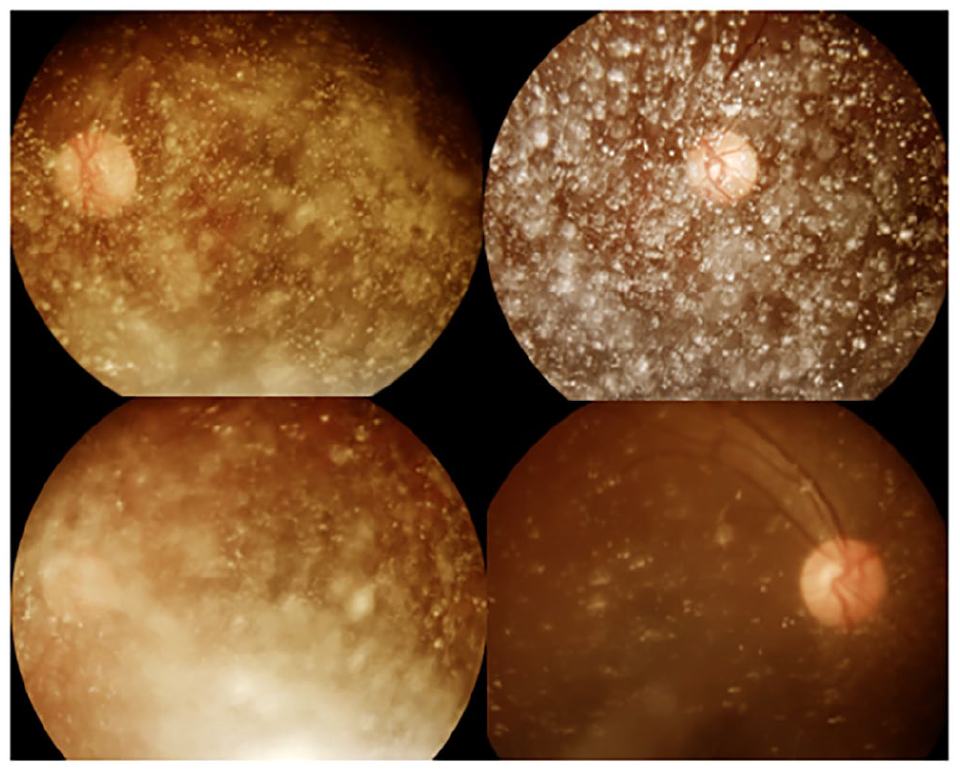
Asteroid hyalosis precluding diabetic retinopathy grading in Brazilian Xavante Indians.
In conclusion, we found an abnormally high frequency of AH in Xavante indigenous individuals, with or without diabetes. Since AH precludes DR screening with retinal photographs, our findings reveal the need for further exams when DR is screened in that population. Further genetic studies are needed in order to shed light on possible inheritance patterns of AH.
Footnotes
Acknowledgements
The authors thank the catholic Salesian Mission and Xavante indigenous community of the São Marcos and Sangradouro/Volta Grande reservations for the collaboration received in the performance of this study. The authors thank Phelcom Technologies for providing the portable retinal camera.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was partially funded by grants from the São Paulo Research Foundation—FAPESP (Proc. 2010/05634-0) and the National Council of Technological and Scientific Development—CNPq (Proc. 476347/2007-6).
